TrumpRx: What’s the Value for Customers?
Editorial Note
This brief was updated on February 24, 2026, to clarify the requirements for health savings accounts.
Introduction
The cost of prescription drugs is a top health policy issue for consumers and policymakers. Half of the people in the United States take at least one prescription drug, and KFF polling from 2025 found that more than 1 in 4 adults under age 65 report difficulty affording their medication; these shares are much higher among those with individual insurance and the uninsured. Aimed at addressing high prescription drug costs, on February 6, 2026, the Trump administration launched TrumpRx, a government website that provides prescription drug discounts to consumers. This Issue Brief examines issues that may impact consumers who access drug discounts through TrumpRx, particularly those with private insurance, and sets out key policy questions going forward.
What is TrumpRx?
In an effort to reduce prescription drug costs, a May 2025 Executive Order seeks to facilitate an option for consumers to purchase prescription drugs at the “most-favored-nation” (MFN) price directly from the drug manufacturer (“direct-to-consumer” purchasing). MFN prices refer to the lowest prices paid in comparable countries. The Trump administration announced that it had made deals with drug manufacturers and negotiated MFN pricing for a range of medications. The details of these deals are confidential and not available to the public.
TrumpRx is an online platform that consumers can use to search for discounted, ostensibly MFN, prices on brand-name medications when paying without using insurance (referred to as “self-pay” or sometimes “cash-pay”). TrumpRx does not offer direct-to-consumer (DTC) purchasing, meaning patients cannot purchase these medications from the TrumpRx website. Instead, for the majority of its advertised drugs, it allows consumers to print drug manufacturer coupons that can be used at retail pharmacies at the time of purchase. Many of the self-pay discounted prices shown on TrumpRx are also available via DTC options on the manufacturer’s website, but in most cases, this requires consumers to go to the manufacturer’s website, search for the drug, and find and interpret the written information describing the discount. Just eight of the advertised drugs on TrumpRx direct consumers to the specific pharmacies (often linked via the manufacturer’s website) where they can purchase the drug directly at the discounted price shown on TrumpRx. In all cases, a valid prescription is still needed to buy the medication.
As of February 20, 2026, 43 different prescription medications from five manufacturers were listed on TrumpRx, used in the treatment of a range of conditions, such as asthma, arthritis, infertility, and diabetes. The 43 prescription drugs currently listed on TrumpRx include one “authorized generic” (of a brand-name product from the same manufacturer) and one biosimilar; the rest are brand-name drugs. There are currently more than 24,000 FDA-approved prescription drugs in the U.S. Additionally, the terms and conditions listed on most of the TrumpRx coupons indicate that they cannot be used in California or Massachusetts. State law in California and Massachusetts prohibit the use of prescription drug coupons unless a generic equivalent is unavailable.
What Sources of Discounted Drug Pricing Already Exist?
Drug discounts have been available for a long time, via different mechanisms and for different populations. From drug manufacturers, there are “copay assistance” coupons for people using private health insurance; free trial offers; discounts for self-pay consumers purchasing the drug directly; and “patient assistance programs” specifically for certain uninsured and/or low-income people. Separately, discounts are offered by several online platforms (such as GoodRx) and online pharmacies (such as Cost Plus Drugs).1
TrumpRx presents one of many avenues for finding discounts on certain drugs. Specifically, those who are insured but choose not to bill through insurance, and those who are uninsured but don’t meet existing requirements for patient assistance programs (such as income), may now be eligible to use these coupons to get discounted prices from manufacturers for drugs included on the platform. While most TrumpRx coupons are also displayed on GoodRx, consumers will find discounts for many more prescription drugs from Cost Plus Drugs and GoodRx than are currently available on TrumpRx.
GoodRx has advertised “exclusive” savings for prescription drugs, including drugs listed on TrumpRx, long before TrumpRx launched. It is not clear how these and other self-pay discounts that drug manufacturers, retailers, or other third-party platforms were already offering before TrumpRx compare to what is available on this new platform. Such comparisons with historic prices are not readily available, but most of the savings from TrumpRx appear to be new. Archived GoodRx pages show that, for most of these drugs, prices available in 2025 or earlier were higher than currently advertised on TrumpRx. Manufacturers with drugs on TrumpRx began announcing their anticipated TrumpRx discounts in late 2025.2 Self-pay discounts for certain dosages of Ozempic, Wegovy, and Zepbound were available prior to TrumpRx and before the Trump administration’s second term, but those prices were higher than their comparable prices now on TrumpRx. According to the manufacturer, the price for the 2 mg dosage of the Ozempic pen ”remains” $499, suggesting that the ”discounted” price shown on TrumpRx does not reflect any recent change.
For those paying with private insurance, many of these drugs already had “copay assistance programs” to help offset some out-of-pocket costs for the commercially insured (and still do). In many cases, out-of-pocket costs could be less than the TrumpRx self-pay discount.
Comparing TrumpRx Self-Pay Discounts to Private Insurance: Issues to Consider
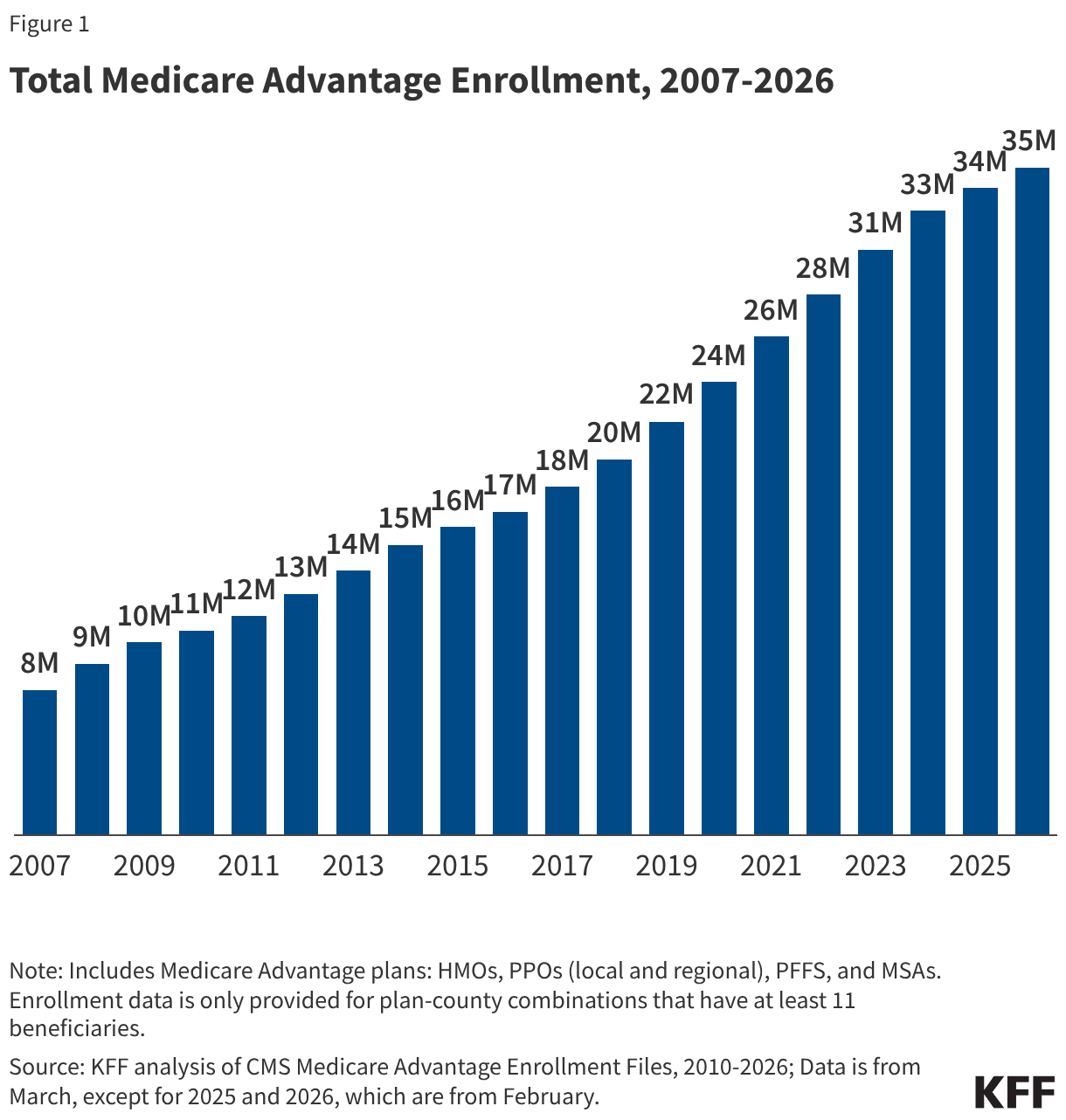
Evaluating the impact of TrumpRx requires a closer look at how most Americans access prescription medication. Sixty-six percent of people under age 65 have private health insurance, including 58% with employer-sponsored coverage and 8% with individual insurance purchased on or off ACA Marketplaces. Nearly all (99%) workers with employer-sponsored coverage are at a firm that provides prescription drug coverage to enrollees in its largest health plan.
The discounts currently advertised on TrumpRx are only available to those purchasing medications without using insurance. The “Frequently Asked Questions” at the bottom of the TrumpRx landing page explicitly state that the discounted pricing is only available for “cash-paying” patients. The webpage for each TrumpRx drug notes that patients with insurance should check what their copay would be if using insurance, as it may be even lower than the TrumpRx price.
Due to the complexity of prescription drug pricing and the variation in private insurance plan designs, several factors need to be considered to evaluate the usefulness of TrumpRx for individual consumers. Three illustrative scenarios are provided below.
Patient has private insurance for a TrumpRx drug, and a generic equivalent is not available
Medication covered by an individual’s private insurance may be less expensive when purchased through insurance. Because TrumpRx coupons are for self-pay consumers, dollars paid for a TrumpRx medication will not count toward a consumer’s insurance deductible or out-of-pocket maximum. In contrast, individuals using private health insurance to purchase the drug instead of the TrumpRx coupon or other manufacturer discount will have their out-of-pocket payments count toward their plan’s deductible and out-of-pocket maximum. Since many of these drugs are used by individuals with chronic illnesses who need their medication throughout the year, the out-of-pocket expenditure may contribute significantly to the deductible and out-of-pocket maximum amounts for the plan, affecting the out-of-pocket costs for other services billed to insurance.
Individuals purchasing through insurance will also have access to a negotiated price through their insurer or employer plan. The “savings” listed on TrumpRx for each drug are based on the manufacturer’s list price for drugs sold to wholesalers or direct purchasers (“wholesale acquisition cost,” or WAC) and typically do not directly reflect what consumers pay. The negotiated prices vary across private plans but are typically lower than the WAC. In such a case, consumers could pay less over the year with their insurance, even having to meet a deductible. Specific cost-sharing arrangements, copay or coinsurance, for the drug depend on the plan formulary, but may also be cheaper than the TrumpRx price.
But deductibles matter. While many patients with private insurance could come out ahead in terms of their annual out-of-pocket costs by using their insurance instead of a TrumpRx coupon or other manufacturer discount for a specific medication, growing insurance deductibles for those with private insurance factor into patient choices and might steer people who have insurance to discounted self-pay options via direct-to-consumer (DTC) manufacturer websites or TrumpRx.
According to the annual KFF Employer Health Benefits Survey (EHBS), among workers covered by employer-sponsored insurance, the average deductible for single coverage was $1,663 in 2025 (including those whose plan does not have a general annual deductible), 23% higher than the average general annual deductible in 2020 ($1,350), and 54% higher than in 2015 ($1,078). Average deductibles are higher for Affordable Care Act (ACA) Marketplace plans sold on HealthCare.gov, though growth over the past decade has increased more slowly than for employer-sponsored plans. In 2025, the average annual individual combined deductible (medical services and drugs) for ACA Marketplace coverage was $2,759. While this is lower than the average deductible in 2020 ($2,962), it is an increase from $1,987 in 2015.3
At least one study has found that for employer-sponsored insurance, out-of-pocket prices for branded retail drugs, on average, increased nearly 6% annually between 2007 and 2020, driven by large increases in deductible and coinsurance payments.
TrumpRx may be an economical option for those who face high out-of-pocket costs for prescription drugs before they meet their plan’s deductible, especially those who do not reach their annual deductible at all. If a consumer, for instance, must pay the retail price for an expensive medication prior to meeting their plan’s deductible, they might look to Trump Rx or DTC self-pay options to reduce their monthly payment for a medication. Self-pay expenses won’t count toward their deductible, but some consumers may choose this option if their monthly income and other household expenses will only allow them to afford the medication at a self-pay discounted price.
Example 1
Terry has a prescription for Prempro to help manage symptoms of menopause. The self-pay discounted price on TrumpRx is $98.84 per month, but she has private health insurance. It is the beginning of the year, though, and Terry has not met any of her plan’s $1,500 annual deductible. If her monthly cost for Prempro is $250 and she has a $30 copay after meeting her deductible, she would pay the full price from January through June, at which point she would have met her $1,500 deductible, then she would just pay the $30 copay from July through December. Assuming no other deductible spending during the year, her total annual out-of-pocket cost for this drug would be $1,680 if she uses her insurance. In this example, she would pay less over the year ($1,186) using the self-pay TrumpRx discount instead of her insurance, though the amount she spends using the discount would not count toward her plan’s deductible or out-of-pocket maximum.
However, some employer plan designs effectively mitigate the impact of high deductibles on prescription drugs. According to the 2025 KFF EHBS, 61% of workers enrolled in an employer-sponsored health plan with a general annual deductible do not have to meet the deductible before prescription drugs are covered. Formularies with a tier for “preferred” brand-name drugs may require a relatively small copay even before the deductible is met. Additionally, 45% of covered workers in firms with 50 or more workers are enrolled in a plan that reduces or waives cost sharing for at least some maintenance drugs for chronic conditions, such as insulin for diabetes.
Example 2
Using the previous example, now assume that Terry’s insurance covers prescription drugs before meeting the deductible, meaning that she is just responsible for the $30 copay for a month of Prempro. Using her insurance to purchase the drug, she would spend $360 over the year, far less than the $1,186 she would spend if she were to pay using the TrumpRx coupon and bypass insurance.
People enrolled in a high-deductible health plan (HDHP) paired with a health savings account (HSA) must pay all medical costs until they meet their high deductible (at least $1,700 for an individual in 2026) to be eligible to establish or contribute funds to an HSA, with some exceptions.4 These pre-deductible coverage exceptions include certain prescription drugs that are ACA-required preventive services, certain insulin products, and other medications deemed preventive for certain chronic conditions. However, beginning this year, people in bronze and catastrophic individual Marketplace plans can establish and contribute to an HSA regardless of whether the plan meets these (and other) requirements. Employer-sponsored plans must still meet these requirements to be paired with an HSA.
For privately insured patients with chronic disease, copay assistance could also be a factor. Manufacturer “copay assistance programs” specifically for consumers using private health insurance are available for over half of the drugs currently available on TrumpRx, which may lower enrollees’ copay and coinsurance payments to as little as $0/month for some drugs, without TrumpRx discounts. Many health plans (group and individual), however, do not count the value of manufacturer copay coupons toward the enrollee’s deductible or out-of-pocket maximum, a feature known as a “copay adjustment program.” As of 2026, at least 25 states and the District of Columbia prohibit or restrict the use of at least some of these types of programs in certain health insurance plans sold in those states.5 These laws do not apply to those in employer self-insured plans regulated only under federal law. Consumers may need to consult their plan documents to find out whether manufacturer copay assistance can be used and, if so, whether their expenses will count toward their plan’s out-of-pocket obligations.
Patient takes a prescription drug that is discounted on TrumpRx, and a generic equivalent is available
According to one analysis, 90% of all prescriptions filled in the U.S. in 2024 were generics. Regardless of the form of payment (private insurance or self-pay), generic equivalents are often cheaper than brand-name drugs, sometimes even after discounts offered through TrumpRx. About half (22) of the drugs on TrumpRx have generic equivalents available in the U.S., at least three-quarters (17) of which are less expensive via GoodRx discounts or direct purchase from Cost Plus Drugs than the TrumpRx coupon price for the brand-name version. Five brand-name drugs on TrumpRx are less expensive on TrumpRx than their generic equivalents on the other two websites. Generic drugs generally have more favorable cost-sharing arrangements than brand-name drugs through insurance, decreasing patient out-of-pocket responsibility for patients using private insurance. Since usual and customary retail prices for these generic drugs are so much lower than their brand-name equivalents, they are cheaper for self-pay patients as well. There is no disclaimer on TrumpRx stating that consumers could pay less than the TrumpRx price by purchasing a generic alternative.
Example 3
Jo has a prescription for Diflucan for an infection. Her insurance has substituted generic fluconazole instead of the brand-name product, with a $10 copay (before deductible) for one bottle. In this case, even with the coupon, it would be cheaper to use her private insurance instead of self-paying with the coupon, which prices Diflucan at $14.06. Additionally, she finds out that the $10 copay will count toward her plan’s out-of-pocket maximum.
If a generic version is available, pharmacists may substitute the generic equivalent for the brand-name drug (and as of 2022, 17 states and the District of Columbia7 required this) unless the prescriber indicates to “dispense as written” on the prescription or the patient specifically requests the brand-name. In these states, a consumer who presents a TrumpRx coupon at the pharmacy for a brand-name drug might automatically end up paying less without using the coupon when the prescription is filled with a generic. Indeed, the “Frequently Asked Questions” at the bottom of the TrumpRx landing page indicates that pharmacies are not required to dispense the TrumpRx discounted drug.
Example 4
Patrick’s physician has written him a prescription for Farxiga for his diabetes. He is uninsured and goes to a pharmacy to fill the prescription. Although the self-pay price is $700, the pharmacist provides a generic equivalent at around half the price. TrumpRx advertises the discounted brand-name drug for a yet lower price of $181.59.
Example 5
Patricia has rheumatoid arthritis and gets a prescription for Azulfidine. She is uninsured and goes to a pharmacy to fill the prescription. Although the self-pay price is $350, the pharmacy only stocks the generic equivalent at $60 a month. This price is lower than the discounted price for the brand-name product advertised on TrumpRx, $99.60.
Patient does not have insurance, or the TrumpRx drug is not covered by their insurance
Those who have already been paying out-of-pocket for certain drugs may see savings from TrumpRx. Some of the drugs on TrumpRx are typically not covered by private health insurance. For example, the KFF Employer Health Benefits Survey found that just one in five (19%) large employers offering health benefits to workers say they cover costly GLP-1 drugs such as Wegovy and Zepbound when used primarily for weight loss in 2025, and fewer than two in five (37%) reported covering fertility medications in 2024. However, some drug discounts on TrumpRx reflect limited-time offers for lower initial doses for new patients. For example, Wegovy pills start at $149/month but increase to $299/month after two monthly fills (for a higher dose).
Example 6
Carol has a prescription for the fertility drug Cetrotide. Her insurance doesn’t cover this drug at all, so she has been buying it from a direct-to-consumer online pharmacy. She pays $49.50 for the generic version, which is more expensive than the brand-name drug with the TrumpRx coupon, at $22.50.
Example 7
Rob receives a prescription to start using Wegovy, which does not have a generic version. He doesn’t have insurance but is able to afford the drug with the one-time introductory offer via TrumpRx of $149 for a month of pills. After that, the monthly price for the drug goes up to $299, making it unaffordable to Rob for continued use even with the discount.
Other patients who could potentially benefit (at least temporarily) from TrumpRx include those who have a gap in insurance coverage, those whose plan formulary has removed coverage for a needed drug, or those whose insurance has utilization management requirements, such as quantity limits or step therapy. As mentioned above, though, since TrumpRx currently only includes 43 drugs, patients will likely find discounts for a much larger selection of drugs using other self-pay discount platforms or from online pharmacies.
Looking Forward
While TrumpRx offers the hope of cheaper medications, whether it will make a significant difference for most people will depend largely on the breadth of prescription drugs available on the website, the cost of the specific medication, state law or pharmacy policy regarding generic drugs, the plan design of the patient’s private insurance plan, if insured, and, particularly for the uninsured, whether there is a less expensive generic version of the drug. This puts a lot more onus on patients, particularly those with private coverage, to understand the many dynamics at play in determining the best option for them. In some cases, TrumpRx advertisement for these discounted brand-name prescription drugs could have the potential to mislead patients into paying more out-of-pocket than they would if they used their insurance and/or purchased a generic alternative.
Future developments that may further impact patient choices include:
- Possible options to allow patients to count discount coupons toward insurance deductibles and out-of-pocket maximums. As part of a February 2026 settlement with the Federal Trade Commission, ExpressScripts, one of the largest pharmacy benefit managers (PBMs) in the country, and its affiliates, agreed to “Provide covered access to TrumpRx as part of its standard offering upon relevant legal and regulatory changes” following allegations that it had created a system that had artificially increased drug prices. Under the proposed consent agreement, enrollees serviced by ExpressScripts or its affiliates would be able to count payments made through the TrumpRx platform toward patient deductibles and out-of-pocket maximums. How this would work in practice, as well as how this would affect other discount platforms, is not clear. Also, patients with private coverage are still awaiting implementation of changes to federal standards regarding the use of copay adjustment programs that could consistently allow manufacturer coupons to count toward their insurance cost sharing.
- Changes to federal law that could expand take-up of high-deductible health plans paired with a health savings account (HSA). The 2025 budget reconciliation law and recent proposed changes increase the availability of Marketplace catastrophic plans. For consumers who turn to these plans, out-of-pocket costs for prescription drugs may increase, potentially steering them to TrumpRx and self-pay DTC options instead of using their insurance. Although, in general, TrumpRx coupons cannot be used with insurance, one manufacturer’s drugs listed on TrumpRx link to the manufacturer’s website, which notes that the expense may be eligible for reimbursement by an HSA.
- Other federal reforms. Broader efforts than a discount website are likely key to addressing system-wide incentives that work to keep prescription drug prices high for all consumers, those with and without insurance. Since most individuals under 65 have employer-sponsored insurance, an important question going forward for this group is whether other current federal efforts, such as recently passed legislation directed at PBM disclosures and pass-through of rebates to employer plans and pending updates to price transparency regulations for prescription drugs, will lower their drug costs.
Endnotes
- GoodRx is a website where consumers can compare discounted self-pay drug prices at retail pharmacies like CVS and Walgreens and access GoodRx coupons whose prices have been negotiated between pharmacies and PBMs. Cost Plus Drugs is an online pharmacy that sells discounted generic (and some brand-name) prescription drugs directly to consumers. ↩︎
- All three manufacturers’ announcements noted that their products would be excluded from the Trump administration’s new tariffs in exchange for committing to these agreements. ↩︎
- Average deductibles vary significantly by metal level and whether the enrollee is eligible for a cost-sharing reduction. ↩︎
- An HSA is a tax-advantaged account that allows people enrolled in certain high-deductible health plans to save and pay for unreimbursed, qualified medical expenses. ↩︎
- See https://theaidsinstitute.org/media/documents/TAI-2025-Report.pdf (21 states as of February 2025; https://www.bleeding.org/news/government-relations-update-may-2025 (3 more states as of May 2025); and https://www.nationalmssociety.org/news-and-magazine/news/new-jersey-copay-accumulator-legislation (another state in 2026). ↩︎
- An 18th state (Indiana) has a similar requirement, but unlike the other state laws, it only applies for Medicare patients. ↩︎