Five Things to Know about the Renewal of Extra Affordable Care Act Subsidies in the Inflation Reduction Act
As part of the Inflation Reduction Act, the Senate recently passed a three-year extension (through 2025) of enhanced subsidies for people buying their own health coverage on the Affordable Care Act Marketplaces. These temporary subsidies were originally slated to last two years (2021 and 2022) and were passed as part of the American Rescue Plan Act (ARPA). The enhanced subsidies increase the amount of financial help available to those already eligible and also newly expand subsidies to middle-income people, many of whom were previously priced out of coverage.
Here’s what to know about the likely renewal of these subsidies:
If signed into law, the Inflation Reduction Act will prevent steep increases in Marketplace premium payments
If Congress extends the temporary subsidies, as appears likely, premium payments in 2023 will hold mostly flat for Marketplace enrollees, since the premium tax credits shelter enrollees from increases in the underlying premium. The passage of the Inflation Reduction Act will extend temporary subsidies, preventing out-of-pocket premium payments from rising across the board next year for virtually all 13 million subsidized enrollees. In the 33 states using HealthCare.gov, premium payments in 2022 would have been 53% higher (more than $700 per year more) on average if not for these enhanced subsidies. The same is true in the states operating their own exchanges. Exactly how much of a premium increase enrollees would have seen in the absence of the Inflation Reduction Act would have depended on the enrollee’s income, age, and the premiums where they live.
For example, using our subsidy calculator, you can see that with the ARPA a 40-year-old couple making $25,000 per year currently pays $0 for a silver plan premium with significantly lowered out-of-pocket deductible costs. That would continue to be true under the Inflation Reduction Act, which continues the ARPA subsidies without interruption for three more years. Using a new version of our subsidy calculator that shows what premium payments in each zip code would have been if the ARPA had not passed, you can see that same couple would have paid $76 per month (or $915 over the course of 2022) without the ARPA. With the Inflation Reduction Act, though, this low-income couple would save $915 per year.
Here’s another example using the new calculator: In the absence of these enhanced subsidies, a 60-year-old couple with an income of $70,000 would have had to pay $1,859 per month (or $22,307 over the course of 2022) for a full-price silver plan. Now, compare this to our 2022 calculator that shows what they currently pay with the ARPA: The same couple currently pays $496 per month (or $5,950 over the course of the year), and would continue to pay a similar amount under the Inflation Reduction Act. Instead of being expected to pay about 32% of their income on insurance, which would likely be unaffordable, the couple is paying 8.5% of their income with enhanced subsidies. So, if Congress passes the Inflation Reduction Act, this older middle-income couple will save over $16,000 per year.
Related: See how 2022 premium payments would increase without the ARPA COVID-19 relief law’s enhanced tax credits. Click the images below to access two versions of the calculator.
The Double Whammy: How 2023 Premium Increases and Subsidy Expiration Would Have Affected Some Enrollees
The Inflation Reduction Act’s renewal of these enhanced subsidies would also prevent some enrollees from experiencing two kinds of premium increases at once. If Congress had allowed enhanced subsidies to expire, the subsidy cliff would have returned, meaning people with incomes over four times poverty (or about $51,520 for a single person) would lose subsidy eligibility altogether. So, without the Inflation Reduction Act, these enrollees would not only pay the increase due to the loss of subsidies, but also any increase in the underlying premium.
Our early look at 2023 premiums shows premiums rising about 10%, with most rate increases falling between about 5% and 14%. This is more than in past years, in part due to inflation and rebounding utilization. These rates are still proposed and will be finalized this month.
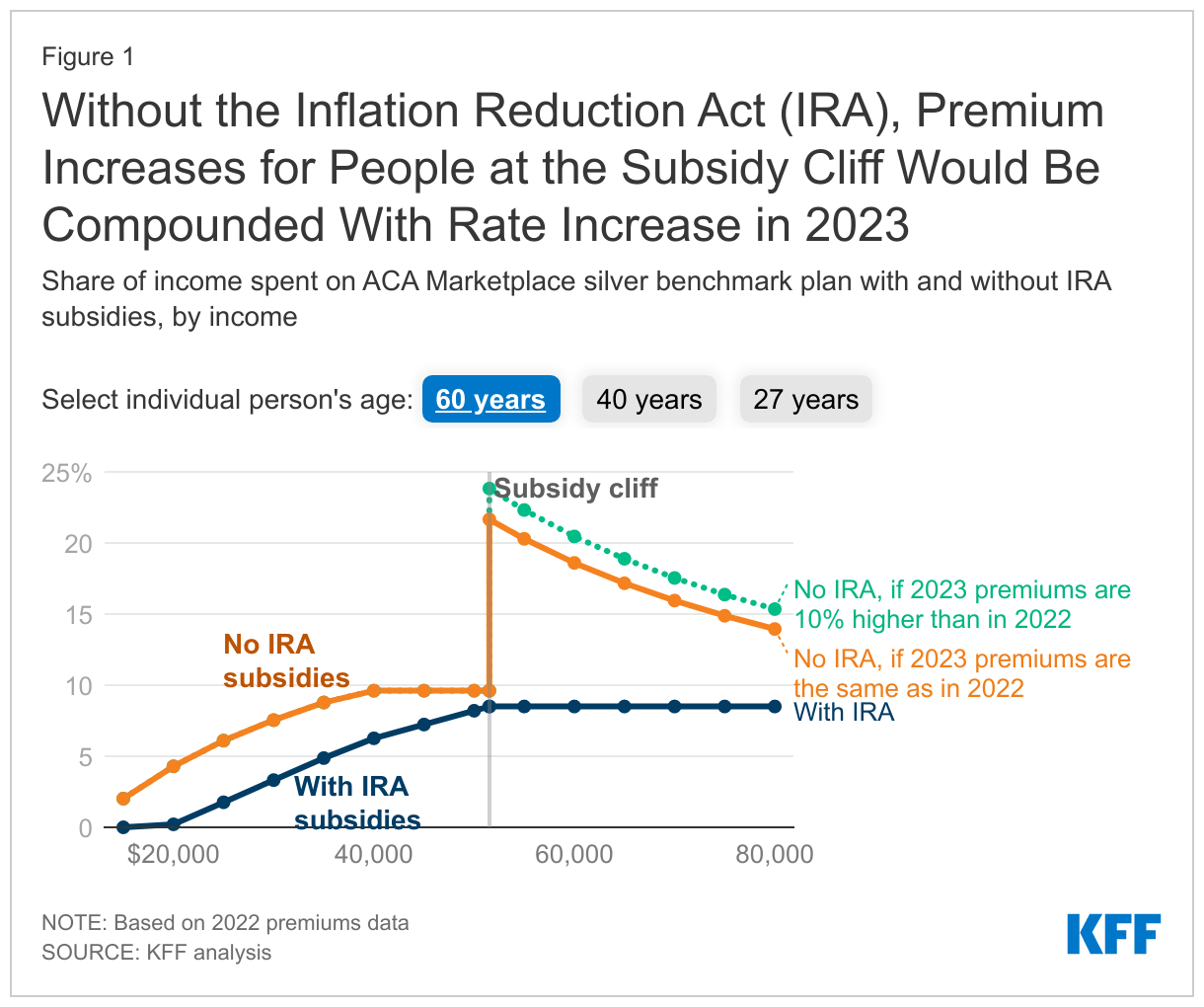
The figure below shows a hypothetical subsidy cliff if premiums do indeed rise by 10%. For example, a 60-year-old making just above four times poverty ($51,521) in 2022 pays 8.5% of their income on a silver plan with enhanced subsidies, but would have paid 22% of their income in 2022 without these subsidies on average across the U.S. If not for the Inflation Reduction Act, and if premiums rise 10% in 2023, this person would pay 24% of their income in 2023.
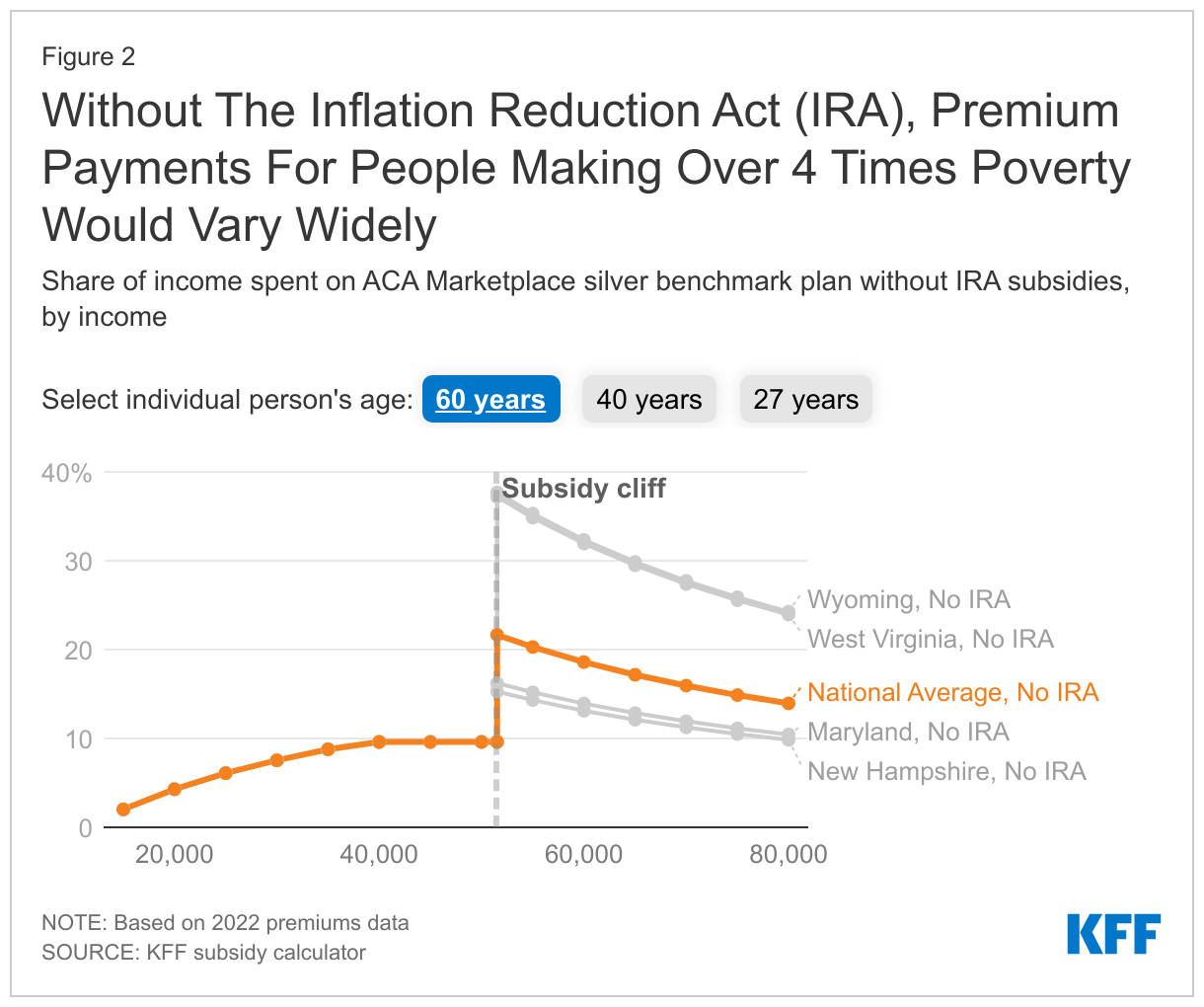
In the states where premiums are currently highest, people losing subsidies would have seen the steepest increases without the Inflation Reduction Act’s continuation of these enhanced subsidies. For example, a 60-year-old making just above four times poverty ($51,521) in 2022 would have paid more than a third of their income on a silver plan without subsidies in West Virginia and Wyoming; and in New Hampshire, the person would have paid 15% of their income without subsidies.
The Ticking Clock: Why the Timing Matters
The timing of the Inflation Reduction Act matters for insurers, regulators, and administrators of state and federal Marketplaces. Insurers are now in the process of finalizing 2023 premiums and some are already factoring in an additional premium increase because they expect ARPA subsidies to expire.
The National Association of Insurance Commissioners (NAIC) wrote to Congress asking to extend these subsidies by July to provide greater certainty as insurers set premiums for next year.
States and the federal government, which operates HealthCare.gov, will need to reprogram their enrollment websites and train consumer support staff on policy changes months ahead of open enrollment this fall.
The End of the Public Health Emergency: How Enhanced Marketplace Subsidies Could Mitigate Coverage Loss
The end of the public health emergency and, with it, the requirement for continuous enrollment in Medicaid is expected to lead to significant coverage losses. So far, the number of uninsured people has not grown during the pandemic and resulting economic crisis. However, ironically, we could see a jump in the uninsured rate as the public health emergency ends if people disenrolled from Medicaid do not find alternative coverage.
With the passage of the Inflation Reduction Act, the enhanced Marketplace subsidies could act as a bridge between Medicaid and the ACA Marketplaces when the public health emergency ends. If enhanced Marketplace subsidies are still in place when the Medicaid maintenance of eligibility (MOE) ends, many people disenrolled from Medicaid could find similarly low-cost coverage on the ACA Marketplaces. If they are eligible for Marketplace subsidies, people losing Medicaid coverage may find Marketplace plans that, like Medicaid, have zero (or near-zero) monthly premium requirement.
The Costs: What This Means for the Federal Budget
Although the Congressional Budget Office (CBO) has not yet released a final score of the Inflation Reduction Act, an early CBO estimate pegged the cost of a permanent extension of enhanced subsidies at about $25 billion per year. The Inflation Reduction Act extends these subsidies for three years (through 2025) – not permanently – though it is likely the average annual cost could be similar. A large part of the estimated cost is due to the CBO’s expectation that millions more people would enroll in the ACA Marketplaces than would if the enhanced subsidies are not extended. The actual cost will depend on how many people enroll and how much premiums rise over the coming years.
Conclusion
Health sector inflation, rising utilization, and other factors may cause 2023 premiums to rise by more than in past years. However, as we’ve written before, Congress’s action to extend the ARPA subsidies through the Inflation Reduction Act will have an even greater influence over how much subsidized ACA Marketplace enrollees pay out-of-pocket for their premiums than will market-driven factors that affect the underlying premium.
Whether subsidies expire at the end of this year or in two or three years, their expiration would result in the steepest increase in out-of-pocket premium payments most enrollees in this market have seen. Because the Inflation Reduction Act extends the enhanced subsidies for three years and not permanently, future Marketplace enrollees may see steep premium increases when the subsidies eventually expire.