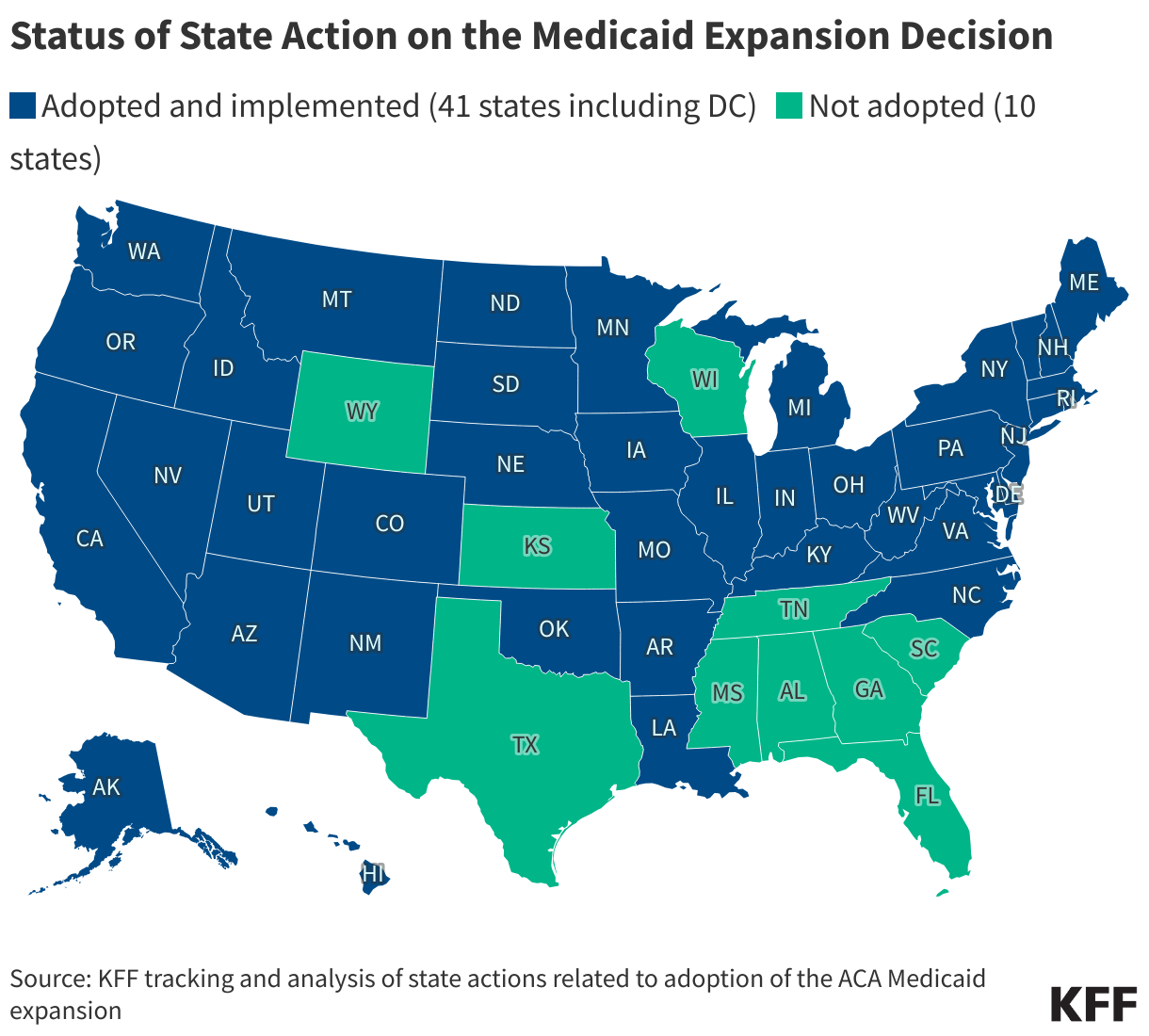
Status of State Medicaid Expansion Decisions
The Affordable Care Act’s (ACA) Medicaid expansion expanded Medicaid coverage to nearly all adults with incomes up to 138% of the Federal Poverty Level ($21,597 for an individual in 2025) and provided states with an enhanced federal matching rate (FMAP) for their expansion populations.
To date, 41 states (including DC) have adopted the Medicaid expansion and 10 states have not adopted the expansion. Current status for each state is based on KFF tracking and analysis of state expansion activity.
These data are also available in a table format. The map may be downloaded as a Powerpoint.
Medicaid Expansion Resources
- Tracking Implementation of the 2025 Reconciliation Law: Medicaid Work Requirements
- 5 Key Facts About Medicaid Expansion
- A Medicaid Per Capita Cap on the ACA Expansion Population: State by State Estimates
- Eliminating the Medicaid Expansion Federal Match Rate: State-by-State Estimates
- Medicaid Expansion is a Red and Blue State Issue
- How Many Uninsured Are in the Coverage Gap and How Many Could be Eligible if All States Adopted the Medicaid Expansion?
- An Update on ACA Medicaid Expansion: What to Watch in North Carolina and Beyond
- A Closer Look at Medicaid Expansion Efforts in Mississippi
- What Does the Recent Literature Say About Medicaid Expansion?: Impacts on Sexual and Reproductive Health
- What Does the Recent Literature Say About Medicaid Expansion?: Economic Impacts on Providers
- New Incentive for States to Adopt the ACA Medicaid Expansion: Implications for State Spending
- The Effects of Medicaid Expansion under the ACA: Studies from January 2014 to January 2020
- Effects of the ACA Medicaid Expansion on Racial Disparities in Health and Health Care
- Building on the Evidence Base: Studies on the Effects of Medicaid Expansion, February 2020 to March 2021
- Medicaid Expansion Enrollment and Spending Leading up to the COVID-19 Pandemic
- Medicaid Waiver Tracker: Approved and Pending Section 1115 Waivers by State
- Eliminating the ACA: What Could It Mean for Medicaid Expansion?
- An Overview of State Approaches to Adopting the Medicaid Expansion
- Medicaid State Fact Sheets