Medicaid Moving Ahead in Uncertain Times: Results from a 50-State Medicaid Budget Survey for State Fiscal Years 2017 and 2018
Benefits, Copayments, Pharmacy, and Opioid Strategies
| Key Section Findings |
| A total of 26 states expanded or enhanced covered benefits in FY 2017 and 17 states plan to add or enhance benefits in FY 2018. The most common benefit enhancements reported were for behavioral health/substance use disorder services and dental services. Most states identified high cost and specialty drugs (including many states that specifically referenced hepatitis C antivirals) as a significant cost driver for state Medicaid programs. The majority (37 states in FY 2017 and 36 in FY 2018) reported actions to refine or enhance their pharmacy programs, especially implementation of new utilization controls (e.g., prior authorization requirements, clinical edits, quantity limits etc.). Thirty-five of 39 MCO states reported that the pharmacy benefit was “generally carved-in.” Of these 35 states, the majority reported requirements that MCOs have uniform clinical protocols (31 states) or uniform preferred drug lists (PDLs) (19 states) that will be in place for one or more drugs as of the end of FY 2018.
What to watch:
Tables 15 and 16 provide a complete listing of Medicaid benefit changes for FY 2017 and FY 2018. Table 17 provides a list of states that reported copayment actions for FY 2017 and 2018, and tables 18 and 19 provide additional details on Medicaid pharmacy benefit management strategies for opioids and naloxone coverage in FFS programs. |
Benefit Changes
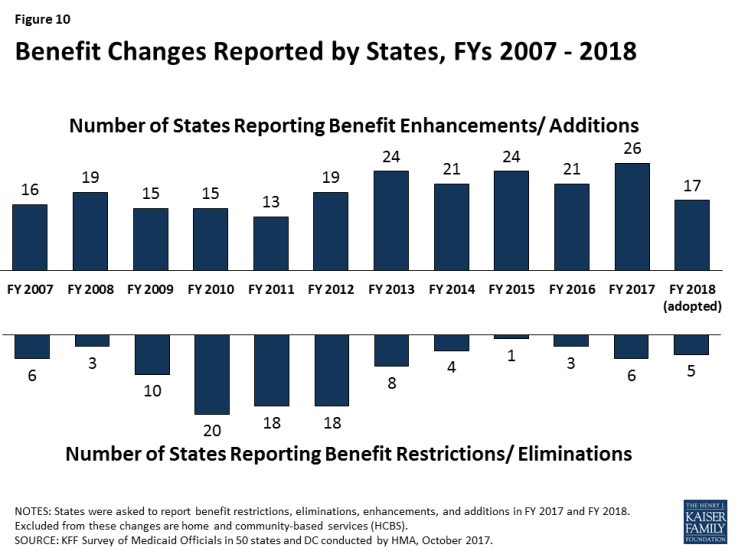
The number of states reporting new benefits and benefit enhancements continues to outpace the number of states reporting benefit cuts and restrictions. Twenty-six states reported new or enhanced benefits in FY 2017, and 17 states plan to add or enhance benefits in FY 2018. Fewer states reported benefit cuts or restrictions – six in FY 2017 and five in FY 2018 (Table 15 and Figure 10).
The most common benefit enhancements reported were for mental health and substance use disorder (SUD) services. Exhibit 12 also highlights states implementing other select benefit enhancements for dental, alternative pain therapies, and telemonitoring/telehealth.
| Exhibit 12: Select Categories of Benefit Enhancements or Additions | ||||
| Benefit | FY 2017 | FY 2018 | ||
| Mental Health/Substance Use Disorder Services | 9 States | IN, MA, NE, NH, NJ, RI, TX, VA, WI | 10 States | CO, HI, IN, MD, NE, NH, OH, UT, VA, WV |
| Dental Services | 5 States | AZ, IN, MD, OR, VT | 3 States | AZ, CA, UT |
| Alternative Pain Therapies (e.g., Chiropractic and Acupuncture) | 4 States | CA, DE, OH, OR | 2 States | IN, OH |
| Telemonitoring/ Telehealth Services | 2 States | NE, RI | 1 State | MD |
Nearly half of states that reported expanded mental health and/or SUD services made the changes as part of a new, comprehensive package of services versus a more limited benefit change. States using Section 1115 authority for SUD enhancements include states responding to CMS guidance2 issued in 2015, which describes a new Section 1115 waiver opportunity that supports states’ ability to provide more effective care to Medicaid beneficiaries with an SUD, including the provision of treatment services not otherwise covered under Medicaid. In addition to the dental and telehealth services benefit enhancements noted in Exhibit 12 and Table 16, many states also reported broader initiatives to increase access to dental care/improve oral health outcomes and to increase access to telehealth. See the “Emerging Delivery System and Payment Reform” section of this report for details on these initiatives.
Other key benefit expansions include:
- Family planning: Oregon is taking many steps to expand access to family planning services. In FY 2017, it added coverage of pharmacist-prescribed oral contraceptives, becoming (according to the state) the first Medicaid program in the country to do so. In FY 2018, it will cover a one-year supply of birth control pills, and is adding coverage of pharmacist-administered contraceptives (e.g., NuvaRing and Depo-Provera). Additional states adding family planning benefits include New Mexico (adding coverage of long-acting reversible contraceptive services as a separately billable service at Federally Qualified Health Centers and Rural Health Centers in FY 2017) and Nevada (adding coverage for a one-year supply of birth control pills in FY 2018).
- Cancer screenings: Four states reported cancer screening-related benefit enhancements. Louisiana and South Dakota added coverage for genetic testing for BRCA3 breast cancer gene mutations in FY 2017, Virginia added coverage for lung cancer screening with low dose computed tomography without prior authorization in FY 2017, and New York added coverage for digital breast tomosynthesis screening services in FY 2018. Louisiana also expanded coverage of breast reconstruction surgery to the contralateral unaffected breast for beneficiaries diagnosed with breast cancer.
Benefit restrictions reflect the elimination of a covered benefit or the application of utilization controls for existing benefits. The most common services restricted were dental services (Connecticut, Nevada, and Wyoming) and non-emergency medical transportation services (Arkansas and Massachusetts); however, most benefit restrictions in FY 2017 or FY 2018 were narrowly targeted. Some states restricting benefits provided exceptions for beneficiaries with mental health conditions or substance use disorders (Massachusetts and Nevada). One additional notable benefit restriction is Utah’s proposal to eliminate Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) coverage for individuals ages 19 to 20 in FY 2018, subject to CMS approval.4
Tables 15 and 16 provide state-level information on benefit changes in FY 2017 and FY 2018.
Copayments
Federal law limits cost-sharing for people with income below 100 percent FPL to “nominal” amounts (defined in federal regulations), with higher amounts allowed for beneficiaries at higher income levels. Certain groups are exempt from cost-sharing, including mandatory eligible children, pregnant women, most children and adults with disabilities, people residing in institutions, and people receiving hospice care. In addition, certain services are exempt from cost-sharing: emergency services, preventive services for children, pregnancy-related services, and family planning services. Also, total Medicaid premiums and cost-sharing for a family cannot exceed 5 percent of the family’s income on a quarterly or monthly basis.5
Most state Medicaid programs require beneficiary copayments, but to varying degrees. Thirteen states reported changes to copayment requirements in either FY 2017 or FY 2018. Details about state actions related to copayments can be found in Table 17 and key changes are described below.
Six states reported new or increased copayment requirements. Key changes include:
- Three states (Michigan, New Hampshire, and New Mexico) reported new or increased copayments for enrollees with income above 100 percent of the FPL. In New Mexico, this change also applies to working individuals with disabilities.
- Three states (Maine, New Mexico, and Utah) reported new or increased copayments for non-emergency use of a hospital emergency department (ED). (These changes are part of pending Section 1115 waiver requests in Maine6 and Utah.)
- Colorado, New Mexico, and Utah are adding or increasing pharmacy copayments. Colorado reported increased copayments for hospital outpatient services.
Seven states reported policies that eliminate or reduce a copayment requirement for some or all covered populations. Key changes include:
- Three states (Indiana, North Dakota, and Tennessee) are reducing or eliminating higher copayments for non-emergency use of the ED.
- Oregon eliminated copayments for preventive services, Utah decreased inpatient copayments, and Vermont exempted sexual assault-related services from copayments.
TABLE 15: BENEFIT CHANGES IN ALL 50 STATES AND DC, FY 2017 AND FY 2018
| States | FY 2017 | FY 2018 | ||
| Enhancements/ Additions | Restrictions/ Eliminations | Enhancements/ Additions | Restrictions/ Eliminations |
|
| Alabama | ||||
| Alaska | ||||
| Arizona | X | X | ||
| Arkansas | X | |||
| California | X | X | ||
| Colorado | X | |||
| Connecticut | X | X | ||
| Delaware | X | |||
| DC | X | |||
| Florida | ||||
| Georgia | ||||
| Hawaii | X | |||
| Idaho | ||||
| Illinois | ||||
| Indiana | X | X | ||
| Iowa | ||||
| Kansas | ||||
| Kentucky | ||||
| Louisiana | X | X | ||
| Maine | ||||
| Maryland | X | X | ||
| Massachusetts | X | X | X | |
| Michigan | X | |||
| Minnesota | X | |||
| Mississippi | ||||
| Missouri | ||||
| Montana | ||||
| Nebraska | X | X | ||
| Nevada | X | X | X | X |
| New Hampshire | X | X | ||
| New Jersey | X | |||
| New Mexico | X | |||
| New York | X | |||
| North Carolina | ||||
| North Dakota | ||||
| Ohio | X | X | ||
| Oklahoma | X | X | X | |
| Oregon | X | X | ||
| Pennsylvania | ||||
| Rhode Island | X | |||
| South Carolina | ||||
| South Dakota | X | |||
| Tennessee | X | |||
| Texas | X | |||
| Utah | X | X | ||
| Vermont | X | |||
| Virginia | X | X | ||
| Washington | ||||
| West Virginia | X | X | ||
| Wisconsin | X | |||
| Wyoming | X | X | ||
| Totals | 26 | 6 | 17 | 5 |
|
NOTES: States were asked to report benefit restrictions, eliminations, enhancements, and additions in FY 2017 and FY 2018. Home and community-based services (HCBS) and pharmacy benefit changes are excluded from this table.
SOURCE: Kaiser Family Foundation Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2017.
|
||||
Table 16: States Reporting Benefit Actions Taken in FY 2017 and FY 20187
| State | Fiscal Year | Benefit Changes |
| Arizona | 2017 | Adults (+): Add coverage for podiatry services (August 6, 2016).
LTSS Adults (+): Add a $1,000 per year dental benefit for MLTSS beneficiaries (October 1, 2016). |
| 2018 | Adults (+): Add a $1,000 per year benefit for emergency dental services (October 1, 2017).
Adults (+): Add coverage of outpatient occupational therapy services (October 1, 2017). |
|
| Arkansas | 2017 | Expansion Adults (-): Eliminate non-emergency medical transportation coverage for expansion adults participating in Employer Sponsored Insurance feature of the Section 1115 waiver renewal (January 1, 2017). |
| California | 2017 | All (+): Restore acupuncture services (eliminated in 2009 for most populations excluding children, pregnant women, and nursing facility residents) (July 1, 2016).
Pregnant Women (+): Add licensed midwives to the Comprehensive Perinatal Services Program (July 1, 2016). |
| 2018 | All (nc): Reaffirm coverage of non-emergency medical transportation as provided in state law (July 1, 2017).
Adults (+): Fully restore coverage for dental services (January 1, 2018). |
|
| Colorado | 2018 | Pregnant Women (+): Add coverage of up to three post-partum depression screenings in the first year following a child’s birth (July 1, 2017).
Adults (+): Add coverage for Physical Therapy/Occupational Therapy services above the 12-hour cap with prior authorization (November 1, 2017). Children (+): Restore coverage of routine circumcisions as an elective benefit. |
| Connecticut | 2017 | Children (-): Apply additional restrictions on coverage of sealants and filling restorations (September 1, 2016). |
| 2018 | Adults (-): Apply annual cap on coverage for dental services (pending passage of FY 2018 state budget). | |
| Delaware | 2017 | Non-expansion Beneficiaries (+): Add coverage of chiropractic services (July 1, 2017). |
| District of Columbia | 2017 | All (+): Add Health Home services (“My Health GPS”) for beneficiaries with three or more chronic conditions (July 1, 2017). |
| Hawaii | 2018 | Adults (+): Expand mental health and substance abuse benefits including addition of intensive case management and tenancy supports for beneficiaries classified as chronically homeless (upon CMS approval). |
| Indiana | 2017 | All (+): Add coverage of physician-administered fluoride varnish (January 1, 2017).
All (+): Expand coverage of tobacco dependence treatment (January 1, 2017). |
| 2018 | Adults (+): Add coverage of chiropractic spinal manipulation for HIP Plus enrollees (February 1, 2018).
All (+): Add coverage of new substance use disorder treatment services, including expanded inpatient detoxification, additional residential services, addiction-specific outpatient treatment services, peer recovery supports, and relapse prevention (February 1, 2018). Adults (+): Increase member incentives for healthy behaviors to $200 per initiative, with a total of no more than $300 annually for HIP Basic and HIP Plus enrollees (February 1, 2018). |
|
| Kansas | 2017 | Children (nc): Expand Autism-related services by moving three services from HCBS waiver coverage to State Plan coverage (January 1, 2017). |
| Kentucky | 2018 | All (nc): Expand non-emergency medical transportation services to include travel to pharmacies (July 1, 2017). |
| Louisiana | 2017 | Pregnant Women (+): Add coverage of mosquito repellant, when prescribed by a physician, for pregnant women and women trying to conceive as a Zika virus prevention measure (July 1, 2016).
All (+): Add coverage of genetic testing for BRCA 1 and BRCA 2 breast cancer gene mutations (July 1, 2016). All (+): Expand coverage of breast reconstruction surgery to the contralateral unaffected breast for beneficiaries diagnosed with breast cancer (October 1, 2016). |
| 2018 | All (+): Expand coverage of preventive services eligible for the one percent increase in federal match under Section 4106 of the ACA (May 1, 2017). | |
| Maryland | 2017 | Children (nc): Add coverage for Applied Behavioral Analysis services for children with autism spectrum disorder to meet federal requirements (January 1, 2017).
Foster Children (+): Expand coverage for dental services for former foster children up to age 26 (January 1, 2017). |
| 2018 | Adults (+): Add substance use disorder residential treatment services (July 1, 2017).
All (+): Add coverage of remote patient monitoring for beneficiaries who meet qualifying medical criteria (January 1, 2018). |
|
| Massachusetts | 2017 | All (+): Expand coverage of substance use disorder treatment services to include residential rehabilitation services and transitional support services (November 4, 2016). |
| 2018 | Medicaid Expansion (-): Eliminate coverage of non-emergency transportation services, except for transportation to substance use disorder treatment services for Medicaid expansion beneficiaries (November 1, 2017).
All (+): Add coverage of enhanced “flexible services” as an incentive for beneficiaries to enroll in an ACO (March 1, 2018). |
|
| Michigan | 2017 | Non-expansion Adults (+): Add coverage of preventive services assigned a grade A or B by the United States Preventive Services Task Force (USPSTF) (July 1, 2017). |
| Minnesota | 2017 | All (+): Add coverage of kidney transplants under Emergency Medical Assistance to eligible beneficiaries who are currently receiving dialysis services (July 1, 2016).
All (+): Add coverage of gender confirmation surgery (January 1, 2017). All (+): Add coverage of community emergency medical technician services after discharge from a hospital or nursing home, and for safe home checks (January 1, 2017). |
| Nebraska | 2017 | Children (+): Add coverage for Multisystemic Therapy/Family Functional Therapy (July 1, 2016).
All (+): Add coverage of telehealth services, including telemonitoring and originating site fee (January 1, 2017). |
| 2018 | All (+): Add coverage of nutrition services (July 1, 2017).
All (+): Add coverage of peer support services (July 1, 2017). |
|
| Nevada | 2017 | All (-): Reduce coverage of targeted case management services, to 10 hours in the initial month and five hours in the following three consecutive calendar months for adults without serious mental illness and children without serious emotional disturbance (February 23, 2017).
All (+): Added coverage for paramedicine services (July 1, 2016). |
| 2018 | Non-expansion Beneficiaries (+): Add coverage of podiatry services (January 1, 2018).
Non-expansion Beneficiaries (+): Add coverage of registered dietician services (July 1, 2017). Non-expansion Beneficiaries (+): Add coverage of home health durable medical equipment services (July 1, 2017). Non-expansion Beneficiaries (+): Add coverage of gender dysphoria services (January 1, 2018). Non-expansion Beneficiaries (-): Limit coverage of private duty nursing services and hospice services (July 1, 2017). Non-expansion Beneficiaries (-): Limit coverage of orthodontia services (July 1, 2017). Non-expansion Beneficiaries (-): Limit coverage of case management services with additional prior authorization requirements (July 1, 2017). All (+): Add coverage of one-year supply of birth control pills (July 1, 2017). |
|
| New Hampshire | 2017 | Non-expansion Adults (+): Expand coverage of substance use disorder treatment services, to include assessment, outpatient services, residential treatment, opioid treatment programs, recovery support services, and recovery monitoring (July 1, 2016). |
| 2018 | Children (+): Expand coverage of behavioral health services for children with serious emotional disturbance (January 1, 2018). | |
| New Jersey | 2017 | Non-expansion Adults (+): Expand substance use disorder benefit to align with the state’s Alternative Benefit Package for Medicaid expansion beneficiaries (July 1, 2016). |
| New Mexico | 2017 | All (+): Add coverage of long-acting reversible contraception services as a separately billable service at FQHCs and RHCs (September 1, 2016).
All (+): Add coverage of medication monitoring services by nurses and physician assistants (January 1, 2017). Pregnant Women (nc): Add coverage of licensed birthing centers as a new provider type to meet federal requirements (February 25, 2017). |
| New York | 2018 | Children (+): Add coverage of pasteurized donor human breast milk for infants <1500 grams (April 1, 2017).
All (+): Add coverage of continuous glucose monitoring devices for beneficiaries with Type 1 diabetes (September 1, 2017). All (+): Add coverage of digital breast tomosynthesis (DBT) screening services (September 1, 2017 for FFS and November 1, 2017 for managed care). All (+): Add limited infertility benefit for women between the ages of 21 to 44 (September 1, 2017, pending CMS approval). |
| North Dakota | 2017 | Children (nc): Add coverage for Applied Behavioral Analysis services for children with autism spectrum disorder to meet federal requirements (June 1, 2017). |
| Ohio | 2017 | All (+): Add coverage of acupuncture services (January 1, 2017). |
| 2018 | All (+): Expand coverage of behavioral health services to include assertive community treatment for adults, family counseling, intensive home-based treatment for youth at risk of out-of-home placement, and primary care services delivered by a behavioral health provider (January 1, 2018).
All (+): Expand provider types who may provide acupuncture services (October 1, 2017). |
|
| Oklahoma | 2017 | Children (+): Mandate polycarbonate lenses for children (September 1, 2016).
Pregnant Women (-): Limit high-risk obstetrical services, such as quantity limits on ultrasounds (September 1, 2016). All (+): Provide coverage of non-emergency medical transportation services for additional passengers (October 1, 2016). Children (+): Remove barriers to receiving school-based services for children with IEPs (November 1, 2016). |
| 2018 | Adults (-): Eliminate coverage of non-mandatory over-the-counter drugs (October 1, 2017). | |
| Oregon | 2017 | Adults (+): Restore previously cut restorative dental benefits (relaxed limitation criteria for dentures; coverage for crowns; scaling and planning) (July 1, 2016).
Adults (+): Expand coverage for alternative back pain therapies including acupuncture, chiropractic manipulation, and yoga (July 1, 2016). Children (nc): Added coverage for Applied Behavioral Analysis services for children with autism spectrum disorder to meet federal requirements (July 1, 2016). All (+): Add coverage of pharmacist-prescribed oral contraceptives, as permitted under state law (January 1, 2017). |
| 2018 | All (+): Add coverage of one-year supply of birth control pills and pharmacist-administered contraceptives (i.e., NuvaRing and Depo-Provera) (January 1, 2018).
All (+): Add coverage of other pharmacist-prescribed medications (TBD), as permitted under state law (January 1, 2018). |
|
| Rhode Island | 2017 | All (+): Add coverage for home stabilization services.
All (+): Add coverage for telehealth services in new managed care contracts. Adults (+): Implement the Sobering Treatment Opportunity Program (STOP), an ER diversion pilot in Providence that will cover an overnight stay and referral to appropriate counseling for beneficiaries with chronic alcohol dependence who are homeless. |
| South Carolina | 2018 | Children (nc): Add autism spectrum disorder services to the State Plan for eligible beneficiaries up to age 21 to meet federal requirements (July 1, 2017). |
| South Dakota | 2017 | Adults (+): Add coverage of genetic testing for BRCA breast cancer gene mutations (July 1, 2016). |
| Tennessee | 2017 | Adults (-): Limit Allergy Immunotherapy to clinical practice guidelines (July 1, 2016). |
| Texas | 2017 | Children (+): Add coverage for family therapy without the patient present as a benefit for children under age 21 (January 1, 2017).
Children (+): Add coverage for Prescribed Pediatric Extended Care Centers for medically fragile children receiving extensive private duty nursing services at home, up to 12 hours (July 1, 2017). |
| Utah | 2018 | All (+): Add coverage of screening, brief intervention, and referral to treatment services (July 1, 2017).
Aged, Blind or Disabled (+): Add coverage of dental services for the blind and disabled (July 1, 2017). Adults (-): Eliminate EPSDT coverage for parents and childless adults age 19 to 20 (effective the later of January 1, 2018, or upon CMS approval). |
| Vermont | 2017 | All (+): Allow licensed dental hygienists to bill Medicaid directly (July 1, 2016). |
| Virginia | 2017 | All (+): Expand coverage of addition recovery treatment services, including residential treatment, day treatment/partial hospitalization, intensive outpatient treatment, medication-assisted treatment, substance use case management, inpatient detoxification, inpatient substance use disorder treatment, and residential or inpatient substance use disorder treatment in an institution of mental disease with greater than 16 beds (April 1, 2017).
All (+): Add coverage of lung cancer screening with low dose computed tomography without prior authorization (January 1, 2017). |
| 2018 | Traditional Beneficiaries (+): Add coverage for peer support services for beneficiaries with serious mental illnesses and/or substance use disorders (July 1, 2017).
Limited Adult Coverage Group (+): Expand coverage of addiction recovery and treatment services and add coverage for peer support services for beneficiaries with serious mental illnesses and/or substance use disorders (October 1, 2017). |
|
| West Virginia | 2017 | All (+): Expand coverage of Hepatitis C antiviral agents with a revised clinical policy (April 1, 2017). |
| 2018 | All (+): Expand coverage of substance use disorder services, including services provided by institutions for mental disease, peer recovery support services, and Naloxone treatment (January 1, 2018). | |
| Wisconsin | 2017 | All (+): Add licensed midwives as an allowable Medicaid provider (January 1, 2017).
All (+): Add coverage of residential substance abuse treatment through comprehensive community service programs (May 1, 2017). |
| Wyoming | 2017 | All (+): Add coverage for dietician services (July 1, 2016).
Aged, Blind and Disabled (-): Reduce nursing facility bed-hold days (October 1, 2016). Aged, Blind and Disabled (-): Limit behavioral health, therapy, and home health services by imposing soft caps (January 1, 2017). Adults (-): Eliminate coverage of dental services. |
Table 17: Copayment Actions Taken in the 50 States and DC, FY 2017 and FY 20188
| State | Fiscal Year | Copayment Changes |
| Colorado | 2018 | Increase: Increase pharmacy copayment to $3.00 per prescription for all non-exempt eligibility groups (1/1/2018).
Increase: Double the hospital outpatient copayments for all non-exempt eligibility groups (1/1/2018). |
| Delaware | 2018 | Decrease: Treatment of pre-eligibility medical expenses in determining post eligibility cost of care contribution for LTSS population; “look-back” period expanded from 30 days to 90 days. Potential to reduce the monthly “patient pay” amount (effective date dependent on SPA approval). |
| Indiana | 2018 | Decrease (for HIP 2.0 expansion population): Eliminating the graduated copayment for non-emergent ER use (2/1/2018). |
| Maine | 2018 | New: Maine’s Section 1115 waiver would impose a copay on all populations for non-emergent use of the ED. (Dual eligibles, those in institutions and a few other groups are exempt.) |
| Michigan | 2017 | Increase (for adult enrollees with incomes between 100% and 133% FPL): Increase in prescription, hospital, and office visit copays. Copays were doubled (4/1/2017). |
| New Hampshire | 2018 | Increase (for adult enrollees with incomes between 100% and 133% FPL): Increase in Copayments for Inpatient Hospital, Primary and BH Care, Imaging, X-rays, and PT/OT Services (1/1/2018). |
| New Mexico | 2018 | New (for most populations): Copays for brand-name prescriptions when there is a less expensive generic equivalent medicine available (1/1/2018).
New (for most populations): Copays for non-emergency use of the emergency department (1/1/2018). New (for Working Disabled, Adult expansion group with income above 100% FPL): New copayments for outpatient office visits (excluding behavioral health), inpatient stays, outpatient surgeries, and pharmacy (1/1/2018). |
| North Dakota | 2017 | Elimination (for all Medicaid groups): Higher copayment for non-emergency use of the ER was eliminated (1/1/2017). |
| Oregon | 2017 | Elimination (for all Medicaid groups): Copayments were eliminated for preventive services, office visits, and pharmacy (1/1/2017). |
| Tennessee | 2017 | Decrease (for waiver-eligible children): Copayment for non-emergency use of the ER was reduced from $10 to $8.20 (12/16/2016). |
| Utah | 2018 | Decrease: Inpatient copayments will be reduced to comply with federal maximum (date TBD).
Increase: Outpatient copayments are being increased for all but children and pregnant women (date TBD). Increase (for current enrollees and childless adults): Establish a $25 copay for non-emergency use of the ER (1/1/18). Increase: Increase pharmacy copayments. |
| Vermont | 2017 | Decrease: Remove copays for sexual assault-related services for all Medicaid groups (10/1/2016). |
| West Virginia | 2018 | Neutral: Changing from a tiered copayment based on cost to $1 generic and $3 brand (date TBD). |
Prescription Drug Utilization and Cost Control Initiatives
Almost all states have implemented aggressive strategies to slow Medicaid spending growth for prescription drugs, including preferred drug lists (PDLs), supplemental rebate programs, and state maximum allowable cost programs. In recent years, however, a disproportionate increase in prescription drug costs relative to overall spending has heightened state attention on pharmacy reimbursement and coverage policies. In this year’s survey, states reported a variety of actions in FY 2017 and FY 2018 to refine and enhance their pharmacy programs, including actions to react to new and emerging specialty and high-cost drug therapies.
Pharmacy Cost Drivers
This year’s survey asked states to identify the biggest cost drivers that affected growth in total pharmacy spending9 (federal and state) in FY 2017 and projected for FY 2018. Consistent with the results of the 2015 and 2016 surveys, most states identified specialty and high cost drugs as the most significant cost driver, with many states pointing specifically to hepatitis C antivirals. For these drugs, high costs are attributable to the high per prescription cost as well as increased utilization. Two states (Georgia and Tennessee) noted that they are seeing hepatitis C antiviral costs moderating (although costs remain high compared to other drugs). Other specialty drugs, behavioral health, and/or substance use disorder drugs were cited as cost drivers, and some specific drug classes (such as hemophilia factor, oncology drugs, and diabetes products) were also identified as major cost drivers. For FY 2018, several states also cited a new spinal muscular atrophy drug (Spinraza), priced at $125,000 a dose, or $750,000 for the first year and $375,000 per year thereafter for life (due to fewer doses per year).
| Medicaid Covered Outpatient Drug Final Rule |
|
State Medicaid programs historically reimbursed pharmacies for the “ingredient cost” of each prescription using an Estimated Acquisition Cost (EAC), plus a dispensing fee.10 The new federal Covered Outpatient Drug final rule11 replaced EAC with “Actual Acquisition Cost” (AAC) and required states to provide a “professional dispensing fee” that reflects the pharmacist’s professional services and costs to dispense a drug to a Medicaid beneficiary. States can determine their own AAC prices or use the pricing files published and updated weekly by CMS – the “National Average Drug Acquisition Costs” (NADACs) – which are derived from outpatient drug acquisition cost surveys of retail community pharmacies.12 Some states had already transitioned to an AAC methodology prior to the issuance of the final rule, but all other states were required to come into compliance by April 1, 2017. The new methodology generally results in lower ingredient cost reimbursement but higher dispensing fees.
–
This year’s survey asked states whether implementation of the rule’s AAC and professional dispensing fee requirements was expected to result in budget savings or greater costs, or be budget neutral. Most states reported that implementation of the rule was expected to have a budget neutral impact (16 states) or result in savings (12 states). Fourteen states reported an expectation of greater costs.13 Several states reported adoption of an AAC methodology prior to FY 2017 (8 states), and one of these states (Idaho) commented that it was continuing to achieve savings as a result of Medicaid provider rate changes and provider taxes and fees in place in FY 2017 and FY 2018. For purposes of this report, implementation of the Covered Outpatient Drug final rule is not counted as a cost containment action because it is an implementation of a federal regulatory requirement.
|
Pharmacy Cost Containment Actions in FY 2017 and FY 2018
Almost all states had prescription drug cost containment policies (including prior authorization requirements and PDLs) in place prior to FY 2017, and most are constantly refining and updating these policies. Although states may not have reported every refinement or routine change in this year’s survey, 37 states in FY 2017 and 36 states in FY 2018 reported implementing or making changes to a wide variety of cost containment initiatives in the area of prescription drugs, comparable to the number of states taking such actions in recent years. By far the most frequently cited action was the application of new or expanded utilization controls (e.g., prior authorization requirements, clinical edits, and quantity limits) reported by 32 states in FY 2017 and 29 in FY 2018. Sixteen states in FY 2017 and 17 in FY 2018 also reported new or expanded initiatives to generate greater rebate revenue, including New York which is implementing a new state law in FY 2018 that applies a cap on Medicaid drug expenditures as a separate component of the global state Medicaid spending cap that the state has had in place since 2011. If the state determines that drug spending will exceed the annual growth limit, the Commissioner of the Department of Health may identify and refer drugs to the Drug Utilization Review (DUR) Board for a recommended target supplemental rebate.
Other frequently cited newly implemented or expanded pharmacy cost containment actions were:
- Provider education or profiling initiatives (14 states in FY 2017 and 16 in FY 2018)
- Initiatives to reduce pharmacy-related fraud, waste, and abuse (13 states in FY 2017 and 14 in FY 2018)
- Medication therapy management programs (8 states in FY 2017 and 7 in FY 2018)
Managed Care’s Role in Delivering Pharmacy Benefits
Since the passage of the ACA, states have been able to collect rebates on prescriptions purchased by managed care organizations (MCOs) operating under capitated arrangements. As a result, many states have chosen to “carve in” the pharmacy benefit to their managed care benefits. As more states have enrolled additional Medicaid populations into managed care arrangements over time, and as Medicaid enrollment has increased due to ACA coverage expansions, MCOs have played an increasingly large role in administering the Medicaid pharmacy benefit. In this year’s survey, states with MCO contracts were asked whether pharmacy benefits were covered under those contracts as of July 1, 2017.
Of the 39 states contracting with comprehensive risk-based MCOs, 35 states reported that the pharmacy benefit was “generally carved-in (with possible exceptions)” including Nebraska that completed a full pharmacy carve-in during FY 2017 and Indiana that completed a pharmacy carve-in for its Hoosier Healthwise program (for low-income pregnant women and children) in FY 2017. Among the states that carved drugs into MCOs, several reported carve-outs for selected drug classes. The most common drugs carved out were behavioral health drugs and HIV drugs (California, Maryland, and Michigan), hemophilia clotting factor (California, Florida, Michigan, and New Hampshire), and hepatitis C antivirals (Colorado, Massachusetts, Michigan, New Hampshire, South Carolina, and Texas). New York reported, however, that it reversed its carve-out of hemophilia clotting factor in July 2017.
Four states (Missouri, Tennessee, West Virginia, and Wisconsin) reported that the pharmacy benefit was “generally carved-out,” including West Virginia that completed a full carve-out as of July 2017. While Wisconsin noted that pharmacy was carved into its Family Care Partnership program (an integrated health and long-term care program for frail elderly and people with disabilities), the state noted that this program had a very small enrollment (approximately 3,000 as of July 201714) and that all other Wisconsin Medicaid enrollees received their pharmacy benefit through the FFS delivery system.
Prior reports show that nearly all states use prior authorization and PDLs in FFS programs. This year’s survey asked whether MCOs were required (in FY 2017) or would be required (in FY 2018) to adhere to uniform clinical protocols (state prescribed medical necessity criteria) for one or more drugs or a uniform PDL (state prescribed requirements for designating a specified drug product as either preferred, meaning covered without the need to obtain prior authorization, or non-preferred). This means that to the extent states impose these policies in FFS, the same policies would apply in managed care. Compared to last year’s survey, there was a notable increase in the number of states with uniform clinical protocols in place and a modest increase in the number of states that reported having a uniform PDL requirement in place. States were also asked whether MCO contracts included risk-sharing provisions for one or more drugs (e.g., risk corridors, risk pools, reinsurance, etc.), a new question not included in last year’s survey (Exhibit 13).
| Exhibit 13: Managed Care Pharmacy Policies | |||||||
| Policy | In Place in FY 2017 | FY 2018 Changes | |||||
| New | Expanded | ||||||
| Uniform Clinical Protocols (1 or more drugs) |
28 States | CA, DC, DE, GA, HI, IA, IL, IN, KS, KY, MA, MD, MI, MS, NE, NJ, NM, NV, NY, OH, OR, PA, RI, TX, UT, VA, WA, WV* | 3 States | LA, ND, VA | 7 States | DE, KY, MA, NV, OH, PA, WA | |
| Uniform PDL (1 or more drug classes) |
15 States | AZ, DE, FL, IA, KS, LA, MN, MS, NE, NV, OR, TX, UT, WA, WV* | 4 States | IL, ND, OH, VA | 2 States | LA, WA | |
| Risk-sharing (for 1 or more drugs) | 15 States | AZ, CA, DE, FL*, HI, IN, KS, MA, NM, NV, OH, OR, PA, RI, VA | 0 States | 5 States | DE, HI, IN, MA, SC | ||
| * WV removed the pharmacy benefit from its MCO contracts July 1, 2017. FL discontinued hepatitis C kick-payments in August 2017. | |||||||
Uniform clinical protocols and PDL requirements reported by states were often limited to one or a few specific drug classes. Hepatitis C antivirals were the most commonly mentioned drug class targeted by uniform clinical protocols (reported by DC, Georgia, Hawaii, Illinois, Maryland, New Jersey, New Mexico, Oregon, Rhode Island, Pennsylvania, and Virginia) and were also reported as a specific focus of uniform PDL requirements in Minnesota and Oregon. Strategies reported by states to mitigate or share financial risk with MCOs for certain high cost drugs included selected drug carve-outs, risk corridors, kick payments,15 and risk pools, and were most commonly applied to hepatitis C antivirals, but in some cases were applied to drugs above a certain dollar threshold (Hawaii), cystic fibrosis drugs (Pennsylvania), and hemophilia clotting factor (Delaware). Two states also commented that new risk-sharing arrangements were currently under consideration for a new spinal muscular atrophy drug and one state was considering a risk sharing arrangement for a Duchenne muscular dystrophy drug.
Opioid Harm Reduction Strategies
According to the Centers for Disease Control and Prevention (CDC), drug overdose deaths continue to increase in the United States and the majority of these deaths (six out of ten) involve an opioid (including prescription opioids and heroin).16 The CDC cites the amount of prescription opioids sold in the United States – which have nearly quadrupled since 1999 – as a driving factor in opioid overdose deaths, which have more than quadrupled since 1999.17 Medicaid plays an important role in addressing the epidemic, covering 3 in 10 people with opioid addiction in 2015 and facilitating access to a number of addiction treatment services.18 In a January 2016 Informational Bulletin,19 CMS highlighted the important role state Medicaid programs can play to help address the opioid epidemic in their states by encouraging safer opioid alternatives for pain relief, working with other state agencies to educate Medicaid providers on best practices for opioid prescribing, employing pharmacy management practices (PDL placement, clinical criteria, prior authorization, quantity limits, etc.) and working to increase access to naloxone, an overdose antidote. In this year’s survey, we asked states about their pharmacy benefit strategies for preventing opioid harm in place in FY 2017 and planned for FY 2018 and their coverage of certain medication-assisted treatment (MAT) medications.
CDC Opioid Prescribing Guidelines
This year’s survey shows a growing number of states choosing to adopt the CDC guidelines for the prescribing of opioid pain medications for adults in primary care settings.20 Both last year and this year, the survey asked states if their Medicaid program has adopted or is planning to adopt these guidelines in their FFS programs or as a requirement for MCOs to adopt. As shown in Exhibit 14 below, 34 states reported adoption or plans for adoption in FY 2018 for their FFS programs (compared to 21 states in last year’s survey). Of the 39 states with MCO contracts, 18 states reported requiring MCOs to adopt the CDC guidelines or plans to do so in FY 2018 (compared to 11 states in last year’s survey). Many other states indicated that these policies were under review for FFS and MCOs.
| Exhibit 14: Number of States Adopting CDC Opioid Prescribing Guidelines | ||||
| Status | For FFS | As a requirement for MCOs to adopt | ||
| Yes, have adopted | 23 States | AR, AZ, CT,* FL, ID, IN, KY, LA, MA, ME, MS, NE, NH, NV, NY, OR, PA, TN, TX,* VA, VT, WA,* WV | 8 States | IN, KY, LA, MS, NE, NH, VA, WA, |
| Plan to adopt in FY 2018 | 11 States | DC, GA, IA, KS, MD, MN, MO, MT, NC, NM, SC | 10 States | DC, DE, IA, KS, MA, MD, MN, NV, PA, SC |
| * CT and TX reported adoption of part, but not all, of the CDC guidelines. WA indicated that its state statutory prescribing guidelines include a Morphine Equivalent Dose (MED) limit (110 mg) that differs from the CDC limit (90 mg). | ||||
States were also asked to describe any implementation challenges related to the CDC guidelines. The most commonly reported challenge was the inability of a state’s claims processing system to apply the Morphine Equivalent Dose (MED) limit across multiple products and multiple prescription claims. Other reported challenges included obtaining stakeholder consensus and support (including providers); titrating dosages downward for patients who have been stabilized on higher dosages; and the inability to control or enforce appropriate prescribing behavior. One state also expressed concern that the CDC’s MED limit is too low and could have the unintended consequence of driving up heroin use and overdoses. A few states reported having state guidelines already in place that were aligned with the CDC guidelines.
Medicaid Pharmacy Benefit Management Strategies
The January 2016 CMS Informational Bulletin highlighted Medicaid pharmacy benefit management strategies for preventing opioid-related harms.21 The survey asked states to report strategies that were in place in FY 2017 for FFS and changes to these strategies planned for FY 2018. Specifically, the survey asked about the following strategies: opioid quantity limits,22 clinical criteria claim system edits23 (subject to prior authorization (PA) override), step therapy PA criteria,24 other PA requirements for opioids, and requirements that prescribers check the state’s Prescription Drug Monitoring Program (PDMP) before prescribing opioids.25 All but one state reported having at least one of these opioid-focused pharmacy management policies in FFS in place in FY 2017, and nearly three-quarters of states (37) plan to take at least one action in FY 2018 to newly implement or increase opioid controls through one of these strategies. See Exhibit 15 and Table 18 for details on states implementing or expanding these controls.
| Exhibit 15: States Implementing Opioid-Focused Pharmacy Benefit Management Strategies in FFS | |||
| Strategy | In Place in FY 2017 (# of states) |
FY 2018 (# of states) | |
| New | Expanded | ||
| Quantity Limits | 48 | 3 | 26 |
| Clinical criteria claim system edits (subject to Prior Authorization override) | 46 | 1 | 21 |
| Step Therapy PA criteria | 34 | 1 | 6 |
| Other Prior Authorization | 32 | 5 | 14 |
| Required use of Prescription Drug Monitoring Programs | 28 | 6 | 3 |
For states that use MCOs to deliver pharmacy benefits, the survey asked whether, as of July 1, 2017, the MCOs were required to follow the state’s FFS pharmacy benefit management policies for opioids. Of the 35 states with MCOs that deliver pharmacy benefits, 12 states responded “yes” and 12 states responded “yes, in part.” Of the 12 states answering “yes in part,” a few indicated that their MCOs were in the process of coming into alignment with the state’s FFS policies. One state indicated that MCOs may conduct additional maximum dose and quantity reviews; one state reported that MCOs must adopt the FFS management strategies but have some latitude in preferred drug selection and specific clinical criteria, and one state reported that MCOs may provide additional naloxone coverage without prior authorization and/or naloxone atomizers.
Other Pharmacy Management Strategies
A few states mentioned other pharmacy management strategies in use or planned including the following:
- Day limits were applied by Arizona and Utah (no more than seven days for the initial fill of any prescription opioid), Colorado (seven-day supply limit for opioid naïve patients), and Vermont (seven-day limit applied for adults and a three-day limit applied for children).
- MED limits were applied or lowered in Colorado, Maryland, and Vermont, and Connecticut implemented an “MME calculator” to provide prescribers with a MME (morphine milligram equivalent) calculation at the point of service.
- Maryland reported a new requirement for prescriber attestations (checked PDMP, drug urine test, offered naloxone, pain management contract).
- Nevada and DC reported pharmacy lock-in programs.26
- Oregon reported expanding access to medication-assisted treatment drug by ending its lock-in program for Suboxone.
Access to Naloxone
Naloxone is a prescription opioid overdose antidote that prevents or reverses the life-threatening effects of opioids including respiratory depression, sedation, and hypotension. There are three FDA-approved formulations of naloxone: an injectable formulation offered as a generic; a brand, prefilled auto-injection formulation (approved in 2014) designed for use by persons without medical training (Evzio); and a brand prepackaged nasal spray (approved in 2015) (Narcan).27 All formulations have experienced significant price increases in recent years; most notably, the list price for the auto-injection formulation increased from $690 in 2014 to $4,500 in 2016.28 In this year’s survey, states were asked whether the various naloxone formulations were available without a prior authorization (PA) in their Medicaid programs in FY 2017 and whether any changes were planned for FY 2018. States were also asked if naloxone coverage was provided for family members and friends obtaining prescriptions on an enrollee’s behalf. See Exhibit 16 and Table 19 for details on state naloxone pharmacy benefit management strategies.
A number of states commented that the auto-injector manufacturer (Evzio) had ended its participation in the federal drug rebate program for this product which allows states to eliminate all Medicaid coverage of this product (with or without PA). Of the 10 states reporting coverage of Evzio without PA in FY 2017, one state reported plans to move the Evzio to non-preferred status in FY 2018 (subject to PA) and three states indicated all coverage would be eliminated.
| Exhibit 16: States Implementing Naloxone Pharmacy Benefit Management Strategies in FFS | |||
| Strategy | In Place in FY 2017 (# of states) | FY 2018 (# of states) | |
| New | Expanded | ||
| Naloxone available in at least one formulation without prior authorization (PA) | 46 | 1 | 1 |
| Naloxone nasal spray covered without PA | 42 | 0 | 1 |
| Naloxone nasal spray atomizer covered without PA | 20 | 0 | 0 |
| Naloxone auto-injector covered without PA | 10* | 0 | 0 |
| Naloxone coverage provided for family members and friends obtaining prescriptions on enrollee’s behalf | 11 | 0 | 0 |
| * Three of these states (LA, MD, and MN) reported ending coverage of naloxone auto-injectors in FY 2018 and one state (NV) changed to non-preferred status. | |||
Medication-Assisted Treatment
The ACA requires state Medicaid programs to provide coverage for treating substance use disorders (SUDs) for their ACA expansion populations, but does not specify which SUD services must be included. This requirement has bolstered states’ work to respond to the opioid epidemic. The standard of care for opioid use disorder is medication-assisted treatment (MAT), which combines psychosocial treatment with medication.29 Compared to psychosocial treatment alone, MAT is associated with greater adherence to treatment, decreased opioid use, and reduced likelihood of overdose fatalities.30 The FDA has approved the following medications that can be used as part of MAT for opioid use disorder: methadone, buprenorphine, and both oral and extended-release injectable naltrexone.31 In this year’s survey, states were asked whether they covered each of these drugs (when used to treat opioid use disorders) or planned to add coverage in FY 2018. All 49 states that responded reported coverage of buprenorphine and both oral and injectable naltrexone, but a somewhat smaller number (36 states) reported coverage of methadone in FY 2017.32 However, one state reported plans to add coverage for methadone in FY 2018 (Indiana) and five states reported that methadone coverage was under consideration (Kentucky, Louisiana, North Dakota, South Carolina, and West Virginia). Seven states (Alabama, Idaho, Iowa, Nebraska, Tennessee, Texas, and Wyoming) reported no coverage or plans to add coverage for Methadone.
TABLE 18: MEDICAID FFS PHARMACY BENEFIT MANAGEMENT STRATEGIES FOR OPIOIDS IN ALL 50 STATES AND DC, IN PLACE IN FY 2017 AND ACTIONS TAKEN IN FY 2018
| States | Opioid Quantity Limits | Clinical Edits in Claim System | Opioid Step Therapy Requirements | Other Prior Authorization Requirements for Opioids | Required use of Prescription Drug Monitoring Programs | Any Opioid Management Strategies | ||||||
| In place FY 2017 | New/Exp FY 2018 | In place FY 2017 | New/Exp FY 2018 | In place FY 2017 | New/Exp FY 2018 | In place FY 2017 | New/Exp FY 2018 | In place FY 2017 | New/Exp FY 2018 | In place FY 2017 | New/Exp FY 2018 | |
| Alabama | X | X | X | X | X | X | ||||||
| Alaska | X | X | X* | X | X | |||||||
| Arizona | X | X | X | X | X | X | X | X | X | |||
| Arkansas | X | X | X | X | X | X | X | |||||
| California | X | X | X | X* | X | X | ||||||
| Colorado | X | X | X | X | X | |||||||
| Connecticut | X | X | X | X | ||||||||
| Delaware | X | X | X | X* | X | X | X | |||||
| DC | X | X | X | X* | X | X | X | |||||
| Florida | X | X | X | X | X | X | X* | X | X | |||
| Georgia | X | X | X | X | X | X | ||||||
| Hawaii | X* | X* | ||||||||||
| Idaho | X | X | X | X | X | X | X | X | ||||
| Illinois | X | X | X | X | X | |||||||
| Indiana | X | X | X | X | X | |||||||
| Iowa | X | X | X | X | X | X | X* | X | X | X | ||
| Kansas | X | X | X | X | X | X | X | X | ||||
| Kentucky | X | X | X | X | X | X | X | X | X | |||
| Louisiana | X | X | X | X | X | X | X | X | X | X | ||
| Maine | X | X | X | X | X | X | ||||||
| Maryland | X | X | X* | X | X | X* | X | X | ||||
| Massachusetts | X | X | X | X | X | X | X | X | ||||
| Michigan | X | X | X | X | X | X | X* | X | X | |||
| Minnesota | X | X | X | X | X | X | X | X | ||||
| Mississippi | X | X | X | X | X | X | X | X | ||||
| Missouri | X | X | X | X | X | X | X | |||||
| Montana | X | X | X | X | X | X | X | X | X | |||
| Nebraska | X | X | X | X | X | |||||||
| Nevada | X | X | X | X* | X | X | ||||||
| New Hampshire | X | X | X | X | X | X | ||||||
| New Jersey | X | X | X | |||||||||
| New Mexico | X | X | X | |||||||||
| New York | X | X | X | X | X | X | X | X | ||||
| North Carolina | X | X | X | X | X | X | X | X | X | X | ||
| North Dakota | X | X | X | X | X | X | X | X | X | X | X | |
| Ohio | X | X | X | X | X | X | X | X | X | X | ||
| Oklahoma | X | X | X | X | X | X | ||||||
| Oregon | X | X | X | X | X | X | X* | X | X | X | ||
| Pennsylvania | X | X | X | X | X | X | X | X | X | |||
| Rhode Island | X* | X | X | X | X | X | X | X* | X | X | ||
| South Carolina | X | X | X | X | X | X | X | X | ||||
| South Dakota | X | X | X | X | ||||||||
| Tennessee | X | X | X | X | X | X | X | X | X | X | ||
| Texas | X | X | X | X | X* | X | X | |||||
| Utah | X | X | X | X | ||||||||
| Vermont | X | X | X | X | X | X | X | X | ||||
| Virginia | X | X | X | X | X | X | X | X | X | |||
| Washington | X* | X | X | X | ||||||||
| West Virginia | X | X | X | X | X | X | ||||||
| Wisconsin | X | X | X | X | X | X | X | |||||
| Wyoming | X | X | X | X | X | X | ||||||
| Totals | 48 | 29 | 46 | 22 | 34 | 7 | 32 | 19 | 28 | 9 | 50 | 37 |
|
NOTES: States were asked to report whether they had select pharmacy benefit management strategies in place in their FFS programs in FY 2017, and/or had plans to adopt or expand these strategies in FY 2018. “*” indicates that a policy was newly adopted in FY 2018, meaning that the state did not have any policy in that category/column in place in FY 2017. |
||||||||||||
TABLE 19: MEDICAID FFS PHARMACY BENEFIT MANAGEMENT STRATEGIES FOR NALOXONE IN ALL 50 STATES AND DC, IN PLACE IN FY 2017 AND ACTIONS TAKEN IN FY 2018
| States | Naloxone Available ‒ At Least One Formulation Without PA | Naloxone Nasal Spray Covered Without PA | Naloxone Nasal Atomizer Covered Without PA | Naloxone Auto-Injectors Covered Without PA | Naloxone Covered for Family/Friends Obtaining Scripts on Enrollee’s Behalf | Any Naloxone Strategies | ||||||
| In place FY 2017 | New/Exp in FY 2018 | In place FY 2017 | New/Exp in FY 2018 | In place FY 2017 | New/Exp in FY 2018 | In place FY 2017 | New/Exp in FY 2018 | In place FY 2017 | New/Exp in FY 2018 | In place FY 2017 | New/Exp in FY 2018 | |
| Alabama | X | X | X | |||||||||
| Alaska | X | X | X | X | ||||||||
| Arizona | X | X | X | X | ||||||||
| Arkansas | X | X | ||||||||||
| California | X | X | X | |||||||||
| Colorado | X | X | X | X | ||||||||
| Connecticut | X | X | X | X | X | |||||||
| Delaware | X | X | ||||||||||
| DC | X* | X | ||||||||||
| Florida | X | X | X | X | X | |||||||
| Georgia | X | X | ||||||||||
| Hawaii | ||||||||||||
| Idaho | X | X | X | X | ||||||||
| Illinois | ||||||||||||
| Indiana | X | X | X | X | X | |||||||
| Iowa | X | X | X | X | ||||||||
| Kansas | X | X | X | |||||||||
| Kentucky | X | X | X | X | ||||||||
| Louisiana | X | X | X | X | X | |||||||
| Maine | ||||||||||||
| Maryland | X | X | X | X | X | |||||||
| Massachusetts | X | X | X | X | X | |||||||
| Michigan | X | X | X | X | ||||||||
| Minnesota | X | X | X | X | X | |||||||
| Mississippi | X | X | X | |||||||||
| Missouri | X | X | X | X | X | |||||||
| Montana | X | X | X | |||||||||
| Nebraska | X | X | X | |||||||||
| Nevada | X | X | X | X | X | X | ||||||
| New Hampshire | X | X | X | X | ||||||||
| New Jersey | X | X | X | X | X | X | ||||||
| New Mexico | X | X | X | X | X | X | ||||||
| New York | X | X | X | X | ||||||||
| North Carolina | X | X | X | X | X | |||||||
| North Dakota | X | X | X | |||||||||
| Ohio | X | X | X | |||||||||
| Oklahoma | X | X | X | |||||||||
| Oregon | X | X | X | X | ||||||||
| Pennsylvania | X | X | X | X | ||||||||
| Rhode Island | X | X | X | X | ||||||||
| South Carolina | X | X | X | X | ||||||||
| South Dakota | X | X | X | |||||||||
| Tennessee | ||||||||||||
| Texas | X | X | X | X | ||||||||
| Utah | X | X | X | |||||||||
| Vermont | X | X | X | X | ||||||||
| Virginia | X | X | X | |||||||||
| Washington | X | X | X | X | ||||||||
| West Virginia | X | X | X | |||||||||
| Wisconsin | X | X | X | X | ||||||||
| Wyoming | X | X | X | |||||||||
| Totals | 46 | 2 | 42 | 1 | 20 | 0 | 10 | 0 | 11 | 0 | 46 | 3 |
|
NOTES: States were asked to report whether they had select pharmacy benefit management strategies in place in their FFS programs in FY 2017, and/or had plans to adopt or expand these strategies in FY 2018. “*” indicates that a policy was newly adopted in FY 2018, meaning that the state did not have any policy in that category/column in place in FY 2017. Three states (LA, MD, and MN) reported ending coverage of naloxone auto-injectors in FY 2018 and one state (NV) changed to non-preferred status.
SOURCE: Kaiser Family Foundation Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2017.
|
||||||||||||