Medicaid Moving Ahead in Uncertain Times: Results from a 50-State Medicaid Budget Survey for State Fiscal Years 2017 and 2018
Long-Term Services and Supports Reforms
| Key Section Findings |
| The vast majority of states in FY 2017 (47) and all states in FY 2018 are employing one or more strategies to expand the number of people served in home and community-based settings. The most common strategies include using HCBS waivers or state plan options, building rebalancing incentives into managed long-term services and supports (MLTSS) contracts, and serving more individuals through Programs of All-Inclusive Care for the Elderly (PACE) programs. Twenty-three states cover LTSS through one or more capitated managed care arrangements.
What to watch: Housing supports are an increasingly important part of state LTSS benefits. Over half of states (27) reported that they implemented or expanded housing-related activities outlined in CMS’s June 2015 Informational Bulletin1 (e.g., housing transition services, housing and tenancy sustaining services) in FY 2017 or FY 2018 (up from 16 states reported last year). In response to a new survey question about how states are addressing LTSS direct care workforce shortages and turnover, 17 states reported efforts in FY 2017 or FY 2018 to increase wages for direct care workers and/or engage in targeted workforce development activities (recruiting, training, credentialing, etc.). Additional information on HCBS expansions implemented in FY 2017 or planned for FY 2018 as well as state-level details on capitated MLTSS models can be found in Tables 10 and 11. |
Medicaid is the nation’s primary payer for long-term services and supports (LTSS), covering a continuum of services ranging from home and community-based services (HCBS) that allow persons to live independently in their own homes or in other community settings to institutional care provided in nursing facilities (NFs) and intermediate care facilities for individuals with intellectual disabilities (ICF-IDs). In 2015, spending on HCBS increased 7 percent while institutional spending decreased slightly, by 0.1 percent. HCBS represented 55 percent of total Medicaid expenditures on LTSS, and institutional LTSS represented 45 percent,2 a dramatic shift from 1995, when institutional settings accounted for 82 percent of national Medicaid LTSS expenditures.3
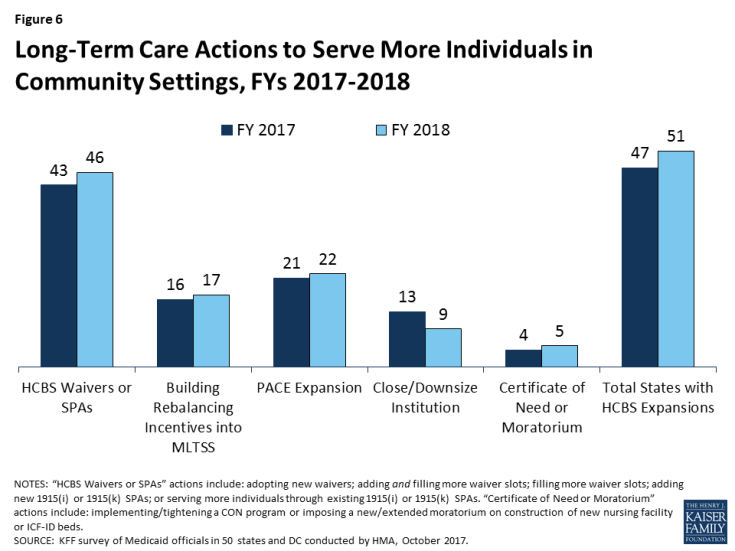
This year’s survey shows the vast majority of states in FY 2017 (47) and all states in FY 2018 (51) employing one or more strategies to expand the number of people served in home and community-based settings (Figure 6 and Table 10).
- Forty-three states in FY 2017 and 46 states in FY 2018 report using HCBS waivers and/or State Plan Amendments (SPAs) to expand the number of people receiving HCBS.4 HCBS waivers and SPAs include Section 1915(c) and Section 1115 waivers5 as well as Section 1915(i) and 1915(k) (“Community First Choice”) state plan options.
- Sixteen states in FY 20176 and 17 states in FY 2018 report including specific rebalancing incentives, performance targets and/or financial incentives, in managed care contracts to encourage MCOs that cover LTSS to expand access to HCBS.
- Twenty-one states in FY 2017 and 22 states in FY 2018 report serving more individuals through Programs of All-Inclusive Care for the Elderly (PACE) programs.7
- Thirteen states in FY 2017 and nine states in FY 2018 are closing or downsizing a state institution and transitioning residents into community settings.
- Four states in FY 2017 and five states in FY 2018 are implementing or tightening a Certificate of Need (CON) program or imposing or extending a moratorium on construction of new NF or ICF-ID beds.
States were also asked whether they have adopted or plan to adopt new restrictions on the number of people served in the community. In FY 2018, Missouri noted they are reducing enrollees’ state plan consumer directed services budgets to equal 60 percent of the cost of nursing home care. In addition, Texas noted that, while the state budget included increased funding to support additional slots in Section 1915(c) waivers, the state has slowed down the rollout of new slots because of unanticipated increases in Community First Choice expenditures.
Table 10 shows state use of LTSS rebalancing tools in FY 2017 and FY 2018.
Housing Supports
In June 2015, CMS issued an Informational Bulletin to clarify when and how Medicaid reimburses for certain housing-related activities, including individual housing transition services, individual housing and tenancy sustaining services, and state-level housing related collaborative activities.8 CMS’s intent was to assist states in designing benefits that support community integration for seniors, individuals with disabilities, and individuals experiencing chronic homelessness. Over half of states (27 states) reported that they implemented or expanded a housing-related strategy outlined in the CMS bulletin in FY 2017 and/or FY 2018 (Exhibit 7).
| Exhibit 7: States Implementing or Expanding Housing-Related Services Outlined in the CMS Informational Bulletin | ||
| FY 2017 only | FY 2018 only | Both FY 2017 and FY 2018 |
| DC, IN, KY, MA, MN, RI, TN, VT | CT, DE, GA, HI, IL, KS, UT | AZ, CA, FL, MD, MI, MS, NJ, NY, OH, PA, SC, WA |
Many of the services outlined in CMS’s Informational Bulletin were developed under the auspices of federal grant programs, including the Money Follows the Person (MFP) rebalancing demonstration. MFP is a federal grant program, enacted under the Deficit Reduction Act of 2005 and extended through September 2016 by the Affordable Care Act, which operated in 44 states.9,10 Enhanced federal funding under MFP has supported the transition of over 63,000 individuals from institutional to home and community-based long-term care settings as of December 2015.11 Under MFP, states identified the lack of affordable and accessible housing as a major barrier to assisting individuals to leave institutional settings of care.12 With MFP resources, many states have offered new housing related services, incorporated housing expertise within the Medicaid program to increase the likelihood of successful community living for persons who need supports, and engaged in strategic activities to assist in identifying and securing housing resources for individuals who choose HCBS.13
After September 2016, with CMS approval, states can continue to transition eligible individuals through 2018 and expend remaining MFP funds through federal FY 2020.14 As of July 2017, 30 states report that they currently offer housing-related services under a state plan, Section 1915(c) waiver, or Section 1115 waiver that the state intends to continue after the expiration of the MFP. However, 21 states report some services will likely be discontinued when MFP funding runs out. Examples of MFP services and activities that states may discontinue include: home delivered meals, vehicle modifications, independent living skills training, housing transition services, peer mentorship, and caregiver education, among others.
LTSS Direct Care Workforce
Many states are struggling to find sufficient numbers of trained direct care workers to meet the growing LTSS demand, including the demand for care in home and community-based settings.15,16 Low wages, few benefits, limited opportunities for career advancement, inadequate training, and high rates of worker injury are all factors that contribute to a workforce shortage and high workforce turnover among paid LTSS direct care workers. In this year’s survey, states were asked to describe any Medicaid initiatives intended to address LTSS direct care workforce shortages or turnover. Seventeen states report efforts underway in FY 2017 or FY 2018 related to wage increases for direct care workers or to workforce development (Exhibit 8).17
| Exhibit 8: Strategies to Address LTSS Direct Care Workforce Shortages & Turnover | ||
| # of States | States | |
| Wage Increases | 11 | IL, IN, KS, ME, MI, MT, NC, NH, NY, RI, UT |
| Workforce Development (including recruiting, training, credentialing etc.) | 6 | AZ, CT, MA, TN, WA, WI |
HCBS Benefit Changes
Fourteen states in FY 2017 and 13 states in FY 2018 reported a wide variety of HCBS benefit additions or expansions. HCBS benefits include those in Section 1915(c) waivers, under Section 1915(i) authority or Section 1915(k) authority (“Community First Choice” or “CFC”), and state plan personal care services, home health services, or private duty nursing, and PACE (Exhibit 9).18 Most HCBS benefit changes reported involve the addition of HCBS services to existing waiver or state plan programs. Examples of HCBS services added by states include assistive technology, home delivered and medically tailored meals, personal supports, unpaid caregiver training, housing transition services and tenancy supports, and supported employment.
Some states implemented new HCBS programs in FY 2017 or FY 2018. Six states report establishing eleven new PACE sites over the reporting period (Exhibit 9). In FY 2017, Tennessee added a new HCBS program for individuals with ID/DD under its Section 1115 waiver (Employment and Community First CHOICES). In FY 2018, Idaho will implement a new Section 1915(i) state plan HCBS option for children with a serious emotional disturbance, Pennsylvania will add a new Community Living waiver for individuals with ID/DD, and Wyoming will implement a new Section 1915(k) (CFC) state plan service.
Only one state, Oregon, reported eliminating an HCBS benefit, proposing to eliminate coverage for a live-in program in FY 2018.
| Exhibit 9: HCBS Benefit Enhancements or Additions | ||
| Benefit | FY 2017 | FY 2018 |
| HCBS Enhancements or Additions to Existing HCBS Authority | CA, KY, MA, MN, MS, NC, NE, PA, SC, SD, WI | CA, DE, NH, NY, PA, TX, UT, VA, WA |
| New PACE site | IN, LA | CA (2 sites), CO, IN, NC (2 sites), TX (3 sites) |
| New Section 1915(c), (i), or (k) | IN, TN | ID, PA, WY |
| Washington’s LTSS Changes through Section 1115 Transformation Waiver |
| Washington is implementing LTSS eligibility and benefit package changes (described below) under its Section 1115 waiver to broaden the array of services available to individuals and to support unpaid family caregivers. The state hopes that these reforms will enable beneficiaries to stay at home and delay or avoid the need for more intensive care, while preserving quality of life, reducing costs, and avoiding the need for beneficiaries to impoverish themselves to access LTSS.
Medicaid Alternative Care (MAC) LTSS benefit package – MAC is a new LTSS benefit package option for Medicaid beneficiaries to support those living at home with assistance provided by unpaid family caregivers. MAC is only available to Medicaid beneficiaries eligible for but not receiving Medicaid-funded LTSS through the state plan or a Section 1915(c) waiver benefit package. MAC benefits include caregiver assistance services, caregiver training and education, specialized medical equipment and supplies, and health maintenance therapy supports. Tailored Supports for Older Adults (TSOA) eligibility pathway for LTSS – TSOA will serve individuals who do not meet existing Medicaid financial eligibility criteria but who are “at-risk” of future Medicaid LTSS use. TSOA creates a new coverage group with access to a limited HCBS benefit package. MAC benefits include caregiver assistance services, caregiver training and education, specialized medical equipment and supplies, health maintenance therapy supports, and personal assistance. |
Capitated Managed Long-Term Services and Supports (MLTSS)
As of July 1, 2017, almost half of states (23 states) covered LTSS through one or more of the following types of capitated managed care arrangements:
- Medicaid MCO covering Medicaid acute care and LTSS (18 states)
- PHP covering only Medicaid LTSS (6 states)
- MCO arrangement for dual eligible beneficiaries covering Medicaid and Medicare acute care and Medicaid LTSS services in a single contract under the federal Financial Alignment Demonstration (FAD) (10 states)
Of the 23 states that reported using one or more of these MLTSS models, nine states reported using two models, and one state (New York) reported using all three. Of the states with capitated MLTSS, 15 offered some form of MLTSS plan on a statewide basis for at least some LTSS populations as of July 1, 2017 (Table 11).
Ten states offered an MCO-based FAD (California, Illinois, Massachusetts, Michigan, New York, Ohio, Rhode Island, South Carolina, Texas, and Virginia) as of July 1, 2017.19,20 The FAD model involves a three-way contract between an MCO, Medicare, and the state Medicaid program.21,22 Massachusetts also operates an administrative alignment demonstration (without financial alignment) for dually eligible beneficiaries (Senior Care Options program). Minnesota only operates an administrative alignment demonstration (without financial alignment) for dually eligible beneficiaries (Minnesota Senior Health Options program).
Other states not participating in a formal demonstration have taken action to encourage improved coordination and integration of services for the dually eligible population under MCO arrangements. Eight states23 require Medicaid-contracting MCOs to be Medicare Dual Eligible Special Needs Plans (D-SNP)24 or Fully Integrated Dual Eligible (FIDE) Special Needs Plans,25 creating an opportunity for improved coordination and integration for beneficiaries. Five states26 encourage MCOs to be a D-SNP or a FIDE-SNP.
MLTSS Enrollment
For geographic areas where MLTSS operates, this year’s survey asked whether, as of July 1, 2017, certain populations were enrolled in MLTSS on a mandatory or voluntary basis or were always excluded. On the survey, states selected from “always mandatory,” “always voluntary,” “varies,” or “always excluded” for the following populations: seniors, persons with ID/DD, nonelderly adults with physical disabilities, and full benefit dual eligible individuals. As shown in Exhibit 10 below, seniors were most likely to be enrolled on a mandatory basis. Persons with ID/DD were excluded from enrollment in only three MLTSS states, though they were least likely to be enrolled on a mandatory basis. No state offering MLTSS always excludes full benefit dual eligible individuals from MLTSS enrollment.
| Exhibit 10: MLTSS Enrollment by Populations, July 1, 2017 (# of States) | ||||
| Seniors | Persons with ID/DD | Nonelderly Adults with Physical Disabilities | Full Benefit Dual Eligibles | |
| Always mandatory | 13 | 7 | 11 | 11 |
| Always voluntary | 5 | 5 | 4 | 6 |
| Varies | 4 | 8 | 6 | 6 |
| Always excluded | 1 | 3 | 2 | 0 |
MLTSS Population Changes
Growth in the use of MLTSS has continued since the prior survey reporting year. South Carolina expanded MLTSS to new regions in FY 2017 while Pennsylvania will expand to new regions in FY 2018 (Exhibit 11). In FY 2018, Virginia will roll out a new MLTSS program. Wisconsin’s Family Care Program will be statewide by the end of FY 2018. Five states extended MLTSS to new populations in FY 2017 (Illinois, New York, South Carolina, Tennessee, and Texas). In FY 2018, two states (New York and Pennsylvania) will extend MLTSS to new populations. No states reported actions or plans to decrease the number of enrollees served in MLTSS in FY 2017 or FY 2018.
| Exhibit 11: MLTSS Population Expansions, FY 2017 and FY 2018 | ||
| FY 2017 | FY 2018 | |
| Geographic Expansions | SC, WI | PA, VA, WI |
| New Population Groups Added | IL, NY, SC, TN, TX | NY, PA |
MLTSS Benefits
Almost every MLTSS state (21 out of 23 states) includes both institutional and HCBS in the same contractual arrangement, while two states (Michigan and Tennessee) report that this varies by MLTSS arrangement. Only one state reported a MLTSS benefit change in FY 2017 or FY 2018. Michigan added hospice benefits to its FAD in FY 2017.
TABLE 10: LONG-TERM CARE ACTIONS TO SERVE MORE INDIVIDUALS IN COMMUNITY SETTINGS IN ALL 50 STATES AND DC, FY 2017 AND FY 2018
| States | Sec. 1915(c) or Sec. 1115 Waiver | Sec. 1915(i) HCBS State Plan Option | Sec. 1915(k) “Community First Choice” Option | Building Rebalancing Incentives into MLTSS | PACE Expansion | Close/ Downsize Institution | Certificate of Need or Moratorium | Total States with HCBS Expansions | ||||||||
| 2017 | 2018 | 2017 | 2018 | 2017 | 2018 | 2017 | 2018 | 2017 | 2018 | 2017 | 2018 | 2017 | 2018 | 2017 | 2018 | |
| Alabama | X | X | X | X | ||||||||||||
| Alaska | X | X | ||||||||||||||
| Arizona | X | X | X | X | ||||||||||||
| Arkansas | X | X | X | X | X | X | ||||||||||
| California | X | X | X | X | X | X | X | X | X | X | X | X | X | X | ||
| Colorado | X | X | X | X | X | X | X | X | ||||||||
| Connecticut | X | X | X | X | X | X | X | X | X | X | ||||||
| DC* | X | X | ||||||||||||||
| Delaware | X | X | X | X | X | X | X | X | X | X | ||||||
| Florida | X | X | X | X | X | X | X | X | ||||||||
| Georgia | X | X | X | X | ||||||||||||
| Hawaii | X | X | X | X | ||||||||||||
| Idaho | X | X | X | X | X | X | X | |||||||||
| Illinois | X | X | X | X | X | X | ||||||||||
| Indiana | X | X | X | X | X | X | X | X | X | X | ||||||
| Iowa | X | X | X | X | X | X | X | X | ||||||||
| Kansas | X | X | X | X | ||||||||||||
| Kentucky | X | X | X | X | ||||||||||||
| Louisiana | X | X | X | X | ||||||||||||
| Maine | X | X | X | X | ||||||||||||
| Maryland | X | X | X | X | X | |||||||||||
| Massachusetts | X | X | X | X | X | X | X | |||||||||
| Michigan | X | X | X | X | X | X | X | X | X | |||||||
| Minnesota | X | X | X | X | X | X | ||||||||||
| Mississippi | X | X | X | X | X | |||||||||||
| Missouri | X | X | X | X | ||||||||||||
| Montana | X | X | X | X | X | X | X | |||||||||
| Nebraska | X | X | X | X | X | X | ||||||||||
| Nevada | X | X | X | |||||||||||||
| New Hampshire | X | X | X | X | X | |||||||||||
| New Jersey | X | X | X | X | X | X | X | X | ||||||||
| New Mexico | X | X | X | X | X | X | ||||||||||
| New York | X | X | X | X | X | X | X | X | X | X | X | X | ||||
| North Carolina | X | X | X | X | X | X | ||||||||||
| North Dakota | X | X | X | X | X | X | X | X | X | X | ||||||
| Ohio | X | X | X | X | X | X | X | X | ||||||||
| Oklahoma | X | X | X | X | X | X | ||||||||||
| Oregon | X | X | X | X | X | X | X | X | ||||||||
| Pennsylvania | X | X | X | X | X | X | X | X | X | X | ||||||
| Rhode Island | X | X | X | X | ||||||||||||
| South Carolina | X | X | X | X | X | |||||||||||
| South Dakota | X | X | X | X | ||||||||||||
| Tennessee | X | X | X | X | X | X | X | X | X | |||||||
| Texas | X | X | X | X | X | X | X | X | X | X | ||||||
| Utah | X | X | X | X | ||||||||||||
| Vermont | X | X | X | X | ||||||||||||
| Virginia | X | X | X | X | X | X | X | X | X | |||||||
| Washington | X | X | X | X | X | X | X | X | ||||||||
| West Virginia | X | X | ||||||||||||||
| Wisconsin | X | X | X | X | X | X | X | |||||||||
| Wyoming | X | X | X | X | X | X | X | |||||||||
| Totals | 41 | 42 | 8 | 13 | 8 | 10 | 16 | 17 | 21 | 22 | 13 | 9 | 4 | 5 | 47 | 51 |
| NOTES: “1915(c) or Sec. 1115 Waiver” actions include: adopting new waivers; adding and filling more waiver slots; or filling more waiver slots. Actions under “1915(i) and 1915(k)” include adding new 1915(i) or 1915(k) SPAs or serving more individuals through existing 1915(i) or 1915(k) SPAs. “Certificate of Need or Moratorium” actions include: implementing/tightening a CON program or imposing a new/extended moratorium on construction of new nursing facility or ICF-ID beds. *DC – Although not reflected in the table/counts above, DC also reported implementing a uniform assessment tool and increasing the availability of Medicaid application assistance, streamlining the eligibility and enrollment process. Several states also highlighted continued rebalancing efforts through the Money Follows the Person (MFP) program; although this federal grant program ended in September 2016, with CMS approval, states can continue to transition eligible individuals through 2018 and expend remaining MFP funds through federal FY 2020. SOURCE: Kaiser Family Foundation Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2017. |
||||||||||||||||
TABLE 11: CAPITATED MLTSS MODELS IN ALL 50 STATES AND DC, AS OF JULY 1, 2017
| States | Medicaid MCO | PHP | Medicare + Medicaid Demonstration | Any MLTSS | Statewide |
| Alabama | |||||
| Alaska | |||||
| Arizona | X | X | X | ||
| Arkansas | |||||
| California | X | X | X | ||
| Colorado | |||||
| Connecticut | |||||
| DC | |||||
| Delaware | X | X | X | ||
| Florida | X | X | X | ||
| Georgia | |||||
| Hawaii | X | X | X | ||
| Idaho | X | X | |||
| Illinois | X | X | X | ||
| Indiana | |||||
| Iowa | X | X | X | ||
| Kansas | X | X | X | ||
| Kentucky | |||||
| Louisiana | |||||
| Maine | |||||
| Maryland | |||||
| Massachusetts | X | X* | X | ||
| Michigan | X | X | X | X | |
| Minnesota* | X | X | X | ||
| Mississippi | |||||
| Missouri | |||||
| Montana | |||||
| Nebraska | |||||
| Nevada | |||||
| New Hampshire | |||||
| New Jersey | X | X | X | ||
| New Mexico | X | X | X | ||
| New York | X | X | X | X | X |
| North Carolina | X | X | X | ||
| North Dakota | |||||
| Ohio | X | X | X | ||
| Oklahoma | |||||
| Oregon | |||||
| Pennsylvania | |||||
| Rhode Island | X | X | X | X | |
| South Carolina | X | X | |||
| South Dakota | |||||
| Tennessee | X | X | X | X | |
| Texas | X | X | X | X | |
| Utah | |||||
| Vermont | |||||
| Virginia | X | X | |||
| Washington | |||||
| West Virginia | |||||
| Wisconsin | X | X | X | ||
| Wyoming | |||||
| Totals | 18 | 6 | 10 | 23 | 15 |
| NOTES: States were asked whether they cover long-term services supports through any of the following managed care (capitated) arrangements as of July 1, 2017: Medicaid MCO (MCO covers Medicaid acute + Medicaid LTSS); PHP (covers only Medicaid LTSS); or Medicare + Medicaid Demonstration (Medicaid MCO covers Medicaid and Medicare acute + Medicaid LTSS). “Medicare + Medicaid Demonstration” – these states use Medicaid MCOs in Financial Alignment Demonstration (FAD) initiatives which involve care coordination for dually eligible beneficiaries. States were also asked whether MLTSS plans were operating in all regions of the state as of July 1, 2017 (statewide). *MA operates a FAD and another administrative alignment demonstration for dually eligible beneficiaries. *MN operates an administrative alignment demonstration (without financial alignment) for dually eligible beneficiaries. *OH offers a Medicaid MCO (MCO offers Medicaid acute + Medicaid LTSS) only in those counties where the FAD is offered; dually eligible seniors who opt out of the FAD must enroll in this Medicaid MCO model for Medicaid services. SOURCE: Kaiser Family Foundation Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, 2017. |
|||||