Medicaid
Long-Term Care
What Staffing Requirements Mean for Nursing Facilities
 In 45 states, fewer than half of nursing facilities currently meet all three staffing minimums in the final federal rule released in April.
In 45 states, fewer than half of nursing facilities currently meet all three staffing minimums in the final federal rule released in April.Medicaid Long-Term Services and Supports
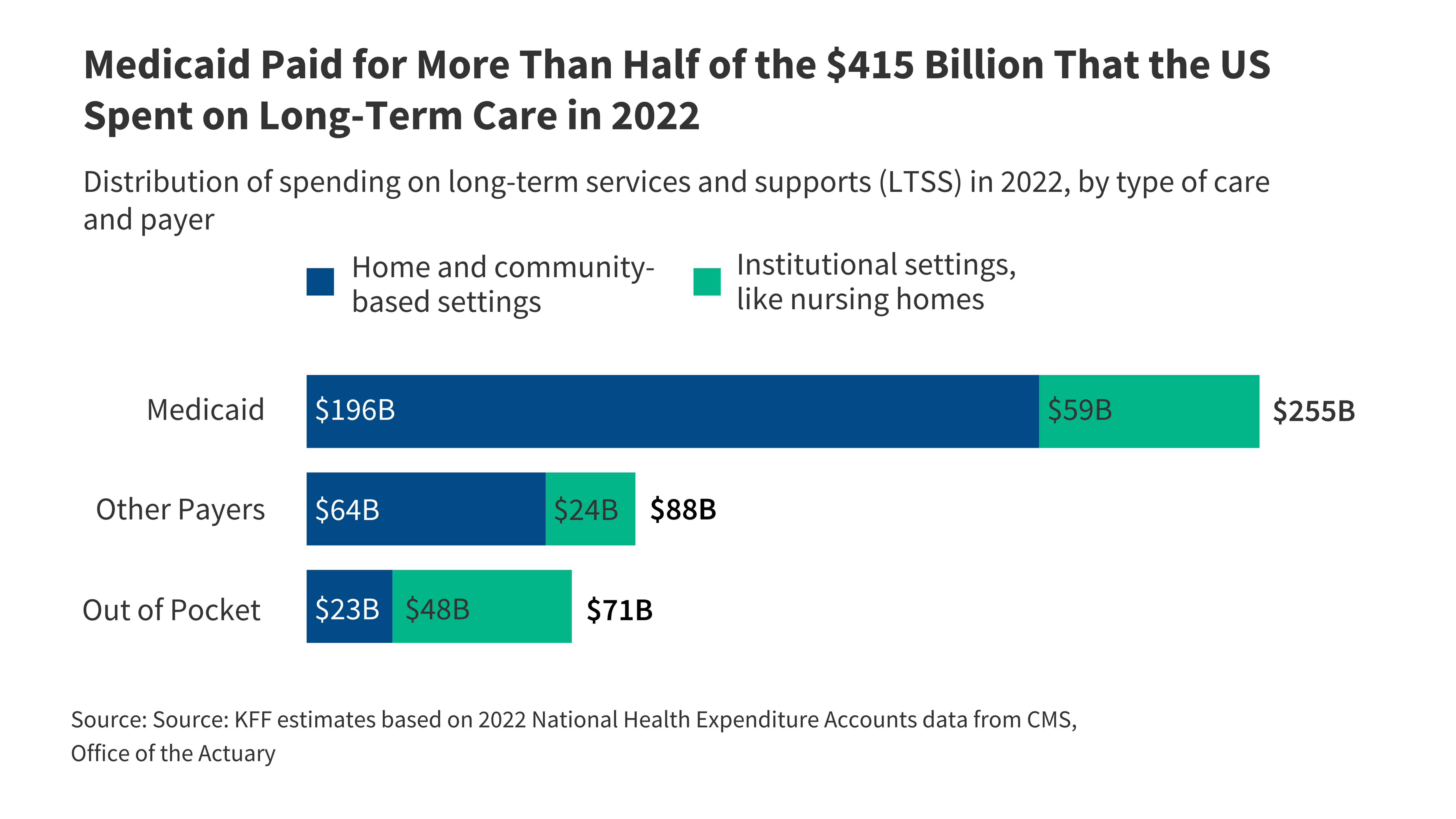 Long-term services and supports (LTSS) are expensive and not generally covered by Medicare or health insurance. Medicaid paid for more than half of U.S. LTSS costs in 2022.
Long-term services and supports (LTSS) are expensive and not generally covered by Medicare or health insurance. Medicaid paid for more than half of U.S. LTSS costs in 2022.Who Uses Medicaid LTSS?
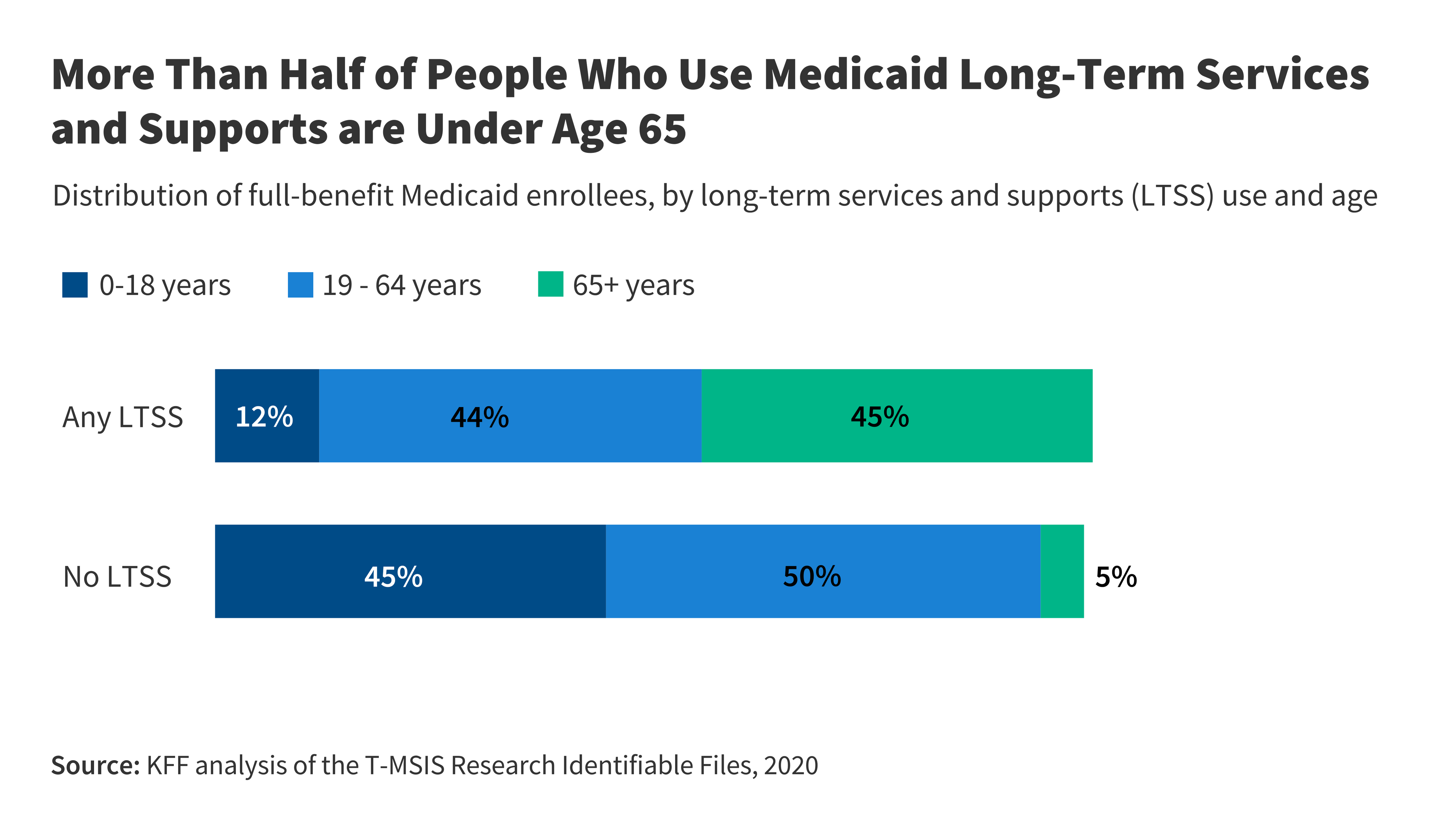 Nearly 6 million people receive Medicaid long-term services and supports (LTSS) for assistance with activities of daily living. Over half of these enrollees are under 65.
Nearly 6 million people receive Medicaid long-term services and supports (LTSS) for assistance with activities of daily living. Over half of these enrollees are under 65.States’ Home- and Community-Based Services Programs
 KFF administers regular surveys of states about their home- and community-based services (HCBS) programs and eligibility policies for seniors and people with disabilities.
KFF administers regular surveys of states about their home- and community-based services (HCBS) programs and eligibility policies for seniors and people with disabilities.America’s Long-Term Care Crisis
 From KFF Health News and The New York Times, Dying Broke is a jointly reported series examining families’ long-term care challenges.
From KFF Health News and The New York Times, Dying Broke is a jointly reported series examining families’ long-term care challenges.
The Essentials
Health Policy 101: Medicaid
KFF’s new primer on U.S. health policy examines how major public programs like Medicaid, Medicare, and the ACA are structured, funded, operated, and more.10 Things: Medicaid Managed Care
Comprehensive managed care is the most common way states deliver Medicaid services to enrollees, and new federal rules strengthen standards for managed care access.Medicaid Financing: The Basics
Medicaid represents $1 out of $6 spent on health care in the U.S. and is the major source of financing for state health coverage and long-term services and supports for low-income residents.
-
Medicaid Section 1115 Waivers, by State
Our Medicaid waiver tracker provides the latest on pending and approved Section 1115 waivers, which make broad changes to eligibility, benefits, provider payments, and other rules. Medicaid State Fact Sheets
Medicaid is a major source of funding for hospitals and community health centers. States operate their programs within federal standards and a range of state options.
Latest News
-

KFF Health News' 'What the Health?': Harris in the Spotlight
-

Un grupo médico atiende a personas que viven en la calle… y gana dinero
-

Misleading Ads Play Key Role in Schemes to Gin Up Unauthorized ACA Sign-Ups, Lawsuit Alleges
-

California Health Care Pioneer Goes National, Girds for Partisan Skirmishes

