Medicaid Moving Ahead in Uncertain Times: Results from a 50-State Medicaid Budget Survey for State Fiscal Years 2017 and 2018
Managed Care Initiatives
| Key Section Findings |
|
Managed care is the predominant delivery system for Medicaid in most states. Among the 39 states with comprehensive risk-based managed care organizations (MCOs), 29 states reported that 75 percent or more of their Medicaid beneficiaries were enrolled in MCOs as of July 1, 2017. Because of nearly full MCO saturation in most MCO states, only a few states reported actions to increase MCO enrollment. Although many states still carve-out behavioral health services from MCO contracts, movement to carve-in these services continues. Nearly all states have managed care quality initiatives in place such as pay for performance or capitation withholds.
–
What to watch:
Tables 4 through 8 include more detail on the populations covered under managed care (Tables 4 and 5), behavioral health services covered under MCOs (Table 6), managed care quality initiatives (Table 7), and minimum Medical Loss Ratio (MLR) policies (Table 8). |
The Centers for Medicare and Medicaid Services (CMS) issued a final rule on managed care in Medicaid and CHIP in April 2016. The new rule represents a major revision and modernization of federal regulations in this area.2 3 On June 30, 2017, CMS released an Informational Bulletin4 indicating they would use “enforcement discretion” to work with states on achieving compliance with the new managed care regulations, except for specific areas that “have significant federal fiscal implications.”
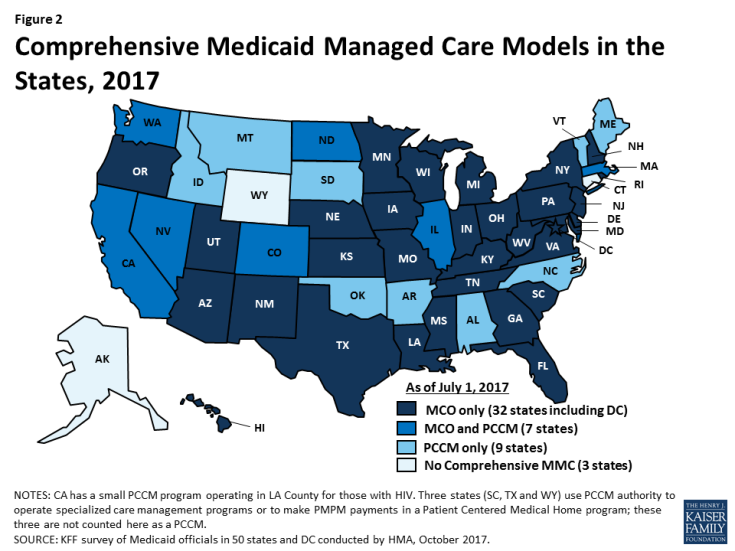
Managed care remains the predominant delivery system for Medicaid in most states. As of July 2017, all states except three – Alaska, Connecticut,5 and Wyoming– had some form of managed care in place, unchanged from July 2016. The number of states contracting with comprehensive risk-based managed care organizations (MCOs) (39 states) or operating a Primary Care Case Management (PCCM) program (16 states) as of July 2017 also remained unchanged from the prior year. PCCM is a managed fee-for-service (FFS) based system in which beneficiaries are enrolled with a primary care provider who is paid a small monthly fee to provide case management services in addition to primary care.
Of the 48 states that operate some form of managed care, seven operate both MCOs and a PCCM program while 32 states operate MCOs only and nine states operate PCCM programs only6 (Figure 2). Wyoming, one of the three states without any managed care (i.e., without either MCOs or a PCCM program), does operate a limited-benefit risk-based prepaid health plan (PHP). In total, 25 states (including Wyoming) contracted with one or more PHPs to provide Medicaid benefits including, behavioral health care, dental care, vision care, non-emergency medical transportation (NEMT), or long-term services and supports (LTSS).
Populations Covered by Risk-Based Managed Care
The share of Medicaid beneficiaries enrolled in MCOs or PCCM programs or remaining in FFS for their acute care varies widely by state. However, the share of Medicaid beneficiaries enrolled in MCOs has steadily increased as states have expanded their managed care programs to new regions and new populations and made MCO enrollment mandatory for additional eligibility groups. This year’s survey showed continued modest growth. The survey asked states to indicate the approximate share of specific Medicaid populations who receive their acute care in MCOs, PCCM programs, and FFS. As shown in Figure 3, among the 39 states with MCOs, 29 states reported that 75 percent or more of their Medicaid beneficiaries were enrolled in MCOs as of July 1, 2017 (up from 28 states in last year’s survey), including four of the five states with the largest total Medicaid enrollment. These four states (California, New York, Texas, and Florida) account for nearly four out of every 10 Medicaid beneficiaries across the country (Figure 3 and Table 4).7
Consistent with past survey results, this year’s survey found that children and adults (particularly those enrolled through the ACA Medicaid expansion) are much more likely to be enrolled in an MCO than elderly Medicaid beneficiaries or those with disabilities. Thirty-five of the 39 MCO states covered 75 percent or more of all children through MCOs. Twenty-eight of the 39 MCO states covered 75 percent or more of low-income adults in pre-ACA expansion groups (e.g., parents, pregnant women) through MCOs. The elderly and people with disabilities were the group least likely to be covered through managed care contracts, with only 16 of the 39 MCO states covering 75 percent or more such enrollees through MCOs (Figure 3).
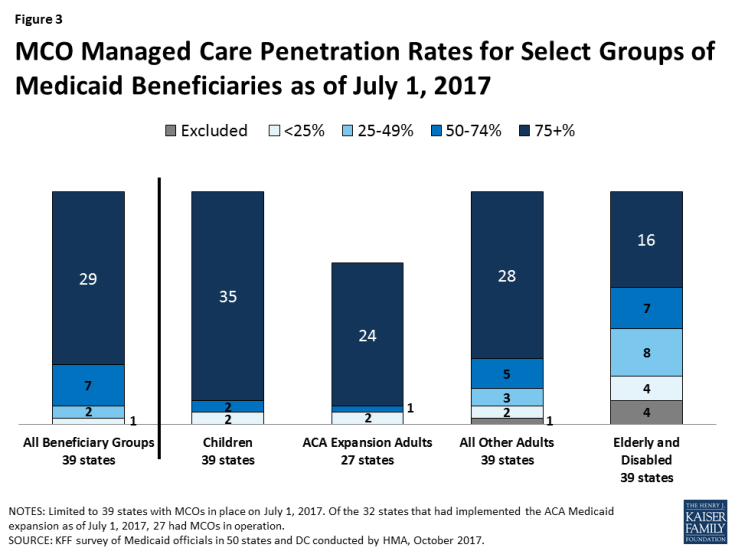
Figure 3: MCO Managed Care Penetration Rates for Select Groups of Medicaid Beneficiaries as of July 1, 2017
Of the 32 states that had implemented the ACA Medicaid expansion as of July 1, 2017, 27 were using MCOs to cover newly eligible adults. (The five Medicaid expansion states without risk-based managed care were Alaska, Arkansas, Connecticut, Montana, and Vermont.) The large majority (24) of these 27 states covered more than 75 percent of beneficiaries in this group through risk-based managed care. New Hampshire, however, reported that approximately 80 percent of its ACA expansion adults receive premium assistance to enroll in Qualified Health Plans in the state’s Marketplace and that only 13.5 percent were enrolled in MCOs. The other two states reporting less than 75 percent MCO penetration for this group were Colorado and Illinois.
Seven of the 16 states with PCCM programs also contract with MCOs. In most of these states, MCOs cover a larger share of beneficiaries than PCCM programs. However, Colorado and North Dakota are exceptions. As of July 1, 2017, a majority of Colorado’s enrollees were in the PCCM program, which is the foundation of the state’s Accountable Care Collaboratives, and 40 percent of enrollees in North Dakota were enrolled in the PCCM program (compared to 25 percent in the MCO program).
Only two states reported policies implemented in FY 2017 or planned for FY 2018 that reduced or will reduce the states’ reliance on the MCO model of managed care: Colorado reported that a small MCO pilot initiated on July 1, 2016 terminated on June 30, 2017, and Massachusetts reported that the implementation of its Accountable Care Organization (ACO) program in FY 2018 will result in the transition of MCO enrollees to ACOs.
Populations with Special Needs
For geographic areas where MCOs operate, this year’s survey asked MCO states whether, as of July 1, 2017, certain subpopulations with special needs were enrolled in MCOs for their acute care services on a mandatory or voluntary basis or were always excluded. On the survey, states selected from “always mandatory,” “always voluntary,” “varies,” or “always excluded” for the following populations: pregnant women, foster children, persons with intellectual and developmental disabilities (ID/DD), children with special health care needs (CSHCNs), persons with a serious mental illness (SMI) or serious emotional disorder (SED), and adults with physical disabilities. This year’s survey found an increase in the number of states reporting that enrollment for these populations is always mandatory (Exhibit 2).
As shown in Exhibit 2 and Table 5, and consistent with results in last year’s survey, pregnant women were the group most likely to be enrolled on a mandatory basis while persons with ID/DD were least likely to be enrolled on mandatory basis and also most likely to be excluded from MCO enrollment. Foster children were the group most likely to be enrolled on a voluntary basis, although they were enrolled on a mandatory basis in a larger number of states. Among states indicating that the enrollment approach for a given group or groups varied, LTSS eligibility was the most frequently cited basis of variation.
| Exhibit 2: MCO Enrollment of Populations with Special Needs, July 1, 2017 (# of States) | ||||||
| Pregnant women | Foster children | Persons with ID/DD | CSHCNs | Persons with SMI/SED | Adults w/ physical disabilities | |
| Always mandatory8 | 32 | 20 | 11 | 20 | 18 | 19 |
| Always voluntary | 2 | 8 | 4 | 3 | 3 | 4 |
| Varies | 4 | 8 | 16 | 14 | 16 | 11 |
| Always excluded | 1 | 3 | 8 | 2 | 2 | 5 |
Acute Care Managed Care Population Changes
In both FY 2017 and FY 2018, only a few states reported actions to increase enrollment in acute care managed care, reflecting full or nearly full MCO saturation in most MCO states. Of the 39 states with MCOs, a total of 14 states indicated that they made specific policy changes in either FY 2017 (7 states) or FY 2018 (8 states) to increase the number of enrollees in MCOs through geographic expansion, voluntary or mandatory enrollment of new groups into MCOs, or mandatory enrollment of specific eligibility groups that were formerly enrolled on a voluntary basis (Exhibit 3). Thirty-six states reported that acute care MCOs were operating statewide as of July 2017 and Illinois reported plans to expand MCOs statewide in FY 2018. The remaining two states without statewide MCO programs (Colorado and Nevada) did not report a geographic expansion planned for FY 2018.
| Exhibit 3: Medicaid Acute Care Managed Care Population Expansions, FY 2017 and FY 2018 | ||
| FY 2017 | FY 2018 | |
| Geographic Expansions | MO | IL |
| New Population Groups Added | LA, NE, OH, TX, WV | IL, NY, PA, TX |
| Voluntary to Mandatory Enrollment | WA | NY, OR, SC, VA, WI |
Some of the notable acute care MCO expansions include:
- West Virginia transitioned its SSI population from FFS to mandatory MCO enrollment in July 2016.
- Missouri extended its MCO program geographically statewide on May 1, 2017 for children, pregnant women, refugees, and custodial parents.
- In January 2018, Pennsylvania will begin to phase-in its Community HealthChoices program which will provide both physical health and long-term services and supports through newly contracted MCOs. CHC enrollees will include individuals in nursing facilities (currently carved out of managed care after 30 days), full benefit dually-eligible individuals, and individuals receiving home and community-based services.
In FY 2017 and FY 2018, states expanded MCO enrollment (either voluntary or mandatory) to additional groups. Some states added multiple groups. Some groups that states added or are planning to add include: foster care or adoption assistance children (New York, Ohio, and Texas); persons eligible for LTSS (Nebraska, New York, Ohio, Pennsylvania, and Texas); ACA expansion, newly eligible adult group and enrollees in the state’s Health Insurance Premium Payment Program (Louisiana); Breast and Cervical Cancer Treatment Program group (Ohio and Texas); children with special health care needs or SSI (Illinois, Ohio, and Texas); SSI population (West Virginia); and persons with intellectual and developmental disabilities (Nebraska and Ohio).
One state in FY 2017 and five in FY 2018 made enrollment mandatory for a specific eligibility group that was formerly enrolled on a voluntary basis: Washington (clients with Third Party Liability (TPL)/other insurance, excluding Medicare); New York (children with special health care needs in 1915(c) waiver programs); Oregon (Medicare/Medicaid dual eligibles); South Carolina (former foster care adults); Virginia (aged, blind, and disabled enrollees); and Wisconsin (SSI adults that do not have LTSS needs).
Services Covered Under MCO Contracts
Behavioral Health Services Covered Under MCO Contracts
Although MCOs are at risk financially for providing a comprehensive set of acute care services, nearly all states exclude or “carve-out” certain services from their MCO contracts, most commonly behavioral health services. In this year’s survey, states with acute care MCOs were asked to indicate whether specialty outpatient mental health (MH) services, inpatient mental health services, and outpatient and inpatient substance use disorder (SUD) services are always carved-in (i.e., virtually all services are covered by the MCO), always carved-out (to PHP or FFS), or carve-in status varies by geographic or other factors.
For purposes of this survey, “specialty outpatient mental health” services mean services used by adults with Serious Mental Illness (SMI) and/or youth with serious emotional disturbance (SED), commonly provided by specialty providers such as community mental health centers. Depending on the service, more than half of the 39 MCO states reported that specific behavioral health service types were carved into their MCO contracts, with specialty outpatient mental health services somewhat less likely to be carved in (Exhibit 4 and Table 6). Also, with the exception of inpatient SUD services, the number of states reporting that the other services were always carved-in increased modestly from last year.
| Exhibit 4: MCO Coverage of Behavioral Health, July 1, 2017 (# of States) | ||||
| Specialty Outpatient MH | Inpatient MH | Outpatient SUD | Inpatient SUD | |
| Always carved-in | 23 | 26 | 26 | 26 |
| Always carved-out | 11 | 8 | 8 | 7 |
| Varies | 5 | 5 | 5 | 6 |
States reporting actions in FY 2017 to carve in behavioral health services into their MCO contracts (in at least some regions/contracts) included six states (Minnesota, Nebraska, South Carolina, Texas, Virginia, and Washington). In FY 2018, ten states (Louisiana, Michigan, Minnesota, Mississippi, New Jersey, New York, Ohio, South Carolina, Washington, and West Virginia) report new/continued actions to carve in behavioral health services.
Institutions for Mental Diseases (IMD) Rule Change
The 2016 Medicaid Managed Care Final Rule9 allows states (under the authority for health plans to cover services “in lieu of” those available under the Medicaid state plan), to receive federal matching funds for capitation payments on behalf of adults who receive inpatient psychiatric or substance use disorder treatment or crisis residential services in an IMD for no more than 15 days in a month.10 States were asked in the survey whether they planned to use this new authority. Of the 39 states with MCOs, 26 states answered “yes” for FY 2017, FY 2018, or both FYs 2017 and 2018, five states answered “no,” and eight states answered “undetermined.”
States were also asked whether they believed the Final Rule allows MCOs sufficient flexibility to provide cost-effective “in lieu of” IMD services to meet acute inpatient or residential treatment needs for members with severe mental illness (SMI) or substance use disorders (SUDs). Only a small number of states (9 for SMI and 8 for SUD) answered “yes.” The remaining MCO states answered “no” (19 for SMI and 19 for SUD) or “don’t know” (11 for SMI and 12 for SUD). Many states commented that the 15-day limit was too restrictive, especially for SUD services, and a number of states indicated plans to seek a Section 1115 waiver to cover more than 15 days per month.11
Additional Services
States with MCO contracts reported that plans in their states may offer a range of services beyond those described in the state plan or waivers. Eleven states reported that MCOs provide limited or enhanced adult dental services beyond contractually required state plan benefits, and nine states reported enhanced vision services for adults. Several states noted that MCOs offer cell phones for reminder services or other technology supports from scales to telemedicine. Half of MCO states reported that MCOs provide a wide variety of non-clinical supports as value added services, including infant car seats and cribs, nominal gift cards for healthy behavior, air conditioners for asthma treatment, weight management classes or memberships, and even support for obtaining a GED. Health education, wellness supports, and non-traditional therapies were also noted by some states.
Managed Care (Acute and LTSS) Quality, Contract Requirements, and Administration
Quality Initiatives
Over time, the expansion of comprehensive risk-based managed care in Medicaid has been accompanied by greater attention to measuring quality and plan performance and, increasingly, to measuring health outcomes. After years of comprehensive risk-based managed care experience within the Medicaid program, many states now incorporate quality into the procurement process, as well as into ongoing program monitoring.
States procure MCO contracts using different approaches; however, most states use competitive bidding, in part because the dollar value is so large. Under these procurements, states can specify requirements and criteria that go beyond price, and may expect plans to compete on the basis of value-based payment arrangements with network providers, specific policy priorities such as improving birth outcomes, or strategies to address social determinants of health, and/or other specific performance and quality criteria. In this year’s survey, states were asked if they used, or planned to use, National Committee for Quality Assurance’s (NCQA’s) Healthcare Effectiveness Data and Information Set (HEDIS®) scores as criteria for selecting MCOs. Of the 39 states with MCOs, 18 indicated that they used or plan to use HEDIS scores as criteria for selecting MCOs.
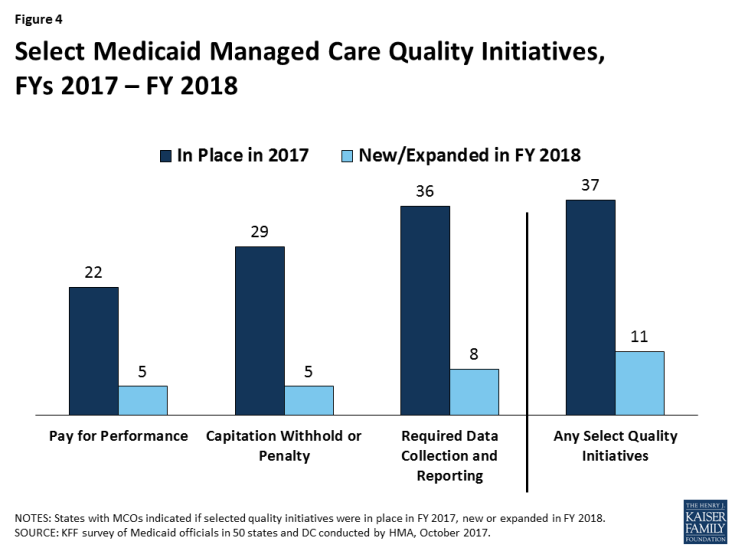
States were asked to indicate whether they had select quality strategies in place in FY 2017 and to indicate newly added or expanded initiatives for FY 2018. Thirty-seven MCO states reported one or more select MCO quality initiatives in place in FY 2017 (Figure 4 and Table 7). The most common strategies were requirements for data collection and reporting (often public reporting) on quality measures and the use of quality-based capitation withholds or penalties. Withhold amounts for acute care services typically ranged from 1 percent (Michigan, Oregon, and Washington) to 5 percent (Minnesota and Missouri); managed long-term services and supports (MLTSS) withhold amounts typically ranged from 0.5 percent (Iowa and Wisconsin) to 3 percent (California and Ohio). Over half the 39 states with managed care contracts reported the use of pay for performance strategies. In addition, several states reported “other” quality initiatives, including the use of liquidated damages for poor performance and the required operation of and reporting on performance improvement projects (PIPs).
In FY 2018, 11 states expect to implement new or expanded quality initiatives (Figure 4). The most common new quality initiatives are pay for performance initiatives while the most common expanded initiatives are data collection and reporting initiatives (Table 7).
Contract Requirements
Alternative [Provider] Payment Models within MCO Contracts
Value-based purchasing (VBP) strategies are important tools for states pursuing improved quality and outcomes and reduced costs of care within Medicaid and across payers. Generally speaking, VBP strategies include activities that hold a provider or MCO accountable for cost and quality of care.12 This often includes efforts to implement alternative payment models (APMs). APMs replace FFS/volume-driven provider payments with payment models that incentivize quality, coordination, and value (e.g., shared savings/shared risk arrangements and episode-based payments). Many states have included a focus on adopting and promoting APMs as part of their federally supported State Innovation Models (SIM) projects and as part of delivery system reform efforts approved under Section 1115 Medicaid waivers.13 States are increasingly encouraging or requiring Medicaid MCOs to adopt APMs to advance VBP in Medicaid. The survey found that:
- Thirteen states (Arizona, California, Delaware, Hawaii, Nebraska, New Hampshire, New Mexico, New York, Ohio, Pennsylvania, Rhode Island, South Carolina, and Washington) identified a specific target in their MCO contracts for the percentage of provider payments, network providers, or plan members that plans must cover via alternative provider payment models in FY 2017 (compared to five states in FY 2016); and
- Nine additional states (District of Columbia, Iowa, Kansas, Louisiana, Michigan, New Jersey, Oregon, Texas, and West Virginia) will include a target percentage in their contracts for FY 2018.
| State APM Targets for Medicaid MCOs |
|
Further, in FY 2017, eight states had contracts that required Medicaid MCOs to adopt specific alternative provider payment models (e.g., episode of care payments, shared savings/shared risk, etc.), while eight states had contracts that encouraged MCOs to adopt specific APMs. In FY 2018, four additional states plan to require the use of specific APMs while five additional states plan to encourage use of specific APMs. The box below provides state examples of APM requirements.
| State-Specific APM Requirements |
|
Social Determinants of Health
In April 2017, the CMS Center for Medicare and Medicaid Innovation selected 32 organizations to implement and test models to support local communities in addressing the health-related social needs of Medicare and Medicaid beneficiaries, aiming to bridge the gap between clinical and community service providers. This “Accountable Health Communities” model represents the first CMS innovation model that focuses on social determinants of health. The goal of the five-year program is to encourage innovation to deliver local solutions that improve access to community-based services.15 This development reflects growing awareness and interest on the part of CMS to address other issues, such as housing and food insecurity, by linking beneficiaries to social services and supports, ultimately to improve health and health outcomes. States have also focused on addressing social determinants of health, so federal and state activity are occurring simultaneously.
The survey found that, of the 39 MCO states, 19 states required while 12 states encouraged MCOs to screen enrollees for social needs and provide referrals to other services in FY 2017. Two additional states plan to require and two plan to encourage MCOs to screen/refer enrollees for social needs in FY 2018.
| Strategies to Address Social Determinants of Health |
|
Criminal Justice-Involved Populations
Engaging Medicaid MCOs in efforts to improve continuity of care for individuals released from correctional facilities into the community is important to ensure that individuals with complex or chronic health conditions, including behavioral health needs, have an effective transition to treatment in the community. In FY 2017, of the 39 states that contract with MCOs, six states (Arizona, Iowa, Kansas, Louisiana, Ohio, and Virginia) require MCOs to provide care coordination services to enrollees prior to release from incarceration, while two states (Kentucky and New Mexico) encourage MCOs to provide care coordination services prior to release. Five states intend to use contracts to encourage or require such care coordination in FY 2018. The following are examples of pre-release state requirements: Louisiana requires plans to offer care management at least 30 days prior to scheduled release; Kansas requires pre-release care management for LTSS populations, and new legislation in Washington will require care coordination pre-release and post-incarceration in FY 2018. New Mexico, a state that encourages but does not require pre-release activity, reported that one health plan is piloting a care coordination model through collaboration with a metropolitan detention center to test and learn effective methods to impact recidivism and improve public health and safety.
Administrative Policies
Minimum Medical Loss Ratios
The Medical Loss Ratio (MLR) is the proportion of total capitation payments received by an MCO spent on clinical services and quality improvement. CMS published a final rule in 2016 that requires states to develop capitation rates for Medicaid to achieve an MLR of at least 85 percent in the rate year, for rating periods and contracts starting on or after July 1, 2017.16 This 85 percent minimum MLR is the same standard that applies in Medicare Advantage and private large group plans. There is no federal requirement that Medicaid plans must pay remittances to the state if they fail to meet the MLR standard, but states have discretion to require remittances.
As of July 1, 2017, 25 of the 39 states that contract with comprehensive risk-based MCOs specified a minimum MLR in Medicaid MCO contracts. Twenty of these 25 states applied the MLR requirement to all MCO contracts, while five states applied it on a limited basis. Seventeen of the 25 states with minimum MLR requirements always require remittance payments to the state if the minimum MLR is not achieved; one state (Ohio) requires remittance under some circumstances.17
Medicaid MLRs vary by state but are most commonly set at 85 percent or higher. A few states noted that their minimum MLRs varied by type of plan or population. For example, in New Jersey, the MLR is calculated separately for each population covered, with an MLR of 85 percent set for acute care contracts and an MLR of 90 percent set for MLTSS contracts.
Table 8 provides state-specific information regarding the use of a minimum MLR.
Auto-Enrollment
Generally, beneficiaries who are required to enroll in MCOs must be offered a choice of at least two plans. Those who do not select a plan are auto-enrolled in a plan by the state. The proportion of MCO beneficiaries who are auto-enrolled varies widely across states. State auto-enrollment algorithms also vary, but usually take into consideration variables like previous plan or provider relationships, beneficiary geographic location, and/or plan enrollments of other family members. States may also aim to balance enrollment among plans. As of July 1, 2017, 11 states took plan quality or performance rankings into consideration in the auto-enrollment algorithm (Arizona, California, Hawaii, Michigan, Minnesota, New Mexico, New York, Ohio, South Carolina, Virginia, and Washington).
PCCM and PHP Program Changes
Primary Care Case Management (PCCM) Program Changes
Of the 16 states with PCCM programs, two reported enacting policies to increase PCCM enrollment in FY 2017 or FY 2018: Colorado reported continued growth in its PCCM-based Accountable Care Collaboratives in both FY 2017 and FY 2018, and Arkansas reported implementing new billing software that would auto-assign beneficiaries to a primary care physician. Two other states reported new PCCM programs: Alaska – one of only three states without either an MCO or PCCM program as of July 1, 2017 – reported plans to implement a PCCM program in FY 2018, and Arizona reported plans to implement an American Indian Medical Home effective October 1, 2017 using PCCM authority.
Three states18 (California, Illinois, and Massachusetts) reported actions to decrease enrollment in a PCCM program in FY 2017 or FY 2018. California plans to transition its one-county HIV PCCM program to a full-risk MCO model in CY 2018; Illinois reported that its Integrated Health Homes would move to managed care under new MCO contracts that would begin in FY 2018, and Massachusetts reported that implementation of its Accountable Care Organization (ACO) program in FY 2018 will include the transition of PCCM members to ACO Plans.
Limited-Benefit Prepaid Health Plans (PHP) Changes
In this year’s survey, the 25 states contracting with at least one PHP as of July 1, 2017, were asked to indicate whether certain services (listed in Exhibit 5 below) were provided under these arrangements. The most frequently cited services provided (of those included in the question) were outpatient mental health services (14 states), followed by non-emergency medical transportation (NEMT) (12 states) and inpatient mental health and outpatient substance use disorder (SUD) treatment services (11 states each).
| Exhibit 5: Services Covered Under PHP Contracts, July 1, 2017 | ||
| # of States | States19 | |
| Outpatient Mental Health | 14 | CA, CO, HI, ID, MA, MI, NC, OR, PA, TN, UT, WA, WI, WY |
| Inpatient Mental Health | 11 | CA, CO, HI, MA, MI, NC, PA, TN, UT, WA, WI |
| Outpatient Substance Use Disorder Treatment | 11 | CO, ID, MA, MI, NC, OR, PA, TN, UT, WA, WI |
| Inpatient Substance Use Disorder Treatment | 9 | CO, MA, MI, NC, PA, TN, UT, WA, WI |
| Non-Emergency Medical Transportation (NEMT) | 12 | FL, IA, KY, ME, MI, NJ, OK, RI, TN, TX, UT, WI |
| Dental | 9 | CA, IA, ID, LA, MI, RI, TN, TX, UT |
| Long-Term Services and Supports | 6 | ID, MI, NC, NY, TN, WI |
| Vision | 1 | TN |
Nine states reported implementing policies to increase PHP enrollment in FY 2017 or FY 2018. Five states (Arkansas, Iowa, Idaho, Nebraska, and Nevada) reported new or expanded dental PHPs in FY 2018, Indiana reported plans for an NEMT PHP contract in FY 2018, California reported adding inpatient SUD treatment to its PHP program in FY 2018, Louisiana will add “Coordinated System of Care” PHPs in FY 2018 (serving youth with behavioral health challenges and their families), and New York reported increased enrollment in its LTSS PHPs in both FY 2017 an FY 2018.
Four states also reported actions to decrease PHP enrollment in FY 2017 or FY 2018. Nebraska and Texas reported ending a behavioral health PHP and folding the covered services into MCO contracts in FY 2017. Washington reported that PHP enrollment decreased in FY 2017 and will decrease further in FY 2018 when the state converts behavioral health PHPs to fully integrated MCO contracts in additional geographic areas. Massachusetts reported that implementation of its Accountable Care Organization (ACO) program in FY 2018 will reduce enrollments in its behavioral health PHP program.
TABLE 4: SHARE OF THE MEDICAID POPULATION COVERED UNDER DIFFERENT DELIVERY SYSTEMS IN ALL 50 STATES AND DC, AS OF JULY 1, 2017
| States | Type(s) of Managed Care In Place | Share of Medicaid Population in Different Managed Care Systems | ||
| MCO | PCCM | FFS / Other | ||
| Alabama | PCCM | — | 86.4% | 13.6% |
| Alaska | FFS | — | — | 100.0% |
| Arizona | MCO | 93.1% | — | 6.9% |
| Arkansas* | PCCM | — | NR | NR |
| California | MCO and PCCM* | 78.9% | — | 21.1% |
| Colorado | MCO and PCCM* | 10.5% | 72.6% | 16.9% |
| Connecticut | FFS* | — | — | 100.0% |
| DC | MCO | 78.0% | — | 22.0% |
| Delaware | MCO | 94.2% | — | 5.8% |
| Florida | MCO | 92.0% | — | 8.0% |
| Georgia | MCO | 73.0% | — | 27.0% |
| Hawaii | MCO | 99.9% | — | <0.1% |
| Idaho* | PCCM | — | 95.0% | 5.0% |
| Illinois | MCO and PCCM | 63.4% | 10.4% | 26.2% |
| Indiana | MCO | 80.0% | — | 20.0% |
| Iowa | MCO | 92.6% | — | 7.4% |
| Kansas | MCO | 95.0% | — | 5.0% |
| Kentucky | MCO | 91.0% | — | 9.0% |
| Louisiana | MCO | 92.0% | — | 8.0% |
| Maine | PCCM | — | NR | NR |
| Maryland | MCO | 89.2% | — | 10.8% |
| Massachusetts | MCO and PCCM | 48.0% | 21.0% | 31.0% |
| Michigan | MCO | 74.5% | — | 25.5% |
| Minnesota | MCO | 76.0% | — | 24.0% |
| Mississippi | MCO | 70.0% | — | 30.0% |
| Missouri | MCO | 75.8% | — | 24.2% |
| Montana | PCCM | — | 72.0% | 28.0% |
| Nebraska | MCO | 99.6% | — | 0.4% |
| Nevada | MCO and PCCM | 72.0% | 6.0% | 22.0% |
| New Hampshire* | MCO | 73.0% | — | 4.1% |
| New Jersey | MCO | 95.8% | — | 4.2% |
| New Mexico | MCO | 88.7% | — | 11.3% |
| New York | MCO | 82.7% | — | 17.3% |
| North Carolina | PCCM | — | 90.0% | 10.0% |
| North Dakota | MCO and PCCM | 25.0% | 40.0% | 35.0% |
| Ohio | MCO | 88.5% | — | 11.5% |
| Oklahoma | PCCM | — | 75.1% | 24.9% |
| Oregon | MCO* | 89.0% | — | 11.0% |
| Pennsylvania | MCO | 82.3% | — | 17.7% |
| Rhode Island | MCO | 90.4% | — | 9.6% |
| South Carolina | MCO* | 76.0% | — | 24.0% |
| South Dakota | PCCM | — | 80.0% | 20.0% |
| Tennessee | MCO | 100.0% | — | 0.0% |
| Texas | MCO* | 91.7% | — | 8.1% |
| Utah | MCO | 84.9% | — | 15.1% |
| Vermont | PCCM | — | 63.0% | 37.0% |
| Virginia | MCO | 76.0% | — | 24.0% |
| Washington | MCO and PCCM | 85.0% | 2.0% | 13.0% |
| West Virginia | MCO | 80.0% | — | 20.0% |
| Wisconsin | MCO | 67.0% | — | 33.0% |
| Wyoming | FFS* | 0.2% | — | 99.8% |
| NOTES: NR – not reported. Share of Medicaid Population that is covered by different managed care systems. MCO refers to risk-based managed care; PCCM refers to Primary Care Case Management. FFS/Other refers to Medicaid beneficiaries who are not in MCOs or PCCM programs. *AR – Most Expansion Adults served by Qualified Health Plans through “Arkansas Works” premium assistance waiver. *CA – PCCM program operates in LA county for those with HIV. *CO – PCCM enrollees are part of the state’s Accountable Care Collaboratives (ACCs). *CT – terminated its MCO contracts in 2012 and now operates its program on a fee-for-service basis using four ASO entities. *ID – The Medicaid-Medicare Coordinated Plan (MMCP) has been recategorized by CMS as an MCO but is not counted here as such since it is secondary to Medicare. *NH – 22.9% of overall population and 80.1% of Expansion Adults are served by Qualified Health Plans under NH’s premium assistance program waiver *OR – MCO enrollees include those enrolled in the state’s Coordinated Care Organizations. *SC – uses PCCM authority to provide care management services to approximately 200 medically complex children. *TX – Texas Medicaid Wellness program provides care management services for high-cost/high-risk enrollees (under PCCM authority).*WY – the state does not operate a traditional PCCM or MCO program, but does use PCCM authority to make PCMH payments. SOURCE: Kaiser Family Foundation Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2017. |
||||
TABLE 5: ENROLLMENT OF SPECIAL POPULATIONS UNDER MEDICAID MANAGED CARE CONTRACTS FOR ACUTE CARE IN ALL 50 STATES AND DC, AS OF JULY 1, 2017
| States | Pregnant Women | Foster Children | Persons with ID/DD | CSHCNs | Persons with SMI/SED | Adults w/ physical disabilities |
| Alabama | — | — | — | — | — | — |
| Alaska | — | — | — | — | — | — |
| Arizona | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| Arkansas | — | — | — | — | — | — |
| California | Always mandatory | Varies | Varies | Always mandatory | Always mandatory | Always mandatory |
| Colorado | Always voluntary | Always voluntary | Always voluntary | Always voluntary | Always voluntary | Always voluntary |
| Connecticut | — | — | — | — | — | — |
| DC | Always mandatory | Varies | Always excluded | Varies | Varies | Varies |
| Delaware | Always mandatory | Always mandatory | Varies | Always mandatory | Always mandatory | Always mandatory |
| Florida | Always mandatory | Always mandatory | Always voluntary | Always mandatory | Always mandatory | Always mandatory |
| Georgia | Always mandatory | Always mandatory | Always excluded | Always excluded | Always excluded | Always excluded |
| Hawaii | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| Idaho | — | — | — | — | — | — |
| Illinois | Varies | Always excluded | Varies | Varies | Varies | Varies |
| Indiana | Always mandatory | Always voluntary | Varies | Varies | Varies | Varies |
| Iowa | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| Kansas | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| Kentucky | Varies | Varies | Varies | Varies | Varies | Varies |
| Louisiana | Always mandatory | Always mandatory | Varies | Always mandatory | Varies | Varies |
| Maine | — | — | — | — | — | — |
| Maryland | Always mandatory | Always mandatory | Varies | Varies | Varies | Always excluded |
| Massachusetts | Always voluntary | Always voluntary | Always voluntary | Always voluntary | Always voluntary | Always voluntary |
| Michigan | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| Minnesota | Always mandatory | Always voluntary | Always excluded | Always voluntary | Varies | Always voluntary |
| Mississippi | Always mandatory | Always voluntary | Varies | Varies | Varies | Varies |
| Missouri | Always mandatory | Always mandatory | Always excluded | Varies | Varies | Always excluded |
| Montana | — | — | — | — | — | — |
| Nebraska | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| Nevada | Always mandatory | Varies | Always excluded | Varies | Varies | Always excluded |
| New Hampshire | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| New Jersey | Varies | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| New Mexico | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| New York | Always mandatory | Varies | Varies | Varies | Always mandatory | Always mandatory |
| North Carolina | — | — | — | — | — | — |
| North Dakota | Always excluded | Always excluded | Always excluded | Always excluded | Always excluded | Always excluded |
| Ohio | Always mandatory | Always mandatory | Varies | Varies | Varies | Always mandatory |
| Oklahoma | — | — | — | — | — | — |
| Oregon | Always mandatory | Varies | Varies | Always mandatory | Always mandatory | Always mandatory |
| Pennsylvania | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| Rhode Island | Always mandatory | Always mandatory | Varies | Always mandatory | Varies | Varies |
| South Carolina | Always mandatory | Always voluntary | Always excluded | Varies | Varies | Varies |
| South Dakota | — | — | — | — | — | — |
| Tennessee | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory | Always mandatory |
| Texas | Always mandatory | Always voluntary | Varies | Always mandatory | Always mandatory | Always mandatory |
| Utah | Varies | Varies | Varies | Varies | Varies | Varies |
| Vermont | — | — | — | — | — | — |
| Virginia | Always mandatory | Always mandatory | Varies | Varies | Varies | Varies |
| Washington | Always mandatory | Always voluntary | Varies | Always mandatory | Always mandatory | Always mandatory |
| West Virginia | Always mandatory | Always excluded | Always excluded | Always mandatory | Varies | Varies |
| Wisconsin | Always mandatory | Varies | Always voluntary | Varies | Always voluntary | Always voluntary |
| Wyoming | — | — | — | — | — | — |
| Always Mandatory | 32 | 20 | 11 | 20 | 18 | 19 |
| Always Voluntary | 2 | 8 | 4 | 3 | 3 | 4 |
| Varies | 4 | 8 | 16 | 14 | 16 | 11 |
| Always Excluded | 1 | 3 | 8 | 2 | 2 | 5 |
| NOTES: “–” indicates there were no MCOs operating in that state’s Medicaid program in July 2017. ID/DD – intellectual and developmental disabilities, CSHCN – Children with special health care needs, SMI – Serious Mental Illness, SED – Serious Emotional Disturbance. States were asked to indicate for each group if enrollment in MCOs is “always mandatory,” “always voluntary,” “varies,” or if the group is “always excluded” from MCOs as of July 1, 2017. SOURCE: Kaiser Family Foundation Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2017. |
||||||
TABLE 6: BEHAVIORAL HEALTH SERVICES COVERED UNDER ACUTE CARE MCO CONTRACTS IN ALL 50 STATES AND DC, AS OF JULY 1, 2017
| States | Specialty OP Mental Health | Inpatient Mental Health | Outpatient SUD | Inpatient SUD |
| Alabama | — | — | — | — |
| Alaska | — | — | — | — |
| Arizona | Varies | Varies | Varies | Varies |
| Arkansas | — | — | — | — |
| California | Always Carved-out | Always Carved-out | Always Carved-out | Always Carved-out |
| Colorado | Always Carved-out | Always Carved-out | Always Carved-out | Always Carved-out |
| Connecticut | — | — | — | — |
| DC | Always Carved-in | Always Carved-in | Always Carved-out | Always Carved-in |
| Delaware | Varies | Always Carved-in | Always Carved-in | Always Carved-in |
| Florida | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Georgia | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Hawaii | Always Carved-out | Always Carved-out | Always Carved-in | Always Carved-in |
| Idaho | — | — | — | — |
| Illinois | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Indiana | Always Carved-out | Always Carved-in | Always Carved-in | Always Carved-in |
| Iowa | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Kansas | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Kentucky | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Louisiana | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Maine | — | — | — | — |
| Maryland | Always Carved-out | Always Carved-out | Always Carved-out | Always Carved-out |
| Massachusetts | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Michigan | Always Carved-out | Always Carved-out | Always Carved-out | Always Carved-out |
| Minnesota | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Mississippi | Always Carved-in | Always Carved-in | Varies | Varies |
| Missouri | Always Carved-out | Varies | Varies | Varies |
| Montana | — | — | — | — |
| Nebraska | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Nevada | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| New Hampshire | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| New Jersey | Varies | Varies | Varies | Varies |
| New Mexico | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| New York | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| North Carolina | — | — | — | — |
| North Dakota | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Ohio | Always Carved-out | Always Carved-out | Always Carved-out | Always Carved-out |
| Oklahoma | — | — | — | — |
| Oregon | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Pennsylvania | Always Carved-out | Always Carved-out | Always Carved-out | Always Carved-out |
| Rhode Island | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| South Carolina | Always Carved-in | Varies | Always Carved-in | Always Carved-in |
| South Dakota | — | — | — | — |
| Tennessee | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Texas | Always Carved-in | Always Carved-in | Always Carved-in | Always Carved-in |
| Utah | Always Carved-out | Always Carved-out | Always Carved-out | Always Carved-out |
| Vermont | — | — | — | — |
| Virginia | Always Carved-out | Always Carved-in | Always Carved-in | Always Carved-in |
| Washington | Varies | Varies | Varies | Varies |
| West Virginia | Always Carved-in | Always Carved-in | Always Carved-in | Varies |
| Wisconsin | Varies | Always Carved-in | Always Carved-in | Always Carved-in |
| Wyoming | — | — | — | — |
| Always Carved-in | 23 | 26 | 26 | 26 |
| Always Carved-out | 11 | 8 | 8 | 7 |
| Varies | 5 | 5 | 5 | 6 |
| NOTES: OP – Outpatient. SUD – Substance Use Disorder. “–” indicates there were no MCOs operating in that state’s Medicaid program in July 2017. For beneficiaries enrolled in an MCO for acute care benefits, states were asked to indicate whether these benefits are always carved-in (meaning virtually all services are covered by the MCO), always carved-out (to PHP or FFS), or whether the carve-in varies (by geography or other factor). “Specialty outpatient mental health” refers to services utilized by adults with Serious Mental Illness (SMI) and/or youth with serious emotional disturbance (SED) commonly provided by specialty providers such as community mental health centers. SOURCE: Kaiser Family Foundation Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2017. |
||||
TABLE 7: SELECT MEDICAID MANAGED CARE QUALITY INITIATIVES IN ALL 50 STATES AND DC, IN PLACE IN FY 2017 AND ACTIONS TAKEN IN FY 2018
| States | Pay for Performance/ Performance Bonus |
Capitation Withhold or Penalty | Required Data Collection and Reporting | Any Select Quality Initiatives | ||||||||
| In Place | New | Expanded | In Place | New | Expanded | In Place | New | Expanded | In Place | New | Expanded | |
| 2017 | 2018 | 2018 | 2017 | 2018 | 2018 | 2017 | 2018 | 2018 | 2017 | 2018 | 2018 | |
| Alabama | ||||||||||||
| Alaska | ||||||||||||
| Arizona | ||||||||||||
| Arkansas | ||||||||||||
| California | X | X | X | |||||||||
| Colorado | X | X | ||||||||||
| Connecticut | ||||||||||||
| DC | X | X | X | X | ||||||||
| Delaware | X | X | ||||||||||
| Florida | X | X | X | X | ||||||||
| Georgia | X | X | X | X | X | X | ||||||
| Hawaii | X | X | X | X | X | |||||||
| Idaho | ||||||||||||
| Illinois | X | X | X | X | ||||||||
| Indiana | X | X | X | X | ||||||||
| Iowa | X | X | X | X | ||||||||
| Kansas | X | X | X | X | ||||||||
| Kentucky | X | X | X | X | ||||||||
| Louisiana | X | X | X | X | X | X | ||||||
| Maine | ||||||||||||
| Maryland | X | X | X | X | ||||||||
| Massachusetts | X | X | X | |||||||||
| Michigan | X | X | X | X | ||||||||
| Minnesota | X | X | X | |||||||||
| Mississippi | X | X | ||||||||||
| Missouri | X | X | X | X | X | X | ||||||
| Montana | ||||||||||||
| Nebraska | X | X | X | X | X | X | ||||||
| Nevada | X | X | X | X | X | |||||||
| New Hampshire | X | X | X | X | X | X | ||||||
| New Jersey | X | X | X | X | ||||||||
| New Mexico | X | X | X | |||||||||
| New York | X | X | X | X | X | X | ||||||
| North Carolina | ||||||||||||
| North Dakota | ||||||||||||
| Ohio | X | X | X | X | ||||||||
| Oklahoma | ||||||||||||
| Oregon | X | X | X | X | ||||||||
| Pennsylvania | X | X | X | X | X | X | X | X | X | X | ||
| Rhode Island | X | X | X | X | ||||||||
| South Carolina | X | X | X | X | ||||||||
| South Dakota | ||||||||||||
| Tennessee | X | X | X | X | ||||||||
| Texas | X | X | X | X | X | |||||||
| Utah | X | X | ||||||||||
| Vermont | ||||||||||||
| Virginia | X | X | X | X | ||||||||
| Washington | X | X | X | |||||||||
| West Virginia | X | X | X | |||||||||
| Wisconsin | X | X | X | X | X | X | X | |||||
| Wyoming | ||||||||||||
| Totals | 22 | 4 | 2 | 29 | 2 | 4 | 36 | 2 | 7 | 37 | 5 | 8 |
| NOTES: States with MCO contracts were asked to report if select quality initiatives were included in contracts in FY 2017, or are new or expanded in FY 2018. The table does not reflect all quality initiatives states have included as part of MCO contracts. SOURCE: Kaiser Family Foundation Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2017. |
||||||||||||
TABLE 8: MINIMUM MEDICAL LOSS RATIO POLICIES FOR MEDICAID MCOs IN ALL 50 STATES AND DC, JULY 1, 2017
| Minimum Medical Loss Ratio (MLR) | ||||
| States | Require minimum MLR | % if required | Remittance required if MCO does not meet minimum MLR? | |
| Acute | LTSS | |||
| Alabama | — | |||
| Alaska | — | |||
| Arizona | Yes — always | 85% | 85% | No |
| Arkansas | — | |||
| California | No | |||
| Colorado | Yes — always | 85% | — | Yes — always |
| Connecticut | — | |||
| DC | Yes — always | 85% | — | No |
| Delaware | No | |||
| Florida | Yes — sometimes | 85% | N/A | No |
| Georgia | No | |||
| Hawaii | No | |||
| Idaho | — | |||
| Illinois | Yes — always | 85%* | 88% | Yes — always |
| Indiana | Yes — always | 85-87%* | — | Yes — always |
| Iowa | Yes — always | 88% | 88% | Yes — always |
| Kansas | No | |||
| Kentucky | Yes — always | 90% | — | Yes — always |
| Louisiana | Yes — always | 85% | — | Yes — always |
| Maine | — | |||
| Maryland | Yes — always | 85% | — | Yes — always |
| Massachusetts | Yes — sometimes | N/A | 80%* | No |
| Michigan | Yes — sometimes | 85% | N/A | No |
| Minnesota | No | |||
| Mississippi | Yes — always | 85% | — | Yes — always |
| Missouri | Yes — always | 85% | — | Yes — always |
| Montana | — | |||
| Nebraska | Yes — always | 85% | — | Yes — always |
| Nevada | Yes — always | 85% | — | Yes — always |
| New Hampshire | Yes — always | 89% | — | No |
| New Jersey | Yes — always | 85% | 90% | Yes — always |
| New Mexico | Yes — always | 86% | 86% | No |
| New York | No* | |||
| North Carolina | — | |||
| North Dakota | No | |||
| Ohio | Yes — sometimes | 85% | N/A | Yes — sometimes* |
| Oklahoma | — | |||
| Oregon | Yes — always | 80% | — | Yes — always |
| Pennsylvania | No | |||
| Rhode Island | No | |||
| South Carolina | Yes — sometimes | 86% | N/A | Yes — always |
| South Dakota | — | |||
| Tennessee | No | |||
| Texas | No* | |||
| Utah | No | |||
| Vermont | — | |||
| Virginia | Yes — always | 85% | 85% | Yes — always |
| Washington | Yes — always | 85-87%* | — | Yes — always |
| West Virginia | Yes — always | 85% | — | Yes — always |
| Wisconsin | No | |||
| Wyoming | — | |||
| Yes — always | 20 | 17 | ||
| Yes — sometimes | 5 | 1 | ||
| No | 14 | 7 | ||
| N/A – No MCOs | 12 | |||
| NOTES: In “Require Minimum MLR” column “–” indicates states that do not have Medicaid MCOs and “–” also appears in “LTSS %” column if state does not have MLTSS. “N/A” appears in “LTSS %” column if state with managed LTSS does not have LTSS MLR or in “Acute %” column if MCO state does not have acute MLR. *IL, IN, and WA indicated that the minimum acute MLR varies by population. *MA Senior Care Options (SCO) program has a minimum MLR of 80%. *NY is implementing MLR for acute and MLTSS in CY 2018 which will be effective retroactively to CY 2017. *TX has experience rebate on plans above a certain profit level. SOURCE: Kaiser Family Foundation Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, 2017. |
||||