Medicaid in an Era of Health & Delivery System Reform: Results from a 50-State Medicaid Budget Survey for State Fiscal Years 2014 and 2015
Benefits Changes
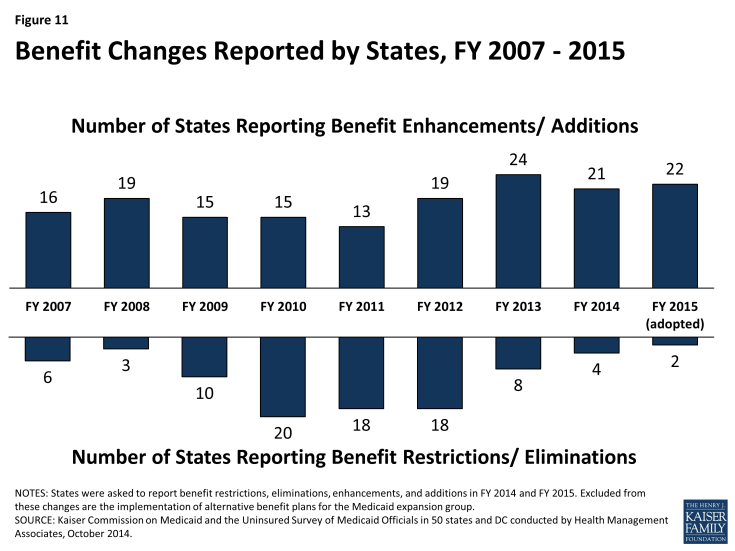
In this year’s survey, the number of states reporting benefit cuts or restrictions – four in FY 2014 and two in FY 2015 – fell to the lowest level since 2008. (Figure 11) A far larger number of states, 21 states in FY 2014 and 22 in FY 2015, reported enhancing or adding new benefits. (Figure 11) The most common benefit enhancements or additions reported were for behavioral health services (10 in FY 2014; 5 in FY 2015.)
Other common benefit enhancements reported include home and community-based services (4 states in FY 2014; 9 states in FY 2015) such as Delaware’s new Pathways Program that provides supported employment services for those with disabilities, as well as dental services (7 states in FY 2014; 4 states in FY 2015.) Some states also reported expanding preventive services (adding coverage of vaccines and tobacco cessation services beyond ACA requirements.) South Carolina is planning to expand preventive services (e.g. diabetes screening, physical and behavioral health assessments, HIV screenings) covered under its family planning program. California is planning a notable benefit expansion for pregnant women in FY 2015: since this group will not qualify as “newly eligible” under the ACA, the state is planning to provide the full Medicaid benefit package to pregnant women up to 138 percent FPL in place of the current, more limited pregnancy-related benefit package.
Benefit restrictions reflect the elimination of a covered benefit or the application of utilization controls for existing benefits. Of the four states in FY 2014 reporting cuts or eliminations, two (New York and West Virginia) reported narrowly targeted benefit eliminations. Three states (including New York) applied narrowly targeted limits or utilization controls to existing benefits.
Pennsylvania included several far-reaching benefit changes as part of its original Healthy Pennsylvania waiver proposal. The original waiver proposal would have resulted in two reformed Medicaid benefit packages for all adults: a “high-risk” plan (for medically frail, disabled, pregnant, institutionalized and dual-eligible enrollees) and a “low-risk” plan with fewer benefits. The waiver approved in August 2014 included a one-year waiver that allows the state to not cover non-emergency medical transportation but did not ultimately include most of these benefit changes; instead these changes will be pursued under state plan amendments, based on the agreement reached by CMS and the state on “the overall benefits approach.1” The benefit changes originally proposed included eliminating coverage of some services (e.g. optometry, podiatry, chiropractic, and some long term care services) while also limiting other services (e.g. physician and clinic visits, radiology, laboratory, long-term services.) At the time of this report, state plan amendments had not yet been submitted to CMS.
Table 10 provides a complete listing of Medicaid benefit changes for FYs 2014 and 2015.
| Alternative Benefit Package |
|
In addition to asking about benefit policy changes, this year’s survey asked each of the 28 states that have implemented, or will implement, the ACA Medicaid expansion to identify any key differences between the Alternative Benefits Plan (ABP) offered to newly-eligible adults and the state’s traditional Medicaid State Plan benefit. Alternative Benefit Plans must meet the “Essential Health Benefits” (EHBs) and mental health parity requirements applicable to Qualified Health Plans offering coverage in a Health Insurance Marketplace and also include certain other mandatory services including EPSDT for those under 21, non-emergency medical transportation, family planning services and supplies and FQHC/RHC services.–
–
Most of the Medicaid expansion states reported that their ABP was fully aligned with their regular Medicaid benefit subject to certain exceptions. In some cases, states reported that benefits were added to the ABP that were not included in the regular Medicaid benefits plan including habilitative services in five states, substance abuse or mental health services in three states, chiropractic services in two states, and additional preventive services and hearing aids in one state. Conversely, a number of states identified services found in their standard benefit package that were not included in the ABP including eight states that excluded long term services and supports (LTSS), one state that excluded dental and vision services and one state that excluded certain behavioral health intervention services and inpatient substance abuse and mental health services. Also, both Iowa and Pennsylvania received waiver authority to not offer non-emergency transportation services during the first year only of their waivers.
–
Indiana has submitted a proposal to amend and renew its existing waiver to implement the Medicaid expansion in FY 2015 using the state’s Healthy Indiana Plan (HIP) as a basis. HIP 2.0, if approved, would offer expansion adults two ABPs: HIP Plus and HIP Basic. Expansion adults who make POWER account contributions (described further below under ACA Medicaid Expansion Premium and Cost Sharing Waivers), are eligible for HIP Plus which includes the Essential Health Benefits (EHBs) plus adult vision and dental. HIP Plus is indexed to a comprehensive commercial market benefit plan. New adults at or below 100 percent FPL who do not make POWER account contributions would be eligible for HIP Basic which includes EHBs (but not adult vision and dental) and would be indexed to the lowest actuarial value EHB option. The HIP 2.0 proposal also seeks to waive Non-Emergency Medical Transportation (NEMT) for both HIP Plus and HIP Basic and vision and dental benefits, which are part of EPSDT, would be waived for beneficiaries 19-20 in HIP Basic.2
|
TABLE 10: BENEFIT CHANGES IN THE 50 STATES AND DC, FY 2014 AND 2015 |
||||
| Benefit Changes | ||||
| STATES | FY 2014 | FY 2015 | ||
| Enhancements/ Additions | Restrictions/ Eliminations | Enhancements/ Additions | Restrictions/ Eliminations | |
| Alabama | ||||
| Alaska | ||||
| Arizona | X | X | ||
| Arkansas | ||||
| California | X | X | X | |
| Colorado | X | |||
| Connecticut | X | X | ||
| Delaware | X | X | ||
| DC | X | |||
| Florida | X | |||
| Georgia | X | |||
| Hawaii | X | |||
| Idaho | ||||
| Illinois | X | |||
| Indiana | ||||
| Iowa | ||||
| Kansas | ||||
| Kentucky | X | |||
| Louisiana | X | |||
| Maine | ||||
| Maryland | X | |||
| Massachusetts | X | X | ||
| Michigan | ||||
| Minnesota | X | X | ||
| Mississippi | X | |||
| Missouri | ||||
| Montana | ||||
| Nebraska | X | |||
| Nevada | X | X | ||
| New Hampshire | X | X | ||
| New Jersey | X | |||
| New Mexico | X | |||
| New York | X | X | X | X |
| North Carolina | ||||
| North Dakota | X | |||
| Ohio | ||||
| Oklahoma | ||||
| Oregon | ||||
| Pennsylvania | X | X | ||
| Rhode Island | ||||
| South Carolina | X | X | ||
| South Dakota | ||||
| Tennessee | ||||
| Texas | X | X | ||
| Utah | ||||
| Vermont | X | X | ||
| Virginia | X | X | X | |
| Washington | X | |||
| West Virginia | X | |||
| Wisconsin | X | |||
| Wyoming | ||||
| Totals | 21 | 4 | 22 | 2 |
| NOTES: States were asked to report benefit restrictions, eliminations, enhancements, and additions in FY 2014 and FY 2015. Excluded from these changes are the implementation of alternative benefit plans for the Medicaid expansion group. SOURCE: Kaiser Commission on Medicaid and the Uninsured Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2014. |
||||
Table 11: Benefit Actions Taken in the 50 States and the District of Columbia, FY 2014 and FY 20153 |
||
| State | Fiscal Year | Benefit Changes |
| Alabama | 2014 | |
| 2015 | ||
| Alaska | 2014 | |
| 2015 | ||
| Arizona | 2014 |
Adults (+) Restored coverage for well visits. (October 1, 2013)
Adults (+): Added coverage for HPV vaccine for adults ages 21-26. (October 1, 2013)
|
| 2015 | Adults (+): Eliminating 25-day inpatient hospital limit. (October 1, 2014) | |
| Arkansas | 2014 | |
| 2015 | ||
| California | 2014 |
Aged & Disabled (-): Reduced in-home supportive service hours by 8 percent. (July 1, 2013)
Adults (+): Restored adult dental coverage. (May 1, 2014)
All (+): Restored coverage for enteral nutrition. (May 1, 2014)
All (+): Expanded coverage of mental health services (such as individual, family and group therapy) and substance abuse disorder benefits to achieve parity with the selected EHB benchmark plan. All mental health benefits are subject to MHPAEA. (January 1, 2014)
|
| 2015 |
Aged & Disabled (+): Planning to partially restore FY 2014 in-home supportive services hour reduction (changing reduction to a 7% cut instead of an 8% cut).
Pregnant Women (+): Expansion to full-scope coverage to pregnant women 60-133% FPL.
|
|
| Colorado | 2014 |
Aged & Disabled (+): Added consumer-directed attendant support to Brain Injury Waiver.
Adults (+): Added adult dental coverage. (April 1, 2014)
Adults (+): Enhanced the substance abuse disorder benefit.
All (+): Added coverage for additional preventive services. (January 1, 2014)
|
| 2015 | ||
| Connecticut | 2014 | All (+): Added coverage for male and female condoms and spermicide. (July 1, 2013) |
| 2015 | Adults (+): Expanded coverage for licensed behavioral health clinician services provided by independent practitioners (licensed psychologists, licensed clinical social workers, licensed marital and family therapists, licensed alcohol and drug counselors, and licensed professional counselors). (July 1, 2014) | |
| Delaware | 2014 |
Aged & Disabled (+): Added supported employment for a small group under the Developmentally Disabled waiver. (October 1, 2013)
Aged & Disabled (+): Increased long-term care home maintenance.
|
| 2015 |
Aged & Disabled (+): Enhancing behavioral health and substance use disorder services through the PROMISE Program. (July 1, 2014)
Aged & Disabled (+): Added 1915(i) supported employment services for individuals with disabilities (Pathways Program). (July 1, 2014)
|
|
| District of Columbia | 2014 | |
| 2015 |
All (+): Expanding transplant services. (October 1, 2014)
Aged & Disabled (+): Adding coverage for adult day homes under 1915(i). (October 1, 2014)
|
|
| Florida | 2014 |
Pregnant Women (+): Added coverage for flu vaccine. (December 19, 2013)
Pregnant Women (nc): Added smoking cessation counseling (ACA requirement). (Jan 2014)
|
| 2015 | ||
| Georgia | 2014 | |
| 2015 | Adults (+): Adding coverage for medically necessary emergency transportation by rotary wing air ambulance. (Effective date TBD) | |
| Hawaii | 2014 |
All (+): Added substance abuse services that are furnished by certified substance abuse Counselors. (October 1, 2013)
Adults (+): Adding specialized behavioral health services including supported employment, supportive housing, peer specialist and representative payee as part of Section 1115 waiver renewal. (October 1, 2013)
All (+): Added cognitive rehabilitation services and habilitation services. (October 1, 2013) |
| 2015 | ||
| Idaho | 2014 | All (nc): Added coverage for aspirin and tobacco cessation services to the state’s Benchmark Plans to comply with the Essential Health Benefit requirement. |
| 2015 | ||
| Illinois | 2014 | |
| 2015 |
Adults (+): Restoring coverage for adult dental services. (July 1, 2014)
Adults (+): Restoring coverage for adult podiatry services. (October 1, 2014)
|
|
| Indiana | 2014 | Aged & Disabled (nc): Implemented care coordination services for those with serious mental disease under a 1915(i) Behavioral and Primary Healthcare Coordination Program. (June 2014) |
| 2015 | Aged & Disabled (nc): Implementing case management services under 1915(i) for persons with End Stage Renal Disease with incomes up to 300% FPL. (October 1, 2014)Adults (Proposed): The state has submitted a waiver proposal, HIP 2.0, which would use the state’s existing HIP program as a platform for an alternative Medicaid expansion. As part of the waiver proposal expansion adults would be offered two ABPs: HIP Plus and HIP Basic.
|
|
| Iowa | 2014 | |
| 2015 | ||
| Kansas | 2014 | |
| 2015 | ||
| Kentucky | 2014 | All (+): Expanded mental health, substance abuse, chiropractic and private duty nursing services and related networks. (January 1, 2014) |
| 2015 | Aged & Disabled (nc): Modifying and adding new HCBS waiver services to better align member needs with services available and to comply with new HCBS federal requirements. | |
| Louisiana | 2014 | Children (+): Added coverage for Applied Behavioral Analysis services. |
| 2015 | ||
| Maine | 2014 | Non-Pregnant Adults (nc): Restoring coverage of smoking cessation products and services as required by the ACA. (January 1, 2014) |
| 2015 | ||
| Maryland | 2014 | |
| 2015 | All (+): Expanding telemedicine services. (October 1, 2014) | |
| Massachusetts | 2014 |
Adults (+): Added hospice for MassHealth Basic and Essential members. (July 2013)
Adults (+): Restored coverage of fillings for back teeth. (March 1, 2014)
Aged & Disabled (+): Added managed behavioral health to individuals in both MFP 1915(c) waivers. (July 1, 2013)
Aged & Disabled (+): Added Alzheimer’s and dementia coaching, medication dispensing system, home delivery of medications, occupational therapy in Frail Elder 1915(c) waiver.
|
| 2015 |
Adults (+): Adding coverage for treatment of gender dysphoria.
Adults (+): Plan to restore coverage for dentures. (May 15, 2015)
Aged & Disabled (+): Planning to add a shared living benefit to the TBI 1915(c) waiver. |
|
| Michigan | 2014 | |
| 2015 | ||
| Minnesota | 2014 |
Adults (+): Expanded adult dental services by adding house calls, oral/IV sedation, and behavior management. Also allowed additional prophylaxis. (July 1, 2013)
Children (+): Added coverage of therapeutic foster care and psycho-education. (July 2013)
|
| 2015 | All (+): Adding coverage for services provided by certified doulas. (July 1, 2014) | |
| Mississippi | 2014 | |
| 2015 | Aged & Disabled Children (+): Adding coverage for Prescribed Pediatric Extended Care Centers (a new provider type). (July 1, 2014) | |
| Missouri | 2014 | |
| 2015 | ||
| Montana | 2014 | |
| 2015 | ||
| Nebraska | 2014 | All (+): Added coverage for all tobacco cessation products. (January 1, 2014). |
| 2015 | ||
| Nevada | 2014 | Adult Non-Citizens (+): Added coverage for emergency ESRD services. (August 1, 2013) |
| 2015 | Aged & Disabled (+): Adding skilled nursing services in the 1915(c) waiver for individuals with intellectual disabilities. | |
| New Hampshire | 2014 | All (+): Eliminated 4 visit limit per state fiscal year on emergency room services. (Aug 2013) |
| 2015 | All (+): Removing service limits on psychotherapy, X-ray and outpatient hospital (to harmonize with Alternative Benefit Plan for the expansion population). | |
| New Jersey | 2014 | |
| 2015 | Aged & Disabled (+): Implementing managed long term services and supports and consolidating 1915(c) waivers into state’s Section 1115 which will provide LTSS beneficiaries with a greater array of LTSS services. (July 1, 2014) | |
| New Mexico | 2014 | All (+): Expanded behavioral health services. (January 1, 2014) |
| 2015 | ||
| New York | 2014 |
Pregnant women (+): Added lactation counseling coverage for those eligible. (April 2013)
All (+): Expanded coverage for hospital observation services. (April 1, 2013)
All (+): Expanded frequency of smoking cessation counseling coverage. (January 1, 2014
All (-): Limited coverage for percutaneous coronary intervention. (July 1, 2013)
All (-): Discontinued coverage for Functional Electrical Stimulators (FES) for Spinal Cord and Head Injury, Cerebral Palsy, and Upper Motor Neuron Disease. (November 1, 2013)
All (-): Discontinued coverage of lumbar discography for chronic low back pain. (November 1, 2013)
All (-): Limited coverage of Transcutaneous Electrical Nerve Stimulation for pain associated with knee osteoarthritis. (November 1, 2013)
All (-): Discontinued coverage of implantable Opioid infusion pumps, except in cases of intractable cancer pain. (November 1, 2013)
|
| 2015 |
All (-): Discontinued coverage for viscosupplementation of the knee for an enrollee with a diagnosis of osteoarthritis of the knee. (April 1, 2014)
All (+): Expanded smoking cessation counseling providers to include dental practitioners. (April 1, 2014 for FFS and July 1, 2014 for managed care)
|
|
| North Carolina | 2014 | |
| 2015 | ||
| North Dakota | 2014 | |
| 2015 | Aged & Disabled (+): Adding personal care with supervision to the Home and Community Based waiver to allow individuals with a primary diagnosis of dementia or traumatic brain injury to receive 24 hour supervision with a daily rate. (October 2014) | |
| Ohio | 2014 | Expansion Adults (nc): Removed hard limits on mental health services for ACA expansion group to comply with Mental Health Parity Act. (January 1, 2014) |
| 2015 | ||
| Oklahoma | 2014 | |
| 2015 | ||
| Oregon | 2014 | |
| 2015 | ||
| Pennsylvania | 2014 | |
| 2015 |
The following benefit changes were originally part of the state’s Healthy PA plan; after reaching a “conceptual agreement” with CMS that will be pursued through SPA:5
Adults (+): Add 1 more inpatient rehab hospital admission a year for high-risk MA group.
Adults (+): Increase limit on inpatient psychiatric hospital days for high-risk MA group.
Adults (-): Eliminate coverage of optometrist, podiatrist, and chiropractor services.
Adults (-): Reduce the number of total combined visits from 18 to 12 per year for those in the low-risk MA plan across the following types: routine adult visits, specialists visits, certified RN practitioner, FQHC/RHCs, clinics and hearing screenings.
Adults (-): Add limits to radiology and laboratory services.
Adults (-): Implement limits on outpatient surgery (SPU/ASC.)
Adults (-): Limit non-emergency inpatient hospital admissions and inpatient drug and alcohol admissions.
Adults (-): Increase visit limit for some outpatient mental health, substance abuse services.
Adults (-): Eliminate behavioral health targeted case management for low-risk MA group.
Adults (-): Limit some long-term care related services (e.g. skilled nursing facility, home health care visits and eliminate ICF/ID and ICF/ORC coverage) for low-risk MA group.
Adults (-): Limit medical supplies ($1000/year for low-risk and $2500/year for high-risk.) |
|
| Rhode Island | 2014 | |
| 2015 | ||
| South Carolina | 2014 | Adults (+): Reinstated the Adult Emergency Dental benefit (April 1, 2014) |
| 2015 |
Family Planning Adults (+): Adding coverage for additional preventive services including diabetes screening, health and behavioral assessments, cholesterol abnormalities screening, and HIV screening. (September 1, 2014)
Adults (+): Adding a preventative dental benefit with a maximum benefit of $750 per beneficiary per state fiscal year. (July 1, 2014)
|
|
| South Dakota | 2014 | |
| 2015 | ||
| Tennessee | 2014 | |
| 2015 | ||
| Texas | 2014 | MLTSS Adults (+): Added coverage of cognitive rehabilitation therapy services to the STAR+PLUS Program. (March 1, 2014) |
| 2015 |
MLTSS Adults (+): Adding supported employment and employment assistance to the HCBS waiver service array in the STAR+PLUS program. (September 1, 2014)
Aged & Disabled (nc): Will allow providers other than Local Mental Health Authorities (LMHAs) to provide Mental Health Targeted Case Management and Mental Health Rehabilitative services already available through STAR Health. (September 1, 2014)
|
|
| Utah | 2014 | |
| 2015 | ||
| Vermont | 2014 |
Non-Pregnant Adults (+): Increased dental cap from $495 to $510. (January 1, 2014)
All (+): Added coverage for face to face tobacco cessation counseling services to all eligible non-pregnant Medicaid beneficiaries. (January 1, 2014)
|
| 2015 |
All (+): Adding a tele-monitoring benefit. (August 1, 2014)
Disabled Children (+): Adding coverage for applied behavioral analysis. (Effective date TBD)
|
|
| Virginia | 2014 |
LTC Adults (-): Limited dental utilization in LTC settings by modifying allowable deductions for dental expenses. (July 1, 2013)
Aged & Disabled (+): Added nutrition counseling and inpatient substance abuse services for Medicaid Works (working disabled eligibility group). (January 1, 2014)
|
| 2015 | Pregnant Women (+): Plan to expand comprehensive dental benefits. | |
| Washington | 2014 |
Adults (+): Restored adult dental coverage. (January 1, 2014)
All (+): Eliminated limits on mental health services and added screening, brief intervention and referral treatment (SBIRT) benefit. (January 1, 2014)
Adults (+): Expanded list of qualified mental health providers (already in place for children). (January 1, 2014)
Adults age 60+ (+): Added coverage for shingles vaccination. (January 1, 2014)
All (+): Added coverage of services provided by naturopath providers. (January 1, 2014)
Pregnant Women (nc): Expanded coverage for smoking cessation services (ACA required for pregnant women). (July 1, 2013)
Expansion Adults (nc): Habilitation added for expansion group only. (January 1, 2014)
|
| 2015 | ||
| West Virginia | 2014 | Children and AFDC-related Adults (-): Eliminated the Mountain Health Choices Basic and Enhanced benchmark benefit plans resulting in the elimination of coverage for weight management services. (December 31, 2013) |
| 2015 | ||
| Wisconsin | 2014 | |
| 2015 | Aged & Disabled (+): Adding the following HCBS waiver services for persons meeting nursing facility level of care: Peer Recovery Support Services, Consultative Clinical and Therapeutic Services for Caregivers, and Training Services for Unpaid Caregivers. (January 1, 2015) | |
| Wyoming | 2014 | |
| 2015 | ||