Medicaid Work Requirements are Back on the Agenda
The Trump Administration aimed to reshape the Medicaid program by newly approving Section 1115 waivers that included work and reporting requirements as a condition of Medicaid eligibility. However, courts struck down many of these requirements and the Biden Administration withdrew these provisions in all states that had approvals. After these withdrawals, in April 2022 the Supreme Court dismissed pending appeals in cases that had found work requirement approvals unlawful. However, these provisions remain in place in Georgia, as a Federal District Court judge vacated the Administration’s rescission of work and premium requirements in the Georgia Pathways waiver. Additionally, other states have indicated they may pursue work requirement waivers in the future, and some Congressional Republicans have recently discussed a federal Medicaid work requirement. This Waiver Watch summarizes the recent history of work requirements, the current status of Georgia’s waiver, and key state and federal issues to watch.
What is the recent history and current status of work requirements in Medicaid?
In a departure from previous administrations, the Trump Administration approved Section 1115 waivers that conditioned Medicaid coverage on meeting work and reporting requirements, but the Biden Administration withdrew these approvals. Thirteen waivers with work requirements had been approved during the Trump administration. Following the Biden Administration’s withdrawals, in April 2022 the Supreme Court dismissed pending appeals in cases that had found work requirement approvals unlawful. The Supreme Court’s dismissal does not preclude future presidential administrations from approving new Section 1115 work requirements. To survive an expected legal challenge, the administrative record in any future approvals would likely have to support the conclusion that such waivers would further Medicaid program objectives.
As most Medicaid enrollees are already working or face barriers to work, work and reporting requirements may result in coverage loss among eligible enrollees without increasing employment. Prior to the pandemic, the majority (63%) of non-elderly adult Medicaid enrollees who did not qualify based on a disability were already working full- or part-time. Most who were not working would likely meet exemptions from work requirement policies (e.g., had an illness or disability or were attending school), leaving just 7% of these enrollees to whom work requirement policies could be directed. Although few Medicaid work and reporting requirements were ultimately implemented due to litigation, state withdrawals, and/or pauses during the COVID-19 pandemic, available implementation data from Arkansas suggests that these requirements were confusing to enrollees and result in substantial coverage loss, including among eligible individuals.
What is the status of Georgia’s waiver?
Although CMS withdrew the work and premium requirement components of Georgia’s waiver, these provisions remain in place after a federal judge vacated the CMS rescission. In December 2021, CMS rescinded work requirement and premium authorities that the Trump Administration had approved as part of a limited coverage expansion in Georgia’s waiver—an action that the state subsequently challenged in court. In August 2022, a Federal District Court judge issued a decision in favor of the state, vacating CMS’s rescission thus reinstating these provisions. Although CMS generally reserves the right to withdraw waiver authorities at any time, the judge found that its rescission of Georgia’s waiver provisions was arbitrary and capricious due to agency errors, including that it failed to weigh that the waiver would have increased Medicaid coverage. CMS did not appeal this decision. Georgia Governor Brian Kemp allocated $52 million in his proposed state fiscal year (FY) 2024 budget to implement the Georgia Pathways program beginning July 1, 2023.
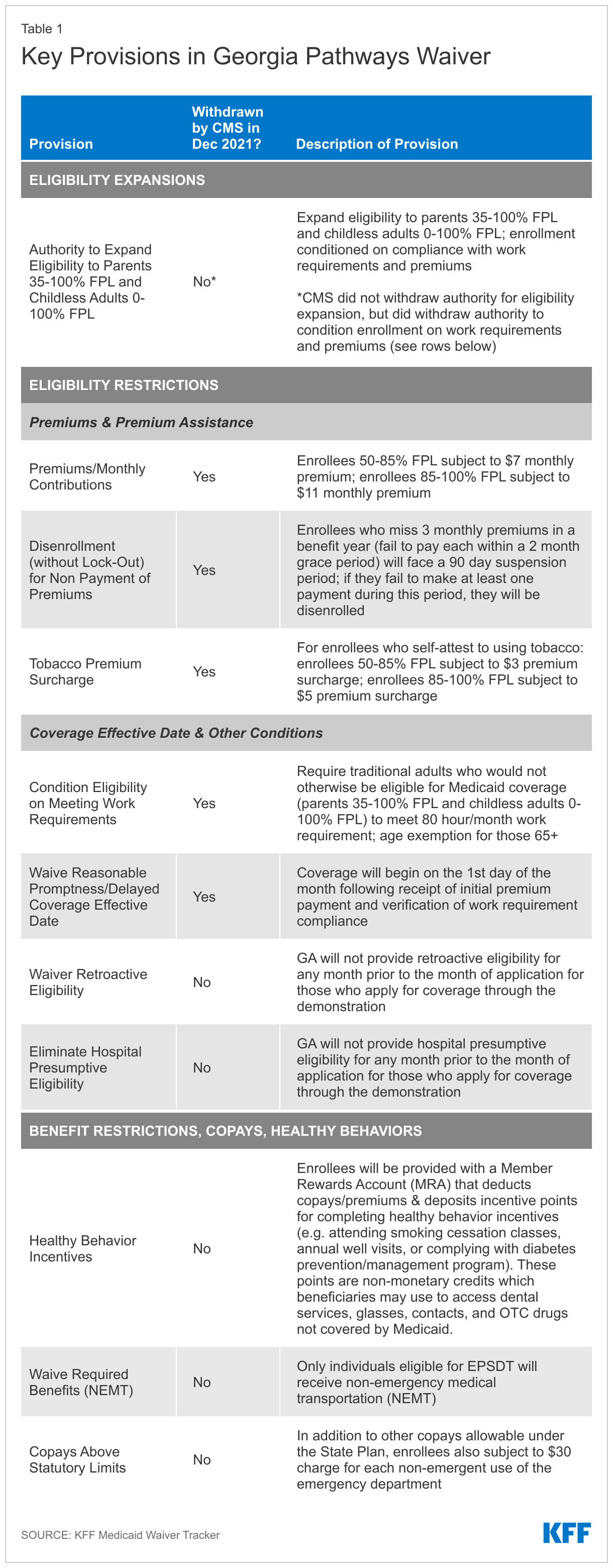
Once implemented, Georgia’s waiver will expand eligibility to 100% of the federal poverty level (FPL), with initial and continued enrollment conditioned on meeting work and premium requirements. These and other provisions of the Georgia Pathways waiver, including additional eligibility and benefit restrictions, are summarized in more detail in Table 1. The work requirement would apply to enrollees below age 65, with “good cause exceptions” (for those who cannot fulfill the requirement in a given month due to a circumstance such as a family emergency) and “reasonable accommodations” (to enable individuals with disabilities to meet the requirement) available. The state originally estimated that the Georgia Pathways waiver would provide coverage to about 64,000 individuals—significantly less than the estimated 269,000 uninsured individuals in the Medicaid coverage gap (parents with incomes that exceed Medicaid eligibility levels but are below the FPL, plus childless adults with incomes below the FPL) who could be covered if Georgia adopted the ACA Medicaid expansion.
What are key issues to watch?
Looking ahead, key questions to watch will play out at the state and federal levels:
- How will implementation of the Georgia waiver go? It remains to be seen exactly how many currently uninsured individuals under 100% FPL will meet the work (as well as premium) requirements necessary to enroll in the new coverage program. Looking ahead, Section 1115 monitoring and evaluation requirements will require Georgia to track and report the number of enrollees who gain and maintain coverage.
- Will other states pursue work requirements? Several other states have indicated they may pursue work requirements, but unlike Georgia, these states have already adopted Medicaid expansion and would not be adding new coverage. In February 2023, Arkansas Governor Sarah Huckabee Sanders directed the state to submit a new work requirement waiver request with a proposed effective date of January 2024. In both Iowa and West Virginia (two states that did not previously pursue work requirement waivers), proposed state legislation would direct each state to seek waivers that include work requirements and to resubmit such requests periodically until approval. Finally, in March 2023, North Carolina Governor Roy Cooper signed a law that would direct the state to expand Medicaid (contingent on appropriations in the biennial budget), and to seek approval to apply a work requirement to this population if there is ever any indication that the federal government would approve such a waiver. Because these states all propose applying a work requirement to an existing Medicaid population rather than to a new coverage group as in Georgia, it is unclear if the rationale that the Federal District Court ruling used in Georgia would apply. While the Biden Administration does not believe work requirements further Medicaid objectives, a future presidential administration could revisit these waiver provisions. However, any future work requirements approved would likely face legal challenges.
- Will there be debate over federal legislation related to Medicaid work requirements? Ahead of federal budget debates, Congressional Republicans have indicated that they will rely on a budget outline that would require Medicaid enrollees to work, or look for work, in order to receive coverage (in addition to other Medicaid programmatic cuts); recently, Republican Speaker of the House Kevin McCarthy highlighted work requirements as a policy to reduce the debt limit. Previously, Republican attempts in 2017 to allow states to require work as a condition of Medicaid eligibility (as part of the ACA repeal and replace debate) were unsuccessful. While some policymakers favor work requirements as a policy, they are unlikely to result in significant savings or result in large increases in enrollee employment rates, since the vast majority of Medicaid enrollees are already working or would likely qualify for exemptions.