Traditional Medicare Spending Fell Almost 6% in 2020 as Service Use Declined Early in the COVID-19 Pandemic
In 2020, spending for traditional Medicare beneficiaries declined for the first time in more than two decades. The drop in spending followed the sharp decline in the use of health care services during the initial months of the COVID-19 pandemic, and reflects a decrease in spending among traditional Medicare beneficiaries on most health care goods and services. The lower spending in traditional Medicare contributed to the relatively slower growth in Medicare spending overall in 2020. However, total Medicare spending increased in 2020 because federal payments per Medicare Advantage enrollee rose 6.9%. Medicare Advantage payments were determined in mid-2019 prior to the pandemic, and therefore, did not reflect the lower utilization that occurred in 2020.
This analysis uses recently released data from the Centers for Medicare & Medicaid Services (CMS) to examine trends in spending and utilization by type of health care service between 2010 and 2020 for Medicare beneficiaries who were enrolled in both Part A and Part B of traditional Medicare. (Similar data for beneficiaries enrolled in Medicare Advantage or for prescription drug spending are not available.) The data include both Medicare and beneficiary out-of-pocket spending on Part A and Part B covered services, but not Part D prescription drug spending. Understanding how spending and utilization changed across different types of services in 2020 is useful for identifying areas where beneficiaries delayed or skipped care in response to the pandemic, which could have longer-term implications for health outcomes and Medicare spending.
We find that Medicare spending declined across most, but not all, types of services, as a smaller share of beneficiaries used most types of Medicare-covered health care services in 2020 compared to 2019. Specifically:
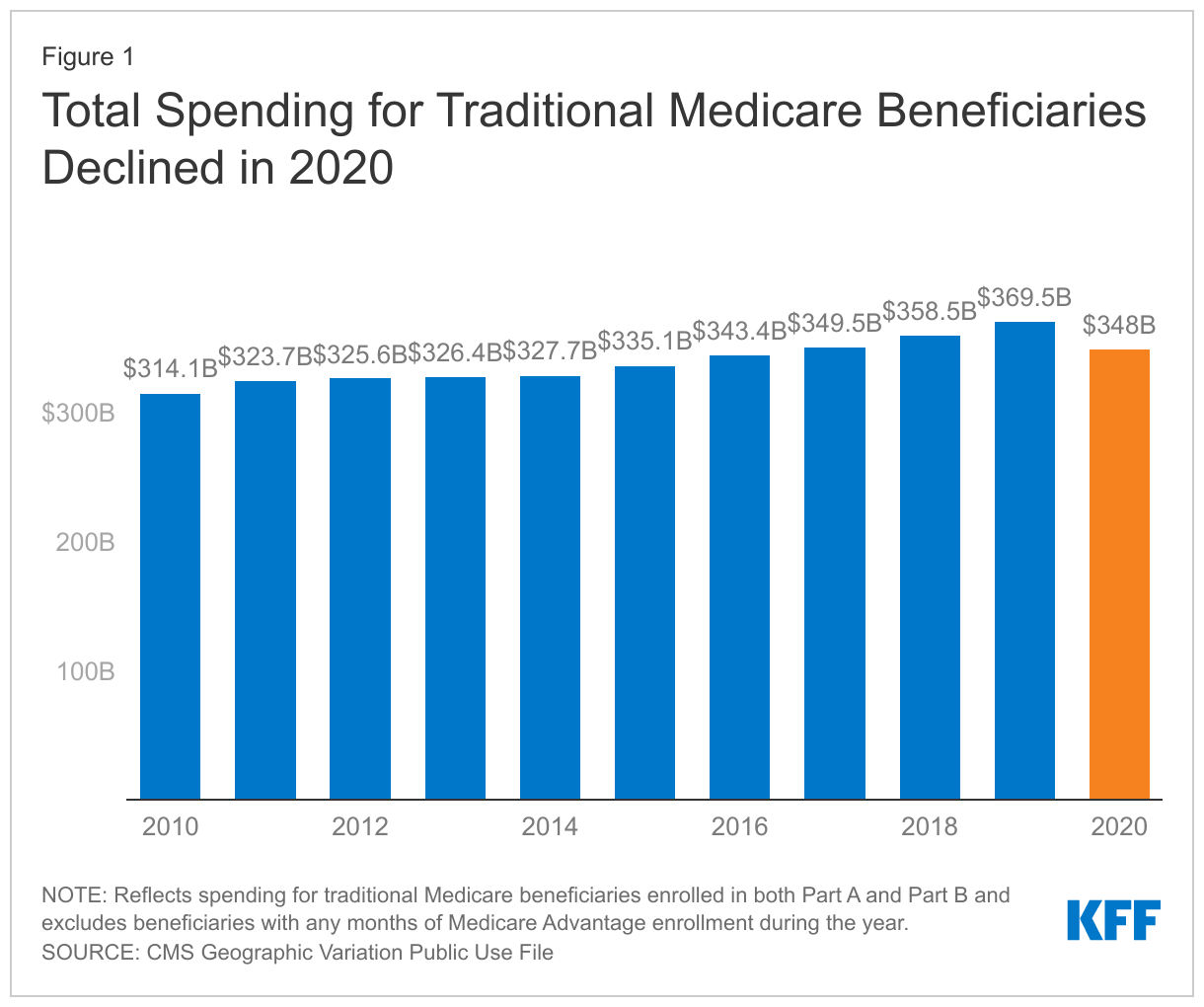
- Total spending on Part A and Part B services for traditional Medicare beneficiaries was $348.0 billion in 2020, a decrease of 5.8% ($21.4 billion) from 2019.
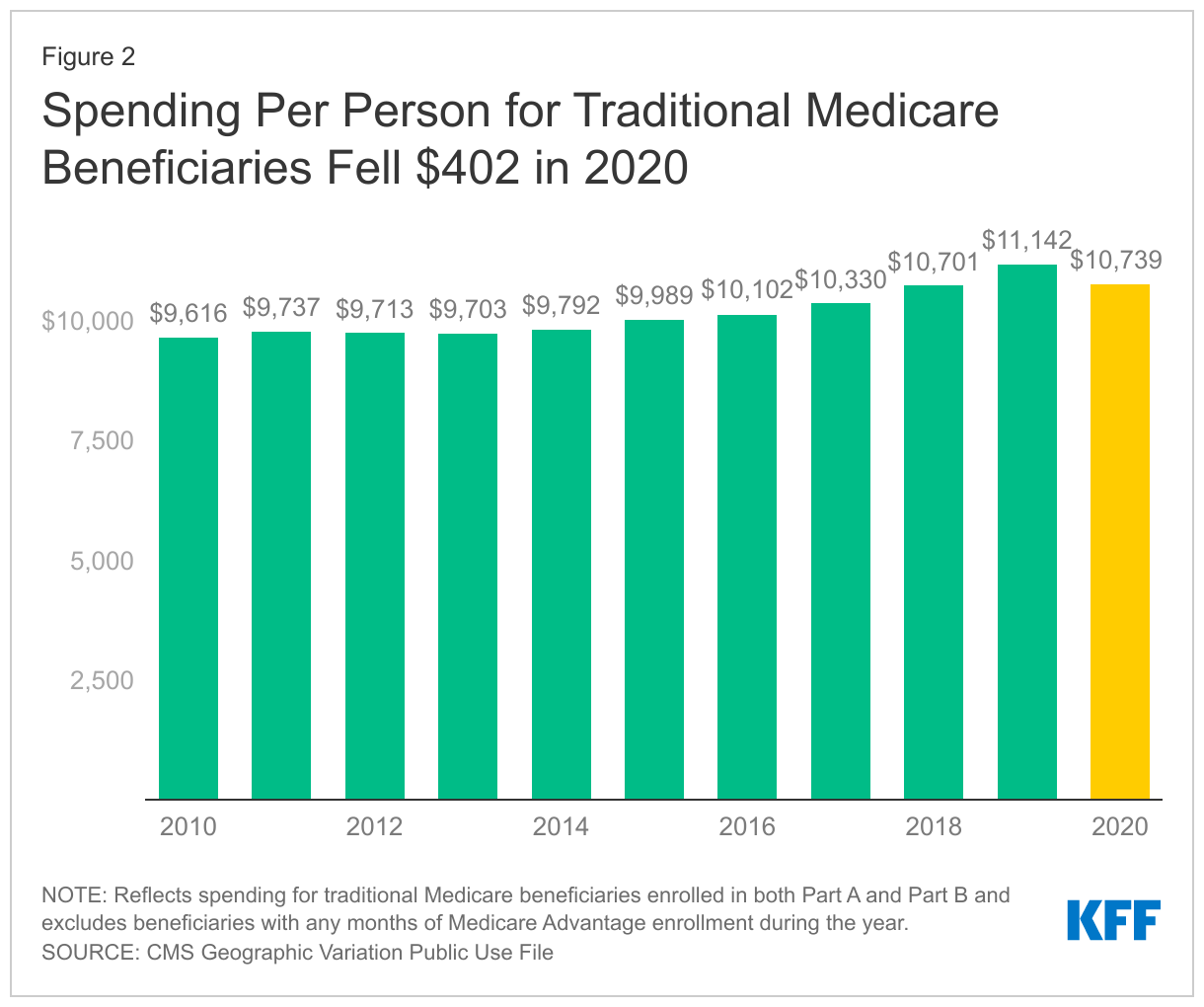
- Spending per traditional Medicare beneficiary for Part A and Part B services fell 3.6%, or $402, to $10,739 per person in 2020, compared to $11,142 per person in 2019.
- The decline in traditional Medicare spending reflects decreases in spending for most types of services, ranging from 0.1% less for durable medical equipment to 13.1% less for procedures, compared to 2019. Only spending on skilled nursing facilities, Part B drugs, and hospice increased in 2020
- Use of nearly all types of services by traditional Medicare beneficiaries was lower in 2020 compared to 2019. Only three types of services had increases across all measures of utilization: hospice, dialysis, and Part B drugs. Skilled nursing facilities had lower use but higher spending (see KFF analysis, Amid the COVID-19 Pandemic, Medicare Spending on Skilled Nursing Facilities Increased More than 4% Despite an Overall Decline in Utilization).
- Among traditional Medicare beneficiaries, average spending per user increased for 12 of the 17 types of services examined.
Findings
Spending
total Spending fell 5.8%, or $21.4 billion, for traditional medicare beneficiaries in 2020
Total spending for traditional Medicare beneficiaries was $348.0 billion. That is $21.4 billion, or 5.8%, lower than in 2019 and represents the only year-over-year decline since 2010 (Figure 1).
Traditional medicare spending per person was 3.6%, OR $402, lower in 2020 than 2019
The decline in total spending for traditional Medicare beneficiaries was driven by a decrease in spending per person, which fell 3.6%, or $402, in 2020 compared 2019 ($10,739 vs. $11,142) (Figure 2). Although spending per person also declined in 2012 and 2014, the decrease in those years was relatively small ( -0.2% in 2012 and -0.1% in 2014). In addition, there was a small drop in the number of beneficiaries enrolled in traditional Medicare in 2020 (data not shown), continuing a trend of declining enrollment in traditional Medicare as the share of Medicare beneficiaries opting for Medicare Advantage has grown.
Traditional medicare spending fell across most types of services in 2020
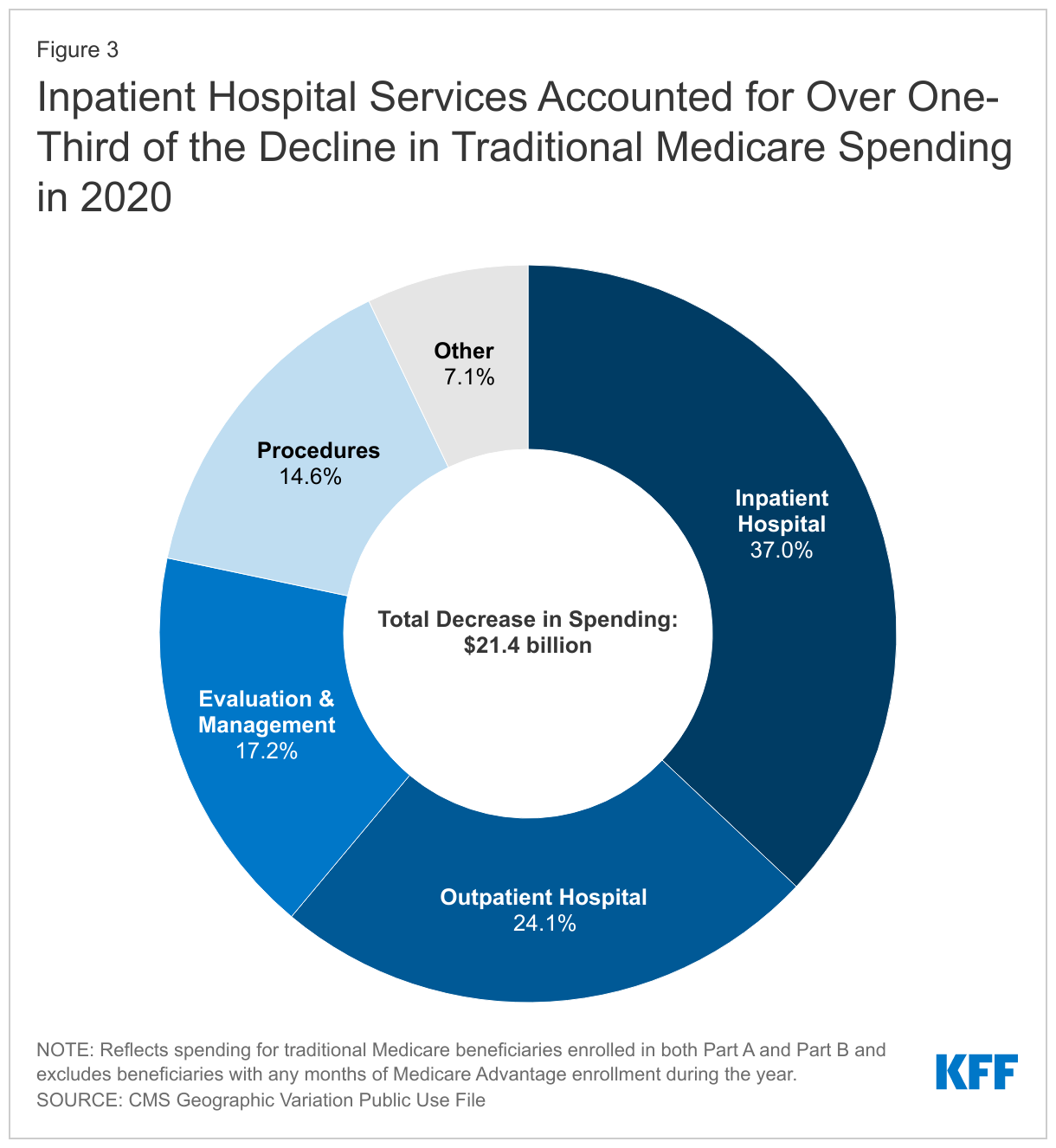
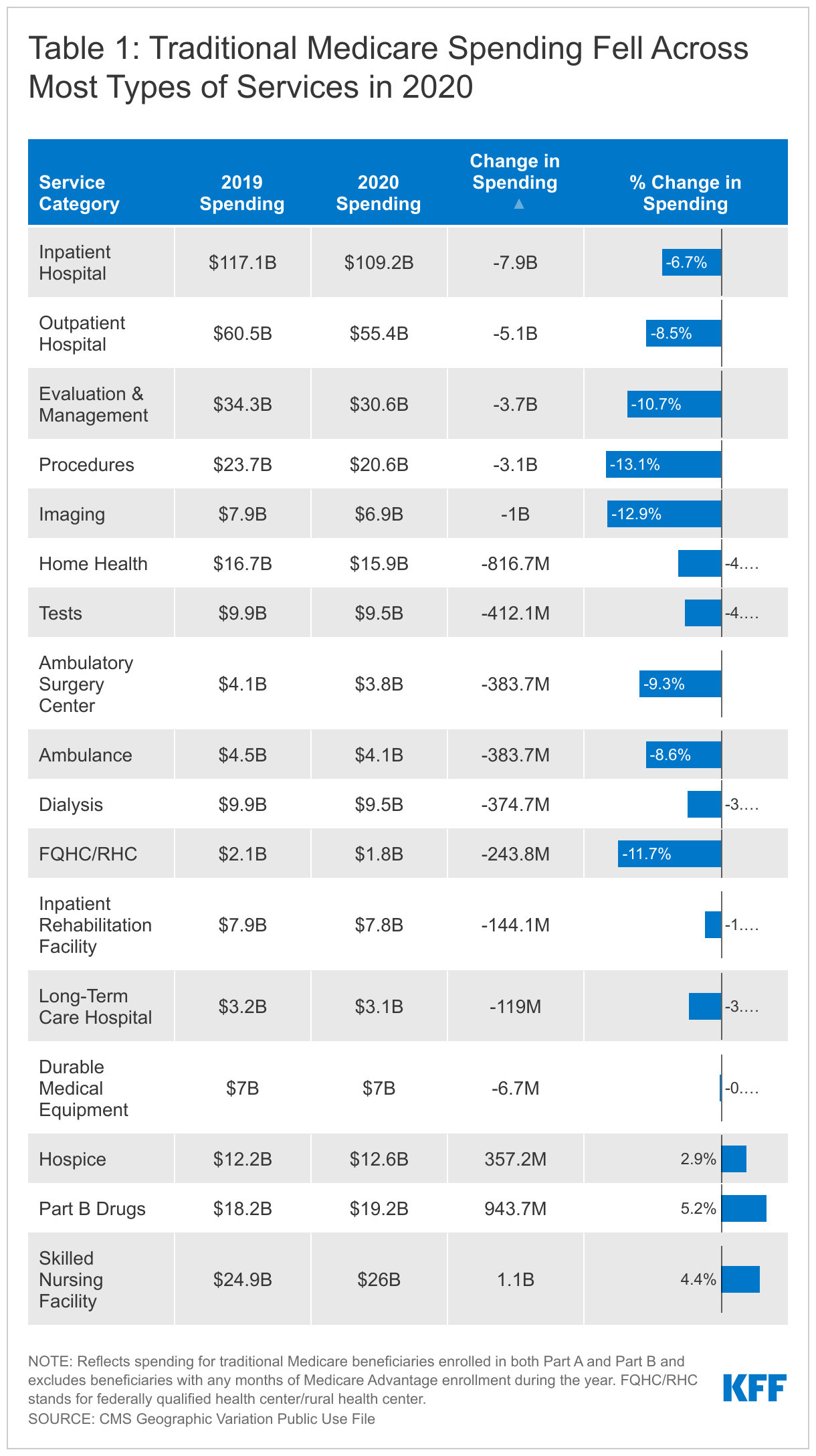
The decrease in Medicare spending reflects a decline in spending for almost all types of Medicare-covered services between 2019 and 2020. The largest declines in dollar terms were for the largest categories of spending: inpatient hospital spending fell $7.9 billion (from $117.1 billion to $109.2 billion, 37.0% of total), outpatient hospital spending fell $5.1 billion (from $60.5 billion to $55.4 billion, 24.1% of total) and evaluation & management (office visit) spending fell $3.7 billion (from $34.3 billion to $30.6 billion, 17.2% of total) (Figure 3 and Table 1).
As a percent of 2019 spending for the respective service categories, spending on procedures declined the most, falling 13.1% (from $23.7 billion to $20.6 billion), followed by spending on imaging (-12.9%, from $7.9 billion to $6.9 billion) and spending on Federally Qualified Health Centers/Rural Health Centers (-11.7%, from $2.1 billion to $1.8 billion). In contrast, spending increased for skilled nursing facilities, Part B drugs and hospice (Table 1).
Utilization
Use of nearly all types of services fell between 2019 and 2020
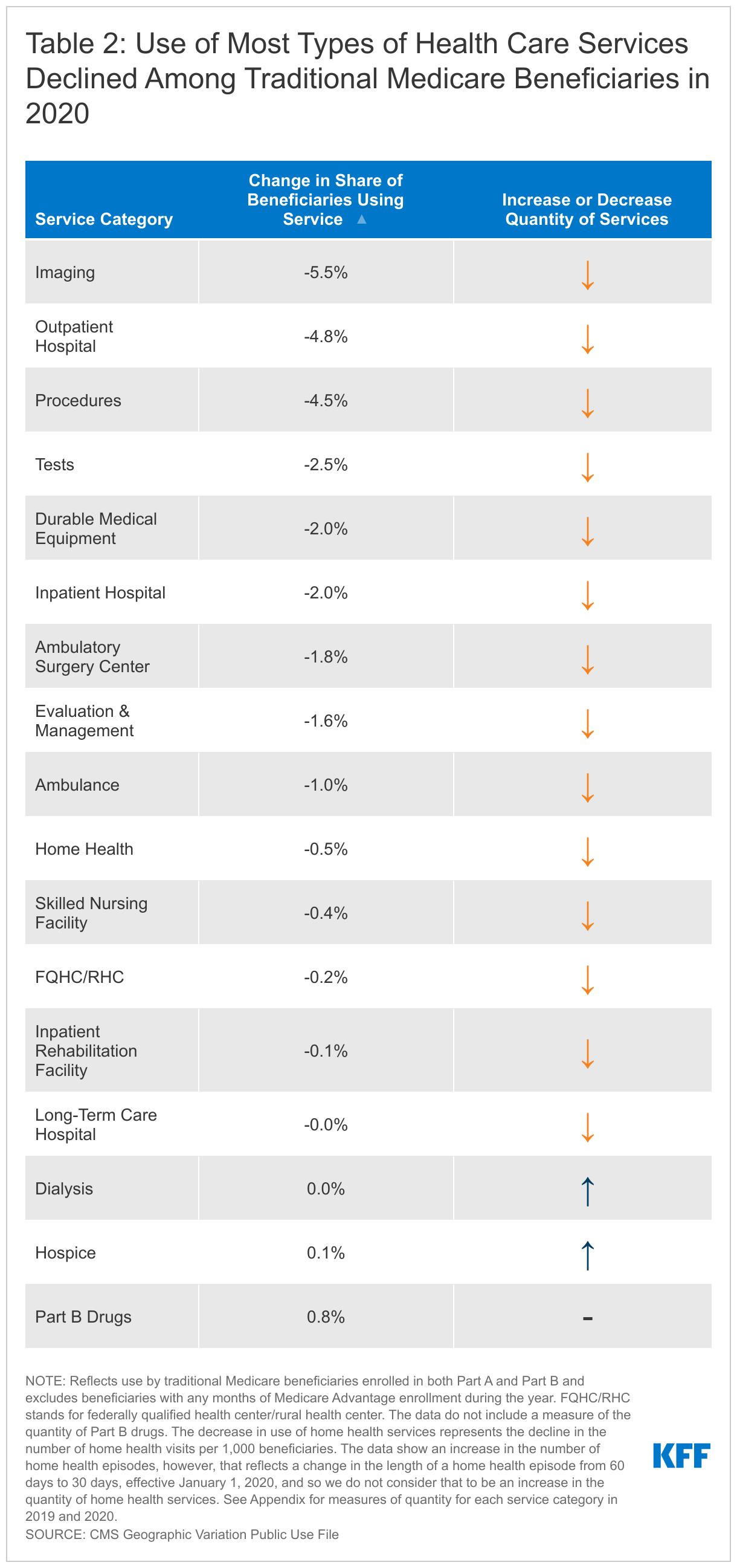
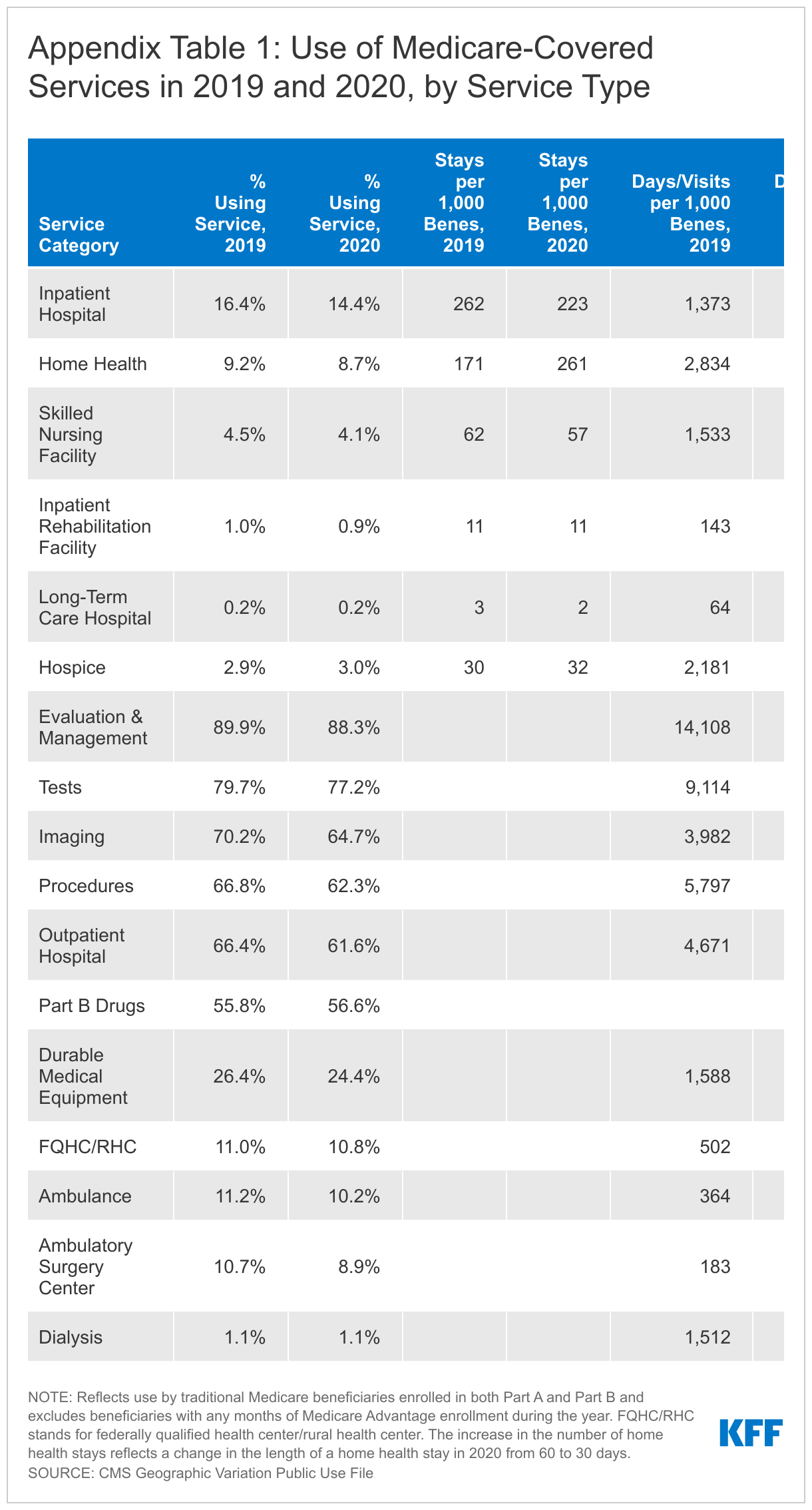
The share of traditional Medicare beneficiaries using specific types of services fell across most categories and was generally accompanied by a decline in the total number of services provided (Table 2). For example, the largest drop in the share of traditional Medicare beneficiaries using a particular type of service was for imaging services, which was 5.5 percentage points lower in 2020 compared to 2019 (64.7% vs 70.2%). Consistent with this decline, traditional Medicare beneficiaries had 574 fewer imaging events per 1,000 beneficiaries in 2020 than in 2019. Outpatient hospital services had the next largest drop in the share of beneficiaries using the service, declining 4.8 percentage points in 2020 compared to 2019 (from 66.4% to 61.6%). There was a corresponding decrease in the number of outpatient hospital visits, which declined by 702 visits per 1,000 beneficiaries in 2020 compared to 2019. See Appendix table for complete 2019 and 2020 utilization data by service category.
use increased for hospice, dialysis and part b drugs
While use of Medicare-covered services generally declined, the share of beneficiaries using hospice, dialysis and Part B drugs increased very modestly, by less than 1 percentage point, between 2019 and 2020. There was also an increase in the number of hospice stays (+2 stays per 1,000 beneficiaries) and days (+58 days per 1,000 beneficiaries) and the number of dialysis visits (+9 visits per 1,000 beneficiaries) in 2020 compared to 2019 (see Appendix). (The data do not include the number of times beneficiaries used Part B drugs because of reported difficulty in constructing a standardized measure.)
Spending Per User
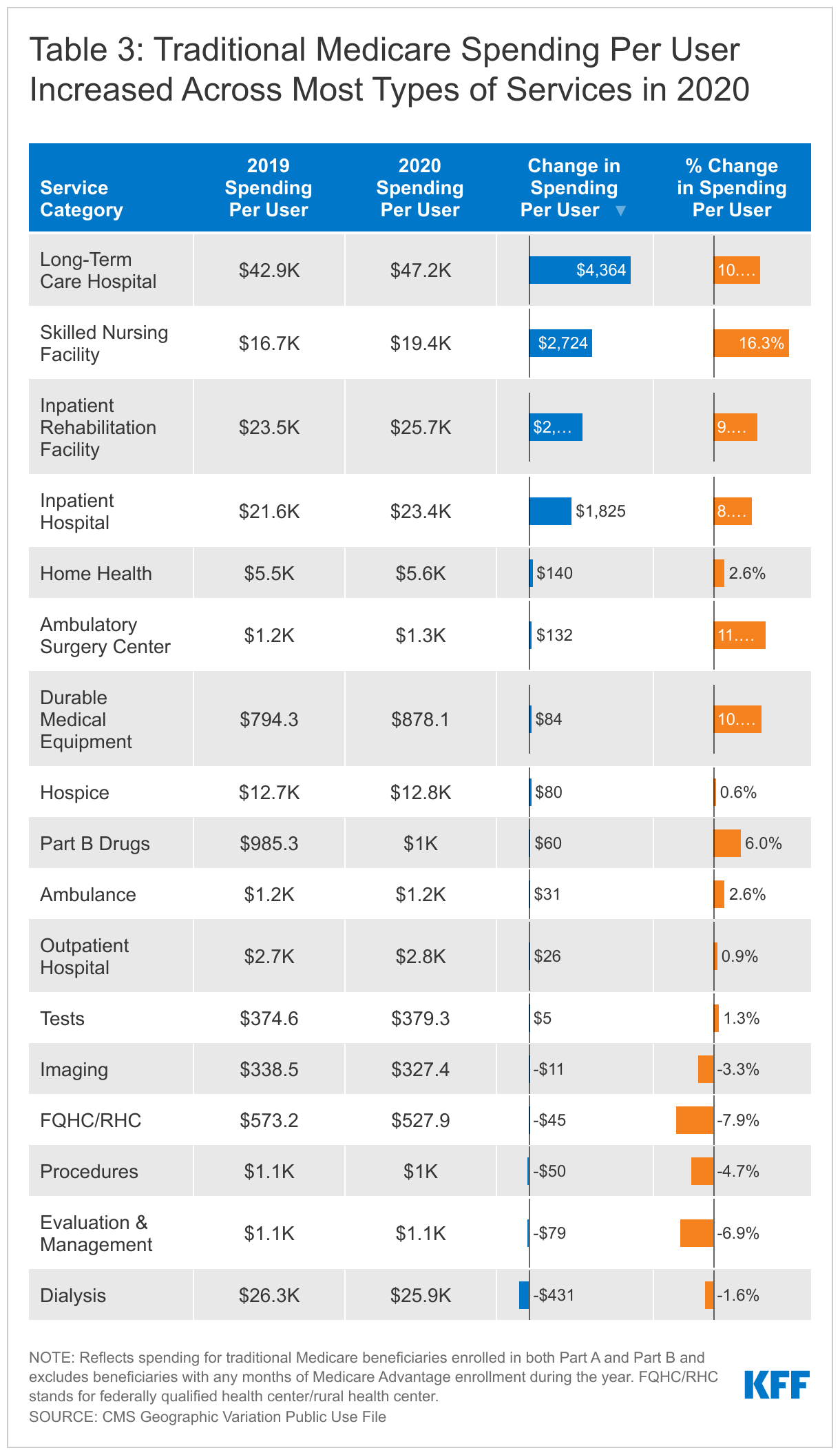
spending per user increased Across 12 of the 17 service categories
While both spending and utilization declined across most types of services between 2019 and 2020, average spending per user increased for 12 of the 17 categories. In dollar terms, the largest increases were for long-term care hospitals (+$4,364, 10.2%), skilled nursing facilities (+$2,724, 16.3%), inpatient rehabilitation facilities (+$2,269, 9.7%), and inpatient hospital (+$1,825, 8.5%). These increases indicate that the beneficiaries who used inpatient hospital and post-acute care services in 2020 required more intensive, and therefore costly, care than beneficiaries who used these services in 2019. The largest decrease per user was for dialysis (-$431, -1.6%), which also saw an increase in the number of users and number of visits, suggesting that all else equal, the new use was relatively lower cost.
Discussion
Total spending among the 32 million traditional Medicare beneficiaries with both Part A and Part B fell in 2020, the first year of the COVID-19 pandemic, corresponding to lower service use across most types of Medicare-covered health care services compared to 2019. The lower spending in traditional Medicare contributed to the relatively slower growth in Medicare spending overall in 2020. However, because spending on Medicare Advantage continued to grow, total Medicare spending rose slightly in 2020. Payments to Medicare Advantage plans are determined prior to the plan benefit year (in mid-2019 for 2020) and so did not incorporate the effects of the pandemic on health care utilization, though plans have historically been paid more per enrollee, on average, than similar beneficiaries would have cost in traditional Medicare. Consistent with higher payments and lower utilization, Medicare Advantage plans had higher gross margins and lower medical loss ratios, on average, in 2020 compared to 2019, suggesting that they became more profitable during the pandemic. Enrollment in Medicare Advantage has grown rapidly over the last decade, reaching nearly 40% of all Medicare beneficiaries in 2020, and is projected to exceed 50 percent of total Medicare population by 2025. That growth in enrollment, and the higher growth in spending per Medicare Advantage enrollee compared to traditional Medicare, has contributed to Medicare Advantage accounting for an increasing share of Medicare spending, and contributed to increases in total Medicare spending.
It is not yet known the extent to which the decline in use across most types of health care services may have affected health outcomes of traditional Medicare beneficiaries. The Medicare population is at risk of having negative effects from delaying or forgoing care because they have relatively high health needs. More than one-fifth of Medicare beneficiaries have five or more chronic conditions and almost one-third have at least one functional impairment. It is possible that the decline in use could have negative implications for future health if people delayed routine care and screenings or were unable to schedule procedures in a timely manner, missing the opportunity for early diagnosis and treatment. The drop in utilization also has the potential to lead to higher future health care spending if more health care services are required or if treatments are more intensive. In addition, Medicare beneficiaries were hit hard by COVID-19, with people age 65 and older accounting for a disproportionate share of cases and deaths. While the long-term effects of COVID-19 are not yet known, they are likely to have a greater impact on people ages 65 and older, including corresponding health care use and Medicare spending.
While use of health care services declined sharply in 2020, that did not necessarily translate into a loss of revenue for most providers because of policies adopted by Congress, states, and both the Trump and Biden Administrations. For example, Congress established the Provider Relief Fund, which authorized $178 billion in funding, nearly all of which has been disbursed, to compensate providers for lost revenue and unexpected costs due to the pandemic.
The decline in spending for traditional Medicare beneficiaries in 2020 represents the first decrease in spending since 1999. The previous decline was primarily a result of changes to Medicare provider payments enacted as part of the Balanced Budget Act of 1997. In contrast, the decrease in 2020 was driven by lower use of health care services amid the COVID-19 pandemic. There is a question of whether any of the changes in spending and use will be sustained, though the expectation is that these were most likely one-time, or otherwise short-lived, changes. While actual data for 2021 is not yet available, Medicare spending is projected to have rebounded and is expected to continue to grow in coming years.
This work was supported in part by Arnold Ventures. We value our funders. KFF maintains full editorial control over all of its policy analysis, polling, and journalism activities.