Amid the COVID-19 Pandemic, Medicare Spending on Skilled Nursing Facilities Increased More than 4% Despite an Overall Decline in Utilization
The use of health care services declined sharply in the early months of the COVID-19 pandemic, as people delayed or skipped care, before rebounding in the latter part of 2020. While total spending for beneficiaries in traditional Medicare dipped in 2020 for the first time since 1999, spending did not decline across all types of services. As described in a separate KFF analysis, Medicare spending increased in 2020 for skilled nursing facilities (SNFs), Part B drugs and hospice. The largest increase in total spending was for SNFs and occurred despite a decline in utilization.
Skilled nursing facilities provide short-term rehabilitation services, usually following discharge from an acute care hospital. Medicare pays SNFs a predetermined amount per day that a beneficiary receives care, which varies based on the day of the stay and the person’s needs, as well as geographic differences in wages. Certain high-cost ancillary services are paid separately. For the first 20 days, beneficiaries do not pay any cost sharing; for days 21-100, there is a daily copayment (equal to $194.50 in 2022). The SNF payment system was modified, effective October 2019, and changes were expected to result in higher payments for patients complex medical needs.
Prior to the pandemic, traditional Medicare beneficiaries were generally required to have a hospital stay of at least three days to qualify for SNF care, and benefits were limited to 100 days. During the COVID-19 public health emergency, CMS has waived the three-day requirement, allowing beneficiaries to be admitted to a SNF directly from the community or following a shorter hospital stay, and has allowed beneficiaries with COVID-19 to extend their benefit for an additional 100 days. While these policies alone would be expected to increase SNF utilization, early reports of deaths attributable to COVID-19 and ongoing concerns about transmission of COVID-19 in SNFs and other long-term care facilities appear to have contributed to a drop in SNF admissions.
This analysis uses recently released Medicare spending data from the Centers for Medicare & Medicaid Services (CMS) for the 32 million beneficiaries enrolled in both Part A and Part B of traditional Medicare to examine the change in Medicare SNF spending and utilization between 2019 and 2020 (see Methods for details). We find:
- Total Medicare SNF spending increased $1.1 billion (4.4%) between 2019 and 2020, despite 200,000 fewer traditional Medicare beneficiaries using SNF services in 2020.
- Average spending per SNF user was $2,724 (16.3%) higher in 2020 compared to 2019, driven by an increase in average spending per day (+$44), with an increase in the average length of stay (+1.6 days) also contributing.
- Medicare beneficiaries under the age of 65 accounted for a disproportionately large share of the increase in total Medicare SNF spending between 2019 and 2020.
Findings
total Skilled nursing facility spending rose 4.4% in 2020, while spending on Most other services declined
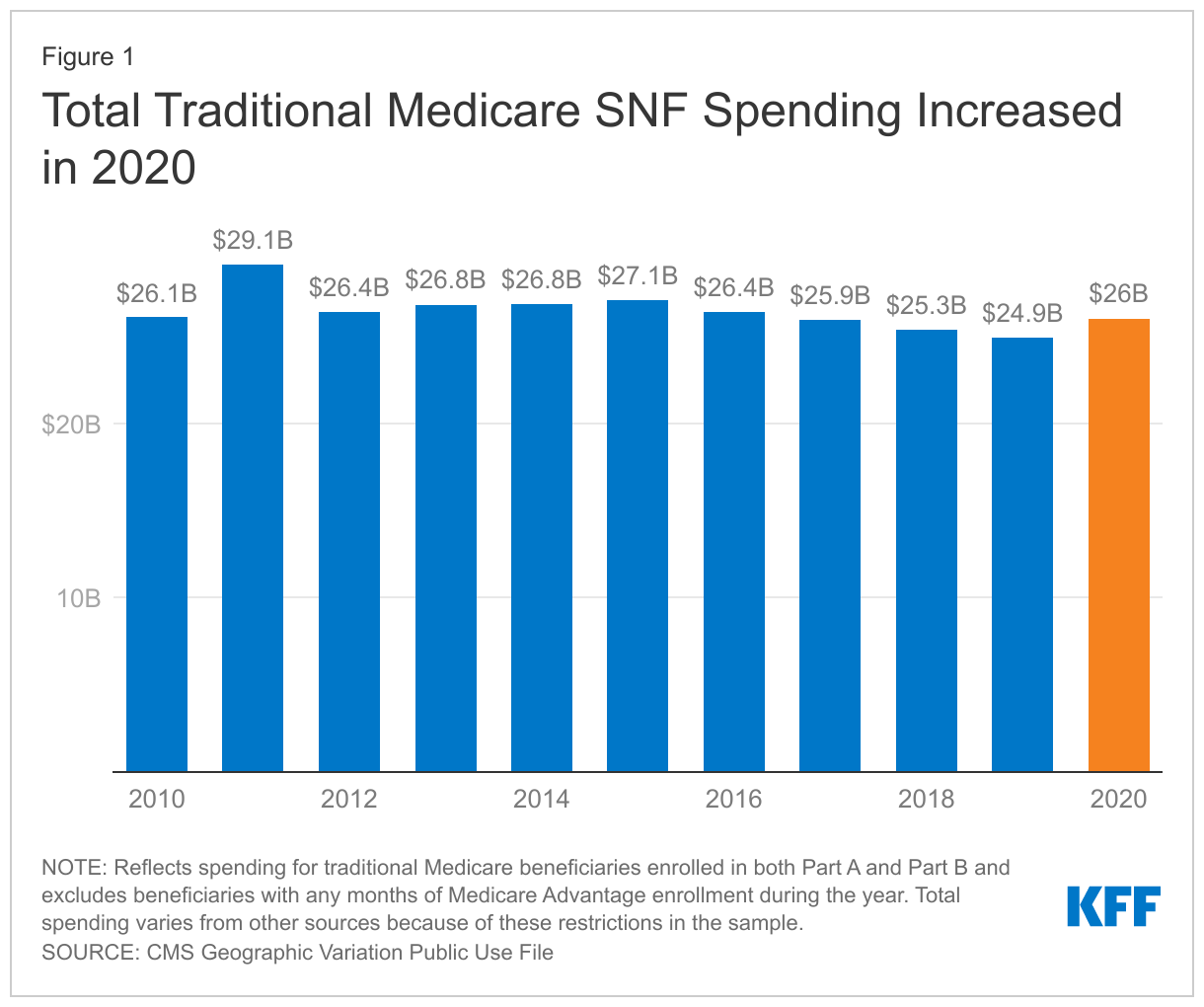
Total spending for traditional Medicare beneficiaries for SNF services was $1.1 billion (4.4%) higher in 2020 than in 2019 – increasing from $24.9 billion to $26.0 billion. The increase is notable because spending on most other types of services declined and because it follows several years of gradually declining spending on SNF services after the implementation of productivity adjustments included in the Affordable Care Act (Figure 1).
The number of Traditional Medicare beneficiaries using SNF Services continued to decline in 2020
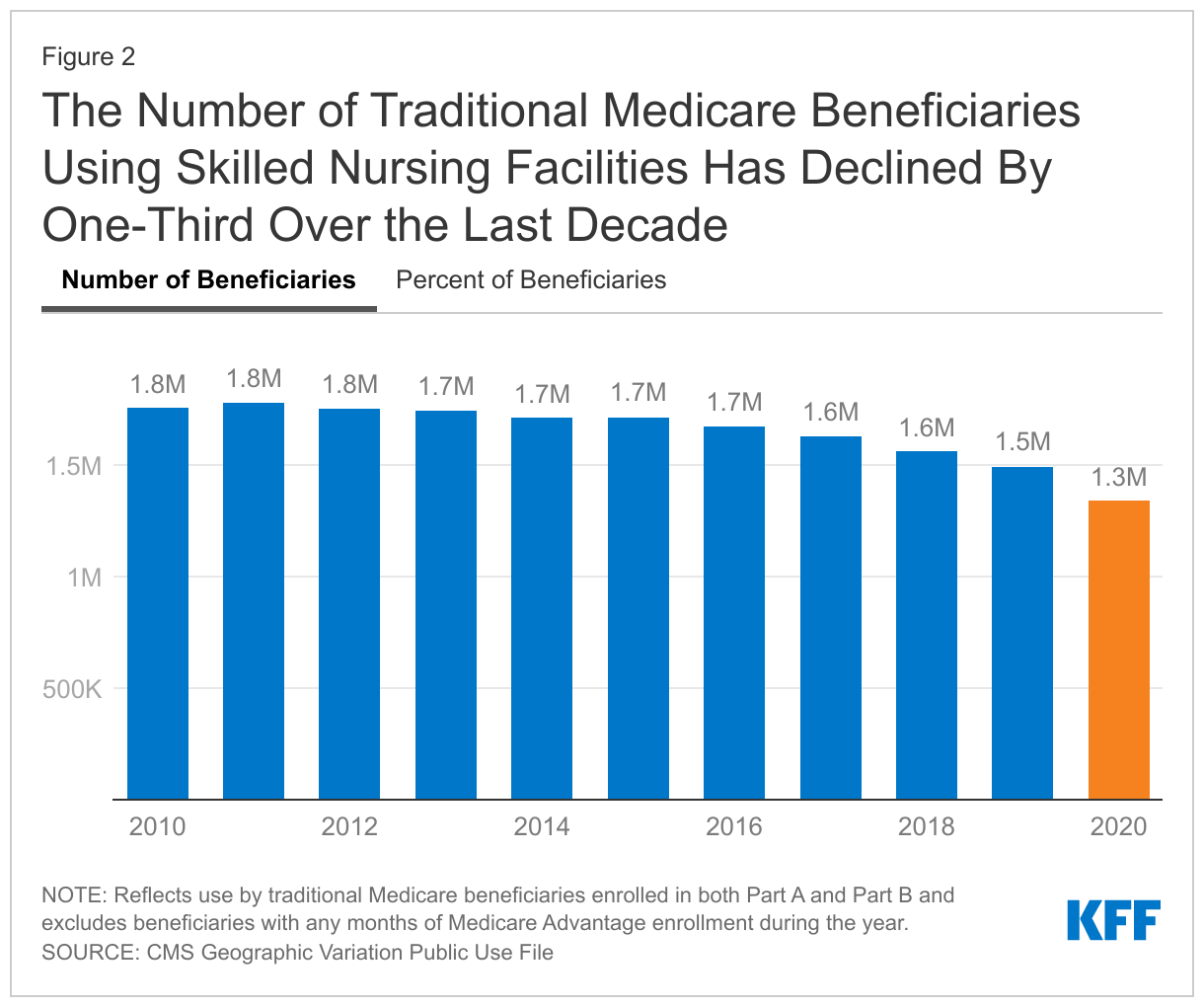
The increase in total SNF spending occurred despite a drop in both the number and share of traditional Medicare beneficiaries using SNF services in 2020. Approximately 1.3 million (4.1%) beneficiaries enrolled in both Part A and Part B of traditional Medicare had a SNF stay in 2020, slightly down from 1.5 million (4.5%) in 2019. That is the lowest number, and smallest share, of beneficiaries to use a SNF in the decade between 2010 and 2020 (Figure 2).
Traditional medicare spending per skilled nursing facility user increased sharply in 2020
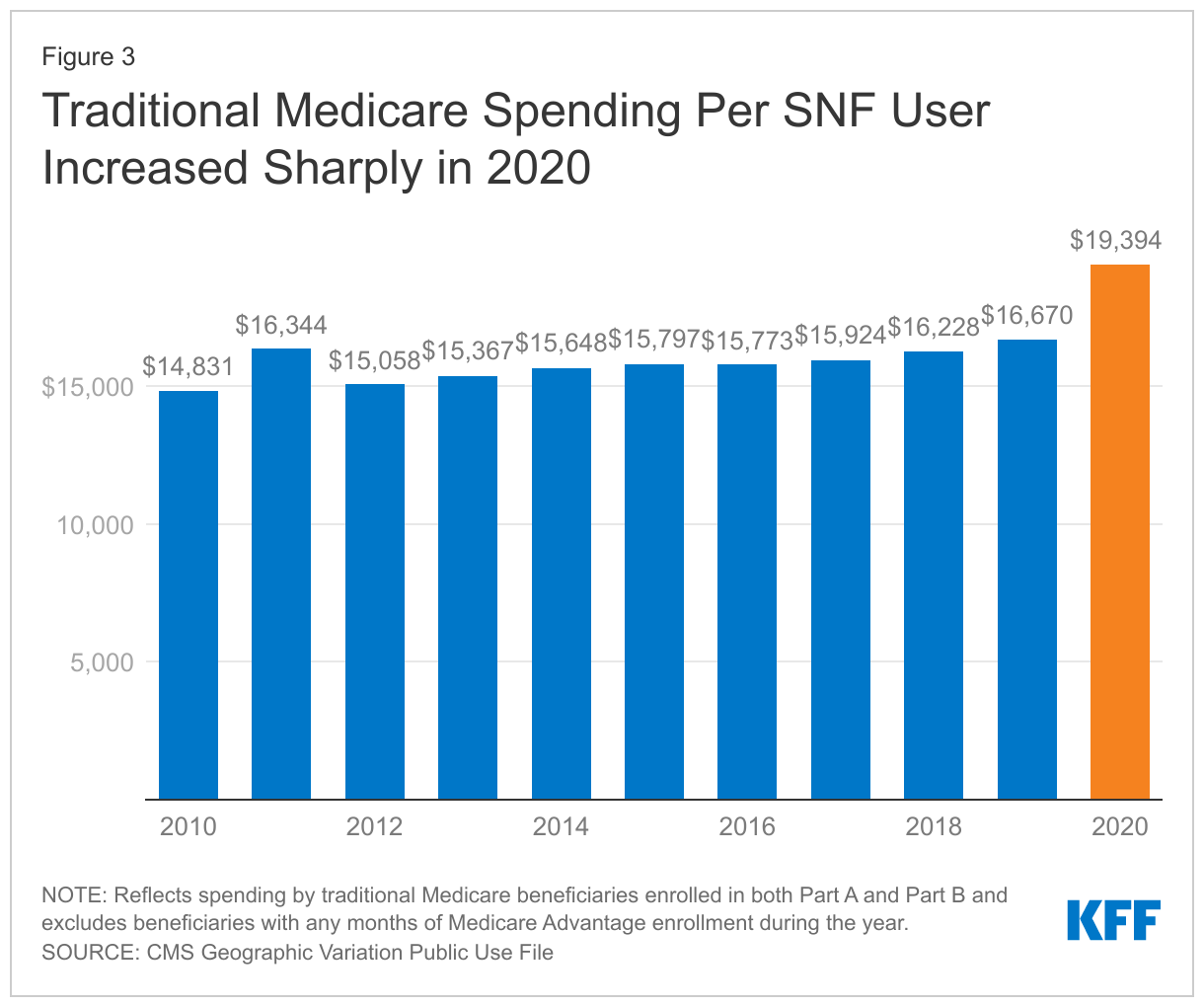
While the number of beneficiaries using SNF services declined (along with the total number of SNF stays), SNF spending per user increased $2,724 (16.3%), rising to $19,394 in 2020 from $16,670 in 2019. This is the amount spent on SNF services only, including spending for multiple SNF stays for beneficiaries who were admitted to a SNF more than once during the year. It does not reflect spending for any ancillary Part B services provided during a SNF stay. The sharp growth in spending follows several years of more gradual increases in spending per SNF user (Figure 3), which averaged 1.5% a year between 2012 and 2019.
SNF stays were longer in 2020
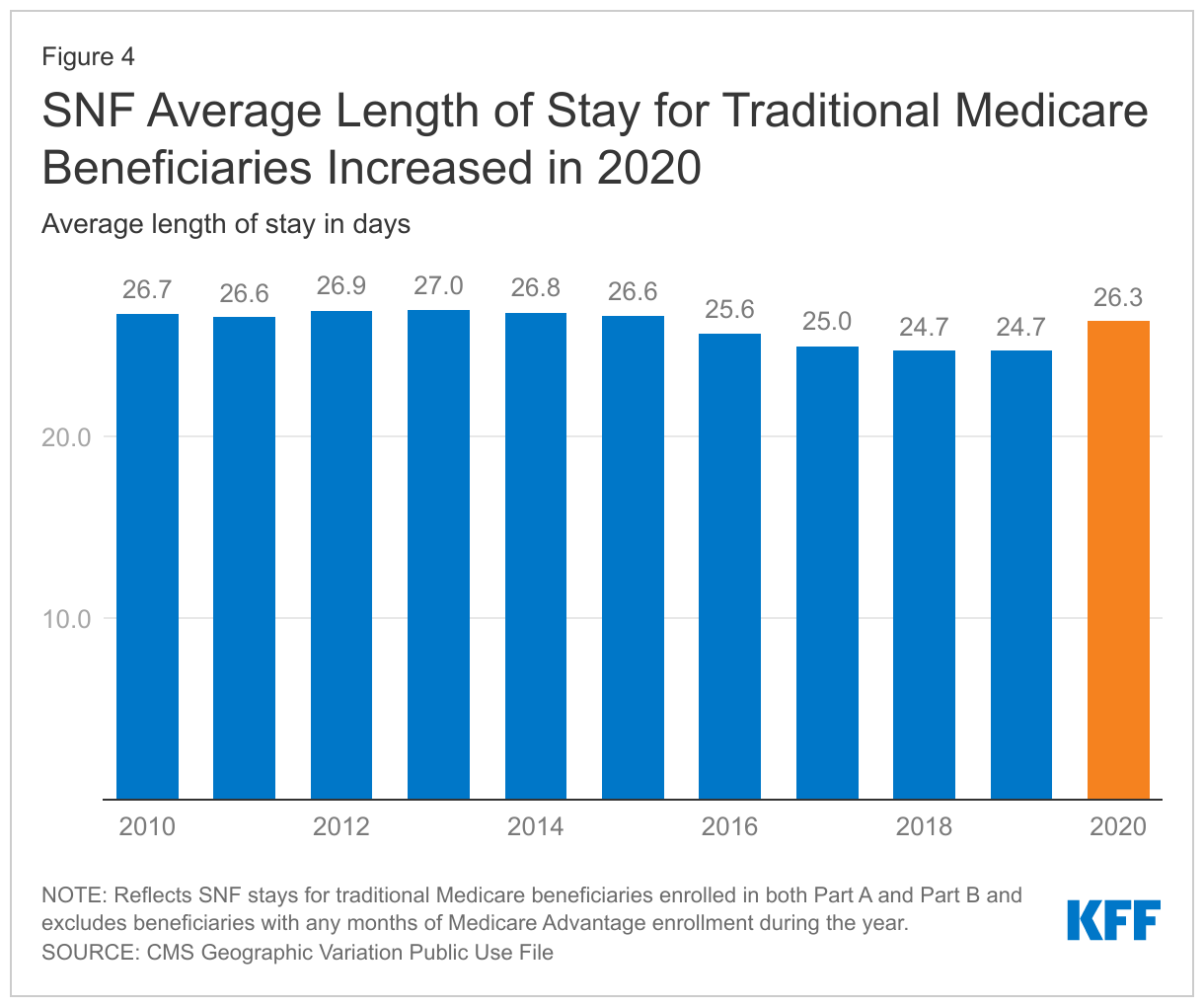
While there were fewer SNF users and fewer total SNF stays in 2020 compared to 2019, the average duration of each stay was slightly longer. In 2020, the average length of stay was 26.3 days, compared to 24.7 days in 2019. That increase follows several years of declining or stable average lengths of stay (Figure 4).
spending per day increased in 2020
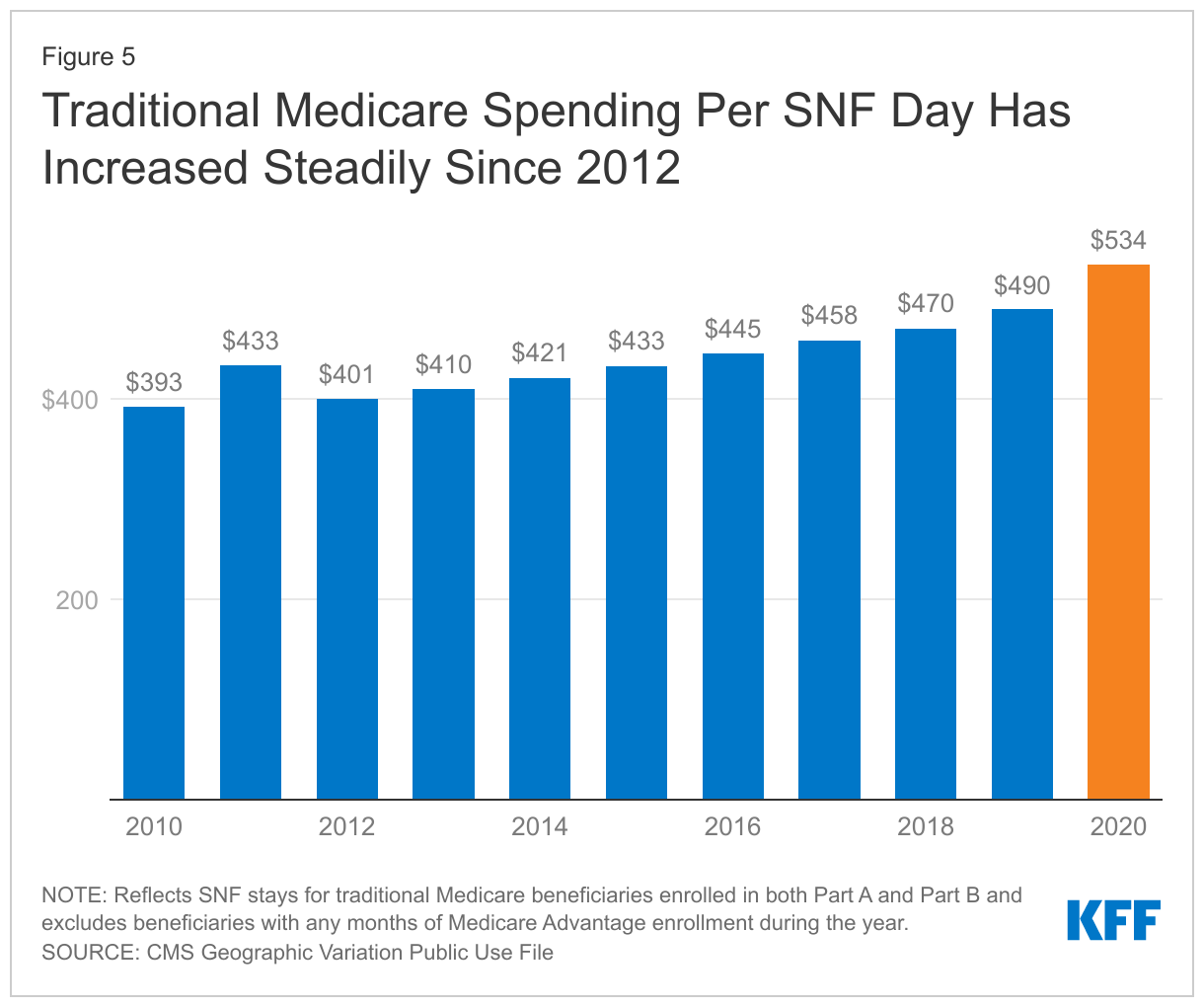
In addition to an increase in the average length of SNF stays, the average Medicare SNF spending per day rose from $490 in 2019 to $534 in 2020, or 9.1%. While SNF spending per day has increased each year since 2012, the rise in 2020 was the largest since 2011 (before changes to SNF payment in the ACA went into effect) (Figure 5). For comparison, between 2012 and 2019, average spending per day increased 2.9% a year on average.
beneficiaries under age 65 account for a disproportonate share of the increase in SNF spending
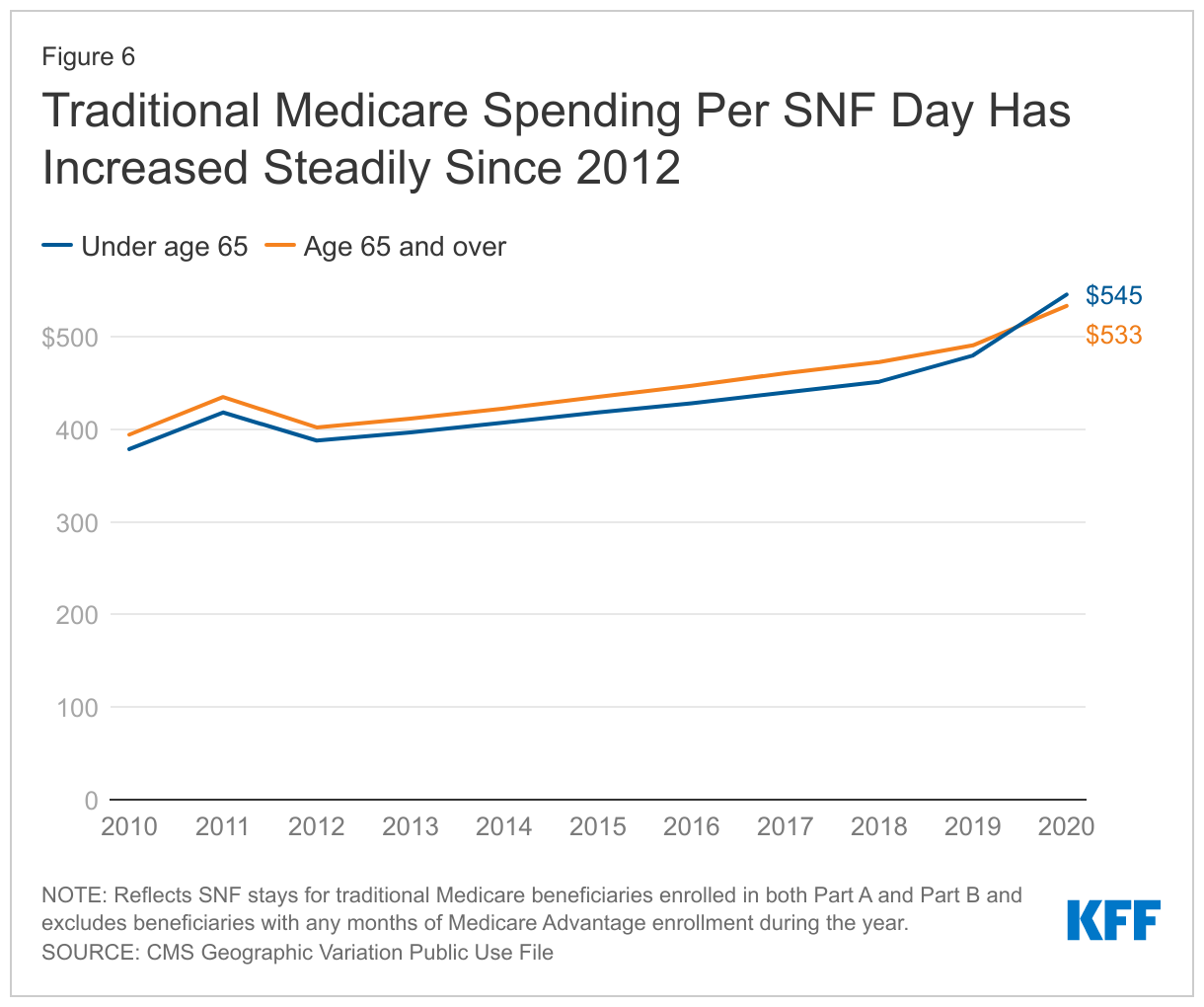
Beneficiaries under the age of 65 with long-term disabilities represent less than 10% of all traditional Medicare beneficiaries using SNF services, or approximately 115,000 of the 1.3 million SNF users in 2020. However, this group accounted for 26% of the increase in SNF spending between 2019 and 2020. This is because both the average length of stay and the spending per day for these beneficiaries rose more than for beneficiaries ages 65 and older. Specifically, the average length of stay increased 2.2 days for those under age 65 (from 25.1 to 27.3 days), compared to an increase of 0.9 days for those ages 65 and over (from 24.6 to 26.5 days). Notably, spending per SNF day was somewhat higher for younger beneficiaries than older beneficiaries for the first time in 2020 ($545 vs. $533), reflecting an increase from 2019 of $65 and $42, respectively (Figure 6). In addition, there was a smaller decline in the number of SNF users under age 65 than ages 65 and over (data not shown).
Discussion
In contrast to most other types of services, Medicare spending for skilled nursing facilities increased in 2020. This increase occurred despite an overall decrease in the number of Medicare beneficiaries using SNF services. The higher spending is explained by longer and more expensive SNF stays in 2020 compared to 2019, both of which increased more sharply for Medicare beneficiaries under the age of 65 than for older Medicare SNF users.
The longer, more expensive stays are likely the result of a change in the composition of Medicare beneficiaries admitted to SNFs, combined with revisions to the SNF prospective payment system (PPS) that went into effect in October 2019. In the first months of the COVID-19 pandemic, nursing home occupancy declined substantially, and remained well below pre-pandemic levels throughout 2020, as fewer patients underwent procedures requiring rehabilitation, such as knee or hip replacements, and people avoided both short- and long-term facilities because of concerns about infections and deaths attributable to COVID-19 in nursing homes and other long-term care facilities. Thus, beneficiaries who used SNF services likely had more intensive care needs that could not be accommodated in other settings.
In addition, to help relieve hospital capacity, CMS waived the requirement that Medicare beneficiaries have a three-day hospital stay before being admitted to a SNF. This policy likely increased occupancy levels above what they would have been otherwise, as over 15% of SNF stays in 2020 were covered under the waiver. The mix of patients also likely changed, as Medicare beneficiaries with COVID-19 were 66% more likely to be discharged from the hospital to a SNF than non-COVID patients.
Further, CMS also waived the 100-day benefit period for skilled care for people with COVID-19. This means Medicare beneficiaries with COVID-19 could renew their SNF benefits for an additional 100 days of care. This may have contributed to the longer average length of stay. In addition, it is possible that COVID-positive patients may have opted to stay longer in a SNF instead of going home and potentially infecting family members. Given the relatively high Medicare margins for SNFs, these facilities may not have had strong incentives to discharge patients quickly.
At the same time, substantial revisions to the SNF PPS went into effect in October 2019. The revised methodology is intended to better reflect the clinical care needs of patients. The changes were estimated to increase payments for medically complex patients and patients with high costs for nontherapy ancillary items. Although the changes were meant to be budget neutral, CMS estimates that the revisions led to a slight increase in payments in fiscal year 2020. These changes explain some of the higher spending per SNF user in 2020.
Notably, the sharp increase in spending per SNF user in 2020 followed relatively slow growth in spending per SNF user and year-over-year declines in total SNF spending between 2012 and 2019. Those trends, combined with early evidence of the potential for accountable care organizations (ACOs) to reduce traditional Medicare spending on SNF services, helped foster an expectation that greater coordination and communication could reduce SNF spending without compromising quality as ACOs expanded. However, the increase in SNF spending amid the pandemic and future projections may temper those expectations. While Medicare spending growth for SNFs is projected to slow once the public health emergency expires and associated waivers end, small year-over-year increases in Medicare spending on SNF services are expected through the end of the decade.
This work was supported in part by Arnold Ventures. We value our funders. KFF maintains full editorial control over all of its policy analysis, polling, and journalism activities.
Methods
We use data from the CMS Geographic Variation Public Use File, which includes spending and utilization for traditional Medicare beneficiaries who are enrolled in both Part A and Part B and have no months of Medicare Advantage enrollment during the year. These data exclude a small subset of traditional Medicare beneficiaries, and so do not match other Medicare spending data exactly.
These data are reported both overall and for beneficiaries under age 65 and age 65 and over separately. The data include the number of traditional Medicare beneficiaries enrolled in Part A and Part B, total Medicare payments for SNF services, Medicare payments per person for SNF services, Medicare payments per SNF user for SNF services, the number of SNF users, the share of traditional Medicare beneficiaries with any SNF use, the number of SNF covered stays per 1,000 beneficiaries, and the number of SNF days per 1,000 beneficiaries. In addition, we calculate the average length of stay and the average spending per day as follows:
Average length of stay = SNF days per 1,000 beneficiaries / SNF covered stays per 1000, beneficiaries
Spending per day = SNF Medicare payments / (SNF covered days per 1,000 beneficiaries * number of traditional Medicare beneficiaries with Part A and Part B / 1,000)