Medicaid Enrollment & Spending Growth: FY 2015 & 2016
Beginning in FY 2014, policy changes introduced by the Affordable Care Act (ACA) have been driving Medicaid enrollment and spending growth. This report provides an overview of Medicaid enrollment and spending growth with a focus on state Fiscal Year (FY) 2015 and state Fiscal Year 2016. Findings are based on interviews and data provided by state Medicaid directors as part of the 15th annual survey of Medicaid directors in all 50 states and the District of Columbia conducted by the Kaiser Commission on Medicaid and the Uninsured (KCMU) and Health Management Associates (HMA). Information collected in the survey on policy actions taken during FY 2015 and FY 2016 can be found in the companion report. Key findings related to Medicaid enrollment and spending growth are described below.
Medicaid enrollment and spending increased substantially in FY 2015, the first full year of implementation of the major ACA coverage expansions. Across all 50 states and DC, Medicaid enrollment increased on average by 13.8 percent in FY 2015, largely due to the ACA coverage expansions. Driven by growth in enrollment, total Medicaid spending increased by 13.9 percent on average in FY 2015. (ES – 1) Beyond enrollment, states reported that the other drivers of increases in spending were provider rate increases and the higher cost of health care, including prescription drugs. Improvements in the economy were a downward pressure on enrollment which affected spending, but downward pressure in enrollment and spending as a result of the improving economy were outweighed by the ACA coverage policy changes.
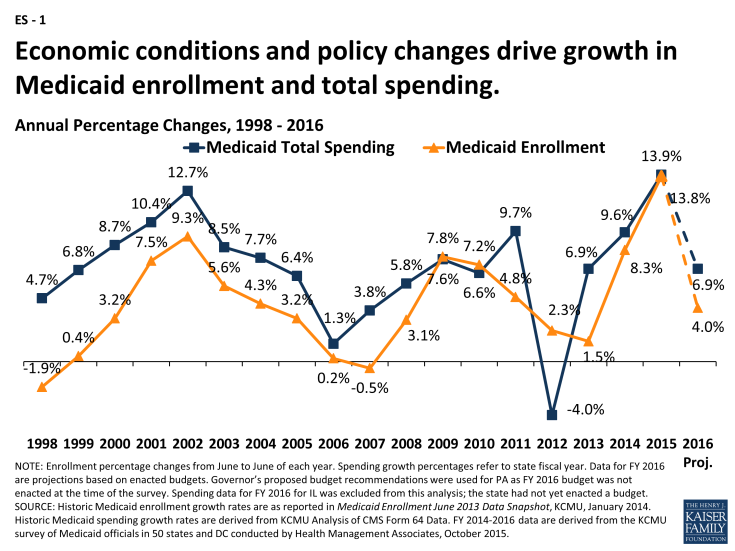
ES-1: Economic conditions and policy changes drive growth in Medicaid enrollment and total spending.
In FY 2015, Medicaid enrollment and total Medicaid spending growth in expansion states far exceeded growth in non-expansion states. Expansion states reported Medicaid enrollment and total spending growth nearly three times the rate of non-expansion states. (Figure 2) A total of 29 states were implementing the ACA Medicaid expansion in FY 2015, up from 26 states in the previous year (FY 2015 additions include: New Hampshire, Pennsylvania and Indiana).
Across the 29 expansion states in FY 2015, enrollment increased on average by 18.0 percent and total spending increased by 17.7 percent; both enrollment and spending growth were driven by increases in enrollment among adults qualifying under the new expansion group. Of the 29 states expanding Medicaid in FY 2015, more than half (17 states) noted that enrollment initially increased faster than expected. Over two-thirds of expansion states reported that per member per month costs for the expansion population were at or below projections.1 Across the 22 states not implementing the Medicaid expansion in FY 2015,2 enrollment and total spending growth was 5.1 percent and 6.1 percent (respectively), much slower growth compared to the expansion states. Increased enrollment among previously eligible parents and children was the primary reason cited for enrollment growth in non-expansion states. (ES – 2)
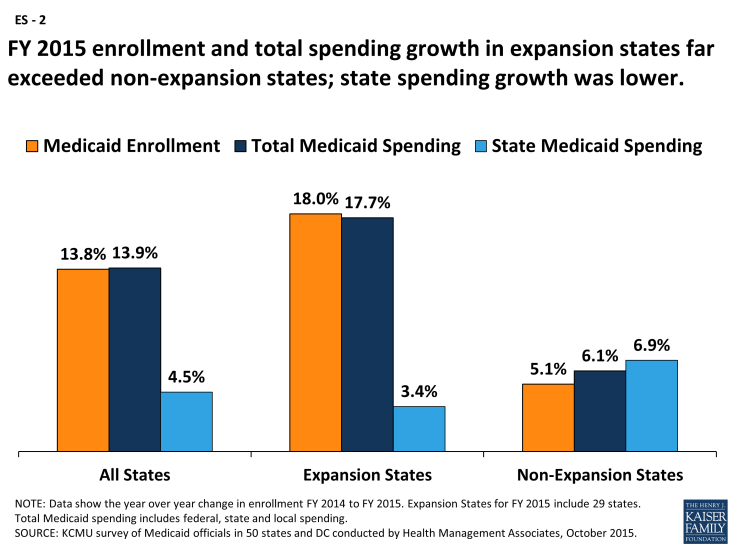
ES-2: FY 2015 enrollment and total spending growth in expansion states far exceeded non-expansion states; state spending growth was lower.
State general fund Medicaid spending3 across all states grew at more modest levels in FY 2015 than total Medicaid spending and Medicaid enrollment growth but there was variation across expansion and non-expansion states. Across expansion states, state general fund Medicaid spending grew at more modest levels compared to total Medicaid spending – primarily due to the enhanced federal match rate for those newly eligible for coverage. For non-expansion states, state Medicaid spending growth in FY 2015 slightly outpaced total Medicaid spending growth. Some non-expansion states attributed growth in state Medicaid spending to annual changes in the formula-driven federal Medicaid match rate that resulted in reductions in the federal Medicaid share for some large non-expansion states, including Texas. Across all states, state general fund Medicaid spending for FY 2015 grew at a similar rate as overall general fund growth (4.5 percent for Medicaid compared to 4.6 percent for state general fund growth).4
Total Medicaid enrollment and spending growth is projected to slow in FY 2016; looking ahead, states will monitor the effects of the ACA and other payment and delivery system reforms on spending. The major effects of the ACA were experienced by states in FY 2015; FY 2016 projections for Medicaid enrollment (4.0 percent) and total spending (6.9 percent) across all states indicate much slower growth on average than in FY 2015. Subsequently, the difference in enrollment and total spending growth rates across expansion and non-expansion states are projected to narrow in FY 2016. Expansion states are continuing to monitor and assess the effects of the Medicaid expansion on the state budget (within and beyond Medicaid). For FY 2015 and FY 2016, a number of Medicaid directors reported savings in areas including behavioral health, uncompensated care and criminal justice as well as increased revenue as a result of implementing the Medicaid expansion. Understanding these effects is important as states look ahead to 2017 when the enhanced match rate for newly eligible Medicaid expansion adults begins to decline; starting January 1, 2017 (halfway through FY 2017 for most states) the match rate will drop from 100 percent to 95 percent, resulting in a state fund share of 5 percent. Many states are also engaged in major payment and delivery system reforms that have implications for care delivery as well as program spending going forward.


