Implementing Coverage and Payment Initiatives: Results from a 50-State Medicaid Budget Survey for State Fiscal Years 2016 and 2017
Eligibility, Enrollment, Premiums, and Copayments
| Key Section Findings |
Tables 1, 2, 3, and 4 at the end of this section include additional details on eligibility, premiums, and cost-sharing policy changes in FYs 2016 and 2017. |
Changes to Eligibility Standards
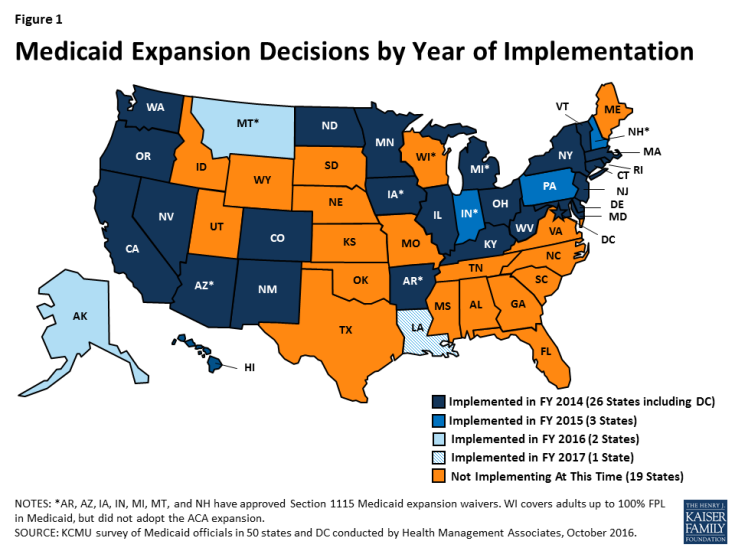
The ACA Medicaid expansion was one of the most significant Medicaid eligibility changes in the history of the program. As of October 2016, 32 states had implemented the ACA Medicaid expansion: 26 states implemented the expansion in FY 2014; three states (Indiana, New Hampshire and Pennsylvania) in FY 2015; two states (Alaska and Montana) in FY 2016, and on July 1, 2016 (FY 2017), the expansion became effective in Louisiana (Figure 1). Beyond the Medicaid expansion, states implemented or adopted only a few eligibility changes generally targeted to a limited number of beneficiaries.
Coverage Transitions
As a result of new coverage pathways (including both expanded Medicaid coverage and the availability of Marketplace subsidies), some states eliminated Medicaid coverage for beneficiaries with incomes above 138 percent FPL (most of this activity occurred in FY 2014 and was covered in earlier surveys). In addition, some individuals who had qualified through more limited Medicaid eligibility pathways, such as those related to pregnancy, family planning, spend-down, and the Breast and Cervical Cancer Treatment (BCCT), could be eligible for more comprehensive coverage through income based pathways in states that adopted the ACA Medicaid expansion. Even with alternative coverage options, many states have maintained most limited coverage options, although enrollment through these pathways may have declined. Changes to coverage above 138 percent of the FPL or to limited pathway coverage in FY 2016 or FY 2017 are listed below. Because individuals have access to Medicaid through another eligibility pathway or to other coverage options, these changes are not counted as positive or negative eligibility changes, but as “no change” (Tables 1 and 2).
- In FY 2016, Connecticut reduced Medicaid parent eligibility levels from 201 percent FPL to 155 percent FPL; many parents previously eligible at the higher levels should be eligible for Marketplace subsidies.
- New Hampshire plans to phase out its BCCT pathway in FY 2017.
- Pennsylvania eliminated spend-down for parents and adults with disabilities over age 21 as part of its Healthy PA waiver, but reinstated this coverage in March 2016.
- Ohio eliminated its family planning waiver in FY 2016. Michigan closed its family planning waiver to new enrollment in April 2014 and officially ended the program June 30, 2016.
Other Eligibility Changes
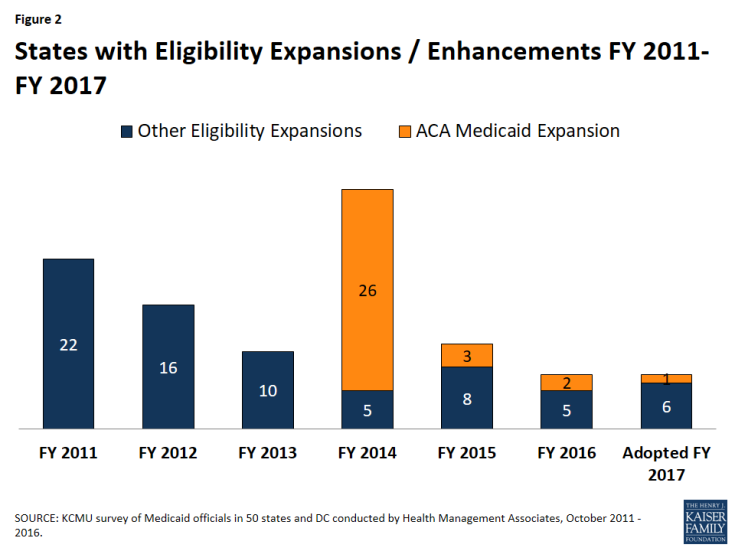
Other eligibility changes aside from the ACA expansion in FY 2016 and FY 2017 were limited and targeted to small numbers of beneficiaries (Tables 1 and 2). For FY 2016, a total of seven states made changes that expanded Medicaid eligibility and for FY 2017, seven states plan to implement Medicaid eligibility expansions (Figure 2). Key expansions include the following:
- Florida in FY 2016 and Utah in FY 2017 are implementing the option to eliminate the five-year bar on Medicaid eligibility for lawfully-residing immigrant children. Utah expects to cover an additional 750 children.
- Michigan implemented the Flint Water Group waiver, which extends Medicaid eligibility to children and pregnant women with incomes up to 400 percent FPL if they were exposed to tainted Flint water. (The waiver also expands benefits for existing eligible individuals by adding Targeted Case Management.)
- Maine will increase eligibility under its family planning pathway to 209 percent FPL in FY 2017.
Only two states in FY 2016 (Ohio and Virginia) and two states in FY 2017 (Arkansas and Missouri) made or plan to make eligibility restrictions. These are mostly targeted restrictions that would affect small groups of beneficiaries. Arkansas is seeking a modification to its “Private Option” waiver to, effective January 1, 2017, eliminate retroactive eligibility for expansion enrollees; the waiver is pending at CMS. Missouri plans to begin the process of suspending its family planning waiver in FY 2017 following legislative restrictions in the FY 2017 appropriations bill.1 The FY 2016 reduction in eligibility for waiver services in Virginia for seriously mentally ill individuals (GAP waiver program) was partially restored in FY 2017.
Coverage Initiatives for the Criminal Justice Population
With the ACA Medicaid expansion to low-income adults, many individuals involved with the justice system are now eligible for Medicaid. Connecting these individuals to health coverage can facilitate their integration back into the community by increasing their ability to address health needs, which may contribute to greater stability in their lives as well as broader benefits to the individual and society as a whole. An increasing number of states have efforts underway to enroll eligible individuals moving into and out of the justice system into Medicaid. In April 2016 guidance, the Centers for Medicare and Medicaid Services (CMS) clarified that incarcerated individuals may be determined eligible for Medicaid and that the state Medicaid agency must accept applications and process renewals for incarcerated individuals.2 Although individuals may be enrolled in Medicaid while they are incarcerated, Medicaid cannot cover the cost of their care, except for inpatient services. In its recent guidance, CMS clarified who is considered an inmate of a public institution and therefore only able to receive Medicaid coverage for inpatient care.3 This survey asked states about a number of initiatives to promote Medicaid coverage for individuals involved with the criminal justice system (Exhibit 1 and Table 3).
The vast majority of states (44) had policies in place as of FY 2015 to obtain Medicaid reimbursement for inpatient care provided to incarcerated individuals who are Medicaid eligible. Four additional states implemented these policies in FY 2016 or plan to in FY 2017.
Given that the Medicaid expansion has significantly increased Medicaid eligibility among individuals moving into and out of the criminal justice system, many states are newly adopting or expanding initiatives to connect this population to Medicaid coverage. States are adopting policies to suspend Medicaid eligibility (rather than terminate eligibility) during incarceration. In FY 2015, 25 states had these policies in place for at least some individuals entering jail or prison, and 41 states are expected to have suspension policies by the end of FY 2017.
Medicaid and corrections agencies are also working together to help connect individuals to coverage as they are released from jail or prison back to the community. Some of these approaches include providing outreach and enrollment assistance pre-release, expedited enrollment processes for individuals being released, and Medicaid eligibility staff dedicated to processing applications for this population. A number of states have such initiatives in place and some states reported expanding these enrollment activities in FY 2016 or 2017. The most common expansions involve increasing the geographic scope of jail initiatives or increasing the number of prisons where eligibility assistance is provided.
The survey did not ask states about initiatives specific to parolees and individuals residing in halfway houses. However, Colorado, Connecticut, and the District of Columbia specifically mentioned initiatives to cover individuals residing in halfway houses.
|
Exhibit 1: Coverage Initiatives for the Criminal Justice Population
(# of States)
|
||||
| Select Medicaid Coverage Policies for the Criminal Justice Population | In Place in FY 2015 | New FY 16 or 17 |
Expanded FY 16 or 17 | In place/ planned for FY 2017 |
| Medicaid coverage for inpatient care provided to incarcerated individuals | 44 | 4 | 4 | 48 |
| Medicaid outreach/assistance strategies to facilitate enrollment prior to release | 31 | 11 | 13 | 42 |
| Medicaid eligibility suspended (rather than terminated) for enrollees who become incarcerated (jails OR prisons) | 25 | 16 | 3 | 41 |
| Arizona Medicaid and Corrections Policies |
| Arizona has implemented a number of strategies to increase coverage and access to care for the criminal justice population. The Arizona Health Care Cost Containment System (AHCCCS), the state’s Medicaid agency, has agreements with most counties, including the two largest, and the Arizona Department of Corrections to allow for suspension of enrollment for jail and prison inmates. Arizona also provides support to counties to help them connect to the state’s eligibility system and facilitate enrollment and train community-based organizations, providers, and others on using the system for application assistance. The two most populous counties in the state have arrangements to provide enrollment assistance to persons on probation and throughout other areas of the system. The state also provides an expedited eligibility determination process for uninsured inmates with critical health needs who are scheduled to be released. Arizona has mandated that all Regional Behavioral Health Authorities have a designated liaison for coordinating care for persons with serious mental illness who are transitioning from the justice system. There is expedited review for individuals being discharged with a medical or behavioral health need so that care can be coordinated promptly. The state is also looking into ways to access data obtained through assessments as part of the probation process and other information that will help coordinate care. |
Medicaid Financed Births
For over three decades, Medicaid has been a key source of financing of births for low- and modest-income families. Women who would not otherwise be eligible can qualify for Medicaid coverage for pregnancy, delivery, and postpartum care due to higher income eligibility thresholds for pregnant women.4 Medicaid directors were asked to provide the most recent available data on the share of all births in their states that were financed by Medicaid. About half of states were able to provide data for calendar 2015 or fiscal year 2015.5 Other states generally provided data from 2013 or 2014. On average,6 states reported that Medicaid pays for just over 47 percent of all births. Eight states (Arkansas,7 Louisiana, Mississippi, Nevada, New Mexico, Oklahoma, South Carolina, and West Virginia) reported that Medicaid pays for 60 percent or more of all births in their state, while nine states reported that Medicaid finances less than 40 percent of all births (Iowa, Kansas, Nebraska, New Hampshire, North Dakota, Pennsylvania, Utah, Virginia, and Wyoming).
Premiums and Copayments
States have flexibility to charge limited premiums and cost-sharing in Medicaid, subject to federal parameters. Premiums are generally prohibited for beneficiaries with income below 150 percent FPL. Cost-sharing for people with income below 100 percent FPL is limited to “nominal” amounts specified in federal regulations, with higher levels allowed for beneficiaries at higher income levels. However, certain groups are exempt from cost-sharing, including mandatory eligible children, pregnant women, most children and adults with disabilities, people residing in institutions, and people receiving hospice care. In addition, certain services are exempt from cost-sharing: emergency services, preventive services for children, pregnancy-related services, and family planning services. Total Medicaid premiums and cost-sharing for a family cannot exceed 5 percent of the family’s income on a quarterly or monthly basis.8
Details about state actions related to premiums and copayments can be found in Table 4.
Premiums
Medicaid generally is not allowed to charge premiums to Medicaid beneficiaries with incomes at or below 150 percent FPL, although in limited cases certain populations, generally with income above 100 percent FPL, may be charged premiums (sometimes referred to as “buy-in” programs). Forty-four (44) states have buy-in programs for working people with disabilities and most of these states impose premiums.9 States also have the option to implement buy-in programs for children with disabilities. States that reported implementing premium-based programs under the Family Opportunity Act (FOA) for children with disabilities in families with incomes that otherwise exceed Medicaid limits include Colorado, Louisiana, North Dakota, and Texas.10 More recently, some states have received approval or were seeking approval to impose premiums under a Medicaid expansion waiver.
Seven states reported that they implemented or plan to implement new or increased premiums in FY 2016 or FY 2017 (Table 4). Three of these premium changes are related to individuals with disabilities. In FY 2016, Iowa increased Medicaid premiums for working people with disabilities. Two other states (Michigan in FY 2016 and Colorado in FY 2017) implemented or plan to implement expanded coverage and premiums for individuals with disabilities.
Five states (Arkansas, Indiana, Iowa, Michigan, and Montana) have received federal waivers to require premiums/monthly contributions for Medicaid expansion enrollees.11 In some cases, monthly contributions may be imposed in lieu of point-of-services copayments.12
Other implemented or proposed changes in premiums or contributions are for the Medicaid expansion populations.
- Montana implemented the Medicaid expansion in January 2016 under a waiver that requires monthly premiums up to 2 percent of household income for newly eligible adults from 51-138 percent FPL.
- Arkansas has waiver amendments pending that would take effect in calendar year 2017. The proposed waiver would replace the current income-based monthly contributions to “Health Independence Accounts,” which are to be used to fund copayments instead of paying at the point of service, with a premium requirement of 2 percent of income for those with incomes above 100 percent of FPL.
- Arizona had a waiver pending that would impose monthly premiums of 2 percent of income or $25, whichever is less, on all Medicaid expansion adults from 0-138 percent FPL, paid into health savings accounts. The waiver was approved on September 30, 2016 and allows for premiums at 2 percent of income for non-medically frail 100-138 percent FPL; individuals that comply with a healthy behavior program could have premiums eliminated for six months.
- Ohio submitted a waiver request in June 2016 to change its traditional expansion to the Healthy Ohio program which would impose monthly contributions, equal to the lesser of 2 percent of annual income or $99 per year, as a condition of eligibility for all beneficiaries except pregnant women and those with zero income. On September 9, 2016 CMS denied the state’s waiver request.
Kentucky has a waiver pending with CMS that would add premiums to its traditional Medicaid expansion program, along with other changes, but the proposed effective date is not until July 1, 2017 (FY 2018) so it is not captured in this report.
Copayment Requirements
- Five states reported new or increased copayment requirements for the Medicaid expansion population: Montana implemented new requirements in FY 2016, Louisiana plans to do so in FY 2017, Michigan plans to double copayments for Healthy Michigan Plan enrollees with incomes above 100 percent FPL in FY 2017, and New Hampshire planned copayment requirements for FY 2017 but these changes are included in waivers pending at CMS. The Ohio waiver that was denied would have increased copayments. The waiver approved in Arizona would allow for copayments (within state plan permissible levels) to be charged retrospectively for certain services such as non-emergency use of the emergency department, seeing a specialist without a referral, and use of brand name drugs when there is an available generic. Beneficiaries would get a quarterly invoice and be charged a monthly amount up to 3 percent of monthly income.
- In FY 2016, Indiana restored copayments for aged, blind, and disabled enrollees in managed care and Minnesota decreased copayment amounts for the Medical Assistance for Employed Persons with Disabilities (MA-EPD) group.
- In FY 2017, New Mexico plans to implement new copayments for non-emergency use of the emergency department for all Medicaid enrollees and new pharmacy copayments for all populations for brand name prescriptions when there is a less expensive generic equivalent available.13
- Four states are eliminating one or more copayment provisions in either FY 2016 or FY 2017 (North Dakota, New York, Oregon, and Vermont).
Table 1: Changes to Eligibility Standards in all 50 States and DC, FY 2016 and FY 2017
| Eligibility Standard Changes | ||||||
| States | FY 2016 | FY 2017 | ||||
| (+) | (-) | (#) | (+) | (-) | (#) | |
| Alabama | ||||||
| Alaska | X – Medicaid Expansion | |||||
| Arizona | ||||||
| Arkansas | X | |||||
| California | ||||||
| Colorado | X | X | ||||
| Connecticut | X | |||||
| Delaware | ||||||
| DC | X | |||||
| Florida | X | X | ||||
| Georgia | ||||||
| Hawaii | ||||||
| Idaho | ||||||
| Illinois | ||||||
| Indiana | ||||||
| Iowa | ||||||
| Kansas | ||||||
| Kentucky | ||||||
| Louisiana | X-Medicaid Expansion | X | ||||
| Maine | X | |||||
| Maryland | X | |||||
| Massachusetts | ||||||
| Michigan | X | X | ||||
| Minnesota | X | |||||
| Mississippi | ||||||
| Missouri | X | |||||
| Montana | X – Medicaid Expansion | |||||
| Nebraska | ||||||
| Nevada | ||||||
| New Hampshire | X | |||||
| New Jersey | ||||||
| New Mexico | ||||||
| New York | ||||||
| North Carolina | ||||||
| North Dakota | ||||||
| Ohio | X | X | X | |||
| Oklahoma | ||||||
| Oregon | ||||||
| Pennsylvania | X | |||||
| Rhode Island | ||||||
| South Carolina | ||||||
| South Dakota | ||||||
| Tennessee | ||||||
| Texas | ||||||
| Utah | X | X | X | |||
| Vermont | X | |||||
| Virginia | X | X | ||||
| Washington | ||||||
| West Virginia | ||||||
| Wisconsin | ||||||
| Wyoming | ||||||
| Totals | 7 | 2 | 7 | 7 | 2 | 3 |
|
NOTES: Positive changes from the beneficiary’s perspective that were counted in this report are denoted with (+). Negative changes from the beneficiary’s perspective that were counted in this report are denoted with (-). Several states made reductions to Medicaid eligibility pathways in response to the availability of other coverage options (including Marketplace and/or Medicaid expansion coverage); these changes were denoted as (#) since most affected beneficiaries will have access to coverage through an alternative pathway.
SOURCE: Kaiser Commission on Medicaid and the Uninsured Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2016.
|
||||||
Table 2: States Reporting Eligibility Changes in FY 2016 and FY 2017
| State | Fiscal Year | Eligibility Changes |
| Alaska | 2016 | Adults (+): Medicaid expansion on September 1, 2015 (estimated first year enrollment of 20,100). |
| Arkansas | 2017 | Adults (-): Pending waiver would eliminate retroactive eligibility for expansion population. |
| Colorado | 2016 | Children (+): Implement the CHIPRA option to eliminate the 5-year bar on Medicaid eligibility for legally-residing immigrant children (estimated to affect 1,699 children). |
| 2017 | Adults (+): Implementing annualized income for eligibility for other adults (affects 20,430 individuals). | |
| Connecticut | 2016 | Adults (#): Effective August 1, 2015 the income limits for HUSKY A parents and caretaker relatives were reduced from 201% FPL to 155% FPL. |
| DC | 2016 | Adults (#): Section 1115 Childless Adult waiver expired 12/31/2015. Adults with incomes from 133% to 210% FPL were transitioned from a Medicaid waiver to Medicaid state plan (8,500 individuals). |
| Florida | 2016 | Aged and Disabled (+): Increased the minimum monthly maintenance income allowance and excess standard for community spouses of institutionalized people. (The number of nursing facility residents eligible for Medicaid is also affected by 2016 cost of living adjustments and increases in the average private pay nursing facility used to set LTSS policy.)
Children (+): Implement the CHIPRA option to eliminate the 5-year bar on Medicaid eligibility for legally-residing immigrant children. |
| 2017 | Aged and Disabled (+): Increased the minimum monthly maintenance income allowance and excess standard for community spouses of institutionalized people. (The number of nursing facility residents eligible for Medicaid is also affected by 2017 cost of living adjustments and increases in the average private pay nursing facility used to set LTSS policy.) | |
| Louisiana | 2017 | Adults (+): Implemented Medicaid expansion on July 1, 2016 (375,000 individuals).
Adults (#): Effective July 1, 2016, 127,109 people covered in the Family Planning State Plan Amendment (SPA) were enrolled in the new Adult Group. The people remaining in the Family Planning SPA do not qualify for the Adult Group. |
| Maine | 2017 | Adults (+): Plan to increase eligibility under family planning pathway to 209% FPL in FY 2017. |
| Maryland | 2016 | Adults (#): Breast and Cervical Cancer Treatment Program continued only for enrollees in active treatment (400 individuals). |
| Michigan | 2016 | Adults (#): Family planning waiver ended 6/30/2016.
Children & Pregnant Women (+): Flint Waiver Group Waiver extends Medicaid eligibility to 400% FPL for children and pregnant women exposed to tainted Flint water (up to 15,000 individuals). Aged & Disabled (+): Increased income and asset limits for working people with disabilities, effective 10/1/15. |
| Minnesota | 2017 | Aged & Disabled (+): Increased income standard for the medically needy from 75% FPL to 80% FPL on 7/1/2016. |
| Missouri | 2017 | Adults (-): Based on restrictions in the FY 2017 appropriation bill, Missouri will begin the process of suspending the Family Planning 1115 waiver. Expected transition 2/1/2017. |
| Montana | 2016 | Adults (+): Implemented ACA expansion via a waiver. Implemented 12-month continuous eligibility for newly eligible adults as part of the waiver. Effective 1/1/2016. |
| New Hampshire | 2017 | Adults (#): State legislation calls for ending the Breast and Cervical Cancer Treatment Program for new enrollees in FY 2017 while allowing current enrollees to continue treatment. |
| Ohio | 2016 | Adults (#): Ended Family Planning coverage group as of 1/1/16.
Other (-): Change in transitional Medicaid for families from twelve-months eligibility to six-months eligibility with possible coverage for two reporting periods. |
| 2017 | Aged & Disabled (#): Conversion from 209(b) to 1634 for SSI related groups. | |
| Pennsylvania | 2016 | Adults (#): Medically Needy Spend-Down for Parents and People with Disabilities was restricted to individuals under the age of 21 as part of Healthy PA implementation. However, it was reinstated in March 2016 and is once again available to these adults. |
| Utah | 2016 | Children (+): Medically Complex Children’s Waiver (165 children).
Children (#): Autism Waiver enrollment closed since autism services were added to the State Plan. |
| 2017 | Children (+): Implementing the CHIPRA option to eliminate the 5-year bar on Medicaid eligibility for legally-residing immigrant children (estimated to affect 750 children).
Adults (+): Proposed limited adult expansion: Parents of dependent children with incomes 40% to 60% FPL; adults without dependent children with incomes up to 5% FPL meeting certain criteria (9,000 to 11,000 individuals). |
|
| Vermont | 2016 | Aged & Disabled (+): Increased asset limits and income disregards for working people with disabilities (70 individuals). |
| Virginia | 2016 | Aged & Disabled (-): Reduced eligibility from 100% to 60% FPL for waiver services for people with serious mental illness (GAP waiver program). |
| 2017 | Aged & Disabled (+): Increased eligibility from 60% to 80% FPL for waiver services for people with serious mental illness (GAP waiver program). | |
| NOTE: Positive changes from the beneficiary’s perspective that were counted in this report are denoted with (+). Negative changes from the beneficiary’s perspective that were counted in this report are denoted with (-). Reductions to Medicaid eligibility pathways in response to the availability of other coverage options (including Marketplace or Medicaid expansion coverage) were denoted as (#). | ||
Table 3: Corrections-Related Enrollment Policies in all 50 States and DC, FY 2015-FY 2017
| States | Medicaid Coverage For Inpatient Care Provided to Incarcerated Individuals | Medicaid Outreach/Assistance Strategies to Facilitate Enrollment Prior to Release | Medicaid Eligibility Suspended Rather Than Terminated For Enrollees Who Become Incarcerated (Jails or Prisons) | |||||||||
| In place FY 2015 | New FY 16/17 |
Expanded FY16/17 | In place/planned for FY17 | In place FY 2015 | New FY 16/17 |
Expanded FY16/17 | In place/planned for FY17 | In place FY 2015 | New FY 16/17 |
Expanded FY16/17 | In place/planned for FY17 | |
| Alabama | X | X | X | X | X | X | X | X | ||||
| Alaska | X | X | X | X | X | X | X | |||||
| Arizona | X | X | X | X | X | X | ||||||
| Arkansas | X | X | X | X | X | X | ||||||
| California | X | X | X | X | X | X | ||||||
| Colorado | X | X | X | X | X | |||||||
| Connecticut | X | X | X | X | X | X | ||||||
| Delaware | X | X | X | X | X | X | ||||||
| DC | X | X | X | X | X | X | ||||||
| Florida | X | X | X | X | ||||||||
| Georgia | X | X | ||||||||||
| Hawaii | X | X | X | X | X | X | ||||||
| Idaho | X | X | X | X | ||||||||
| Illinois | X | X | X | X | X | X | ||||||
| Indiana | X | X | X | X | X | X | ||||||
| Iowa | X | X | X | X | X | X | ||||||
| Kansas | X | X | X | X | ||||||||
| Kentucky | X | X | X | X | X | X | X | |||||
| Louisiana | X | X | X | X | X | X | X | |||||
| Maine | X | X | X | X | ||||||||
| Maryland | X | X | X | X | X | X | X | |||||
| Massachusetts | X | X | X | X | X | X | ||||||
| Michigan | X | X | X | X | X | X | ||||||
| Minnesota | X | X | X | X | X | X | ||||||
| Mississippi | X | X | X | X | X | X | X | |||||
| Missouri | X | X | X | X | ||||||||
| Montana | X | X | X | X | X | X | X | X | ||||
| Nebraska | X | X | X | X | ||||||||
| Nevada | X | X | ||||||||||
| New Hampshire | X | X | X | X | X | X | X | |||||
| New Jersey | X | X | X | X | X | X | ||||||
| New Mexico | X | X | X | X | X | X | X | X | X | |||
| New York | X | X | X | X | X | X | X | |||||
| North Carolina | X | X | X | X | X | X | ||||||
| North Dakota | X | X | X | X | X | X | X | |||||
| Ohio | X | X | X | X | X | X | X | |||||
| Oklahoma | X | X | ||||||||||
| Oregon | X | X | X | X | X | X | ||||||
| Pennsylvania | X | X | X | X | X | X | ||||||
| Rhode Island | X | X | X | X | X | X | X | |||||
| South Carolina | X | X | X | X | X | X | X | X | ||||
| South Dakota | X | X | X | X | ||||||||
| Tennessee | X | X | X | X | ||||||||
| Texas | X | X | X | X | X | X | ||||||
| Utah | X | X | X | X | ||||||||
| Vermont | X | X | ||||||||||
| Virginia | X | X | X | X | X | X | ||||||
| Washington | X | X | X | X | X | X | ||||||
| West Virginia | X | X | X | X | X | X | ||||||
| Wisconsin | X | X | X | X | ||||||||
| Wyoming | ||||||||||||
| Totals | 44 | 4 | 4 | 48 | 31 | 11 | 13 | 42 | 25 | 16 | 3 | 41 |
|
NOTES: States were asked to indicate if any of the above corrections-related policies were in effect in FY 2015 and if they were newly adopted or expanded in FY 2016 or FY 2017. The “in place/planned for FY 2017” columns indicate states that either had a given policy in place as of FY 2015, newly implemented the policy in FY 2016, or plan to newly implement the policy in FY 2017. States with “Medicaid outreach assistance strategies to facilitate enrollment prior to release” include those with Medicaid led/coordinated efforts on outreach/enrollment assistance prior to release, expedited enrollment prior to release (e.g. presumptive eligibility), and/or Medicaid eligibility staff devoted to processing determinations prior to release.
SOURCE: Kaiser Commission on Medicaid and the Uninsured Survey of Medicaid Officials in 50 states and DC conducted by Health Management Associates, October 2016.
|
||||||||||||
Table 4: States Reporting Premium and Copayment Actions Taken in FY 2016 and FY 2017
| State | Fiscal Year | Premium and Copayment Changes |
| Arizona | 2017 | Premiums (New non-medically frail adults 100-138% FPL): Waiver approved September 30, 2016 would allow premiums of 2 percent of income for adults with incomes 100-133% FPL. Individuals that comply with a health behavior program could have premiums eliminated for six months.
Copayments (New non-medically frail adults 100-138% FPL): The approved waiver would allow for copayments (within state plan permissible levels) to be charged retrospectively for certain services such as non-emergency use of the emergency department, seeing a specialist without a referral and use of brand name drugs when there is an available generic. Beneficiaries would get a quarterly invoice and be charged a monthly amount up to 3% of monthly income. Premiums and copayments together would be limited to the 5% cap of household income per quarter. |
| Arkansas | 2017 | Premiums (New for expansion population): Pending “Arkansas Works” waiver amendments would replace current required contributions to “Health Independence Accounts” in lieu of point-of-service copayments with required monthly premiums of 2% of household income for individuals between 100 and 138% FPL |
| Colorado | 2017 | Premiums (New option for LTSS populations): Implement a Medicaid Buy-In program for 3 HCBS waivers (7/1/16). |
| Indiana | 2016 | Copayments (New): Restore copayments for ABD enrollees in managed care (Jan 2016). |
| Iowa | 2016 | Premiums (Increased): The premium for working people with disabilities is based on state employee health insurance premium which increased in 2016. Unknown for 2017. |
| Louisiana | 2017 | Copayments (New for expansion population): New cost-sharing requirements for the expansion population are the same as those in place for the rest of the Medicaid population. |
| Michigan | 2016 | Premiums (Increased): Premiums for the Freedom to Work population are now calculated using a percent of a beneficiary’s MAGI income (10/1/2015). |
| 2017 | Copayments (Increase): Increase in prescription, hospital, and office visit copays for Healthy Michigan Plan enrollees with incomes above 100% FPL. | |
| Minnesota | 2016 | Premiums (Decreased): Minimum premium for Medical Assistance for Employed Persons with Disabilities (MA-EPD) reduced (Sep 2015).
Copayments (Decreased): Decreased copayment amounts for MA-EPD group (Sep 2015). |
| Montana | 2016 | Premiums (New only for expansion population): Newly eligible adults between 51 and 138% FPL required to pay monthly premiums up to 2% of household income (1/1/2016).
Copayments (New for expansion population): Childless adults with incomes below 138% FPL and parents with incomes between 51% and 138% FPL (1/1/2016). Copayments (Neutral): Cost sharing for adults with incomes up to 50% FPL was standardized with some amounts increased and some decreased (6/1/2016). |
| New Hampshire | 2016 | Copayments (Increased): Pharmacy copayments for the expansion population (those above 100% FPL) are being increased from $1/$4 (generic/brand) to $2/$8 (Jan 2016). |
| 2017 | Copayments (New only for expansion population): Pending waiver would subject expansion population to copayments on some medical services. | |
| New Mexico | 2017 | Copayments (New for all populations): Copays for non-emergency use of the emergency department (1/1/2017 target date).
Copayments (New for all populations): Copays for brand-name prescriptions when there is a less expensive generic equivalent medicine available (1/1/2017 target date). |
| New York | 2016 | Copayments (Elimination): Exemption from Medicaid co-pays for members with incomes below 100% FPL, hospice patients, and American Indians/Alaskan Natives who have never received a service from IHS, tribal health programs, or under contract health services referral (10/1/15). |
| North Dakota | 2017 | Copayments (Elimination): Higher copayment for non-emergency use of the ER will be eliminated (1/1/2017). |
| Ohio | 2017 | Premiums (New and would apply to all Medicaid beneficiaries except pregnant women and individuals with zero income): Waiver request to impose monthly premiums (the lesser of 2% of income or $99 per year). CMS denied Ohio’s pending waiver in September 2016.
Copayments (Increase): Healthy Ohio 1115 waiver would increase copayments for all beneficiaries covered by the waiver at the maximum amounts allowable under federal law and copayments would be paid into a Health Savings Account and paid from that account at point of service. CMS denied Ohio’s pending waiver in September 2016. |
| Oregon | 2017 | Copayments (Elimination): Copayments are being eliminated for preventive services for all Medicaid groups (1/1/2017). |
| Vermont | 2017 | Copayments (Elimination): Remove copays for sexual assault-related services for all Medicaid groups (10/1/2016). |
| NOTE: New premiums or copayments as well as new requirements such as making copayments enforceable are denoted as (New). Increases in existing premiums or copayments are denoted as (Increased), while decreases are denoted as (Decreased) and eliminations are denoted as (Eliminated). | ||