What are the Implications of Long COVID for Employment and Health Coverage?
Long COVID has been described as our “next national health disaster” and the “pandemic after the pandemic,” but we know little about how many people are affected, how long it will last for those affected, and how it could change employment and health coverage landscapes. This policy watch reviews what we know and outlines key questions to watch for regarding employment and coverage outcomes. We continue to follow the research on who is most at risk of long COVID and whether there are interventions that can reduce its incidence, length, or severity. The numbers are already daunting and infections continue to rise. The newest subvariant—BA.5— readily infects the vaccinated and people with prior immunity. Vaccines and prior immunity protect against severe illness and death, but it is unclear whether they protect against long COVID. One study of the VA health system found that the risks of long COVID increased with each subsequent reinfection.
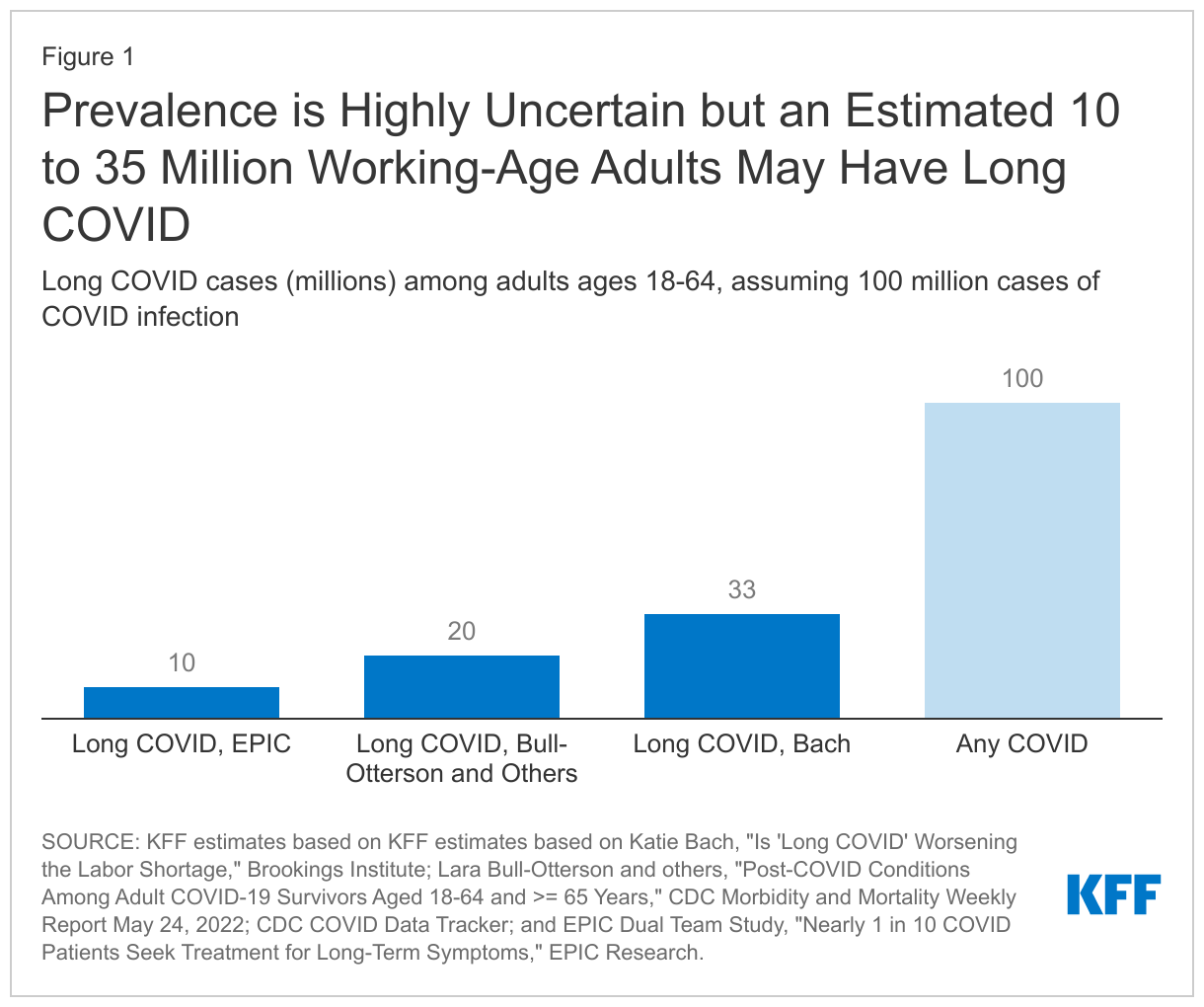
Long COVID involves a range of potentially disabling symptoms and may affect 10 to 33 million working-age adults in the United States (Figure 1). Long COVID is not a single condition but rather “a wide range of new, returning, or ongoing health problems that people experience after first being infected with the virus that causes COVID-19,” according to the CDC. Patients report a wide range of physical and mental health conditions including malaise, fatigue, breathing challenges, cardiovascular abnormalities, migraines, and mental health impairments. There is no standard presentation of or treatment for long COVID. It is a new phenomenon and the ICD-10 code to identify medical claims only became available in October 2021. Also unknown is how long people with long COVID will remain ill, although one study reported that 29 percent of long COVID patients had self-reported symptoms for more than one year. The prevalence of long COVID is equally uncertain with studies finding that the percentage of working age adults with COVID who develop long COVID could be 10 percent, 20 percent, or 33 percent. If we conservatively assume 100 million working age adults have been infected, that implies 10 to 33 million may have long COVID.
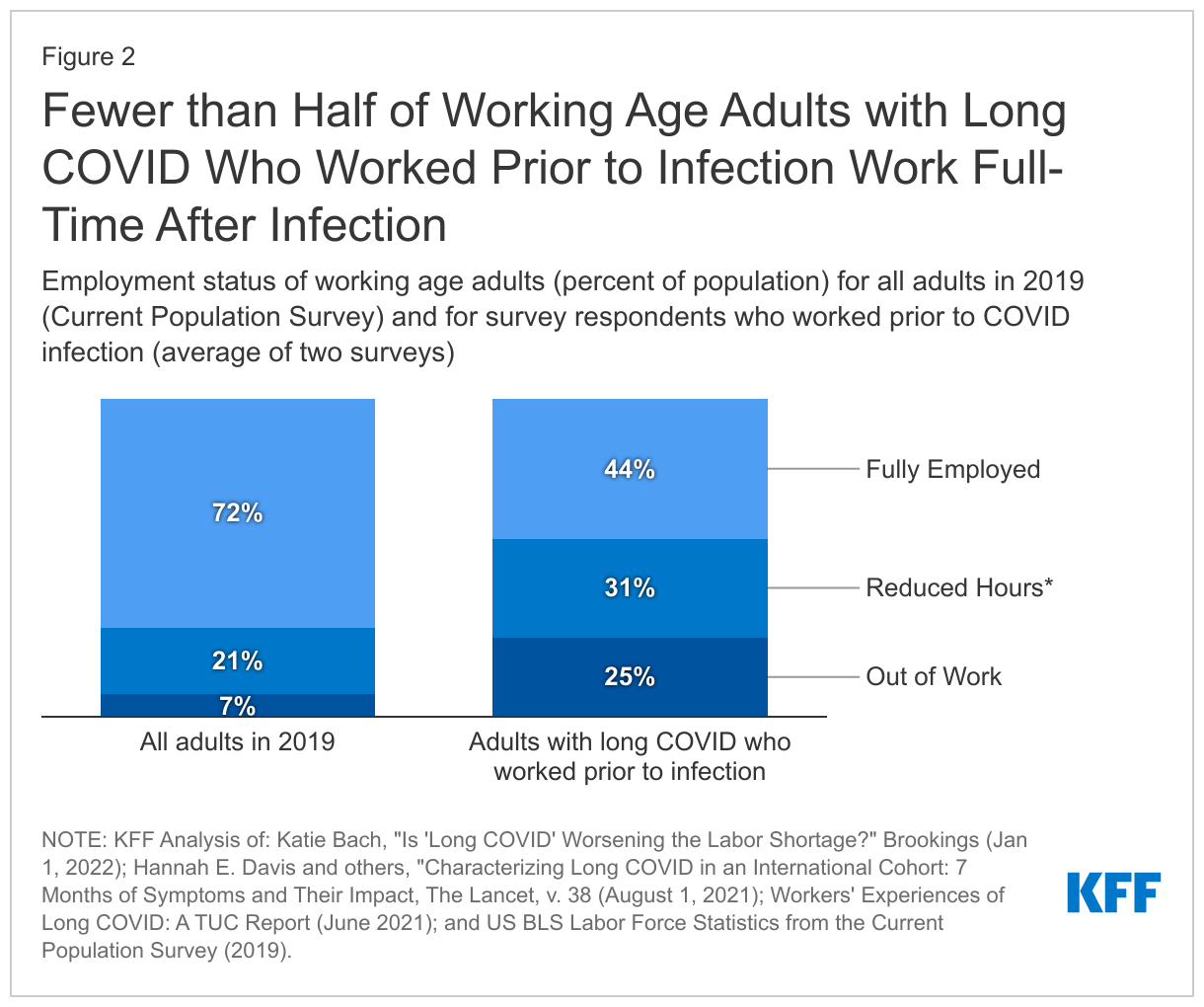
Preliminary evidence suggests there may be significant implications for employment: Surveys show that among adults with long COVID who worked prior to infection, over half are out of work or working fewer hours (Figure 2). Many conditions associated with long COVID—such as malaise, fatigue, or the inability to concentrate—limit people’s ability to work, even if they have jobs that allow for remote work and other accommodations. Two surveys of people with long COVID who had worked prior to infection showed that between 22% and 27% of those workers were out of work after getting long COVID. In comparison, among all working-age adults in 2019, only 7% were out of work. Given the sheer number of working age adults with long COVID, the employment implications may be profound and are likely to affect more people over time. One study estimates that long COVID already accounts for 15 percent of unfilled jobs.
It is too early to have comprehensive data or a clear picture of employment outcomes but there are reports that claims associated with long COVID are rising for disability insurance, workers compensation, and group health insurance. Those higher claims could increase costs for insurers and eventually, employers. It is unclear how long-term these challenges will be and whether health insurance spending will rise because of long COVID. It is also unclear how employment consequences will be spread across industries, but some industries are likely to be disproportionately affected—particularly those with higher rates of initial infection, such as health care.
There may be significant changes in health coverage associated with long COVID. Over 60% of working-age adults have their health insurance coverage through an employer. Changes in employment would therefore have significant effects on people’s sources of health insurance. People who are no longer able to work could eventually lose their existing coverage and would also experience loss of income. Some could newly qualify for help paying for private health insurance through the ACA marketplaces. Others could newly qualify for Medicaid – though eligibility is more limited in the dozen states that have not expanded the program under the ACA. Those with high medical spending could qualify for Medicaid through medically needy programs.
An important question for the future is whether federal disability programs will count long COVID as a disability. The Office of Civil Rights within the U.S. Department of Health and Human Services determined that long COVID can be a disability under the Americans with Disabilities Act if an individual assessment determines that it substantially limits one or more major life activities. Despite the recognition that long COVID can be a disability, to qualify for federal programs, Social Security Disability Insurance (SSDI) and Supplemental Security Income (SSI), applicants must be unable to work and have health conditions that last for at least one year or result in death. At this point, it is unclear how many people with long COVID will qualify for disability benefits under this definition. If people with long COVID quality for federal disability programs, more people will have publicly funded health insurance through Medicare and Medicaid. People who are eligible for SSDI become eligible for Medicare after a 2-year waiting period and people who are eligible for SSI are generally eligible for Medicaid. If people with long COVID are unable to work, federal disability programs could play a key role helping those patients access the health care they need to recover.