Section 1115 Waiver Watch: How California Will Expand Medicaid Pre-Release Services for Incarcerated Populations
On January 26, the Centers for Medicare and Medicaid Services (CMS) approved California’s Section 1115 request to cover a package of reentry services for certain groups of incarcerated individuals 90 days prior to release. This approval is the first to include a partial waiver of the statutory Medicaid inmate exclusion policy, which prohibits Medicaid from paying for services provided during incarceration (except for inpatient services). Justice-involved individuals are disproportionately low-income and often have complex and/or chronic conditions, including behavioral health needs (mental health conditions and/or substance use disorder (SUD)). Reentry services aim to improve care transitions for these high-need Medicaid enrollees upon release and increase continuity of health coverage, prevent disruptions in care, and lead to improved health outcomes. This Waiver Watch summarizes the California approval and examines similar pending requests from 14 additional states to provide pre-release services.
What is the background?
The 2018 SUPPORT Act directed CMS to issue guidance on how waivers can improve care transitions for incarcerated individuals who are otherwise eligible for Medicaid. The SUPPORT Act required the Secretary of Health and Human Services (HHS) to convene a group of stakeholders to help inform the design of a demonstration opportunity to improve care transitions for individuals leaving incarceration. Findings from that convening were summarized in a report from the Office of the Assistant Secretary for Planning and Evaluation (ASPE), and the report includes promising practices and key considerations for the demonstration opportunity such as giving states options to customize the demonstration population, invest in data infrastructure, implement strategic partnerships, and include pre-arrest diversion activities. CMS has indicated that the guidance for the new waiver opportunity is forthcoming and will closely align with the approved approach to pre-release services in California.
States have used Medicaid strategies to help maintain eligibility and coordinate care for individuals transitioning from incarceration. While California is the first state to receive a partial waiver of the inmate exclusion, states can adopt other strategies to coordinate care for incarcerated Medicaid enrollees, such as by suspending (rather than terminating) eligibility for enrollees who became incarcerated and by developing managed care requirements and fee-for-service initiatives related to pre-release care coordination. The Biden Administration has encouraged states to propose waivers that address health-related social needs, expand coverage, and reduce health disparities, including by investing in initiatives for justice-involved populations.
What is included in the California waiver?
California estimates that approximately 200,000 people each year will be eligible to receive pre-release services under the demonstration waiver. While the waiver is complex and includes many provisions, key aspects of the “Reentry Demonstration Initiative” include the following:
- Eligibility based on health needs: Services will be available to all Medicaid-eligible adults who are inmates in state prisons and county jails and meet health criteria, beginning 90 days prior to their expected date of release. The health criteria aim to identify inmates at high risk of adverse health outcomes pre- and post-release, including those with behavioral health needs or other chronic conditions. Also, all inmates of youth correctional facilities will be eligible for services 90 days pre-release, without meeting any clinical criteria.
- Reentry benefit package: The limited benefit package is intended to improve care transitions for individuals upon release and prevent hospitalization as well as adverse outcomes including suicide, overdose, and recidivism. Covered services include case management, physical and behavioral health clinical consultation services, laboratory and radiology services, medications and medication administration, medication-assisted treatment (MAT) for substance use disorder, and Community Health Worker (CHW) services. Upon release, enrollees will also receive covered outpatient prescribed medications and over-the-counter drugs (a minimum 30-day supply, as clinically appropriate) and durable medical equipment (DME).
- Implementation timing and funds: The waiver also includes authority to spend $410 million on pre-release application planning and information technology through California’s “Providing Access and Transforming Health” (PATH) initiative. California will use these funds to provide capacity grants and case management services beginning in April 2024, with the pre-release service package being phased in over two years. California also must provide pre-release education and outreach, along with Medicaid eligibility and enrollment support, to all incarcerated individuals while the demonstration functions.
CMS recognizes that effective implementation of California’s pre-release services program will require forging new partnerships with and providing significant technical assistance to correctional authorities, providers, and community-based organizations. To help ensure access to care upon release and for other Medicaid enrollees, California is also required to increase and (at least) sustain base Medicaid payment rates of at least 80% of Medicare rates for primary care, behavioral health, and obstetrics providers (this requirement is consistent with other states that recently received approvals to address health-related social needs).
What is pending in other states?
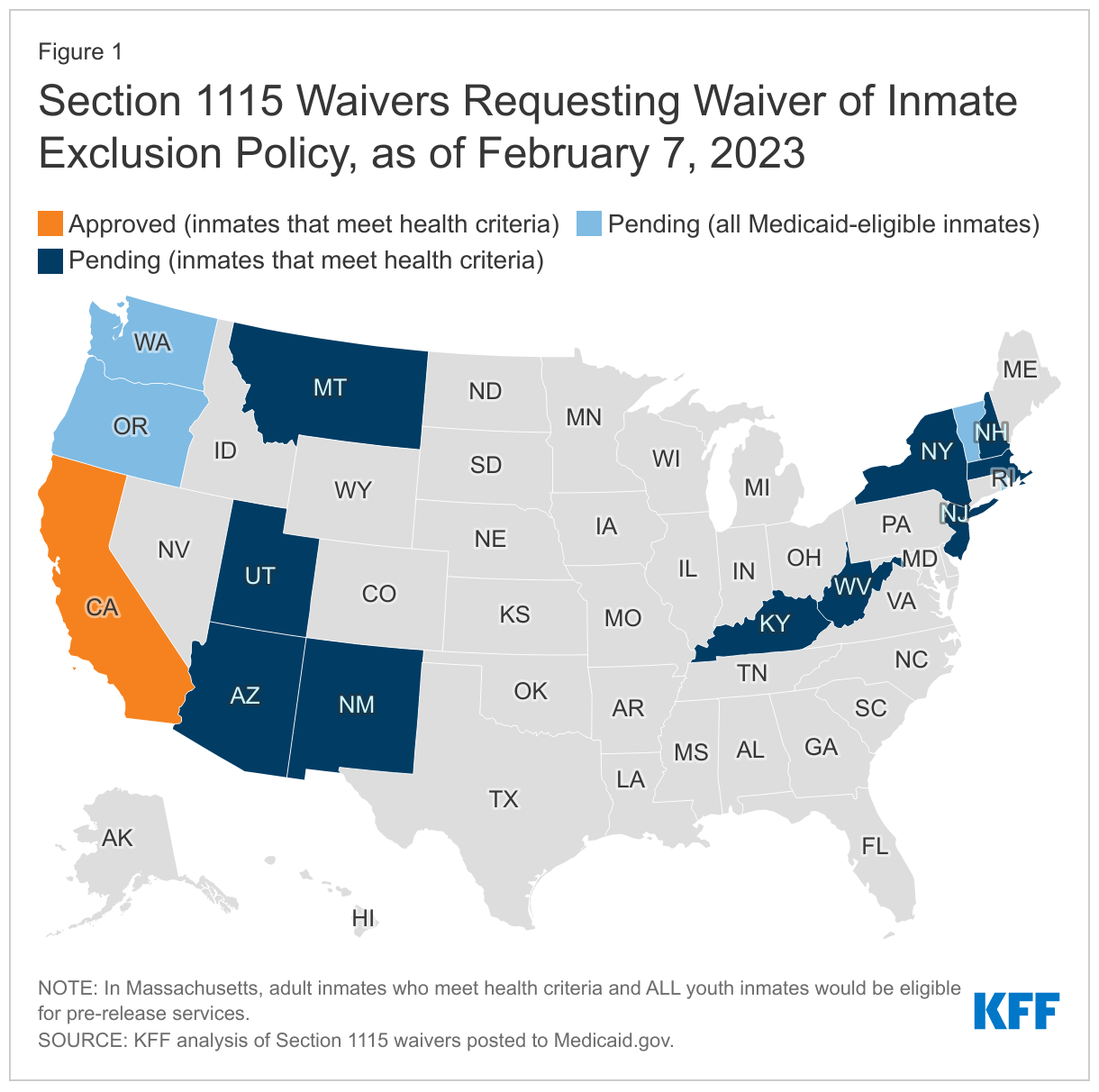
As of February 7, 14 additional states are also seeking partial waivers to the inmate exclusion policy to provide pre-release services to some eligible incarcerated individuals (Figure 1). The parameters of these proposals may change to reflect the California approval and upcoming CMS guidance. Currently, these pending requests vary in scope by pre-release period, eligibility and benefits:
- Pre-release period. Most states (9 out of 15) intend to provide coverage to eligible inmates 30 days prior to release. Of the remaining states, three (New Hampshire, New Jersey, and Vermont) seek to provide coverage between 45 and 90 days prior to release. Kentucky proposes to provide fee-for-service benefits for the duration of an inmate’s commitment and through an MCO beginning 30 days prior to release. The other two states (Oregon and Massachusetts) would cover some inmates throughout the duration of their commitment, while covering other groups for a more limited pre-release period.
- Eligibility. Four states (Oregon, Rhode Island, Vermont, and Washington) are seeking to provide benefits to all inmates of state and county facilities. The remaining states would limit these services to inmates who meet health or risk criteria (frequently related to behavioral health needs).
- Benefits. Four states (Massachusetts, Rhode Island, Utah and Vermont) seek to provide full Medicaid State Plan benefits to eligible inmates during the pre-release period. Oregon proposes to provide full benefits to individuals in jail, while state prison inmates would receive a limited package of care coordination services. The remaining states would provide a limited benefit package for all eligible inmates (typically to include services such as reentry support, enhanced case management, and behavioral health care).
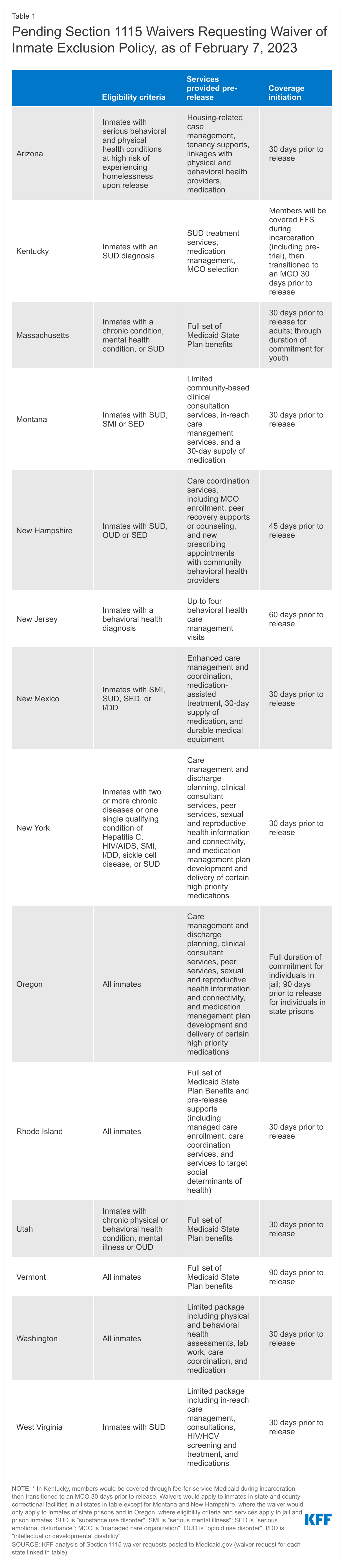
For further state-by-state details on Section 1115 pre-release requests, see Table 1.