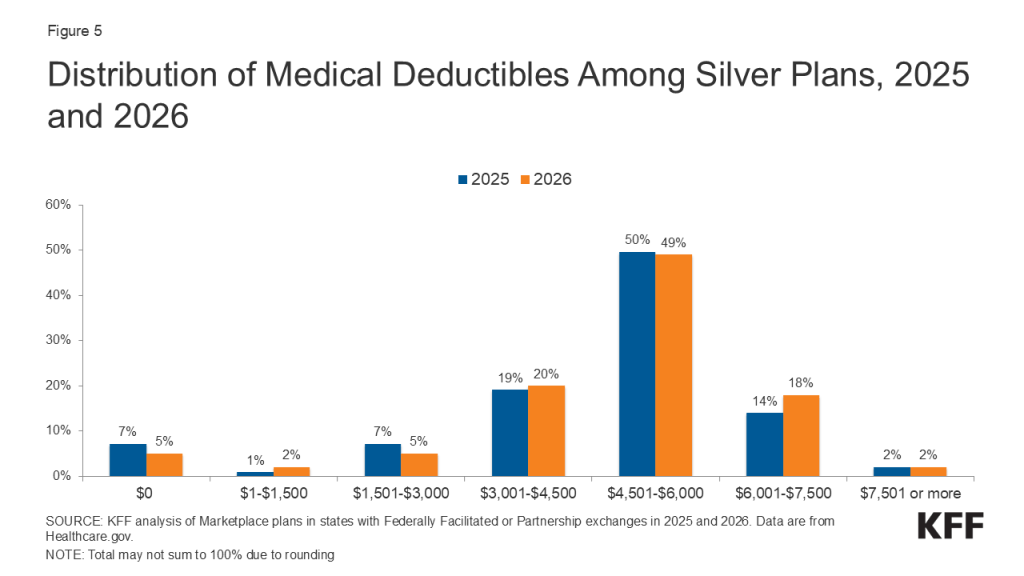Deductibles in ACA Marketplace Plans, 2014-2026
Editorial Note
This page was updated on May 19, 2026 to incorporate new weighting for average ACA Marketplace deductibles in 2014-2016 and 2026.
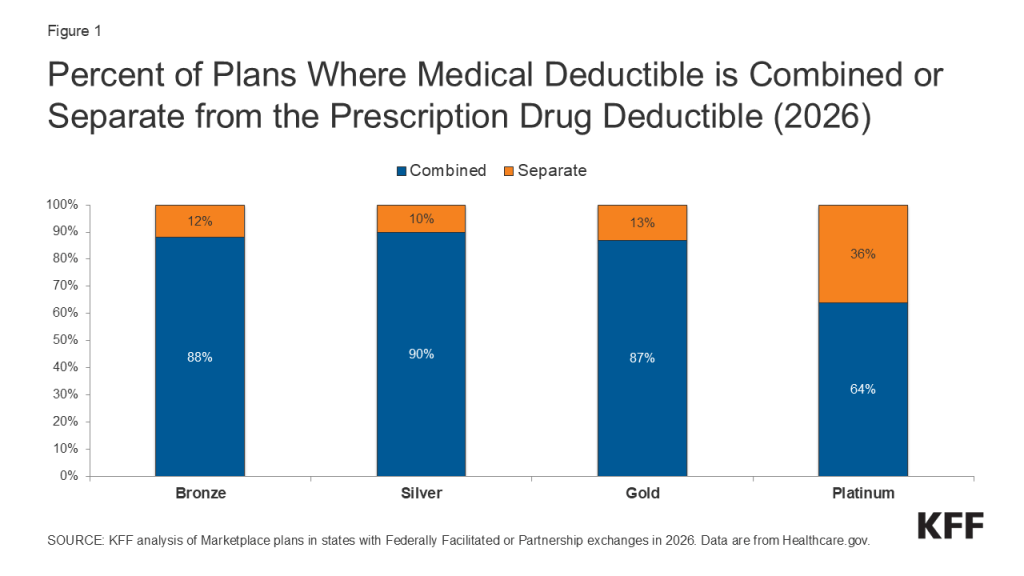
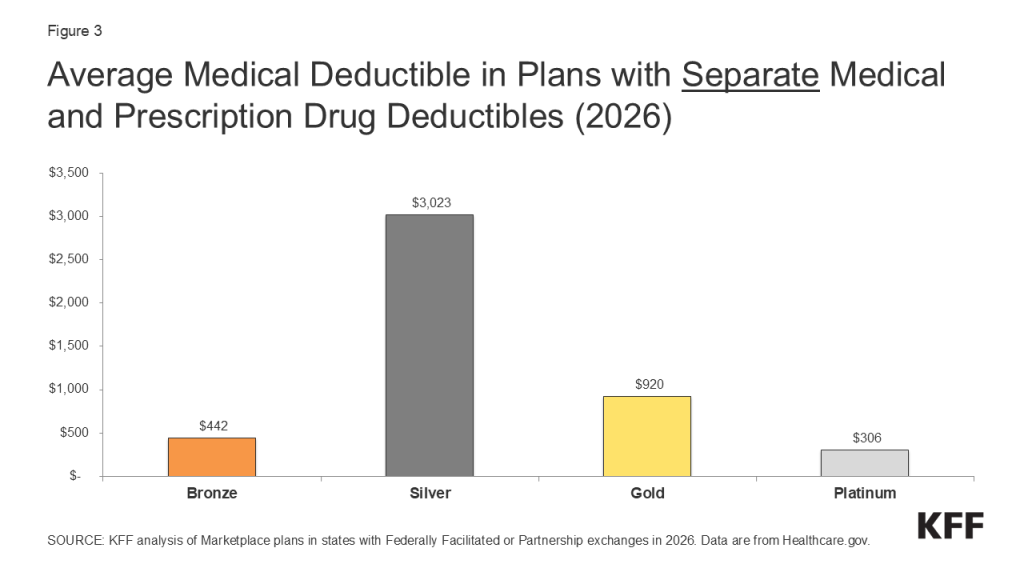
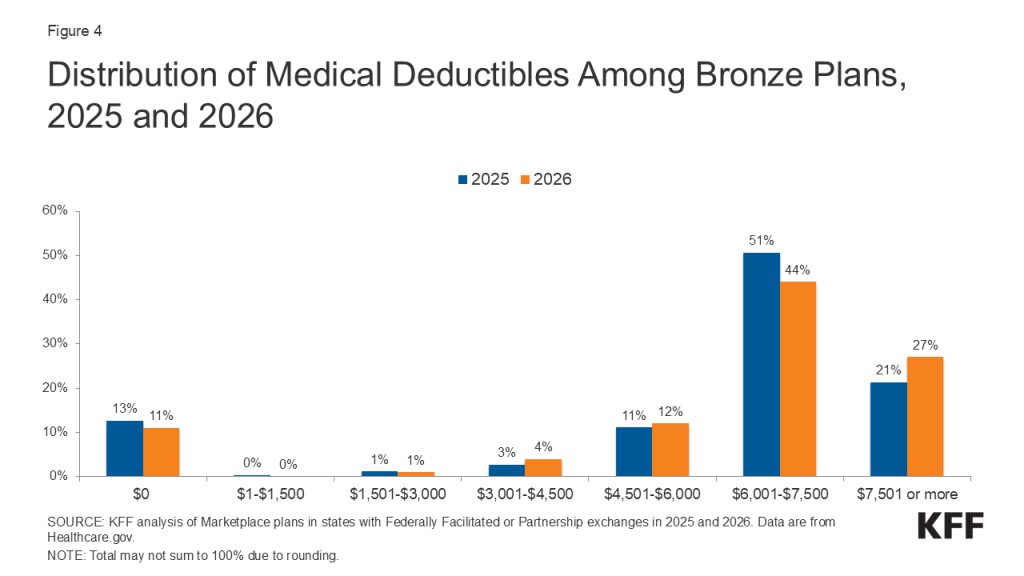
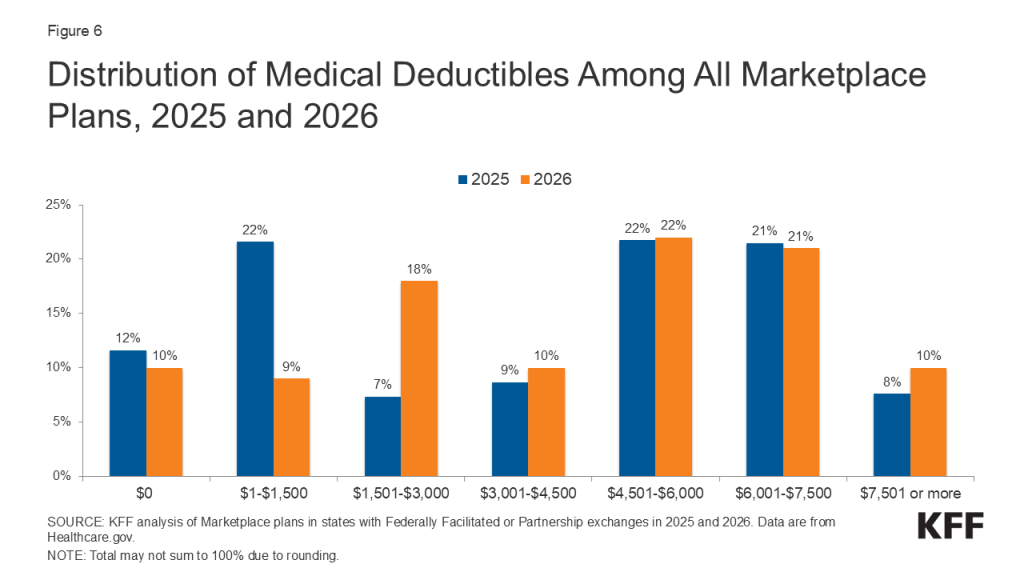
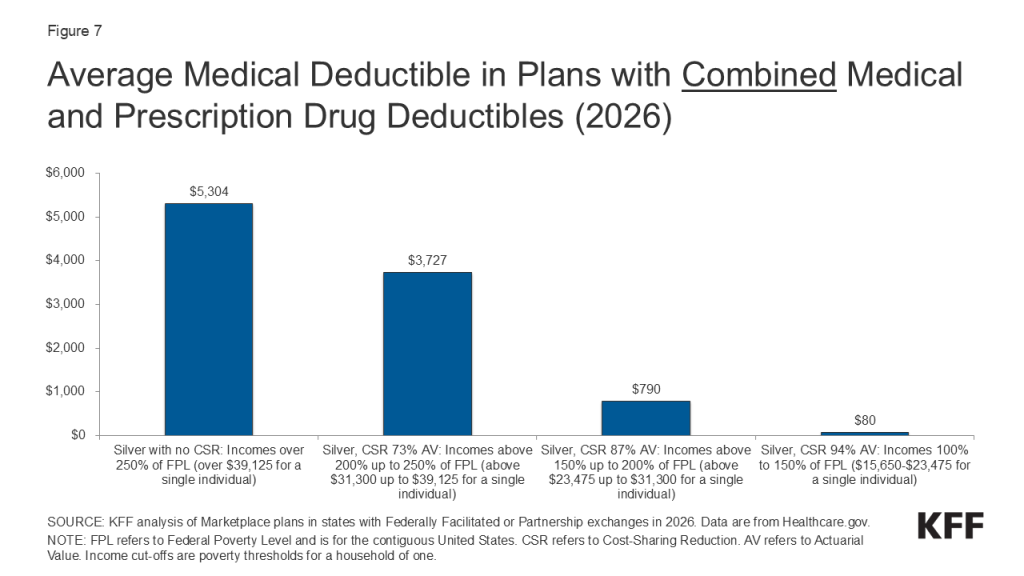
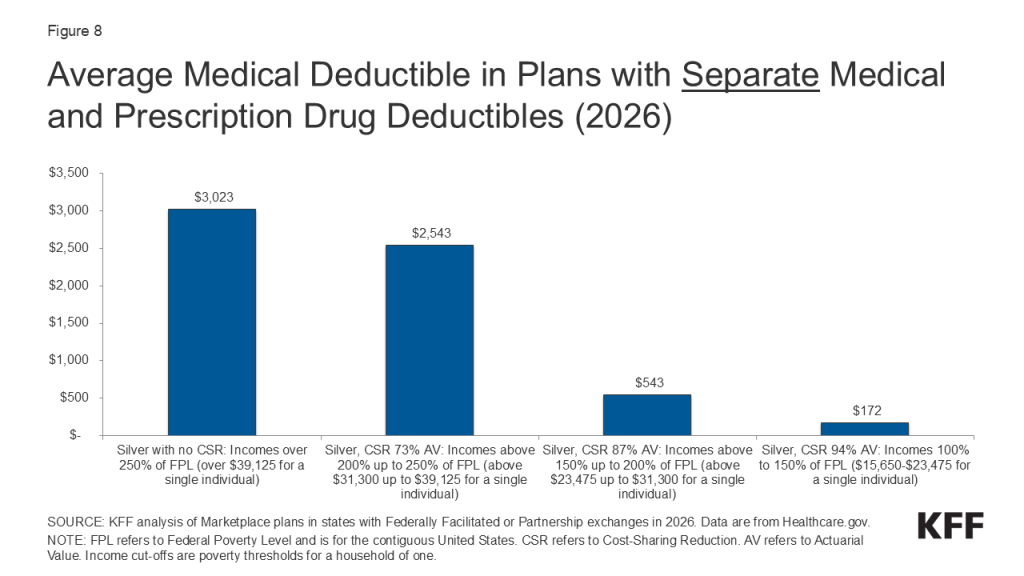
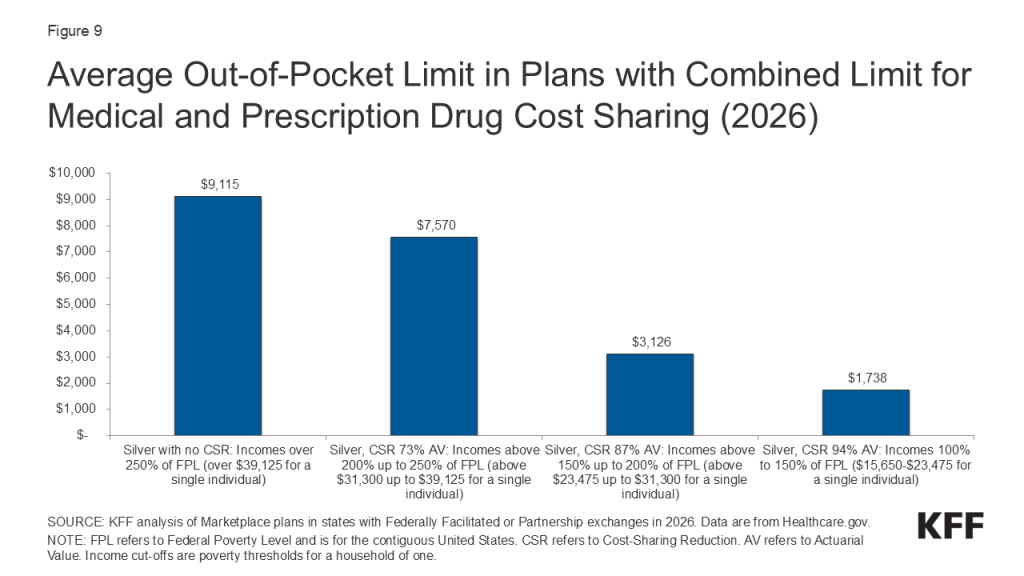
These chart collections provide key data about deductibles and other cost-sharing requirements included in plans sold through the Affordable Care Act (ACA) health insurance marketplaces. Marketplace plans, like most other private health coverage, require enrollees to pay a portion of the cost when they access health services. Cost-sharing can include deductibles, copayments, and coinsurance, though the deductible is a simple and visible measure of how much an enrollee may be expected to pay for major health services. The deductible is the amount an enrollee must pay toward the cost of in-network covered services before the plan will start paying for most types of care. Some plans have a separate deductible amount for medical care and prescription drugs. Under the Affordable Care Act, private plans are required to pay the full cost of certain in-network preventive services (even before the enrollee has met the deductible amount). Marketplace plans are categorized into “metal levels” based on deductible and other cost-sharing amounts.
Cost-Sharing for Plans Offered in the Federal Marketplace, 2026(.ppt)
Download Prior Years’ Analyses
Methods
Information on plan cost-sharing provisions for the plans offered in federally-facilitated and partnership exchanges was downloaded from HealthCare.gov. Distinct plans from the landscape file were analyzed to calculate the average deductibles for individuals. A distinct plan is defined by having a unique state, issuer, metal level, and cost sharing design combination. In 2014 and 2015, a distinct plan took into consideration the plan marketing name.
Simple averages and distributions of the available plans are shown, and neither are weighted by enrollment. Information for “expanded bronze” and “bronze” plans are reported together.
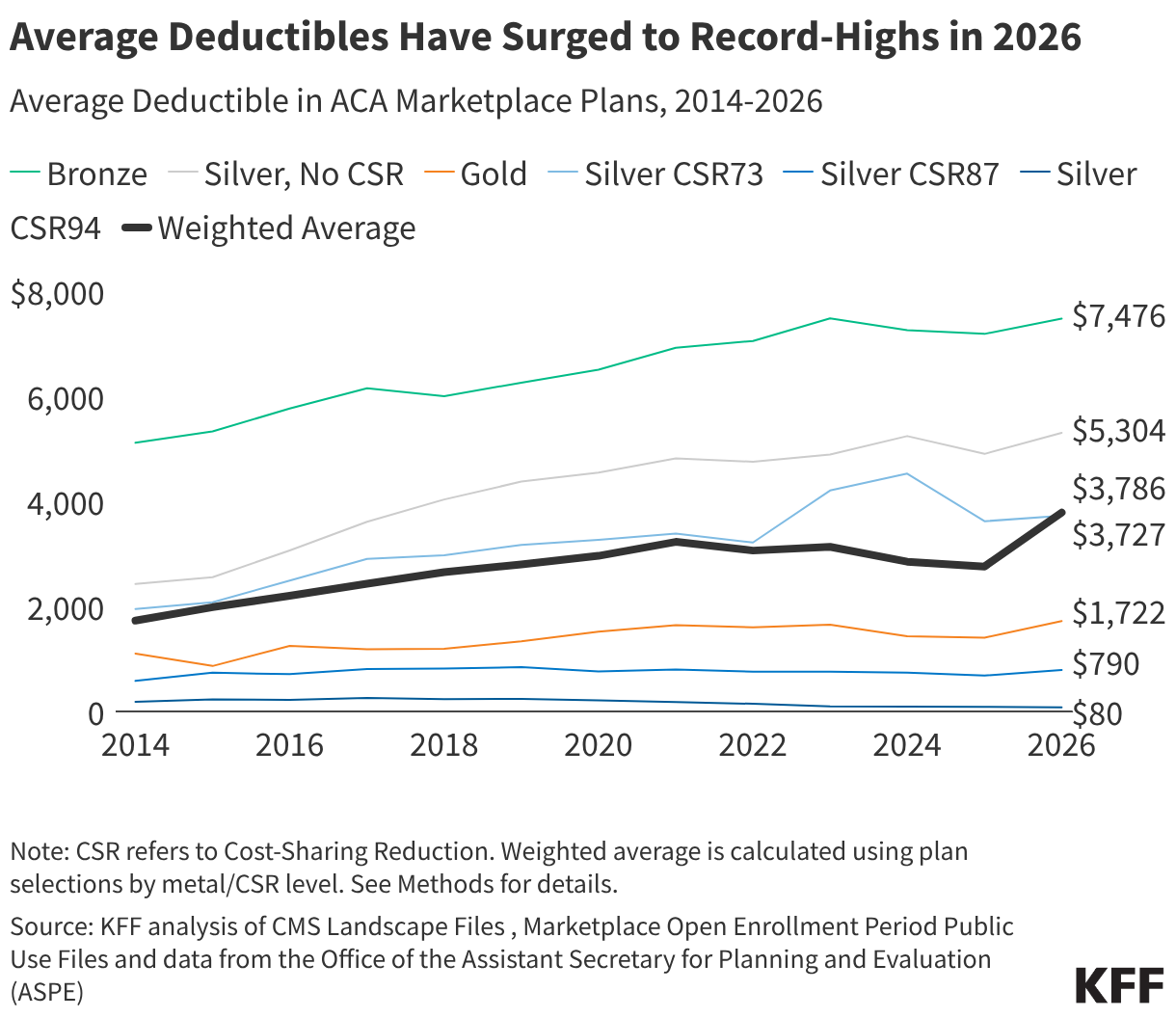
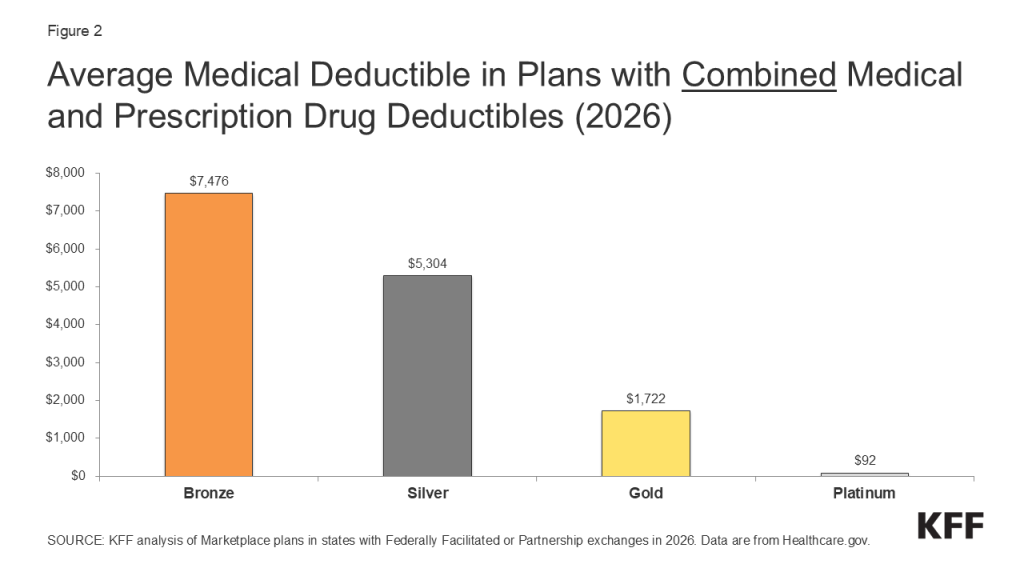
Average deductible over time by plan type trends the individual medical deductible in plans with combined medical and prescription drug deductibles for only plans offered in the federally facilitated Marketplace. Plans included were not adjusted for states transitioning to state-based exchanges. The weighted average was calculated using plan selection data at the metal and CSR (or FPL) level from Marketplace Open Enrollment Period Public Use Files and data from the Office of the Assistant Secretary for Planning and Evaluation (ASPE), excluding catastrophic and platinum plans. Share of CSR and non-CSR variants among those selecting silver plans for 2017 and earlier were from the 2017 Open Enrollment income distribution among silver plan selections; consumers selecting a silver plan with income ≥100% to ≤150% of FPL , >150% to ≤200% of FPL , and >200% to ≤250% of FPL were assumed to have selected CSR94, CSR87, and CSR73 variants, respectively. All other years, including 2026, used plan selection, metal level, and CSR distributions from that year.