How Health Insurers and Brokers Are Marketing Medicare
Executive Summary
Most of the 65 million beneficiaries who receive health insurance coverage through the federal Medicare program are enrolled in some form of private plan. In 2023, 31 million Medicare beneficiaries are enrolled in Medicare Advantage (Medicare Part C) plans administered by private health insurers. The other 34 million beneficiaries are in traditional Medicare, including 22 million beneficiaries who are enrolled in a Medicare Part D prescription drug plan offered by private sponsors, and more than 14 million who have Medicare supplemental insurance (Medigap) offered by private insurers (traditional Medicare beneficiaries may be enrolled in a Part D plan, a Medigap plan, or both).
Private plan offerings have grown in recent years, most notably in the Medicare Advantage market. More Medicare Advantage plans are available in 2023 than in any prior year. Medicare Advantage enrollment has doubled since 2010, due in part to extensive marketing efforts and the draw of extra benefits and attractive cost features. Each year, beginning on October 1st, insurers, as well as brokers and other third-party entities, are permitted to begin marketing Medicare Advantage for the annual open enrollment period for coverage in the following year. The open enrollment period for Medicare Advantage and Medicare Part D plans runs from October 15th through December 7th. Television ads are one of many marketing activities used by insurers, brokers and other third-party entities to boost enrollment.
Recently, the Centers for Medicare and Medicaid (CMS) has reported a steep rise in beneficiary complaints related to the marketing of Medicare Advantage and Part D plans. Many of these complaints have centered on the activities of brokers and other third-party entities, referencing misleading claims and aggressive sales tactics. Concerns raised by the National Association of Insurance Commissioners and in a report released by the majority staff of the U.S. Senate Committee on Finance have also called attention to this issue. In response, CMS published updated regulations, effective June 2022, mandating stricter oversight of these third parties by the insurers they represent. Additional CMS requirements intended to curtail misleading marketing activities came into effect in June 2023, and will apply to the open enrollment period for 2024 coverage and beyond.
To capture the state of television marketing activities and consider the implications for people with Medicare, KFF analyzed ad data compiled by the Wesleyan Media Project, that were obtained from Vivvix (formerly Kantar) CMAG, a data analytics and consulting firm, and were coded by the Wesleyan Media Project in collaboration with KFF. The data set included all English-language TV ads that aired across national and local markets on broadcast television or national cable, from October 1st, 2022, through December 7th, 2022, the period that includes the Medicare open enrollment period for coverage in 2023. (see Methods).
Key Takeaways:
- TV airways were flooded with ads for Medicare plans. Nearly 650,000 airings of Medicare ads appeared during the nine weeks of advertising, more than 9,500 airings per day. Most of these ads were aired in local media markets. While most TV ads were sponsored by health insurers, about one in every five TV ads were sponsored by brokers and other third-party entities, such as marketing firms.
- TV ads for Medicare Advantage comprised more than 85% of all airings for the open enrollment period for 2023. The remaining ads focused on other types of plans, such as Medigap and stand-alone Part D prescription drug plans, or promoted the open enrollment period more generally. Medicare Advantage ads were disproportionately sponsored by health insurers who offer plans that comprise a relatively small share of Medicare Advantage enrollees.
- TV ads for Medicare Advantage often showed images of a government-issued Medicare card or urged viewers to call a “Medicare” hotline other than the official 1-800-Medicare hotline. More than a quarter of all airings (27%) included a government-issued Medicare card or image that resembled it, including 28% of insurer-sponsored airings and 21% of airings sponsored by brokers and other third-party entities, a trend that CMS has flagged as potentially misleading to beneficiaries. Roughly 16% of airings featured a privately-run phone line described as a “Medicare” hotline, most of which were sponsored by brokers and other third-party entities.
- Some ads suggested that people with Medicare miss out on benefits to which they are entitled if they are not enrolled in a Medicare Advantage plan. These TV ads were more common among ads sponsored by brokers and other third-party entities than those sponsored by health insurers, and used language that implied viewers were “missing out” on benefits they were “entitled to,” or receiving incomplete coverage under Medicare Parts A and B if they were not enrolled in a Medicare Advantage (Part C) plan
- The vast majority of Medicare Advantage ad airings touted low costs and extra benefits, while few mentioned quality ratings. Nearly all Medicare Advantage ad airings emphasized extra benefits, such as dental, vision, and hearing (92%) or the potential for lower out-of-pocket spending (85%). Airings sponsored by brokers and other third-party entities often (67%) promoted the potential for enrollees to get money back in their Social Security check (or lower their Medicare Part B premium). Few airings (4%) mentioned quality star ratings.
- Medicare Advantage ad airings often featured active seniors engaged in physical activities, but rarely showed people who appeared to have a serious health problem or visible disability. One in four Medicare Advantage ad airings (26%) showed seniors taking part in activities such as hiking or yoga, but few included people with visible disabilities (4%) or the appearance of serious illness (1%) for whom health insurance coverage and choice of providers may be a high priority.
- TV ads sponsored by brokers and other third-party entities used celebrity endorsements more often than health insurers to promote Medicare Advantage. Celebrities, such as actors, athletes, and politicians, appeared in more than half of Medicare Advantage ad airings sponsored by brokers and other third parties (55%), but rarely appeared in airings sponsored by insurers (3%). Familiar figures included Joe Namath, Lionel Richie, William Shatner, and JJ Walker. Joe Namath was featured more than any other celebrity, appearing in nearly 56,000 airings.
Medicare beneficiaries have a wealth of choices for their health insurance coverage. While beneficiaries may appreciate the ability to select from multiple options, the variable costs, benefits, provider networks, and other characteristics of Medicare Advantage plans make the decision complex, especially in light of the barrage of advertising. Additionally, information about coverage under traditional Medicare is rarely included in television ads, leaving beneficiaries with an incomplete view of their coverage options and the tradeoffs among them. While CMS has issued new rules to address concerns about aggressive and misleading marketing tactics, ongoing monitoring and resources independent of commercial interests could help to improve beneficiary decision-making.
This work was supported in part by Arnold Ventures. KFF maintains full editorial control over all of its policy analysis, polling, and journalism activities.
Jeannie Fuglesten Biniek, Alex Cottrill, Nolan Sroczynski, Meredith Freed and Tricia Neuman are with KFF. Breeze Floyd, Laura Baum, and Erika Franklin Fowler are with the Wesleyan Media Project. We thank Markus Neumann, Jielu Yao (Wesleyan University) and Sarah Gollust (University of Minnesota). We also thank the numerous undergraduate student research assistants at Wesleyan University for their efforts on this project.
Report
Introduction
During the annual Medicare open enrollment period that runs from October 15th through December 7th, Medicare beneficiaries can review the coverage options available in their area and make changes for the upcoming year. Drawn by the prospect of strong financial performance, buoyed by generous payments from the federal government, many insurers have expanded their Medicare Advantage offerings in recent years. In 2023, Medicare beneficiaries can choose from an average of 43 Medicare Advantage plans, offered by 9 different insurers, the highest number ever available. Traditional Medicare beneficiaries selecting prescription drug coverage can choose from an average of 24 stand-alone Part D plans.
Plans rely on TV advertising, among other marketing activities, to attract and retain enrollees during the open enrollment period. Recent years have seen an increase in print and television ads from third-party marketing organizations, such as agents and brokers, lead generation businesses, and media firms. At the same time, the Centers for Medicare and Medicaid Services (CMS) has reported a steep rise in beneficiary complaints related to the marketing of private Medicare plans, from less than 16,000 in 2020 to nearly 40,000 in the first eleven months of 2021, many of them centered on the marketing activities of these third-party entities.
In May 2022, the National Association of Insurance Commissioners (NAIC) sent a letter to Congress urging action on this issue, citing concerns about misleading claims and aggressive sales tactics. The following November, the majority staff of the Senate Finance Committee released a report detailing complaints and associated marketing materials from key stakeholders across 14 states. In response, CMS released new regulations, effective June 2022 and June 2023, tightening restrictions on health insurers and third parties who market Medicare Advantage and Part D plans.
This report describes the content and characteristics of all English-language TV ads focused on Medicare that aired on broadcast television or national cable between October 1, 2022 and December 7, 2022. Ads were obtained by the Wesleyan Media Project from Vivvix (formerly Kantar) CMAG, a data analytics and consulting firm, and coded by trained undergraduate student coders using an instrument developed jointly by the Wesleyan Media Project and KFF. The KFF analysis includes 1,267 unique ads that aired 643,852 times during the advertising period and focuses mainly on Medicare Advantage ads, the dominant Medicare plan type advertised during the period (see Methods).
Background
Trends in Medicare Coverage
More than 65 million people receive health insurance coverage through the federal Medicare program. Increasingly, this coverage is provided by private companies who contract with the federal government to offer Medicare Part A and Part B covered services (Medicare Advantage or MA), Part D prescription drug plan coverage (PDP), or both (MA-PD). Medicare Advantage enrollment has doubled since 2010, covering over half (31 million people) of eligible Medicare beneficiaries in 2023. Among traditional Medicare beneficiaries, 22 million are enrolled in a stand-alone PDP and most have some form of private supplemental coverage, including more than 14 million who purchase a private Medigap supplement policy.
The growth in Medicare Advantage enrollment is due, in part, to the extra benefits and attractive cost features offered by most Medicare Advantage plans. Virtually all Medicare Advantage plans offer some benefits not included in traditional Medicare, such as coverage of dental, vision, or hearing services. Additionally, unlike traditional Medicare, which places no cap on out-of-pocket spending for hospital or physician services, Medicare Advantage plans are required to set out-of-pocket limits for services covered by Parts A and B. At the same time, Medicare Advantage plans often have restrictions, such as prior authorization and referral requirements, rarely used in traditional Medicare, and most include networks that set limits on which providers enrollees may see. Close to 60% of Medicare Advantage beneficiaries are enrolled in HMO plans that typically do not cover out-of-network services.
Marketing Complaints and Regulatory Response
The report from the majority staff of the Senate Finance Committee documents numerous examples of beneficiary complaints about marketing practices used by Medicare Advantage insurers, as well as brokers and other third-party entities, including false or misleading information about plan costs and available benefits, concerns which have been raised by the National Association of Insurance Commissioners as well. For example, advertisements promising lower Part B premiums or higher Social Security checks were a common source of complaints. States frequently reported incidents in which agents or brokers used this claim to attract potential enrollees, even when advertising in service areas where no such plans were available, or when enrolling beneficiaries in a plan that offered this benefit would be an otherwise poor fit for their needs. In 2023, just 17% of Medicare Advantage plans offer a rebate toward the Part B premium.
Likewise, CMS has raised concerns that the prominent use of the word “Medicare” in company names or headers and images of the Medicare card or logo in print and TV ads creates confusion for beneficiaries and may lead them to believe that these organizations are speaking on behalf of the Medicare program. Focus groups conducted by KFF in the fall of 2022, suggest that beneficiaries find these ads to be misleading, often reporting uncertainty about who had sponsored the ads they saw on TV and whether they were endorsed by the Medicare program or the federal government.
CMS has moved to address these issues in several ways. Regulations that went into effect in June 2022, and apply to all Medicare Advantage and Part D ads discussed in this analysis, broaden the definition of third-party marketing organizations, mandate greater oversight by health insurers of the third parties who represent them, and require third parties to include a standard disclaimer in all communications and marketing materials informing beneficiaries that they do not represent every plan available in their area and advising them to contact official CMS resources for a complete list of their options (though CMS does not specify whether or not this disclaimer may be featured in fine print). In April 2023, CMS finalized additional requirements to address misleading marketing practices that will apply to the upcoming Medicare open enrollment period that begins in October 2023, for coverage in 2024. (See Appendix for details.)
TV Ads For the 2023 Medicare Open Enrollment Period
Key Takeaways:
- TV airways were flooded with ads for Medicare plans.
- TV ads for Medicare Advantage comprised more than 85% of all airings for the open enrollment period for 2023.
- TV ads for Medicare Advantage often showed images of a government-issued Medicare card or urged viewers to call a “Medicare” hotline other than the official 1-800-Medicare hotline.
- Some ads suggested that people with Medicare miss out on benefits to which they are entitled if they are not enrolled in a Medicare Advantage plan.
- The vast majority of Medicare Advantage ad airings touted low costs and extra benefits, while few mentioned quality ratings.
- Medicare Advantage ad airings often featured active seniors engaged in physical activities, but rarely showed people who appeared to have a serious health problem or visible disability.
- TV ads sponsored by brokers and other third-party entities used celebrity endorsements more often than health insurers to promote Medicare Advantage.
TV airways were flooded with ads for Medicare plans.
There were 643,852 airings of English-language Medicare ads run on broadcast television and national cable between October 1, 2022, and December 7, 2022, an average of more than 9,500 airings per day, more than were seen for any individual Healthcare.gov open enrollment period between 2013 and 2018. Just over 40,000 Spanish-language airings (not included in our analysis) bring the total number of Medicare-related airings close to 690,000.
Medicare ads were most common during the weekday afternoons. Across the top 20 markets, viewers of programs aired on Fox affiliates saw an average of at least 6 ads per day, viewers of programs aired on ABC and NBC affiliates saw an average of at least 5 ads per day and viewers of programs aired on CBS saw an average of at least 4 ads per day each weekday afternoon between October 1, 2022 and December 7, 2022 (data not shown).
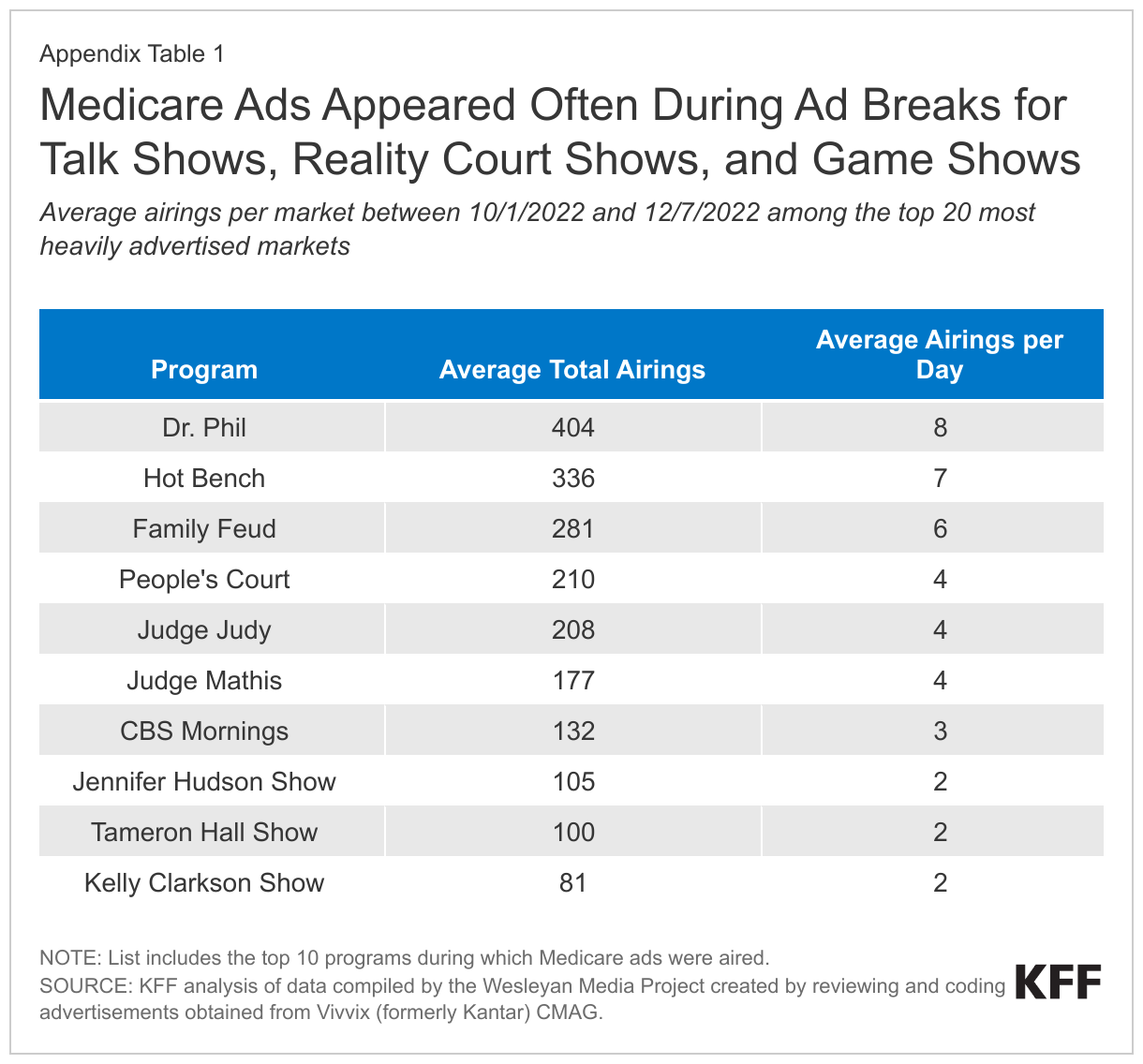
The most common television programs during which Medicare ads were aired included talk shows, reality court shows and game shows. For example, across the top 20 markets, regular viewers of Dr. Phil saw an average of 404 Medicare ads, or 8 ads per day that were directed at the open enrollment period. Regular viewers of Hot Bench saw 336 ads on average, or 7 ads per day, and regular viewers of Family Feud saw 281 ads on average, or 6 ads per day (Appendix Table 1).
Local news broadcasts also often included commercials for Medicare plans. On December 1st, the day with the highest number of airings, a person watching News 5 at 5pm on ABC in Cleveland would have seen nine Medicare ads during the one-hour broadcast. Likewise, a person watching WCCO Mid-Morning on CBS in Minneapolis would have seen seven ads during the hour, and a person watching Eyewitness News 4 at Midday on NBC in Albuquerque would have seen six in the hour (data not shown).
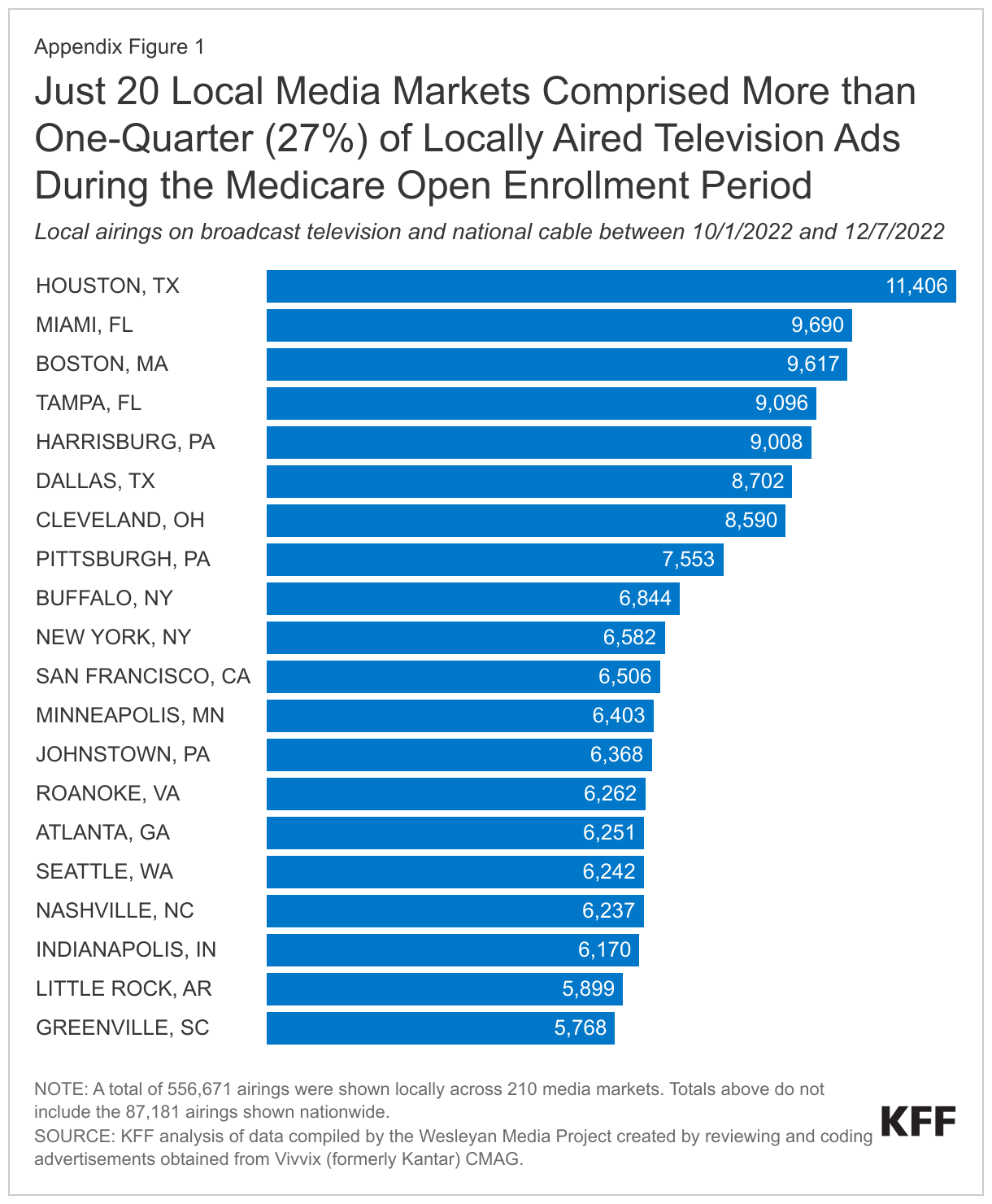
Most Medicare ads aired in local media markets rather than nationally. Of the 643,852 Medicare ad airings analyzed, the vast majority (86%) aired locally, while 14% aired nationally. The targeting of TV ads to local media markets likely reflects a strategy to compete and grow enrollment in specific regions and service areas. (See Appendix for details.)
While health insurers sponsored the majority of Medicare TV ad airings, brokers and other third-party entities had a significant presence, especially with ads that aired nationally. Roughly 73% of all Medicare ad airings (468,808) were sponsored by health insurers, while more than one in five (21%, 135,699) were sponsored by brokers and other third-party entities. Just 3% (18,321) were sponsored by the Department of Health and Human Services or other government agency (Figure 1). Brokers and other third parties relied more on national airings than local markets, accounting for 50% of national airings but just 16% of all local airings.
Roughly 3% (21,024) of all Medicare ad airings did not identify the organization who sponsored the ad. Among national airings, nearly one in ten did not include this information, a pattern that may reflect the larger share of national ads sponsored by brokers and other third parties, who may have less to gain from brand recognition.
TV ads for Medicare Advantage comprised more than 85% of all airings for the open enrollment period for 2023.
Of the 643,852 airings of Medicare ads that ran during the nine-week advertising period for open enrollment for coverage in 2023, 556,068 (86%) promoted Medicare Advantage. Many of these airings also mentioned Part D benefits, but a review of the top 150 most-frequently aired ads (representing more than 80% of all Medicare ad airings) showed that nearly all of these were marketing Medicare Advantage plans that included Part D coverage, rather than offering stand-alone Part D plans as a separate product. Of the remaining 87,784 airings, 7,790 (1%) promoted Medigap plans and 465 (less than 1%) promoted stand-alone Part D plans with no mention of Medicare Advantage. Another 32,692 airings (5%) promoted multiple types of plans, while 46,837 (7%) did not mention any type of plan, instead offering general information on the open enrollment period or counseling on Medicare plan choice (Figure 2).
The emphasis on Medicare Advantage matches trends in Medicare enrollment. As of 2023, just over half of all eligible Medicare beneficiaries receive their Medicare Part A and Part B benefits through a Medicare Advantage plan, a twofold increase in the past decade that has outpaced the more modest growth seen in Medigap enrollment. Likewise, enrollment in stand-alone Part D plans has declined as a growing share of beneficiaries enroll in Medicare Advantage plans that include prescription drug coverage. At the same time, a KFF analysis of private Medicare advertising for the 2008 open enrollment period demonstrated that insurers have devoted the largest share of their advertising resources to Medicare Advantage plans for some time.
The remaining discussion is focused on Medicare Advantage, as these ads made up the vast majority of Medicare ad airings for the open enrollment period.
Four of every five Medicare Advantage ad airings were sponsored by health insurers, with the remaining sponsored by brokers and other third-party entities, such as marketing companies. Among the 556,068 ads promoting Medicare Advantage, health insurers sponsored a majority (79%) of ad airings while brokers and other third-party entities sponsored 19%. The remaining 2% of sponsors were not readily identifiable. Ads sponsored by brokers and other third parties rarely listed the specific Medicare Advantage organizations they represented or the plans they offered, though many advertised specific benefits and plan features that might be available. Brokers may contract with multiple insurers, and offer plans with varying benefits and costs, across many service areas, which may lead to confusion if beneficiaries are unaware which of the plan features advertised are available where they live. Further, brokers have a financial incentive to steer people towards Medicare Advantage plans over other coverage options. In the 2023 plan year, brokers receive $601 per new enrollee in most Medicare Advantage plans, substantially higher than for new enrollees in most Part D plans ($92). Though comparable data do not exist for Medigap plans, brokers report substantially lower commissions for Medigap enrollment.
Though not applicable to these ads, new regulations from CMS came into effect in June 2023 which prohibit brokers and other third parties from advertising specific plans or plan features without clearly identifying the insurers that offer them. Further, all groups are prohibited from marketing benefits in service areas where those benefits are not available (see Appendix for details).
UnitedHealthcare and Humana comprise nearly half of Medicare Advantage enrollment but sponsored just 20% of insurer-sponsored ad airings. Many TV ad airings promoting Medicare Advantage were sponsored by health insurers that enroll a relatively small share of Medicare Advantage enrollees. While UnitedHealthcare and Humana together comprise nearly 50% of Medicare Advantage enrollment in recent years, these two insurers sponsored less than 20% of airings for Medicare Advantage plans. In contrast, three insurers accounted for a larger share of airings than enrollment: Blue Cross Blue Shield affiliates (26% of airings vs. 14% of enrollment), Centene (12% vs. 4%), and Cigna (9% vs. 2%). Roughly one in five airings (24%) came from insurers that account for less than 2% of Medicare Advantage enrollment each, and 16% as a group (Figure 3). Despite rapid growth, Medicare Advantage enrollment remains concentrated among a small group of firms, and insurers with a smaller footprint in the Medicare Advantage market may rely more heavily on TV advertising to promote their plans and expand market share.
TV ads for Medicare Advantage often showed images of a government-issued Medicare card or advertised a “Medicare” hotline other than 1-800-Medicare.
Over one in four ad airings (27%) promoting Medicare Advantage showed a government-sponsored Medicare card or an image that resembled it, and 16% included a phone number other than 1-800-Medicare that was described as a “Medicare” hotline. Both CMS and the Senate Finance Committee have expressed concern that the use of the Medicare name, logo, or card in private marketing materials could confuse beneficiaries and lead them to believe they are contacting an official government resource. New regulations from CMS aim to address this issue by prohibiting the use of the Medicare card, except for educational purposes (see Appendix for details).
The Medicare card or a similar image appears on screen in more than one-quarter of ad airings for Medicare Advantage. Images of the Medicare card, or something that closely resembles it, appeared in more than one-quarter (27%) of all ad airings for Medicare Advantage, including 28% of insurer-sponsored airings and 21% of airings sponsored by brokers and other third-party entities. Some of these framed the screen with a red, white, and blue border that resembles the Medicare card design, in some instances, for the duration of the airing.
Though not applicable to these ads, new regulations, which will apply to the upcoming open enrollment period in October 2023, prohibit misleading use of the Medicare name, logo, or card in private marketing and communication materials, or any use without prior approval from CMS. CMS has stated that it will approve use for educational purposes only, such as a graphic showing beneficiaries how to tell the difference between their federally-issued Medicare card and their insurer-issued Medicare Advantage plan card. However, it is unclear whether images that are similar, but not identical, to a Medicare card will still be permitted in marketing materials, such as the use of a Medicare card design to frame the screen.
Most Medicare Advantage ad airings sponsored by brokers and other third parties featured a “Medicare” hotline that is not the official government-sponsored 1-800-Medicare hotline. A large majority of Medicare Advantage airings sponsored by brokers and other third-party entities (83%) featured a “Medicare” hotline other than the 1-800-Medicare line run by the federal government (Figure 4). These were often described using general names such as a “Medicare Helpline,” “Medicare Benefits Support Line,” or “Medicare Benefits & Questions Line,” with no reference to a specific company name. In contrast, airings sponsored by health insurers rarely included this type of “Medicare” hotline, instead directing viewers to call their own agents (data not shown). Virtually no ad airings promoting Medicare Advantage mentioned 1-800-Medicare, the official Medicare phone number, outside of fine print.
Among airings sponsored by brokers and other third parties, 19% included both an image of the Medicare card and mention of a privately-run “Medicare” hotline, increasing the possibility that beneficiaries will believe that the ad and its contents were sponsored by an official government agency.
VIDEO: Medicare Advantage ads often showed images of a government issued Medicare card or urged viewers to call a “Medicare” hotline other than 1-800-Medicare.
Focus groups conducted by KFF in the fall of 2022 suggest that beneficiaries are often overwhelmed by the volume and complexity of choices available to them, yet few make use of official Medicare resources such as 1-800-Medicare. Airings sponsored by brokers and other third parties often referenced this volume of choices, encouraging beneficiaries who felt “overwhelmed” or “confused” by their coverage options to call their privately-operated “Medicare” hotline for advice.
Under current rules that became effective in June 2022, and are applicable to the period examined, ads sponsored by brokers and other third-party entities are required to include a disclaimer explaining that they do not represent every plan available in a service area and advising beneficiaries to call 1-800-Medicare for a complete list of their coverage options. While this disclaimer was included in the subset of third-party airings we reviewed, it was often shown for just a few seconds or written in small font, potentially making it difficult for viewers to read.
In some cases, ads advised callers against giving their personal information to national hotlines or “1-800 numbers,” suggesting that local experts were more trustworthy. While these messages may be aimed at other broker-sponsored hotlines that operate at the national level, they may also discourage viewers from calling 1-800-Medicare for additional information.
Some ads suggest that people with Medicare miss out on benefits to which they are entitled if they are not enrolled in a Medicare Advantage plan.
More than 50,000 Medicare Advantage ad airings used language that suggested people with Medicare are “missing out” on important benefits if they are not enrolled in a Medicare Advantage plan. Additionally, some ads tell viewers that they are “entitled” to receive supplemental benefits or cost savings offered by some Medicare Advantage plans. Language such as “missing” or “entitled” may give some viewers the impression that they have incomplete coverage or have overlooked a necessary enrollment step if they receive their Medicare coverage from traditional Medicare.
Medicare Advantage plans often include low or $0 supplemental premiums and extra benefits not included in traditional Medicare, such as coverage of dental, vision, and hearing services. The language used in the TV ads refers to these benefits by emphasizing that they are not covered by Medicare Parts A and B, and beneficiaries “do not get these benefits automatically” without enrolling in Medicare Advantage (also referred to as Medicare Part C). For example, some common phrases included:
“It’s a new year, and you may be entitled to new benefits.”
“If you only have Medicare Parts A and B, you may be missing out on extra benefits.”
“That’s right! There are people on Medicare that don’t have a Medicare Part C plan!”
“You are now entitled to eliminate copays.”
This messaging may be especially confusing when paired with references to the Medicare name, logo, or card. Ads with this messaging were more commonly sponsored by brokers and other third-party entities. These third-party sponsored ads also included a privately-run “Medicare” hotline in four out of every five airings, often alongside images of (and references to) the Medicare card. While these references may be intended to alert Medicare beneficiaries that these ads are directed at them, they may lead some viewers to believe the ads were produced by a government source, creating the impression that the government is endorsing the message that Medicare Advantage is “missing” from traditional Medicare coverage.
The vast majority of Medicare Advantage ad airings touted low costs and extra benefits, while few mentioned quality ratings.
More than 90% of airings for Medicare Advantage promoted extra benefits, such as dental, vision, and hearing, and 85% promoted cost features, such as $0 co-pays, no additional premiums, or reductions to the standard Part B premium (Figure 5). A KFF analysis of private Medicare advertising in 2008 also found extra benefits to be the most common message appearing in TV, print, and radio ads for Medicare Advantage.
By contrast, only one in five airings (22%) mentioned plan features that promote flexible access to providers and services, such as nationwide networks and out-of-network coverage, and fewer than 4% made any reference to a plan’s quality star rating.
Ads promoting Medicare Advantage touted a range of supplemental benefits. Mentions of dental, vision, hearing, and prescription drug benefits each appeared in more than 50% of all airings promoting Medicare Advantage. Dental coverage was included in 84% of airings, more often than any other type of supplemental benefit or any cost-related message (Figure 6).
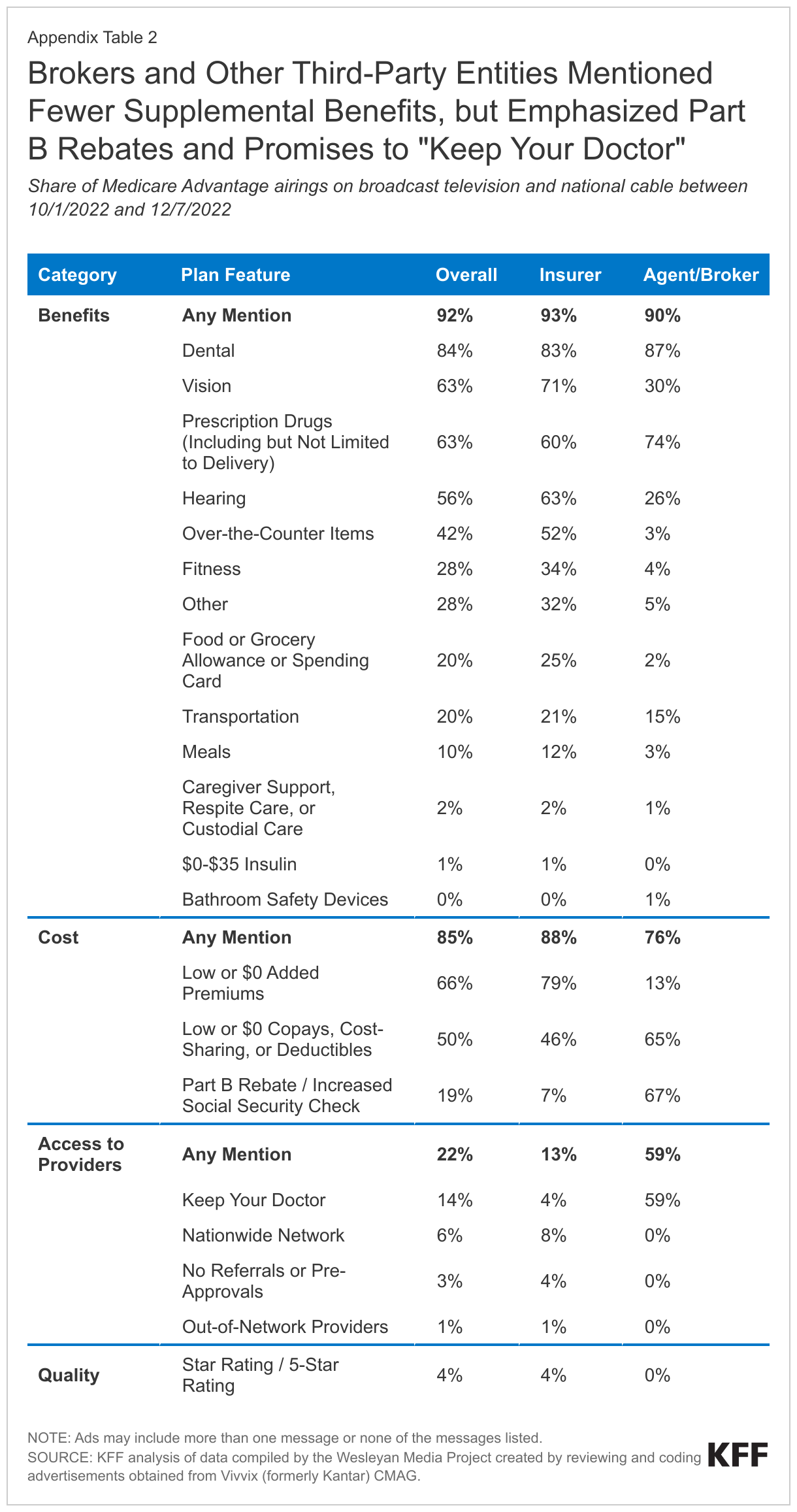
Benefits that may appeal to people in poorer health were marketed substantially less often, including allowances for food or grocery spending (20%), transportation services (20%), and meals (10%), though these were somewhat more common in insurer-sponsored airings than broker or other third-party airings (Appendix Table 2). Other benefits that are valuable to people with serious illnesses or mobility impairments were uncommon regardless of sponsor. Caregiver support, such as respite care or custodial care, was included in just 2% of airings, and bathroom safety devices such as bathtub rails and grab bars were included in less than 1%.
Supplemental benefits are a common feature of Medicare Advantage plans. In 2023, virtually all Medicare Advantage plans offer some supplemental benefits, most often dental, vision, hearing, gym memberships or other fitness benefits, and telehealth services, all of which were offered in at least 97% of available plans. Just 43% of plans included coverage for transportation services, and fewer than 15% included coverage for in-home support services, caregiver support, or bathroom safety devices, consistent with the smaller share of airings that mentioned these benefits.
More than two-thirds of airings sponsored by brokers and other third parties mentioned money back in your Social Security check. Two in three (67%) Medicare Advantage airings sponsored by brokers and other third-party entities included messaging about Part B premium rebates, compared to just 7% of insurer-sponsored airings and 19% overall (Figure 7; Appendix Table 2). While all Medicare Advantage enrollees must continue to pay the Part B premium (or in the case of dual-eligible individuals, have it paid on their behalf), Medicare Advantage plans can offer a rebate against the Part B premium as a supplemental benefit. This is sometimes referred to as the “give back” benefit and results in beneficiaries receiving higher Social Security payments each month.
Airings that included this message often featured endorsements from national celebrities. Joe Namath was featured more than any other celebrity (appearing in nearly 56,000 airings) and mentioned Part B premium rebates in 100% of his appearances.
Few airings, regardless of sponsor, stated that Medicare Advantage enrollees were required to pay the standard Part B premium, which may lead to confusion when plans are advertised as having “no premium.” Frequency of this message could not be measured precisely, due to the very small number of airings in which it appeared (see Methods for details).
Part B premium rebates are less common than many other supplemental benefits, offered by just 17% of plans available in 2023, with an even smaller share of enrollees (10%) opting for plans with this benefit. Though not applicable to these ads, new CMS rules, effective June 2023, prohibit marketing of benefits that are not available in the service area where the ad is aired, which may lead to fewer mentions of this benefit during the upcoming open enrollment period.
Low or $0 supplemental premiums were frequently mentioned among airings sponsored by Medicare Advantage insurers. Roughly two-thirds (66%) of airings promoting Medicare Advantage mentioned low or $0 supplemental premiums. Two-thirds of Medicare Advantage plans available in 2023 do not have a premium (other than the Part B premium) and among all plans the average premium is $15 per month. Mentions of low or $0 premiums were more common in airings sponsored by health insurers (79%) than those sponsored by brokers and other third-party entities (13%) (Appendix Table 2).
By contrast, airings promoting low out-of-pocket spending, including low or $0 co-pays, low cost-sharing, and low deductibles, were common among insurers and third-party sponsors, appearing in half (50%) of all Medicare Advantage airings (Figure 7; Appendix Table 2).
Messages about low premiums were often presented in contrast to the cost of supplemental plans such as Medigap. Traditional Medicare places no cap on out-of-pocket spending for hospital or physician services, and supplement plans can help to insulate beneficiaries from financial risk, but Medigap plans can be costly, with premiums ranging from less than $100 to more than $300 per month. Traditional Medicare beneficiaries may choose to purchase a Medicare supplement to assist with cost-sharing for services covered under Medicare Parts A and B.
VIDEO: Nearly all Medicare Advantage ads touted low costs and extra benefits.
Messages about low out-of-pocket spending sometimes featured estimates of savings that beneficiaries could expect to retain by enrolling in a Medicare Advantage plan. While not applicable to these ads, new regulations from CMS include a prohibition against advertising unrealized “savings” that are calculated relative to the expenses borne by uninsured individuals, the unpaid costs of beneficiaries dually eligible for Medicare and Medicaid, or other unrealized costs of a Medicare beneficiary. According to CMS, these savings estimates can be misleading, as they do not reflect the out-of-pocket costs paid by most Medicare beneficiaries and may give an unrealistic impression of the cost difference between plans.
About one in five Medicare Advantage TV airings emphasized access to doctors. Roughly one in five (22%) Medicare Advantage airings mentioned plan features that reflect flexible access to providers and services, such as promises to “keep your doctor” (14%), nationwide networks (6%), no referrals or pre-approvals for covered services (3%), or coverage for out-of-network providers (1%) (Figure 8). These messages were less common among TV ad airings sponsored by health insurers (13%) than brokers and other third-party entities (59%) (Appendix Table 2).
Health insurers may not choose to advertise access to providers as often as supplemental benefits because most plans employ networks, which place restrictions on which providers enrollees may see or offer more limited coverage for out-of-network services. Further, virtually all Medicare Advantage enrollees are in a plan that requires prior authorization for at least some services.
In contrast, 59% of Medicare Advantage airings sponsored by brokers and other third-party entities include the promise to “keep your doctor” (Appendix Table 2). Many brokers offer a range of plans with different networks, and may feel confident that they can offer a plan that includes a beneficiary’s current doctor, but it is unlikely that most beneficiaries would be able to keep their doctor regardless of the plan they choose. In 2023, 58% of Medicare Advantage plans are HMOs, which typically do not cover out-of-network services
Less than 4% of Medicare Advantage ad airings reference quality star ratings. CMS regularly publishes quality ratings of Medicare Advantage plans to assist beneficiaries in comparing the options available in their area. Plans are rated on a 5-star scale, with 1 star indicating poor performance, 3 stars indicating average performance, and 5 stars indicating excellent performance. While these ratings are intended, in part, to help consumers select a plan, they are very rarely used in TV advertising. Fewer than 4% of Medicare Advantage airings made any reference to a plan’s star rating (Figure 5).
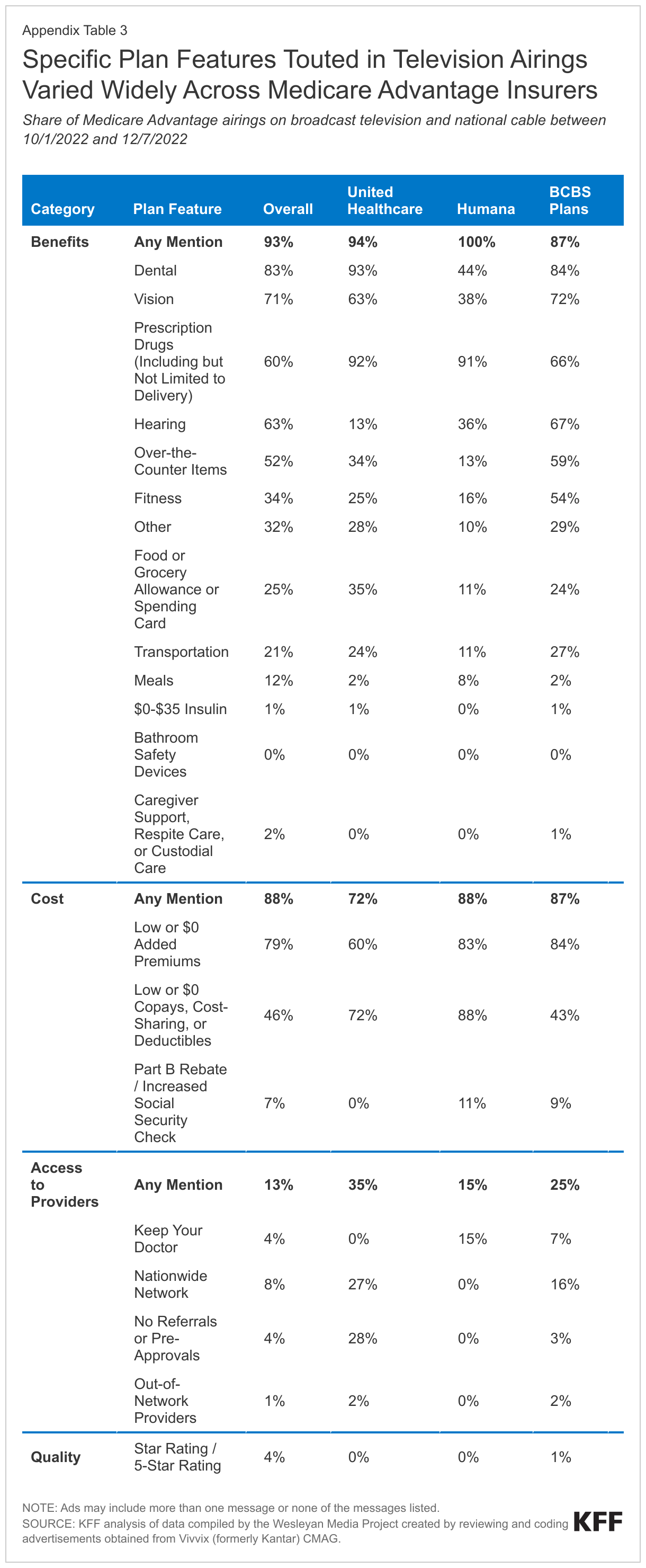
An exception was Kaiser Permanente, which promoted the quality star rating of their plans in 86% of airings, while no other single insurer mentioned star ratings in more than 5% (Appendix Table 3). This may be due to the high ratings received by most Kaiser Permanente plans. Virtually all Medicare Advantage beneficiaries enrolled in Kaiser Permanente were in a plan with a quality rating of at least four stars in 2022, the highest share of any major insurer.
Focus groups conducted by KFF in the fall of 2022 suggest that beneficiaries do not generally take star quality ratings into account when choosing a plan. In 2023, 7 in 10 (71%) Medicare Advantage beneficiaries were enrolled in plans with a rating of 4 or more stars, which may make the rating system less meaningful to beneficiaries looking to distinguish between plans with similar scores. MedPAC has raised concerns about the star rating system in recent years, noting, among other things, that star ratings are reported at the contract rather than the plan level, which may make them less useful to beneficiaries interested in the quality of a specific plan.
Medicare Advantage insurers varied in whether they promoted particular supplemental benefits, the potential for savings, access to providers, or quality most often. Medicare Advantage insurers differed in the plan features they chose to emphasize (Appendix Table 3). UnitedHealthcare, Blue Cross Blue Shield affiliates, and CVS all touted dental coverage more often than any other supplemental benefit, consistent with the overall trend. In contrast, Humana mentioned dental coverage in just 44% of airings, but included mentions of cost features such as low or $0 premiums and low or $0 co-pays in more than 80% of airings. Centene mentioned less common offerings more often than other insururers, including benefits such as meals, transportation, and vouchers for food and groceries or over-the-counter items in more than 50% of airings.
UnitedHealthcare mentioned plan features related to access to providers more often than other insurers, promoting a nationwide network in 27% of airings and lack of referrals or prior authorization requirements in 28% (compared to just 8% and 4% of insurer-sponsored Medicare Advantage airings overall).
Medicare Advantage ad airings often featured active seniors engaged in physical activities, but rarely showed people who appeared to have a serious health problem or visible disability.
Most Medicare Advantage airings (78%) featured people in some capacity. While ads were diverse in terms of the race, ethnicity, gender, and age of people shown (data not shown), people were generally shown to be in good health and free from serious illness. A prior KFF analysis of private Medicare advertising found a similar pattern among print, radio, and TV ads for Medicare Advantage plans in 2008, with one in ten showing seniors engaging in physical sports, just 3% showing people under 65 with a visible disability, and none showing people with visible signs of illness or frailty (such as a walker or a cane).
About one-quarter (26%) of Medicare Advantage airings show seniors participating in physical activity. One in four Medicare Advantage airings (26%) (Figure 9), including 32% of those sponsored by health insurers, showed seniors engaging in some form of physical activity. While some ads featured wellness activities, such as yoga or stretching, others showed seniors engaging in activities that demand much greater health and fitness, such as mountain biking, ziplining, trampoline jumping, and other forms of vigorous exercise. These ads may be targeting healthier seniors who might find these activities appealing or aspirational, and may promote the message that these plans ensure a certain standard of health, but they may also signal to those in poorer health that the plans promoted in these ads are not designed to meet more serious health needs.
VIDEO: Medicare Advantage ads often featured active seniors engaged in physical activity.
Fewer than 5% of airings include a person with a physical disability or someone receiving treatment for a serious illness. People with physical disabilities were shown in less than 4% of airings promoting Medicare Advantage, while just 1% showed a person receiving treatment for serious illness (Figure 9). Nearly all of these airings were sponsored by health insurers, as virtually no airings sponsored by brokers or other third-party entities featured people in either demographic. While this may represent an effort by insurers to associate their plans with good health, this pattern does not represent the demographics of Medicare beneficiaries as a whole. One-fifth (22%) of Medicare beneficiaries are in fair or poor self-reported health, and more than one-quarter (28%) have at least one functional impairment. Among beneficiaries under 65 and living with a permanent disability, these shares are much higher, 57% and 52% respectively.
Just over one-fifth (22%) of Medicare Advantage airings show a senior using technology. One in five Medicare Advantage airings (22%) (Figure 9), including 25% of those sponsored by health insurers, showed seniors using technology such as laptops, smartphones, or tablets. As with ads that show physical activity or exercise, this may be an attempt to appeal to a younger, more engaged group of beneficiaries, rather than those who struggle with serious health issues such as cognitive impairment.
TV ads sponsored by brokers and other third-party entities used celebrity endorsements more often than health insurers to promote Medicare Advantage.
More than half (55%) of all Medicare Advantage airings sponsored by brokers and other third-party entities featured endorsements from celebrities such as actors, athletes, and politicians. Most featured celebrities who were seniors themselves, and virtually all national celebrities featured in these ads were men. In contrast, just 3% of insurer-sponsored ads featured celebrities. Brokers and other third parties may feel more of a need to give viewers a familiar name to catch their attention, while insurers may have more of an interest in establishing their own brand.
Focus groups conducted by KFF in the fall of 2022 suggest that beneficiaries are not swayed by celebrity endorsements and frequently disregard them. Nonetheless, many reported encountering these ads, suggesting that they are memorable, and that celebrities may help draw attention and promote a brand, even if beneficiaries do not regard them as credible.
Joe Namath was featured more often than any other celebrity, appearing in nearly 10% of all Medicare Advantage airings (55,839). One ad in which he appeared aired more often than any other single Medicare ad during the advertising period, and a second was in the top ten, with 41,252 airings and 14,421 airings respectively. No other celebrity appeared in more than 1% of Medicare Advantage airings. Other familiar figures included former sports stars such as David Ortiz, Magic Johnson, and Joe Montana, musicians such as Lionel Richie, politicians such as Mike Huckabee, and popular actors such as William Shatner, J.J. Walker, and William Devane.
VIDEO: Ads sponsored by brokers and other third parties often used celebrity endorsements to promote Medicare Advantage.
Discussion
Every fall, Medicare beneficiaries are flooded with TV ads during the nine-week marketing period for open enrollment, most of which promote Medicare Advantage plans. The open enrollment period for 2023 coverage saw an average of more than 9,500 Medicare ad airings each day, nearly all of them from health insurers and third-party entities, such as brokers. This volume of advertising has been accompanied by a rise in beneficiary complaints related to aggressive and misleading marketing tactics, leading to heightened attention from CMS, the NAIC, and other policymakers.
New rules from CMS, effective June 2022 and June 2023, aim to address these issues by strengthening oversight of third-party marketing organizations, requiring greater transparency pertaining to the availability of advertised benefits and plan features, and prohibiting the use of certain language and images, such as the Medicare name, logo, or card, in ways that may be misleading to beneficiaries. While not all of these regulations applied to the ads discussed in this analysis, all will be in effect for the open enrollment period that begins in October 2023. Some of the observations described in this report, such as the use of a government-issued Medicare card, which may lead viewers to think the ads are sponsored by the government rather than a private company, may occur less frequently, if at all, in the future. While the new rules may address some concerns about aggressive and misleading marketing tactics, ongoing monitoring and resources independent of commercial interests could help to improve beneficiary decision-making.
Few if any ads mentioned the traditional Medicare program, the alternative to private Medicare Advantage plans, except in the context of the small number of ads promoting supplemental coverage, such as Medigap and stand-alone Part D plans. This is not surprising, since TV ads are sponsored by health insurers and brokers selling private plans, although it may leave beneficiaries without a clear understanding of their coverage options, and the tradeoffs that arise from one choice over another. Many beneficiaries may find it helpful to have support when making decisions about their Medicare coverage, including from financially disinterested sources such as State Health Insurance Assistance Programs, Social Security Administration district offices, and 1-800-Medicare. A recent survey found that many people age 65 and older would like to know more about the out-of-pocket costs and benefits of their Medicare coverage options and felt that they would benefit from one-on-one help. Adequate resources to meet the demands for assistance – beyond brokers, who have a financial interest in steering people to certain options — may help ensure Medicare beneficiaries are choosing the coverage option that best meets their needs.
Appendix
Additional Data and Figures
Time Slots, Concurrent TV Programs, and Broadcast Networks of Medicare Ad Airings: Medicare advertisements appeared at all times of day, and throughout the week, but airings were most frequent on weekday afternoons (24%), weekday mornings (19%), and in the hours leading up to prime time (16%). Airings were most often shown during local news broadcasts (data not shown), while court shows, game shows, and talk shows were among the top single programs during which Medicare ads were aired (Appendix Table 1). The largest number of airings appeared on the four major broadcast networks: the Fox Broadcasting Company (16%), the American Broadcasting Company (ABC) (16%), Columbia Broadcasting System (CBS) (15%), and the National Broadcasting Company (NBC) (14%). Local advertising was more concentrated in some areas than others, with the top 20 local media markets comprising 27% of all local airings (Appendix Figure 1).
Common Messages Featured in Medicare Ad Airings by Sponsor Type and Insurance Firm:
CMS Regulations
Rules Effective June 2022: Current rules from CMS, which came into effect in June 2022 and applied to all Medicare Advantage and Part D ads discussed in this analysis, include several changes aimed at tightening oversight of third-party marketing activities. The rules introduce a broad definition of third-party marketing organizations, encompassing all organizations and individuals paid to perform lead generation, marketing, sales, or enrollment functions on behalf of a private Medicare plan, either directly or indirectly through another third party.
Health insurance companies that offer Medicare plans are now responsible for ensuring that third-party marketing organizations adhere to any CMS requirements that apply to plans themselves (previously only required for direct contractors). In the context of TV advertising, some examples include existing rules that forbid ads from using the term “free” to describe a $0 premium, implying that a plan is recommended or endorsed by CMS or another government office, or implying that a plan is only available to seniors rather than all eligible Medicare beneficiaries. Health insurers are also required to add certain monitoring and oversight provisions to any direct contract with a third-party marketing organization, and keep track of any downstream relationships that organization is using to represent their plans.
Finally, third-party marketing organizations are now required to include a standardized disclaimer in all communications and marketing materials informing beneficiaries that they do not represent every plan available in their service area and encouraging them to contact Medicare.gov or 1-800-MEDICARE for a complete list of their options.
Rules Effective June 2023: Additional rules from CMS, which came into effect in June 2023 and will apply to the upcoming open enrollment period that begins in October, introduce several more provisions aimed at curtailing misleading marketing practices. While some of these provisions go beyond the scope of TV advertising, several will have a direct impact on TV ads in the fall and in future periods.
Ads are now prohibited from mentioning any benefits or plan features that are not available in the service area where the ad appears. Ads that air in media markets that cross multiple service areas are required to list which benefits apply to each service area (Medicare Advantage and Part D service areas are defined at the county level). The Washington, DC market, for example, includes not only DC itself but also surrounding counties in Maryland and Virginia, representing several distinct service areas for which an insurer may offer plans with different premiums, cost-sharing, and benefits.
Ads are also prohibited from using the Medicare name, logo, or card in ways that could be misleading to beneficiaries. Any use requires prior approval from CMS, and CMS has stated that it will only grant this approval in cases where it is serving an educational (as opposed to marketing) purpose. CMS defines marketing as any material or activity that meets certain standards for both intent (to influence enrollment decisions or draw attention to plans) and content (any mention of specific plan features such as benefits, costs, or quality rankings), standards which would likely apply to any ad targeting open enrollment.
Third-party marketing organizations, such as agents and brokers, are prohibited from advertising specific plans or plan features without identifying the Medicare Advantage organizations or Part D sponsors that offer them. CMS requires these names to be displayed in the same font size, or read at the same pace, as any benefits included in the ad. Third parties are prohibited from airing ads without the plan sponsors promoted in the ads agreeing to their content, and sponsors may be subject to penalties for endorsing ads that do not comply with CMS regulations.
Additional regulations include prohibiting the mention of unrealized “savings” calculated relative to the expenses borne by uninsured individuals, the unpaid costs of beneficiaries dually eligible for Medicare and Medicaid, or other unrealized costs of a Medicare beneficiary; prohibiting the use of superlatives such as “best” and “most” in marketing materials, taglines, or logos; and revising the disclaimer required for all third-party ads (described in the section above) to include State Health Insurance Assistance Programs (SHIPs) alongside Medicare.gov and 1-800-MEDICARE as a resource that beneficiaries can turn to for more information about their coverage options.
File & Use: Health insurers and third parties must submit all marketing materials to CMS for review before they can be aired, or in the case of some third parties, have them submitted by the insurer they represent. Until recently, CMS permitted TV ads to be submitted through its File & Use framework. Materials designated as File & Use may be aired five days after submission to CMS, though CMS reserves the right to review these materials for compliance both during and after this five-day window. Marketing materials that do not qualify for File & Use must be submitted forty-five days before they are aired, prospectively approved or disapproved during this timeframe, or “deemed approved” if no decision is reached within forty-five days. Beginning January 1st, 2023, in light of ongoing concerns, CMS no longer allows TV ads to be submitted as File & Use. Ads slated to air on October 1st, 2023 must be submitted to CMS by mid-August, allowing a longer window for prospective review.
Methods
Our data consist of 1,267 unique ads and 643,852 total airings, representing all English-language TV ads focused on Medicare that aired on broadcast television or national cable between October 1st, 2022 and December 7th, 2022. While the open enrollment period does not begin until October 15th each year, sponsors are permitted to advertise beginning October 1st. Ads were supplied to the Wesleyan Media Project by Vivvix (formerly Kantar) CMAG along with additional information on the timing of the airing, the media market, TV station, and broadcast network where it was aired, and the TV programming shown on the same station during that time slot. The Wesleyan Media Project compiled and processed all data flagged by Vivvix CMAG as relevant to our study, including ads classified as “Medical & Dental Insurance” or “Insurance Agencies & Brokers,” ads sponsored by the Department of Health and Human Services or AARP, and any ad with Medicare in the title.
In the first phase of processing, the Wesleyan Media Project used optical character recognition (OCR) to extract the textual information on screen and automatic speech recognition (ASR) to extract the audio into text for each video. Ads that did not contain the word Medicare in either OCR or ASR were removed from the set. The Wesleyan Media Project then assessed the degree of text similarity from the ASR data to identify advertising that was greater than 90% matching in audio content. Ads with 90% or higher similarity were grouped and only one ad per group was flagged for human coding (described below), along with any ads that did not match with others. Finally, the Wesleyan Media Project identified and removed Spanish-language advertising that ran on Spanish-language networks Telemundo, Unimas, and Univision. A secondary step to filter out Spanish-language advertising was conducted in the human coding stage. This left us with a final analytical set of 1,267 unique ads.
KFF and the Wesleyan Media Project then developed a coding instrument to analyze ad content. Key variables included in the instrument were those relevant to the evolving policy context surrounding Medicare marketing, such as the sponsor, Medicare products, and plans represented in each ad, as well as messaging on plan features, slogans or repeated phrases, activities and characteristics of people shown in the ad, websites and contact information, and use of the Medicare name, logo, or card.
Ten undergraduate student coders received training and completed four sets of practice ads prior to beginning live coding. A random sample of ads (20%) were double coded to assess intercoder reliability, and all Krippendorff’s alpha statistics were calculated for each variable. All results described in this report all met the 0.7 threshold for acceptable levels of reliability, with some exceptions noted below. For ads that included fine print, coders were asked to indicate whether they could read the fine print without pausing. While coder impressions are noted where relevant, this variable is not scientific, as monitor sizes vary, which affects readability. Coders were also asked to flag any ads that stood out to them as surprising, misleading, or notable in some other way and offer their qualitative impressions.
KFF analyzed the frequency of ad characteristics in the data as a whole, as well as by sponsor type, advertised product, and media market. Insurer sponsored ads were also analyzed by firm. KFF further reviewed a sample of ads in their entirety, including ads for which coders had given qualitative comments, to identify relevant examples of common messages, elements, and themes. Messages related to in-home support services, caregiver support, and bathroom safety devices were categorized as “other supplemental benefits” by our coding instrument. These were identified by coders in a free text field and reviewed by KFF as described, but were not formally assessed for intercoder reliability. Likewise, some characteristics, such as the message that beneficiaries were required to pay the standard Part B premium, appeared too rarely to meet the 0.7 threshold for acceptable intercoder reliability. In these cases, we noted that the characteristic was rare, but were not able to report its frequency with precision.
We focused much of our analysis on the substantial majority of ads promoting Medicare Advantage, the most common product advertised during the period.