Community Health Centers Are Taking Actions to Prepare for the Unwinding of the Public Health Emergency
Community health centers, a national network of safety-net primary care providers serving low-income, medically underserved communities, also assist their patients and low-income community members with applying for and enrolling in health coverage, including Medicaid, the Children’s Health Insurance Program (CHIP), and Marketplace plans. Given this dual role, health centers are poised to be on the front lines of the unwinding of the Medicaid continuous enrollment requirement when the public health emergency (PHE) ends.
Provisions in the Families First Coronavirus Response Act (FFCRA) require states to provide continuous coverage for Medicaid enrollees until the end of the month in which the PHE ends in order to receive enhanced federal funding. The current PHE runs through July 15, 2022; however, it is expected to be extended for at least another three months. The Biden Administration has said that it will give states a 60-day notice before the PHE expires. When the PHE ends, states will begin processing redeterminations, and recent estimates indicate that between 5.3 million and 14.2 million Medicaid enrollees could lose coverage if they are no longer eligible or face administrative barriers despite remaining eligible.
Nearly half of health center patients are covered by Medicaid, meaning large coverage losses could have significant effects for health centers and their patients. Throughout the pandemic, health centers have provided a broad range of services to their Medicaid and other patients, including COVID-19 testing, treatment and vaccinations, mental health and opioid use disorder services, as well as social and supportive services. In 2020, health centers served over 13 million Medicaid patients who comprised 46% of total health center patients that year. The number and share of Medicaid patients served by health centers have likely increased since then as total Medicaid enrollment has continued to grow over the past year. As such, health centers have the ability to reach about one in six Medicaid enrollees through their patients alone and can reach even more by providing outreach and assistance to community members who are not patients.
With funding for enrollment activities included in their federal grants, health centers are able to employ staff and provide outreach and enrollment assistance throughout the year. In 2020, health centers employed over 4,200 enrollment assisters and provided over 3.5 million assists to individuals seeking help in applying for or renewing coverage. Those numbers are down slightly from 2019 when health centers employed over 4,400 enrollment assistance staff and provided about five million assists. Both staffing and enrollment assistance visits will likely need to increase in the coming year If health centers hope to meet expected demand for assistance.
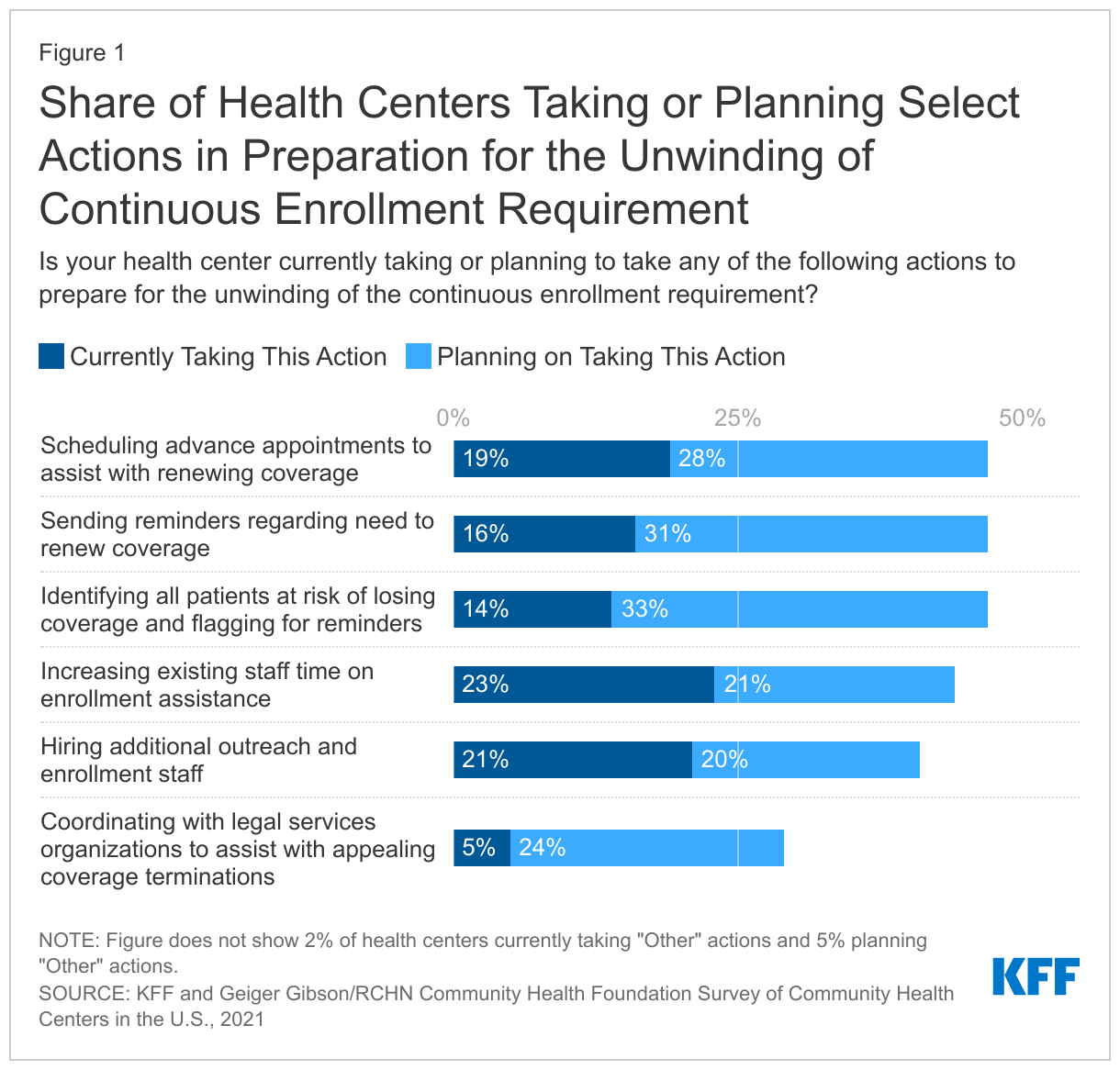
Anticipating the end of the PHE, health centers are taking steps to prepare, including by contacting patients and bolstering enrollment staff. According to findings from a survey of health centers conducted in late 2021, roughly two-thirds (66%) of health centers were planning or taking actions to help their patients retain coverage when the PHE expires (Figure 1). Overall, just under half of health centers had already begun reaching out or planned to reach out to patients to assist them with renewing coverage:
- 47% said they would schedule or were planning to schedule advance appointments to assist patients with coverage renewals;
- 47% planned to send reminders to patients regarding the need to renew coverage; and
- 46% said they would identify all patients at risk of losing coverage and flag their charts for reminders.
Health centers also reported plans to boost enrollment assistance staff capacity:
- 43% planned to increase staff time on enrollment activities (23% said they were already increasing staff time) and
- 41% had hired or planned to hire new staff.
Health centers can be effective in raising awareness about Medicaid renewal requirements and in providing the help needed for enrollees to maintain Medicaid or transition to other coverage. The Centers for Medicare and Medicaid Services (CMS) encourages states to reach out to key stakeholders as they develop their plans for resuming normal operations. As of late 2021, about one in five health centers said they had received information from their state or primary care association regarding their state’s plan. That number is expected to increase as states finalize their plans and once there is greater clarity on when the PHE will end. Until then, health centers appear to be moving forward with their own plans for providing outreach and assistance to underserved and medically vulnerable Medicaid enrollees.