Analysis of National Trends in Medicaid and CHIP Enrollment During the COVID-19 Pandemic
Note: To get the latest data on Medicaid enrollment, disenrollment, and procedural disenrollments, visit KFF’s Medicaid Enrollment and Unwinding Tracker. The analysis below uses CMS data about Medicaid and CHIP enrollment through December 2022, providing information about Medicaid enrollment levels during the pandemic.
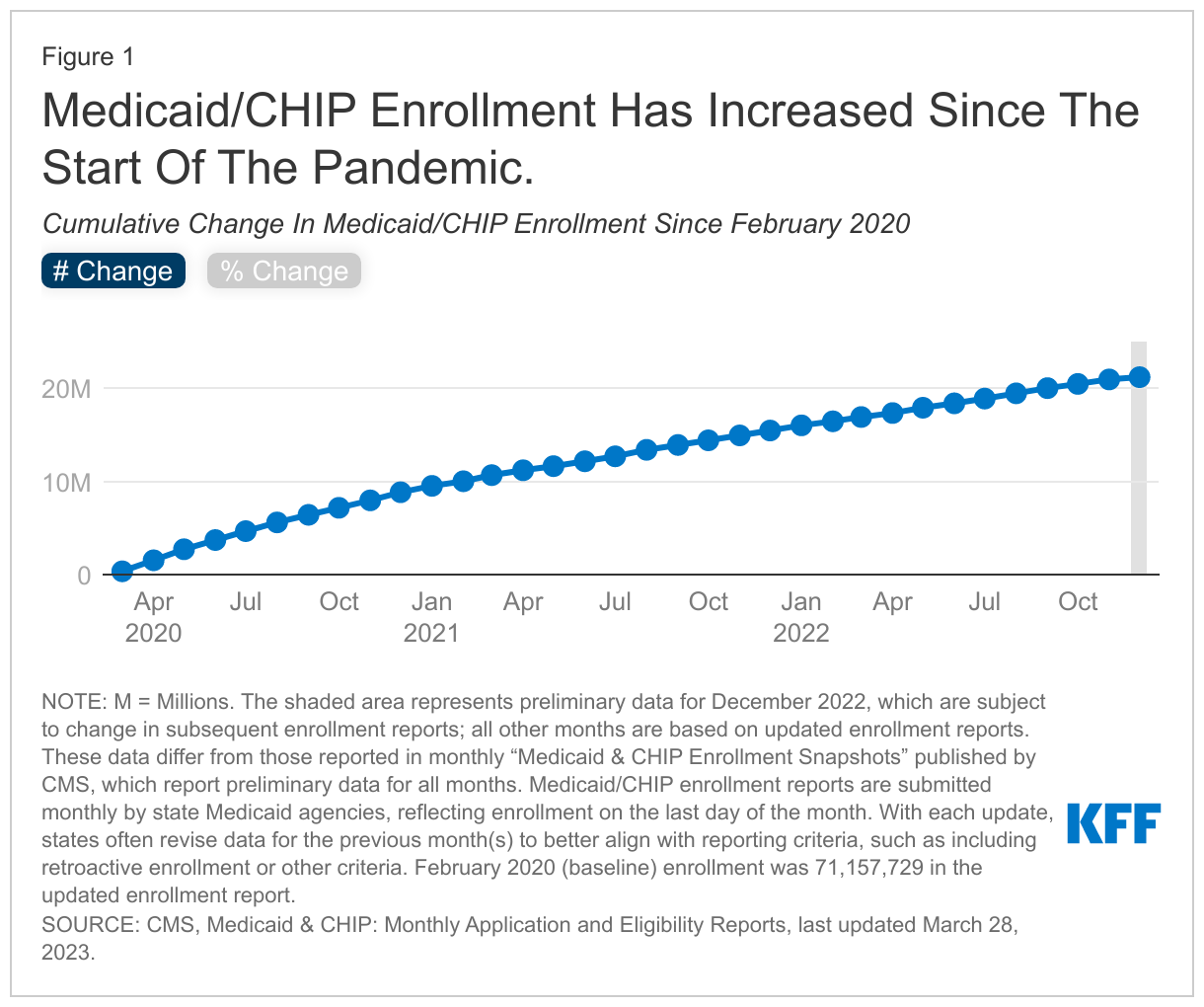
This data note looks at national and state-by-state Medicaid and CHIP enrollment data through December 2022. After declines in enrollment from 2017 through 2019, preliminary data for December 2022 show that total Medicaid/CHIP enrollment grew to 92.3 million, an increase of 21.2 million from enrollment in February 2020 (29.8%), right before the pandemic and when enrollment began to steadily increase (Figure 1).1 Increases in enrollment may reflect changes in the economy, changes in policy (like recent adoption of the Medicaid expansion in the Affordable Care Act), and the temporary continuous enrollment provision created by the Families First Coronavirus Response Act (FFCRA). Under the continuous enrollment provision, states generally cannot disenroll Medicaid enrollees while the provision is still in effect and in exchange, states receive a temporary increase in the federal Medicaid match rate. The continuous enrollment provision has halted churning in Medicaid – the temporary loss of coverage in which enrollees disenroll and then re-enroll within a short period of time – in addition to preventing Medicaid coverage loss during the pandemic. As part of the Consolidated Appropriations Act, signed into law in December 2022, Congress set an end to the continuous enrollment provision on March 31, 2023, and will phase down the enhanced federal Medicaid matching funds through December 2023. States that accept the enhanced federal funding can resume disenrollments beginning in April 2023 but must meet certain reporting and other requirements during the unwinding process. KFF estimates that Medicaid/CHIP enrollment will reach roughly 95 million enrollees in March 2023 before states may resume disenrollments during the “unwinding” of the continuous enrollment provision.
The information in this data note is based on KFF analysis of the Centers for Medicare and Medicaid Services (CMS) Performance Indicator Project Data. Medicaid/CHIP enrollment data are submitted monthly by state Medicaid agencies and, with each monthly update, states often revise the previous months’ enrollment to include retroactive enrollment and to better align with reporting criteria. Except for the latest month’s enrollment (December 2022), this brief reports data from the updated enrollment reports for all other months to reflect the most current enrollment data possible. However, the data presented in this brief will differ from those presented in monthly Medicaid and CHIP Enrollment Snapshots published by CMS, which use exclusively preliminary enrollment reports for all months.
Medicaid/CHIP enrollment increased following the implementation of the Affordable Care Act (ACA) but was declining in the two years prior to the pandemic. Following the implementation of the ACA Medicaid expansion to low-income adults in 2014, there were large increases in Medicaid and CHIP enrollment across states that followed steady growth in coverage of children over the past decade. These increases reflected enrollment among newly eligible adults in states that implemented the expansion as well as enrollment among previously eligible adults and children due to enhanced outreach and enrollment efforts and updated enrollment procedures tied to the ACA. This trend began reversing when enrollment started to decline in 2018 and continued to decline in 2019. Total enrollment fell from 73.3 million in December 2017 to 71.0 million in December 2019, a decline of 2.3 million people or 3.1%. Month-to-month enrollment declines slowed but continued until February 2020. The declines in enrollment, in part, reflected a robust economy, but experiences in some states suggested that they may have also reflected enrollment losses among people who were still eligible for coverage due to challenges completing enrollment or renewal processes.
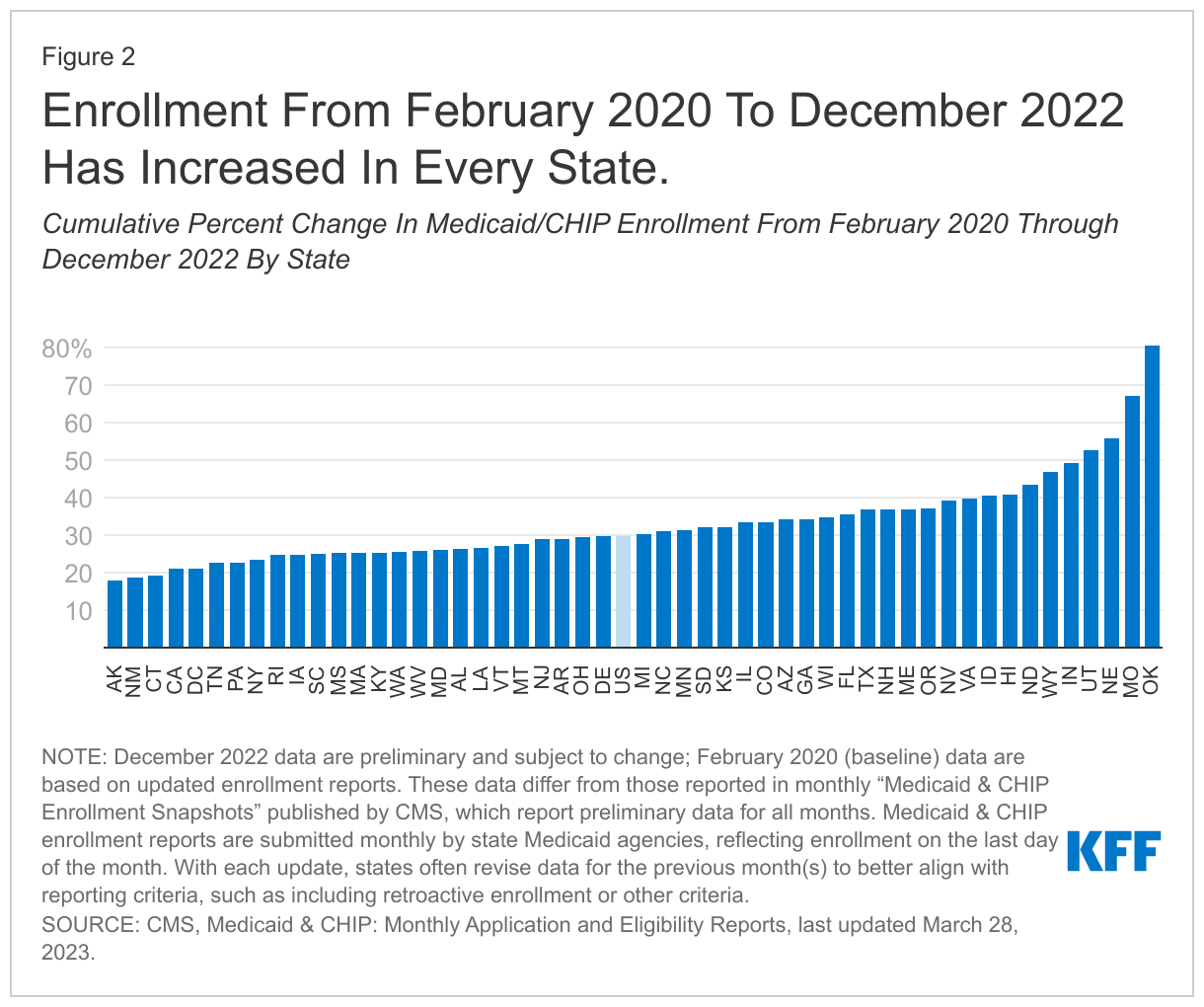
Data show that Medicaid/CHIP enrollment is increasing amid the coronavirus pandemic, growing by 21.2 million enrollees or 29.8% from February 2020 to December 2022. Over this period, all states experienced total Medicaid/CHIP enrollment growth ranging from 18.1% to 80.6% (Figure 2).2 The state with the largest growth since February 2020, Oklahoma, implemented the Medicaid expansion on July 1, 2021. Four other states have implemented expansion since 2020 – Utah and Idaho in January 2020, Nebraska in October 2020, and Missouri (where the state began to process applications3 in October with coverage retroactive to 7/1/2021) – contributing to higher-than-average rates of enrollment growth in these states as well.
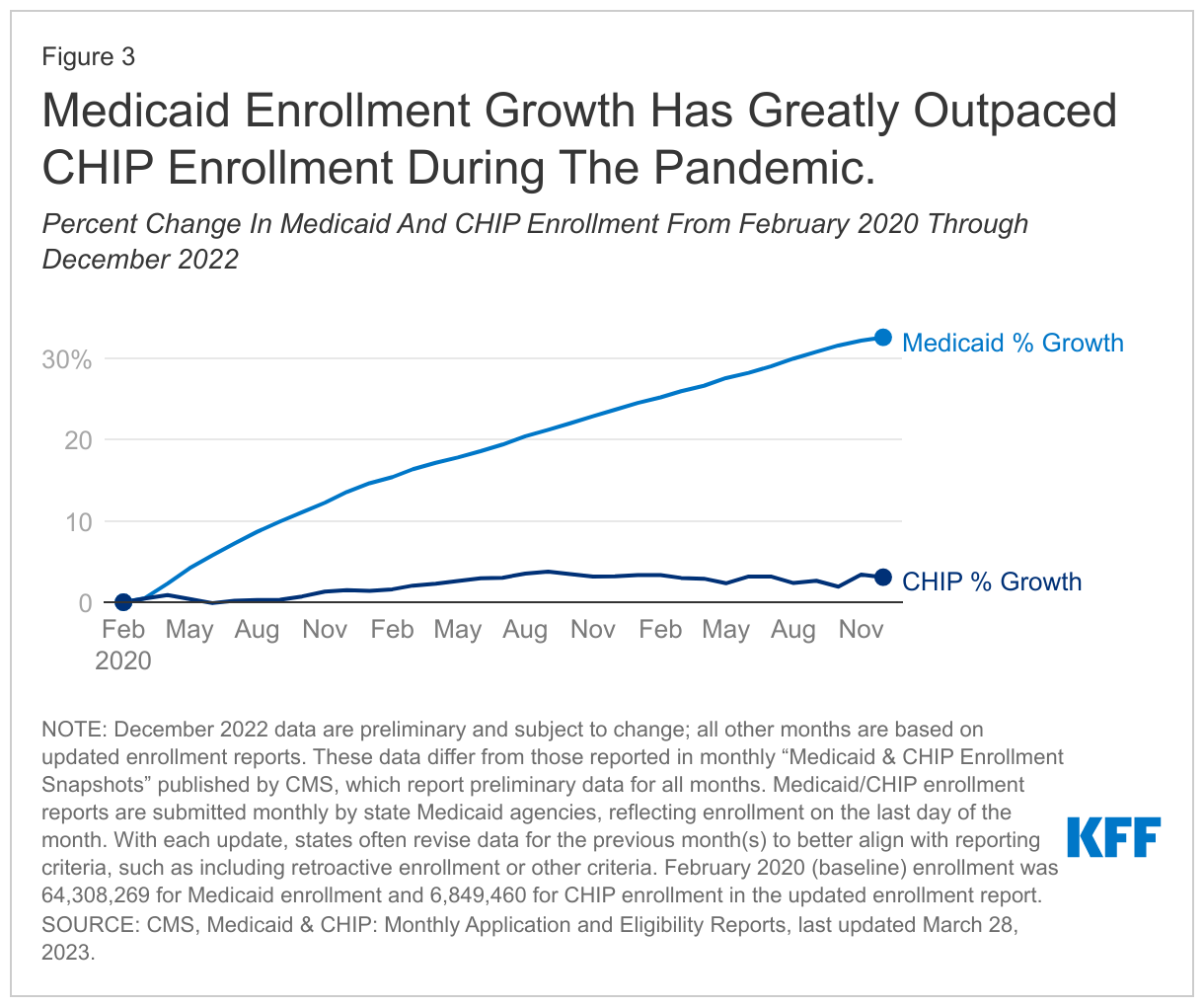
Virtually all growth was concentrated in Medicaid, which grew by 32.6% (21.0 million enrollees) from February 2020 to December 2022 data (Figure 3). Conversely, CHIP has seen less enrollment growth since February 2020 (3.1% or 211,000 enrollees) and several states (17) have seen declines in CHIP enrollment from February 2020 through December 2022 reports. These declines in CHIP enrollment for some states could reflect changes in family income, causing children to move from CHIP to Medicaid coverage. As discussed below, all states reported increases in child enrollment for Medicaid/CHIP overall during this time period.
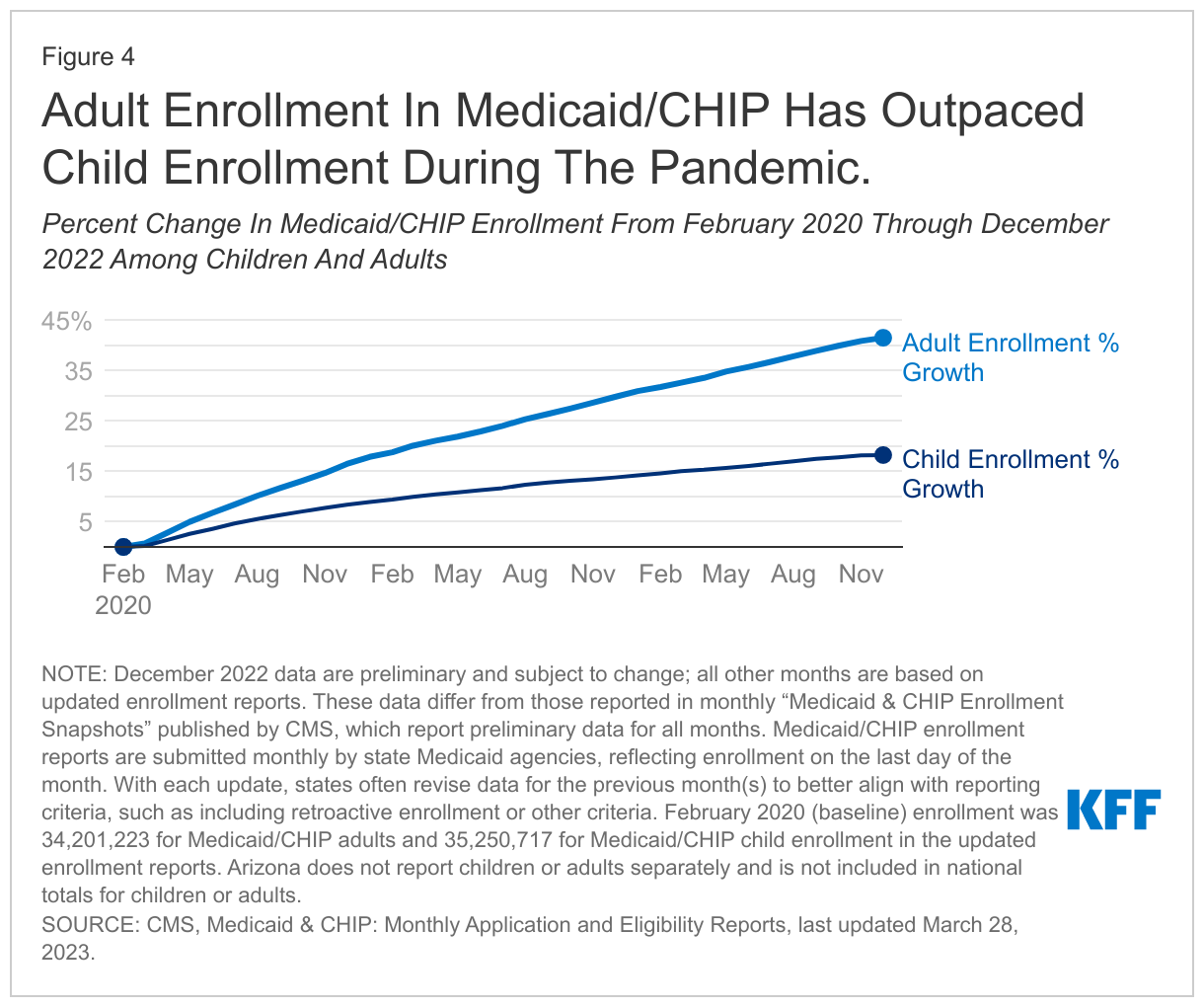
Adult enrollment in Medicaid/CHIP has increased rapidly during the pandemic, growing by 41.5% from February 2020 through December 2022 enrollment reports (Figure 4). This growth amounts to an additional 14.2 million adults in the 49 states and DC that report adult/child monthly enrollment (Arizona does not report children or adults separately). As mentioned above, five states began newly enrolling expansion adults since January 2020 (Idaho, Missouri, Nebraska, Oklahoma, and Utah), contributing to increased adult enrollment. Child enrollment grew as well, but at a slower pace: 18.2% or 6.4 million enrollees in the same period. Still, every state reporting these data saw an increase in child Medicaid/CHIP enrollment from February 2020, despite declines in CHIP enrollment in some states (as discussed above).
Many could lose coverage as states resume disenrollments starting in April 2023, once the continuous enrollment provision expires. As part of the Consolidated Appropriations Act, signed into law in December 2022, Congress set an end to the continuous enrollment provision on March 31, 2023, allowing states to resume disenrollments in April 2023, though states must meet certain reporting and other requirements during the unwinding process. plan to take the full 12 to 14 months allowed by CMS for completing redeterminations and returning to normal operations, though some states will complete the process more quickly, with five states planning to take 9 to 12 months and one state planning to take less than 9 months (data are currently unavailable for two states, Ohio and Texas). During this time, millions could be disenrolled from Medicaid if they no longer qualify or if they face administrative barriers during renewal even if they continue to be eligible. How states manage the large volume of redeterminations during the “unwinding” of the continuous enrollment provision, as well as how states engage with enrollees and other stakeholders, will impact the continuity of coverage for millions of Medicaid enrollees.
- Medicaid/CHIP enrollment reports are submitted monthly by state Medicaid agencies, reflecting enrollment on the last day of the month. With each update, states often revise data for the previous month(s) to better align with reporting criteria, such as including retroactive enrollment or other criteria. December 2022 data are preliminary and subject to change; all other months presented in this brief are based on updated enrollment reports. The data presented in this brief differ from those reported in monthly “Medicaid & CHIP Enrollment Snapshots” published by CMS, which use exclusively preliminary enrollment reports for all data reported. ↩︎
- Although all states report an increase in Medicaid/CHIP enrollment from February 2020 through December 2022, some states have occasionally reported month-to-month decreases in their updated enrollment reports starting in late 2020 and into 2022 (AK, CT, DE, ID, IL, IN, KS, KY, LA, MT, NM, ND, PA, RI, UT, and WV). Generally, these month-to-month declines appear sporadic and so do not likely represent a trend. In July 2021, Kentucky’s total Medicaid/CHIP enrollment decreased by 6.7% and the state attributed the decrease to removing individuals who had been receiving temporary coverage under the state’s presumptive eligibility policy during the pandemic, according to the CMS Enrollment Snapshot for July 2021. Month-to-month decreases in Medicaid/CHIP enrollment generally represent data reporting issues that have not yet been resolved by states, or they may represent data reporting corrections where historical data has not yet been corrected. Nine states (AK, GA, IA, KS, MD, MO, MT, NJ, and ND) reported a decline in total Medicaid/CHIP enrollment from the updated November 2022 report to the preliminary December 2022 report. These declines were generally small and reflect preliminary enrollment data for December 2022, which is typically updated in subsequent enrollment reports as states update their enrollment counts (for example, to better capture retroactive enrollment or to better align with CMS’s reporting criteria). In many cases, updated reports show slight increases in enrollment from preliminary reports. ↩︎
- Missouri has also expanded Medicaid since 2020. Medicaid coverage under expansion began when the state started processing applications in October 2021, with coverage retroactive to July 1, 2021, consistent with a state supreme court order. However, news reports indicate that the state was slow to process applications and enroll newly eligible expansion adults, although the state has worked with CMS to streamline the enrollment process and had made improvements in average application processing times as of September 2022. The state has still had higher-than-average enrollment increases from February even prior to implementing expansion. ↩︎