Medicare Advantage 2015 Spotlight: Enrollment Market Update
Issue Brief
Despite concerns that reductions in payments to Medicare Advantage plans enacted in the Affordable Care Act of 2010 (ACA) would lead to reductions in Medicare Advantage enrollment, the number and share of Medicare beneficiaries enrolling in Medicare Advantage plans has continued to climb.1 Since the enactment of the ACA, Medicare Advantage enrollment has increased by 5.6 million, or by 50 percent. The ACA payment reductions aimed to reduce historical overpayments to Medicare Advantage plans, relative to traditional Medicare.
This Data Spotlight reviews national and state-level enrollment trends as of March 2015 and examines variation in enrollment by plan type and firm. It analyzes the most recent data on premiums, out-of-pocket limits, Part D cost sharing, and plans’ quality ratings for Medicare Advantage enrollees. Key findings include:
- Medicare Advantage enrollment has continued to grow and increased in virtually all states in 2015. Almost one in three (31 percent) people on Medicare (16.8 million beneficiaries) were enrolled in a Medicare Advantage plan in March 2015 – up by more than one million beneficiaries from 2014.
- Medicare Advantage enrollment continues to be highly concentrated among large firms, both nationally and in local markets. Together, UnitedHealthcare and Humana account for 39 percent of all Medicare Advantage enrollment, and three other firms and BCBS affiliates account for another 33 percent of enrollment in 2015. In 15 states and the District of Columbia, more than half of all enrollees are in plans offered by one company – an indicator that these markets that may not be very competitive.
- Despite the growth in enrollment in new plan types, most enrollees continue to be in HMOs (64% in 2015). As in prior years, enrollees in HMOs, on average, pay lower premiums and have lower limits on total out of pocket expenses than enrollees in other plan types.
- The share of enrollees in plans with 4 or more stars rose from 37 percent in 2013 to 61 percent in 2015.
- While growth in premiums has been relatively modest, Medicare Advantage plans provide less financial protection to Medicare enrollees than they have in the past. While average monthly premiums for MAPDs (weighted by enrollment) remain relatively flat ($38 per month in 2015, an increase of $3 per month from 2014), they vary across plan types and states.
- Average out-of-pocket spending limits have continued to rise, exposing enrollees with significant medical needs to higher costs, and in 2015, the average out-of-pocket limit is $5,041. All plans have been required to limit enrollees’ out-of-pocket expenses to no more than $6,700 since 2011, and are encouraged have lower limits. The growth in out-of-pocket limits makes it increasingly critical that beneficiaries receive good information to help them choose effectively among the complex array of choices they face.
Overall Trends in Enrollment
Nationwide Enrollment
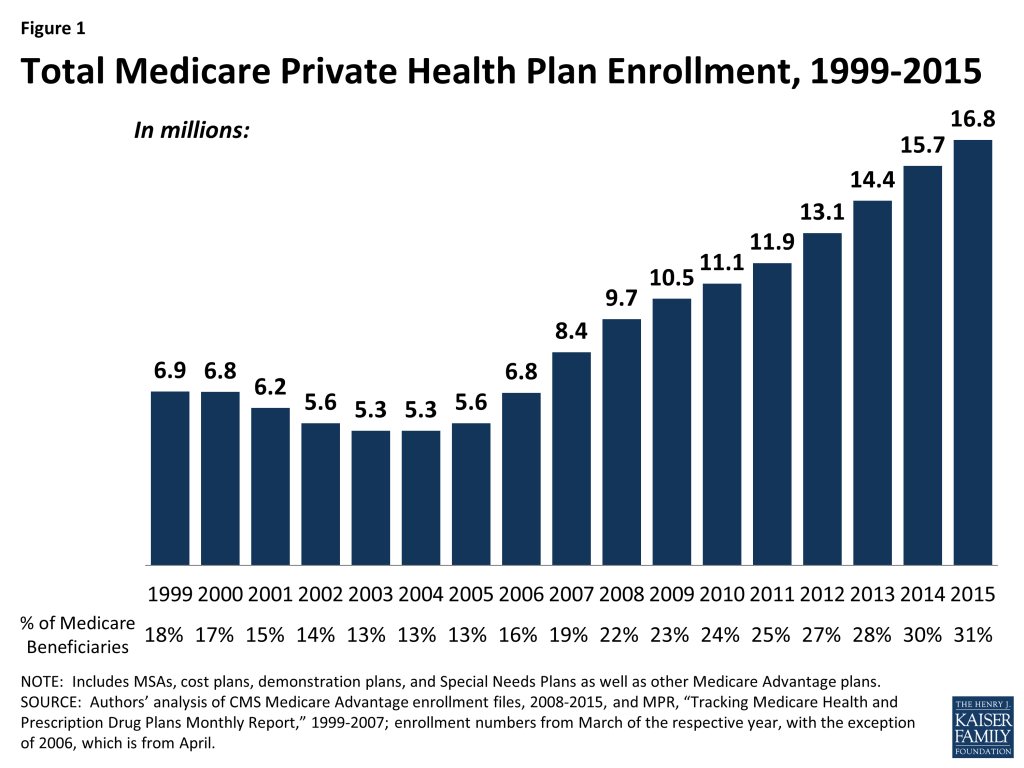
There are 16.8 million beneficiaries – 31 percent of the Medicare population – are enrolled in Medicare Advantage plans in 2015 (Figure 1). Total Medicare Advantage enrollment grew by more than 1 million beneficiaries, or 7 percent, between 2014 and 2015. This pattern continues the rapid growth in enrollment that occurred concurrently with the introduction of Part D (prescription drug coverage) in 2006 and other changes in the Medicare Advantage program authorized by the Medicare Prescription Drug, Improvement and Modernization Act (MMA) of 2003. While some of the growth in Medicare advantage enrollment reflects the influence of the baby boomers newly eligible for Medicare, recent evidence has indicated that enrollment growth also reflects small shifts in the larger pool of current beneficiaries switching from traditional Medicare to Medicare Advantage plans.2 Medicare enrollment has continued to grow despite the fact that the average number of plans available to enrollees nationwide declined from a high of 48 plans in 2009 to 20 plans in 2012 and to 18 in 2014 and 2015, as firms made changes to plans offered under their Medicare Advantage contracts.3
Trends in Enrollment by Plan Type
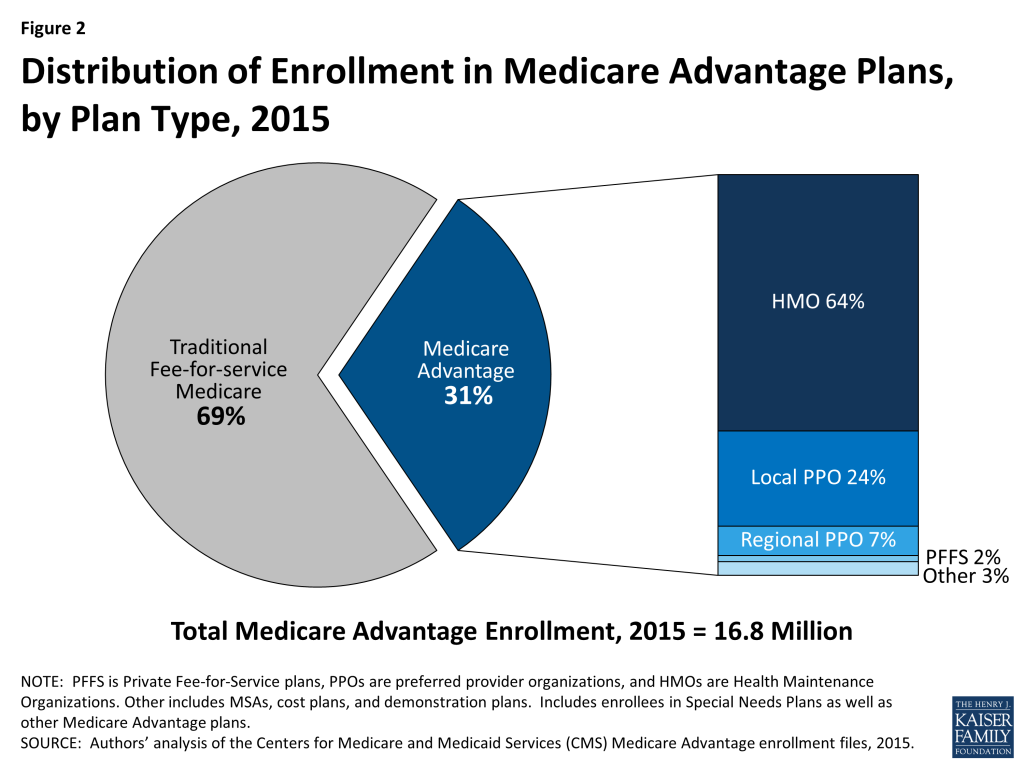
Similar to each year since 2007, about two-thirds (64%) of Medicare Advantage enrollees are enrolled in HMOs in 2015 (Figure 2). Almost one-third of enrollees are in either local PPOs (24%) or regional PPOs (7%), 2 percent are in PFFS plans, and 3 percent are in other types of plans, including cost plans and Medicare Medical Savings Accounts (MSAs).
PFFS plans were the primary alternative to HMOs from 2007 through 2009 but their role in the Medicare Advantage market has now been more than eclipsed by that of PPOs (especially local PPOs) since the Medicare Improvements for Patients and Providers Act (MIPPA) of 2008 required PFFS plans (with some county-specific exceptions) to have networks of providers by 2011.4
- HMOs. In absolute numbers, enrollment in HMOs grew more than other plan types. Enrollment in HMOs increased by 0.7 million to 10.7 million beneficiaries in 2015, a seven percent increase (Figure 3).
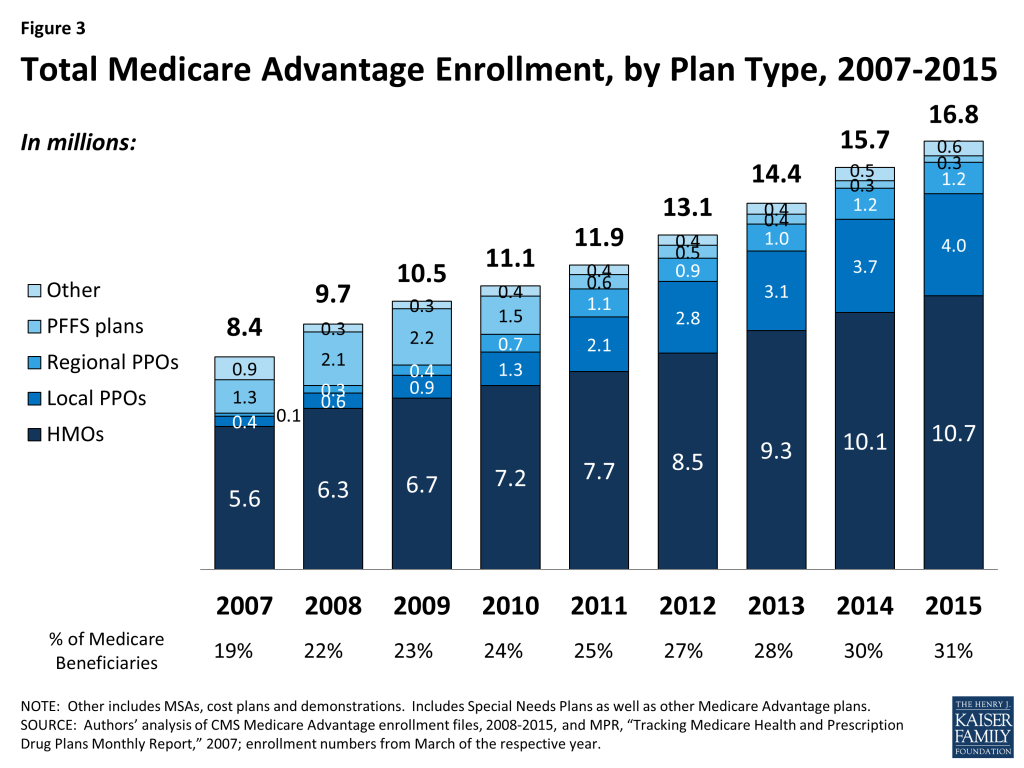
- PPOs. Enrollment in local PPOs increased by 0.3 million to 4.0 million beneficiaries in 2015, a nine percent increase. In contrast, enrollment in regional PPOs (1.2 million) remained flat between 2014 and 2015. Between 2007 and 2015, total PPO enrollment increased ten-fold from about 500,000 to 5.2 million, with most of the growth in local PPOs. Regional PPOs have had limited traction nationwide, although they account for a not insignificant share of the market in a small number of states (Table A1).5 –A key difference between an HMO and a PPO is that the latter provides enrollees with more flexibility to see providers outside of the plan’s provider network, although cost sharing associated with out-of-network providers typically is substantially higher than for providers in a plan’s network. Local PPOs, like HMOs, are open to beneficiaries who live in specified counties. Regional PPOs are required to serve areas defined by one or more states with a uniform benefit package across the service area.
- PFFS Plans. Enrollment in PFFS plans (0.3 million) has been fairly flat since 2014, and is substantially lower in 2015 than the high of 2.2 million enrolled in 2009.6 Enrollment has fallen precipitously since MIPPA of 2008 required PFFS plans in most parts of the country to have networks of providers. Among PFFS plan enrollees, 29% are in counties in which PFFS plans are exempted from network requirements.
Group Enrollment
Most Medicare beneficiaries who enroll in Medicare Advantage plans do so as individuals, but a small share is enrolled through groups, comprised largely of employment-sponsored Medicare Advantage plans for retirees. Under these arrangements, employers contract with a Medicare Advantage insurer to provide its retirees supplemental benefits, and Medicare pays the plan a fixed payment per enrollee to provide benefits covered by Medicare, and the employer pays a premium for any additional benefits.7
In 2015, 3.1 million of the 16.8 million Medicare Advantage enrollees (19%) were in a group plan, (Figure 4 and Table A2).
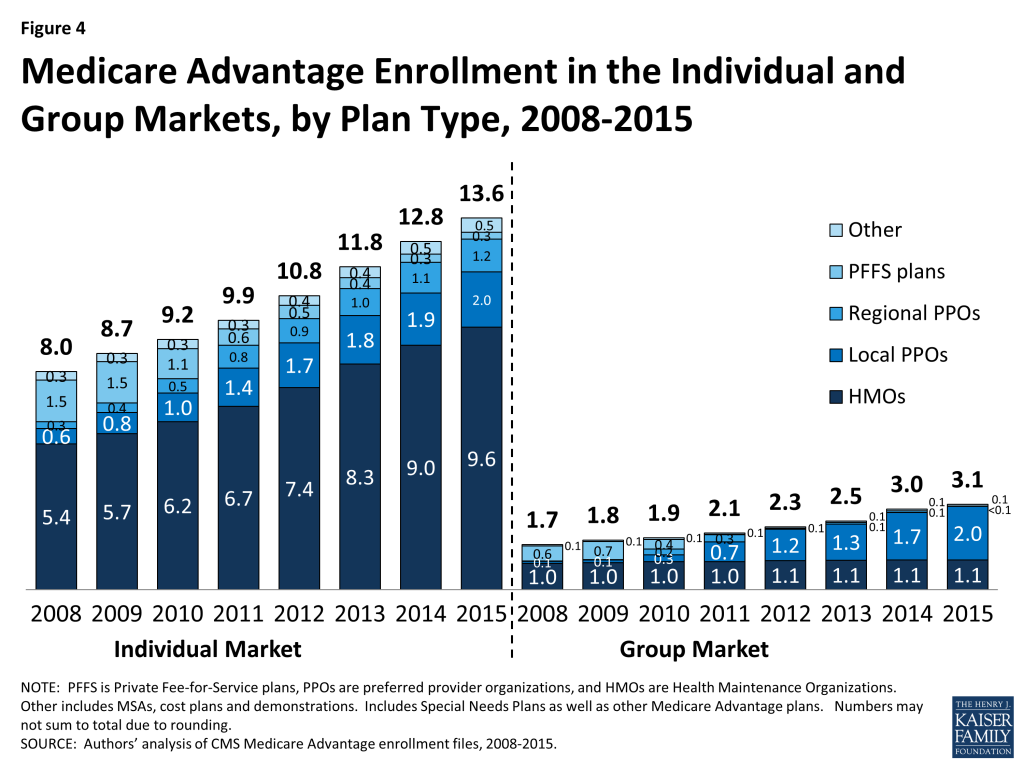
The share of Medicare Advantage enrollees in group plans has never been very large, but the numbers are growing, consistent with trends in the overall Medicare Advantage market. In some states, the share of Medicare Advantage enrollees in group plans is much larger than average, including West Virginia (55%), Michigan (49%), Kentucky (42%), Illinois (41%), Ohio (38%), Maryland (32%), New Hampshire (31%), and the District of Columbia (30%). Higher rates of Medicare Advantage group enrollment in these states are likely due to a higher prevalence of employers offering retiree health benefits, including public and unionized industries.8
Employers (and their retirees) appear to continue to favor local PPOs over HMOs, which contrasts with the individual market. Most of the enrollment growth in the group market between 2014 and 2015 was in local PPOs, with enrollment increasing to 2.0 million from 1.7 million.
According to the Medicare Payment Advisory Commission (MedPAC), group Medicare Advantage plans typically receive higher Medicare payments and have higher bids, on average, than plans offered in the individual Medicare Advantage market.9 Their analysis shows that the average payment to group Medicare Advantage plans is 106 percent of traditional Medicare spending whereas the average payment to all Medicare Advantage plans is 102 percent of traditional Medicare spending in 2015. MedPAC attributes the differences to incentives for firms in the group market to maximize Medicare revenue to offset employer costs by bidding at the benchmark, whereas firms in the individual Medicare Advantage market have an incentive to bid below the benchmark, in order to receive a rebate (a percent of the difference between the bid and the benchmark) with which they can provide extra benefits to individual plan enrollees.
Medicare Advantage Enrollment Growth by State
Enrollment increased in virtually all states in 2015, with the exception of Maryland in which enrollment declined by less than 1 percent (Table 1). Five states and the District of Columbia saw particularly large increases in enrollment (19% in SD, 18% in ND, 14% in DC, 14% in GA, 14% in IL, and 14% in ME). High rates of growth typically reflect small states with limited prior year enrollment whose growth rates are sensitive to small changes in enrollment; for example, South Dakota has the highest growth rate (19%) and has historically had relatively low enrollment in Medicare Advantage plans.
While HMOs are the most common type of plan nationally, they are not equally important in all states. For example, HMOs constitute 75 percent of Medicare Advantage enrollment in 11 states (AZ, CA, CO, CT, LA, MA, NJ, NV, RI, UT, and WA) but less than half of Medicare enrollment in 25 states, 6 of whom (AK, MT, ND, SD, VT, and WV) have less than 10 percent HMO enrollment (see Table A1). Geographic variation in the composition of Medicare Advantage plans is important since HMOs tend to perform better on certain measures of efficiency and tend to have lower premiums.10 In addition, there is more evidence on the quality of care in HMOs than in other model types.11
Enrollment Growth by County, based on Medicare Spending Quartiles.
Over the years, Congress and various Administrations have made a number of changes to payment and participation rules for Medicare Advantage plans. Many of these changes have revolved around plan payment levels, seeking to balance plan participation and plan choices for beneficiaries with parity in payments between traditional Medicare and Medicare Advantage. The ACA reduced payments to all plans, and varied payment policy with the level of traditional Medicare spending in counties, grouped evenly into four quartiles. In 2017, when payments are fully phased in, they will range from 95 percent of traditional Medicare spending for counties in the top quartile of spending to 115 percent of traditional Medicare spending in the bottom quartile of such spending, and 100 percent and 107.5 percent of traditional Medicare spending in the two middle quartiles.
As of 2015, payment reductions have been fully implemented in 78 percent of all counties nationwide; these counties account for 69 percent of all Medicare beneficiaries nationwide and 68 percent of all Medicare Advantage enrollees.
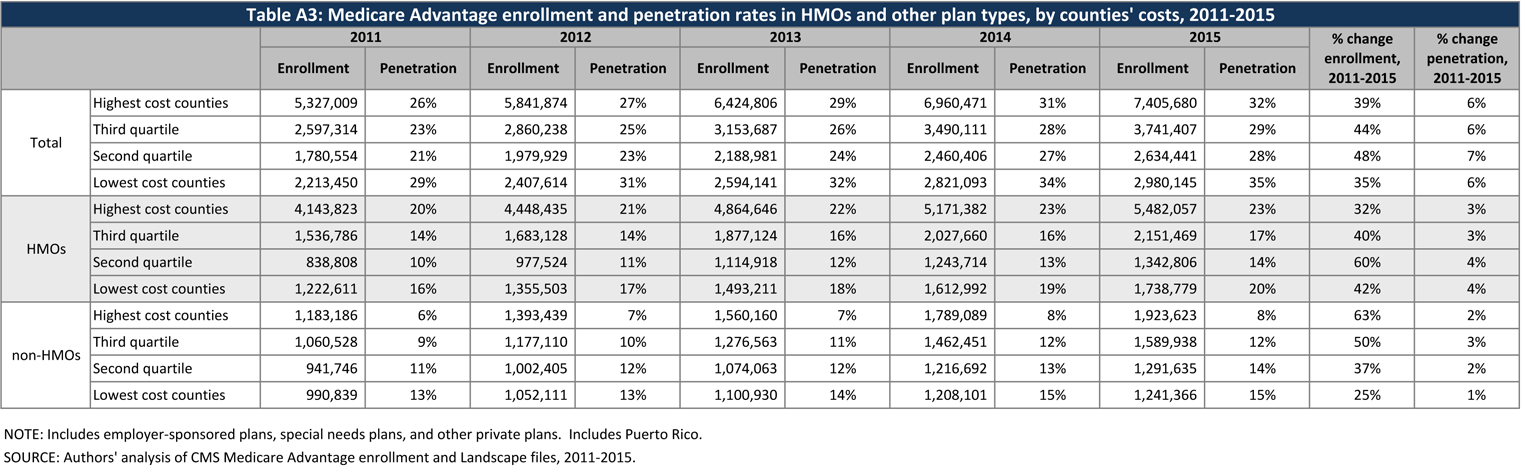
Enrollment continues to grow relatively equally across counties in each of the four quartiles of traditional Medicare spending (Table A3). Between 2014 and 2015, enrollment grew by 6 percent in both the highest quartile counties and in the lowest quartile counties, and by 7 percent each in the two middle quartiles. Overall penetration is also similar across the quartiles (ranging from 28% to 35%). Thus, enrollment continues to grow across counties, irrespective of changes in payments that differ according to traditional Medicare spending.
| Table 1: Medicare Advantage Enrollment and Penetration Rate, by State, 2014-2015 | ||||||
| State | 2014 Total Enrollment | 2015 Total Enrollment | Change in Total Enrollment, 2014-2015 | Percent Change in Enrollment, 2014-2015 | 2014 Penetration Rate | 2015 Penetration Rate |
| Total U.S. | 15,732,081 | 16,761,673 | 1,029,592 | 7% | 30% | 31% |
| Alabama | 220,640 | 238,091 | 17,451 | 8% | 24% | 25% |
| Alaska | N/A | 56 | N/A | N/A | N/A | <1% |
| Arizona | 401,626 | 425,454 | 23,828 | 6% | 38% | 38% |
| Arkansas | 107,713 | 114,326 | 6,613 | 6% | 19% | 19% |
| California | 2,061,617 | 2,127,666 | 66,049 | 3% | 38% | 38% |
| Colorado | 263,788 | 281,467 | 17,679 | 7% | 36% | 37% |
| Connecticut | 146,372 | 157,692 | 11,320 | 8% | 24% | 25% |
| Delaware | 12,623 | 13,841 | 1,218 | 10% | 7% | 8% |
| District of Columbia | 9,714 | 11,033 | 1,319 | 14% | 11% | 13% |
| Florida | 1,438,325 | 1,570,845 | 132,520 | 9% | 38% | 40% |
| Georgia | 404,628 | 460,670 | 56,042 | 14% | 28% | 31% |
| Hawaii | 108,143 | 110,465 | 2,322 | 2% | 46% | 46% |
| Idaho | 81,440 | 87,837 | 6,397 | 8% | 33% | 32% |
| Illinois | 326,678 | 371,007 | 44,329 | 14% | 16% | 18% |
| Indiana | 244,970 | 264,104 | 19,134 | 8% | 22% | 23% |
| Iowa | 77,032 | 81,541 | 4,509 | 6% | 14% | 14% |
| Kansas | 59,018 | 61,600 | 2,582 | 4% | 13% | 13% |
| Kentucky | 198,052 | 212,948 | 14,896 | 8% | 24% | 25% |
| Louisiana | 213,280 | 232,445 | 19,165 | 9% | 28% | 30% |
| Maine | 58,234 | 66,307 | 8,073 | 14% | 20% | 22% |
| Maryland | 76,464 | 76,375 | -89 | 0% | 9% | 8% |
| Massachusetts | 229,400 | 233,084 | 3,684 | 2% | 20% | 19% |
| Michigan | 547,372 | 595,239 | 47,867 | 9% | 30% | 32% |
| Minnesota | 448,301 | 480,474 | 32,173 | 7% | 51% | 53% |
| Mississippi | 69,962 | 76,776 | 6,814 | 10% | 13% | 14% |
| Missouri | 285,066 | 311,364 | 26,298 | 9% | 26% | 28% |
| Montana | 31,125 | 34,758 | 3,633 | 12% | 17% | 18% |
| Nebraska | 33,507 | 34,982 | 1,475 | 4% | 13% | 11% |
| Nevada | 135,599 | 146,094 | 10,495 | 8% | 33% | 33% |
| New Hampshire | 15,905 | 17,295 | 1,390 | 9% | 6% | 7% |
| New Jersey | 219,494 | 222,846 | 3,352 | 2% | 15% | 15% |
| New Mexico | 107,064 | 113,807 | 6,743 | 6% | 30% | 31% |
| New York | 1,151,620 | 1,212,239 | 60,619 | 5% | 35% | 37% |
| North Carolina | 475,432 | 512,924 | 37,492 | 8% | 28% | 29% |
| North Dakota | 15,202 | 17,878 | 2,676 | 18% | 14% | 15% |
| Ohio | 794,226 | 811,503 | 17,277 | 2% | 38% | 38% |
| Oklahoma | 106,706 | 111,013 | 4,307 | 4% | 16% | 17% |
| Oregon | 305,794 | 323,765 | 17,971 | 6% | 43% | 44% |
| Pennsylvania | 971,144 | 1,001,864 | 30,720 | 3% | 39% | 40% |
| Rhode Island | 70,627 | 71,009 | 382 | 1% | 36% | 35% |
| South Carolina | 193,641 | 209,812 | 16,171 | 8% | 22% | 23% |
| South Dakota | 22,242 | 26,400 | 4,158 | 19% | 15% | 17% |
| Tennessee | 376,577 | 412,042 | 35,465 | 9% | 32% | 34% |
| Texas | 990,399 | 1,098,678 | 108,279 | 11% | 29% | 31% |
| Utah | 107,139 | 113,034 | 5,895 | 6% | 34% | 33% |
| Vermont | 8,368 | 8,984 | 616 | 7% | 7% | 7% |
| Virginia | 196,993 | 206,427 | 9,434 | 5% | 15% | 16% |
| Washington | 329,087 | 348,467 | 19,380 | 6% | 29% | 30% |
| West Virginia | 96,604 | 99,454 | 2,850 | 3% | 24% | 24% |
| Wisconsin | 352,842 | 388,732 | 35,890 | 10% | 35% | 38% |
| Wyoming | 1,997 | 2,071 | 74 | 4% | 3% | 2% |
| NOTE: Includes employer-sponsored plans, special needs plans, and other private plans. N/A indicates too few (less than 50) enrollees to report. Total U.S. includes Puerto Rico.SOURCE: Authors’ analysis of CMS Medicare Advantage enrollment and Landscape files, 2014-2015. | ||||||
Medicare Advantage Penetration
While Medicare Advantage enrollment is increasing in many states, in 6 states (AK, DE, MD, NH, VT and WY) less than 10% of beneficiaries are enrolled in Medicare Advantage plans in 2015, which was also the case in at least the prior three years (Figure 5). In contrast, in 22 states (versus 18 states in 2014 and 15 states in 2013) more than 30 percent of beneficiaries are enrolled in Medicare Advantage plans in 2015. Additionally, in 5 states (FL, HI, MN, OR, and PA) more than 40 percent of beneficiaries are enrolled in Medicare Advantage plans, and Medicare Advantage enrollment these states account for 6% of all Medicare beneficiaries and 21% of all Medicare Advantage enrollees. This variation reflects the urban origins of health maintenance organizations (HMOs) in Medicare Advantage and other factors, such as the history of managed care in the state and the prevalence of employer sponsored insurance for retirees. Within states, Medicare Advantage penetration varies across counties. For example, 43 percent of beneficiaries in Los Angeles County, California are enrolled in Medicare Advantage plans compared to only 8 percent of beneficiaries in Santa Cruz County, California.
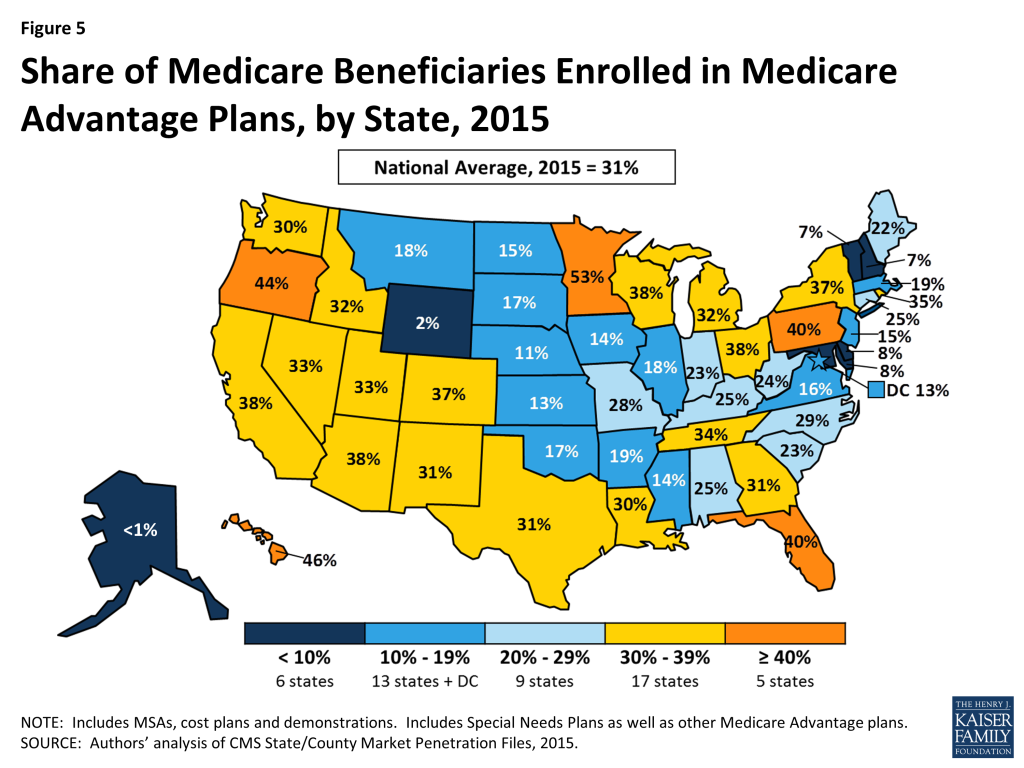
Premiums
Medicare Advantage enrollees are responsible for paying the Part B premium, in addition to any premium charged by the plan. The Medicare Advantage premium paid by enrollees reflects the difference between the plan’s costs of providing Part A and B benefits and any supplemental benefits offered, and the federal payment to the plan for the benefits. Plans receive a percentage of the difference between their bid and the maximum federal payment (known as a rebate) and are required to use this amount to offer extra benefits, reduce cost sharing, or reduce the Part B premium. If the plan offers the Part D drug benefit, as most plans do, the plan may also use the rebate to reduce the Part D premium.
This brief analyzes premiums for Medicare Advantage plans that offer prescription drug benefits (MA-PDs) because the vast majority (88%) of Medicare Advantage enrollees is in MA-PDs.
Average Premium Trends
The average MA-PD enrollee pays a monthly premium of about $38 in 2015, a $3 per month (7%) increase from 2014 (Figure 6). Actual premiums paid by enrollees vary by plan type, locale, and characteristics, such as relative breadth of the provider network and/or benefits.12
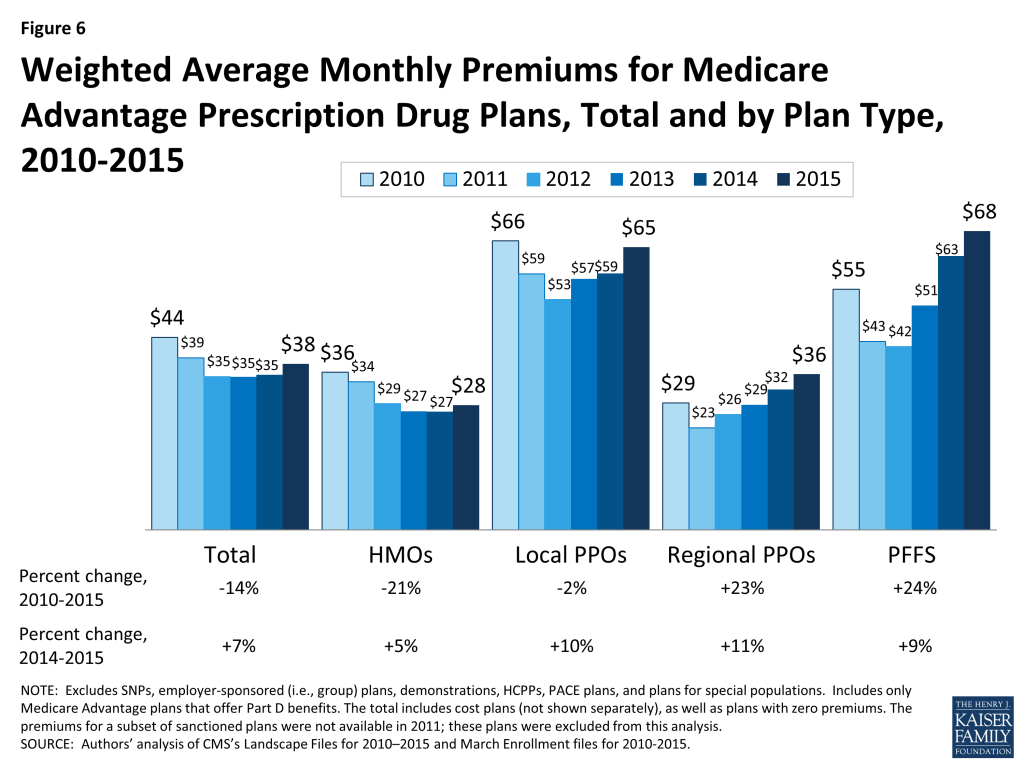
Average premiums range from $28 per month (for HMO enrollees) to $68 per month (for PFFS plan enrollees). Average premium increases were lower for HMO enrollees ($1 per month) than for local PPO enrollees ($6 per month), regional PPO enrollees ($4 per month), and PFFS plan enrollees ($5 per month).
Average Medicare Advantage premiums for HMO enrollees and local PPO enrollees are lower in 2015 than in 2010, prior to the ACA payment changes; premiums are higher in 2015 than in 2010 for regional PPOs and PFFS plans.
Zero Premium Plans
As in prior years, most Medicare beneficiaries (78%) had a choice of at least one MA-PD that charged no additional premium for coverage, other than the monthly Part B premium, also known as “zero premium plans”.13
Between 2014 and 2015, the share of enrollees in zero premium MA-PDs declined from 56 percent to 48 percent, which is about the same share as in 2010 (Figure 7). Similar to prior years, a larger share of enrollees in HMOs was enrolled in zero-premium plans (59%) than enrollees in regional PPOs (39%) or local PPOs (18%). No zero premium PFFS plans are offered in 2015.
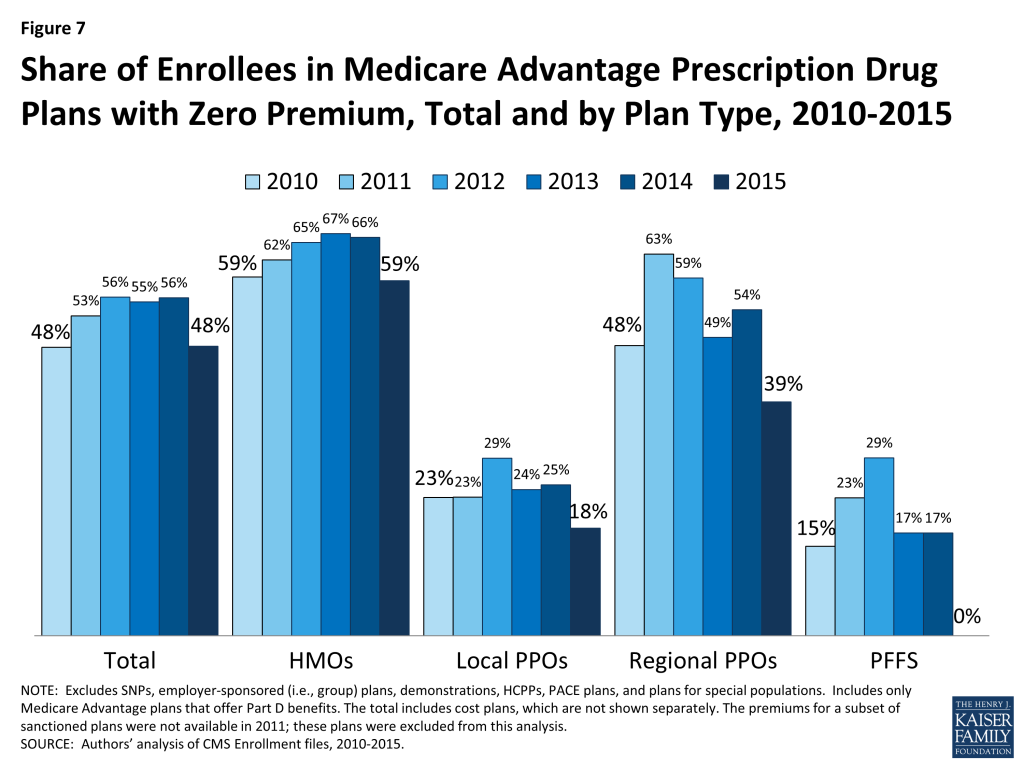
Premium Variation Across States
Comparing premiums across states is complicated by the fact that premiums reflect many factors, including the underlying costs of care in a given county relative to the national average, the level of payments to Medicare Advantage plans in the area, and firms’ strategy about whether to use plans’ rebates to offer extra benefits, reduce cost-sharing, or lower premiums. Additionally, as previously discussed, premiums vary across plan types, with HMOs having the lowest average premiums, and enrollment by plan type varying across states.
Average monthly premiums paid by enrollees vary across states (Figure 8). While the average premium nationwide is $38 per month, in four states (MA, MI, MN, and PA,) average monthly premiums exceed $90 in 2015.14 In contrast, average monthly premiums are less than $20 in seven states (AZ, IA, FL, LA, MO, NV, and TX). (States with fewer than 50,000 Medicare Advantage enrollees are not displayed in the exhibit).
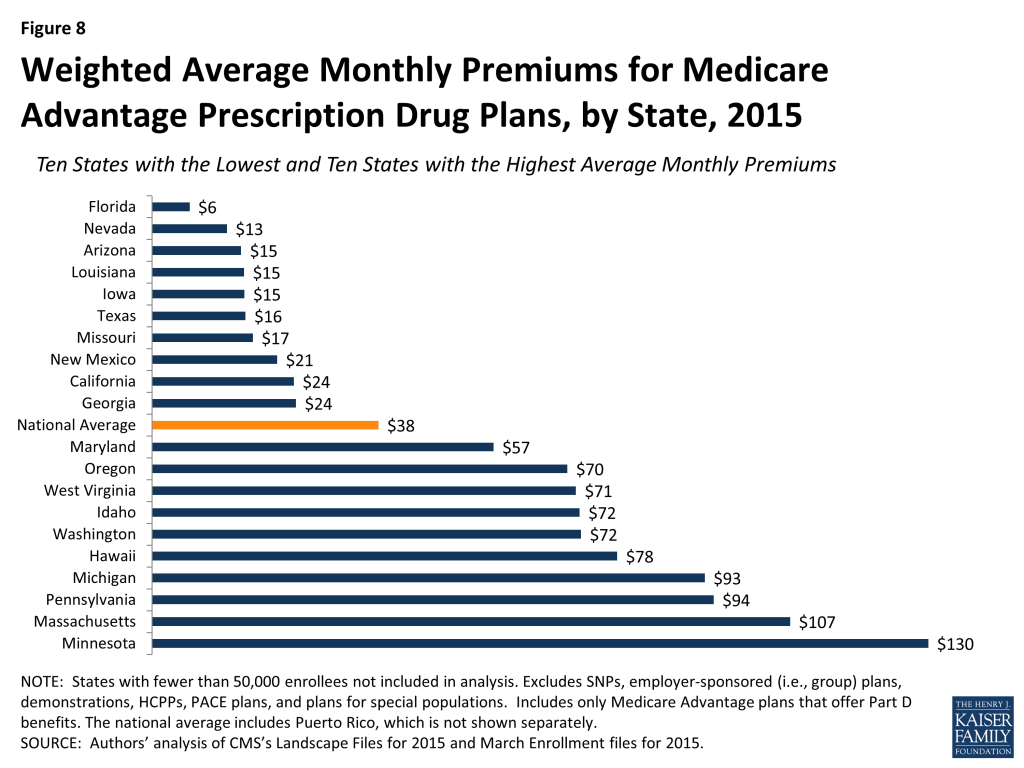
Premiums also vary greatly within a state since plans and federal payments to plans vary by county. For example, in Los Angeles County, California, Medicare Advantage enrollees pay an average of $2 per month for an MA-PD. In contrast, in San Francisco County, California, enrollees pay an average of $65 per month for an MA-PD. Similarly, in New York County, New York, enrollees pay an average of $18 per month for an MA-PD whereas in Albany County, New York, enrollees pay an average of $73 per month for an MA-PD.
Structuring Cost Sharing in the Medicare Benefit
Medicare Advantage plans are required to provide all Medicare covered services. In addition, plans are required to limit enrollees’ out-of-pocket expenditures for Part A and Part B covered services and may provide additional benefits that are not covered by traditional Medicare. Out-of-pocket limits define ultimate financial liability for Medicare benefits for in-network Medicare-covered benefits and are especially important for people with relatively high health expenses. Actual financial liability will vary with a beneficiary’s health status and use of medical care.
Out-Of-Pocket Limits
Although traditional Medicare does not include an annual out of pocket limit on cost sharing for Medicare A and B benefits, the CMS began requiring all Medicare Advantage plans to have a limit no higher than $6,700 annually, and recommended a limit of $3,400 or lower, for in-network services, as of 2011.15
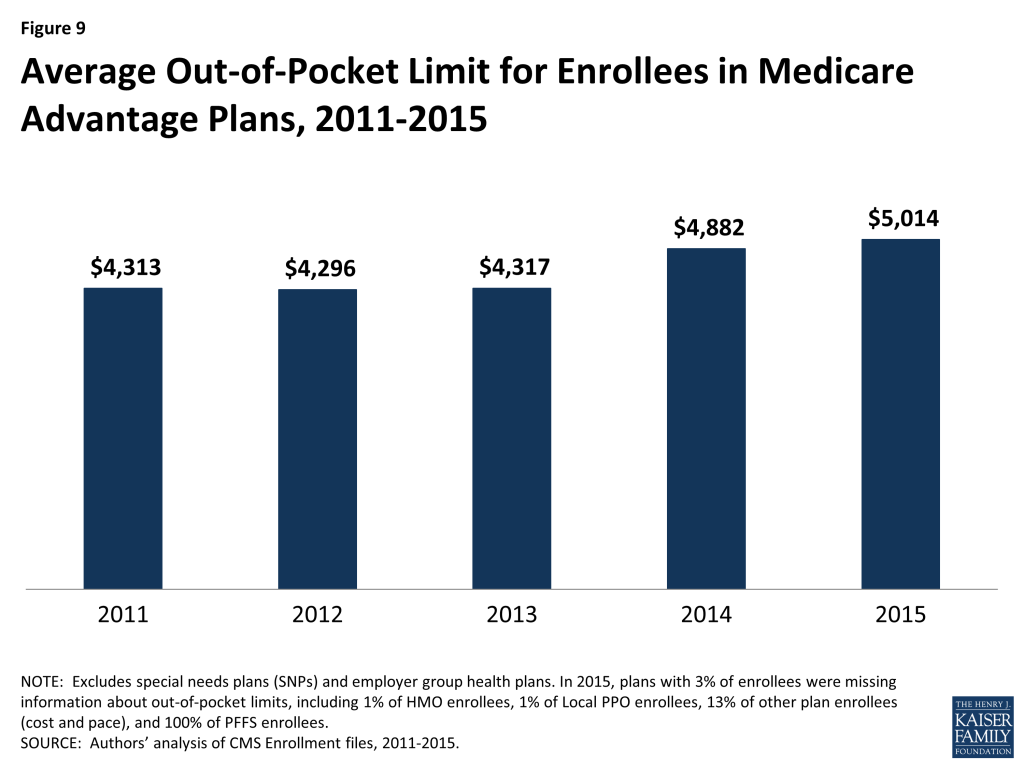
In 2015, the average out-of-pocket limit for Medicare Advantage enrollees is $5,041 (Figure 9). Nearly half of all enrollees (46%) are in plans with limits above $5,000 in 2015, roughly the same share as in 2014. Between 2011 and 2015, the share of enrollees in plans with a limit above $5,000 nearly doubled, from 24 percent in 2011 to 46 percent in 2015. Concurrently, the share of beneficiaries in plans with limits below $3,400 has declined from 51 percent in 2011 to 27 percent in 2015.
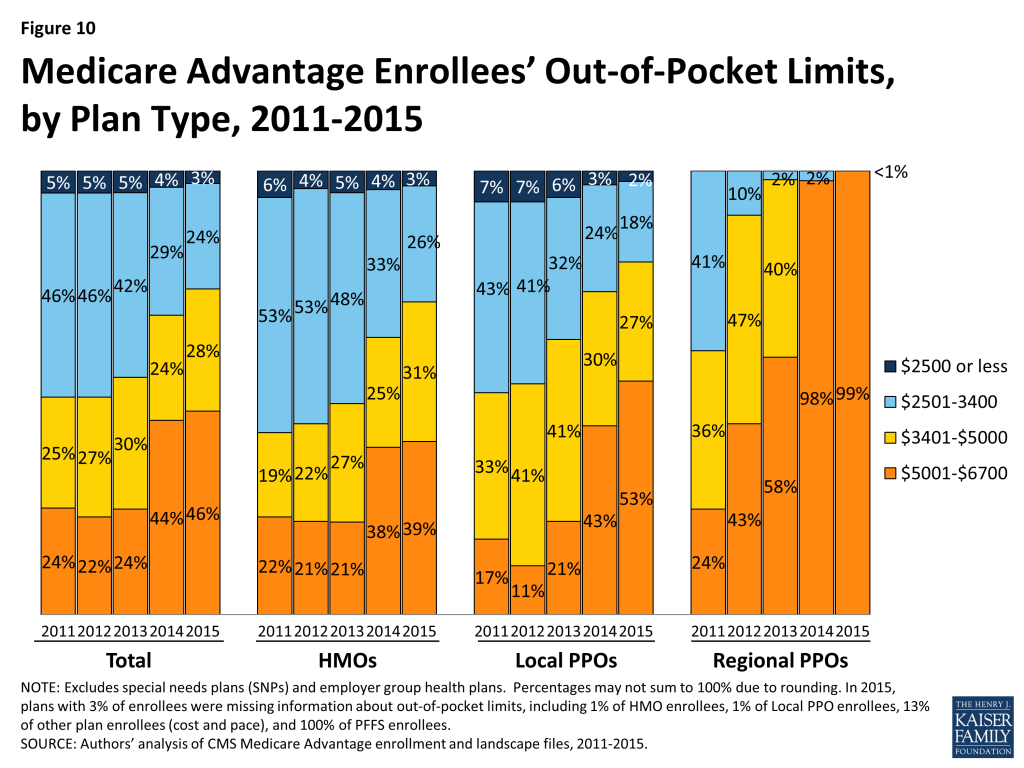
HMOs have generally had lower out-of-pocket limits than local PPOs or regional PPOs, and this remains the case in 2015 (Figure 10). Virtually all regional PPO enrollees (99%) and more than half of local PPO enrollees (53%), compared to more than one-third of HMO enrollees (39%), are in plans with limits above $5,000 in 2015. Less than one-third (29%) of HMO enrollees are in plans with limits below $3,400 in 2015, a decline from 59 percent of HMO enrollees in 2011. About one in five (20%) local PPO enrollees and less than 1 percent of regional PPO enrollees are in plans with limits below $3,400.
Part D Cost Sharing
The standard Medicare Part D benefit in 2015, for both stand-alone prescription drug plans (PDPs) and MA-PDs, has a $320 deductible and 25 percent coinsurance up to an initial coverage limit of $2,960 in total drug costs, followed by a coverage gap (the so-called “donut hole”), until their total out of pocket Part D spending reaches $4,700 when the catastrophic limit kicks in and beneficiaries pay 5 percent of the cost of drugs.
Part D Deductibles
Medicare Advantage plans have the flexibility to vary the design of their Part D benefit; however, the deductible cannot exceed $320 in 2015. In 2015, most MA-PD enrollees (58%) are in plans without a Part D deductible (Figure 11). Only 11 percent are in plans with the maximum deductible of $320. Nearly one-third of MA-PD enrollees have deductibles ranging from $160-$319.
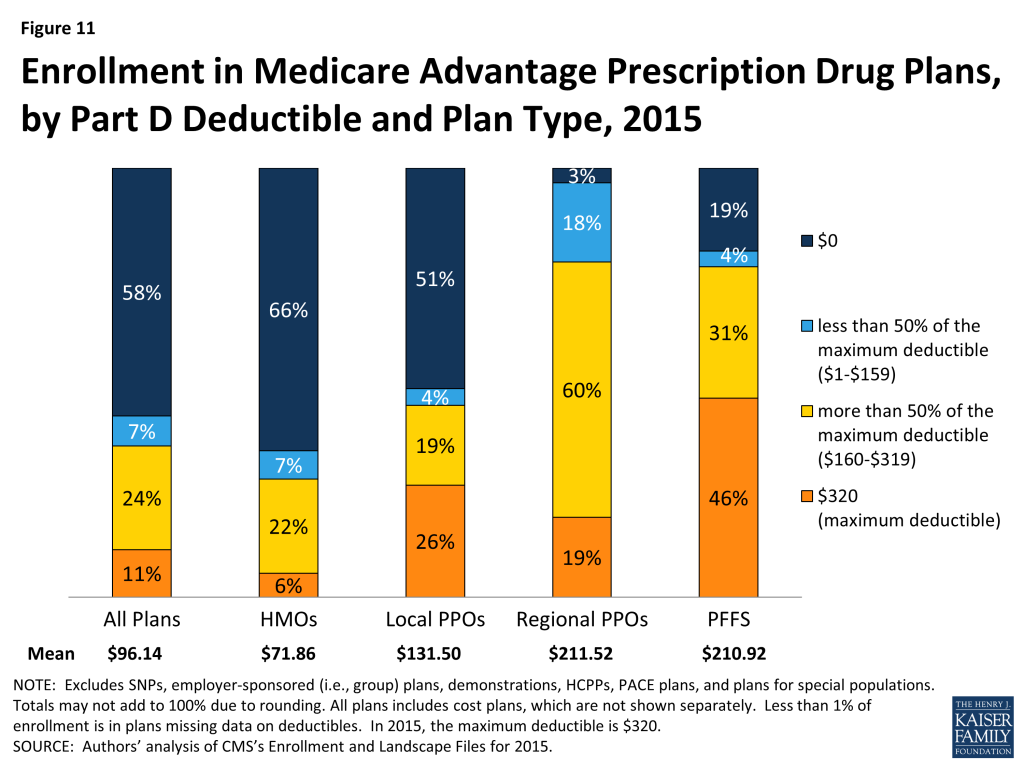
Two-thirds (66%) of MA-PD HMO enrollees and half (51%) of local PPO enrollees do not have a Part D deductible. In contrast, the preponderance of regional PPO enrollees (97%) and PFFS plan enrollees (81%) do have a Part D deductible. Six percent of HMO enrollees are in plans with the maximum deductible, compared to 26 percent of local PPO enrollees, 19 percent of regional PPO enrollees, and 46 percent of PFFS plan enrollees.
Coverage in the Part D Donut Hole
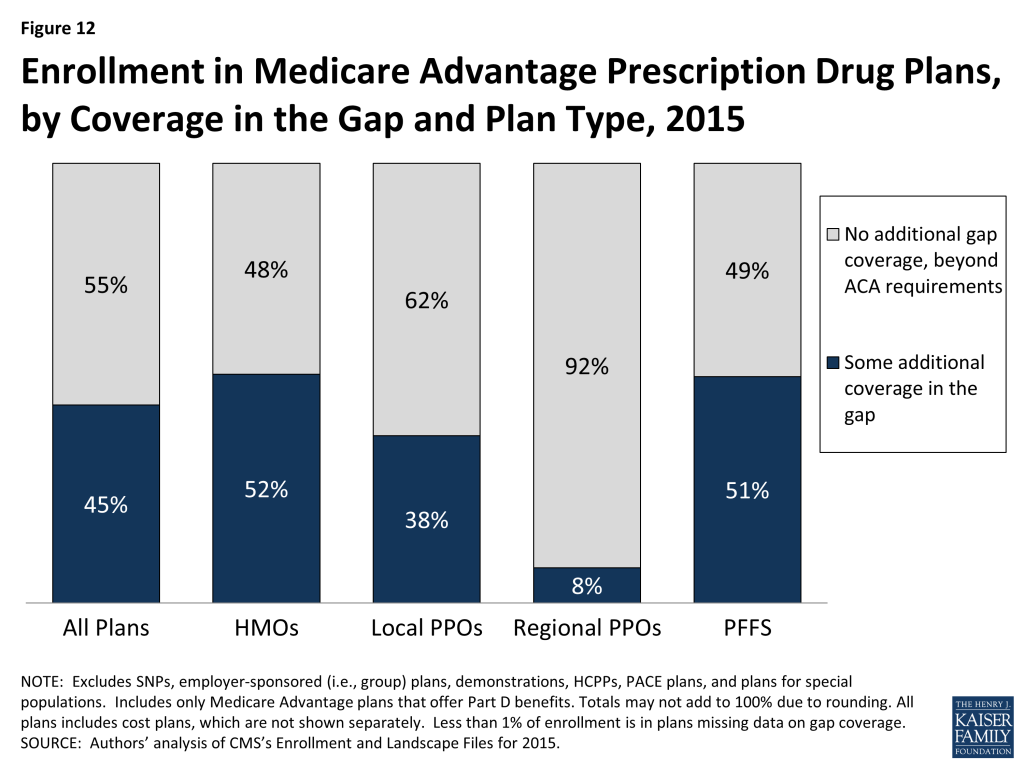
The ACA gradually closes the coverage gap by 2020. Plans have the option to close the gap before then, but few have. In 2015, 45 percent of enrollees are in plans that provide some additional coverage – beyond what is required by law – a decline from 51 percent in 2014 (Figure 12). Enrollees in plans with no additional gap coverage will pay 45 percent of the total costs of brand-name drugs and 65 percent of the total cost of generics in the gap in 2015 until they reach the catastrophic limit. A larger share of enrollees in PFFS plans (51%) and HMOs (52%) are in plans that provide some coverage in the gap, than enrollees in local PPOs (38%) or regional PPOs (8%).16
Star Quality Ratings
For many years, the CMS has posted quality ratings of Medicare Advantage plans to provide beneficiaries with additional information about plans offered in their area. All plans are rated on a 1 to 5 star scale, with 1 star representing poor performance, 3 stars representing average performance, and 5 stars representing excellent performance. The quality scores for Medicare Advantage plans are derived from plan and beneficiary information collected in three surveys – HEDIS®, CAHPS®, and HOS – and administrative data. CMS assigns quality ratings at the contract level, rather than for each individual plan, meaning that each plan covered under the same contract receives the same quality rating (and most contracts cover multiple plans of the same type).
In 2012, Medicare Advantage plans began receiving bonus payments based on quality ratings. These payments were initially established in the ACA and provided for bonuses to plans that receive 4 or more stars and to unrated plans beginning in 2012. In addition, CMS launched a demonstration for 2012 through 2014 that increased the size of bonuses for these plans, and also provided bonuses to plans rated as average (receiving 3 or 3.5 stars), using the same 1 to 5 star scale. CMS indicated that one goal of the demonstration was to provide an initial boost to plans in meeting the more stringent 4 star goals.17 In 2015, the bonus payments have reverted back to those that were authorized under the ACA, and plans with 3 or 3.5 stars do not receive bonus payments. Beneficiaries can enroll in a plan with 5 stars at any time during the year, not just during the annual open enrollment period.
Between 2013 and 2015, the share of enrollees in plans with 4 or more stars has steadily increased, from 37 percent in 2013 to 61 percent in 2015 (Figure 13). Much of the increase in enrollment in plans with four or more stars has occurred in the plans with 4 or 4.5 stars, while the share of enrollees in plans with 5 stars has been relatively stable.
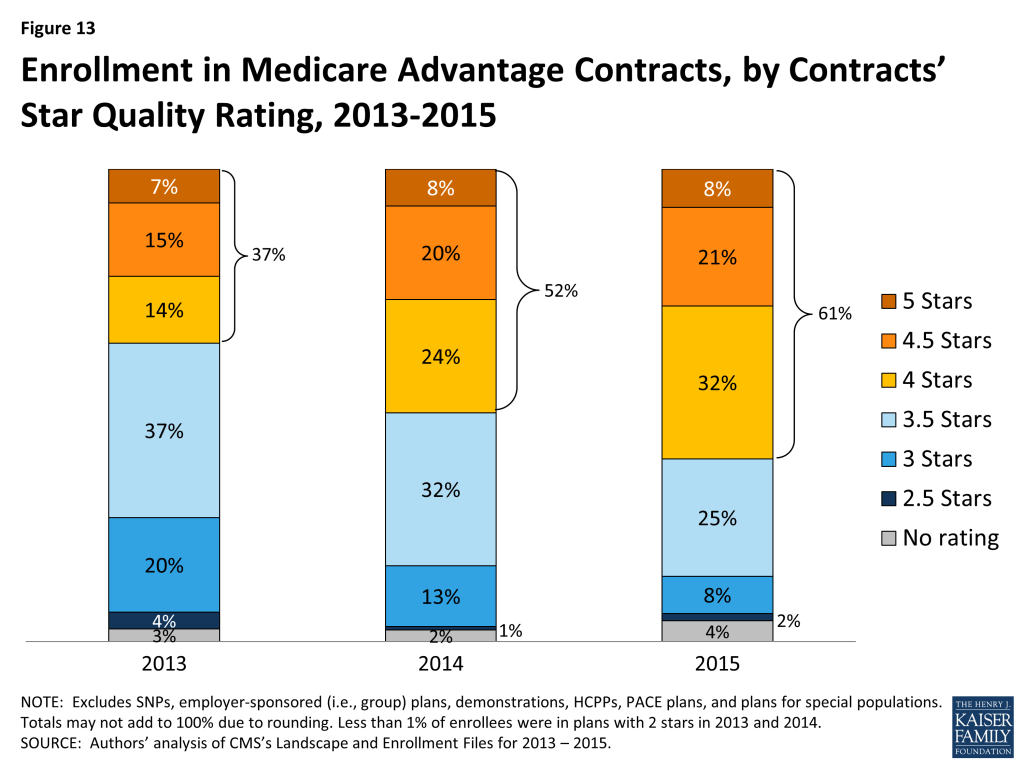
Notably, while a larger share of beneficiaries is in plans with relatively high star ratings, seniors have said in focus groups that they do not use the star ratings to select their plan.18 Nonetheless, the star ratings may be correlated with factors that seniors do use to select their plan, including provider networks, and plan benefits and costs, and thus may be correlated with enrollment. It is noteworthy that the share of beneficiaries in plans with 5 stars did not materially change between 2013 and 2015. Some have argued that the measures required to achieve 5 stars are more demanding than lower level star ratings, requiring integration that some plans find more difficult to achieve.
Medicare Advantage Firms
Enrollment by Firm
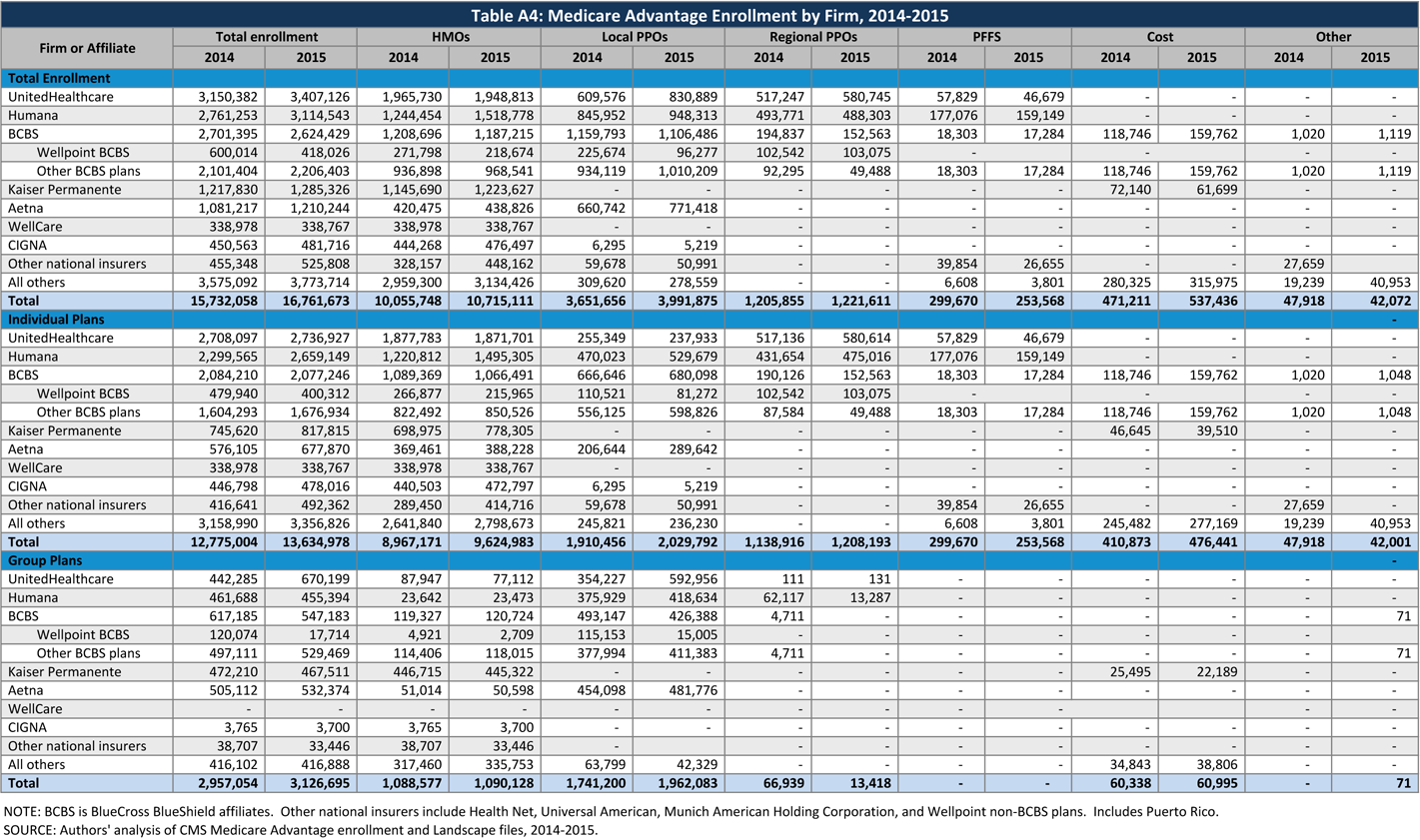
As in prior years, Medicare Advantage enrollment in 2015 tends to be highly concentrated among a small number of firms (Figure 14 and Table A4). In 2015, six firms or BCBS affiliates accounted for 72 percent of the market: UnitedHealthcare (20%), Humana (19%), Blue Cross Blue Shield (BCBS) affiliated plans (16%), Kaiser Permanente (8%), Aetna (7%), and Cigna (3%). Another six national firms account for 5 percent of the market, including Wellcare, HealthNet, Universal American, Munich American Holding Corporation, and Wellpoint plans not affiliated with BCBS. The remaining enrollees are in plans offered by more locally or regionally focused firms.
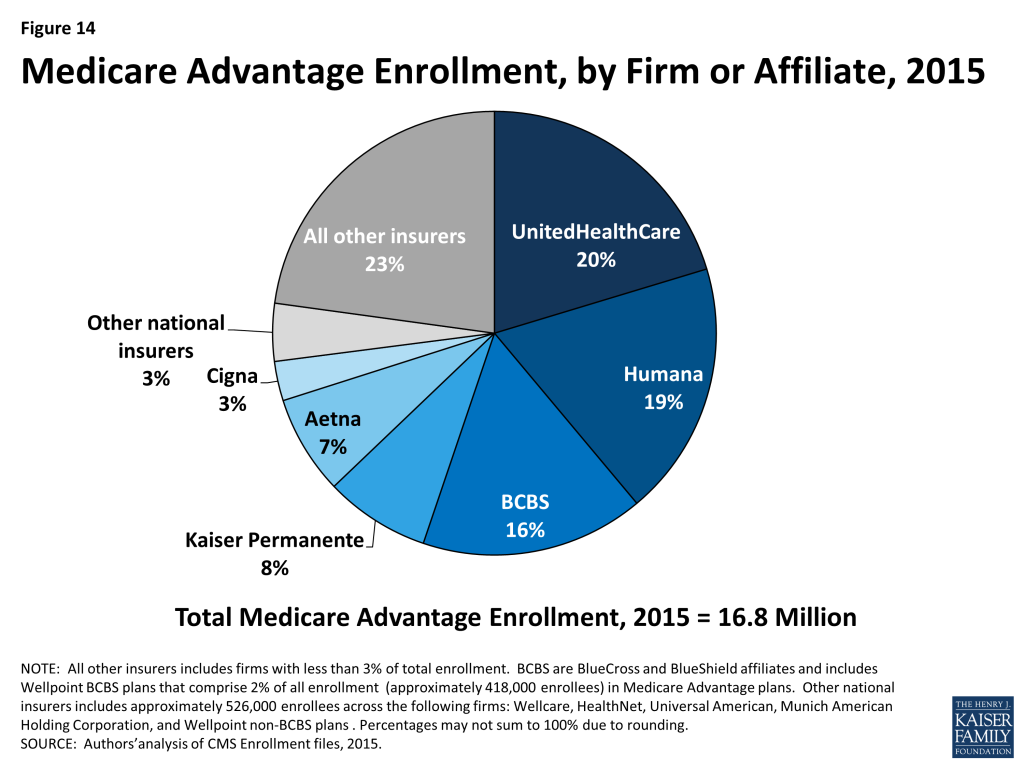
Enrollment in Humana’s plans in absolute numbers grew by more than 350,000 beneficiaries between 2014 and 2015 – more than any other national firm – and its national share of the Medicare Advantage market increased from 17% in 2014 to 19% in 2015. UnitedHealthcare and Aetna also had large increases in enrollment, growing by more than 250,000 and 125,000, respectively, between 2014 and 2015. Other national firms saw smaller changes in enrollment between 2014 and 2015, including Wellpoint BCBS affiliated plans, which had a net decline in enrollment.
Firms differ in how they position themselves in the market, including the plan types they offer. Almost all of Kaiser Permanente’s enrollees (95%) are in HMOs with the remainder (5%) in similarly structured cost plans (Figure 15). In contrast, UnitedHealthcare’s enrollment is in HMOs, local PPOs, regional PPOs, and PFFS plans, and enrollment among plan types has shifted somewhat between 2014 and 2015. A smaller share of UnitedHealthcare’s enrollees is in HMOs in 2015 than in 2014 (57% versus 62%, respectively) and a larger share are in local PPOs (24% versus 19%, respectively).
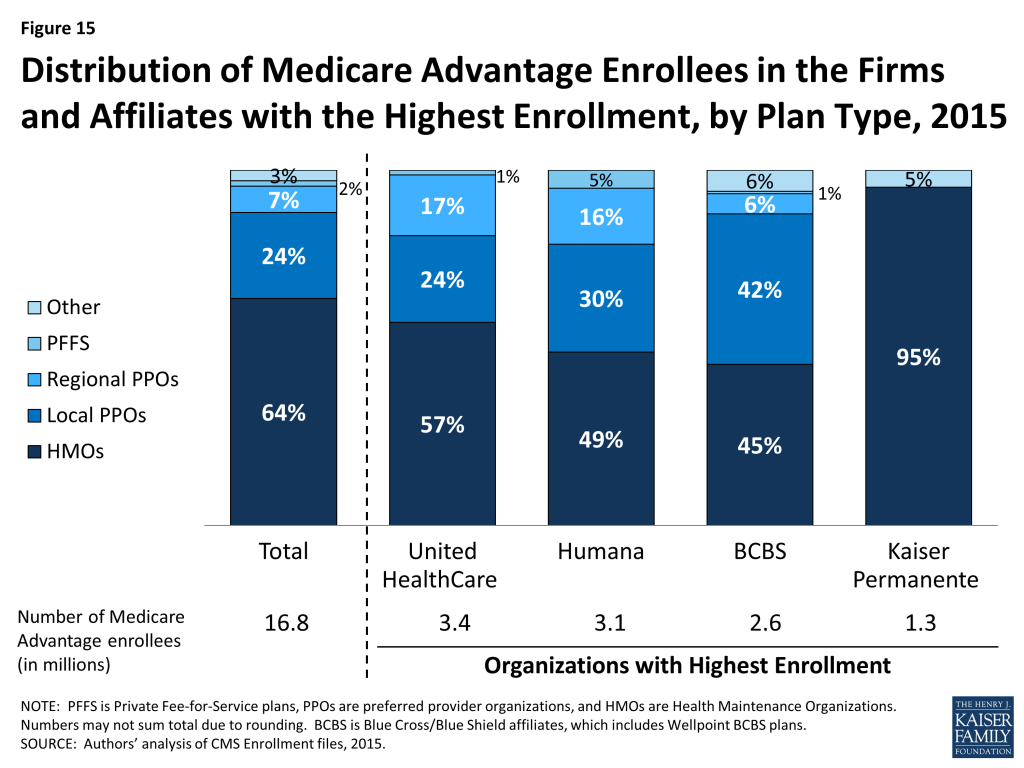
Compared to UnitedHealthcare, Humana and BCBS affiliated plans have a smaller share of their enrollment in HMOs (49% for Humana and 48% for BCBS versus 57% for United Healthcare). Humana’s distribution of enrollment across plan types continues the shift from earlier years when a much larger share of Humana’s enrollees was in PFFS plans. The share of Humana’s enrollees in HMOs increased from 45 percent in 2014 to 49 percent in 2015, while the share of Humana’s enrollees in other types of plans decreased.
Group Enrollment by Firm
Most of the growth in Medicare Advantage enrollment is in the individual market, but enrollment through group plans has been a major factor in the experience of some firms, and for UnitedHealthcare in particular (Table A4). Enrollment in group plans represents 20 percent of total enrollment in UnitedHealthcare plans, up from 14 percent in 2014. Similar to 2014, growth in the group market accounts for almost all of the net growth in UnitedHealthcare’s enrollment over the past year.
As in prior years, enrollment in the group market in 2015 is particularly important to Aetna (44% of enrollment, down from 47% in 2014) and Kaiser Permanente (36% of enrollment, down from 39% in 2014). Group enrollment historically has been less central to Humana’s strategy (15% of enrollment, down from 17% in 2014). Notably, all three firms saw stronger growth in their individual enrollment than group enrollment (with both Kaiser Permanente and Humana experiencing an actual decline in such enrollment). Total Medicare Advantage enrollment in Wellpoint BCBS’s plans also declined between 2014 and 2015 in part due to the large decline in group enrollment (from roughly 120,000 to 17,000). The role of individual versus group accounts in firm enrollment will vary with firm strategy, where firms are located in relation to large group accounts, and decisions made by those accounts about whether to continue retiree benefits and how to structure them (i.e., group products versus subsidies for individual purchase of products and which plans to offer or subsidize).
Firm Market Concentration by State
As is the case nationally, a small number of firms dominate Medicare Advantage enrollment in most states (Figure 16). Similar to prior years, in all but one state (NY), the three largest firms or BCBS affiliates account for more than 50 percent of enrollment. In 38 states and the District of Columbia, at least 75 percent of enrollment is in the three largest firms, including 17 states in which at least 90 percent of enrollment is in the three largest firms. Some states with highly concentrated markets (three firms accounting for at least 90 percent of enrollment) have Medicare Advantage penetration rates below the national average (AK, DE, KS, KY, MS, MT, ND, NE, SC, SD, VT, WV, WY), but several other such states do not (LA, NC, NV, RI).
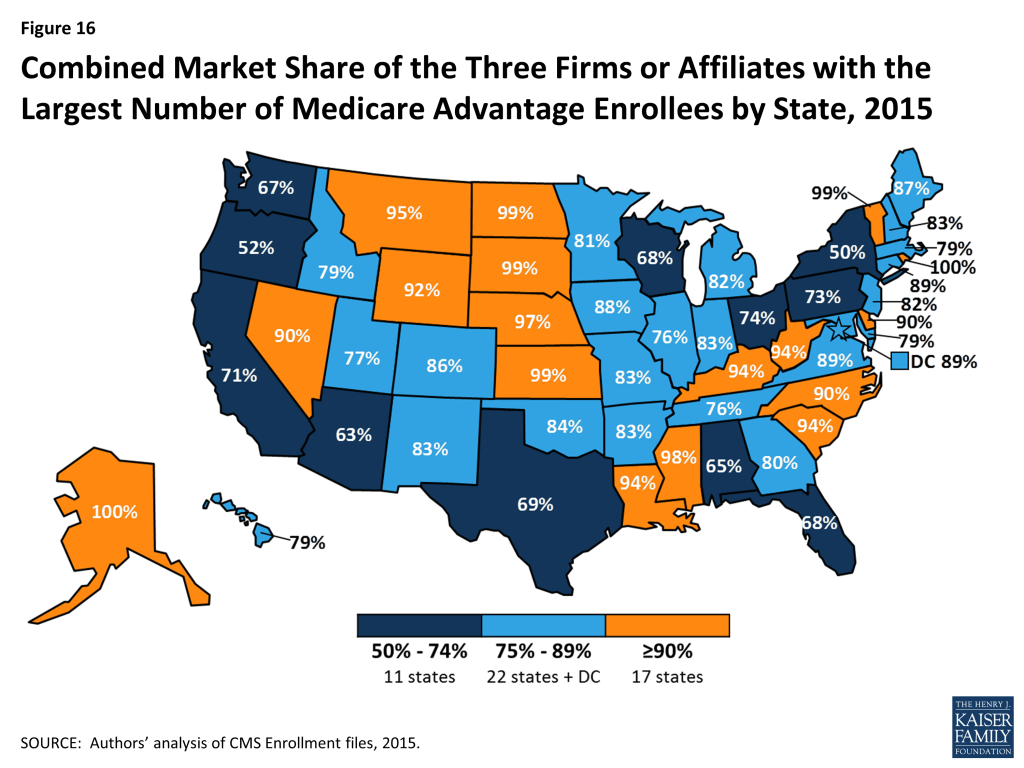
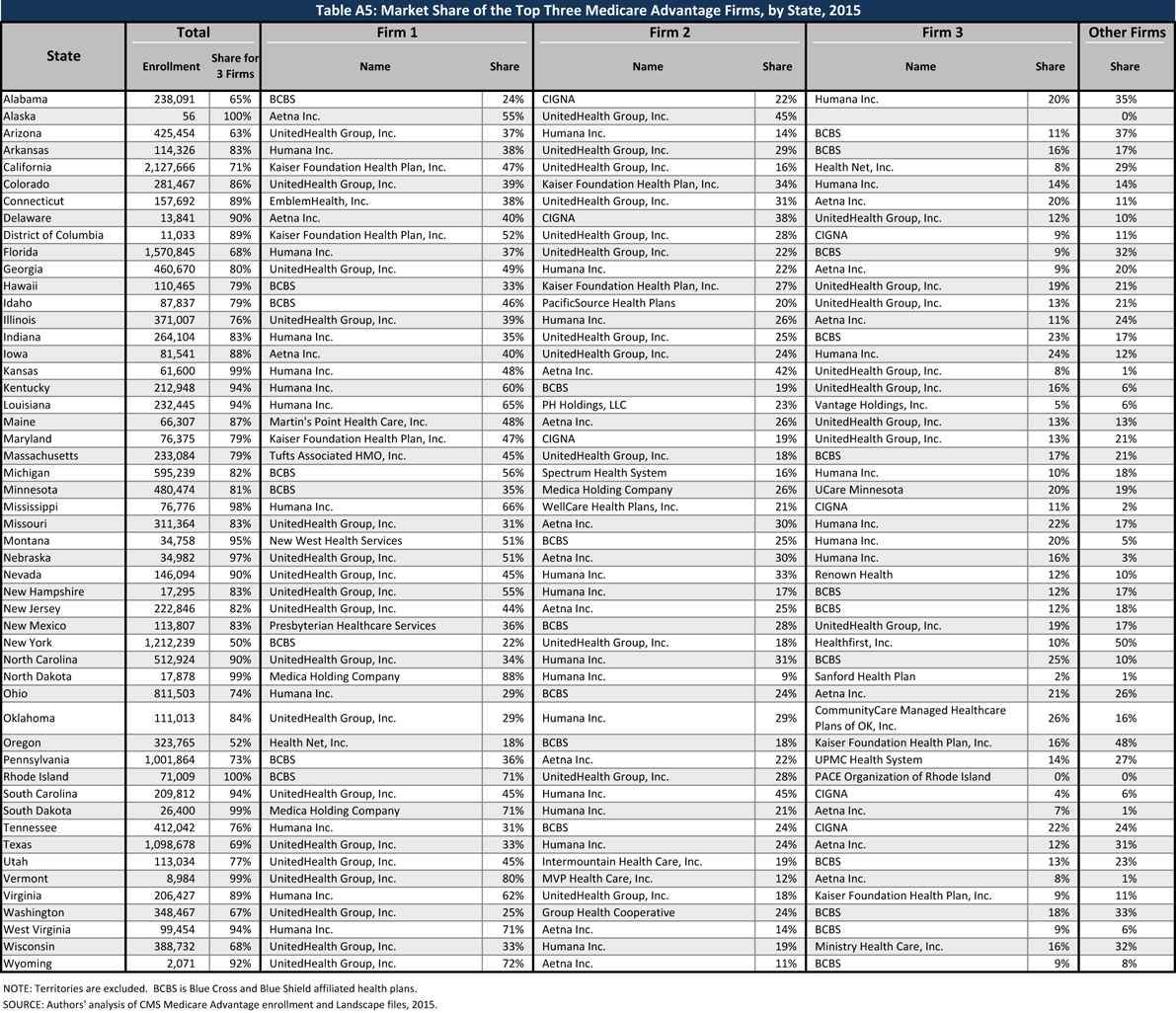
In 15 states and the District of Columbia, one company has more than half of all Medicare Advantage enrollment – an indicator that these markets that may not be very competitive (Table A5). For the most part these large firms include large players dominant nationally, but in some cases they are local organizations that may be small nationally but having a substantial share in many states. United Healthcare has the largest share in 18 states and is among the top three firms in an additional 19 states and the District of Columbia. Humana has the largest enrollment in 11 states and is among the top 3 firms in another 19 states. Plans offered by BCBS affiliates have the most enrollees in 8 states and are among the top firms in another 18 states. Kaiser Permanente’s presence is more geographically focused than other major national firms, with a heavy concentration in California, Colorado, the District of Columbia and Maryland. Kaiser Permanente has more enrollees than any other firm in California, the District of Columbia and Maryland.
Similar to prior years, locally dominant plans, that is, those with the most Medicare Advantage enrollees in their state include EmblemHealth (CT), Martin’s Point Health are (ME), Tufts Associated HMO (MA), New West (MT), Presbyterian Healthcare Services (NM), and Medica Holding Company (ND and SD). While these large plans do not necessarily have a large national presence, they are very important in some local markets where their enrollment may equal or exceed some national players. In 2015, local firms include a total of 3.7 million Medicare Advantage enrollees, or 23 percent of Medicare Advantage enrollment.
Discussion
Despite controversy over the reductions in payments for Medicare Advantage plans that were included in the ACA, enrollment in Medicare Advantage plans continues to grow nationally, by state, and across quartiles of traditional Medicare spending. As of 2015, the Medicare Advantage payment reductions have been fully phased in for the majority of counties.
While Medicare Advantage premiums have remained relatively flat, out-of-pocket limits have been increasing over the past few years, providing less financial protection to Medicare enrollees with significant medial needs than they have in the past. Additional work is needed to understand plans’ cost-sharing and provider networks, including changes over time and variation across plans. A key concern is whether beneficiaries have the information they need to make fully informed health plan choices from one year to the next, taking into account changes in their plan’s coverage and/or provider network, and changes in their own health care needs.
As in prior years, enrollment in the Medicare Advantage market is concentrated among a handful of firms. Six firms or BCBS affiliates account for almost three-quarters (72%) of the market. Two firms, UnitedHealthcare and Humana, account for almost four in ten Medicare Advantage enrollees. Enrollment is even more highly concentrated in some states, with three firms or affiliates accounting for more than 90 percent of enrollment in 17 states, and one firm accounting for more than half of enrollment in 15 states and the District of Columbia. A key, unanswered question is what this market concentration means for consumers.
From the perspective of the Medicare program overall, it is clear that Medicare Advantage has become an increasingly important way in which Medicare beneficiaries receive their benefits and all signs suggest that this will only increase in the future. With such a large share of the program dependent on products offered from a relatively small number of private firms operating at the national and local levels, the ability of Centers for Medicare and Medicaid Services (CMS) to serve as a strong fiduciary for the program becomes increasingly important as well as challenging.
Gretchen Jacobson and Tricia Neuman are with the Kaiser Family Foundation; Anthony Damico is an independent consultant; and Marsha Gold is a Senior Fellow Emeritus with Mathematica Policy Research and independent consultant.
Appendix
Appendix A: Special Needs Plans
Special Needs Plans (SNPs) restrict enrollment to specific types of beneficiaries with significant or relatively specialized care needs, including beneficiaries: (1) dually eligible for Medicare and Medicaid (D-SNPs); (2) requiring a nursing home or institutional level of care (I-SNPs); or (3) with severe chronic or disabling conditions (C-SNPs.)
Enrollment in SNPs increased modestly from 1.9 million to 2.0 million beneficiaries between 2014 and 2015 (Figure A1 and Table A6). As a share of the total Medicare Advantage population, enrollment in SNPs is relatively low, and the 2.0 million SNP enrollees in 2015 account for about 12 percent of total Medicare Advantage enrollment. Yet, in four states and the District of Columbia, enrollment in SNPs is more than one-fifth of total Medicare Advantage enrollment (31% in DC, 28% in SC, 22% in AZ, 21% in AR, and 20% in AL; data not shown).

Similar to prior years, most SNP enrollees are in HMOs (86%), with 11 percent enrolled regional PPOs and 3 percent in local PPOs. The majority of SNP enrollees (82%) are in plans serving those dually eligible for Medicare and Medicaid (D-SNPs). Enrollment of dually eligible beneficiaries in D-SNPs varies greatly by state, and is particularly prevalent in Hawaii (49%) and Arizona (41%) (Table A6).
Separately, several states (including CA, IL, MA, MI, MN, NY, OH, SC, TX, and VA) are undertaking demonstrations with CMS to improve the alignment of Medicare and Medicaid for dually eligible beneficiaries using a capitated model. These enrollees are not included in the SNP enrollment statistics provided here because they operate under unique authority and CMS classifies them as demonstrations. Minnesota is an exception because the demonstration uses its existing D-SNPs to improve the administrative alignment of Medicare and Medicaid in these dual SNPs. (Enrollment in Minnesota’s demonstration is included in the SNP enrollment in Table A6.)
It is unclear how the demonstration will affect the growth in D-SNP enrollment over time in states pursing capitated demonstrations. As of March 2015, more than 300,000 dual eligibles were enrolled in the demonstrations. Between 2014 and 2015, enrollment in D-SNPs increased or remained stable in the majority of demonstration states but enrollment in D-SNPs declined in California, Michigan, and Ohio.
Appendix B: Tables
| Table A1: Medicare Advantage Enrollment by State and Plan Type, 2015 | |||||||
| State | Total | Distribution of Enrollment, by State and Plan Type | |||||
| % in HMOs | % in Local PPOs | % in Regional PPOs | % in PFFS Plans | % in Cost Plans | % in Other Plans | ||
| Total U.S. | 16,761,673 | 64% | 24% | 7% | 2% | 3% | <1% |
| Alabama | 238,091 | 62% | 31% | 7% | <1% | 0% | <1% |
| Alaska | 56 | 0% | 100% | 0% | 0% | 0% | 0% |
| Arizona | 425,454 | 91% | 7% | 1% | 1% | <1% | 0% |
| Arkansas | 114,326 | 39% | 16% | 26% | 18% | 0% | <1% |
| California | 2,127,666 | 98% | 2% | 0% | <1% | <1% | <1% |
| Colorado | 281,467 | 80% | 9% | 0% | 1% | 8% | <1% |
| Connecticut | 157,692 | 85% | 12% | 3% | 0% | 0% | 0% |
| Delaware | 13,841 | 62% | 37% | 0% | 0% | 0% | 1% |
| District of Columbia | 11,033 | 16% | 32% | 0% | 0% | 52% | 0% |
| Florida | 1,570,845 | 70% | 7% | 23% | <1% | <1% | <1% |
| Georgia | 460,670 | 30% | 44% | 24% | 2% | 0% | 0% |
| Hawaii | 110,465 | 42% | 55% | 3% | 0% | 0% | 0% |
| Idaho | 87,837 | 52% | 47% | 0% | 1% | 0% | 0% |
| Illinois | 371,007 | 44% | 52% | 2% | 1% | <1% | 0% |
| Indiana | 264,104 | 15% | 65% | 19% | 2% | 0% | 0% |
| Iowa | 81,541 | 31% | 56% | 0% | 2% | 11% | <1% |
| Kansas | 61,600 | 44% | 46% | 2% | 7% | 0% | <1% |
| Kentucky | 212,948 | 18% | 57% | 23% | 2% | 0% | 0% |
| Louisiana | 232,445 | 86% | 5% | 8% | <1% | 0% | <1% |
| Maine | 66,307 | 64% | 32% | 0% | 3% | 0% | 0% |
| Maryland | 76,375 | 32% | 20% | 0% | 0% | 47% | <1% |
| Massachusetts | 233,084 | 75% | 17% | 4% | 0% | 0% | 1% |
| Michigan | 595,239 | 39% | 55% | 4% | 1% | 0% | <1% |
| Minnesota | 480,474 | 25% | 8% | 0% | <1% | 67% | 0% |
| Mississippi | 76,776 | 51% | 18% | 28% | 3% | 0% | 0% |
| Missouri | 311,364 | 68% | 19% | 10% | 3% | 0% | <1% |
| Montana | 34,758 | 2% | 88% | 0% | 11% | 0% | 0% |
| Nebraska | 34,982 | 53% | 28% | 0% | 19% | 0% | <1% |
| Nevada | 146,094 | 89% | 11% | 0% | 0% | 0% | 0% |
| New Hampshire | 17,295 | 42% | 35% | 0% | 23% | 0% | 0% |
| New Jersey | 222,846 | 78% | 21% | 0% | 0% | 0% | 1% |
| New Mexico | 113,807 | 62% | 36% | 0% | 1% | 0% | <1% |
| New York | 1,212,239 | 72% | 18% | 7% | 2% | <1% | <1% |
| North Carolina | 512,924 | 45% | 47% | 6% | 3% | 2% | <1% |
| North Dakota | 17,878 | 0% | 9% | 0% | 1% | 89% | 1% |
| Ohio | 811,503 | 44% | 46% | 7% | 1% | 2% | <1% |
| Oklahoma | 111,013 | 66% | 27% | 3% | 4% | 0% | <1% |
| Oregon | 323,765 | 60% | 40% | 0% | <1% | 0% | <1% |
| Pennsylvania | 1,001,864 | 62% | 34% | 1% | 1% | 0% | 1% |
| Rhode Island | 71,009 | 93% | 4% | 2% | 0% | 0% | <1% |
| South Carolina | 209,812 | 29% | 20% | 46% | 5% | 0% | <1% |
| South Dakota | 26,400 | <1% | 27% | 0% | 2% | 71% | 0% |
| Tennessee | 412,042 | 69% | 28% | 2% | 0% | 0% | <1% |
| Texas | 1,098,678 | 59% | 23% | 13% | 3% | 2% | <1% |
| Utah | 113,034 | 82% | 18% | 0% | 0% | 0% | 0% |
| Vermont | 8,984 | 6% | 21% | 45% | 27% | 0% | <1% |
| Virginia | 206,427 | 38% | 25% | 12% | 14% | 9% | 1% |
| Washington | 348,467 | 83% | 17% | 0% | <1% | 0% | <1% |
| West Virginia | 99,454 | 7% | 82% | 5% | 6% | 0% | 0% |
| Wisconsin | 388,732 | 48% | 33% | 4% | 3% | 12% | <1% |
| Wyoming | 2,071 | 9% | 18% | 0% | 66% | 0% | 3% |
NOTE: Total U.S. includes Puerto Rico. Includes employer-sponsored plans, special needs plans, and other private plans.SOURCE: Authors’ analysis of CMS Medicare Advantage enrollment and Landscape files, 2015. | |||||||
| Table A2: Medicare Advantage Enrollment in the Individual and Group Markets, by State, 2015 | ||||
| State | Total | Individual plans | Group plans | % enrollees in group plans |
| Total U.S. | 16,761,673 | 13,634,978 | 3,126,695 | 19% |
| Alabama | 238,091 | 226,722 | 11,369 | 5% |
| Alaska | 56 | 0 | 56 | 100% |
| Arizona | 425,454 | 380,348 | 45,106 | 11% |
| Arkansas | 114,326 | 109,552 | 4,774 | 4% |
| California | 2,127,666 | 1,647,253 | 480,413 | 23% |
| Colorado | 281,467 | 232,166 | 49,301 | 18% |
| Connecticut | 157,692 | 142,843 | 14,849 | 9% |
| Delaware | 13,841 | 10,656 | 3,185 | 23% |
| District of Columbia | 11,033 | 7,738 | 3,295 | 30% |
| Florida | 1,570,845 | 1,465,892 | 104,953 | 7% |
| Georgia | 460,670 | 333,521 | 127,149 | 28% |
| Hawaii | 110,465 | 83,119 | 27,346 | 25% |
| Idaho | 87,837 | 86,197 | 1,640 | 2% |
| Illinois | 371,007 | 217,198 | 153,809 | 41% |
| Indiana | 264,104 | 218,813 | 45,291 | 17% |
| Iowa | 81,541 | 76,739 | 4,802 | 6% |
| Kansas | 61,600 | 57,017 | 4,583 | 7% |
| Kentucky | 212,948 | 124,342 | 88,606 | 42% |
| Louisiana | 232,445 | 213,612 | 18,833 | 8% |
| Maine | 66,307 | 53,713 | 12,594 | 19% |
| Maryland | 76,375 | 51,724 | 24,651 | 32% |
| Massachusetts | 233,084 | 196,422 | 36,662 | 16% |
| Michigan | 595,239 | 302,171 | 293,068 | 49% |
| Minnesota | 480,474 | 437,232 | 43,242 | 9% |
| Mississippi | 76,776 | 74,762 | 2,014 | 3% |
| Missouri | 311,364 | 279,712 | 31,652 | 10% |
| Montana | 34,758 | 32,961 | 1,797 | 5% |
| Nebraska | 34,982 | 31,769 | 3,213 | 9% |
| Nevada | 146,094 | 138,940 | 7,154 | 5% |
| New Hampshire | 17,295 | 12,005 | 5,290 | 31% |
| New Jersey | 222,846 | 170,491 | 52,355 | 23% |
| New Mexico | 113,807 | 94,595 | 19,212 | 17% |
| New York | 1,212,239 | 999,021 | 213,218 | 18% |
| North Carolina | 512,924 | 385,512 | 127,412 | 25% |
| North Dakota | 17,878 | 17,775 | 103 | 1% |
| Ohio | 811,503 | 500,372 | 311,131 | 38% |
| Oklahoma | 111,013 | 100,538 | 10,475 | 9% |
| Oregon | 323,765 | 272,682 | 51,083 | 16% |
| Pennsylvania | 1,001,864 | 798,441 | 203,423 | 20% |
| Rhode Island | 71,009 | 65,268 | 5,741 | 8% |
| South Carolina | 209,812 | 195,819 | 13,993 | 7% |
| South Dakota | 26,400 | 26,006 | 394 | 1% |
| Tennessee | 412,042 | 389,994 | 22,048 | 5% |
| Texas | 1,098,678 | 909,082 | 189,596 | 17% |
| Utah | 113,034 | 109,107 | 3,927 | 3% |
| Vermont | 8,984 | 7,338 | 1,646 | 18% |
| Virginia | 206,427 | 179,573 | 26,854 | 13% |
| Washington | 348,467 | 304,472 | 43,995 | 13% |
| West Virginia | 99,454 | 44,273 | 55,181 | 55% |
| Wisconsin | 388,732 | 347,663 | 41,069 | 11% |
| Wyoming | 2,071 | 1,681 | 390 | 19% |
NOTE: Total U.S. includes Puerto Rico.SOURCE: Authors’ analysis of CMS Medicare Advantage enrollment and Landscape files, 2015. | ||||
| Table A6: Enrollment in Special Needs Plans (SNPs), by Plan Type and State, 2015 | ||||||
| State | Enrollment in Special Needs Plans | Total Dual Eligibles (in 2013) | % of Dual Eligibles in D-SNPs | |||
| Total | Dual eligibles(D-SNPs) | Institutional(I-SNPs) | Chronic or disabling conditions(C-SNPs) | |||
| Total U.S. | 2,011,505 | 1,657,554 | 48,740 | 305,211 | 10,705,500 | 15% |
| Alabama | 48,409 | 48,391 | 136 | – | 220,060 | 22% |
| Alaska | – | – | – | – | 16,520 | 0% |
| Arizona | 95,008 | 75,703 | 1,746 | 17,559 | 186,160 | 41% |
| Arkansas | 24,389 | 12,308 | – | 12,081 | 136,060 | 9% |
| California | 214,208 | 170,334 | 3,645 | 40,229 | 1,358,140 | 13% |
| Colorado | 12,773 | 10,270 | 2,425 | 78 | 102,800 | 10% |
| Connecticut | 12,242 | 9,742 | 2,500 | – | 173,400 | 6% |
| Delaware | 2,223 | 885 | 457 | 881 | 29,100 | 3% |
| District of Columbia | 3,394 | 3,218 | 68 | 108 | 30,940 | 10% |
| Florida | 266,831 | 205,219 | 3,196 | 58,416 | 787,040 | 26% |
| Georgia | 87,737 | 44,328 | 2,236 | 41,173 | 317,440 | 14% |
| Hawaii | 19,118 | 19,118 | – | – | 39,120 | 49% |
| Idaho | 1,460 | 1,460 | – | – | 42,840 | 3% |
| Illinois | 11,648 | 9,547 | 615 | 1,486 | 382,340 | 2% |
| Indiana | 4,454 | 821 | 93 | 3,540 | 190,460 | <1% |
| Iowa | 585 | 169 | – | 416 | 90,640 | <1% |
| Kansas | 289 | – | 227 | 62 | 70,860 | 0% |
| Kentucky | 3,977 | 3,505 | – | 472 | 194,180 | 2% |
| Louisiana | 27,784 | 26,293 | – | 1,491 | 214,220 | 12% |
| Maine | 1,548 | 1,548 | – | – | 102,000 | 2% |
| Maryland | 11,164 | 4,839 | 2,808 | 3,517 | 139,100 | 3% |
| Massachusetts | 34,195 | 33,794 | 191 | 210 | 302,300 | 11% |
| Michigan | 18,966 | 18,664 | 198 | 104 | 321,400 | 6% |
| Minnesota | 36,188 | 36,188 | – | – | 146,460 | 25% |
| Mississippi | 13,752 | 12,036 | – | 1,716 | 169,580 | 7% |
| Missouri | 23,756 | 10,871 | 21 | 12,864 | 200,440 | 5% |
| Montana | – | – | – | – | 27,380 | 0% |
| Nebraska | 364 | – | – | 364 | 45,920 | 0% |
| Nevada | 8,511 | 15 | – | 8,496 | 54,940 | 0% |
| New Hampshire | 19 | 19 | – | – | 34,240 | 0% |
| New Jersey | 11,207 | 9,526 | 1,460 | 221 | 226,420 | 4% |
| New Mexico | 10,950 | 9,991 | 297 | 662 | 76,080 | 13% |
| New York | 192,449 | 177,861 | 14,276 | 312 | 857,220 | 21% |
| North Carolina | 21,052 | 16,157 | 2,417 | 2,478 | 342,720 | 5% |
| North Dakota | – | – | – | – | 17,580 | 0% |
| Ohio | 13,453 | 11,201 | 1,203 | 1,049 | 369,500 | 3% |
| Oklahoma | 115 | – | 115 | – | 123,600 | 0% |
| Oregon | 25,460 | 21,675 | 581 | 3,204 | 118,820 | 18% |
| Pennsylvania | 119,052 | 103,998 | 2,927 | 12,127 | 456,240 | 23% |
| Rhode Island | 1,538 | 14 | 1,524 | – | 42,080 | 0% |
| South Carolina | 58,005 | 22,242 | – | 35,763 | 162,020 | 14% |
| South Dakota | – | – | – | – | 21,920 | 0% |
| Tennessee | 68,356 | 68,356 | – | – | 287,800 | 24% |
| Texas | 163,979 | 133,966 | 198 | 29,815 | 726,120 | 18% |
| Utah | 8,155 | 8,155 | – | – | 38,100 | 21% |
| Vermont | – | – | – | – | 30,900 | 0% |
| Virginia | 3,817 | 1,329 | 89 | 2,399 | 201,920 | 1% |
| Washington | 24,563 | 23,084 | 1,479 | – | 189,940 | 12% |
| West Virginia | 133 | 133 | – | – | 88,180 | <1% |
| Wisconsin | 21,109 | 18,454 | 1,612 | 1,043 | 176,620 | 10% |
| Wyoming | – | – | – | – | 12,160 | 0% |
NOTE: Total U.S. includes Puerto Rico. Blank cells indicate no plans offered.SOURCE: Authors’ analysis of CMS Medicare Advantage enrollment and Landscape files, 2015. Number of dual eligibles by state is derived from the CMS Chronic Conditions Data Warehouse standard analytic files for 2013. | ||||||
Endnotes
- In this document, the ACA refers to the Patient Protection and Affordable Care Act of 2010 (P.L. 111-148; PPACA) as amended by the Health Care and Education Reconciliation Act of 2010 (P.L. 111-152). ↩︎
- G. Jacobson, P. Neuman, and A. Damico. “At Least Half of New Medicare Advantage Enrollees Had Switched From Traditional Medicare During 2006-11,” Health Affairs, vol. 34 no. 1, p. 48-55, January 2015. Also see G. Jacobson, T. Neuman, and A. Damico. “Medigap Enrollment Among New Medicare Beneficiaries: How Many 65-Year Olds Enroll In Plans With First-Dollar Coverage?” Washington DC: Kaiser Family Foundation, April 2015. Available at: https://modern.kff.org/medicare/issue-brief/medigap-enrollment-among-new-medicare-beneficiaries/, Last accessed June 5, 2015. ↩︎
- G. Jacobson, A. Damico, T. Neuman, and M. Gold. “Medicare Advantage 2015 Data Spotlight: Overview of Plan Changes,” Washington DC: Henry J. Kaiser Family Foundation, December 2014. Available at: https://modern.kff.org/medicare/issue-brief/medicare-advantage-2015-data-spotlight-overview-of-plan-changes/ ↩︎
- M. Gold. “Medicare Advantage in 2008.” (Table 1: PFFS Contracts by Firm and Number of Counties Covered by the Contract, 2006-2008), Kaiser Family Foundation, June 2008. Available at: https://modern.kff.org/medicare/issue-brief/medicare-advantage-in-2008/ ↩︎
- M. Gold. “Medicare’s Private Plans: A Report Card on Medicare Advantage,” Health Affairs Web Exclusive, November 24, 2008. ↩︎
- M. Gold, D. Phelps, G. Jacobson, and T. Neuman. “Medicare Advantage 2010 Data Spotlight: Plan Enrollment Patterns and Trends,” Washington DC: Henry J. Kaiser Family Foundation, June 2010. Available at: https://modern.kff.org/wp-content/uploads/2013/01/8080.pdf#page=7 ↩︎
- F. McArdle, T. Neuman and J. Huang. “Retiree Health Benefits at the Crossroads”. Washington DC: Henry J. Kaiser Family Foundation, April 2014. Available at: https://modern.kff.org/medicare/report/retiree-health-benefits-at-the-crossroads/ ↩︎
- Kaiser Family Foundation and Health Research and Education Trust, “Section 11. Retiree Health Benefits.” Employer Health Benefits: 2013 Annual Survey. Washington, DC: Kaiser Family Foundation, 2013, pp. 191-199; and P. Fronstein and N. Adams. “Employment Based Retiree Health Benefits: Trends in Access and Coverage: 1997-2010.” EBRI Education and Research Institute, 2012. ↩︎
- Medicare Payment Advisory Commission “Chapter 13. The Medicare Advantage Program: Status Report” in Report to Congress: Medicare Payment Policy, Washington DC, March 2015. pp 313-343. ↩︎
- Medicare Payment Advisory Commission “Chapter 13. The Medicare Advantage Program: Status Report” in Report to Congress: Medicare Payment Policy, Washington DC, March 2015. pp 313-343 and Marsha Gold and Maria Cupples Hudson. “Analysis of the Variation in Efficiency among Medicare Advantage Plans” Research Brief Washington DC: Mathematica Policy Research, April 2013. ↩︎
- Marsha Gold and Giselle Casillas. “What Do We Know about Quality and Access in Medicare Advantage versus Traditional Medicare” Washington DC: Kaiser Family Foundation, November 2014. Available at: https://modern.kff.org/medicare/report/what-do-we-know-about-health-care-access-and-quality-in-medicare-advantage-versus-the-traditional-medicare-program/ ↩︎
- In the fall of 2014, we calculated that beneficiaries who were enrolled in Medicare Advantage plans at that time would pay a premium of $41 per month in 2015, compared to $34 per month in 2014, which assumed they remained in the same plan. Among Medicare Advantage enrollees in 2015, the average premium actually paid by enrollees ($38 per month) is slightly lower than the amount estimated in the fall, with the difference in estimates reflecting both changes in beneficiaries enrolled in Medicare Advantage plans from 2014 to 2015 and shifts by enrollees among plans and plan types. ↩︎
- G. Jacobson, A. Damico, T. Neuman, and M. Gold. “Medicare Advantage 2015 Data Spotlight: Overview of Plan Changes,” Washington DC: Henry J. Kaiser Family Foundation, December 2014. Available at: https://modern.kff.org/medicare/issue-brief/medicare-advantage-2015-data-spotlight-overview-of-plan-changes/ ↩︎
- In Minnesota, 67% of private plan enrollment is in cost plans, which have higher average premiums than Medicare Advantage plans. ↩︎
- Limits were required for regional PPOs since they were first authorized in 2006. ↩︎
- The files used for this analysis provide limited details on the type or extent of coverage in the Part D coverage gap that plans provide, and some additional coverage may be minimal. ↩︎
- Department of Health and Human Services, Centers for Medicare and Medicaid Services, “Medicare Announces Quality Bonus Payment Demonstration for Medicare Health Plans,” November 2010. ↩︎
- G. Jacobson, C. Swoope, M. Perry, and M.C. Slosar. “How are Seniors Choosing and Changing Health Insurance Plans?” Kaiser Family Foundation, May 2014. Available at: https://modern.kff.org/medicare/report/how-are-seniors-choosing-and-changing-health-insurance-plans/ ↩︎