10 Reasons Why Medicare Advantage Enrollment is Growing and Why It Matters
For the first time in Medicare’s history, more than half of all eligible people with Medicare, or 30.8 million people in 2023, are enrolled in private Medicare Advantage plans. Medicare Advantage plans are offered by private health insurance companies that receive payments from the federal government to provide Medicare-covered services. People with Medicare have a choice between traditional Medicare (sometimes called fee-for-service Medicare or Original Medicare) and Medicare Advantage plans. The growth in Medicare Advantage enrollment is driven by a number of factors, including the Medicare payment system, which has served to attract and retain insurers and beneficiaries, rather than reduce Medicare spending.
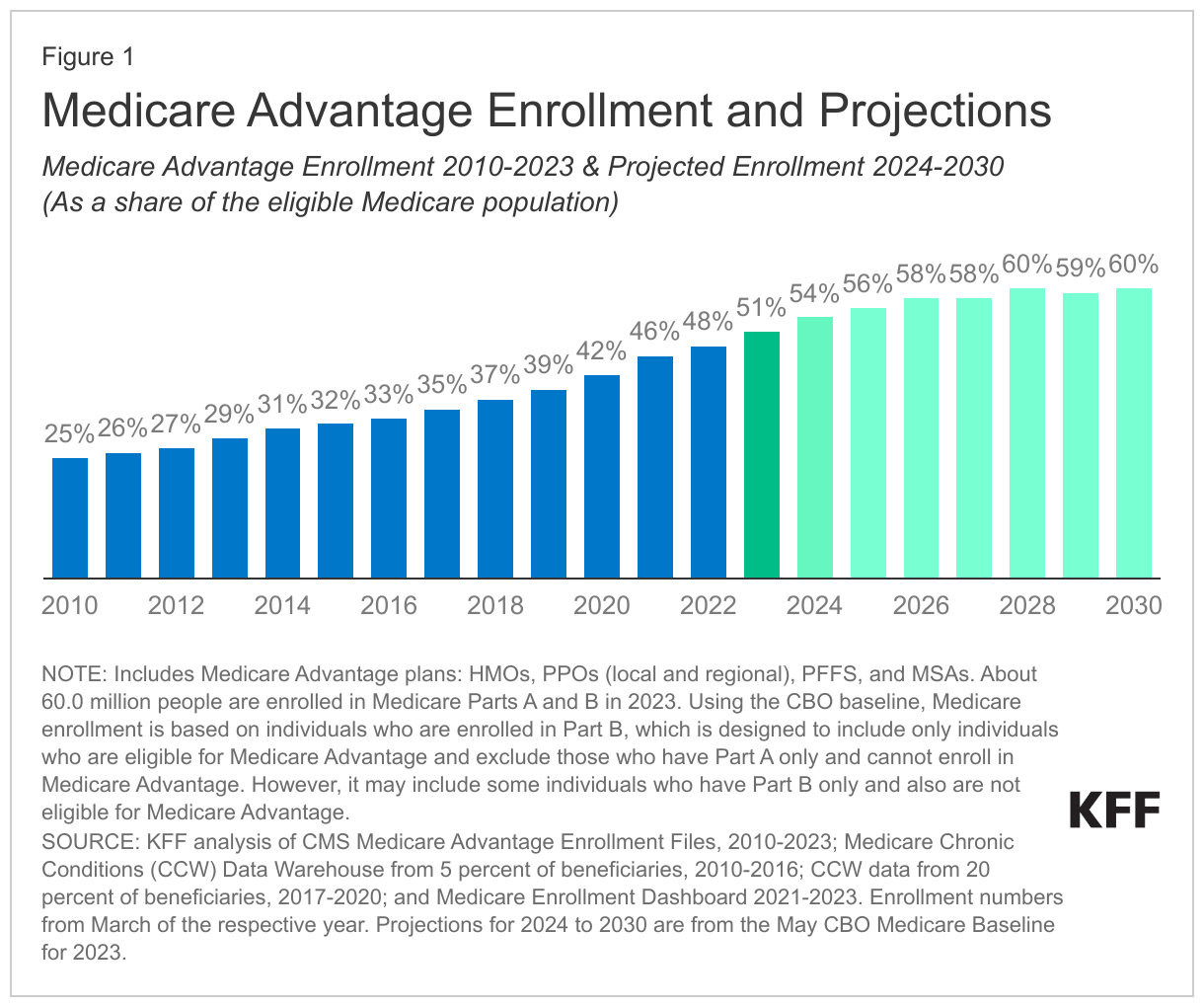
Medicare Advantage enrollment has more than doubled since 2010 and is projected to grow from 54% of the eligible population in 2024 to 60% by the end of this decade (Figure 1).
While some of the larger Medicare Advantage insurers are reporting lower profits due to a slowdown in enrollment growth and higher than expected utilization and costs among enrollees this year, there are many reasons to expect continued Medicare Advantage enrollment growth in the years ahead, given the financial incentives embedded in Medicare’s payment system.
The Medicare Payment Advisory Commission (MedPAC) recently reported that Medicare will pay Medicare Advantage plans an estimated 123% of the cost of similar beneficiaries in traditional Medicare, on average, in 2024, factoring in rebates, coding intensity (i.e., how plans record the health conditions of enrollees for payment purposes), and favorable selection. This year, MedPAC made a change in its estimation methodology to take into account the effects of favorable selection, building on the work of other researchers. Favorable selection occurs when plans are enrolling healthier and lower cost enrollees than predicted by the current payment system.
MedPAC now estimates that these higher payments to Medicare Advantage plans translate into $88 billion in additional Medicare spending in 2024 and $13 billion in higher Medicare Part B premiums paid by Medicare beneficiaries in 2024. While some may take issue with the methodology used to generate these estimates, the projected impact on Medicare spending is likely to raise concerns among some policymakers. Higher Medicare spending affects the solvency of the Medicare Hospital Insurance (HI) Trust Fund and increases Medicare premiums for beneficiaries in both Medicare Advantage and traditional Medicare.
In light of these spending projections, here we lay out 10 reasons why Medicare Advantage enrollment has been growing and why we can expect more growth in the years to come.
- People with Medicare are drawn to Medicare Advantage for the extra benefits. Medicare Advantage plans offer extra benefits, like reduced cost-sharing, dental coverage, gym memberships and debit cards for over-the-counter medical supplies that are not covered by traditional Medicare. These extra benefits are funded by what are known as “rebates,” that is, the difference between the amount that plans bid (estimated spending per enrollee on Medicare-covered services) and the benchmark (the maximum amount Medicare will pay per enrollee in a given county). Plans are required to use rebate dollars to reduce cost sharing or premiums, or provide extra benefits, while also keeping a share of rebate dollars for profit and administrative overhead.
- People with Medicare are drawn to Medicare Advantage plans that are marketed as “zero premium” products. Like traditional Medicare beneficiaries, Medicare Advantage enrollees are required to pay the Medicare Part B premium, but unlike beneficiaries in traditional Medicare, they typically do not pay a separate premium for additional coverage or for Part D prescription drug premium because Medicare Advantage rebate dollars cover these costs.
- Premiums for Part D stand-alone prescription drug plans that supplement traditional Medicare are rising rapidly. On a related note, beneficiaries in traditional Medicare are seeing premiums for stand-alone prescription drug plans rising rapidly, which may lead some to switch to Medicare Advantage to lower monthly expenses. The estimated enrollment-weighted premium for Part D stand-alone drug plans is projected to increase by 21% between 2023 and 2024, from $40 to $48 per month, according to KFF analysis.
- People with Medicare are attracted to the financial protection that comes with an annual out-of-pocket limit that Medicare Advantage plans are required to provide. In contrast, traditional Medicare, with about 30 million beneficiaries, does not have an out-of-pocket limit. The Affordable Care Act requires private employer and individually-purchased insurance plans to cap out-of-pocket costs.
- Beyond financial benefits, people with Medicare are attracted to the simplicity and convenience of Medicare Advantage, which provides all coverage in one plan, obviating the need to obtain a Medicare Part D plan and a Medigap plan, as many traditional Medicare beneficiaries have.
- Insurers are marketing Medicare Advantage aggressively, perhaps because gross margins, which are an inexact proxy for profitability, are substantially higher for Medicare Advantage than individual (non-group) or the fully insured group (employer) market. TV airways were flooded with ads for Medicare plans during the 2023 open enrollment period, with more than 9,500 TV airings per day. Traditional Medicare, the alternative to Medicare Advantage, does not market the same way.
- Brokers have a financial incentive to encourage enrollment in Medicare Advantage plans because commissions are higher for Medicare Advantage than for Medigap and Part D plans that are purchased to complement traditional Medicare.
- A growing share of large employers are shifting their Medicare-age retirees into Medicare Advantage plans for both Medicare and supplemental benefits. KFF research has shown that employers are shifting their retirees to Medicare Advantage as a strategy to maintain benefits, simplify administration and lower their own costs. The shift to Medicare Advantage may reduce costs to employers and unions but also means that retirees may not have the option to choose traditional Medicare, unless they forfeit their retiree health benefits.
- Medicare beneficiaries may be reluctant to switch from Medicare Advantage to traditional Medicare if they run the risk of being denied a Medigap policy due to a pre-existing condition. Medicare Advantage enrollees can switch to traditional Medicare during the annual open enrollment period but may not be able to purchase a Medigap policy. Federal law provides very limited protections for people with pre-existing conditions to enroll in a Medigap policy. Only four states have guaranteed issue protections for Medigap.
- Beneficiaries may not be familiar with potential tradeoffs in choosing Medicare Advantage over traditional Medicare. For example, Medicare Advantage plans may have network restrictions that could prevent enrollees from being seen by certain doctors, hospitals and skilled nursing facilities, and often use prior authorization to manage utilization, which may make it difficult for some enrollees to get treatment or may delay treatment recommended by their doctors, and creates administrative hassles for their providers.
As Medicare Advantage enrollment continues to climb, traditional Medicare is on track to diminish as a source of Medicare coverage, leaving in its place a program that looks more like a marketplace of private health insurance plans, funded by the federal government. This doesn’t come as a surprise. Policy choices made over the years have resulted in higher payments to plans relative to spending for similar people in traditional Medicare, allowing plans to reduce cost sharing and offer extra benefits that appeal to beneficiaries and have boosted enrollment well beyond expectations.
At the same time, gaps in data make it difficult to assess the impact of Medicare Advantage coverage on people who enroll in these plans, particularly those with significant health needs. Given these trends, policymakers are likely to struggle in the years ahead with how to contain the cost to the federal government of Medicare Advantage, what that means for enrollees, and what the future holds for traditional Medicare.
This work was supported in part by Arnold Ventures. KFF maintains full editorial control over all of its policy analysis, polling, and journalism activities.