Community Health Centers Prepare for Funding Uncertainty
The Community Health Center Fund (CHCF), which was established by the Affordable Care Act (ACA) and now accounts for the majority of health center grant funding, is due to expire at the end of September unless Congress acts to extend it. Health centers have faced this situation before. In 2017, the CHCF lapsed for five months before Congress extended it for two years. Although funding was ultimately restored, health centers around the country reported that they faced difficult decisions to reduce care, close service sites, and lay off staff because of the delay. Health centers are considering similar actions to prepare for another potential loss of funding, which will have implications for the patients and communities they serve. This data note reports findings from the 2019 KFF/Geiger Gibson Community Health Center Survey on how health centers may respond to ongoing funding uncertainty.
The Community Health Center Fund
The Community Health Center Fund is a key source of revenue for health centers, accounting for 72% of all federal health center grant funds. Initially authorized in 2010 under the ACA for a five-year period, the CHCF has been extended twice, in 2015 and 2018, growing from $1 billion in FY 2011 to $4 billion in FY 2019. Funding from the CHCF allows health centers to serve patients without health insurance, expand capacity, and offer a broader range of health services, including oral health care for adults and mental health and substance use disorder services. From 2010 to 2017, the number of health center sites increased by 59% and total patients served by 43%, and the share of health centers offering mental health and substance abuse services grew by 22% and 75%, respectively. CHCF funding also enables health centers to furnish services that improve patients’ access to care, such as transportation and interpretation services, that are not typically covered by public or private health insurance.
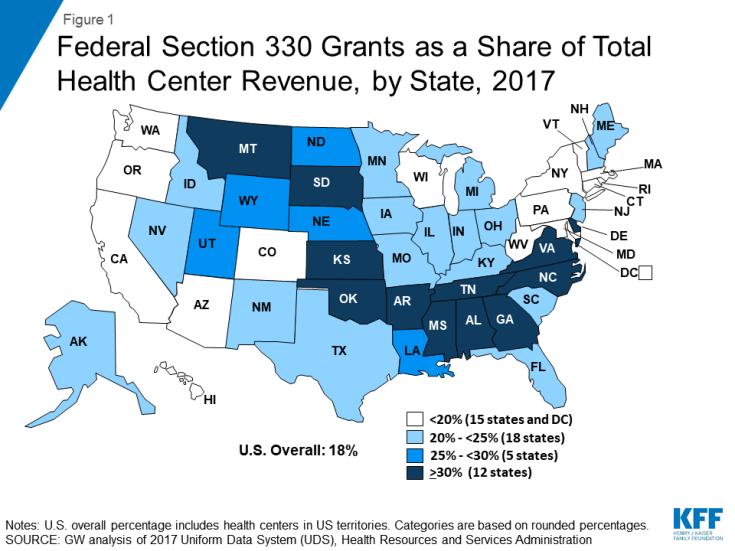
Federal grant funding represents nearly one-fifth of total health center revenue, more for health centers in states that have not expanded Medicaid. Federal grant funding, also known as Section 330 funding, totaled over $4.7 billion in calendar year 2017 and accounted for 18% of health centers’ total revenue that year (Figure 1). Health centers located in states that have not implemented the ACA Medicaid expansion are especially reliant on federal grants to support their operations. In these states, where uninsured rates are considerably higher, grant funding accounts for 26% of total health center revenue. In 2017, Section 330 funding accounted for 30% or more of total health center revenue in 12 states.
Health Centers’ Response to a Potential Funding Delay
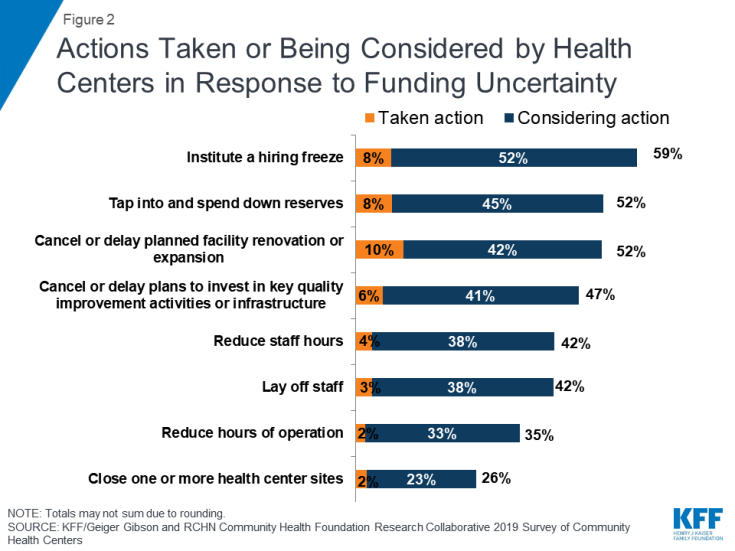
Anticipating a delay in extending the CHCF, health centers have taken or are considering a number of actions that could affect patients’ access to care. To prepare for a possible reduction in funding, a small number of health centers have limited or reduced staffing costs, and many more are considering doing so. Nearly six in ten (59%) health centers have in place or are considering adopting a hiring freeze, and over four in ten (42%) say they are considering laying off staff or reducing staff hours (Figure 2). Some heath centers report considering steps that would even more directly affect their capacity to serve their patients, such as reducing operating hours (35%) or closing one or more health center sites (26%). Other actions health centers report taking or considering include tapping into reserves (52%) and canceling or delaying renovations or expansions (52%).
Although less common, health centers are considering cutting some services. With funding still in place, few health centers (1%-2%) have already taken steps to eliminate or reduce services, but more are weighing cutting services if funding is delayed. Nearly four in ten (39%) say they have or might scale back enabling services, such as case management, transportation, and education services, and a quarter had implemented or are considering reductions in dental services (Figure 3). In addition, one in five had or is considering eliminating or reducing mental health services and about one in six (17%) is targeting substance use disorder treatment services.
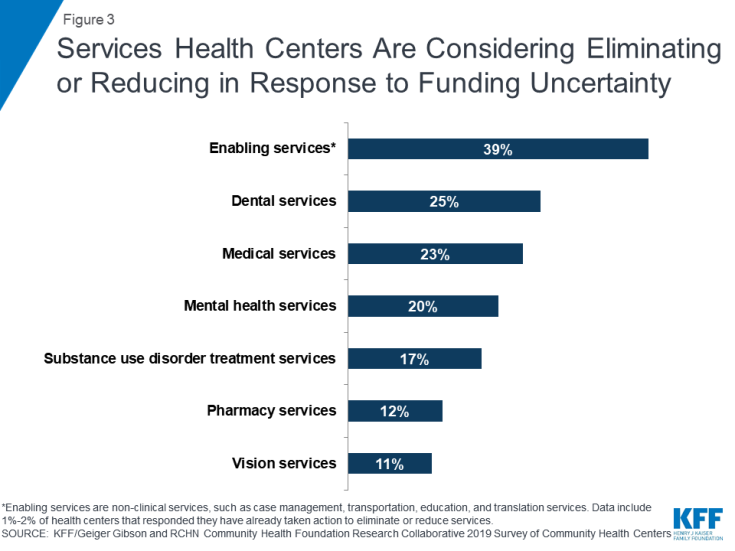
Figure 3: Services Health Centers Are Considering Eliminating or Reducing in Response to Funding Uncertainty
Health centers in non-expansion states were more likely to report having taken or considering actions. With their greater reliance on CHCF funding to support operations, health centers in states that have not expanded Medicaid appear more sensitive to a funding delay. Compared to those in Medicaid expansion states, health centers in non-expansion states were more likely to say they have or are considering reducing operating hours (44% vs. 31%) and have already closed or are weighing closing one or more health center sites (34% vs. 22%) (Figure 4). They were also more likely to report they have or are considering reducing or eliminating certain services, including dental, mental health, and substance use disorder services.
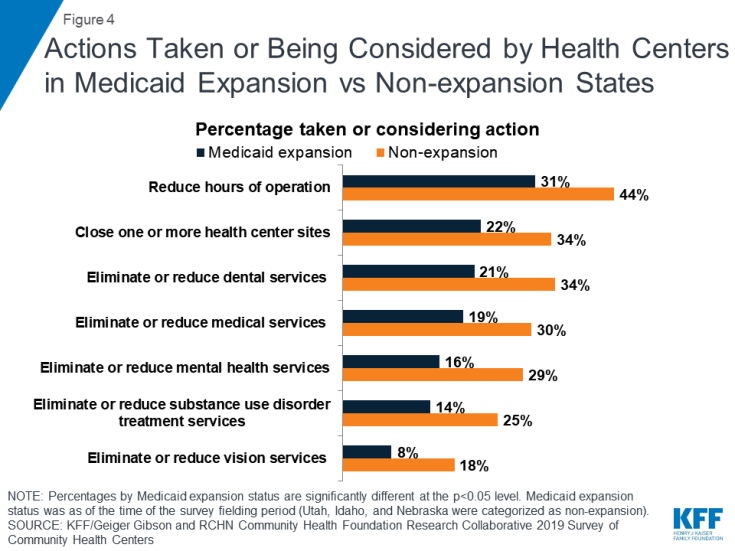
Figure 4: Actions Taken or Being Considered by Health Centers in Medicaid Expansion vs Non-expansion States
What’s Next?
Bills to extend the CHCF at current funding levels await votes in both chambers of Congress. In both the House and the Senate, bills that include provisions to extend the CHCF have advanced out of Committee but were not voted on prior to Congress adjourning for the August recess. The House bill (HR 2328) would extend the CHCF for four years, through the end of fiscal year 2023, at the current funding level of $4 billion per year. The Senate bill (S 1895) would extend the fund for five years, through the end of fiscal year 2024, also at current funding levels. Upon returning from the August recess, Congress will have just over three weeks to pass legislation before the CHCF expires.
A funding delay could limit access to care for millions of health center patients. Health centers are an important source of care for over 28 million patients in medically underserved rural and urban areas throughout the country and play a leading role in efforts to address public health crises, such as the recently announced Trump administration initiative to stop new HIV infections. In response to funding uncertainty, a small number of health centers are already taking steps to reduce or curtail services, and more are considering such actions, particularly those in states that have not expanded Medicaid.
The 2019 Kaiser Family Foundation/George Washington University Survey of Community Health Centers was designed and analyzed by researchers at KFF and GWU, and conducted by the Geiger Gibson Program in Community Health Policy at GWU. The survey was fielded from May to July 2019 and was emailed to 1,342 CEOs of federally funded health centers in the 50 states and the District of Columbia identified in the 2017 Uniform Data System. The response rate was 38%, with 511 responses from 49 states and DC. Additional support for the survey was provided by the RCHN Community Health Foundation.