The New Help for Medicare Beneficiaries with High Drug Costs That Few Seem to Know About
The Inflation Reduction Act of 2022 includes several provisions to lower out-of-pocket drug costs for people with Medicare. Some provisions of the law have already taken effect, including a $35 cap on monthly cost sharing for insulin and free vaccines under Part D, Medicare’s outpatient drug benefit. Medicare’s new drug price negotiation program is also getting underway, with negotiated prices first taking effect in 2026. And a new cap on Part D out-of-pocket prescription drug costs for people with Medicare takes effect in January 2024 – a change that will save thousands of dollars for people who take high-cost drugs.
Beginning in 2024, people enrolled in Part D plans will no longer be required to pay 5% coinsurance after they reach the catastrophic threshold. Eliminating this 5% coinsurance requirement means that in 2024, Part D enrollees will pay no more than about $3,300 for all brand-name drugs they take – a change KFF estimates will help well over 1 million Medicare beneficiaries. And starting in 2025, out-of-pocket drug spending will be capped at a lower amount, $2,000 (indexed annually for growth in Part D costs.)
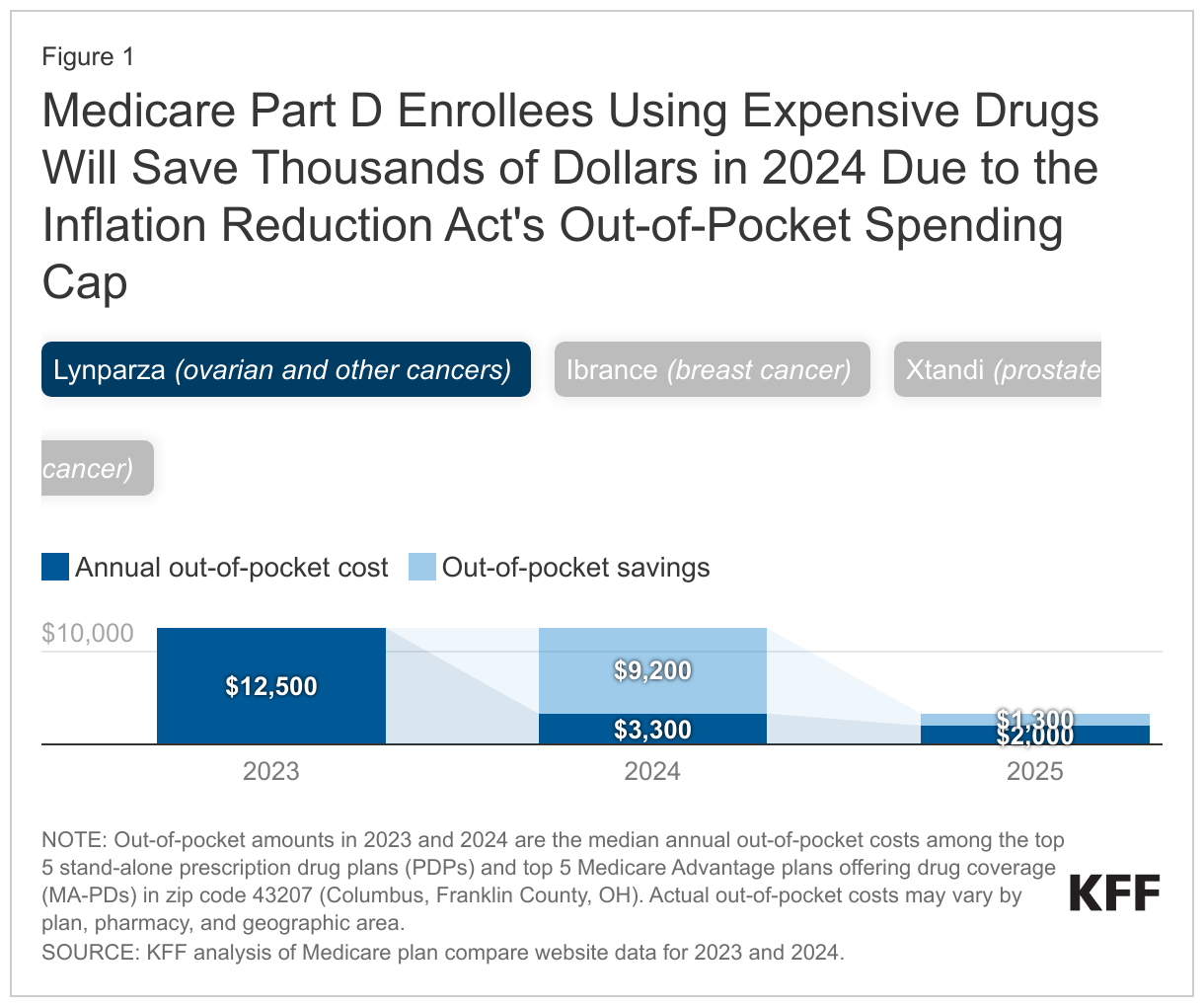
To illustrate the impact of Part D’s new out-of-pocket cap, consider three drugs taken to treat various forms of cancer – Lynparza, Ibrance, and Xtandi – each with annual retail prices well over $100,000. In 2023, Medicare Part D enrollees who used any of these drugs for the entire year faced annual out-of-pocket costs around $12,000, but in 2024, out-of-pocket costs will drop to about $3,300 for each of these drugs (Figure 1). This translates to annual savings of $8,100 to $9,200 compared to 2023. Out-of-pocket costs for these drugs will drop even further beginning in 2025 when the $2,000 cap takes effect.
The current 5% coinsurance requirement for catastrophic coverage may seem like a small amount, but with many drugs coming to market priced at $150,000 or more, that 5% translates into thousands of dollars in annual out-of-pocket costs for expensive drugs. Paying this amount can be a particular burden for older adults, many of whom live on fixed incomes and have limited financial resources to tap to pay for high-cost medications.
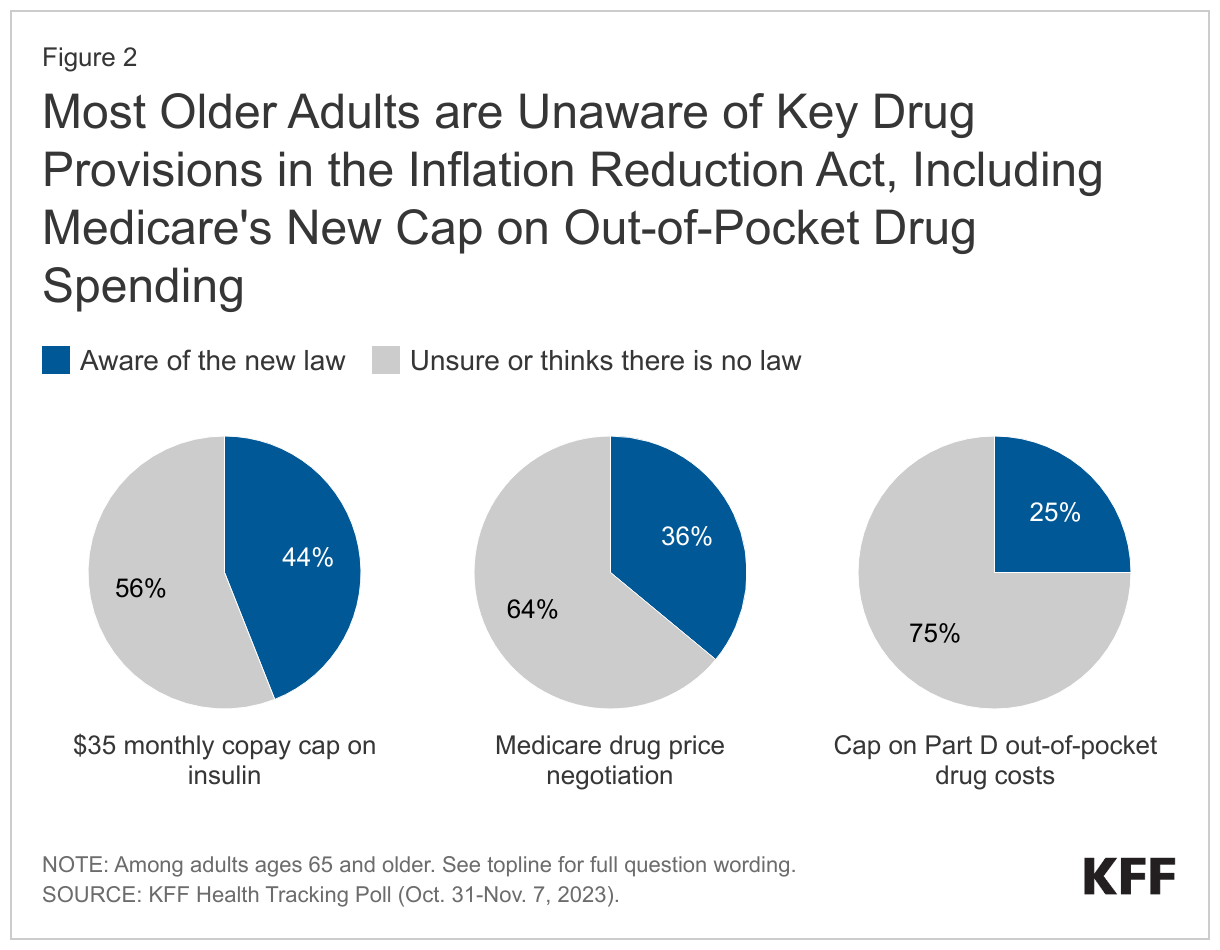
Although changes to prescription drug costs in the Inflation Reduction Act are underway, recent KFF polling finds low levels of awareness among older adults about key features of the law. Only a quarter of all older adults know about the new cap on out-of-pocket prescription drug costs for people with Medicare that takes effect in January. A larger share, but still less than half, of all older adults knows about the new insulin copay cap for Medicare beneficiaries, and around one-third know about the change that requires the government to negotiate prices for some high-cost drugs in Medicare (Figure 2).
At a time when the affordability of health care is among the key issues that voters want to hear about from presidential candidates, the results of KFF polling suggest that more work could be done to inform people with Medicare about the prescription drug changes in the 2022 law. But regardless of what people do or don’t know about these changes, more older adults will begin to see real savings very soon, particularly those who take high-cost drugs.