Telehealth Has Played an Outsized Role Meeting Mental Health Needs During the COVID-19 Pandemic
There has been a rapid increase in the use of telehealth thus far into the COVID-19 pandemic for both mental and physical health concerns. While many employer health plans covered telehealth prior to the pandemic, utilization of these services was relatively low, accounting for less than 1% of outpatient visits. At its pandemic peak, telehealth represented 13% of outpatient visits between March and August of 2020. As in-person care resumed, telehealth began to represent a smaller share of outpatient care (8% between March and August 2021). While many continue to envision an expanded role for telehealth in the delivery of care following the pandemic, there remains considerable uncertainty in what services will be available, where and how providers will be able to practice, how benefits will be structured, and how providers will be paid.
The COVID-19 pandemic has taken a toll on the nation’s mental health, with 3 in 10 adults in the U.S. reporting symptoms consistent with depression or anxiety disorder since April 2020. Over 20% of adults reporting poor mental health also report not receiving counseling or therapy during the pandemic. Telehealth has played a particularly significant role in meeting the need for mental health services. Thus far into the pandemic, some private payers have improved coverage for mental health and substance use, removing pre-pandemic restrictions on coverage for these services via telehealth. Similarly, Medicaid expanded coverage of telehealth services during the pandemic for mental health and substance use services. Many state Medicaid programs reported that telehealth has had particular value in maintaining or improving access to such services during the pandemic.
This analysis looks at outpatient visits during five six-month periods between March 2019 and August 2021, using data from Cosmos, a HIPAA-defined Limited Data Set of more than 126 million patients from over 156 Epic organizations, including 889 hospitals and 19,420 clinics across all 50 states. Mental health and substance use visits were identified based on the primary ICD-10-CM diagnosis code listed for the visit. We find that a year and a half into the pandemic, telehealth continues to play a significant role in providing services, particularly for mental health and substance use services.
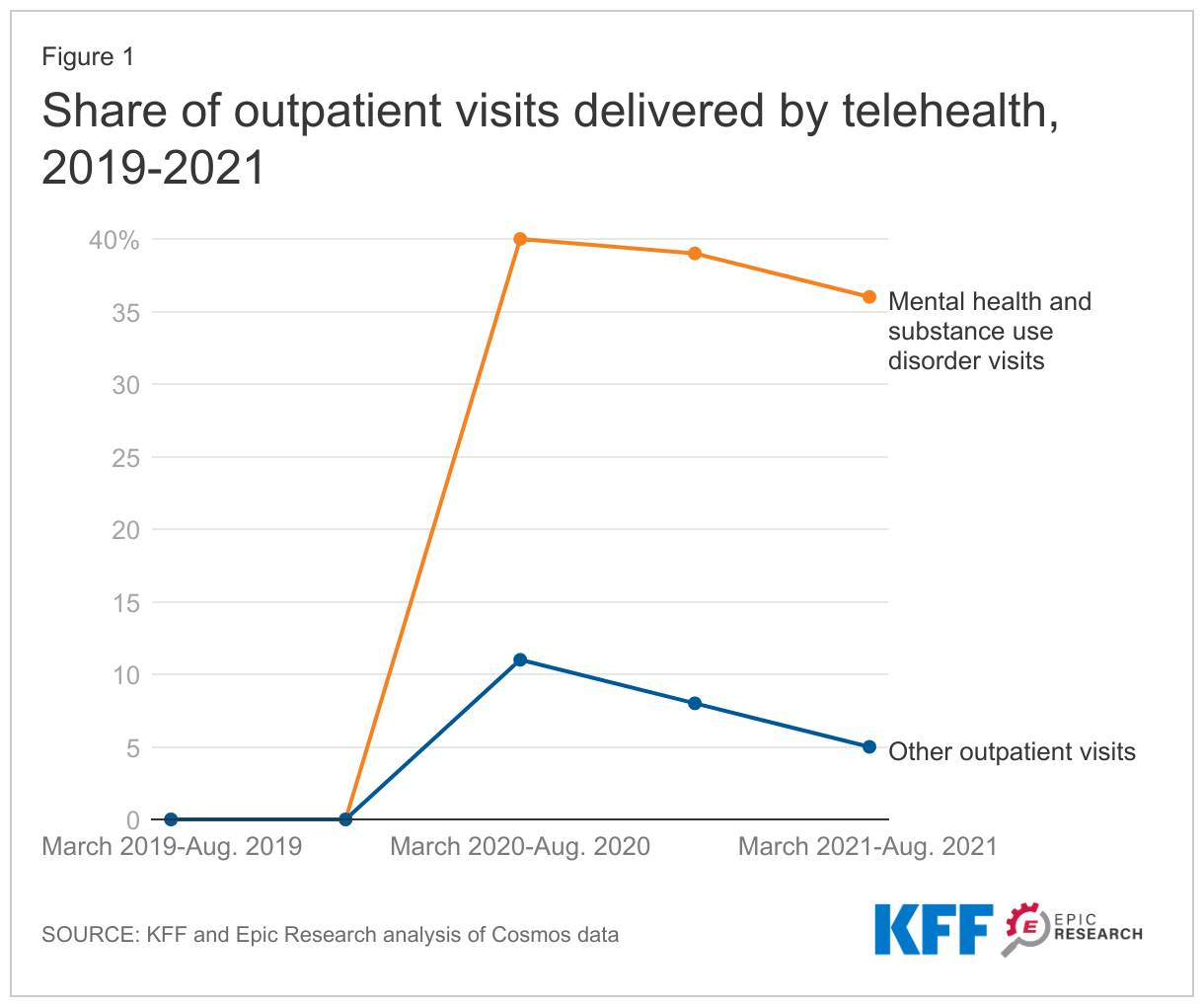
Mental health and substance use services by telehealth has remained elevated whereas other outpatient care use by telehealth has declined
Telehealth represented less than 1% of outpatient care before the pandemic (rounding to zero) for both mental health and substance use and other concerns. However, at its pandemic peak, telehealth represented 40% of mental health and substance use outpatient visits and 11% of other visits (during the March- August 2020 period). Since then, in-person care has returned and telehealth visits have dropped off to represent 5% of other outpatient care visits, those without a mental health or substance use claim in the March-August 2021 period. However, telehealth use has remained strong for mental health and substance use treatment, still representing 36% of these outpatient visits.
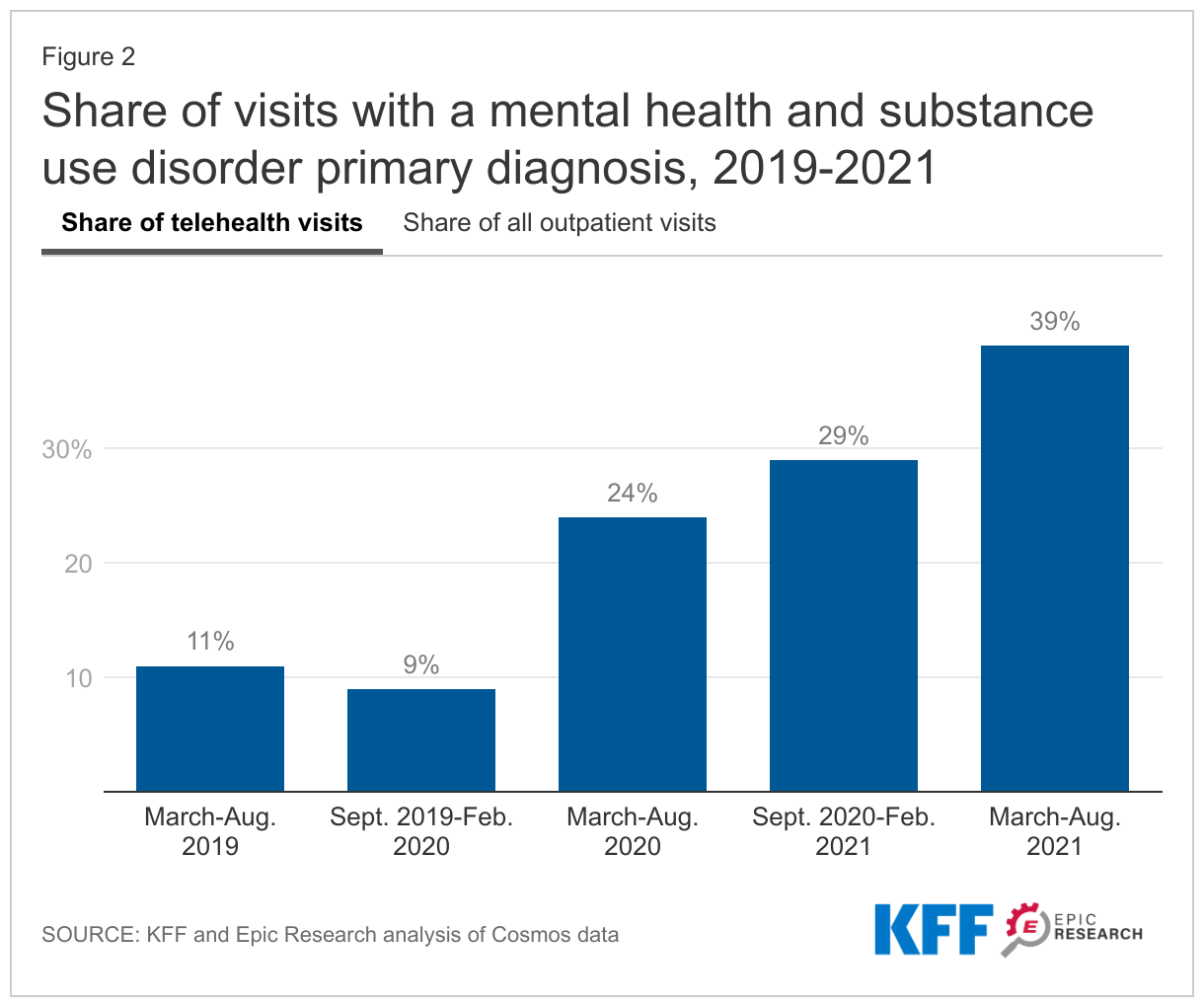
Telehealth use for mental health or substance use continues to grow as a share of all telehealth visits
Mental health and substance use visits represent a growing share of both telehealth visits and outpatient visits overall, but the trend is much more pronounced for telehealth. By the period of March-August 2021, 39% of telehealth outpatient visits were primarily for a mental health or substance use diagnosis compared to 24% a year earlier and 11% two years earlier. Among all outpatient visits (in-person and over telehealth), the share with a mental or substance use diagnosis grew from 4% in March-August 2019 to 8% during the pandemic, and has remained at 8% in March-August 2021.
This is a product of several factors, including the tremendous increase in need for mental health services as a result of the pandemic, social distancing and ensuing economic turmoil, as well as a return to in-person visits for other outpatient care.
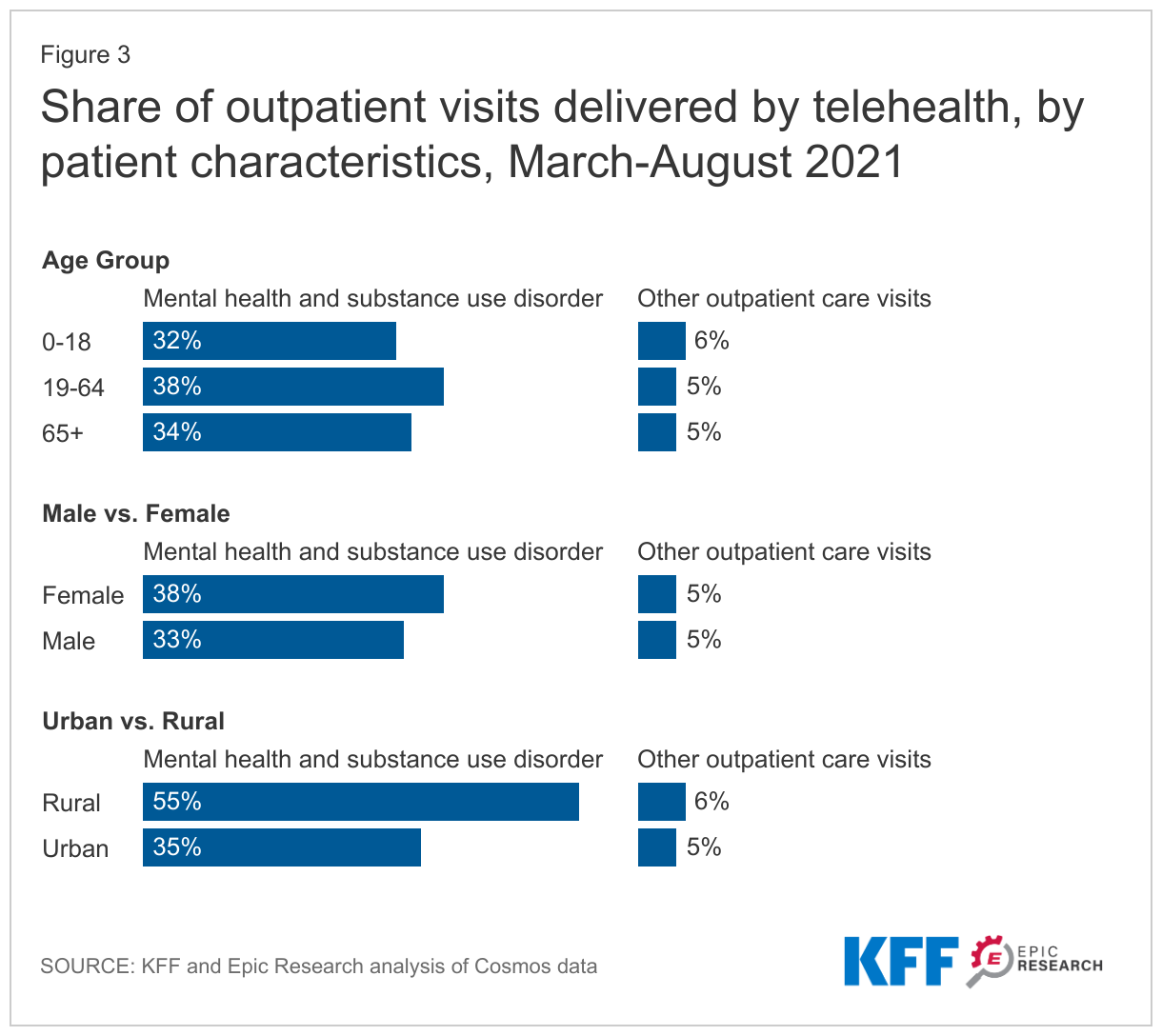
Rural residents are more likely to use telehealth for mental and substance use disorder visits
The adoption of telehealth varies based on the health needs of patients, their readiness and ability to adopt the technology, and the restrictions or incentives they face from payers and providers. Looking at the most recent study period (March-August 2021), a relatively high share of patients in rural areas relied on telehealth to receive outpatient mental health and substance use services (55%) compared to those in urban areas (35%). This pattern is especially pronounced in comparison to other outpatient health care services, where we observed a similar rate across urban and rural (5% vs. 6%) areas. This may be impacted by the number of rural areas which have a shortage of mental health providers.
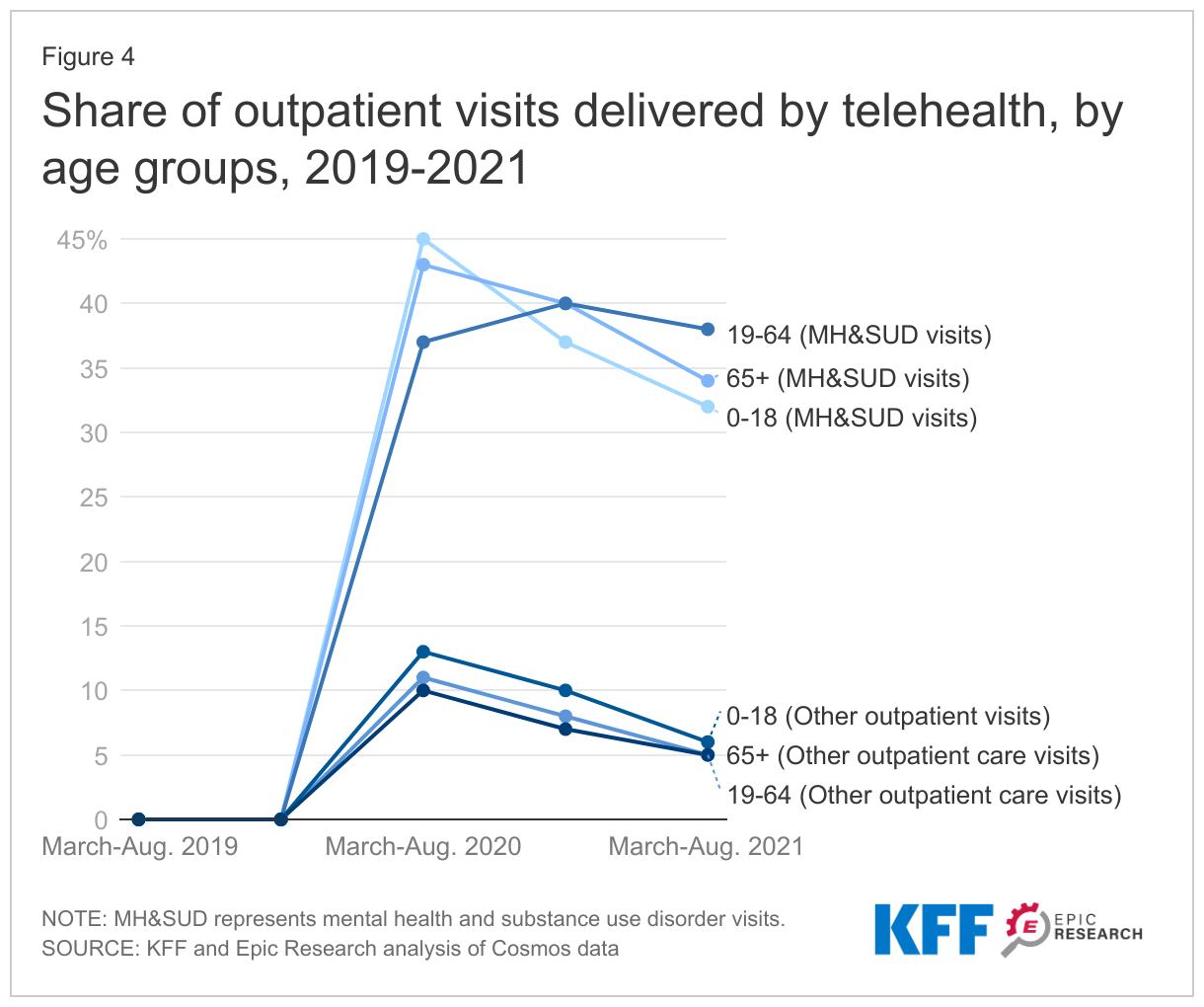
Non-elderly adults consistently used telehealth to access mental health and substance use services
Early on in the pandemic (March-August 2020), outpatient services for mental health and substance use were delivered by telehealth at a similar rate among children and the elderly, and a slightly lower rate among non-elderly adults. A year later (March-August 2021), non-elderly adults were somewhat more likely to be treated via telehealth compared to kids and seniors. In the most recent period, 58% of all mental health or substance use outpatient visits, and 62% of these visits performed via telehealth, were among people in the 19-64 age group.
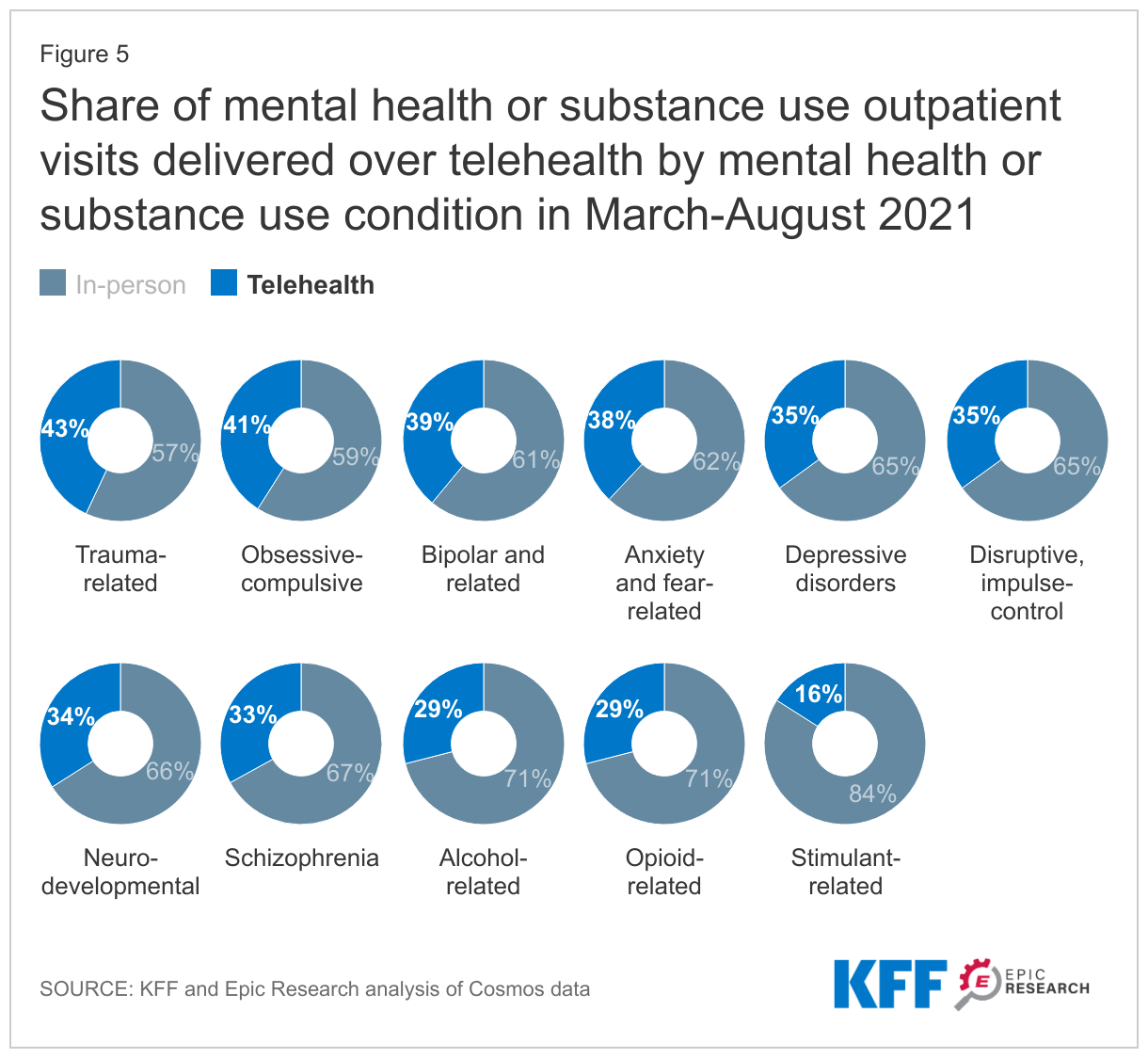
Telehealth use is significant across major mental health and substance use disorder conditions
The primary ICD-10-CM diagnosis code listed on an outpatient visit was categorized into conditions based on the Clinical Classifications Software Refined (CCSR). Major conditions were selected if there were more than 5,000 total visits (in-person and telehealth) during the March-August 2021 period. A large share of outpatient visits for major mental and substance use conditions were delivered over telehealth during this period, including for substance use disorders such as opioid-related disorders (29%) and alcohol-related disorders (29%). For mental health needs, over 1 in 3 outpatient visits were delivered by telehealth (for example, 35% and 38% of outpatient visits were over telehealth for depression or anxiety, respectively).
Discussion
How the mass adoption of telehealth affects access, cost, and quality of mental health and substance use disorder services remains to be seen. Telehealth may provide a way to improve access to mental health and substance use disorder care, particularly for people living in areas with fewer providers. Though differences in comfort with technology, digital literacy and lack of internet at home may hinder access to telehealth for some.
Payers’ and regulators’ policies governing telehealth services continue to evolve. As required under the Consolidated Appropriations Act of 2021 (CAA), and as implemented under the CY 2022 Medicare Physician Fee Schedule Final Rule, Medicare has permanently removed geographic restrictions for mental health and substance use services and permanently allows beneficiaries to receive those services at home. Also under the Physician Fee Schedule final rule, CMS will now permanently cover audio-only visits for mental health and substance use services, though only when the beneficiary is not capable of, or does not consent to, the use of two-way, audio/video technology.
States have broad flexibility to determine Medicaid coverage of telehealth services as well as providers’ licensure requirements to practice and prescribe during a telehealth consultation. States expanded Medicaid telehealth coverage in response to the pandemic, with nearly all states covering and paying parity for audio-visual and audio-only mental health and substance use disorder visits in their fee-for-service Medicaid programs as of July 2021. Many states plan to maintain all or some of these expanded telehealth policies post-pandemic, especially flexibilities for behavioral health visits. However, some states have moved to reinstate certain rules that limit telehealth use, providers’ ability to practice across state lines, and providers’ ability to prescribe medication without an in-person visit. In some other states, telehealth coverage expansions for Medicaid are tied to the COVID-19 public health emergency (PHE) and will expire with the PHE unless extended. State and federal laws regarding providers’ abilities to prescribe medication via telehealth and practice across state lines will also affect telehealth use in the future. Temporary federal policies that gave qualified providers more flexibility to prescribe controlled substances over telehealth are set to expire at the end of the PHE.
Data during the pandemic suggest there is a concerning increase in the number of individuals reporting symptoms of depression or anxiety and showing signs of substance use disorder. Many employers have expressed concern about the availability of mental health providers in their plan network. Given the increased need for services and concerns about the availability of mental health and substance use care providers, some payers may look to bolster access to these services through telehealth.
As policy makers continue to look at how to regulate and pay for telehealth services, it is important to consider opportunities for patient choice so that telehealth is not necessarily given as the only option for those looking for care. Additionally, the Substance Abuse and Mental Health Services Administration (SAMHSA) has called for refining clinical guidelines for tele-mental health services, including broader adoption of telehealth for mental and substance use disorders. In particular, how laws affecting prescribing patterns for mental health and substance use therapies are devised after the COVID-19 public health emergency ends may influence the long-term use of telehealth for mental health and substance use disorders.
Justin Lo is with Epic Research. Matthew Rae, Krutika Amin, Cynthia Cox, and Nirmita Panchal are with KFF. Benjamin F. Miller is with Well Being Trust.
Methods
This analysis was done using Epic’s Cosmos dataset, a HIPAA-defined limited data set of electronic health records from over 150 Epic organizations. Estimates in this report are based on this population and not weighted to be nationally representative. The analysis used data on outpatient visits for 94 data contributors to Cosmos from March 1, 2019 through August 31, 2021 and was analyzed in 6-month periods. Mental health and substance use services delivered by third-party vendors may not be included. Organizations were then excluded if they had software go-lives or mergers during the study time period, had multiple weeks of missing data, or showed discrepancies. Mental health and substance use visits were identified based on the primary ICD-10-CM diagnosis code listed on the outpatient visit. Primary diagnosis codes were then grouped based on the Agency for Healthcare Research and Quality (AHRQ) Clinical Classifications Software Refined (CCSR) grouping. Rural patients are those who do not reside in a core based statistical area (CBSA).