A Look at Vaccine and Booster Rates in Nursing Facilities as New Boosters Become Available
Keeping nursing facility staff and residents current on their COVID-19 vaccines is an important tool for reducing deaths from COVID-19. This is particularly relevant now since KFF analysis found that over one-fifth of all U.S. COVID-19 deaths occurred in long-term care facilities and death rates from COVID-19 are rising for people ages 65 and older, who comprise most nursing facility residents. The number of COVID-19 deaths per month among people 65 and over doubled between April 2022 and July 2022, exceeding 11,000 for the months of July and August.
Although initial vaccination rates for both groups were quite high, take-up of boosters has been lower. Those are troubling numbers because a recent report from the CDC found that receipt of a second COVID-19 booster dose was 90% effective against death and 74% effective against severe COVID-19-related outcomes for nursing facility residents. This data note describes COVID-19 vaccination rates of nursing facility residents and staff between August 2021 and the week ending September 18th, 2022. We briefly explore how federal policy actions have affected vaccine take-up thus far, and what that might mean for take-up of the new, bivalent boosters. Federal policy may be important to promoting take-up of those boosters as the KFF COVID-19 Vaccine Monitor from September 2022 show half of adults have heard little or nothing at all about the new boosters.
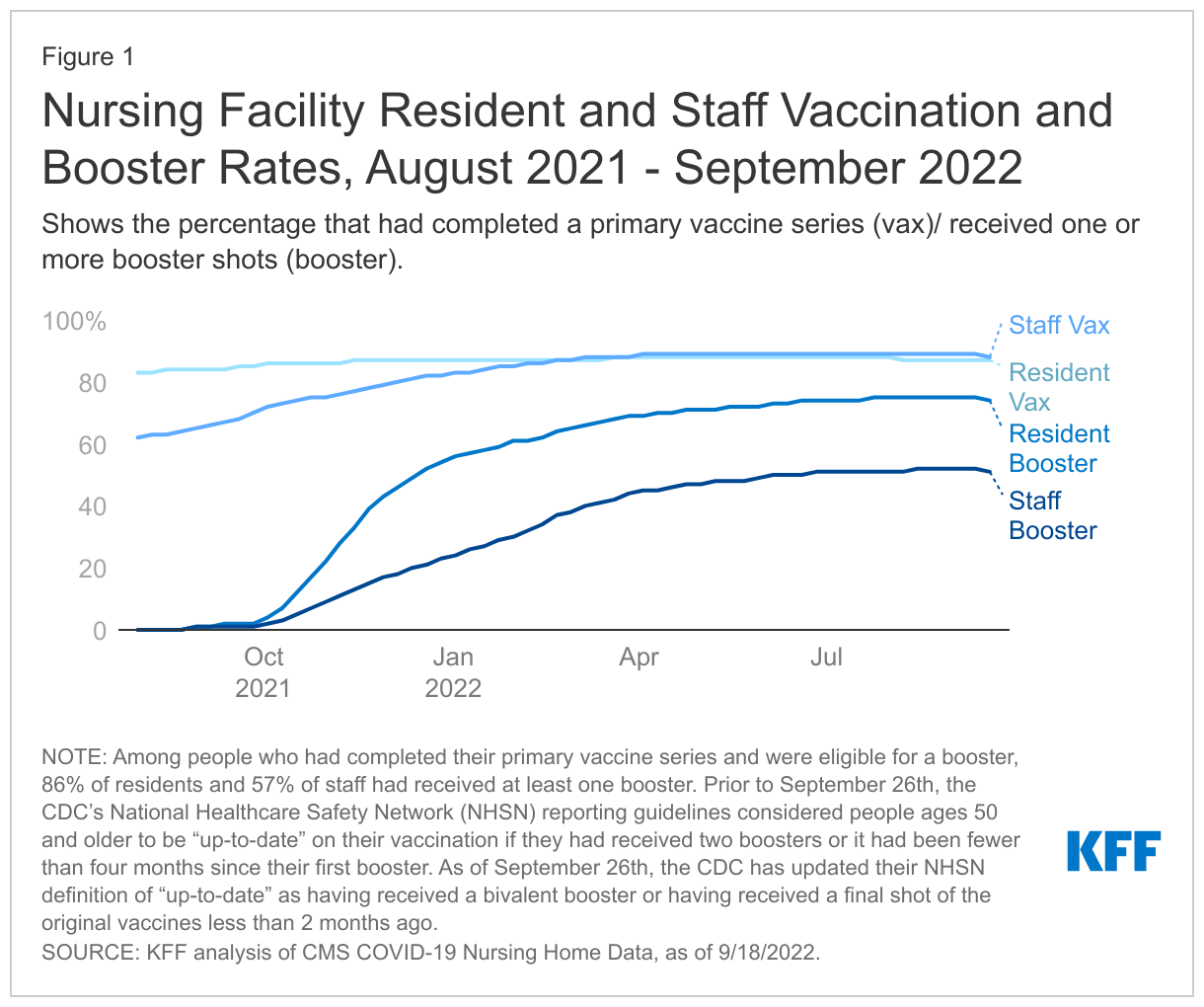
Take-up of the initial vaccine series has been relatively high, with over 85% of residents and staff completing the primary series as of September 18, 2022 (Figure 1). Among nursing facility residents, 87% completed a primary vaccine series, which includes either 2 doses of the Pfizer-BioNTech, Moderna, or Novavax vaccines; or a single dose of the Janssen vaccine. There has been minimal change in that rate over the last year among nursing facility residents – in August 2021, 83% of residents had completed their primary series. Among nursing facility staff, 88% completed a primary vaccine series by September 18, 2022. That rate increased from 62% in August 2021 to 88% in March 2022 and has remained stable since.
Take-up of boosters has been lower: Only 74% of all residents and 51% of all staff had received one or more booster shots as of September 18, 2022. Among the population who completed the initial vaccine series and were eligible for a booster, 86% of residents and 57% of staff had received one or more boosters. The CDC began recommending booster shots for nursing facility residents in September 2021, after data indicated that vaccinations become less effective over time, especially among older adults. Initial take-up among residents was rapid and the percentage of vaccinated residents who had a booster shot increased from 1% in September 2021 to nearly 60% in January 2022. Since then, the percentage of residents who have had a booster has increased but at a much slower rate, rising to 74% in September 2022. Booster take-up has been much lower among nursing facility staff. Between September 2021 and September 2022, the percentage of vaccinated staff who had received a booster grew from 1% to 51%. Any booster dose given to nursing facility residents or staff after September 1, 2022 is the new bivalent booster.
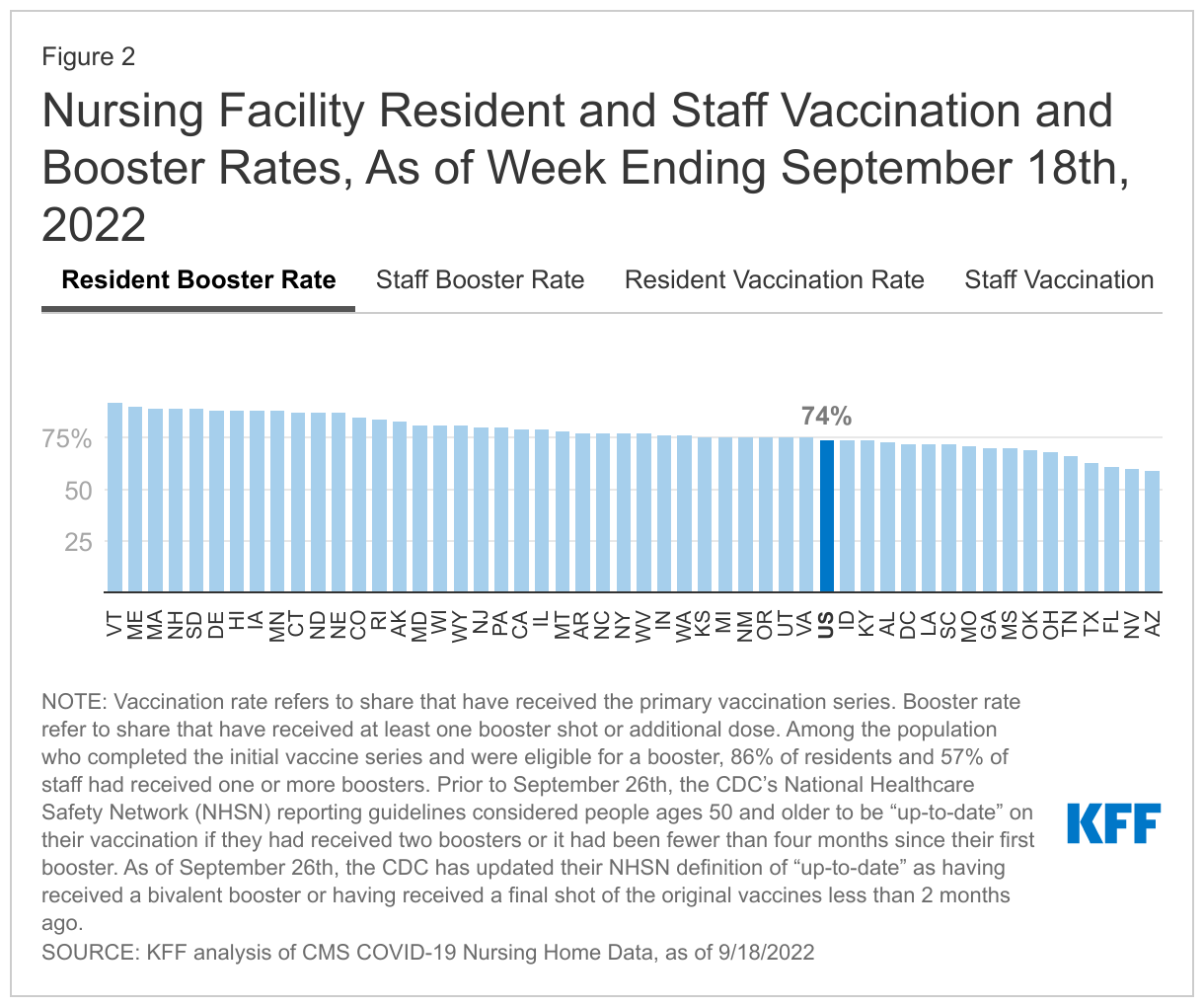
Vaccination and booster rates vary considerably across the states and in 30 states, fewer than half of all staff had received one or more booster shots as of September 18, 2022 (Figure 2). Vaccination rates for nursing facility residents range from 76% in Arizona to 97% in Vermont. Booster rates are lower, ranging from 59% in Arizona to 92% in Vermont. Among staff, the vaccination rate ranges from 78% in Ohio, Idaho, and Missouri to 100% in New York and Maine. The percentages who have received a booster range from 32% in Missouri, Alabama, and Mississippi to 96% in Massachusetts.
Looking forward, both federal policy and local outreach efforts could be important to promoting take-up of the new bivalent boosters among nursing facility residents and staff. One likely reason for the quick initial take-up of vaccines and boosters during 2021 among nursing facility residents and staff was that there were three on-site vaccination clinics held at all long-term care facilities participating in the Federal Pharmacy Partnership for Long-Term Care Program. (Other factors contributing to high take-up rates include very high death rates from COVID-19 among people in nursing facilities and the fact that they were a main focus of the initial vaccine roll-out.) Facilities are still able to request additional clinics, but it’s unclear how many facilities are doing so or how many pharmacy partners continue to participate. Current CDC guidance encourages facilities to let residents and staff know about opportunities to receive vaccines in the community. It is possible that lower take-up of boosters could reflect increased difficulty in getting vaccinated in the community rather than on-site. Among nursing facility staff, initial take-up of COVID-19 vaccines was low until the health care worker vaccination mandate required providers that participate in Medicare and/or Medicaid to be vaccinated. Along with other factors, this mandate led to increased take-up of the primary vaccination series among nursing facility staff and early evidence suggests that it did not increase the frequency of staffing shortages.
Creating new opportunities for on-site vaccinations and updating the health care worker vaccination mandate to reflect current CDC guidance could increase the number of nursing facility residents and staff who are up to date with their COVID-19 vaccinations. The CDC recently updated the definition of “up-to-date” vaccination status for long-term care facilities to align with the definition of “up-to-date” that the CDC rolled out earlier more broadly across the country. Starting on September 2nd across the country and on September 26th for long-term care facilities’ reporting/surveillance purposes, the CDC’s new definition of “up-to-date” is having received a bivalent booster or having received a final shot of the original vaccines less than 2 months ago. Nursing facilities may have been subject to this delayed definition of “up-to-date” to align better with quarterly reporting periods. As such, they began reporting the percentage of residents who met the new “up-to-date” standard starting September 26th, 2022. After there are sufficient data available using the new definition, KFF will update this analysis and provide state-level results on State Health Facts.
Methods
This analysis uses federal data on staffing reported weekly by facilities to the CDC’s National Healthcare Safety Network (NHSN) and reflects weekly data through the week ending September 18th, 2022. These data are updated regularly to reflect revised data from previous weeks, so future versions of this dataset reflecting the same time period may output different values.
Each week, approximately 15,200 nursing facilities submit data through NHSN. CMS performs data quality checks to identify facilities that may have entered incorrect data before publishing this data for public download. Facilities that have submitted erroneous data will have an “N” displayed in the column titled “Passed Quality Assurance Check”. Our final sample of nursing facilities in this analysis excludes facilities that CMS flagged in their data quality check, as well as facilities that are missing shortage measures. This analysis reflects data from anywhere between 14,118 nursing facilities (93% of all facilities) and 15,043 nursing facilities (99% of all facilities) each week.