What Worked and What’s Next? Strategies in Four States Leading ACA Enrollment Efforts
Executive Summary
States have taken different approaches to implementing the Affordable Care Act (ACA) and have had varied enrollment experiences to date. This brief highlights the experiences of four states—Colorado, Connecticut, Kentucky, and Washington—that established a State-based Marketplace (SBM), implemented the ACA’s Medicaid expansion, and achieved success enrolling eligible individuals into coverage. Based on interviews with key stakeholders in each state, it identifies effective strategies that contributed to enrollment and current priorities looking forward. Key themes are summarized below; details on specific strategies and approaches utilized by the states are described in the full report.
Lessons Learned
Marketing and Branding
Broad marketing campaigns by the SBMs in all four states raised public awareness of new coverage options. Stakeholders identified several aspects of the campaigns that contributed to their success, including:
- Branding the coverage expansions as state initiatives;
- Conducting statewide marketing across diverse channels; and
- Providing promotional materials, like reusable shopping bags, to consumers.
Outreach and Enrollment Initiatives
Building on the broad branding and marketing efforts, local level outreach and enrollment efforts played a pivotal role in educating consumers and encouraging them to enroll into coverage. Stakeholders highlighted several successful aspects of the study states’ outreach and enrollment efforts, including:
- Conducting extensive outreach through numerous local avenues;
- Reaching large groups of people through events and local media;
- Going mobile with outreach and establishing walk-in enrollment sites;
- Utilizing existing data to facilitate enrollment; and
- Engaging providers in outreach and enrollment efforts.
CONSUMER ASSISTANCE
Given that consumers often require significant time and education to enroll, stakeholders agreed that one of the most important elements of enrolling people into coverage is one-on-one assistance provided through trusted individuals in the community. Lessons learned about consumer assistance efforts included:
- Recruiting a diverse group of assisters with ties to local communities;
- Developing strong relationships between assisters and brokers;
- Coordinating assistance through a regional hub and spoke structure;
- Providing readily available support to consumer assisters; and
- Expanding call center capacity and creating tiered assistance levels.
Systems and Operations
The effectiveness of the study states’ enrollment systems and their ability to quickly respond to technological glitches contributed to their enrollment successes. In addition, certain aspects of state policies and operations helped promote coverage efforts. Elements highlighted by stakeholders included:
- Developing close relationships between staff and contractors and setting realistic expectations for systems;
- Building effective enrollment systems with consumer-friendly features;
- Implementing workarounds and incremental fixes to quickly address system problems; and
- Using data and feedback loops to identify and respond to needs as they were identified.
Current and Future Priorities
The states were looking ahead to make continued improvements and focus on helping newly covered people access care. Stakeholders identified a range of key priorities looking forward including the following:
Enrollment and renewal
- Educating consumers about continued Medicaid enrollment and Special Enrollment Periods;
- Reaching remaining eligible but uninsured;
- Supporting continuity of coverage; and
- Continuing enrollment system upgrades and enhancements.
Consumer Assistance
- Enhancing training and support for assisters; and
- Ensuring adequate networks of consumer assistance are available.
Access and Utilization of Care
- Increasing health insurance and health care literacy among consumers;
- Connecting individuals to sources of care; and
- Maintaining safety-net provider capacity.
Issue Brief: Introduction & Background
As of summer 2014, states are reflecting on their experiences during the first open enrollment period for the new Health Insurance Marketplaces established by the ACA and looking forward to the next open enrollment period, which begins on November 15, 2014. States faced many challenges over the past year as they planned for and implemented the ACA coverage expansions. All State-based Marketplace (SBM) websites, as well as the Federally-facilitated Marketplace (FFM) website, HealthCare.gov, faced technological glitches and limitations during initial implementation, although the extent of these problems varied widely across states. States also faced the task of implementing major changes in policies and programs within a limited timeframe and coordinating and collaborating across programs, agencies, and stakeholders. Despite these challenges, as of April 2014, over 8 million Americans were enrolled in new Marketplace coverage and total Medicaid enrollment had grown by an estimated 6 million individuals since just before the start of open enrollment.1 , 2 States have taken different approaches to implementing the ACA and have had varied enrollment experiences to date. This brief highlights the experiences of four states—Colorado, Connecticut, Kentucky, and Washington—that each established their own SBM, implemented the ACA’s Medicaid expansion, and achieved success enrolling eligible individuals into coverage. It identifies key strategies that contributed to their success during open enrollment and highlights their current and future priorities. It is based on in-person interviews conducted during May 2014 with a range of stakeholders in each state, including Medicaid and Marketplace officials, advocates, enrollment assisters, and providers.
Background
The two primary ways the ACA increases coverage are through the creation of new Health Insurance Marketplaces that offer health insurance plans and advanced premium tax credits to help offset the cost of coverage for moderate-income individuals and the expansion of Medicaid to low-income adults. States have options with regard to how they implement these expansions. They can establish their own SBM, default to the FFM, or build a Marketplace in partnership with the federal government. As enacted, the ACA also required all states to expand Medicaid to nearly all adults with incomes at or below 138% FPL ($27,310 for a family of three in 2014) beginning January 2014, but the June 2012 Supreme Court ruling on the ACA effectively made this expansion a state option. As of July 2014, 27 states including the District of Columbia are implementing the Medicaid expansion in 2014.3
Regardless of their implementation choices for the ACA coverage expansions, all states must also implement streamlined Medicaid enrollment processes that offer individuals multiple options to apply (including online, by phone, in person, and by mail), rely on electronic data to verify information, and seek to provide real-time eligibility determinations. These processes are designed to be coordinated across Medicaid, the Children’s Health Insurance Program (CHIP), and Marketplace coverage to create a “no wrong door” enrollment system. Whether an individual applies directly to Medicaid or through a Marketplace, he or she is to be enrolled in the program for which he or she is eligible. To implement these new processes, many states have needed to make significant upgrades to antiquated Medicaid enrollment systems or build new systems.
The four study states—Colorado, Connecticut, Kentucky, and Washington—vary geographically and demographically (See Appendix Table 1). However, all four states elected to build their own SBM4 and implemented the full Medicaid expansion as of January 2014, with three of the four states (Colorado, Connecticut, and Washington) using available options to get an early start on extending Medicaid to adults. Moreover, all four states achieved significant enrollment in both their Marketplace and Medicaid programs over the course of the 2014 open enrollment period. Medicaid gains, in particular, were very strong, far exceeding the national average and outpacing some of the states’ growth estimates. As discussed below, stakeholders credit this enrollment success to a range of strategies employed for their marketing and branding campaigns; outreach and enrollment initiatives; consumer assistance networks; and overall systems, operations, and leadership. Looking ahead, the study states are focused on an array of future priorities and continued improvements to further build upon their successes to date.
Issue Brief: Lessons Learned
Marketing and Branding
Broad marketing campaigns conducted by the SBMs in all four study states raised public awareness of new coverage options. Stakeholders identified several aspects of the campaigns launched within the study states that contributed to their success, including:
Branding the coverage expansions as state initiatives.Employing lessons learned from the implementation of CHIP, the four study states used state-specific branding for their Marketplaces, which helped detach the coverage expansions from the ACA or “Obamacare” (Figure 1). This state-specific branding proved important, especially in Kentucky and in portions of the other three states, where many residents are distrustful of government programs and not politically supportive of the ACA. Kentucky directed all residents seeking health insurance to “kynect, Kentucky’s Health Care Connection.” It also created animated characters that were representative of different types of Kentuckians who could benefit from the new coverage options, to which stakeholders felt consumers responded well (Figure 2). Stakeholders in Washington indicated that its Marketplace name, “Healthplanfinder,” was intended to sound like a commercial product, which research showed would attract broad interest. Connecticut focused on making its Marketplace, “Access Health CT,” stand out from other entities by choosing orange as a brand color instead of blue, which is used by other entities in the state, including the University of Connecticut and the state seal. Connecticut and Washington also have state-specific names for their Medicaid programs. Connecticut named its Medicaid program for adults Husky D, and Washington changed the name of its Medicaid and CHIP program for children, “Apple Health for Kids,” to “Washington Apple Health” when it expanded to adults.

“I think the approach that the governor took on this whole thing was to not talk about it in terms of Obamacare or the Affordable Care Act. He talked about it in terms of…Kentucky’s health…This is not about President Obama, it’s not about Governor Beshear, it’s not about politics, it’s not about any of these things. It’s about improving the health of our state, so that kind of takes the argument out of it.” –Kentucky Marketplace Official

Conducting statewide marketing across diverse channels. All four states began extensive statewide marketing campaigns for the coverage expansions early and used diverse channels, including television, radio, print, billboards, and social media. Messaging during the early part of open enrollment conveyed a simple, straightforward message about the availability of new coverage options and focused on raising brand awareness of the new Marketplace. Some messaging emphasized the opportunity to improve residents’ health and the availability of financial assistance. Most messaging did not distinguish between Medicaid and Marketplace coverage options.
Adapting messaging over time. In all four study states, messaging evolved toward the latter end of open enrollment to focus on the March 31st enrollment deadline and to highlight how consumers have benefited from new coverage options (Figure 3). For example, Connect for Health in Colorado launched a digital billboard that counted down the days until the end of open enrollment. Connecticut created a “Because I Got Covered” print campaign in English and Spanish to disseminate stories about how gaining health insurance helped a variety of different people and to encourage individuals to enroll before the deadline. Stakeholders in Washington also noted that they sought to create a sense of urgency to enroll by running new ads toward the end of open enrollment.
“I think the idea of creating a sense of urgency is always important if you want to get people to take action, especially on something where there’s a deadline…And a lot of our earned media outreach had to do with the deadline and pushing news out there about the deadline and we got our lead organizations out there pushing news on the deadline.” –Washington Marketplace Official

Providing promotional materials for consumers. Stakeholders also noted that promotional materials were helpful tools to garner consumer interest and increase brand awareness for the Marketplaces. For example, Kentucky distributed reusable shopping bags that were extremely popular among consumers. The state gave away over 100,000 bags during open enrollment, including 22,000 bags over the course of 12 days at the state fair. The bags were branded with the kynect logo and caricatures, and had Marketplace contact information, including the website and call center phone number. Kentucky also gave away branded napkins and fans. During the summer before open enrollment, Connecticut Marketplace staff distributed sunscreen on the state’s beaches that had the Access Health CT logo and website address.
Outreach and Enrollment Initiatives
Broad branding and marketing efforts helped raise consumer awareness of new coverage options, and local level outreach and enrollment efforts played a pivotal role in educating consumers and encouraging them to enroll into coverage. Stakeholders highlighted several successful aspects of the study states’ outreach and enrollment efforts, including:
Conducting extensive outreach through numerous local avenues.Stakeholders in the four study states stressed the importance of conducting a broad range of outreach and enrollment initiatives at the local level and identified a variety of avenues where they successfully reached consumers, including churches, college campuses, beauty and barber shops, local grocery or community stores, libraries, extension centers, small businesses, and even people’s homes. They noted the importance of developing trust when reaching consumers through these avenues and of finding a local champion within each community to support outreach efforts. For example, in Connecticut, Navigators worked to engage local small businesses in outreach. To reach consumers in a rural farming community in Kentucky, one assister had a local farmer discuss the importance of insurance. The farmer’s ability to reference specific accidents that might happen on a farm for which it would be important to have health coverage resonated with the community. A number of community-based organizations noted that they promoted health coverage enrollment as part of a broader array of services they offer. In Washington, for example, one organization that provides meals and other services, such as counseling and employment referrals, to homeless and at-risk youth integrated healthcare enrollment into the package of services offered. Because of their existing relationships serving the community, these organizations were often viewed as credible messengers by consumers.
“We built teams of really highly performing assistors that were really good at enrollment and outreach. And we built these teams around our most critical zip codes…These teams would then do zip code specific outreach to small businesses. They hit every barber shop, every nail salon…every PTA meeting. They went to car dealerships and pizza shops and every little mom and pop shop in their zip code.” –Connecticut Marketplace Official
.
“You need to… find that local champion; so, for example, in my community where I grew up, that was my mother …. She set up for me to speak at her church and then stay afterwards and answer anyone’s questions. …Where my grandma lives, we set up an enrollment day at my grandma’s house…”
–Kentucky Assister
Developing customized outreach materials and resources. Assisters indicated that they developed customized outreach materials and resources to better connect with the specific communities they serve and meet their specific cultural and linguistic needs. For example, in an area of Connecticut with a large Portuguese-speaking immigrant population, brokers and assisters created fact sheets in Portuguese. Similarly, an assister in Colorado who serves the African American community developed informational materials that focus on the importance of obtaining health coverage to address some of the specific health problems faced by African Americans. Assisters also developed customized tip sheets and checklists to help ensure that individuals had all the information they needed to enroll when they started an application.
“…In one of our flyers that we created just to advertise our site, we would list things that would help; please bring… your Social Security card, your driver’s license, your last pay stub, citizenship status….” –Colorado Assister
Reaching large groups of people through events and local media.In all four study states, local community events such as fairs and sporting events served as valuable opportunities for states and assisters to efficiently reach large numbers of people. For example, in Washington, the Marketplace built a phone charging station at a popular music festival and stationed assisters by it to reach out to young adults. The state also sponsored roller derby, minor league hockey, and select league soccer and football games. In Kentucky, Marketplace and Medicaid officials and assisters attended festivals and events throughout the state, including the state fair, where they distributed information about new coverage options and encouraged people to enroll (See Box 1). States and assisters also created their own enrollment events. For example, in Kentucky, the Marketplace promoted a “Sign-up Saturday” event at local libraries, during which assisters helped people enroll using the library computers. Assisters in Colorado also hosted group enrollment appointments at local schools and libraries. Additionally, in some cases, assisters used local media outlets to reach large numbers of consumers. For example, some assisters in Kentucky participated in a weekly call-in show on the local news station, during which consumers could call in with questions about coverage options.
Box 1: Using the State Fair to Promote Outreach and Branding in Kentucky
The state fair in Kentucky has been a tradition for over 100 years. The fair is held in August at the Kentucky Exposition Center and attracts about 600,000 people annually. The 2013 state fair and other festivals and large sporting events across the state served as a key opportunity to provide information about new coverage options to large numbers of people. Marketplace and Medicaid officials and assisters hosted informational booths at these events to raise awareness about the new coverage options available through kynect and initiate one-on-one conversations with interested consumers (Figure 4). Officials and assisters found that starting with the question, “Do you know somebody that doesn’t have health insurance?” was a highly effective way to initiate conversations with individuals at these events. In addition, one successful way they engaged consumers at these events was by giving away reusable kynect shopping bags. These popular, colorful bags included the kynect logo and the caricatures that appeared in ads and other kynect marketing and have been credited with successfully raising awareness of kynect and initiating a marketing buzz. In total about 100,000 bags were given away during open enrollment with 22,000 given out in the 12 days of the 2013 state fair. Replicating the logo and characters on t-shirts and even hot air balloons made it difficult to go anywhere in the state without hearing about kynect.

“[The bags] were like gold. I mean they were just really pretty, colorful, and instead of us sitting there talking about healthcare, we’d say, ‘have you heard about kynect, let me tell you about kynect’ and then people would stop and listen, and ‘do you have health insurance,’…and if they said ‘yes, I have health insurance,’ ‘well do you have a child or do you have somebody that you know that doesn’t have?’ We made those connections and I think that that was one of our biggest success factors…. The state fair is getting ready to come up again in August. We’ll have a presence there. We’ll have a big booth.” –Kentucky Medicaid Official
Going mobile with outreach.The four study states employed a number of successful mobile outreach and enrollment strategies to reach uninsured consumers in places where they live, work, and play. Marketplace staff in Colorado and Kentucky travelled across their respective states in branded Marketplace RVs to promote coverage and get people enrolled (Figure 5). Washington and Colorado also deployed street outreach teams to do targeted outreach. Staff from the King County Public Health Department in Washington used tablets to find and collect information from uninsured homeless individuals and submitted Medicaid applications on their behalf. In Colorado, outreach street team members used tablets to collect contact information from young adults and Latinos in heavily populated areas. They then forwarded the information to the Marketplace staff, which would follow up with individuals about next steps to enroll. Consumers who spoke with a street team member also immediately received a thank you email with information on where to obtain enrollment assistance. The outreach street teams in Colorado spoke with over 64,000 people in more than 230 locations, including community events, shopping areas, theaters, gyms, coffee shops, and on streets with heavy foot traffic. In Connecticut, Marketplace staff conducted outreach at grocery stores and other retail outlets prior to open enrollment. Contact information was collected from those who stopped by booths in these locations, and individuals were subsequently sent information on enrollment assistance and enrollment events in their area. The state ultimately enrolled about 25 percent of those with whom they spoke at the retail outreach sites.

“So what we learned from the RV campaign was that when you did publicity, because we did press releases and we used our paid media channel, when we could promote the fact that we were going to be in certain communities for these opportunities…. people showed up, there were lines…” –Colorado Marketplace
Establishing walk-in enrollment sites.Marketplaces in Colorado and Connecticut provided additional opportunities for individuals to enroll in their communities by establishing walk-in enrollment sites. Access Health CT built storefronts in densely-populated urban areas to encourage people to walk in, collect information about coverage options, and obtain enrollment assistance from assisters or brokers. Data suggest that approximately 15,000 people visited the enrollment storefronts during open enrollment, and nearly 8,000 of them enrolled in coverage on the spot. Others obtained educational materials and often enrolled later. In March, Colorado opened five temporary walk-in enrollment sites in heavily populated areas that were staffed by Connect for Health Colorado and Medicaid agency staff, enrollment assisters, and insurance brokers. Nearly 3,000 people received help through these sites during the three weeks they were open.
Utilizing existing data to facilitate enrollment.Colorado, Connecticut, and Washington took up opportunities to get an early start on expanding Medicaid to adults prior to full implementation of the Medicaid expansion to adults in January. When the full Medicaid expansion took effect in January 2014, they automatically transitioned adults from these early expansion programs to the expansion. Colorado also enrolled more than 40,000 adults who were on the waitlist for the early expansion, which had limited enrollment. After enrollment began, Colorado also used data generated from the Connect for Health Colorado enrollment system to target outreach and enrollment efforts. Staff made outbound calls to individuals who started an account or application but did not complete enrollment to encourage them to enroll and refer them to local sources of enrollment assistance or a local enrollment event (See Box 2).
Box 2: Coordinating Targeted Outreach Campaigns with Local Enrollment Events in Colorado
In Colorado, Marketplace officials noted that one of their most successful outreach and enrollment initiatives was a series of targeted outbound campaigns from the Marketplace that directed individuals who had created a Marketplace account to local enrollment events. Over the course of open enrollment, the Marketplace generated lists of individuals who created an account but did not yet complete their enrollment into coverage. The Marketplace then conducted a series of outbound campaigns to these account holders to remind them to complete enrollment and direct them to sources of local assistance. When the Marketplace held an enrollment event in a specific community, it would reach out to account holders who had not completed in their enrollment in that community prior to the event to let them know about the event. They also used these campaigns to direct people to the temporary walk-in enrollment sites that were created in March and local enrollment events hosted by community partners and assisters. In total, the Marketplace made over 100,000 calls and sent over 500,000 emails to individuals who had created an account.
“What we would do is if we had an event that, say a broker group or an assistant site was having in a community, we would reach out directly to our account holders in that community and tell them about that… event. So, we did targeted outreach to our account holders and to potential customers to let them know about where they could get local assistance, when there was local assistance available.” –Colorado Marketplace Official
Engaging providers in outreach and enrollment efforts. Safety net providers were key partners in outreach and enrollment efforts since a large share of their patient populations are uninsured and eligible for the coverage expansions. Stakeholders noted that hospitals and community health centers played an important role in enrollment because they have existing relationships with their patients and their staff is often well-versed and experienced in communicating with their patients and with enrolling people into Medicaid and CHIP coverage. For example, in Kentucky, federally-qualified health centers conducted extensive “in-reach” to their uninsured patients to help enroll them in coverage. In addition, they helped enroll other uninsured individuals in the community. Similarly, a community health center in Washington reached out to uninsured patients in its service area by phone and email to encourage them to visit the clinic for help enrolling.
“The community health centers [sent letters] to their patient population that they knew were uninsured…they have this… audience that they know is uninsured… and they know who they are and they know how to reach them and they have staff who speak their language who are skilled in doing enrollments.” –Connecticut Assister
Consumer Assistance
Stakeholders in all four study states agreed that one of the most important elements of getting people successfully enrolled into coverage is personalized, one-on-one assistance provided through trusted individuals in the community. Within the study states, stakeholders identified a number of lessons learned about successful consumer assistance efforts including:
Recognizing that enrollment often requires time and education.Stakeholders noted that in order to develop trust and overcome misperceptions or fears about the ACA, individuals often require time and multiple touches from an assister. This was especially true among rural populations and immigrants. Since many newly enrolling consumers have limited experience with insurance, stakeholders indicated it is important to educate individuals about insurance and allow them time to familiarize themselves with what insurance is, what their costs would be, and various plan options. Given these consumer needs, successful enrollment of an individual or family sometimes requires multiple touches or visits with an assister.
“…Rarely does somebody walk in and an hour and a half later they walk out with a plan. It’s typically a series of many different appointments and hours spent.”–Colorado assister
.
“I think we acknowledged very early on… this… wasn’t going to be a big ad blitz and people were just going to miraculously sign up. People were going to really want to have their hand held…You can do some of that through the call center but I think people distinctively wanted to have the opportunity to do this in person.” –Connecticut Marketplace Official
.
“I think we achieved really good geographic distribution and then we also managed to really help serve specific targeted populations, which was also a goal…And then I was really happy to see that most of the state’s rural areas, they were all very much aware of the need for bilingual assistance and …looking at those vulnerable populations and rural areas as well.” –Colorado Marketplace official
Recruiting a diverse group of assisters with ties to local communities. The study states established extensive consumer assistance networks that often drew on existing networks of assistance, including those providing Medicaid and CHIP enrollment assistance, health clinics, community-based organizations, hospitals, and advocacy organizations. Several different types of paid and volunteer assisters supported outreach and enrollment efforts, including Navigators, In-Person Assisters, and Certified Application Counselors.5 Assisters had varied backgrounds and were able to provide personalized assistance to the communities they served. In Connecticut and Washington, assister organizations were required to have bilingual staff that spoke the predominant languages of the areas in which they worked and who identified with the communities’ culture. For example, in Connecticut, the Hispanic Health Council was the lead assistance organization in a region with a predominantly Hispanic population. Some assisters also said that because of their personal ties to the community, local organizations, schools, and other groups were often willing to work closely with them and sometimes offered resources, such as space and equipment, to support enrollment.
Developing strong relationships between assisters and brokers.In addition to enrollment assisters, insurance brokers played an important role in enrollment. Washington estimates that brokers enrolled over 100,000 people into coverage during open enrollment, including one in ten new Medicaid enrollments. In Kentucky, roughly 40 percent of enrollments into qualified health plans were facilitated by insurance brokers. The Marketplaces in all four states undertook significant efforts to engage brokers in enrollment and, despite some early fears and concerns among brokers, a large number of brokers in the four study states were certified and often worked collaboratively with assisters to enroll uninsured people. For example, in a hospital in Connecticut, brokers and enrollment assisters worked together closely, with the brokers referring Medicaid questions to the enrollment assisters and the assisters often relying on the brokers to share details of plans or private coverage options. Similarly, in Colorado, where over 1,500 brokers and agents were trained and certified by the Marketplace, stakeholders noted that having brokers and enrollment assisters attend enrollment events together strengthened their efforts. An assister could help an individual complete the application and then a broker could help that individual make a plan choice. Some assisters noted that brokers were particularly helpful in assisting individuals with specific health needs such as HIV and diabetes. Because they often had more familiarity with the plans, brokers were well-equipped to advise consumers about which drug formularies and services were covered in each plan.
“Agents felt very threatened about it, so very early on, both the Commissioner of Insurance and our folks assured agents that they’re going to have a role and they’re going to have a very important role. And so when we set up the advisory broad, we established several subcommittees and one of them was a subcommittee called Agents and Navigators. …The idea was that we were going to put the two competing forces…together and see if we couldn’t work out some kind of agreed to relationship.” –Kentucky Marketplace Official
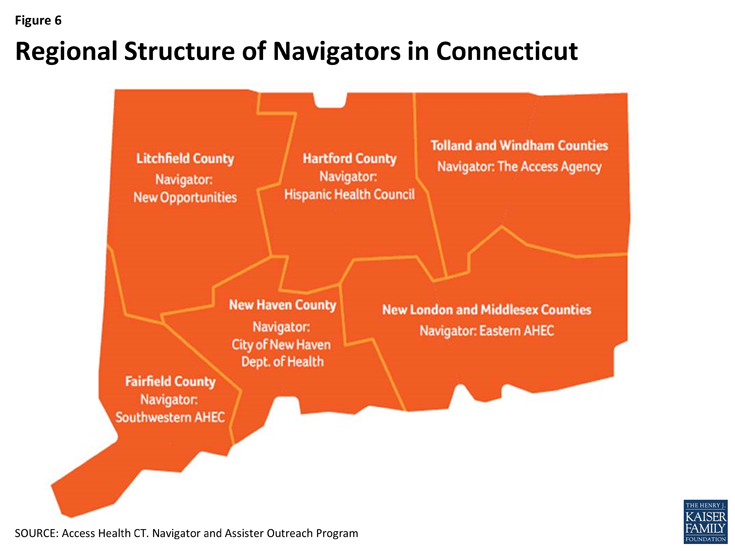
Coordinating assistance through a regional hub and spoke structure.All four states utilized a regionally-based hub and spoke structure to organize and coordinate assister activities. Within this model, several lead regional organizations helped organize and coordinate activities of assisters in their area, disseminate updates and information from the state to assisters, and provided feedback on implementation to the state. For example, Access Health CT divided the state into six regions and assigned Navigator organizations to oversee the work of assisters in each area (Figure 6). In some states, broader coalitions of stakeholders also helped coordinate and organize activities. For example, in Louisville, the local Board of Health established an outreach and enrollment coalition that coordinated efforts, shared best practices, and provided feedback on experiences in the field to the state. Similarly, in Colorado, an existing statewide coalition served as a liaison between on-the-ground assisters and the Medicaid agency and Marketplace. The coalition was valuable for sharing information between assisters and state officials to help address issues that arose during open enrollment. Assisters in Kentucky and Connecticut also used shared online calendars to indicate where and when they were planning events, which helped prevent gaps and overlaps in outreach and enrollment efforts.
“We had a lead organization run point on that region of the state. And within those lead organizations that were selected for the respective regions…they had to demonstrate how they were going to set up a network that was going to be able to help them reach goals as it related to enrollment and assistance and outreach…and it had to include outreach [in] different languages, different backgrounds, depending on where they were…There was a lot of creativity provided by these lead organizations and they did a really good job.”
–Washington Marketplace Official
Providing readily available support to consumer assisters. All four study states established resources for assisters and brokers to obtain support when they had questions or needed assistance while helping a consumer. Assisters had dedicated telephone lines to reach call center staff, which helped reduce long waits when they needed support. Colorado and Connecticut had several Marketplace staff members dedicated to addressing assister needs and questions. At the launch of open enrollment, the staff held daily phone calls with assisters to provide updated information on processes and obtain feedback, which was used to continually improve processes and systems. The staff was also readily available by phone or email to help assisters with complex cases, website problems, and other issues. In Connecticut, the Marketplace placed staff, called Navigator Coordinators, in each of the regional lead consumer assistance organizations. These coordinators had greater access to the eligibility system than Navigators or assisters and could help troubleshoot technical problems. Marketplace staff in Connecticut also organized monthly meetings of regionally-based assisters to share best practices, coordinate events, and discuss strategies for reaching particular populations. In Washington, the Marketplace sent weekly emails to lead assistance organizations to communicate key lessons, responses to questions, and the status of system fixes and also hosted weekly calls. Kentucky also maintained close and regular communication with assisters to both share updates and information and receive feedback on implementation.
“I really love the people that work with Assistance Network of Connect for Health Colorado; they are really responsive, they are really open, and they know their stuff…. During open enrollment they hosted weekly support calls with all the health coverage guides and application counselors and… whenever somebody had a question or an issue it got resolved right then and… whenever I send them an email… it always gets responded even when if it’s.. 8 pm or 10 pm….” –Colorado Advocate
Expanding call center capacity and creating tiered assistance levels.Stakeholders in all four study states noted that their Marketplace and Medicaid call centers were an important resource for consumers. Because of early technological challenges with the enrollment portals, the call centers became a primary resource to answer consumer questions, take phone applications, and work through glitches. Consumer demand for the call centers exceeded expectations early during open enrollment. In Washington, for example, the Marketplace call center anticipated receiving about 2,500 calls per day but averaged between 8,000 and 10,000 calls daily. The states enhanced capacity to respond to this increased demand by training and hiring more staff, contracting with additional vendors, extending call center hours, and creating tiered levels of assistance so calls could be directed based on what type of assistance a caller was seeking. For example, consumers seeking information would be routed to different staff than those attempting to complete enrollment via the phone.
“…Nobody, I mean nobody anticipated the demand or volume of calls or even the length of the calls.”–Kentucky Marketplace Official
Systems and Operations
The study states took different approaches to building their enrollment systems and faced varying degrees of early technological challenges. The effectiveness of the study states’ enrollment systems and the states’ ability to quickly respond to technological challenges also contributed to their enrollment successes. In addition, stakeholders identified certain aspects of state policies and program operations that helped promote coverage efforts. Elements highlighted by stakeholders included:
Developing close working relationships between staff and contractors and setting realistic expectations for the system builds. Stakeholders stressed that close collaboration among policy staff, IT systems staff, and contractors were vital during both the initial builds of the system and on an ongoing basis to manage systems and quickly resolve problems. Connecticut had Marketplace staff dedicated to working with contractors to monitor their work and track their progress. In all four states, contactors were co-located on site with state policy and IT staff to facilitate close and constant communication. Moreover, stakeholders stressed the importance of setting reasonable expectations for system capabilities, recognizing that enhanced features can continue to be added over time. For example, Access Health CT limited the extent of features it planned to include halfway through its system build to focus on core functions.
“It’s an excellent relationship. I mean [the IT contractor] is right here in this building…they got 45 staff here that work with our staff…and we’re all located here in this building, which is very important so if we have an issue… we just go down the hall to see what’s going on, and we meet with them regularly, so they’ve been a great partner.” –Kentucky Marketplace official
.
“Creating disciplined processes [was important]. So figuring out what you can do well and what you can’t….For example, in January of 2013, we rolled back by 30 percent what we had originally asked [the contractor] to build for us in the fall of 2012. That was the most important decision we made. If we had kept with our original plan, I’m not sure we would have been up and running.
–Connecticut Marketplace official
Building effective enrollment systems with consumer-friendly features. Kentucky and Washington built single, integrated eligibility systems for Medicaid and Marketplace coverage. This allowed for a streamlined enrollment process that did not require any transfers of applications between programs. Moreover, consumers only receive a single notice of their determination rather than separate notices from each program, which minimized confusion. Stakeholders indicated that, while these systems faced some early technological glitches, and the states continue to work through problems, they worked well for most consumers, particularly toward the end of open enrollment. The systems are also able to make real-time determinations for most cases and can handle complex situations in which members of a family may be eligible for different types of coverage. Colorado and Connecticut maintained two separate systems for Medicaid and Marketplace coverage and faced some challenges coordinating enrollment between the two systems. However, as described below, through workarounds and ongoing system improvements, they were still able to enroll people successfully. Stakeholders also highlighted certain features of systems that proved particularly valuable. For example, in Kentucky and Connecticut, stakeholders highlighted a pre-screen feature that allows consumers to anonymously shop for coverage after answering a few quick questions, as well as the ability to electronically upload documentation when it is required.
“It’s a one stop shop. You know, it takes maybe 30 to 45 minutes. You enter your information. If you’re Medicaid eligible, you pick a Medicaid managed care organization. If you’re QHP eligible, you pick a qualified health plan. So, certainly that one stop shop streamlined application process I think really attributed to our success.” –Kentucky Marketplace Official
Implementing workarounds and incremental fixes to quickly address enrollment system problems. Stakeholders noted that although all of the study states faced early problems with their enrollment systems, they implemented workarounds and solutions that allowed them to continue to enroll people. For example, in Washington, assisters used paper applications during the early part of open enrollment while the system was experiencing problems. Similarly, in Colorado, consumers were redirected to the call center to complete applications during the initial launch of open enrollment as full functionality for the Marketplace system was still being established. Connecticut is still continuing to work to improve the process to transfer applications from the Marketplace to Medicaid, but in the interim is sending notifications to providers advising them that individuals determined eligible for Medicaid through the Marketplace can access services before they receive a benefit card. All states also created workarounds to address system glitches that affected some immigrant families, people formerly involved in the criminal justice system, and those in other complex family situations. Beyond implementing workarounds, the states made ongoing improvements to their systems throughout open enrollment to fix problems as they were identified. For example, the Medicaid agency in Colorado established a flexible contract with its vendor that provided dedicated time for system fixes to be implemented each week.
“One thing that I think [the Medicaid enrollment system] did really well is that, when they realized that there was some sort of… problem or barrier for people, they changed things.” –Colorado Advocate
Using data and feedback loops to identify and respond to needs as they were identified.Medicaid and Marketplace officials in the study states received frequent enrollment data updates that helped them identify any problems with their enrollment systems and target outreach and enrollment efforts. For example, in Connecticut, the Marketplace shared regular data updates on enrollment by zip code with regionally-based assisters to help them target their community-based outreach efforts. Similarly, the study states obtained regular feedback from assisters and community-based organizations and quickly responded to any implementation issues they identified. For example, Colorado launched a statewide brand awareness campaign in English and Spanish, but learned that the Spanish messaging was not resonating with consumers. In response, the Marketplace quickly organized a stakeholder group meeting and brought in the translation firm to create revised materials that would better connect with the Spanish-speaking community.
“…We had staff… that monitored the system. We had what we called our command center…where we would watch all the statistics so, how many applications, is the system up, what’s our capacity? We even monitored the call center at the command center…. The first of order of business was to determine if there is some kind of a system error that’s going on here; is this a user error that’s going on so, and as we got complaints about things…you build up this tracking system or this ability to see what kind of changes need to be made.”
–Kentucky Marketplace official
Collaboration and Leadership
Promoting coverage efforts through strong leadership. Stakeholders in the study states noted that there was strong leadership for their coverage efforts. For example, in Kentucky, the Governor made successful implementation of the coverage expansions a priority, and this leadership carried down through state officials. Stakeholders reported that Marketplace and Medicaid officials were highly engaged and personally committed to achieving success and were often present at outreach and enrollment events. Similarly, stakeholders in Colorado and Washington noted that implementation of the ACA built on earlier state health reform efforts that created streamlined Medicaid enrollment policies and helped establish a culture of coverage in the state.
Collaborating with key stakeholders. In addition to strong leadership, the study states cited close collaboration between stakeholders as a key contributor to their success. In Kentucky, all state agencies involved in health reform implementation, including Medicaid, the Marketplace, and the Department of Insurance are peer agencies housed within the Kentucky Cabinet for Health and Family Services. Stakeholders indicated that this structure helped promote strong working relationships among the agencies and that they worked hand-in-hand throughout planning and implementation of the coverage expansions. Stakeholders in Colorado also indicated that close collaboration between the Medicaid agency, Marketplace, and Department of Insurance was important and noted that an interdepartmental website was developed to share information with consumers. In addition, in all four states, advocates and community-based organizations were engaged early and often throughout planning processes and implementation. For example, in 2012, Connecticut began a series of town hall meetings called “Healthy Chats” and invited advocates, insurance carriers, and other relevant stakeholders to learn about progress in implementation and share feedback.
“We have weekly stakeholder meetings over at [the Marketplace]. It gets us all in a room and it’s a lot harder to fuss when you’re looking at somebody because we’re all peer agencies. We’re all under the same umbrella but it’s easy to get frustrated. If you all get in a room once a week it’s hard to stay frustrated because you just ask the questions and work through things. I think they’ve been very effective.” –Kentucky Medicaid Official
.
“I would say the foundations of our success from an outreach, communications, and marketing standpoint are that we had a strong foundation of working with stakeholders and we continued to be committed to that process to today. So every policy decision that the Board made, we had stakeholder discussions…before they made their decisions. So from a policy prospective, from an operational prospective, but also from an outreach and communications prospective they were at the table.”
–Colorado Marketplace Official
Issue Brief: Current And Future Priorities
To build on their successes and lessons learned from the past open enrollment period, the study states were looking ahead to make continued improvements and focus on new priorities related to helping newly covered people understand how to use their health insurance and access needed care.
Enrollment and renewal
Educating consumers about continued Medicaid enrollment and Special Enrollment Periods for Marketplace coverage. Stakeholders indicated that now that open enrollment has ended, they are focused on making sure that consumers know they can still enroll in Medicaid and may qualify for a Marketplace special enrollment period. Assisters are playing a key role in spreading this message and some of the states are conducting outreach with this information (Figure 7). Medicaid and Marketplace staff also noted plans to continue outreach to groups such as graduating students and new mothers who may be Medicaid eligible or able to enroll through a special enrollment period.

Reaching remaining eligible but uninsured. Although all four study states successfully enrolled a large number of people in coverage, stakeholders recognized that there remain eligible individuals that they were not able to reach and enroll and are focused on identifying strategies to reach these consumers. In all states, Medicaid and Marketplace staff indicated that they are in the process of collecting more detailed information on who enrolled, including data on race, ethnicity, and language. Some also are conducting surveys to learn about consumers’ experiences enrolling. Staff indicated that they plan to analyze data to gain a better sense of who the remaining eligible but uninsured are in their state and determine the best strategies to reach them. Stakeholders highlighted several hard-to-reach groups whom they plan to target through specific outreach efforts during the next open enrollment periods, such as veterans, the LGBTQ community, individuals with limited English proficiency, young adults, and justice-involved populations. Marketplace staff in all states are also focused on increasing enrollment of small businesses in their Small Business Health Options Program (SHOP).
“Once we get a firm sense for sort of who we just enrolled, that leads to the next question which is, well, who’s still left? And we’d like to go back out to the Marketplace and then try to assess what the uninsured rate currently looks like and then who those people are.” –Connecticut Marketplace Official
Supporting continuity of coverage. Stakeholders are also focused on ensuring that individuals who enrolled in coverage maintain it. Connecticut, Kentucky, and Washington are already conducting Medicaid renewals through their new integrated enrollment systems. Based on early data that suggested that the renewal rates in Washington after this change were lower than expected, the state implemented a multi-pronged renewal reminder system, which helped raise renewal rates to pre-ACA implementation levels (See Box 3). Medicaid staff in Colorado indicated that they are still in the process of determining how they will conduct Medicaid renewals and are seeking to make the process as automated as possible. State officials in Colorado noted that they provided enrollees a pre-populated renewal form prior to ACA implementation and would continue to renew based on existing information unless a consumer reported a change in circumstances. The states are also exploring options to remind consumers about maintaining coverage. Connecticut began doing robo-calls to individuals not paying premiums, and Washington is considering sending text and email renewal reminders for Medicaid beneficiaries.
Box 3: Facilitating Retention in Washington through a Multi-Pronged Reminder System
In late 2013, the Washington Health Care Authority implemented a multi-pronged renewal reminder system to promote retention among Medicaid and CHIP enrollees and facilitate the transfer of their electronic accounts into the new Washington Healthplanfinder eligibility system. In 2014, all Medicaid and CHIP enrollees in Washington must complete their annual renewals by submitting a new simplified application to the Healthplanfinder online, through the mail, or in person. The Washington Health Care Authority, concerned that enrollees may not be familiar with this new process, began sending reminder letters 60, 40, and 20 days prior to enrollees’ scheduled renewal date with information about how to renew and how to obtain help from community-based organizations. Enrollees also receive a reminder call. Individuals who do not successfully renew by their renewal date receive a letter explaining that to continue receiving coverage, they may mail in a tear-off stub at the bottom of the letter using a self-addressed postage pain envelope (included with the letter), send an email, or call a designated toll-free hotline.
As of March 2014, nearly 417,000 renewals had been successfully completed in the new Washington Healthplanfinder portal and renewal rates have not reached a level consistent with what they were pre-ACA implementation. State officials credit the multi-pronged approach with increasing public awareness of the need to renew coverage and are looking forward to 2015, when most renewals occur through electronic matches with existing data sources and without the need for consumers to take any action.
“I think we all knew to a degree, that this conversion was a big lift…The renewal process of the future is going to be a much simpler, more passive process for the enrollee, with the auto data match capacity of the Exchange.” –Washington Medicaid Official
Continuing enrollment system upgrades. All four study states continually improved the functionality of their enrollment systems throughout the open enrollment period and plan continued improvements and enhancements moving forward. Colorado is planning to move to a single integrated system for Medicaid and Marketplace determinations and to add more features, including electronic uploads of documentation. Kentucky is moving all Medicaid determinations, including disability-based determinations, as well as those for other social service programs, to its new system. It also plans to enhance the plan browsing experience for consumers by incorporating estimated premium tax credit subsidies into the prices they view. Washington is building the ability for Medicaid enrollees to enroll in a managed care plan through the Marketplace portal instead through the separate Medicaid system. Connecticut is continuing work to upgrade its Medicaid system to allow for greater coordination with the Marketplace. The Connecticut Marketplace also recently launched an enrollment app for smartphones and tablets, based on data collected indicating that large shares of individuals enrolled on smartphones and tablets. Colorado launched its mobile app in 2013 and is working to enhance its functions for the next open enrollment period.
Consumer Assistance
Enhancing training and support for assisters. Stakeholders in all four study states generally indicated that it will be important to enhance and improve training for assisters for the next enrollment period to address gaps in knowledge and improve their ability to handle complex cases. For example, some assisters emphasized a need for more hands-on training with the eligibility portal. Given that a large number of assisters in Connecticut had prior experience in Medicaid, some suggested they would benefit from increased training on private coverage and strategies to convey information about premiums and cost sharing to enrollees. Conversely, brokers and other assisters indicated a desire for more training on Medicaid, and, in Colorado, both Medicaid and Marketplace officials indicated that they plan to incorporate more information on Medicaid into the training sessions. Some stakeholders also suggested that combined training sessions with assisters and brokers would beneficial and allow them to share tips and other information. Finally, a few assisters noted that, because many consumers are continuing to rely on them for other types of assistance beyond enrollment, it would be helpful to incorporate additional professional development training into curricula, including modules on effective documentation, conflict resolution, cultural competency, and how to access other social services. Beyond enhanced training, stakeholders also indicated that it will be important to continue to develop the technical assistance and support made available to assisters to make sure they have readily available access to help that can answer questions, assist with complex cases, and help resolve any technological related enrollment problems.
Ensuring adequate consumer assistance. Stakeholders also agreed that one-on-one in-person assistance will remain essential for the next open enrollment period, especially for targeting hard-to-reach populations. However, there are uncertainties about future funding for existing assisters, and contracts in some states have ended or are scheduled to end in early 2015. Several of the assister groups stressed that it would be important to recertify and continue to fund organizations that played a central role in assistance during the first open enrollment period given that they have already developed trusted relationships with individuals in the community and learned many lessons that they could employ in the future. Because assisters are also providing significant post-enrollment assistance to consumers, advocates noted that continued funding, training, and support for these individuals will be important to ensure that newly enrolled individuals are able to access care and renew coverage. While decisions about funding for assisters are not yet final, Marketplace staff in Connecticut indicated that they are trying to collect best practices from the most successful assisters to disseminate more broadly. Both state officials and advocates also noted that brokers will also likely continue to play an important role in helping individuals enroll into coverage. Looking ahead to the next open enrollment period, states are also planning for larger call center capacity and developing strategies that will allow them to adjust capacity to accommodate surges in enrollment.
Access and Utilization of Care
Increasing health insurance and health care literacy. Stakeholders in all four study states heavily stressed that one of the biggest priorities they are facing is helping newly covered individuals gain a better understanding of how health insurance works and how to access needed care. In Colorado, Medicaid and Marketplace officials are developing messaging and videos for consumers to educate them on how to use benefits as well as seasonal messaging related to health and wellness. Medicaid staff in Washington developed a First Timers Guide to Washington Apple Health, which instructs new enrollees on how to use their benefit cards and how a health plan works, and includes answers to some frequently asked questions, including how to find a primary care provider or make an appointment. In Connecticut, Marketplace officials are working with local foundations to develop some materials relating to health insurance literacy and launch a campaign encouraging people to “own their own health.” Assisters and brokers also have developed their own materials, including pamphlets and flyers in languages appropriate for the specific populations they serve and indicated that they continue to help consumers understand their plans, benefits, and notices they receive from Medicaid and the Marketplace.
“There’s a responsibility we have to get people to understand what insurance is; what it does; what it means. Stop the average person on the street, they don’t know what a co-pay is; they don’t know what a deductible is…So we’re going to be doing a lot of messaging around that because what we realize is we’re creating a whole new group of consumers who maybe don’t have a true understanding of what they’ve gotten or how to use it.” –Connecticut Marketplace Official
.
“The education around using your coverage, accessing care, getting assigned a primary care provider, how to work with your plan when it’s appropriate and how to work with us when it’s appropriate. That will continue…It is going to be an ongoing, continual process.” – Washington Medicaid Official
Supporting access to care for the newly insured. Stakeholders in the study states also noted that they are focused on ensuring that the gains in coverage lead to improvements in access to care. In Kentucky, early insights show that newly insured individuals have increased access to specialist care, prescription drugs, and behavioral health and substance abuse services. Kentucky also broadened Medicaid coverage for behavioral health and substance use disorder services, which stakeholders noted will be key services for many newly covered individuals. Medicaid officials in Colorado noted that they currently are heavily focused on provider recruitment for increase access for its growing base of enrollees. Moreover, some providers in the study states indicated that they are engaged in efforts to help get newly enrolled individuals connected to primary care services. For example, one community health center in Washington established a tracking system that allows have health center staff to schedule a primary care appointment for individuals as soon as they enroll. Using funding from internal reserves, the health center is also modifying assisters’ roles to allow them to call and conduct follow-up and home visits with enrollees about missed appointments to determine if there are other barriers such as lack of transportation that prevent them from obtaining preventive care. Similarly, an assister in Washington that serves at-risk youth recently received grant funding for a pilot project to help homeless youth enroll in coverage and select a health plan, and then provide staff to accompany individuals to their first doctor’s visit to help with care coordination. Further, the primary hospital system in Waterbury, Connecticut, which served as one of the largest assisters in the region, has implemented a system to coordinate care for newly enrolled beneficiaries (Box 4, next page).
Box 4: Coordinating Enrollment and Care Among Providers in Waterbury, Connecticut
The Waterbury hospital system serves the greater Waterbury area, which includes 19 towns in the eastern region of Connecticut and has among the highest uninsured rates in the state. During open enrollment, the hospital system built upon its previous experience serving the uninsured by enrolling uninsured patients in new health insurance coverage options and connecting them to care. In 2004, the hospital received grant funding to hire case managers to coordinate care for the uninsured, develop a shared database, and enroll eligible individuals into Medicaid and CHIP. Under the ACA, the hospital trained additional staff in two emergency rooms, a federally-qualified health center, and two hospital outpatient clinics to identify uninsured patients as they seek care and provide one-on-one enrollment assistance. Assisters also conducted outreach in homeless shelters and churches in the region.
During open enrollment, assisters within the Waterbury hospital system enrolled more than 1,000 people into coverage, and as patients enrolled in coverage, case managers provided education about using services and helped connect them to primary care. Now that open enrollment has ended, assisters continue to help uninsured patients enroll into Medicaid and CHIP and are collecting information on those who missed the Marketplace open enrollment period but may be eligible to purchase private coverage to do targeted outreach to them during the next open enrollment period
“It wasn’t just signing up people for insurance …we really say when we engage someone is; we want you to be able to get healthcare and get it in the right way.” –Assister in Waterbury Hospital, Connecticut
Maintaining safety net provider capacity. Safety net providers are facing significant changes as the ACA coverage expansions are implemented. As a result of the coverage expansion many of the patients they serve may gain coverage, which will increase their ability to obtain reimbursement for services. However, as patients gain coverage and access to a broader array of providers, safety net providers also indicated the need to adopt strategies to remain competitive and maintain their patient base, such as upgrading facilities and rebranding themselves. Moreover, with the increases in coverage, they face new demands to enhance their administrative capacity to bill to multiple insurers. Some stakeholders also noted concerns about potential decreases in grants and other sources of funding for safety net providers, since funders may believe there is a decreased need for these funding sources because of increased reimbursements stemming from coverage gains.
Conclusion
Although all states faced challenges during the first open enrollment for new Marketplace coverage, data show that as of April 2014 over 8 million individuals had enrolled in coverage through the Marketplaces and more than 6 million were added to the Medicaid program from before open-enrollment. While all states took different approaches to implementing the ACA, this report highlighted experiences in four states that achieved significant success in reaching and enrolling individuals into coverage, which provide important lessons learned and guidance for other states.
Each state implemented innovative approaches that contributed to this success; however, it is also clear that there was not one single strategy, but rather a combination of strategies related to marketing and branding, outreach and enrollment, consumer assistance, and systems and operations that supported successful coverage efforts. Underlying all of these strategies, strong leadership and close collaboration across stakeholders were also hallmarks for success. Finally, the ability to be nimble and make adjustments along the way as issues and problems were identified and recognized was an important lesson learned. From marketing to staffing call centers to reaching the uninsured to launching new enrollment systems, nearly all states hit some road blocks, but one of the keys to success in these states was the ability to quickly implement adjustments, fixes and workarounds.
Looking ahead, states have a number of consistent priorities for their current work and the next open enrollment period. Key priorities include a continued focus on enrollment and renewal, particularly related to education about ongoing Medicaid enrollment and special enrollment periods for the Marketplaces, maintaining coverage for those that have successfully enrolled, reaching those who remain uninsured, and maintaining an adequate network of consumer assistance. These states also are planning continued upgrades and enhancements to their enrollment systems and consumer assistance training programs to address outstanding limitations and gaps. However, one of the most significant priorities currently facing states is increasing consumer knowledge and understanding of health insurance and supporting access and utilization of care among the many individuals who have newly gained coverage.
This brief was prepared by Samantha Artiga, Jessica Stephens, and Robin Rudowitz from the Kaiser Family Foundation and Michael Perry from PerryUndem Research and Communication. The authors extend their deep appreciation to the state officials and other stakeholders for sharing their time and experiences to inform this project.
Appendix

| Appendix Table 1: Selected Data on Demographics and Health Coverage in Colorado, Connecticut, Kentucky and Washington | ||||||||
| COLORADO | CONNECTICUT | KENTUCKY | WASHINGTON | |||||
| POPULATION & DEMOGRAPHICS | ||||||||
| Total Nonelderly Population (2011-12)1 | 4.5 million | 3.0 million | 3.7 million | 6.0 million | ||||
| Distribution of Nonelderly Population by Race/Ethnicity (2010-11)1 | ||||||||
| White | 69% | 69% | 84% | 68% | ||||
| All People of Color | 31% | 31% | 16% | 32% | ||||
| Black | 4% | 10% | 8% | 4% | ||||
| Hispanic | 21% | 14% | 4% | 4% | ||||
| Asian | 3% | 6% | 1% | 10% | ||||
| Other Race/Ethnicity | 2% | 1% | 2% | 6% | ||||
| Nonelderly Non-Citizens (2010-11)1 | 9% | 13% | 5% | 14% | ||||
| Nonelderly with Limited English Proficiency, 20112 | 6% | 8% | 2% | 8% | ||||
| Share of Total Population Living in a Non-Metropolitan Area1 | Data Not Available | 4% | 43% | 6% | ||||
| Share of Total Population Living in Poverty, (2011-12)1 | 16% | 21% | 19% | 19% | ||||
| Median Annual Household Income (2009-11)3 | $59,803 | $67,165 | $42,331 | $59,370 | ||||
| UNINSURED | ||||||||
| Uninsured Rate Among Nonelderly (2011-12)1 | 17% | 15% | 24% | 17% | ||||
| Nonelderly Uninsured (2012-13)4 | 737,000 | 286,000 | 647,000 | 948,000 | ||||
| Share Eligible for Medicaid4 | 46% | 38% | 54% | 47% | ||||
| Share Eligible for Tax Credit Subsidies4 | 22% | 25% | 22% | 23% | ||||
| Share Ineligible for Financial Assistance4 | 33% | 38% | 23% | 23% | ||||
| MEDICAID & CHIP | ||||||||
| Medicaid/CHIP Eligibility Limits as a Share of the FPL5 | 2013 | 2014 | 2013 | 2014 | 2013 | 2014 | 2013 | 2014 |
| Children | 250% | 265% | 300% | 323% | 200% | 218% | 300% | 317% |
| Pregnant Women | 250% | 265% | 250% | 263% | 185% | 200% | 185% | 198% |
| Parents (in a family of three) | 106% | 138% | 191% | 201% | 57% | 138% | 71%6 | 138% |
| Childless Adults (for an individual) | 20% | 138% | 70% | 201% | 0% | 138% | 0%6 | 138% |
| Change in Medicaid and CHIP Enrollment, Summer 2013 to April 20147 | 263,452 | Data Not Available | 265,091 | 364,724 | ||||
| 34% | 32% | 33% | ||||||
| MARKETPLACE | ||||||||
| Marketplace Name | Connect for Health CO | Access Health CT | Kynect | WA Healthplanfinder | ||||
| Portal Languages | English and Spanish | English | English and Spanish | English and Spanish | ||||
| SHOP Marketplace in 2014? | Yes | Yes | Yes | In 2 counties | ||||
| Number of Insurers Participating in Individual Marketplace8 | 10 | 3 | 3 | 8 | ||||
| Number of Individuals Who Selected a Plan, as of April 20149 | 125,402 | 79,192 | 82,747 | 163,207 | ||||
| Marketplace Enrollees as Share of Potential Marketplace Population, as of April 201410 | 25% | 37% | 27% | 32% | ||||
| 1KCMU/Urban Institute estimates based on 2011-2012 ASEC Supplements to the CPS.2 KCMU/Urban Institute analysis of 2010 American Community Survey.3U.S. Census Bureau, Current Population Survey, 2009 to 2011 Annual Social and Economic Supplements.4 Kaiser Family Foundation analysis based on January 2014 Medicaid eligibility levels and 2012-13 CPS.5 Eligibility limits for parents and other adults include income disregards for 2013 and the standard 5 percentage point of the FPL disregard for 2014. Based on a national survey conducted by the KCMU and the Georgetown University Center for Children and Families, 2013 and Based on data from the Centers for Medicare and Medicaid Services (CMS), State Medicaid and CHIP Income Eligibility Standards Effective April 1, 2014.2014.6 In Washington, prior to the ACA, adults with income up to 133% FPL were eligible for more limited coverage under the state’s’ Basic Health waiver.7CMS, Medicaid & CHIP Monthly Applications, Eligibility Determinations, and Enrollment Reports: March 2014 (Updated) and April 2014; accessed June 4, 2014.8Kaiser Family Foundation analysis of insurance company rate filings.9KCMU analysis of Health Insurance Marketplace: Enrollment Reports. Office of the Assistant Secretary for Planning and Evaluation (ASPE), Department of Health and Human Services (HHS); November 2013 – April 2014.10Based on data from Health Insurance Marketplace: March Enrollment Report, October 1, 2013 – April 19, 2014, Office of the Assistant Secretary for Planning and Evaluation (ASPE), Department of Health and Human Services (HHS); May 1, 2014 and State-by-State Estimates of the Number of People Eligible for Premium Tax Credits Under the Affordable Care Act, Kaiser Family Foundation, November 5, 2013. | ||||||||
Endnotes
- KCMU analysis of Health Insurance Marketplace: Enrollment Reports. Office of the Assistant Secretary for Planning and Evaluation (ASPE), Department of Health and Human Services (HHS); November 2013 – April 2014 ↩︎
- CMS, Medicaid & CHIP Monthly Applications, Eligibility Determinations, and Enrollment Reports: March 2014 (Updated) and April 2014; accessed June 4, 2014. ↩︎
- CMS, Medicaid Moving Forward. State Medicaid and CHIP Eligibility Standards as of April 1, 2014. ↩︎
- In addition, Connecticut, Colorado, and Kentucky established small business Marketplaces (SHOP) for businesses with 50 or fewer employees to search for plans for their employees. As of 2014, the Washington SHOP Marketplace was only available to individuals in small businesses in two counties. ↩︎
- For more information, see: KFF, Helping Hands: A Look at State Consumer Assistance Programs Under the Affordable Care Act. September 2013. ↩︎