Talking About Medicare: Your Guide to Understanding the Program, 2012
Welcome
Medicare is the federal health insurance program for people 65 and older and for some younger adults with permanent disabilities and medical conditions. Prior to 1965, the year in which the Medicare program was established, about half of all seniors lacked health insurance. Today, virtually all people 65 and older have coverage under Medicare, and are eligible for this coverage without regard to their income or medical history. Medicare currently provides health insurance coverage for nearly 50 million Americans.
Even with Medicare, people face many choices when they enroll in the program, and each year thereafter. “Talking About Medicare” is intended to provide answers to some basic questions related to Medicare coverage, as well as information to help you make decisions on a range of topics related to enrollment, plan choices and prescription drug coverage.
The Additional Resources section of this guide provides a state-by-state list of key agencies that can answer specific questions about Medicare, Medicaid, supplemental health insurance, the Medicare prescription drug benefit, and long-term care. We hope this guide will be a useful tool for you.
The Kaiser Family Foundation appreciates the significant contributions of the Medicare Rights Center to the 2012 update of Talking About Medicare.
Report: Medicare At A Glance
Download a printable pdf version of this section.
Download a printable pdf version of the entire guide.
Medicare is the federal health insurance program for Americans age 65 and older and for younger adults with permanent disabilities, End-Stage Renal Disease (ESRD), or Amyotrophic Lateral Sclerosis (ALS). Knowing the basics about Medicare can help you make good decisions about your health coverage and care.
- Are you Eligible for Medicare?
- What Medicare Covers
- What Medicare Does Not Cover
- Original Medicare or Medicare Advantage?
- Insurance to Supplement Original Medicare
- How and When to Enroll in Medicare
Are you Eligible for Medicare?
If you are age 65 or older, you qualify for Medicare if:
- You collect or qualify to collect Social Security or Railroad Retirement benefits OR
- You are a current U.S. resident and either a U.S. citizen or a permanent U.S. resident having lived in the United States for 5 continuous years.
If you are under age 65, you qualify for Medicare if:
- You have been getting Social Security Disability Insurance (SSDI) or Railroad Disability Annuity checks for at least 24 months,
- You have Amyotrophic Lateral Sclerosis (ALS) and receive Social Security Disability Insurance (SSDI) or Railroad Disability Annuity checks, or
- You have end-stage renal disease (ESRD) and you, your spouse, or your parent have paid Medicare taxes for a sufficient period of time. ESRD means your kidneys do not work properly and you need dialysis or a kidney transplant to live.
What Medicare Covers
The Medicare program is comprised of four parts – Part A, Part B, Part C (also known as Medicare Advantage), and Part D. Together, these four parts provide coverage for basic medical services and prescription drugs.
Part A (Hospital Insurance): Part A covers inpatient hospital care, some skilled nursing facility stays, home health care, and hospice care. If you or your spouse have worked for at least 40 quarters (10 years) and paid Medicare payroll taxes, you qualify for Part A coverage, and you don’t have to pay a monthly premium for it. This is referred to as “premium-free Part A.”
If you are not entitled to premium-free Medicare Part A because you do not have enough working quarters, you may still qualify for Part A but you will have to pay a monthly premium. In 2012, the Part A premium is $248 per month if you have worked between 30 and 39 quarters, and $451 per month if you worked fewer than 30 quarters.
For all people with Medicare, there is a charge for most health care services in the form of deductibles and coinsurance or copayments.
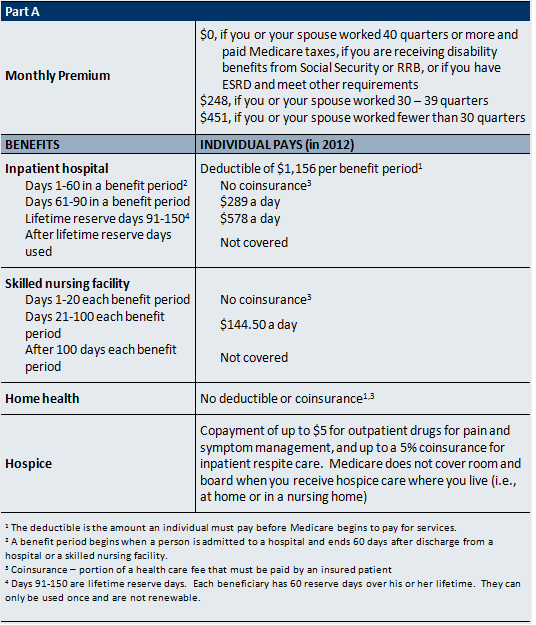
Source: Medicare & You. Centers for Medicare and Medicaid (CMS). 2012Available at http://www.medicare.gov/Publications/Pubs/pdf/10050.pdf
Part B (Medical Insurance): Part B, or the Supplementary Medical Insurance (SMI) program, helps pay for physician services, outpatient hospital care, and some home health visits not covered under Part A. It also covers laboratory and diagnostic tests, such as X-rays and blood work; durable medical equipment, such as wheelchairs and walkers; certain preventive services and screening tests, such as mammograms and prostate cancer screenings; outpatient physical, speech and occupational therapy; outpatient mental health care; and ambulance services.
As part of the 2010 health reform law, you pay no coinsurance or deductible for many preventive services under Part B (if your doctor accepts assignment). For instance, Medicare pays in full for a one-time “Welcome to Medicare” preventive visit in your first year of enrolling in Part B, and an “Annual Wellness Visit” after your first year in Part B. During the “Welcome to Medicare” visit, your doctor will review your health and provide information and counseling regarding preventive care you can receive and referrals for additional services. The “Annual Wellness Visit” is similar but takes place on a yearly basis. During your annual wellness visit, your doctor will create or update a preventive care screening plan for you for the next 5 to 10 years.
All people with Medicare pay a monthly premium for Part B. Most people who pay a Part B premium have it automatically deducted from their Social Security check. If your income is limited, you may qualify for programs that will pay the Part B premium on your behalf. For more information, see the Medicare and People with Low Incomes section.
The standard monthly Part B premium in 2012 is $99.90. Some people on Medicare with higher annual incomes (more than $85,000/individual; $170,000/couple) pay a higher monthly Part B premium, ranging from $139.90 to $319.70 per month in 2012, depending on their income.
Part B also has an annual deductible of $140 in 2012—that is, you must pay $140 out-of-pocket before Medicare begins paying. After you meet the deductible, most Part B services require a 20 percent coinsurance; this means you pay 20 percent of the cost of the service. If a doctor is a “participating provider” then the most he or she can ever charge you is 20 percent of the Medicare-approved amount for a service. This is called “accepting assignment.”
Some doctors do not “accept assignment” – that is, they choose not to accept the Medicare-approved amount as payment for services and procedures. These doctors are called “non-participating providers.” If a doctor does not accept the Medicare-approved amount, he or she can charge you both a 20 percent coinsurance, as well as a “limiting charge” that can be up to 15 percent above the Medicare-approved amount for non-participating providers (although some states have stricter limiting charges).
A limited number of doctors do not accept Medicare at all. These doctors face no restrictions on the amounts they can charge their Medicare patients, as long as the patient signs an agreement saying they will pay for the full cost of the services.
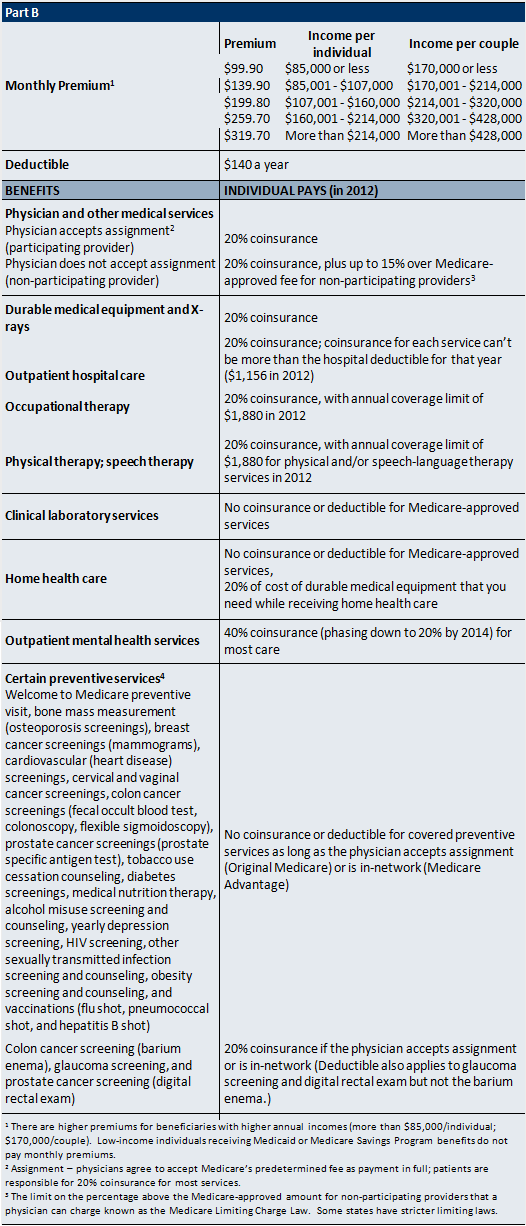
4For a full list of Medicare-covered preventative services, conditions of coverage, and charges,see the Medicare and You guide published by the Centers for Medicare and Medicaid (CMS). 2012Available at http://www.medicare.gov/Publications/Pubs/pdf/10050.pdf
Part C (Medicare Advantage): Part C allows beneficiaries to enroll in a private insurance plan, called a Medicare Advantage plan. Medicare Advantage plans are managed care plans, such as Health Maintenance Organizations (HMOs) or Preferred Provider Organizations (PPOs). Medicare Advantage plans must cover all Part A and B services and usually include Part D (prescription drug coverage) benefits in the same plan. These plans sometimes cover additional benefits not covered by traditional Medicare, such as routine vision and dental care. All plans have an annual limit on your out-of-pocket costs for Part A and B services, and once you reach that limit, you pay nothing for covered services for the rest of the calendar year. The out-of-pocket limit can be high but may help protect you if you need a lot of health care or need expensive treatment. Out-of-pocket costs include deductibles, copayments and coinsurance.Although Medicare Advantage plans must cover Part A and B services, they can have different rules, costs and restrictions. Some plans have higher cost-sharing requirements than Original Medicare for some services, and most plans apply restrictions that limit your choices of doctors or hospitals. For more details on Medicare Advantage, see the Medicare Advantage Plans section.
Part D (prescription drug coverage): In 2006, Medicare began offering outpatient prescription drug coverage under Medicare Part D. Medicare drug coverage is optional for most people with Medicare and is offered only through Medicare private plans. If you have Original Medicare and want Part D drug coverage, you can get a stand-alone prescription drug plan (PDP). People who want a Medicare Advantage plan and drug coverage must generally get it through one plan called a Medicare Advantage prescription drug plan (MA-PD).
There is a monthly premium for Part D. Premiums vary widely among plans, as do the drugs that are covered and the amounts charged for prescriptions. The standard Part D benefit has a deductible, which in 2012 can be no more than $320, and 25 percent coinsurance on covered drugs up to an initial coverage limit. This is followed by a coverage gap, during which enrollees are responsible for a larger share of their total drug costs than during the initial coverage period, until they reach the catastrophic coverage limit. Thereafter, enrollees have low costs for their drugs. For people on Medicare with limited incomes and resources, financial assistance is available to reduce or eliminate premiums, deductibles, and co-pays. For more details on Part D, see the Medicare and Prescription Drug Coverage section.

What Medicare Does Not Cover
Medicare does not cover all health care services. For example, Medicare pays for a limited amount of long-term care services; it does not pay for home or community-based care, assisted living facilities, or nursing homes. Medicare also does not cover regular eye exams, most eyeglasses, hearing aids, routine dental care, or most care provided outside the United States.
Original Medicare or Medicare Advantage?
There are two ways to get Medicare health coverage.
- Original Medicare: This is the traditional fee-for-service program provided through the federal government. Original Medicare (also referred to as traditional Medicare) includes Part A (Hospital Insurance) and/or Part B (Medical Insurance) coverage. Beneficiaries with Original Medicare have the option of enrolling in a Part D (Prescription Drug) plan from a private insurance company, and may also enroll in a Medicare Supplement Insurance (Medigap) Plan from a private insurance company.
- Medicare Advantage Plan: A Medicare Advantage plan is a private insurance plan that combines Part A and Part B. People who want a Medicare Advantage plan and Part D drug coverage must generally get both as part of the same plan (Medicare Advantage Drug Plan).
People on Medicare throughout the country have the option to get their Medicare benefits under the fee-for-service program (Original Medicare) or through a Medicare Advantage plan. Medicare Advantage plans, such as Health Maintenance Organizations (HMOs) and Preferred Provider Organizations (PPOs), are offered by private insurers that receive payments from the government to provide Medicare benefits to enrollees. The majority of elderly and disabled beneficiaries today are covered under Original Medicare. One in four people with Medicare is enrolled in a Medicare Advantage plan.
An important question facing people on Medicare is whether to enroll in a Medicare Advantage plan, and if so, which plan. There are many factors to consider when choosing between Original Medicare and a Medicare Advantage plan. Some beneficiaries prefer Original Medicare because it allows them the broadest possible access to medical providers, it does not require them to receive prior authorization for services, it allows them access to any provider who accepts Medicare when they travel, and/or it works well with their supplemental plan (such as employer-sponsored retiree health plan or Medigap plan).
Others prefer Medicare Advantage plans because they are often cheaper than purchasing a supplemental plan to wrap around Original Medicare (Medigap). People might also be attracted to the lower cost sharing under some Medicare Advantage plans, the limit on out-of-pocket spending Medicare Advantage plans must have, the additional services covered by some Medicare Advantage plans that are not covered by Original Medicare, or because they may have had a positive experience with a similar HMO or PPO offered by the same company before becoming eligible for Medicare.
See the Medicare Advantage Plans section for additional information.
Insurance to Supplement Original Medicare
To help cover gaps in Medicare coverage and cost sharing such as deductibles and coinsurance, most Medicare beneficiaries supplement their coverage in some way. There are several types of supplemental insurance that work with Original Medicare. Some options include insurance from a former employer, supplemental insurance policies such as Medigap, or programs for people with limited incomes.
If you choose Original Medicare, you may be able to get supplemental insurance from a former employer or union (retiree coverage). About one in three Medicare beneficiaries have supplemental coverage from their former or current employer. If you are not yet on Medicare, find out what employee benefits you may be eligible for when you go on Medicare, and ask how these benefits coordinate with Medicare.
If you do not get retiree coverage and choose Original Medicare, you can buy Medicare supplemental insurance directly from an insurance company. These are called “Medigap” plans, and they only work with Original Medicare. About one in five Medicare beneficiaries has a Medigap policy. For more information on Medigap, see the Medicare Supplemental Insurance section.
Depending on your income and savings, you may also qualify for supplemental coverage through the Medicaid program or a Medicare Savings Program. Twenty percent of Medicare beneficiaries are dually eligible for Medicare and Medicaid. For more information on programs for low-income Medicare beneficiaries, see the Medicare and People with Low Incomes section.
How and When to Enroll in Medicare
Qualifying for Medicare because you are over age 65. In general, if you are receiving Social Security or Railroad Retirement Board (RRB) retirement benefits when you turn 65, you will automatically be enrolled in Part A and Part B. If you are eligible for, but not receiving Social Security or RRB benefits yet (for example, if you are still working), you will NOT be automatically enrolled; instead, you will need to apply at a Social Security office during your Initial Enrollment Period (the seven-month period that includes the three months before you turn 65, the month you turn 65, and the three months after you turn 65).
If you plan to enroll in Part B, it is very important that you do so when you first qualify to avoid having to pay a late enrollment penalty. There are limited circumstances when you can delay enrolling in Part B without having to pay a penalty, for example, if you have a group health plan from a current employer, as discussed in the “Employer Coverage and Medicare” section below. Contact your local Social Security office to find out whether you need to enroll in Part B when you first qualify for it. The contact information to make an appointment with your local Social Security office is available in the Additional Resources section of this guide.
Qualifying for Medicare due to disability. If you are under age 65 and have a permanent disability or medical condition, you will automatically get Medicare Parts A and B after you have received disability benefits from Social Security or the Railroad Retirement Board (RRB) for 24 months. If you have Amyotrophic Lateral Sclerosis (ALS), you will automatically get Medicare Parts A and B when your disability benefits begin. If you have End-Stage Renal Disease (ESRD), you need to call Social Security for more information about your Medicare eligibility, and to sign up for Part A and/or Part B.
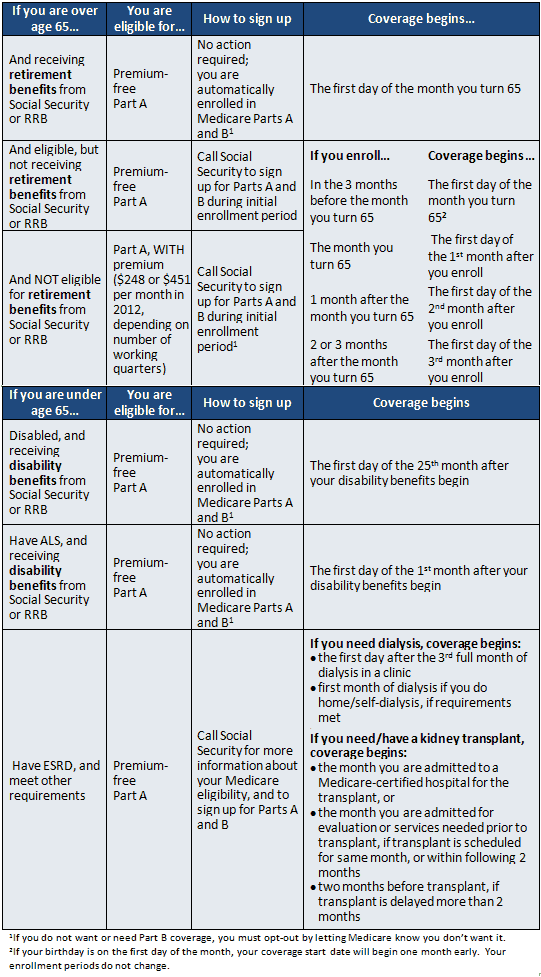
See the sections on Medicare Advantage Plans, Medicare and Prescription Drug Coverage, and Medicare Supplemental Insurance for more information on how to apply for each.
If you do not enroll in Medicare Parts A, B, or D during your Initial Enrollment Period, you can do so later on, but you may have to pay a penalty for late enrollment. More information on late enrollment penalties is below.
The official Medicare website has a Medicare Eligibility tool that may answer any questions you have about eligibility and/or enrollment; for more information, visit http://www.medicare.gov/medicareeligibility/home.asp .
Employer Coverage and Medicare. Some people decide not to take Part B when they first qualify for it because they have insurance from their current employer or their spouse’s current employer. Before deciding whether or not to enroll in Part B, contact your employer plan and the Social Security Administration to find out how your employer plan will work with Medicare. Ask whether your insurance is primary or secondary to Medicare. Primary coverage pays first for your health care costs, and secondary insurance pays some or all of the remaining costs.
You should almost always take Part B when you first qualify if your current employer coverage is secondary to Medicare. If your current employer coverage is primary to Medicare, you may choose to delay enrolling in Part B to avoid duplicating coverage and paying monthly premiums for two forms of insurance.
If you have health coverage from your current employer or your spouse’s current employer when you turn 65, you have a Special Enrollment Period to enroll in Medicare without penalty any time while you are still working and for up to eight months after your employer coverage ends or becomes retiree coverage, whichever comes first. Your Medicare coverage will begin the month after you enroll.
You should check with your local Social Security office or your employer before declining Part B to be sure that Medicare is not your primary insurance and that you will not have to pay a penalty for late enrollment. Information on contacting your local Social Security office is available in the Additional Resources section of this guide.
Retiree health coverage or COBRA and Medicare. If you have retiree health coverage, or continuation health care coverage from a former employer (COBRA), and you plan to enroll in Medicare Parts A and B, you should do so during your Initial Enrollment Period. Retiree health coverage and COBRA do not count as current employer coverage, so you must enroll in Part B when you first qualify in order to avoid having to pay a premium penalty for late enrollment and/or gaps in coverage. If you already have COBRA coverage, your COBRA coverage may end when you are eligible for Medicare. More information on Medicare and COBRA is available at http://www.ssa.gov/disabilityresearch/wi/medicare.htm#cobra.
If you have employer coverage, you may also wonder if you should enroll in Part D when you first qualify for Medicare. If you or your spouse have “creditable drug coverage” through a current or former employer, you can delay enrollment in the Medicare drug benefit without penalty. When drug coverage is “creditable,” that means it is at least as good as the standard Medicare Part D benefit. You should check with your employer to see if your drug coverage is creditable. Your employer should also notify you in writing each year whether your employee or retiree drug coverage is creditable. You may avoid paying a late enrollment penalty for Part D if you enroll in Part D within 63 days of the time that your employer-sponsored creditable drug coverage ends.
Late Enrollment Penalties. If you do not enroll in Medicare Parts B or D during your Initial Enrollment Period, you can do so later on, but you may have to pay a penalty for late enrollment (the same is true for Part A, although most people qualify for premium-free Part A). However, if you are eligible for a Special Enrollment Period, then you may not have to pay late enrollment penalties. More information on Special Enrollment Periods is provided below.
- Part B late enrollment penalty. Once your Initial Enrollment Period has passed, you can only enroll in Part B during the “General Enrollment Period” (from January 1 to March 31 each year, with coverage beginning on July 1). The Part B late enrollment penalty is a 10 percent increase in your Part B premium for each full 12-month period that your enrollment was delayed; this penalty is permanent, so you will have to pay the penalty for as long as you have Medicare. For example, if you delay signing up for Part B for 30 months after your Initial Enrollment Period ends, (since 30 months only includes 2 full 12-month periods) your Part B premium penalty would be 20 percent of the Part B premium.
- Part D late enrollment penalty. Once your Initial Enrollment Period has passed, you can generally only enroll in Part D during the “Fall Open Enrollment Period” (from October 15 to December 7 each year, with coverage beginning on January 1). The Part D late enrollment penalty is 1 percent of the national average premium for each month enrollment was delayed. If you qualify for Extra Help, the program that helps pay for prescription drug costs for people with limited income and resources, you can enroll in Part D right away and will not need to pay a penalty for late enrollment. See the Medicare and Prescription Drug Coverage section for more information on the Part D late enrollment penalty, and an example of how it is applied. See the discussion of “Extra Help with Prescription Drug Costs” in the “Medicare and People with Low Incomes” section.
Enrollment Period Summary
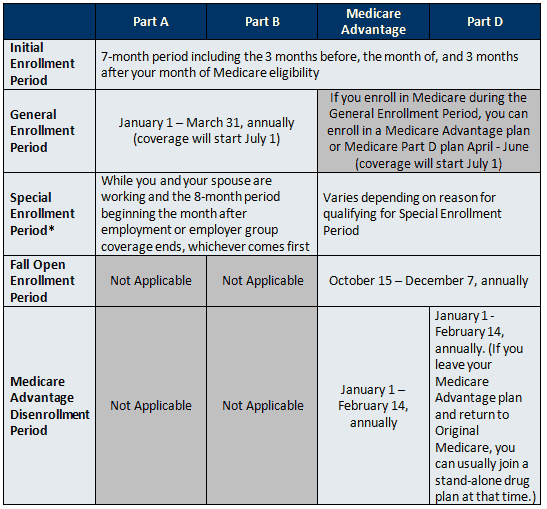
There are several different ways to qualify for a Special Enrollment Period to enroll in or switch Medicare Advantage or Part D plans. You may qualify for a Special Enrollment Period if…
- You move;
- You have Medicaid or Extra Help;
- You lose Medicaid or Extra Help;
- You just moved into, currently live in, or just moved out of an institution (including a skilled nursing facility or long-term care hospital);
- You lose other drug coverage that is creditable;
- You have a chance to get other coverage from your employer or a union; or
- Your plan leaves Medicare
When you can make changes and what changes you can make depend on the reason you qualify for the Special Enrollment Period. For more information on Special Enrollment Periods, see the “Understanding Medicare Enrollment Periods” tip sheet at Medicare.gov, available here: www.medicare.gov/Publications/Pubs/pdf/11219.pdf
Report: Medicare And Prescription Drug Coverage
Download a printable pdf version of this section.
Download a printable pdf version of the entire guide.
- Basics of the Medicare Prescription Drug Benefit
- Is the Medicare Drug Benefit Right for You?
- Medicare Drug Plan Options
- Choosing a Medicare Drug Plan
- Enrolling in a Medicare Drug Plan
- Switching Medicare Drug Plans
- Getting Help With Medicare Drug Costs for People With Limited Incomes
Many people on Medicare rely on prescription drugs to manage their health conditions. This section offers general information about the Medicare drug benefit (Medicare Part D), advice for determining if the Medicare drug benefit is right for you, key considerations for selecting a Medicare drug plan that best meets your needs, and information about extra financial assistance with drug costs available for those with limited incomes.
The federal government helps to cover the cost of the Medicare prescription drug benefit; however, private companies administer the benefit on behalf of the government. Therefore, to get the Medicare prescription drug benefit, you need to enroll in one of these plans.
There are two types of plans offering Medicare drug coverage:
- A Medicare stand-alone prescription drug plan (PDP) that covers only prescription drugs. If you would like to get coverage of your Medicare health benefits through Original Medicare, then you can enroll in a stand-alone prescription drug plan to add the drug benefit to your health coverage.
- A Medicare Advantage plan, like a Medicare HMO or PPO, that offers prescription drug coverage (MA-PD plan). If you enroll in a Medicare Advantage plan, you will usually receive all Medicare benefits through your Medicare Advantage plan, including health care coverage and prescription drugs if covered by the plan.
You can sign up for the drug benefit during your Initial Enrollment Period, which is a seven-month period including the three months before you become eligible for Medicare, the month you become eligible for Medicare and the three months after you become eligible for Medicare. You can also sign up (or switch plans) between October 15 and December 7 of each year, with drug coverage effective January 1 of the following year. For a discussion of these enrollment periods, as well as Special Enrollment Periods, see the Medicare At a Glance section, under How and When to Enroll in Medicare.
Enrollment in the Medicare drug benefit is voluntary. However, if you decide not to sign up, it is important to be aware of the potential consequences. If you do decide to enroll later, you may need to pay late enrollment penalty and will only be able to enroll during certain times.
Basics of the Medicare Prescription Drug Benefit
All people with Medicare, regardless of their medical history or income, have access to plans that offer drug coverage. The enrollment period runs from October 15 to December 7, and coverage begins January 1 of the following year.
The Medicare drug benefit is designed to reduce drug costs and protect against catastrophic drug expenses, but it is not free. When you get Medicare prescription drug coverage, you pay part of the costs and Medicare pays part of the costs. Your costs include premiums, deductibles, and copayments and/or coinsurance, and will vary depending on which plan you choose. However, all plans must, at a minimum, provide you with a standard level of coverage, as described below. People with low incomes may qualify for assistance with these costs; see Extra Help with Prescription Drug Costs in the “Medicare and People with Low Incomes” section.
Typically, you will pay a monthly premium for your drug coverage. The cost of the monthly premium varies greatly depending on the plan you choose, but the national average premium is projected to be $31.08 per month in 2012. If your annual income is above $85,000 for an individual or $170,000 for a couple, you will need to pay a higher Part D premium that depends on your income.
There are four possible coverage periods you may encounter within a given year, depending on the design of the Part D plan you enroll in and your total drug costs. The benefit structure outlined below is the standard benefit design.
- The Deductible: The deductible is the amount you must pay before your drug plan will start paying for your drugs. In 2012, the deductible cannot be more than $320 in any plan. Some plans charge less or no deductible.
- Initial Coverage Period: During this period, you pay a portion of your drug costs and your plan pays a portion of your drug costs. In the standard benefit, you pay 25 percent and the plan pays 75 percent. However, most plans do not follow the standard benefit design. You should check with your plan to see what your coinsurance or copayments will be; copayments typically differ for generic and brand-name drugs. In 2012, the initial coverage period ends when what you and your plan have spent in total drug costs equals $2,930.
- Coverage Gap: Once you and your plan have spent $2,930 in total drug costs, a coverage gap begins(sometimes referred to as the “doughnut hole”). During the coverage gap, you are responsible for a larger share of the costs of your drugs. In 2012, you receive a 50 percent discount for brand-name drugs during the coverage gap and a 14 percent discount for generic drugs in the standard plan. The coverage gap will be completely phased out in 2020, when you will pay no more than 25 percent of the cost of your brand or generic drugs.
- Catastrophic Coverage: After you have spent $4,700 in total out-of-pocket costs in 2012 (including the deductible and costs in the initial coverage period and the coverage gap), you will reach catastrophic coverage. Under catastrophic coverage, you pay either 5 percent of the cost of the drug or $6.50 for brand-name drugs and $2.60 for generics, whichever is greater. The $4,700 that you have paid out-of-pocket includes amounts paid by some others including family members, most charities, State Pharmaceutical Assistance Programs (SPAPs), AIDS assistance programs, and the Indian Health Service. The 50 percent discount for brand-name drugs in the coverage gap is also included in the $4,700 total that triggers catastrophic coverage. The total amount, however, does not include your monthly premium, the 14 percent discount on generic drugs, or any amount your plan paid for your drugs.
Although these are costs under the standard benefit design, most Medicare prescription drug plans offer a different benefit design. Most plans do not have a $320 deductible and do not use a 25 percent coinsurance for each prescription filled. Instead, most plans impose different drug copayment amounts, depending on the medication. Typically, they have multiple tiers of covered drugs, with the lowest copayments for generic drugs and preferred brand-name drugs. Most Medicare drug plans do not offer benefits in the coverage gap beyond what the law requires. For tips on how to manage your spending in the coverage gap, see the Choosing a Medicare Drug Plan section.
Is the Medicare Drug Benefit Right for You?
The first thing to consider is whether you currently have drug coverage. If you do not have coverage, the Medicare drug benefit may help to lower your out-of-pocket drug spending and protect you from facing very high drug expenses. Even if you do not use a lot of medications now, having the drug benefit may help protect you if your health care needs change. For many people, the coverage helps alleviate the burden of drug costs, because Medicare subsidizes the cost. If you decide not to sign up, it is also important to be aware of the potential consequences of not doing so. If you do decide to enroll later, you may need to pay late enrollment penalty and will only be able to enroll during certain times.
Assessing Your Current Source of Drug Coverage (if you have one)
The following is a list of scenarios that may describe your current drug coverage situation and help you decide whether to sign up for a Medicare drug plan.
Do you get your drug coverage from a former or current employer or union?
In general, benefits offered by employers are more generous than the standard Medicare drug benefit. You should have received a letter from your former or current employer letting you know whether your coverage is “creditable,” which means it is at least as good as the standard Medicare prescription drug benefit. Save this letter. If you did not receive this information, contact your employer.
If your drug plan is creditable, you can either keep your employer health plan or enroll in a Medicare prescription drug plan; in some instances you may be able to do both. Compare the benefits and out-of-pocket costs under your employer plan with the benefits offered by Medicare drug plans in your area so you can be sure which plan is best for you. You should check with your employer if you are thinking about enrolling in a Medicare drug plan. Some employer plans work with Part D but some do not. If you join a Medicare drug plan that does not work with your employer plan, you and your dependents who are covered by the same plan may lose your employer health and drug coverage. If you drop your employer coverage, you may not be able to get your employer coverage back.
If your employer plan does not meet the “creditable coverage” standard, you may want to consider enrolling in a Medicare drug plan. If you lack “creditable coverage” and do not sign up for a Medicare drug plan when you are first eligible, you will likely have to pay a late enrollment penalty if you sign up later on. The late enrollment penalty is 1 percent of the national average premium for each month you delay enrollment and do not have creditable drug coverage. More information on the late enrollment penalty is below. Also, you can only enroll in a Medicare drug plan during certain times of the year.
If your creditable coverage ends, or if you decide later that you want to drop your employer or retiree coverage, you can enroll in a Medicare prescription drug plan at that time. You will not have to pay a late enrollment penalty as long as you join a Medicare drug plan within 63 days after your employer coverage ends (and as long as that coverage is creditable).
These are the things to know about employer coverage that are important to consider when making your choice about the Medicare drug benefit:
- Employer plans usually include other benefits besides drug coverage, so you should consider not only the drug coverage, but all health care benefits offered by the employer plan. Enrolling in a Medicare drug plan could cause you to lose all your retiree health care coverage.
- Dropping employer coverage could affect coverage for your dependents; talk to your employer about how a change in your status may affect your dependents before making any changes to your coverage.
- If you decide to drop your employer coverage, you will probably not be able to rejoin the plan in the future if you change your mind, so make sure you think through your decision.
- A final consideration is whether you may qualify for additional help with Medicare drug plan expenses that is available to people with limited incomes and resources. This help can be quite valuable, but is not typically available to you if you keep your employer coverage.
Are you currently enrolled in a Medicare Advantage (MA) Plan?
Most Medicare Advantage plans provide prescription drug coverage. If you choose to be covered under a Medicare Advantage plan rather than the Original Medicare program, check to be sure the plan offers drug coverage.If you are dissatisfied with your Medicare Advantage Prescription Drug (MA-PD) plan and want to switch to another Medicare Advantage plan with prescription drug coverage, you can usually only do so once a year during the annual open enrollment period from October 15 through December 7. See the Medicare Advantage Plans section for more information. If you decide to disenroll from your Medicare Advantage plan and opt for health coverage through Original Medicare, you will most likely need to sign up for a stand-alone prescription drug plan if you would still like drug coverage.
If you choose Original Medicare with a stand-alone drug plan, you will typically pay both a monthly Part B premium and a premium for your Part D plan (unless you qualify for Medicaid or other programs that help low-income beneficiaries; see Extra Help with Prescription Drug Costs in the “Medicare and People with Low Incomes” section for more information).
Does Medicaid help pay for your medical care?
If you have both Medicare and Medicaid, your drug coverage is provided by a Medicare prescription drug plan, and you are automatically eligible for Extra Help (also known as the Low-Income Subsidy program). Extra Help is a federal program that helps pay some or most of your drug costs, including premiums, deductibles, and copayments. If you qualify for Extra Help, you will be automatically enrolled in a Medicare prescription drug plan if you don’t choose one yourself. If you do not have Medicaid, but have a limited income, you might still be eligible for Extra Help. For more information on extra help paying for a prescription drug plan, see Extra Help with Prescription Drug Costs in the “Medicare and People with Low Incomes” section.
Understanding the Late Enrollment Penalty
If you do not sign up for a Medicare drug plan when you are first eligible and do not have “creditable” prescription drug coverage from another source (such as an employer plan or the Veterans’ Administration) for 63 days or more after you first qualified for benefits, you will most likely be charged a premium penalty for late enrollment. The late enrollment penalty is based on the number of months you delay enrollment after you are first eligible to sign up for a Medicare drug plan.
The premium penalty will increase the cost of your prescription drug coverage for as long as you are enrolled in a Medicare drug plan. The penalty is 1 percent of the national average premium multiplied by the number of months you delayed enrollment without creditable coverage. The national average Medicare drug plan premium for 2012 is $31.08. If you delayed enrollment for 9 months, your penalty this year would be $31.08 × 1% × 9, or $2.80. You would pay this each month in addition to the monthly premium. Since the national average premium increases each year, your penalty would also increase each year.
The premium penalty is permanent. Individuals subject to the penalty would pay a higher premium each month they are enrolled in a Part D plan. People who receive Extra Help do not pay the premium penalty.
Medicare Drug Plan Options
There are two types of Medicare drug plans you can buy, and you should consider which type of plan is best for you before making a decision.
Medicare Prescription Drug Plan (PDP)
The first type of plan, called a Medicare stand-alone prescription drug plan (PDP), covers prescription drugs only. These plans, offered by private insurance companies, are generally best for people who need drug coverage but prefer to get their other health benefits, such as coverage for hospital stays and physician visits, from Original Medicare. There are many prescription drug plans offered in most states, but your options depend on which drug plans serve the area where you live. With a PDP, you receive prescription drug coverage directly from the private plan, and get coverage for your hospital and outpatient care from Original Medicare.
Medicare Advantage Prescription Drug (MA-PD) Plan
Before starting your research, make a list of drugs and dosages you are currently taking. If you select a lan that does not cover all of your drugs, your doctor or pharmacist may be able to suggest a generic version or a different medication covered by your plan.
The second type of plan, called a Medicare Advantage plan, covers Medicare benefits under Parts A and B, and may also cover the Medicare Part D drug benefit. Medicare Advantage plans that include drug coverage are called Medicare Advantage Prescription Drug (MA-PD) plans. These plans are offered by private insurance companies and are usually either Health Maintenance Organizations (HMOs) or Preferred Provider Organizations (PPOs).
If you receive your health benefits from a Medicare Advantage HMO or PPO plan, and you want Medicare drug coverage, you usually must get your drug coverage from the same plan that provides your health coverage. Medicare Advantage plans sometimes offer additional benefits beyond what traditional Medicare offers, but the plans typically impose restrictions on which doctors and hospitals enrollees may visit. In some areas, there are dozens of Medicare Advantage plans available. For more information, see the Medicare Advantage Plans section.
Choosing a Medicare Drug Plan: Consider the Following Questions
If you choose to enroll in a Medicare prescription drug plan or want to switch plans, you should first decide whether you want a stand-alone prescription drug plan (PDP) or a Medicare Advantage prescription drug (MA-PD) plan. Then, you will want to compare the various features of plans available in your area. Plans set their own premiums and benefits within certain guidelines established by Medicare. There are important differences between plans, including premiums, deductibles, which drugs are covered, and how much you will pay to fill your prescriptions for different types of drugs (generics vs. Brand-name drugs). There may also be differences in the availability of in-network pharmacies across plans, so it is important to do some comparison shopping before signing up for a plan. Consider the following questions when selecting a Medicare drug plan.
Are my prescription medications on the plan’s list of covered drugs?
Each plan has a formulary – a list of drugs covered by the plan. Although all plans must meet Medicare’s requirements to cover at least two drugs in each therapeutic class or category, formularies vary across plans and some plans may not cover all of the drugs that you take.
Formularies might also include restrictions on what you have to do to get the drugs you take, including getting your doctor and the plan to approve the medication you take (prior authorization), getting you to try other, similar drugs before taking one that has been prescribed to you (step therapy), and how many pills you can get at a time (quantity limits).
Plans are expected to provide access to a large number of drugs, including almost all drugs within the following classes: antidepressants, antipsychotics, anticonvulsants, antiretrovirals, immunosuppressants, and antineoplastics (used to treat cancer). You can use the Medicare Plan Finder on http://www.medicare.gov or call 1-800-MEDICARE to identify plans in your area that cover your drugs.
Drug plans can change the drugs they cover and the prices that they charge for covered drugs during the year. If your plan makes mid-year changes to a covered drug that you are currently taking, the change will generally not affect you for the remainder of the calendar year. However, these changes would apply the following year, unless you get special permission from the plan for continued coverage of the drug.
If possible, it’s best to choose a plan that includes all your drugs on its formulary without restrictions. However, if you enroll in a plan that doesn’t cover your drugs or places restrictions on them, you have the right to a one-time transition refill of those prescriptions during your first 90 days in the plan. You can also apply for an exception for coverage for the rest of the year. For more information about these procedures, call 1-800-MEDICARE or contact your plan.
How much will I have to pay for each of my prescriptions?
After checking to see whether your drugs are included on the formulary and whether any restrictions apply, you will want to know how much the plan charges for each medication. You may be required to pay different amounts for different drugs on the formulary because most plans have multiple levels (known as “tiers”) of copayments. Most plans have different tiers for generic and brand-name drugs, and many plans also have what is called a “specialty-tier” for certain high-cost medications. Typically, plans charge less for generics than brand-name drugs.
If you sign up for a Medicare drug plan that does not cover all of your prescriptions, the money that you spend out-of-pocket to purchase drugs not covered by your plan will not count toward the $4,700 out-of-pocket spending catastrophic coverage limit.
You can find estimates of your prescription drug costs in different Medicare drug plans by entering your list of prescriptions and dosages and your preferred pharmacy into the Medicare Plan Finder, available at http://www.medicare.gov/find-a-plan/.
Is my regular pharmacy in the plan’s network?
Drug plans must contract with pharmacies in your area, but they do not have to contract with all pharmacies. You will pay the least if you use pharmacies that are preferred network pharmacies. Before signing up with a plan, check to make sure the pharmacies you use are preferred in-network pharmacies. Some plans also allow you to get your prescriptions delivered to you through the mail at a lower cost than purchasing them at a retail pharmacy.
If you’re not sure which plans include your local pharmacy in their network, ask your pharmacist for a list of plans accepted there. If you fill a prescription at a pharmacy that is not in your plan’s network, you will usually have to pay the full cost of the medication. Your plan will only approve coverage from out-of-network pharmacies if you could not get to a network pharmacy and you do not usually use pharmacies that are out of network.
Enrolling in a Medicare Prescription Drug Plan
There are a number of ways that you can sign up for a Medicare prescription drug plan:
- Mail in or fax a paper application. Contact the company offering the drug plan you select and request that they send you an application. Once you fill out the application, mail or fax it back to the company.
- Call the plan, or visit the plan’s website. You can enroll in a plan by calling the company and speaking with a representative, or by filling out your application online.
- Call 1-800-MEDICARE, or visit Medicare’s website. You are also able to enroll in most drug plans at http://www.medicare.gov through Medicare’s online enrollment center. Drug plan participation in Medicare’s enrollment center is voluntary, so not all plans offer this option.
To enroll in a plan, you will have to provide your Medicare number, and the date that your Part A and/or Part B coverage started; this information is printed on your Medicare card. You must also indicate whether you want to be billed for the premium or to have it deducted from your Social Security check. Finally, keep copies of any forms you mail and record the date and time of the calls you make, as well as the name of the representative.
Medicare drug plans are not allowed to call you and enroll you in a plan. If a plan calls you, do not give your personal or financial information over the phone. Call 1-800-MEDICARE to report any plans that call you and request personal information.
Once your enrollment is processed, the company offering the plan will send you an acknowledgement letter confirming your enrollment. This letter serves as your proof of insurance until your membership card arrives. Take that letter with you to the pharmacy if you need to fill a prescription before your membership card arrives. Along with the card, you will receive a member handbook, a list of covered drugs, a pharmacy provider directory, complaint and appeal procedures, and other important information about being a plan member.
Switching Medicare Drug Plans
Fall Open Enrollment is from October 15 to December 7 each year. You can change your Medicare drug plan during Fall Open Enrollment; the change will take effect on January 1. You can also enroll in a plan during this time if you did not enroll during your Initial Enrollment Period. In most cases, you will not be allowed to make a change outside of this designated time period.
For this reason, if you are already enrolled in a plan, you may want to re-evaluate your plan options during the Fall Open Enrollment Period each year. You can do this by reading your plan’s Annual Notice of Change, which notifies you how your plan will be different next year. Plans are required to mail this notice to current enrollees before the Open Enrollment Period each year; for example, Medicare Drug Plans may change the list of drugs they cover, their premiums, and the costs of the drugs they cover. While you may be satisfied with your current plan, be sure to check whether your coverage will stay the same for the following year. If your plan is making benefit changes, you may want to see if there are other plans that better suit your needs and preferences.
If you decide to switch your plan, you can switch to a new plan by enrolling in another drug plan during Fall Open Enrollment; coverage through your old Medicare drug plan will automatically end when coverage through your new drug plan begins.
Individuals who receive Extra Help and those who reside in nursing homes are able to switch plans on a monthly basis during the year. In addition, people who move to another region where their plan is not available and those whose “creditable” drug coverage is terminated are also able to enroll in or switch plans during the year.
Getting Extra Help with Medicare Drug Costs for People With Limited Incomes
Medicare provides extra help paying for prescription drug costs for people with limited income and resources. If your annual income is below $16,755 in 2012 ($22,695 for a couple) and your resources are less than $13,070 ($26,120 for a couple) in 2012, you may be eligible for additional assistance. Those who qualify get help paying for their drug plan’s monthly premium, yearly deductible, and prescription copayments or coinsurance. The amount of extra help you can get is based on your income and resources. For more information on Extra Help, see Extra Help with Prescription Drug Costs in the “Medicare and People with Low Incomes” section.
Report: Medicare Advantage Plans
Download a printable pdf version of this section.
Download a printable pdf version of the entire guide.
- Basics of Medicare Advantage
- Medicare Advantage Plan Options
- Choosing a Medicare Advantage Plan
- Enrolling in a Medicare Advantage Plan
- Switching Medicare Advantage Plans
Basics of Medicare Advantage
One in four people enrolled in Medicare today are covered under Medicare Advantage rather than Original Medicare. Medicare Advantage plans are health plans offered by private companies that contract with Medicare to provide Medicare benefits. There are many different types of Medicare Advantage plans. The most common types are Health Maintenance Organizations (HMOs), Preferred Provider Organizations (PPOs) and Private fee-for-service (PFFS) plans. To enroll in a Medicare Advantage plan, you must have both Medicare Part A and Part B, and pay the premiums as applicable. To make an informed decision, and to be able to decide which plans best meet your health needs and financial constraints, you need to first understand how these health plans work and how they differ.
There are different types of Medicare Advantage plans. Medicare Advantage plans provide all benefits covered under Medicare Part A and Part B, but can do so with different cost-sharing than Original Medicare. Medicare Advantage plans have an annual out-of-pocket limit on cost-sharing for benefits covered under Parts A and B of Medicare. They may also provide additional benefits, such as vision and dental care. Medicare Advantage plans are also not allowed to charge you more than Original Medicare for certain services, including dialysis and chemotherapy. Medicare Advantage plans may charge a premium, in addition to the Part B monthly premium. In addition to variations in premiums, Medicare Advantage plans vary in benefits, cost-sharing requirements, and provider networks.
Medicare Advantage Plan Options
Health Maintenance Organizations (HMOs)
In Medicare HMOs, you can generally only use doctors, hospitals, and other providers in the HMO’s network, unless it is an emergency or urgent situation. A network is a group of providers that contract with a plan to provide services for its members. Usually, if you see a doctor outside of the plan’s network you will have to pay for the full cost of your care.
If you join a Medicare HMO, you often need to choose a primary care physician. You may need to get permission or a referral from your primary care doctor before you can see a specialist.
If you are in a Medicare HMO and want Medicare drug coverage, you must get your drug coverage from the same HMO that provides your health coverage.
Preferred Provider Organizations (PPOs)
HMOs and PPOs differ in two key ways:
- PPOs typically will cover part of the cost of your care if you see a doctor out of the network, but you’ll likely have to pay more than when you see in-network doctors.
- Medicare PPOs allow you to see a specialist without referral from your primary care physician.
As with HMOs, if you want Medicare drug coverage and you are in a PPO, you must receive your drug coverage from the same plan that provides your health coverage.
Regional PPOs became available under Medicare in 2006. These plans are similar to local PPOs, but serve a larger geographic area (either a single state or multi-state area) and must offer the same premiums, benefits, and cost-sharing requirements to all beneficiaries in the region. As with local PPOs, individuals who sign up for a regional PPO will typically pay more if they go to providers outside of the network.
Private Fee-for-Service (PFFS) Plans
Private fee-for-service plans are another type of Medicare Advantage plan. In a PFFS plan, the providers you use must accept the plan’s terms and conditions. If you are considering enrolling in a PFFS plan, make sure your doctors and hospitals are willing to accept the PFFS plan’s payments for services before you enroll.
In addition, some PFFS plans have networks. If your plan has a network, you will usually pay more if you see providers who are not in the plan’s network. Be sure you understand a plan’s benefits and cost sharing requirements before you enroll.
PFFS plans are not required to offer drug coverage, but most do. If you want Medicare drug coverage and you are in a PFFS plan that does not provide drug coverage, you can join a stand-alone prescription drug plan.
Medicare Medical Savings Accounts (MSAs)
Medicare Medical Savings Accounts (MSAs) are another type of Medicare Advantage plan. Here is how Medicare MSAs work:
- The plan makes an annual deposit on behalf of each beneficiary into a bank of the plan’s choice. The money in the account will not be taxed as long as the beneficiary uses it for qualified medical expenses. Beneficiaries may not contribute their own funds to the account.
- A beneficiary enrolled in this type of plan must meet a high annual deductible (no more than $10,600 in 2012) before the plan will begin to pay for health care expenses. After the deductible is met, the plan is responsible for the full cost of all services covered under Medicare Part A or B.
- Beneficiaries can use the money in the MSA towards either meeting the deductible or to pay for health care services not covered by Medicare. At the end of the year, if any amount in the MSA account is unspent, it can be rolled over to cover the beneficiary’s costs incurred in the following year. Beneficiaries enrolled in MSAs are still required to pay the Part B monthly premium; however, there is no additional monthly premium for these plans.
- MSAs do not cover Part D prescription drugs. Beneficiaries with an MSA should enroll in a stand-alone prescription drug plan (PDP) if they want Part D drug coverage.
For additional information about Medicare Advantage plans, call 1-800-MEDICARE, or get information about Medicare options in your area on the Medicare Options Compare website at www.medicare.gov/find-a-plan/questions/home.aspx
Medicare Special Needs Plans (SNPs)
If you meet the qualifications of a Special Needs Plan (SNP) in your area, you have the option to enroll in it instead of having Original fee-for-service Medicare. SNPs are a type of Medicare Advantage plan that were created to improve the management of care for Medicare beneficiaries who are either dually eligible for Medicare and Medicaid, require an institutional level of care, or have certain chronic conditions. Like other Medicare Advantage plans, SNPs have contracts with Medicare and are run by private companies. All SNPs include Part D coverage. The Medicare program pays the plans fixed monthly amounts. If you have full or partial coverage from Medicaid in addition to Medicare, you have a continuous special enrollment period. This means that you can enroll and disenroll from any plan at any time during the year. Also, if you have a chronic health condition that a SNP in your area treats, you have a special enrollment period to join that SNP.
Medicare Advantage and Prescription Drugs
All companies offering Medicare Advantage plans must offer prescription drug coverage in at least one of their plans. About 80 percent of Medicare Advantage plans include drug coverage. Medicare Advantage plans with drug coverage may vary in their premiums, deductibles, formularies and cost-sharing, depending on the type of Medicare Advantage plan you select. In most cases, if you want to join a Medicare Advantage plan, you will need to get your Medicare prescription drug coverage through that plan. See the Medicare and Prescription Drug Coverage section for more information.
Choosing a Medicare Advantage Plan
Each January, plans change their coverage and costs. During the Fall Open Enrollment Period, you should find out how your current plan will change in January and review your coverage choices. You can keep your coverage through your Medicare private plan if the plan continues operating in your area from year to year. If you think you may want to change, the next step is to find out which plans are offered where you live. While Original Medicare is available in all parts of the U.S., certain types of private plans may not be. In some areas of the U.S., people with Medicare have a limited choice of private plans, while in other areas, there are many Medicare private plans to choose from.
For a list of plans in your area and a copy of the Medicare handbook, Medicare & You, call Medicare at 1-800-MEDICARE or visit Medicare’s website at www.medicare.gov. For free help in understanding differences among Medicare plans, you can call your State Health Insurance Assistance Program (SHIP). Contact information for your state’s SHIP is found in the Medicare handbook and in this guide under Additional Resources.
You should consider these important factors before signing up for a plan:
- Accessibility of doctors and hospitals. Can you continue to see the doctors you know and trust if you join a certain plan? Your doctor or specialist might be in one plan’s network, but not in another plan’s network.
- Extra benefits. The additional benefits offered by Medicare private plans vary widely and may change every year.
- Prescription Drugs. Remember that you must typically get your Part D prescription drug benefits through the same private health plan that offers your health benefits. Make sure that the prescription drug plan covers the drugs you need and that you understand any limits that may apply. Also, make sure the plan includes the pharmacies you use in its network.
- Cost. You might want to consider the following questions: How much are the monthly premiums and copayments associated with different health care services? Is there a deductible? How do the costs for various services differ from Original Medicare? Keep in mind that costs generally change each calendar year.
- Quality ratings. Not all Medicare private plans are the same. The Centers for Medicare and Medicaid Services (CMS) post quality ratings of Medicare Advantage plans that may be a useful tool. Find your plan’s star rating from Medicare and try to talk to plan members about their experiences. To find your plan’s star rating, visit Medicare’s website at www.medicare.gov/find-a-plan.
Know your Rights
No matter which plan you choose – Original Medicare, a Medicare HMO, or another Medicare private plan – understand your rights as a patient and a consumer. If you believe you have been unfairly denied any benefits covered by Medicare or your Medicare Advantage plan, you have the right to appeal. You should send a copy of the denial notice to the company that issued the denial and, if possible, a letter from your doctor explaining your need for the denied service and a letter requesting a review.
Enrolling in a Medicare Advantage Plan
There are a number of ways that you can sign up for a Medicare Advantage plan:
- Mail in or fax a paper application. Contact the company offering the plan you select and request that they send you an application. Once you fill out the application, mail or fax it back to the company.
- Call the plan, or visit the plan’s website. You can enroll in a plan by calling the company and speaking with a representative, or by filling out your application online.
- Call 1-800-MEDICARE, or visit Medicare’s website. You are also able to enroll in most plans at www.medicare.gov through Medicare’s online enrollment center. Plan participation in Medicare’s enrollment center is voluntary, so not all plans offer this option.
To enroll in a plan, you will have to provide your Medicare number and the date that your Part A and/or Part B coverage started. This information is on your Medicare card.
If you are already in a Medicare Advantage plan and are switching to a new one, you do not need to disenroll from your old plan. Simply enroll in the new plan. Your coverage in the old plan will automatically end when your new coverage begins.
Medicare Advantage plans are not allowed to call you and enroll you in a plan. If a plan calls you, do not give your personal or financial information over the phone. Call 1-800-MEDICARE to report any plans that call you and request personal information.
Once your enrollment is processed, the company offering the plan will send you an acknowledgement letter confirming your enrollment. This letter serves as your proof of insurance until your membership card arrives.
Switching Medicare Advantage Plans
Fall Open Enrollment is from October 15 to December 7 each year. During this period, you can join a Medicare Advantage plan. You can also switch Medicare Advantage plans, and add, drop, or switch Medicare prescription drugs plans at this time. You can enroll in a Part D plan during this time even if you did not enroll during your Initial Enrollment Period.
In most cases, you will not be allowed to make a change outside of this designated time period. However, if you do need to make a change outside of the Fall Open Enrollment period, you can switch to a Medicare Advantage plan or a Part D plan that has the highest overall plan performance rating of 5 stars at any time during the year. You can find star ratings for plans in your area by going to www.medicare.gov/find-a-plan.
Changes you make during Fall Open Enrollment will take effect on January 1 of the following year. If you decide to switch your Medicare Advantage plan, you can simply enroll in the Medicare Advantage plan of your choice. Your old Medicare Advantage plan will automatically end when your new plan begins.
There is another period from January 1 through February 14 each year called the Medicare Advantage Disenrollment Period. During this time, you can drop your Medicare Advantage plan and return to Original Medicare. If you would like to begin receiving or continue to receive Medicare drug coverage, you can also usually enroll in a stand-alone drug plan during this period. Changes made during this period will take place on the first of the month after the change is made.
There are certain situations in which you might qualify for a Special Enrollment Period. A Special Enrollment Period is a time outside of the standard enrollment periods when you can add, drop or change your plan. A few examples of Special Enrollment Periods include (1) if you move outside the plan’s service area, (2) if you enter, reside in or leave a skilled nursing facility, nursing home, or (3) if you receive Medicaid or Extra Help.’
Report: Medicare Supplemental Insurance

Download a printable pdf version of this section.

Download a printable pdf version of the entire guide.
- Basics of Medicare Supplemental Insurance (Medigap)
- Choosing a Medigap Policy
- Enrolling in a Medigap Plan
- Switching Medigap Policies
Medicare provides broad protection against the costs of many health care services, but has relatively high cost-sharing requirements and significant gaps in coverage. As a result, most beneficiaries have some form of supplemental coverage.
If you want to stay in Original Medicare, you may want to consider your options for supplemental coverage. Insurance that is supplemental to Medicare pays after Medicare. It helps pay Medicare costs and pay for care that Medicare does not, such as emergency care outside of the U.S. Without such coverage, your out-of-pocket costs could be high if you require medical care.
About one in three Medicare beneficiaries receive supplemental coverage through employer-sponsored retiree health coverage. If you have access to this type of supplemental coverage, there are advantages to keeping this coverage. Some retiree policies may be more generous than other types of coverage. They are sometimes less expensive than other policies, since employers tend to pay at least part of the cost. If you are not yet on Medicare, find out what employee benefits you may be eligible for when you go on Medicare, and ask how these benefits coordinate with Medicare.
Other beneficiaries who have limited incomes have access to supplemental coverage under Medicaid. Today, about 20 percent of Medicare beneficiaries are dually eligible for Medicare and Medicaid. For more information, see the Medicare and People with Low Incomes section.
For those in Original Medicare without access to employer-sponsored retiree health coverage or Medicaid, Medigap is one option for supplemental coverage. Medigap policies help make health care costs more predictable and stable. Medigap policies charge a monthly premium and cover some or all of your Medicare costs. Medigap policies typically require no additional paperwork to get your medical bills paid. Medicare usually pays its share of the health care bill and then sends it to your Medigap insurer to pay. Today, about one in five Medicare beneficiaries has supplemental insurance through an individually-purchased Medigap policy. The information below will address Medigap coverage, and will not discuss other sources of supplemental coverage.
Basics of Medicare Supplemental Insurance (Medigap)
If you want to buy a Medicare supplemental insurance policy, known as a “Medigap” policy, you will need to decide which benefit package to buy and which insurer to use. Before making a decision, it is helpful to understand what benefits are covered and how to compare plans.
There are 10 different standardized Medigap plans, labeled A, B, C, D, F, G, K, L, M, and N. Each Medigap plan pays for a particular set of benefits. Core benefits are benefits that every Medigap plan must cover, such as Medicare Part A copayments. Not all plans are available in all states. Massachusetts, Minnesota and Wisconsin have their own standardized Medigap plans.
Insurance companies that sell Medigap policies are not required to sell all Medigap plan types; however, they are required to offer at least plan A if they offer any other Medigap plans. Plan A offers the fewest benefits of the ten standardized Medigap plans.
The most popular Medigap plans are C and F; these two plan types are also the only two that cover both the Part A and Part B deductibles.
On June 1, 2010, plans M and N were created. Prior to June 1, 2010, there were also plans E, H, I, and J. While these plans are no longer sold, individuals who have these policies can keep their policy as it is, and will be able to continually renew it.
Plans sold starting June 1, 2010 will no longer include the at-home recovery benefit. All plans will now include hospice care as a core benefit.
Medigap plans K and L have high deductibles. This means that they only start paying in full for your care after you have spent a certain amount of money out-of-pocket. Compared to other Medigap options, these plans are designed to provide more protection when you are very sick but include less coverage of your initial expenses. They require you to pay part of your costs for most Medicare-covered services until you have spent a certain amount out of pocket each year. Once you reach your out-of-pocket limit, both plans cover all of your Medicare deductibles and coinsurance for that year. Medigap premiums often vary widely – even for identical plan coverage. The cost of your Medigap policy depends on the type of Medigap plan you choose, the company from which you buy your policy, and the cost of Medigap plans in the state or county where you live. Once you have chosen the plan you want, it pays to shop around. Plans with the same letter name offer the same benefits, but the premiums vary from company to company.
No Medigap insurance policy fills gaps in coverage for Medicare HMOs or any of the other Medicare Advantage private health plans. Should you select an HMO, PPO, or other type of Medicare Advantage plan, you should budget for any costs that the plan doesn’t cover.
For free assistance with understanding your options, contact your local State Health Insurance Assistance Program (see Additional Resources). More information about Medigap plans can be found at: www.medicare.gov/Publications/Pubs/pdf/02110.pdf.
This chart shows the Medigap plan benefits for plans effective January 1, 2012:
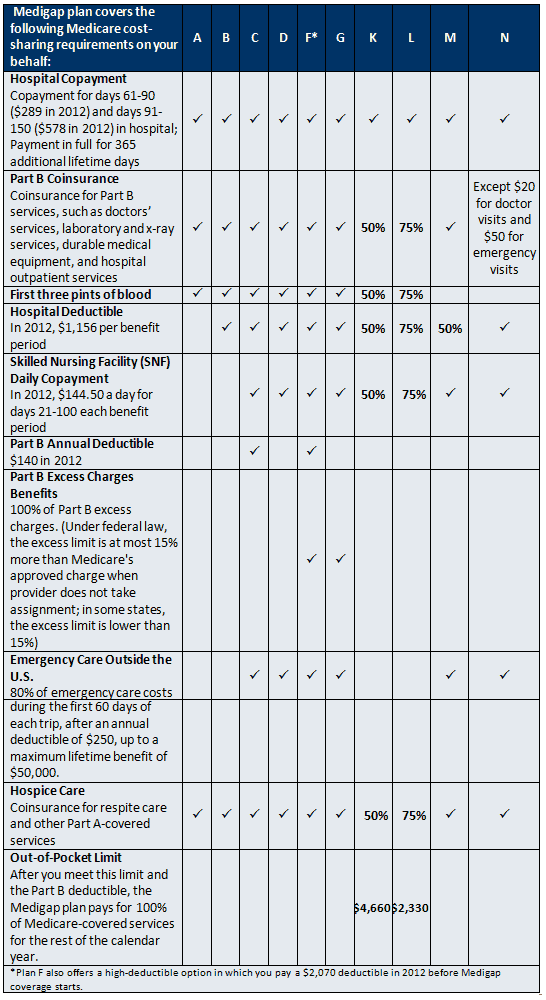
Choosing a Medigap Policy
If you decide to purchase a Medigap policy, and have selected a type of plan (A-N), then the next step is to decide from which insurance company you wish to purchase your policy. The following steps will help you decide wisely.
- Call the insurance department in the state where you live for a list of companies that offer Medigap policies. Compare the premiums for the plan you want; premiums may vary considerably and rates may change each year.
- Understand how premiums are calculated and how they will change as you get older. Medigap premiums are calculated in three different ways:
- Attained-age rated: premiums are based on your current age, and typically increase as you get older. In states that allow this, if you keep your Medigap policy, your monthly premium might increase as you age.
- Issue-age rated: premiums are based on the age you are when you originally purchased the policy. Premiums are lower for people who purchase policies at a younger age. Once enrolled in a plan, your premiums won’t change based on your age, but they may go up because of inflation or other factors.
- Community-rated: premiums are the same for policyholders regardless of age; premiums may still increase because of inflation or other factors, but do not vary based on age.
After you’ve decided on the insurance company and Medigap plan that is best for you, contact the insurance company for a summary of the Medigap policy and an application. Fill out the application form carefully and completely. Remember, if you are applying for a policy in the first 6 months after you turn 65 and have Part B, or within 63 days of losing certain kinds of insurance, the insurance company cannot deny you a Medigap policy or change the price of a policy based on your answers to the medical questions. Your Medigap coverage typically begins on the first day of the month after you apply.
Enrolling in a Medigap Plan
You have the right to buy a Medigap policy only at certain times.
- Starting the month you turn 65 and are enrolled in Part B, you have an open enrollment period to sign up for any Medigap plan available in your state.
- If you are 65 or older, you have a “guaranteed issue right” to enroll in certain Medigap polices within 63 days of losing certain types of coverage, such as a retiree health plan or a Medicare Advantage plan.
These are the federal open enrollment periods. Some states have much broader open enrollment periods. Check with your state’s department of insurance for more information about enrollment rules in your state.
Federal law does not require Medigap insurers to sell Medigap policies to Medicare beneficiaries under age 65; however, some states do require insurers to sell Medigap policies to beneficiaries under age 65. If you are under 65, check with your state’s department of insurance or State Health Insurance Assistance Program for more information.
Under federal law, Medigap insurers cannot refuse to sell people age 65 or older a Medigap policy and cannot raise premiums because of a person’s health status during their open enrollment period or guaranteed issue period. Outside of these times, Medigap insurers can refuse to offer you a Medigap plan or can charge you higher premiums because of your health status, unless your state has more generous enrollment rules that prohibit them from doing so.Additionally, if you are in a guaranteed issue period, your insurer cannot make you wait for coverage of pre-existing conditions. During your open enrollment period, plans can wait to cover your pre-existing conditions for up to six months unless you had continuous coverage from certain types of insurance for at least six months prior to enrolling in the Medigap plan.
Switching Medigap Policies
In most cases, insurance companies are not required to sell you a Medigap plan, unless you are in your 6-month open enrollment period or have guaranteed issue rights. As mentioned above, however, some states have more generous requirements. Check with your state’s insurance department about your Medigap rights and protections.
Before you switch to a new plan, be sure to compare the benefits and premiums before switching. As when you first purchased your Medigap policy, be sure to understand how your premiums are calculated, and how they may increase as you age.
Report: Medicare And People With Low Incomes

Download a printable pdf version of this section.

Download a printable pdf version of the entire guide.
- How Medicaid Helps People with Low Incomes
- Getting Help through a Medicare Savings Program (MSP)
- Extra Help with Prescription Drug Costs
If, like millions of seniors and people with disabilities, you are living on little income and have few resources (or assets), you may be able to get financial assistance from Medicaid, a Medicare Savings Program, or programs that help with prescription costs. If you qualify, you could receive help with your monthly Medicare premiums and/or Medicare’s cost-sharing requirements. You may also qualify for additional Medicaid benefits, such as long-term care. You may also qualify for extra financial assistance with Medicare drug coverage.
Below are some of the basic rules for programs that exist for people on Medicare with low incomes. To get additional information about whether you qualify for full Medicaid benefits or one of the Medicare Savings Programs in your state, contact your state Medicaid program (see Additional Resources). Another option is to use the online tool provided by the National Council on Aging (www.benefitscheckup.org).
How Medicaid Helps People with Low Incomes
Who are the “Dual Eligibles?”
Nine million low-income elderly and disabled people are dually eligible for Medicare and Medicaid. Medicaid is jointly funded by the federal government and the states, and covers medical care for people with low incomes and assets. The Medicaid program varies from state to state. Each state has its own way of determining eligibility for Medicaid depending on people’s age, family size, medical condition and financial situation. States typically use income and asset rules from the SSI (Supplemental Security Income) program to assess Medicaid eligibility for people with Medicare. If you receive some form of health care coverage from both Medicare and Medicaid, you fall into the category of a “dual eligible.”
Qualifying for Medicaid as a Medicare Beneficiary
To qualify for Medicaid, you must have income and assets below a defined level. Most dual eligibles qualify for full Medicaid benefits as well as coverage of Medicare premiums and cost sharing; in most states, this entails having an annual income no greater than $8,387 for individuals in 2012 ($12,579 per couple), and assets no greater than $2,000 for individuals and $3,000 for couples. However, some states have higher, more generous income and asset limits. For low-income beneficiaries with somewhat higher income or assets, Medicaid will cover their Medicare premiums, and in some instances their cost sharing, through Medicare Savings Programs (MSPs).
Understanding Your Medicaid Benefits as a Dual Eligible
Full Medicaid benefits: Most dual eligibles qualify for full Medicaid benefits. Medicaid pays after Medicare and may cover benefits that Medicare does not, such as routine dental coverage. Medicare beneficiaries can receive full Medicaid benefits through several pathways.
If you receive cash assistance under the Supplemental Security Income (SSI) program, you are eligible for full Medicaid benefits in most states. To receive SSI, your annual income cannot exceed $8,387 in 2012 ($12,579 per couple) and your assets must be no greater than $2,000 ($3,000 per couple), although some types of income and assets (such as the value of your home) are not counted. Some states allow people with Medicare to have higher monthly incomes and assets to be eligible for Medicaid.
Medicaid programs also have the option of providing full Medicaid benefits to people with slightly higher incomes, certain nursing home residents, and beneficiaries eligible for home and community based services (HCBS). If you are eligible because you fall into one of these categories, you may still qualify for Medicaid if you have higher income and resources than the SSI program will allow.
Medicaid benefits for people with slightly higher incomes: Many states provide full Medicaid benefits to Medicare beneficiaries with slightly higher incomes than SSI will allow. For more information, contact your state Medicaid program (see Additional Resources).
Medicaid benefits for the medically needy: Most states also have a medically needy or equivalent program that allows individuals with higher income to qualify for Medicaid benefits if they have high medical expenditures. Your eligibility is computed in these programs by deducting your individual medical costs from your individual income, and thus as a beneficiary, you “spend down” your income to the “medically needy income level,” The eligibility limits for the medically needy programs vary considerably across states, and are permitted to vary within states.
Medicaid benefits for people needing nursing home care: Most Medicaid programs accept nursing home residents who have higher incomes (up to 300 percent of the SSI level) since few Medicare beneficiaries can afford the high cost of nursing homes. In addition, most states let people use nursing home and other health care costs to spend down to medically needy income limits. Also, all states have Medicaid home and community based services (HCBS) for Medicare beneficiaries who would otherwise need to be treated in nursing homes, hospitals or institutions for the mentally disabled. States are given latitude in designing HCBS financial eligibility requirements, groups of people covered, and types of HCBS programs provided. HCBS programs can cover a variety of long-term care services, including home health care, personal care, respite care, as well as rehabilitative, homemaker and adult day health services.
Many HCBS programs are available only if you need institutional care, but in some cases, states can also offer these services before you need institutional care. HCBS programs differ widely across states. Contact your Medicaid office for specific details on programs in your state.
Getting Help through a Medicare Savings Program (MSP)
What are Medicare Savings Programs (MSPs)?
If your income or assets are too high to qualify for full Medicaid benefits, you may be eligible for one of the Medicare Savings Programs (MSPs), which cover Medicare premiums, and in some instances cost-sharing, for Medicare beneficiaries with slightly higher incomes or assets. There are four different Medicare Savings Programs: QMB, SLMB, QI and QDWI. Most people with full Medicaid also qualify for a Medicare Savings Program to help pay their Medicare costs.
The federal government sets minimum income and asset limits, but states can make eligibility rules more generous. The asset limits for QMB, SLMB and QI increase with inflation each year; the limits for QDWI are not indexed, and instead they remain the same from year to year.
Who is Eligible for an MSP?
- Qualified Medicare Beneficiaries (QMBs): As a QMB, you are eligible for assistance with both Medicare premiums and cost sharing, while other MSP beneficiaries receive assistance only with Medicare premiums. The monthly federal income limit for QMBs is $951 for an individual ($1,281 for a couple), and the asset limit is $6,940 for an individual ($10,410 for a couple) in 2012. For those who qualify, the state will pay Medicare premiums, deductibles and coinsurances.
- Specified Low-Income Medicare Beneficiaries (SLMBs): As a SLMB, you are eligible for assistance with Medicare Part B premiums, and must have a monthly income between $951 and $1,137 for an individual ($1281– $1,533 for a couple) and assets no more than $6,940 as an individual ($10,410 for a couple) in 2012.
- Qualified Individuals (QIs): The QI program is a limited expansion of the program for SLMBs, with an entitlement block-grant to the states for the program. Enrollment in the QI program is limited by the federal appropriations, and applications are approved on a first-come-first-served basis. As a QI, you are eligible for assistance with Medicare Part B premiums, and must have a monthly income between $1,137 and $1,277 for an individual ($1,533 – $1,723 for a couple) and assets no more than $6,940 for an individual ($10,410 for a couple) in 2012.
- Qualified Disabled and Working Individuals (QDWIs): You may be eligible for assistance with your Medicare Part A premiums through the QDWI program if you are younger than 65 years old, have a disabling impairment, and are no longer entitled to free Medicare Part A because you have successfully returned to work. To receive this Medicaid assistance, your monthly income must be at or below $3,809 for an individual ($5,129 for a couple) and assets must be no more than $4,000 as an individual ($6,000 for a couple) in 2012.
Additionally, QMBs, SLMBs, and QIs automatically get assistance with their prescription drug costs through the Low-Income Subsidy (LIS) program, which provides assistance with Medicare Part D premiums and cost sharing. LIS is also available for individuals with annual incomes at or below $16,755 ($22,695 for couples) and assets no greater than $13,070 ($26,120 for couples) in 2012. The asset levels allow for an additional $1,500 per person for burial expenses.
The income and asset limits for Medicare Savings Programs vary by state. Some states, such as New York, do not count your assets for the Medicare Savings Programs, and some states have much higher income limits. You are not penalized for applying even if it is determined that you do not qualify. To learn more about these programs or to apply, contact your local Medicaid office see Additional Resources.Back to the Top
Extra Help with Prescription Drug Costs
Medicare provides extra help paying for prescription drug costs for people with limited income and resources. If your annual income is below $16,755 ($22,695 for a couple) and you have resources up to $13,070 ($26,120 for a couple) in 2012, you may be eligible for assistance through the Extra Help program. Those who qualify get help paying for their drug plan’s monthly premium, yearly deductible, and prescription copayments and/or coinsurance. The amount of extra help you get is based on your income and resources (see box titled Which Resources are Counted for Extra Help?).
The following descriptions are intended to help you get an idea of whether you may be eligible for Extra Help.
Who Should Apply for Extra Help?
If you receive full Medicaid benefits, are enrolled in a Medicare Savings Program (MSP) or receive Supplemental Security Income (SSI), you are automatically eligible for Extra Help with your drug costs and do not need to apply separately for Extra Help. You will be automatically enrolled in Extra Help. You will also be automatically enrolled in a Part D plan if you do not already have one and do not choose a plan yourself.
If you do not have Medicaid, an MSP, or SSI, you may still be eligible for Extra Help if you meet the income and asset limits. However, you will not be automatically enrolled and will have to apply for Extra Help. If you apply and are approved for Extra Help, you will be automatically enrolled in a Part D plan if you do not already have one and do not choose a plan yourself.
People on Medicare Who Also Get Help from Medicaid
If you have both Medicare and Medicaid, your drug benefits are provided by a Medicare prescription drug plan. You will have very low copayments for your prescription drugs. Extra Help will also pay your Part D premium if you are enrolled in a plan with a premium below a certain level, also known as a premium-free or “benchmark” plan. The maximum premium that Extra Help will pay for a Part D plan is called the “benchmark,” an amount which varies by state. If you choose to enroll in a plan that has a premium above this amount, you will be required to pay the difference. You will not be required to pay a deductible.
If you are enrolled in Extra Help, you have the option to choose your own plan, and can switch plans each month. You will always have the option of at least one premium-free plan. During the fall, you will receive a notice if your plan will no longer qualify as a premium-free plan for the following year, in which case you have the option to choose another premium-free plan. If you choose to stay in the same plan, you will need to pay the difference.
If you do not choose a plan yourself, Medicare will enroll you in a premium-free plan, and will automatically notify and reassign you to a new plan if the plan no longer qualifies as a premium-free plan.
If you have Medicaid, you automatically get Extra Help. Your drug costs will be as follows:
- If you have full Medicaid and your annual income is up to $11,170 for an individual ($15,130 for a couple) in 2012, then you will pay $1.10 for generic drugs and $3.30 for brand-name drugs in 2012 that are covered by your plan. After your total drug spending reaches $6,658, you will not have to pay anything for your prescription drugs.
- If you have full Medicaid and your monthly income is over $11,170 for an individual ($15,130 for a couple) in 2012, or if you do not have full Medicaid but have a Medicare Savings Program or SSI, you will pay $2.60 for generic drugs and $6.50 for brand-name drugs in 2012 that are on your plan’s formulary. After your total drug spending reaches $6,658, you will not have to pay anything for your prescription drugs.
Regardless of your yearly income, if you have full Medicaid coverage and are in a nursing home (such as a skilled nursing facility or intermediate care facility) or you have full Medicaid and receive home and community-based services (HCBS), you will not pay anything for your prescription drugs, as long as your plan covers the drugs you need and the nursing home buys them at a pharmacy that is in the plan’s network. If you are in a nursing home, but not on full Medicaid, you will still have to pay a co-pay for your drugs.
Other Beneficiaries with Limited Incomes and Resources
If you are not automatically eligible for Extra Help, but you have limited income and resources, you may still qualify for Extra Help.
Receiving Extra Help is generally a two-step process for people who do not automatically qualify; that is, if you do not have Medicaid, an MSP or SSI. First, you need to complete an application for Extra Help through the Social Security Administration (SSA). Then, you should enroll in a prescription drug plan to begin using the benefit. If you apply and qualify for Extra Help but do not choose a plan yourself, Medicare will enroll you in a plan available to you for zero premium.
Applications for Extra Help are available from your local Social Security or Medicaid office (see Additional Resources for contact information). You can also submit an application online through SSA’s website at www.ssa.gov.
There is no charge for applying, even if you don’t qualify. You need to provide information about your income and resources but do not need to provide any documentation confirming that information. If you do not have all of the information available, fill out what you know and mail or submit the application online. Someone from SSA will call you and help you complete the rest of the application over the phone or follow up with any further questions.
If you are approved for Extra Help, the amount of assistance you get depends on your income and assets. You will either get Full Extra Help or Partial Extra Help.
- If your annual income is up to $15,080 for an individual ($20,426 for a couple) in 2012 and your assets are up to $8,440 for an individual ($13,410 for a couple), you will get Full Extra Help. You will pay no deductible or monthly premium as long as you are enrolled in a premium-free (benchmark) plan. You will pay $2.60 for generic drugs and $6.50 for brand-name drugs for drugs that are on your plan’s formulary. After your total drug spending reaches $6,658, you will not have to pay anything for your prescription drugs in 2012.
- If your income and/or assets are too high to qualify for Full Extra Help but your 2012 annual income is below $16,755 for an individual ($22,695 for a couple) and your assets are no more than $13,070 for an individual ($26,120 for a couple), you will get Partial Extra Help. You will pay reduced monthly premiums that will depend on your income and either a $65 deductible or the plan’s standard deductible, whichever is cheaper. You will pay 15% of the costs of your prescription drugs until total drug spending reaches $6,658, at which point you will pay $2.60 for generic drugs and $6.50 for brand-name drugs in 2012.
See box above titled Which Resources are Counted for Extra Help?
Signing up for a drug plan
In general, Medicare pays the entire monthly Part D plan premium for people receiving Extra Help, but only up to a certain amount. You should check to see if the premium will be fully paid for the plan you want. If you enroll in a higher premium plan or a plan with enhanced benefits, you will have to pay part of the monthly premium. Enhanced benefits include additional coverage in the coverage gap beyond what the law requires plans to cover.
Switching plans
If you are enrolled in Extra Help, you have the option to choose your own plan, and you can switch plans each month. You will receive a notice during the fall if your plan will no longer be premium-free for you next year. You have the option to stay in your plan next year and pay a premium or to choose a cheaper plan. Medicare will automatically enroll you in a premium-free plan unless you choose one yourself or indicate you wish to keep your current plan.
Report: Additional Resources

Download a printable pdf version of this section.

Download a printable pdf version of the entire guide.
Information Sources to Select a Plan
There are a number of useful information sources that can help you learn more about Medicare, compare the plans serving your area, and make choices that work best for you.
The Medicare & You Handbook
The official Medicare handbook is mailed to all people on Medicare each year. The handbook contains a summary of Medicare benefits and cost-sharing requirements, coverage options, and answers to frequently asked questions about Medicare. The handbook is also available online at www.medicare.gov/publications/pubs/pdf/10050.pdf.
Medicare.gov, the Official Medicare Website
Medicare.gov is the official Medicare website, and contains general and detailed information about Medicare, including information about benefits covered, limits, and costs. Medicare.gov also has tools to compare drug and health plans in your area.
To compare plans or find out more information about a particular drug coverage option, you can visit Medicare’s Plan Finder website at www.medicare.gov. The website offers detailed information on monthly premium amounts and the deductible. For drug plans, it also lists what drugs are covered under the plan and how much you pay for each individual drug.
The Medicare Plan Finder can be used in various ways:
- You can enter your zip code and what type of plan you are interested in, and the tool shows you a list of all of the plans in your area. From there, you can research the individual plan’s features, or
- For drug plans, you can narrow your search by entering your list of drugs and/or your preferences for the amount you would pay for the premium and deductible, whether the plan offers mail order, and what pharmacy you prefer.
Either way you navigate the site, you will be able to get contact information for the plans and even sign up for most plans through www.medicare.gov.
To compare different Medigap policies that are offered in your area, you can visit Medicare’s Medigap Policy Finder website at www.medicare.gov. Similar to the Medicare Plan Finder, the Medigap Policy Finder offers information on plans available in your area. For this plan finder, you can enter your zip code and health status, select the benefit structure and plan type that you are interested in, and view the companies that sell Medigap policies in your area.
1-800-MEDICARE, the Official Medicare Hotline
The Medicare program operates a toll-free hotline, 1-800-MEDICARE (1-800-633-4227) to answer your questions 24 hours a day, including weekends. If you do not have internet access to use the Medicare Plan Finder or the Medigap Policy Finder on the Medicare website, you may call 1-800-MEDICARE for similar information.
State Health Insurance Assistance Programs
You can also get help in understanding your Medicare options and finding the best plan for you by calling your State Health Insurance Assistance Program (SHIP). Phone numbers and websites for the SHIP in your state are listed in the table below. SHIPs offer local health insurance counseling at no charge. Your state SHIP will be able to help you find the coverage options that are best for you, and address any concerns about your Medicare rights, billing problems, or answer your other Medicare-related questions.
Community Organizations
Other community-based groups may hold Medicare information sessions at local senior centers, libraries, government centers or other community areas. Some events may be sponsored by companies offering plans in your area or brokers that sell policies for plans. Make sure to find out who is sponsoring any event you are interested in attending, so you can know who is presenting the information, whether it is educational or marketing information, and whether it covers all plans available in your area, or only those offered by a specific company.
<insert table>