Understanding Medicaid Procedural Disenrollment Rates
As states unwind the Medicaid continuous enrollment provision, data show that large shares of people are being disenrolled for paperwork or procedural reasons as opposed to being determined ineligible. These high procedural disenrollment rates are raising concerns that many people who remain eligible for Medicaid may, nevertheless, be losing coverage. But, there are different procedural disenrollment rates being reported that can be confusing to interpret. This policy watch explains how the different rates are calculated, provides insights for interpreting the data, and describes steps the Centers for Medicare and Medicaid Services (CMS) and states are taking to reduce procedural disenrollments.
What are procedural disenrollments?
Procedural disenrollments occur when there is no definitive determination of ineligibility. Procedural disenrollments may happen because enrollees do not receive renewal notices or face barriers to completing the redetermination process, such as not understanding what steps need to be taken. In some cases, people may be procedurally disenrolled because eligibility workers are not able to process documents enrollees have submitted before cases are automatically closed. Some enrollees may know they are no longer eligible, perhaps because of an increase in income or other change in circumstance, and do not respond to the renewal request so the state cannot make a definitive determination that the person is no longer eligible. While some states are reporting reasons for procedural terminations that indicate whether someone may be over income or did not respond, these data are limited. The main concern with procedural disenrollments is that many people losing Medicaid for these paperwork reasons may still be eligible and do not have another source of health coverage.
How are the procedural disenrollment rates calculated and how should different rates be interpreted?
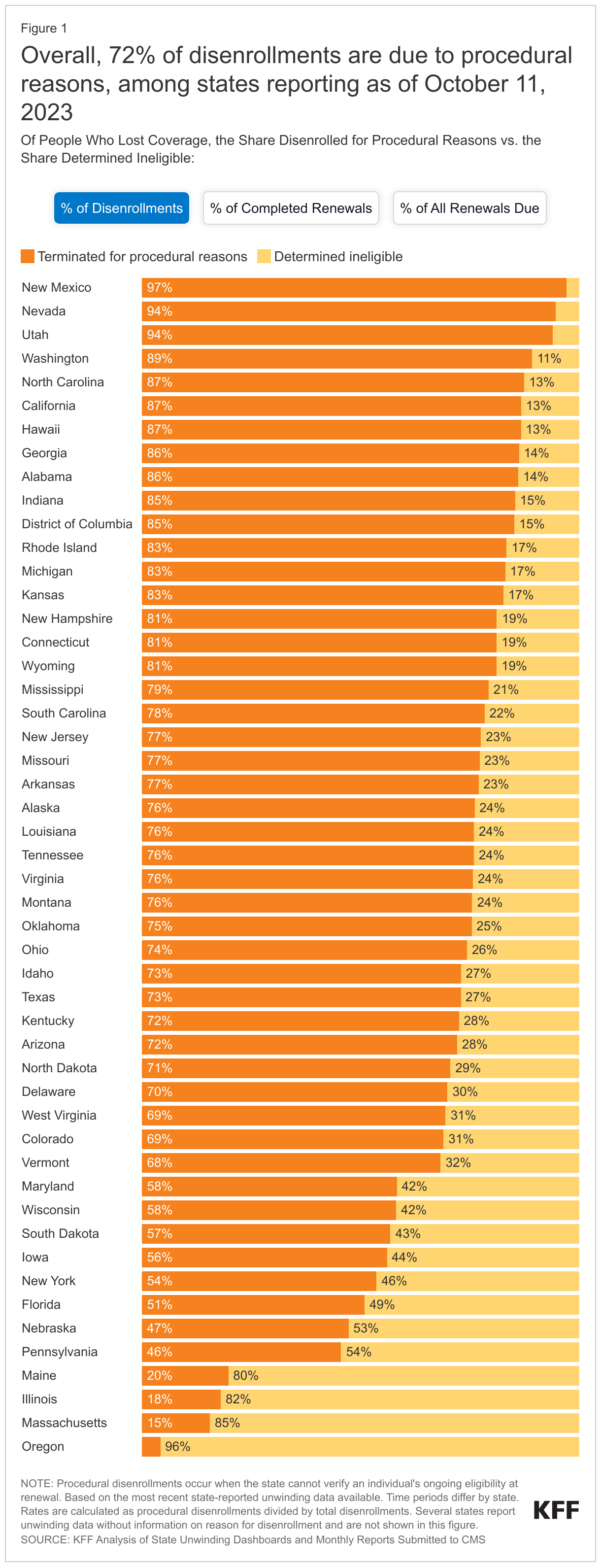
Different procedural disenrollment rates are being reported for states because of differences in how those rates are calculated. When calculating procedural disenrollment rates, the denominator and timeframe matter. A procedural disenrollment rate calculated using total disenrollments as the denominator is going to be higher than a rate that uses all initiated renewals, which includes enrollees whose coverage was renewed as well as cases that remain pending, as the denominator. Additionally, a cumulative procedural disenrollment rate based on all reported renewal data since the start of the unwinding period is going to differ from one that is cohort based and reflects only procedural disenrollments for a single month. The cumulative procedural disenrollment rate reported by KFF, 73% as of September 5, 2023, uses total disenrollments as the denominator, highlighting that a substantial majority of disenrollments are for paperwork reasons rather than for people being definitively determined ineligible. In contrast, the cumulative procedural disenrollment rate using all initiated renewals as the denominator is 20%, reflecting the fact that many people have had their coverage renewed (Figure 1).
Reporting procedural disenrollments as a share of total disenrollments isolates procedural disenrollments and can help to identify systems or other issues. High procedural disenrollment rates using this methodology may reflect problems with mail delivery, backlogs in processing returned forms, or problems complying with federal regulations related to processing redeterminations. In contrast, states with lower procedural disenrollments as a share of total disenrollments may have more effective processes and procedures for contacting enrollees; they may provide a longer timeframe for enrollees to respond; or they may have more robust systems that streamline the process for returning renewal forms or submitting documentation.
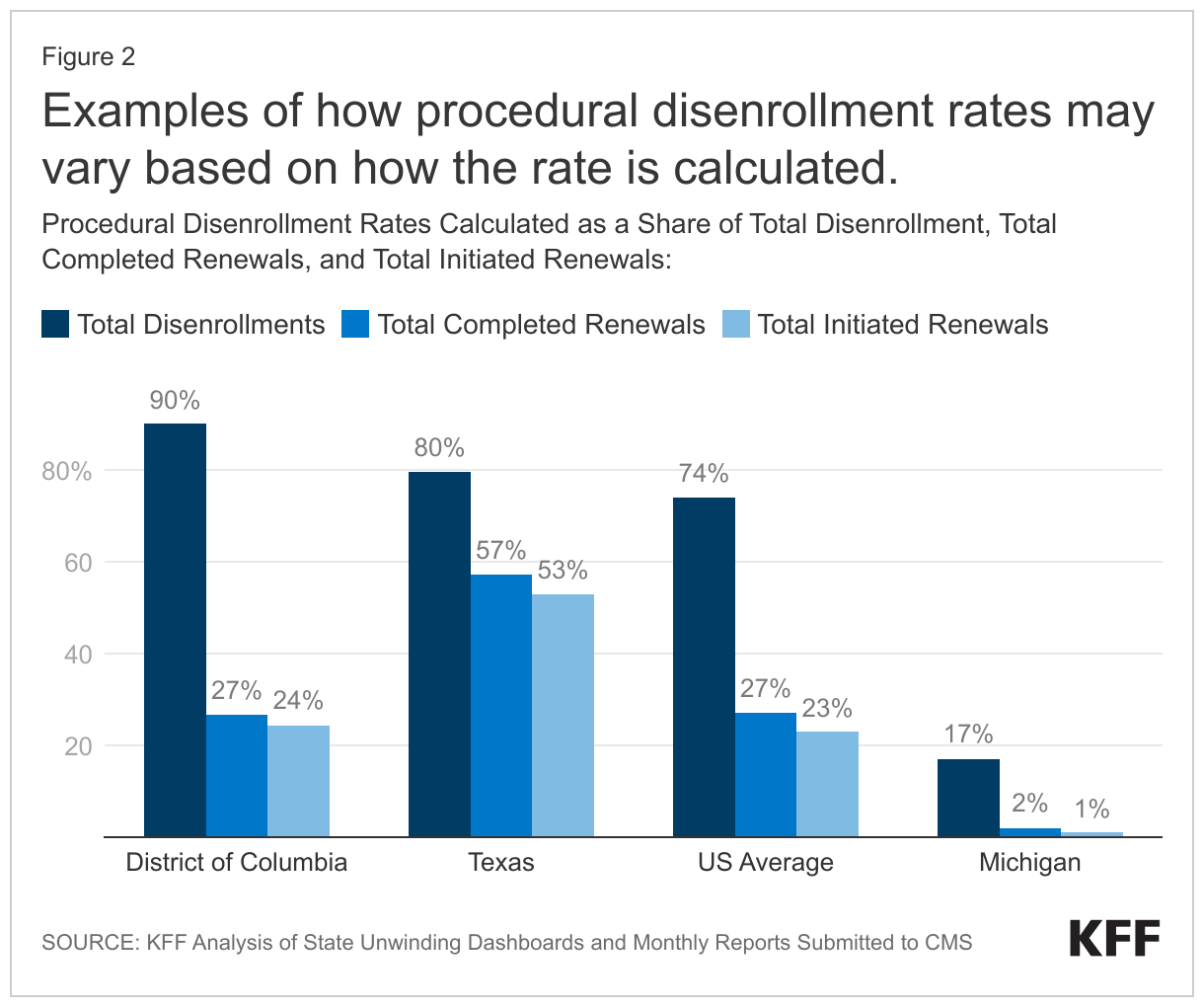
Examining procedural disenrollments as a share of people renewed or the share of all initiated renewals can provide important context for understanding the data. States that are renewing large shares of people each month or that are holding redetermination cases open to give enrollees more time to respond may have lower overall disenrollment rates, even if their procedural disenrollment rates as a share of total disenrollments are high. An example is the District of Columbia, which has a 90% procedural disenrollment rate as a share of total disenrollments that drops to just 27% when calculated as a share of total completed renewals because DC is renewing coverage for 70% of enrollees (Figure 2). While some states, such as Texas, have procedural disenrollment rates that are higher than the national average for each measure, other states, such as Michigan, have rates that are lower.
How are CMS and states addressing high procedural disenrollment rates?
CMS has sent letters to states identifying concerns with high procedural disenrollment rates and potential systems issues contributing to inappropriate procedural terminations. On August 9, 2023, CMS sent letters to states expressing general concern over procedural disenrollment rates and urging states to take action to reduce those rates. CMS flagged 28 states where the agency deemed the procedural disenrollment rate to be too high. The rates reported in the letters were for May 2023 only, using total renewals initiated in the month as the denominator, and CMS defined a high procedural disenrollment rate as greater than 10%, More recently, CMS sent a letter to state Medicaid Directors on August 30, 2023 identifying a potential issue related to how some states are processing ex parte renewals (i.e., renewals that make use of electronic data sources documenting income and other circumstances) that could be contributing to inappropriate procedural terminations for some individuals, including children. According to the letter, any state that is out of compliance with federal rules must implement a mitigation strategy until the issue is fixed, reinstate coverage for all individuals who were improperly terminated for procedural reasons, and pause procedural disenrollments for individuals who may be affected.
Most states have adopted at least some of the flexibilities CMS has made available during the unwinding period aimed at reducing procedural disenrollment rates. More recently but prior to the release of the CMS letters, some states extended renewal notice timelines by 30 days to give people additional time to respond and to give states additional time to reach out to enrollees who have not yet responded. Other states temporarily paused procedural disenrollments for certain cohorts or for all enrollees. In light of the recent CMS letters, states can be expected to adopt additional strategies to reduce procedural disenrollments.