Could Consumer Assistance be Helpful to People Facing Medical Debt?
A recent KFF Health Care Debt Survey finds that most adults (57%) have experienced owing money due to medical or dental bills at some point in the past 5 years. Among insured adults under age 65, the figure is 61%. Serious health consequences may result from health care debt as many in debt are denied services or skip care to avoid further bills; and financial consequences can also be severe, including depletion of savings, going without other household needs, and damage to credit scores. Many adults with health care debt say they received a medical or dental bill that they thought contained an error and most say a state consumer assistance program would be helpful to them.
Billing Errors Confound Consumers and Cause Debt
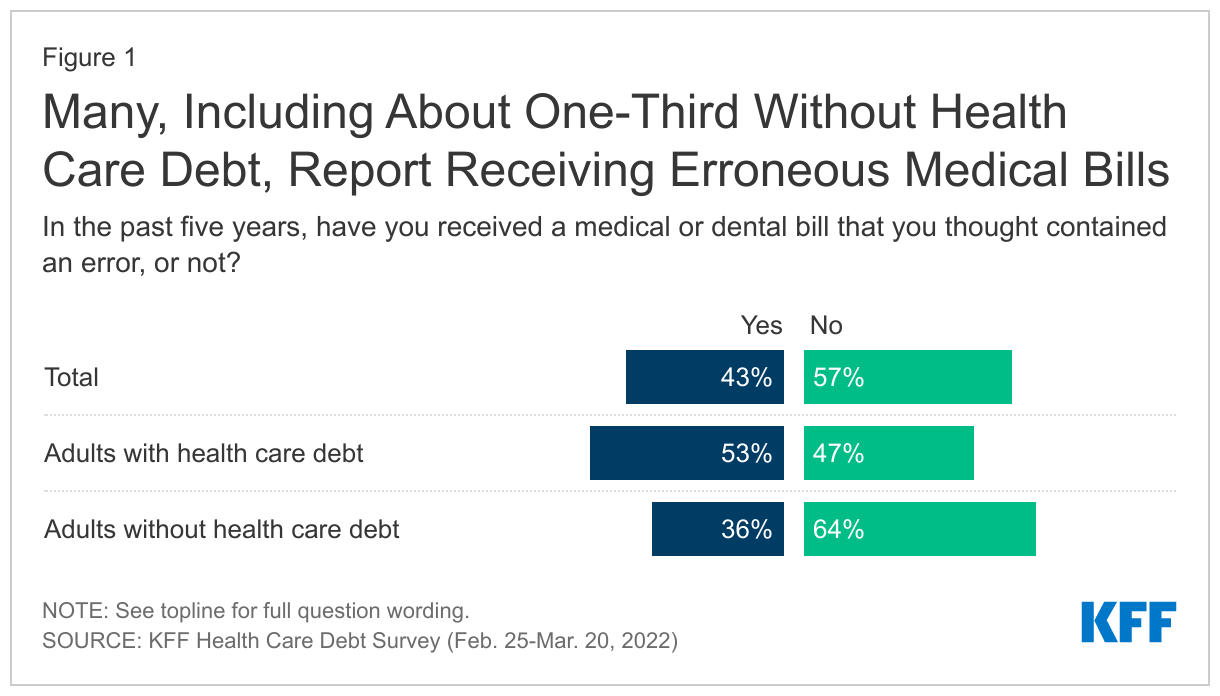
The KFF Survey found that a majority (53%) of adults with health care debt, and 43% of all adults, say they have received a medical or dental bill they thought contained an error. (Figure 1) About two-thirds of these adults say the error involved being billed for something that should have been covered by their health insurance. Other provider errors were also reported, including being billed for services never received or for bills that had already been paid.
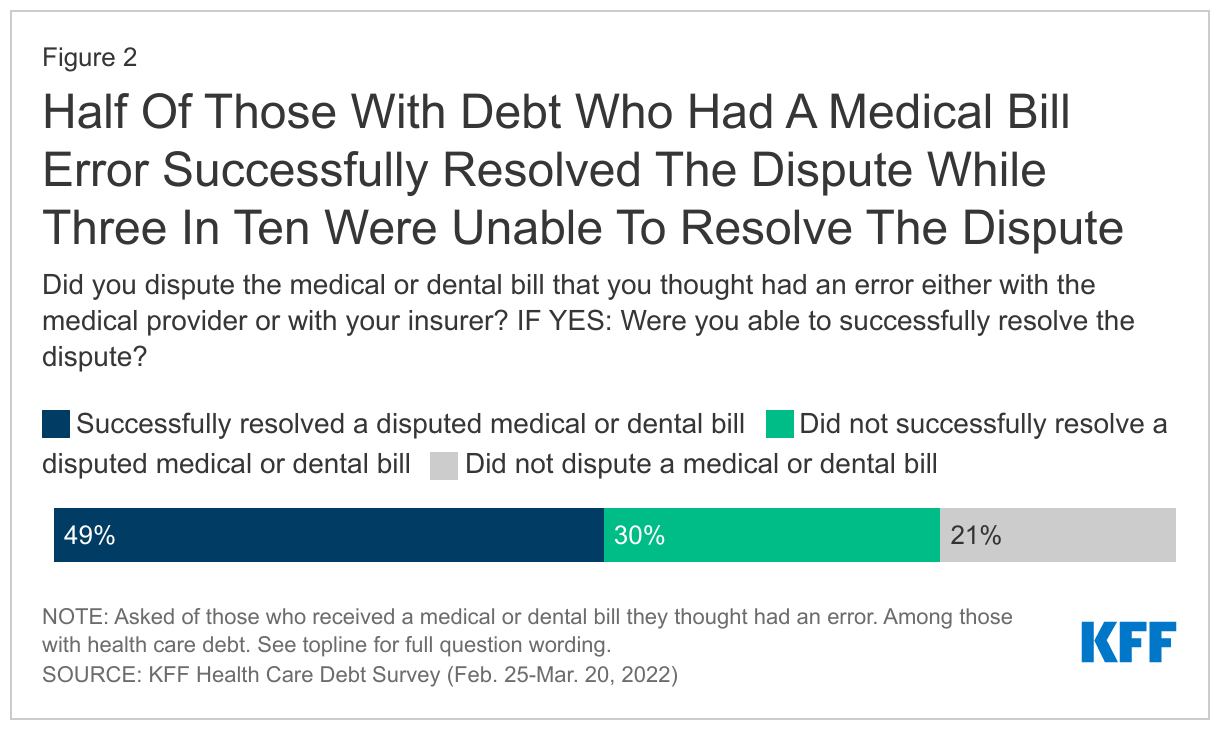
The vast majority (79%) of adults with health care debt who say they received a bill that contained an error took some action to dispute the mistake with their insurer or provider, and in many cases they succeeded in resolving the mistake. However, 51% of all adults with health care debt who received an erroneous bill either could not successfully fix the disputed bill or did not even try to dispute it in the first place. (Figure 2) In addition, about a third (32%) of adults with health care debt who received a bill they thought had an error say they have had a disputed bill sent to collections, which can have a significant impact on their credit score and their future access to credit, loans and financing.
Consumers Want Help With Billing and Claims Errors
The KFF survey asked adults about policy interventions to address or assist those with health care debt, including State-Consumer Assistance Programs (CAPs). CAPs were established in 2010 to help individuals, including those with employer coverage, resolve problems with insurance providers and disputed medical bills. By law, CAPs not only help consumers file appeals and resolve billing disputes, they report data to regulators on consumer experiences to inform oversight. However, Congress has not provided funding for CAPs since the initial appropriation of $30 million in 2010. As a result, a few programs have since closed their doors; most others operate on state funding and other outside resources, though they could help more people if federal funding resumed.
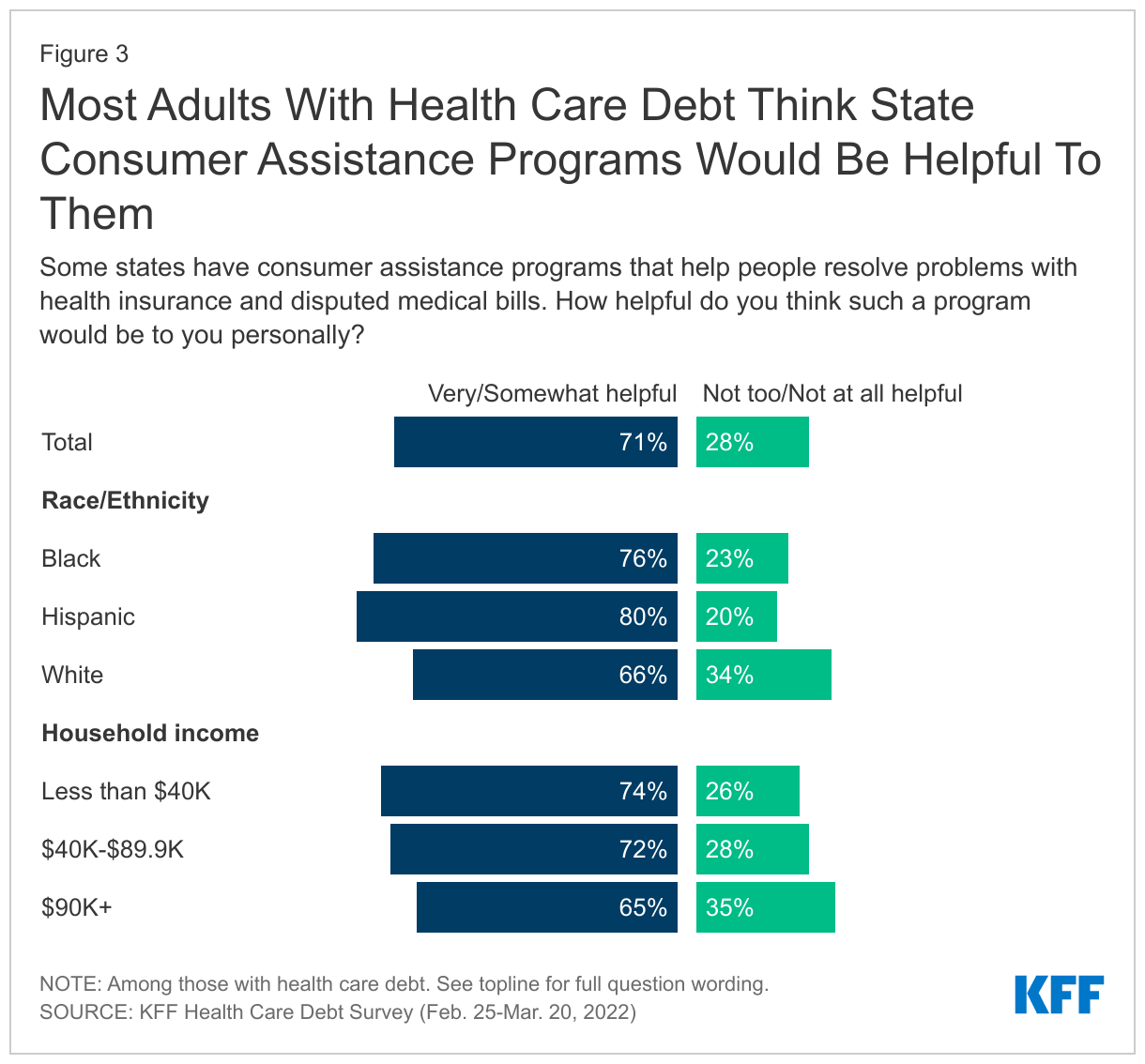
The KFF survey finds that seven in ten adults with health care debt say they think a CAP could be helpful to them personally. Black (76%) and Hispanic (80%) adults with debt were more likely than their White counterparts to think these programs could have helped. (Figure 3)
A report on the first year operations of CAPs found they saved consumers millions of dollars by resolving health coverage disputes. Subsequent reports by several state CAPs show programs still in operation continue to help consumers save millions in medical bills each year; for some CAPs, assisting consumers with medical debt has become a major focus.
In recent years Congress has taken other steps – including the No Surprises Act – to strengthen health insurance protection and limit patients’ exposure to out-of-pocket medical bills. However, protections may effectively be limited if consumers aren’t aware of their new rights or how to pursue them – for example, another recent KFF poll found nearly 8 in 10 adults know little or nothing about this new law. CAPs were established to educate consumers about health insurance and their protections and to provide expert help resolving problems that arise. Such help would be welcomed by most consumers, though funding for it continues to compete against other priorities.