Potential Impacts of Increased Immigration Enforcement on School Attendance and Funding
Introduction
Immigrants and their children form a growing share of the U.S. population and, as of 2023, there were over 47 million immigrants residing in the country, accounting for 14% of the total population. Regardless of their countries of birth, about three in four (77%) immigrant adults say they moved to the U.S. for a better future for their children. Research shows that children of immigrants attain higher educational outcomes than the children of U.S.-born parent(s), play an outsized role in the U.S. health care workforce, and contribute more in taxes on average than the rest of the U.S.-born population. Actions being undertaken by the federal government to restrict immigration, including attempts to end birthright citizenship, rescission of protections from immigration enforcement in schools, and plans to carry out mass deportation, could negatively impact children living in immigrant families and have longer-term ramifications for the U.S. workforce and economy. Some states have also proposed actions to verify student immigration status in schools, which could further exacerbate fears and challenges among children in immigrant families.
Recent reports indicate that immigrant families are scared to send their children to school and that there have been declines in school attendance among children in immigrant families since President Trump took office. Declines in school participation and performance may not only negatively influence children’s educational outcomes and health but may also have impacts on school funding. This brief presents research on the impacts of immigration enforcement on children, including school attendance and performance; provides data on the share and number of school-aged children by state who live in immigrant families based on KFF analysis of the 2023 American Community Survey (ACS); and discusses potential implications of declines in school enrollment and/or attendance among these children on school funding. Key takeaways include:
- Increased immigration enforcement can increase absenteeism and negatively impact academic outcomes and student health. Research shows that increased immigration enforcement in schools is associated with chronic absenteeism, drops in school enrollment, exacerbation of racial and/or ethnic disparities in student outcomes, and negative physical and mental health outcomes among children in immigrant families, who are predominantly U.S.-born. Negative impacts on education may also have consequences for children’s long-term health. Adults with higher educational attainment tend to have longer life spans and be healthier than their counterparts with lower educational attainment. High educational attainment also is associated with better jobs that are more likely to provide employer-sponsored health coverage and higher incomes which, in turn, improve access to health care and resources to support health.
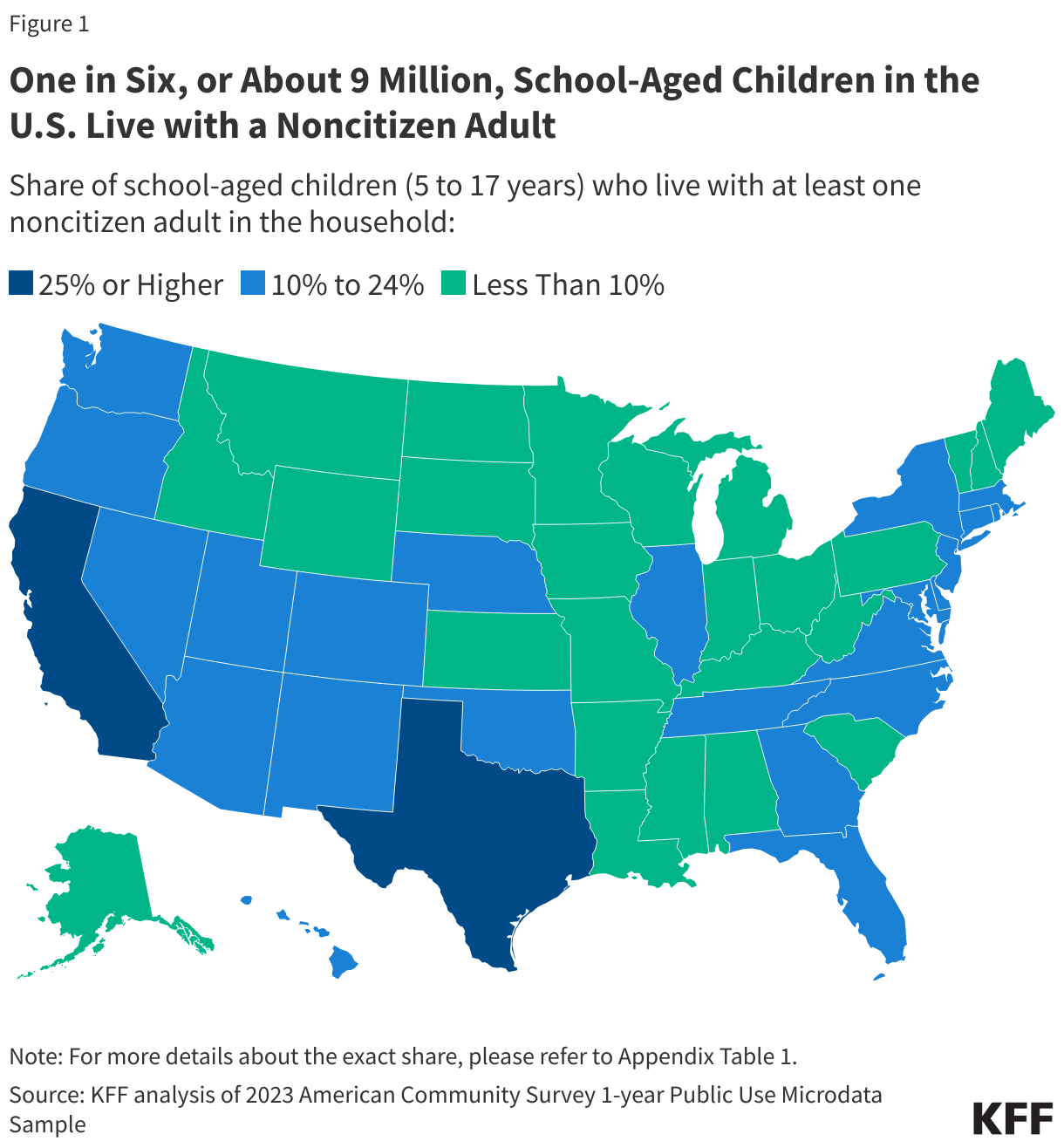
- Nationwide, about one in six (17%) or 9 million, school-aged children (5 to 17 years old) live in a household with at least one noncitizen adult, who could be impacted by immigration enforcement fears. This share increases to one in three (32%) school-aged children in California and about one in four in Texas (25%), New Jersey (24%), and Nevada (23%).
- Increases in absenteeism or decreased enrollment arising from enhanced immigration enforcement activity could lead to decreases in school funding. Public schools in the U.S. are primarily funded through a combination of state and local funding. Each state has its own formula for funding school districts, but they all are directly or indirectly based on the number of students served by a school district as determined through student attendance or enrollment. Schools in states that use attendance-based models to determine student counts for school funding may be particularly affected by increases in absenteeism or decreases in enrollment due to immigration-related fears. These states include California and Texas, which are home to the largest shares of school-aged children living in immigrant families. While the overall decrease in funding may be relatively small, school districts that serve large shares of students from immigrant families may be more heavily impacted by funding cuts.
- Schools may also face increased challenges addressing fears among children in immigrant families to prevent declines school performance and negative impacts on health. Some teachers and schools are working to mitigate negative impacts of increased immigration-related fears among families by preparing safety plans, establishing policies for dealing with ICE encounters, and providing families information about their legal rights.
Background
President Trump has increased immigration enforcement efforts, which have impacts across immigrant families, including the millions of U.S. citizen children living in them. These efforts include a slew of immigration policy changes focused on restricting both lawful and unlawful immigration into the U.S., increasing interior enforcement to support mass deportation, attempts to end birthright citizenship for the children of noncitizen immigrants, and rescinding protections against enforcement action in previously protected areas such as schools and health care facilities. KFF analysis shows that one in four, or 19 million, children in the U.S. have an immigrant parent, and the vast majority of these children are U.S. citizens. About one in ten (12%) children in the U.S. are citizen children with a noncitizen parent. Other analysis estimates that about 4.4 million U.S.-born children live with an undocumented immigrant parent.
Research shows that enhanced immigration enforcement actions have a wide array of impacts on children, including on school attendance and performance and mental and physical health. Specifically, research shows that increased immigration enforcement can lead to chronic absenteeism, drops in school enrollment (including among U.S.-born students), as well as increases in students’ moving out of school districts with high enforcement. Further, increased immigration enforcement is associated with “declines in academic achievement”, an exacerbation of racial and ethnic gaps in educational outcomes, feelings of lack of safety in schools, and negative mental and physical health outcomes among children of immigrants. Negative impacts on education may also have consequences for children’s long-term health. Adults with higher educational attainment tend to have longer life spans and be healthier than their counterparts with lower educational attainment. High educational attainment also is associated with better jobs that are more likely to provide employer-sponsored health coverage and higher incomes which, in turn, improve access to health care and resources to support health.
Recent reports indicate that immigrant families are scared to send their children to school and that there have been declines in school attendance among children in immigrant families since President Trump took office. Schools, which were historically considered to be “safe” spaces, are now within the purview of immigration enforcement following the Trump administration rescinding protections against enforcement action there. Recent reports suggest declines in school attendance due to immigration-related fears. In the Boston-area, reports suggest that over 1,000 students did not show up to school following news of Immigration and Customs Enforcement (ICE) activity nearby, similar to Fresno, where attendance dropped by around 1,000 per day following President Trump’s inauguration. In Chicago, one educator serving immigrant families noted a nearly 50% drop in school attendance in the days immediately following President Trump’s inauguration. In some cases, there have been reports of school officials sharing information with parents about potential ICE encounters on school property which later turned out to be false. In response to growing fears among immigrant families, a number of teachers and schools are working to prepare safety plans, establishing policies for dealing with ICE encounters, and providing families information about their legal rights.
Fears and attendance declines among children in immigrant families may be exacerbated by other state-level actions. For example, Tennessee is in the process of advancing a bill “that would require public K-12 and charter schools to verify student immigration status and… bar children who cannot prove they lawfully reside in the United States unless they pay tuition.” Oklahoma also has proposed a rule that would require parents or legal guardians to provide proof of citizenship and/or immigration status for children enrolled in the state’s public schools. While Oklahoma’s proposed rule does not explicitly bar enrollment for students who may be undocumented, it is likely to cause fear among immigrant families about their immigration status being recorded and may lead to drops in student enrollment due to chilling effects. Similar bills have also been proposed by lawmakers in Texas, Indiana, and New Jersey, but it is unclear if there is a clear pathway to passage for such legislation.
Findings
This analysis uses 2023 ACS data to identify school-aged children living in a household with a noncitizen adult who could be impacted by immigration-related fears overall and by state. Additionally, it provides an overview of state school funding models based on data from the Education Commission of the States to give insight into where schools may be at particular risk for decreased funding due to declines in school attendance or enrollment.
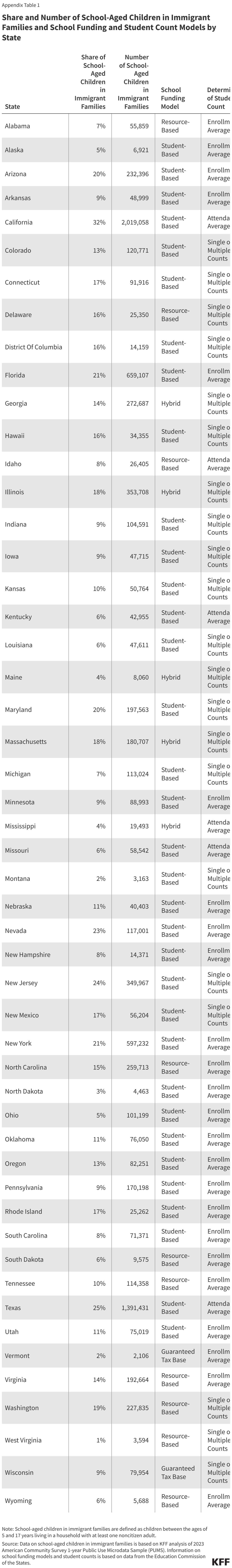
Nationwide, about one in six (17%), or 9 million, school-aged children (5 to 17 years) live in a household with at least one noncitizen adult, who could be impacted by immigration enforcement fears. This share rises to nearly one in three (32%) or 2 million school-aged children in California and about one in four school-aged children in Texas (25%), New Jersey (24%) and Nevada (23%) (Figure 1 and Appendix Table 1). By region, the West has the highest share (24%) of school-aged children in a household with at least one noncitizen adult, followed by about one in six school-aged children in the Northeast (17%) and the South (16%); and about one in ten school-aged children in the Midwest (9%). As noted, five states (Indiana, New Jersey, Oklahoma, Tennessee, and Texas) have introduced bills to verify student immigration status. Over 2 million school-aged children in these states live with at least one noncitizen adult in the household, including about one in four school-aged children in Texas (25%) and New Jersey (24%), and about one in ten in Oklahoma (11%), Tennessee (10%), and Indiana (9%).
All state school funding models are directly or indirectly tied to the number of students served by a school district. Most (35) states plus DC fund schools on a per student basis (Figure 2). In these states “districts receive a base amount of funding per student.” Nine states use a resource-based funding model, in which districts receive funds based on the resources they anticipate needing (such as teachers and supplies) depending on how many and what types of students the school districts serve. Four states use hybrid models that combine aspects of student- and resource-based funding, and two states use a guaranteed tax base model that allows districts to determine per student spending on a state-guaranteed tax base.
States employ a variety of methods to determine a district level student count for their funding models, including attendance averages, single or multiple student counts, or enrollment averages. To determine the student count that goes into funding models, six states use the average daily attendance in school districts over a year, also known as an attendance average; 20 states plus DC use student enrollment or attendance from a single day or multiple days, also known as single or multiple counts; and 24 states use the average daily enrollment in school districts over a year (or over a 20-day period in the fall in Alaska), also known as enrollment average (Figure 3). Districts in states that base student counts on attendance are more likely to have their school funding negatively impacted by short-term absenteeism among children in immigrant families due to increased immigration enforcement. These states include California and Texas, which are home to the largest shares of school-aged children in households with a noncitizen adult. Districts in states that base student counts on enrollment could also be impacted if, over the longer-term, immigrant families disenroll their children from school or move out of school districts due to immigration-related fears. While the overall decrease in funding may be relatively small, school districts that serve large shares of students from immigrant families may be more heavily impacted by funding cuts.