Sexual and Reproductive Health Related Preventive Services for Adults Covered by the ACA
Last Updated on June 27, 2025
The Affordable Care Act (ACA) requires most private health insurance plans and Medicaid ACA expansion programs to cover preventive services related to sexual and reproductive health with no cost-sharing. These include—but are not limited to—contraceptive services and supplies for women, as well as counseling and testing for sexually transmitted infections (STIs) and human immunodeficiency virus (HIV), and pre-exposure prophylaxis (PrEP) for HIV prevention.
The required services are recommended by the U.S. Preventive Services Task Force (USPSTF) and the Health Resources and Services Administration (HRSA) based on recommendations issued by the Women’s Preventive Services Initiative. The Advisory Committee on Immunization Practices recommends vaccines for adults and children that must also be covered without cost-sharing.
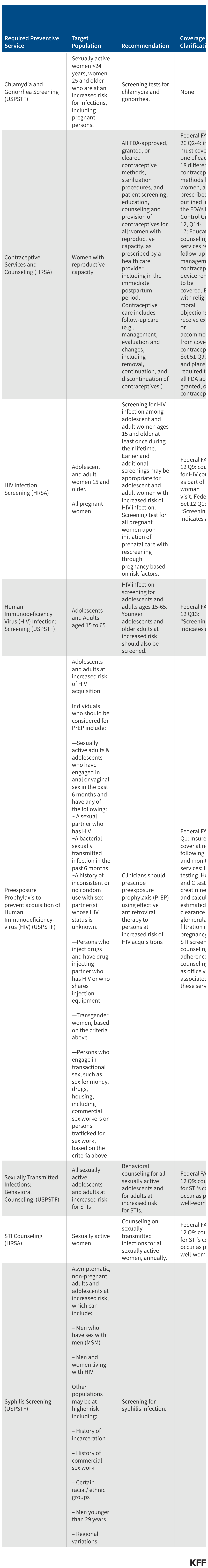
The table below presents detailed information on sexual and reproductive health related preventive services that are covered under the ACA, including a summary of the recommendation, the target population, effective date of coverage, and related coverage clarifications.