Medicare’s Role for People Under Age 65 with Disabilities
Issue Brief
Medicare was established in 1965 as the health insurance program for Americans age 65 and over; since 1973, it has also covered people under age 65 who receive Social Security Disability Insurance (SSDI) benefits.1 To qualify for SSDI, people must be unable to engage in “substantial gainful activity” because of a medically-determined physical or mental impairment expected to last at least 12 months or until death. Medicare also covers certain widows and widowers under age 65 with disabilities, as well as disabled adult children of retired, deceased, or disabled workers. Today, Medicare covers 9.1 million people with disabilities who are under age 65,2 or 16% of the Medicare population, up from 7% (1.7 million people with disabilities under age 65) in 1973.3 When people under age with disabilities on Medicare turn 65, their coverage from Medicare continues.4
How do people under age 65 with disabilities qualify for Medicare?
People under age 65 become eligible for Medicare if they have received SSDI payments for 24 months. Because people are required to wait five months before receiving disability benefits, SSDI recipients must wait a total of 29 months before their Medicare coverage begins. People under age 65 who are diagnosed with end-stage renal disease (ESRD) or amyotrophic lateral sclerosis (ALS) automatically qualify for Medicare upon diagnosis without a waiting period.5 Of those who were receiving SSDI in 2014, 34% qualified due to mental disorders, 28% due to diseases of the musculoskeletal system and connective tissue, 4% due to injuries, 3% due to cancer, and 30% due to other diseases and conditions.6
What are the characteristics of Medicare beneficiaries under age 65 with disabilities compared to beneficiaries age 65 or older?
Medicare beneficiaries under age 65 with disabilities differ from beneficiaries age 65 or older in several ways, including their demographic, socioeconomic, and health status profiles.
Income: In 2012, a much larger share of beneficiaries under age 65 with disabilities than older beneficiaries had low annual incomes (Figure 1). Nearly one quarter (24%) of younger beneficiaries with disabilities had incomes less than $10,000 per year and two-thirds (67%) had incomes less than $20,000 per year, compared to 13% and 39%, respectively, of older beneficiaries.7
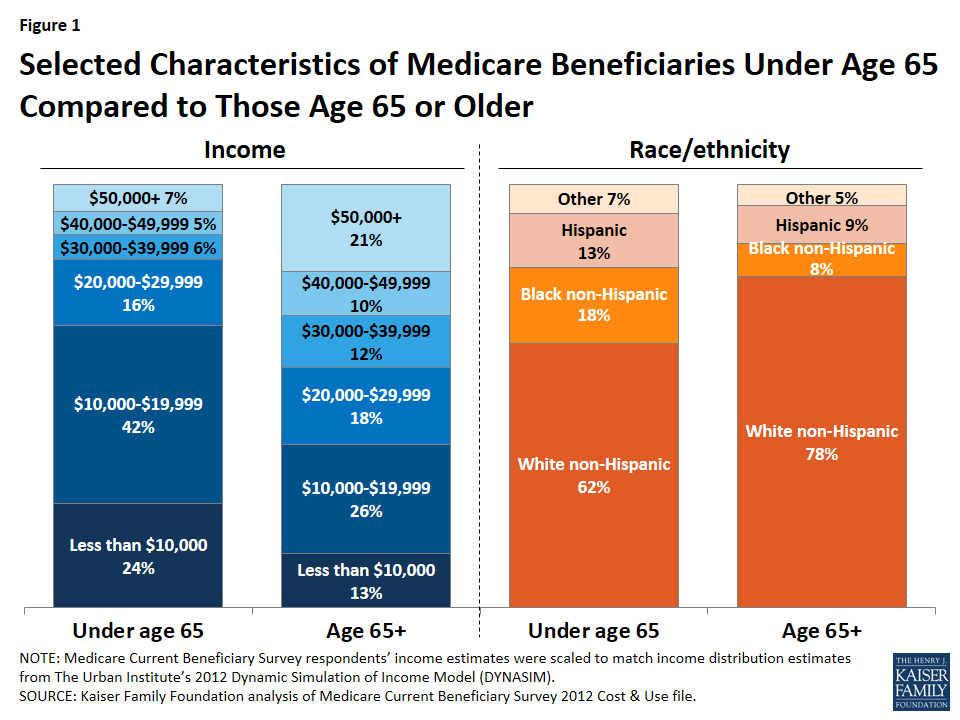
Race/ethnicity and gender: A larger share of beneficiaries under age 65 than older beneficiaries are black (18% and 8%, respectively) and Hispanic (13% and 9%, respectively), and a larger share are male (53% and 44%, respectively).
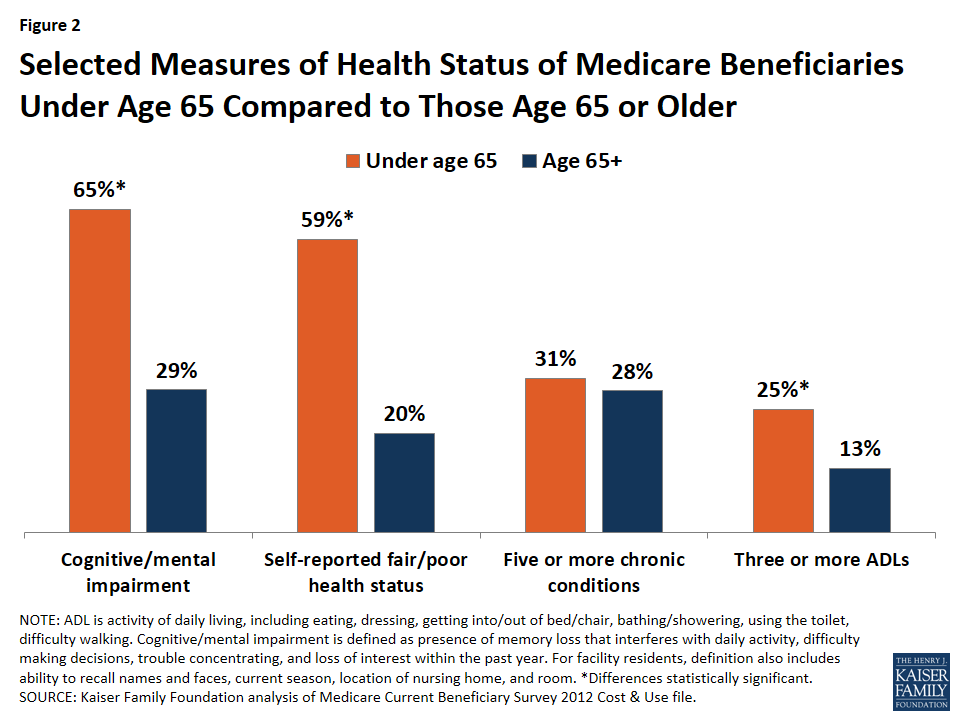
Health status: Nearly two-thirds of all younger Medicare beneficiaries (65%) had a cognitive or mental impairment in 2012, compared to 29% of older beneficiaries (Figure 2). This includes memory loss that interferes with daily activity, difficulty making decisions, trouble concentrating, and loss of interest within the past year.8 Nearly 6 in 10 (59%) reported their health status as fair or poor and almost the same share (58%) reported having one or more limitations in their activities of daily living, compared to 20% and 34% of beneficiaries age 65 or older, respectively. But roughly the same share of both younger beneficiaries with disabilities and older beneficiaries report having five or more chronic conditions (31% and 28%, respectively).
How do sources of supplemental coverage and prescription drug coverage differ for Medicare beneficiaries under age 65 with disabilities and older beneficiaries?
Supplemental coverage
Most Medicare beneficiaries, including those under age 65 with disabilities, have public or private supplemental insurance to help cover Medicare’s cost-sharing requirements.9 A much larger share of beneficiaries under age 65 with disabilities than older beneficiaries rely on Medicaid to supplement Medicare (35% versus 10%) because of their relatively low incomes (Figure 3).10 Medicaid helps with Medicare premiums and cost-sharing requirements, and covers services needed by many people with disabilities that are not covered by Medicare, particularly long-term services and supports.
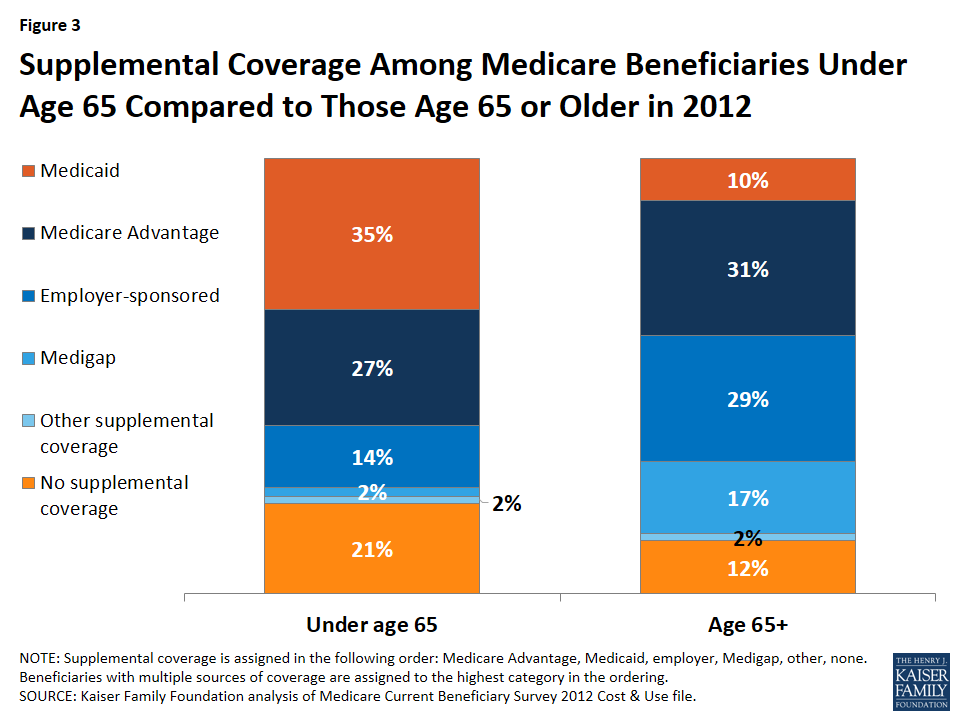
A smaller share of beneficiaries under age 65 with disabilities than older beneficiaries have employer-sponsored coverage (14% and 29%, respectively), Medigap (2% and 17%, respectively), or are enrolled in a Medicare Advantage plan (27% and 31%, respectively). A larger share of older beneficiaries have employer-sponsored coverage as a result of having retiree health benefits from former employers or because they are currently working and have Medicare as a secondary payer. The small share of beneficiaries under age 65 with disabilities who report having a supplemental Medigap policy may be largely due to the fact that federal law does not require insurance companies to sell Medigap policies to people under age 65, and while some states do impose this requirement, others do not.11 Insurers also may use medical underwriting in deciding whether to issue a Medigap policy to people with disabilities and how much to charge. By contrast, people who qualify for Medicare when they turn 65 have a six-month open enrollment period when they can purchase Medigap coverage without medical underwriting and regardless of what state they live in or their health status, as well as certain other special enrollment periods.
Just over 1 in 5 (21%) beneficiaries under age 65 has no supplemental coverage, compared with 12% of those age 65 or older. Lack of supplemental coverage among Medicare beneficiaries is associated with higher rates of access problems, but rates of access problems are higher among younger beneficiaries with disabilities who lack supplemental coverage than among older beneficiaries, including not seeing a doctor for a health problem when they think they should (31% and 10%, respectively) and having trouble getting needed health care (17% and 5%, respectively).12 Regardless of whether or not they have supplemental coverage, however, a larger share of younger beneficiaries with disabilities than older beneficiaries experience access and cost-related burdens (see discussion under “Access to Care and Cost-Related Problems” below).
Prescription drug coverage
The Medicare Part D drug benefit, which offers outpatient prescription drug coverage through private stand-alone prescription drug plans (PDPs) or Medicare Advantage drug plans (MA-PDs), is the primary source of drug coverage for all Medicare beneficiaries, but covers a larger share of those under age 65 with disabilities than older beneficiaries.
Three-fourths (75%) of Medicare beneficiaries under age 65 are enrolled in a Part D drug plan, either a stand-alone prescription drug plan (PDP) (52%) or a Medicare Advantage drug plan (24%), compared to roughly two-thirds (63%) of older beneficiaries enrolled in Part D (Figure 4). Reflecting their lower incomes and higher rate of Medicaid enrollment, more than half of all Medicare beneficiaries under age 65 (55%) receive the Part D Low-Income Subsidy (LIS), compared to just 16% of beneficiaries age 65 or older.
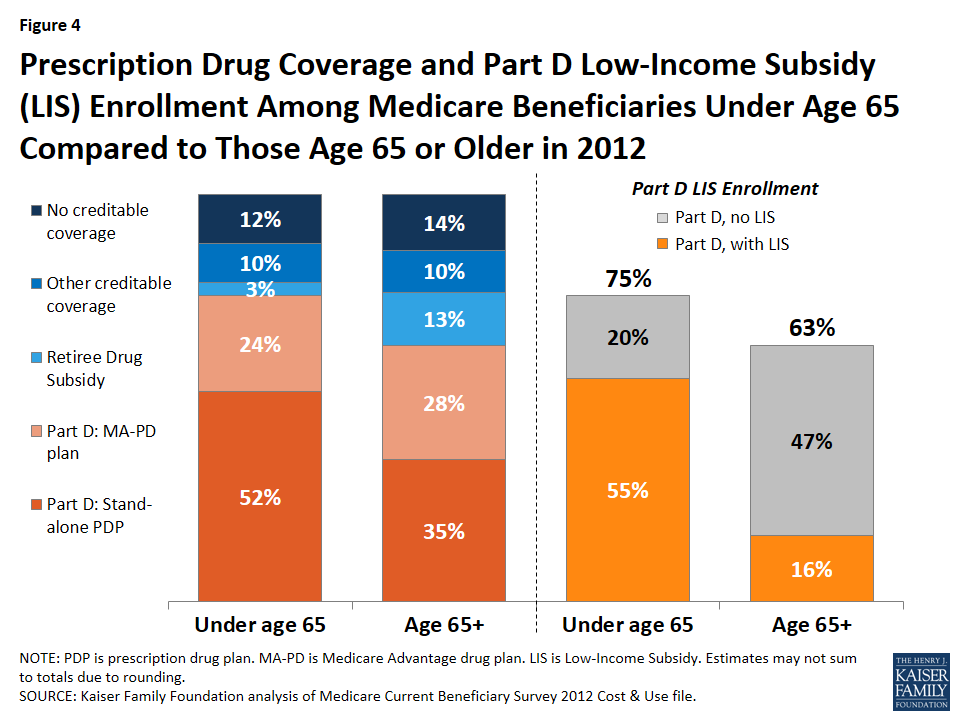
Roughly the same share of younger beneficiaries with disabilities and older beneficiaries have no reported source of creditable drug coverage (12% and 14%, respectively). Creditable coverage is drug coverage that is at least equal in value to the standard Part D benefit and can include, for example, coverage from employer-sponsored retiree health benefits, the Department of Veterans Affairs, and TRICARE.
How do Medicare spending and use of services differ for beneficiaries under age 65 with disabilities and older beneficiaries?
Medicare per capita spending
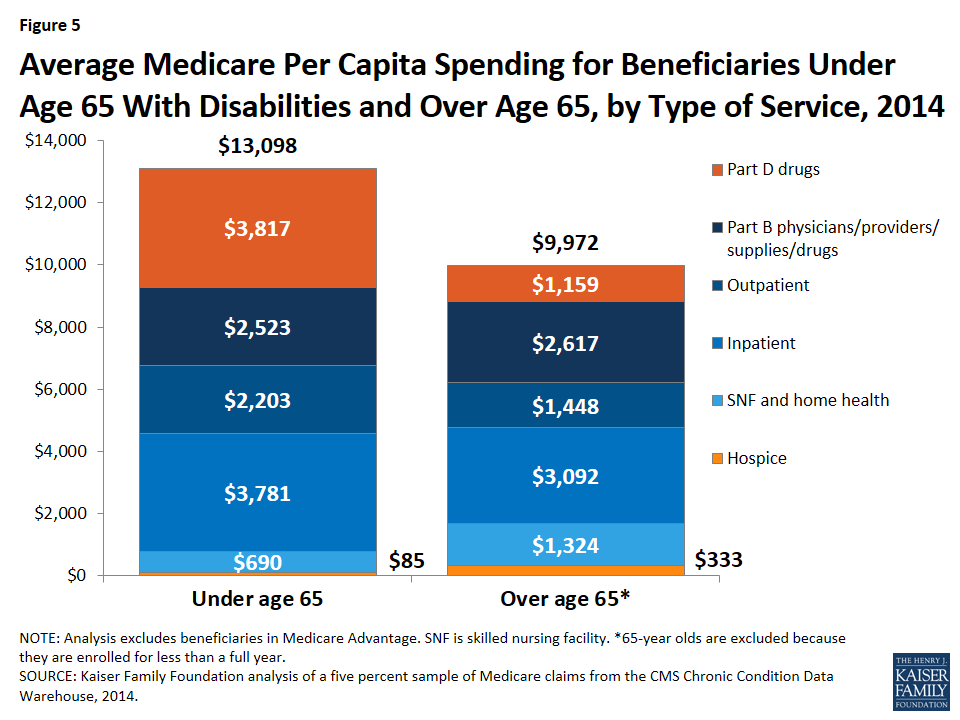
Average total Medicare spending is higher for traditional Medicare beneficiaries under age 65, mainly due to higher Part D prescription drug spending.13 Medicare per capita spending for beneficiaries younger than age 65 averaged $13,098 in 2014, nearly one third more than average per capita spending for beneficiaries over age 65 ($9,972).14 Excluding Part D drug spending, the difference narrows considerably to $9,281 for beneficiaries under age 65 and $8,814 for those over age 65, on average. On average, beneficiaries under age 65 have higher per capita spending for drugs covered under Part D and for inpatient and outpatient services, but lower spending on post-acute and hospice care than beneficiaries over age 65 (Figure 5; Table 1).
Use of medical services
Among beneficiaries in traditional Medicare in 2012,15 a somewhat smaller share of younger beneficiaries with disabilities than older beneficiaries had an office visit (66% and 77%, respectively), but a somewhat larger share of younger beneficiaries than older beneficiaries had an emergency department visit (19% and 14%, respectively) (Table 3). A smaller share of younger beneficiaries with disabilities than older beneficiaries used dental services (35% and 49%, respectively), and, as might be expected, use of post-acute care services, including skilled nursing facility stays and home health visits, was also lower among those with disabilities. But the same share of both groups had a hospital stay (18%) and the vast majority of both groups used prescription drugs (88% and 90%, respectively).
How do beneficiaries’ out-of-pocket spending and access to care differ for those under age 65 with disabilities and those age 65 and older?
Out-of-pocket spending
Although total Medicare per capita spending is higher for Medicare beneficiaries under age 65 with disabilities than for older beneficiaries, younger beneficiaries in traditional Medicare spend significantly less out of pocket, on average. This is likely due to the fact that a greater share of younger beneficiaries with disabilities than older beneficiaries have Medicaid coverage (35% and 10%, respectively16 ), as well as Part D Low-Income Subsidies (55% and 16%, respectively), that help cover their premiums and cost sharing. Overall, out-of-pocket spending by younger beneficiaries with disabilities is 40% less than that of older beneficiaries (averaging $3,706 and $6,146, respectively) (Table 2). Younger beneficiaries have lower average out-of-pocket spending than older beneficiaries for insurance premiums ($1,383 and $2,979, respectively) and for medical and long-term care services combined ($2,324 and $3,167, respectively).
On average, in 2012 beneficiaries in traditional Medicare with disabilities spent the largest share of their total non-premium out-of-pocket costs on medical providers (29%), followed by prescription drugs (26%) and long-term care facility costs (20%). These services also were the top three in terms of out-of-pocket costs for older beneficiaries, but in a different order: older beneficiaries spent the largest share of their out-of-pocket costs on facility costs (31%), followed by medical providers (24%) and prescription drugs (17%).
Access to care and cost-related problems
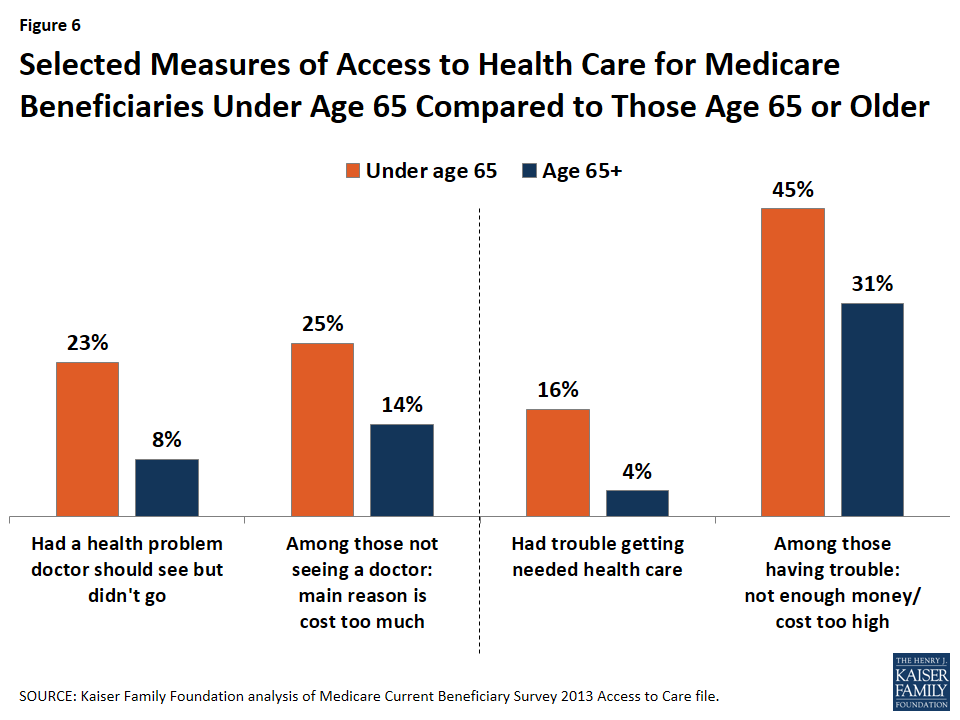
Access to care is generally good for a majority of Medicare beneficiaries overall across a number of standard measures, but a larger share of younger beneficiaries with disabilities than older beneficiaries report experiencing a range of access problems, often due to the cost of care. In 2013, nearly one quarter (23%) of younger beneficiaries with disabilities reported that they had a health problem they think a doctor should see but didn’t see a doctor about, compared to 8% of older beneficiaries. And of those not seeing a doctor, 25% of beneficiaries with disabilities cited cost as the main reason they didn’t see a doctor, compared to 14% of older beneficiaries. Also in 2013, 1 in 6 (16%) beneficiaries under age 65 with disabilities reported that they had trouble getting needed health care, compared to only 4% of beneficiaries age 65 or older. Among those reporting trouble getting care, close to half (45%) of younger beneficiaries with disabilities reported that it was because they did not have enough money or the cost was too high, compared to 31% of older beneficiaries (Figure 6).
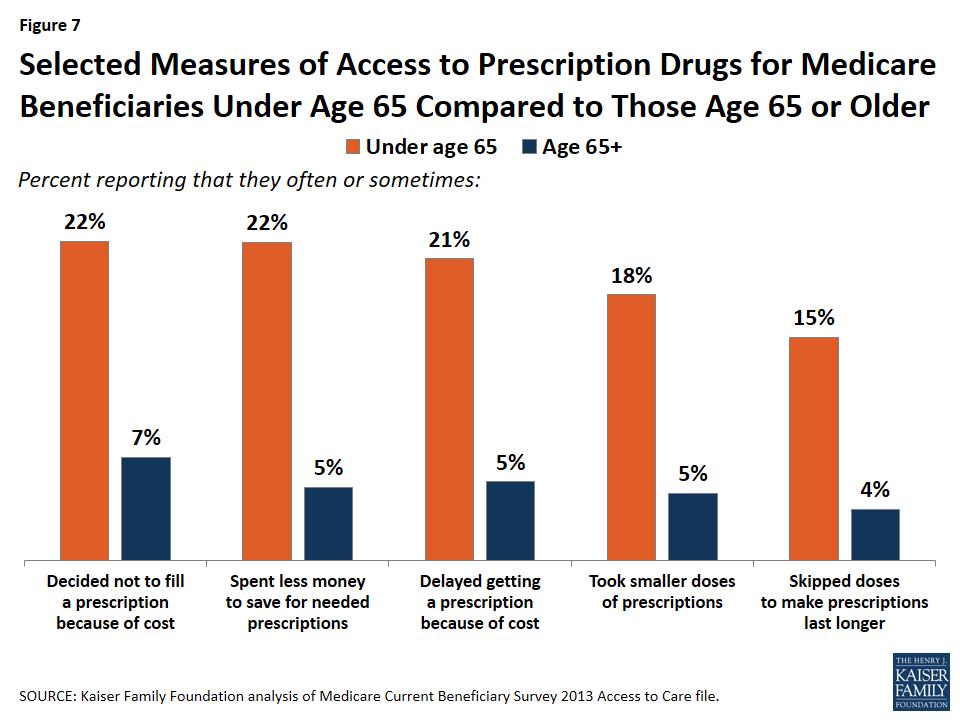
The fact that a majority of both younger Medicare beneficiaries with disabilities and older beneficiaries have some source of drug coverage does not mean that the two groups are alike in the shares facing access and cost-related problems in obtaining medications. A larger share of beneficiaries under age 65 than older beneficiaries report that they often or sometimes: decided not to fill a prescription because of cost (22% and 7%, respectively); spent less money to save for needed prescriptions (22% and 5%, respectively); delayed getting a prescription because of cost (21% and 5%, respectively); took smaller doses of prescriptions (18% and 5%, respectively); and skipped doses to make prescriptions last longer (15% and 4%, respectively) (Figure 7).
Perhaps related to their higher likelihood of experiencing cost-related access problems, a much larger share of beneficiaries with disabilities than older beneficiaries report worrying about their health more than others their age (63% and 18%, respectively), trying to keep their illnesses to themselves when they get sick (50% and 35%, respectively), and doing almost anything to avoid going to the doctor (38% and 27%, respectively).
Discussion
Since 1973, Medicare has been an important source of health insurance for people with disabilities who are under age 65. More recently, the Affordable Care Act (ACA) of 2010 improved access to health insurance and coverage of benefits under Medicare, improvements which could be especially helpful for people with disabilities. Specifically, the law expanded access to health insurance coverage through expansion Medicaid or Marketplace plans, which could be especially helpful for SSDI recipients in the 24-month Medicare waiting period. Prior to the ACA, many people with disabilities in the waiting period for Medicare faced difficulties obtaining or affording health insurance in the private market.17
For all people on Medicare, including those under age 65 with disabilities and older beneficiaries, the ACA also has helped to alleviate out-of-pocket spending burdens by phasing out the Part D coverage gap and by eliminating cost sharing for certain preventive services. Filling the coverage gap could be especially helpful for younger beneficiaries with disabilities due to their higher prescription drug costs than older beneficiaries. And for those beneficiaries who are dually eligible for Medicare and Medicaid, which includes a disproportionate share of younger beneficiaries with disabilities, the law expanded coverage of home- and community-based care, and created a new federal office to help coordinate benefits and coverage under the two programs.
Yet despite broader access to public and private coverage and improvements in Medicare benefits brought about by the ACA, people with disabilities are likely to face ongoing challenges if their coverage, including Medicare, does not provide the services and supports they need to live as independently and productively as possible. Evidence points to a consistent pattern of differences in the health care experiences of younger beneficiaries with disabilities and those of older Medicare beneficiaries, with younger beneficiaries encountering significantly more cost-related barriers to care than older beneficiaries. Given high rates of health problems and relatively low incomes among Medicare’s beneficiaries under age 65 with disabilities, the needs of this relatively vulnerable population require careful attention in ongoing Medicare policy discussions.
Juliette Cubanski and Tricia Neuman are with the Kaiser Family Foundation.Anthony Damico is an independent consultant.
Tables
| Table 1: Amount and Distribution of Medicare Per Capita Spending Overall and By Type of Service for Traditional Medicare Beneficiaries Under Age 65 and Over Age 65, 2014 | |||||
| Type of service | Part of Medicare covering service | Under age 65 | Over age 651 | ||
| Amount | Percent of total | Amount | Percent of total | ||
| Total | $13,098 | 100.0% | $9,972 | 100.0% | |
| Part D drugs | D | 3,817 | 29.1% | 1,159 | 11.6% |
| Acute inpatient hospital | A | 3,141 | 24.0% | 2,722 | 27.3% |
| Outpatient hospital | A | 2,203 | 16.8% | 1,448 | 14.5% |
| Other inpatient hospital | A | 640 | 4.9% | 369 | 3.7% |
| Evaluation & management | B | 503 | 3.8% | 459 | 4.6% |
| Other Part B procedures | B | 370 | 2.8% | 524 | 5.3% |
| Skilled nursing facility | A | 366 | 2.8% | 826 | 8.3% |
| Physician office services | B | 365 | 2.8% | 416 | 4.2% |
| Home health | A or B2 | 324 | 2.5% | 499 | 5.0% |
| Part B drugs | B | 287 | 2.2% | 360 | 3.6% |
| Tests | B | 271 | 2.1% | 239 | 2.4% |
| Durable medical equipment | B | 225 | 1.7% | 132 | 1.3% |
| Other Part B services | B | 211 | 1.6% | 164 | 1.6% |
| Imaging | B | 130 | 1.0% | 171 | 1.7% |
| Hospice | A | 85 | 0.6% | 333 | 3.3% |
| Dialysis | B | 59 | 0.5% | 13 | 0.1% |
| Anesthesia | B | 52 | 0.4% | 53 | 0.5% |
| Ambulatory surgery center | B | 50 | 0.4% | 86 | 0.9% |
| NOTE: Analysis excludes beneficiaries in Medicare Advantage. 165-year olds are excluded because these beneficiaries are enrolled for less than a full year. 2Home health services can be covered under Part A or Part B depending on whether or not the services follow a hospital stay.SOURCE: Kaiser Family Foundation analysis of a five percent sample of Medicare claims from the CMS Chronic Conditions Data Warehouse, 2014. | |||||
| Table 2: Amount and Distribution of Out-of-Pocket Spending Overall and By Type of Service for Traditional Medicare BeneficiariesUnder Age 65 and Age 65 or Older, 2012 | ||||||
| Type | Under age 65 | Age 65 or older | ||||
| Amount | Percent of total | Percent ofnon-premiumspending | Amount | Percent of total | Percent ofnon-premiumspending | |
| Total out-of-pocket spending | $3,706 | 100% | n/a | $6,146 | 100% | n/a |
| Premium out-of-pocket spending1 | 1,383 | 37% | n/a | 2,979 | 48% | n/a |
| Non-premium out-of-pocket spending | 2,324 | 63% | 100% | 3,167 | 52% | 100% |
| Medical providers | 671 | 18% | 29% | 767 | 12% | 24% |
| Prescription drugs | 605 | 16% | 26% | 548 | 9% | 17% |
| Long-term care facility | 464 | 13% | 20% | 995 | 16% | 31% |
| Dental | 203 | 5% | 9% | 359 | 6% | 11% |
| Inpatient | 149 | 4% | 6% | 103 | 2% | 3% |
| Outpatient | 140 | 4% | 6% | 156 | 3% | 5% |
| Skilled nursing facility | 87 | 2% | 4% | 110 | 2% | 3% |
| Home health | 4 | <1% | <1% | 129 | 2% | 4% |
| NOTE: Analysis excludes beneficiaries in Medicare Advantage. 1Missing out of pocket premium amounts were imputed following a hotdecking approach, stratified by categories of supplemental coverage.SOURCE: Kaiser Family Foundation analysis of Medicare Current Beneficiary Survey 2012 Cost & Use file. | ||||||
| Table 3: Utilization of Service by Traditional Medicare BeneficiariesUnder Age 65 and Age 65 or Older, 2012 | ||
| Type of service | Under age 65 | Age 65 or older |
| Percent using service | Percent using service | |
| Prescription drugs | 88% | 90% |
| Office visit | 66% | 77% |
| Outpatient visit | 64% | 64% |
| Dental | 35% | 49% |
| Emergency department (ED) visit | 19% | 14% |
| 2+ ED visits | 7% | 3% |
| Any inpatient stay | 18% | 18% |
| 2+ inpatient stay | 7% | 6% |
| Home health visit | 5% | 10% |
| Skilled nursing facility (SNF) stay | 2% | 6% |
| 2+ SNF stays | <1% | 2% |
| Hospice | 1% | 3% |
| NOTE: Analysis excludes beneficiaries in Medicare Advantage.SOURCE: Kaiser Family Foundation analysis of Medicare Current Beneficiary Survey 2012 Cost & Use file. | ||
Endnotes
- This provision was included in the Social Security Amendments of 1972, with Medicare coverage effective July 1, 1973. ↩︎
- Centers for Medicare & Medicaid Services (CMS), Office of Enterprise Data and Analysis, Office of the Actuary, CMS Fact Facts, available at https://www.cms.gov/fastfacts/. ↩︎
- CMS, 2013 Medicare & Medicaid Statistical Supplement, Table 2.1 Medicare Enrollment: Hospital Insurance and/or Supplementary Medical Insurance Programs for Total, Fee-for-Service and Managed Care Enrollees as of July 1, 2012: Selected Calendar Years 1966-2012. ↩︎
- In 2014, 4.5 million people on Medicare age 65 or older (10% of all beneficiaries age 65 or older) initially qualified for Medicare due to receiving disability insurance benefits, having end-stage renal disease, or both prior to turning age 65; based on Kaiser Family Foundation analysis of a five percent sample of 2014 Medicare claims from the CMS Chronic Conditions Data Warehouse. ↩︎
- In 2014 0.3 million people on Medicare under age 65 (3% of all beneficiaries under age 65) qualified for Medicare due to having ESRD (separate estimates for ALS are not available); based on Kaiser Family Foundation analysis of a five percent sample of 2014 Medicare claims from the CMS Chronic Conditions Data Warehouse. ↩︎
- U.S. Social Security Administration, Office of Retirement and Disability Policy, Office of Research, Evaluation, and Statistics, Annual Statistical Report on the Social Security Disability Insurance Program, 2014, November 2015, Table 6: Beneficiaries in Current-Payment Status, Distribution, by sex and diagnostic group, December 2014, available at: http://www.socialsecurity.gov/policy/docs/statcomps/di_asr/2014/. ↩︎
- We scaled respondents’ income estimates reported in the Medicare Current Beneficiary Survey to match income distribution estimates from The Urban Institute’s 2012 Dynamic Simulation of Income Model (DYNASIM). ↩︎
- This applies to Medicare beneficiaries residing in the community; for facility residents, the definition of cognitive/mental impairment also includes ability to recall names and faces, current season, location of nursing home, and room. ↩︎
- We assign supplemental coverage in the following order: Medicare Advantage, Medicaid, employer, Medigap, other, none. Beneficiaries with multiple sources of coverage are assigned to the highest category in the ordering. ↩︎
- Our methodology of assigning supplemental coverage in a hierarchical manner understates the share of beneficiaries with Medicaid, since those who also have Medicare Advantage are included in that coverage group. In 2012, a total of 45% of beneficiaries under age 65 with disabilities and 14% of beneficiaries age 65 or older were dually-eligible for Medicare and Medicaid. ↩︎
- See https://www.medicare.gov/supplement-other-insurance/when-can-i-buy-medigap/when-can-i-buy-medigap.html; see also Kaiser Family Foundation, “Medigap: Spotlight on Enrollment, Premiums, and Recent Trends,” April 2013, available at https://modern.kff.org/medicare/report/medigap-enrollment-premiums-and-recent-trends/. ↩︎
- Kaiser Family Foundation analysis of the Medicare Current Beneficiary Survey 2013 Access to Care file. ↩︎
- Analysis of per capita Medicare and out-of-pocket spending among beneficiaries enrolled in Medicare Advantage plans is not possible due to lack of or insufficient data. ↩︎
- Juliette Cubanski, Tricia Neuman, and Anthony Damico, “Similar But Not the Same: How Medicare Per Capita Spending and Service Use Compares for Younger and Older Beneficiaries,” Kaiser Family Foundation, August 2016, available at https://modern.kff.org/medicare/issue-brief/similar-but-not-the-same-how-medicare-per-capita-spending-compares-for-younger-and-older-beneficiaries. ↩︎
- Analysis of service use among beneficiaries enrolled in Medicare Advantage plans is not possible due to lack of data. ↩︎
- Irrespective of the supplemental coverage hierarchy, these estimates are 45% and 14%, respectively. See endnotes 9 and 10. ↩︎
- Juliette Cubanski and Tricia Neuman, “Medicare Doesn’t Work As Well for Younger, Disabled Beneficiaries As It Does for Older Enrollees,” Health Affairs, September 2010, vol. 29 no. 9 1725-1733. ↩︎