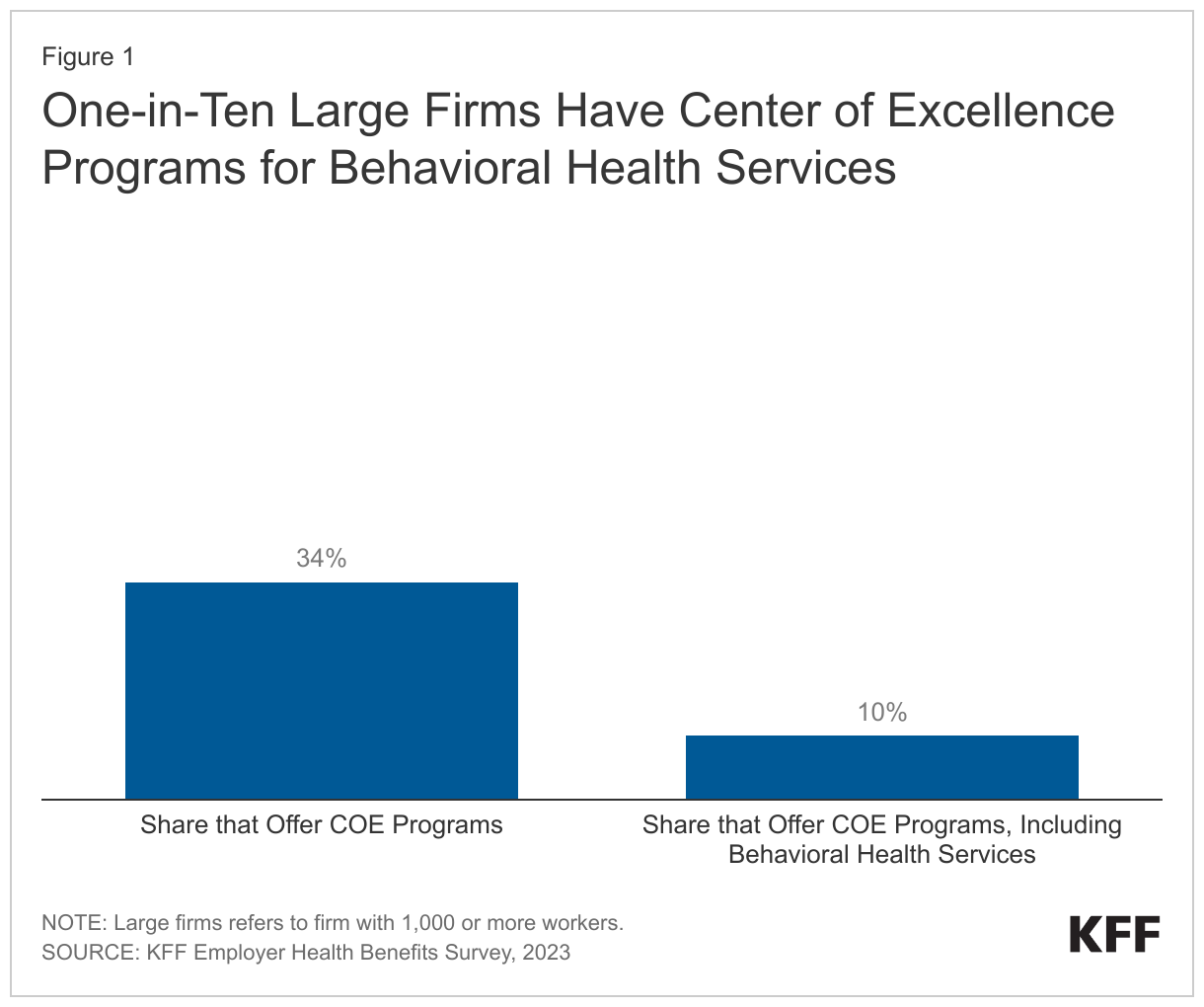
Employers Use of Center of Excellence Programs as a Pathway for Behavioral Health Services
A growing number of employer-sponsored health plans use Center of Excellence (COE) programs as a way to provide enrollees with specialized care for selected health services. COE programs designate providers or facilities based on cost and quality of the care they deliver. Providers participating in COE programs often specialize in selected services, and may provide additional case management and other support services for patients. Participating providers may be chosen based on the outcomes they achieve, such as lower readmission rates, or because they have earned additional accreditations. Plans vary in how they structure their COE programs, with some plans limiting coverage to providers participating in the COE, and others providing lower cost-sharing for enrollees to use a provider within the program. KFF’s 2023 Employer Health Benefits Survey asked employers about the COE programs included in their largest plans, including those focusing on behavioral health services (these include mental health and substance use disorder services).
In 2023, 34% of large firms (firms with 1,000 or more employees) reported sponsoring COE programs, with a higher share (45%) reported among the largest firms (firms with 5,000 or more employees). Firms may sponsor a variety of COE programs for different services. Many of these large firms (firms with 1,000 or more employees) with COE programs reported offering programs for behavioral health services. Among large firms with COE programs, 29% reported offering behavioral health services (this includes 25% offering mental health services and 25% offering substance use services). In other words, one out of ten large firms have a COE program that includes at least some behavioral health services (Figure 1). It should be noted that 13% of large firms with COE programs did not know whether their programs included any of the services listed in KFF’s EHBS survey (bariatric surgery, mental health, substance use, back or spine surgery, or joint replacement).
Among large firms (firms with 1,000 or more employees) with a COE program, approximately one-quarter (27%) reported adding a new COE program within the last two years. However, it is not known whether these newly added services pertain to mental health or substance use treatment.
COE programs have often been used for high-cost specialized surgeries, such as transplant, spinal or bariatric surgeries. In recent years several insurers have established COE programs for mental health and substance use disorders, such as programs for autism, eating disorders and residential addiction services. COE programs may limit in-network coverage for select services to a smaller group of providers than participate in the provider network overall. While this may allow enrollees to access more providers who have additional specialized capacities, or achieved outcomes for specific services, enrollees may also face certain limitations. For example, with a limited number of providers, enrollees may have difficulty with timely access to services; and enrollees who prefer providers that do not participate in COE programs may face higher out-of-pocket costs.
A recent report to Congress on federal agency implementation of certain provisions of the Mental Health Parity and Addiction Equity Act (MHPAEA) noted a new enforcement focus on illegal exclusions of coverage for residential treatment and specific treatments for autism. This along with increased scrutiny of behavioral health provider network composition may have resulted in employers adding these services to their benefit packages. Center of Excellence programs might be one way employers have attempted to control costs and channel patients to specific behavioral health providers and residential treatment centers.