Health Insurer Financial Performance in 2024
Introduction
The largest private health insurance companies often offer plans in multiple markets, including the Medicare Advantage, Medicaid managed care, individual (non-group), and fully-insured group (small and large employer) health insurance markets. Each market has unique features, including eligibility, payment, and coverage rules, which affect insurers’ overhead and potential profit. In recent years, private insurers are playing a growing role in public insurance programs, with more than half of eligible Medicare beneficiaries enrolled in a private Medicare Advantage plan and more than three-quarters of Medicaid enrollees obtaining coverage through a managed care plan (typically a private insurer).
This brief examines two measures of financial performance – gross margins and medical loss ratios – in the Medicare Advantage, Medicaid managed care, individual, and fully insured group health insurance markets using data reported by insurance companies to the National Association of Insurance Commissioners (NAIC) and compiled by Mark Farrah Associates, through the end of 2024 (the most recent year of annual data). The Medicare Advantage market is made up of around 33M people in 2024. In comparison, this is less than half of the population for Medicaid managed care and about 70% of the size of the fully insured group market. However, the Medicare Advantage market is about 1.4 times larger than the individual market.
In 2024, per enrollee gross margins in dollars were highest in the Medicare Advantage market, and medical loss ratios (measured as percentages) were lowest in the individual insurance market. In 2024, the Medicaid managed care market had both the lowest gross margins per enrollee and highest medical loss ratio. While both gross margins and medical loss ratios are indicators of financial performance, higher margins and lower loss ratios (as they are calculated in this analysis) do not necessarily translate into greater profitability since they do not account for administrative expenses or tax liabilities. Additionally, the increasingly complex structure of insurance companies, including the rise in consolidation and vertical integration, and role of subsidiaries, make it difficult to isolate the revenues and expenses associated with a particular insurance market. (A detailed description of each market is included in the Appendix).
Measures of Financial Performance in 2024
Gross margins
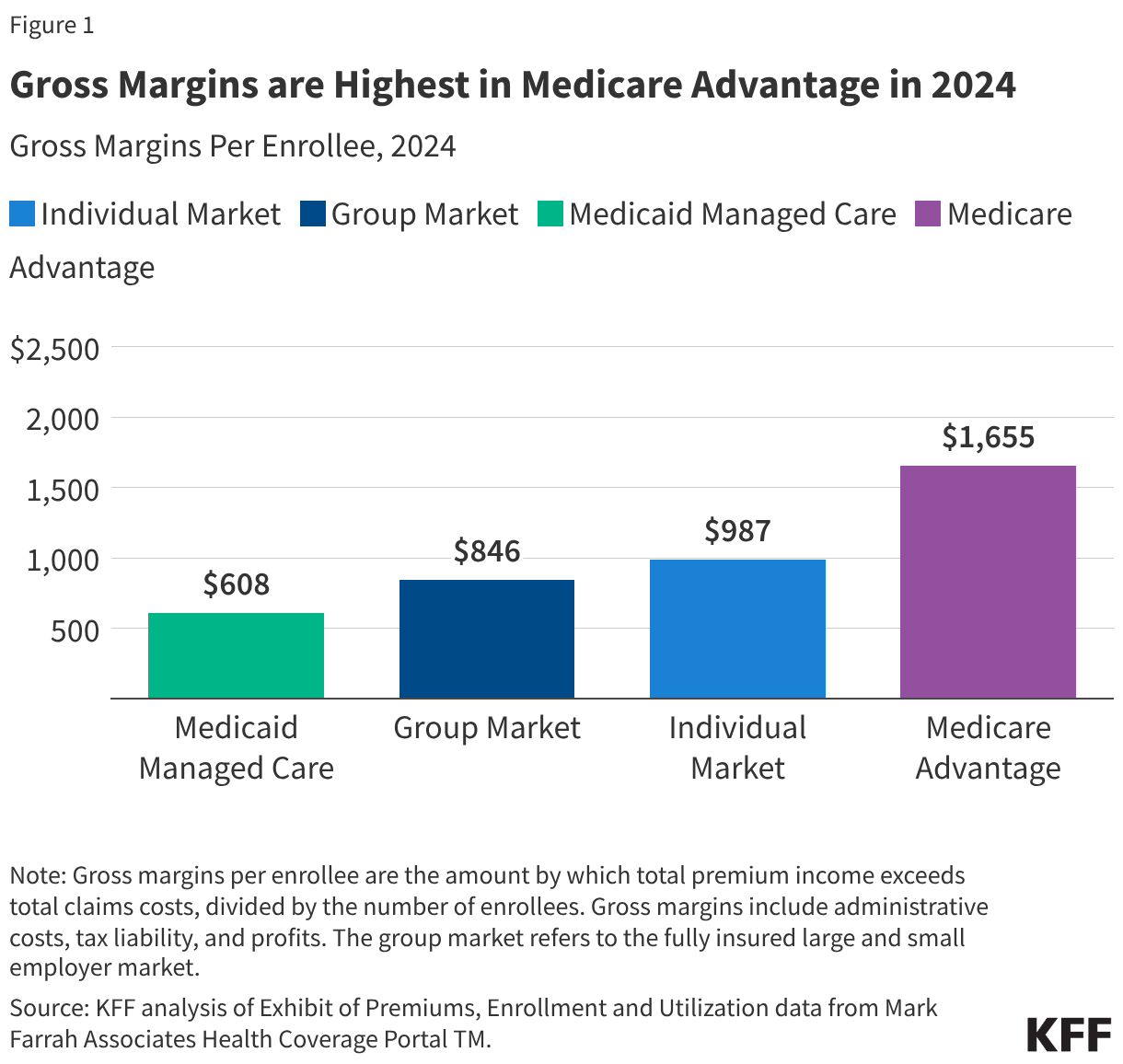
The gross margin per enrollee is the amount by which total premium income exceeds total claims costs per person over a specified time period (i.e., per year).
At the end of 2024, gross margins per enrollee ranged from $608 in the Medicaid managed care market to $1,655 in the Medicare Advantage market. Gross margins per enrollee in the group market was $846, roughly half the level observed among Medicare Advantage plans on average. Per enrollee gross margins in the individual market in 2024 amounted to $987. The level of margins reflects, in part, the overall health needs and spending in a market segment. A similar margin in percentage terms will translate to a higher margin in dollars per enrollee when average health expenses are higher.
Medical loss ratios
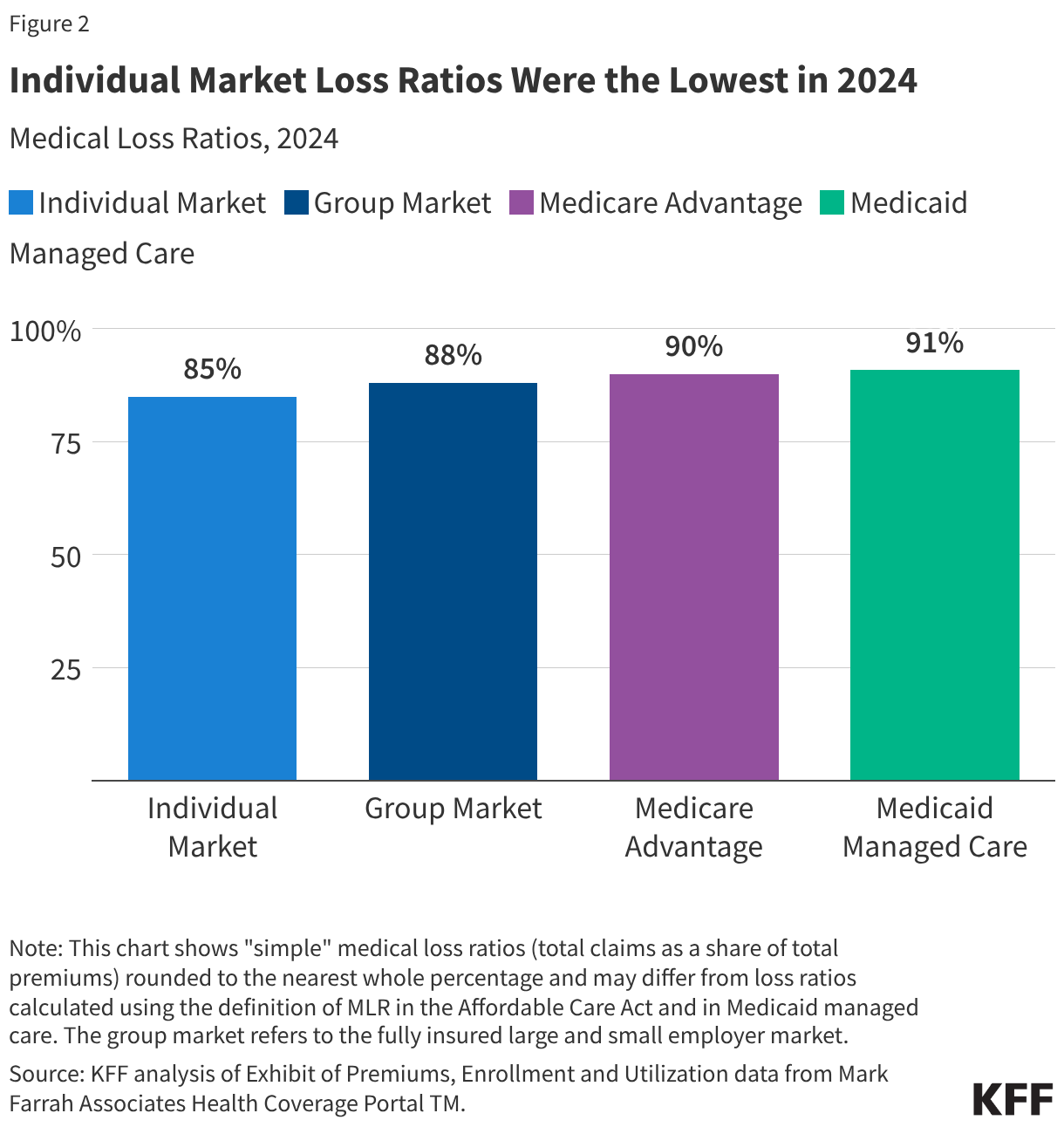
Another way to assess insurer financial performance is to look at medical loss ratios (MLRs), or the percent of premium income that insurers pay out in the form of medical claims. Generally, lower MLRs mean that insurers have a higher share of income remaining after paying medical costs to use for administrative costs or keep as profits. Each health insurance market has different administrative needs and costs, so a lower MLR in one market does not necessarily mean that market is more profitable than another market.
MLRs are used in state and federal insurance regulation in a variety of ways. In the commercial insurance (individual and group) markets, insurers must issue rebates to individuals and businesses if their MLRs fail to reach minimum standards set by the ACA. Medicare Advantage insurers are required to report MLRs at the contract level (which typically combines multiple plans) and are required to issue rebates to the federal government if their MLRs fall short of the required level of 85% and are subject to additional penalties if they fail to meet MLR requirements for multiple consecutive years. For Medicaid managed care organizations (MCOs), CMS requires states to develop capitation rates for Medicaid to achieve an MLR of at least 85%. There is no federal requirement for Medicaid plans to pay remittances if they fail to meet their MLR threshold, but a majority of states that contract with MCOs require remittances in at least some cases. The MLRs shown in this issue brief are simple loss ratios (claims as a share of premium income) and may differ from loss ratios calculated using the definition of MLR in the ACA and in Medicaid managed care.
In 2024, MLRs were similar between the Medicare Advantage, Medicaid managed care, and group markets. However, individual market loss ratios were lower. Simple loss ratios were around 85% in individual market, 88% in the fully insured (group) market, 90% in the Medicare Advantage market, and 91% in the Medicaid managed care market.
Trends in Gross Margins
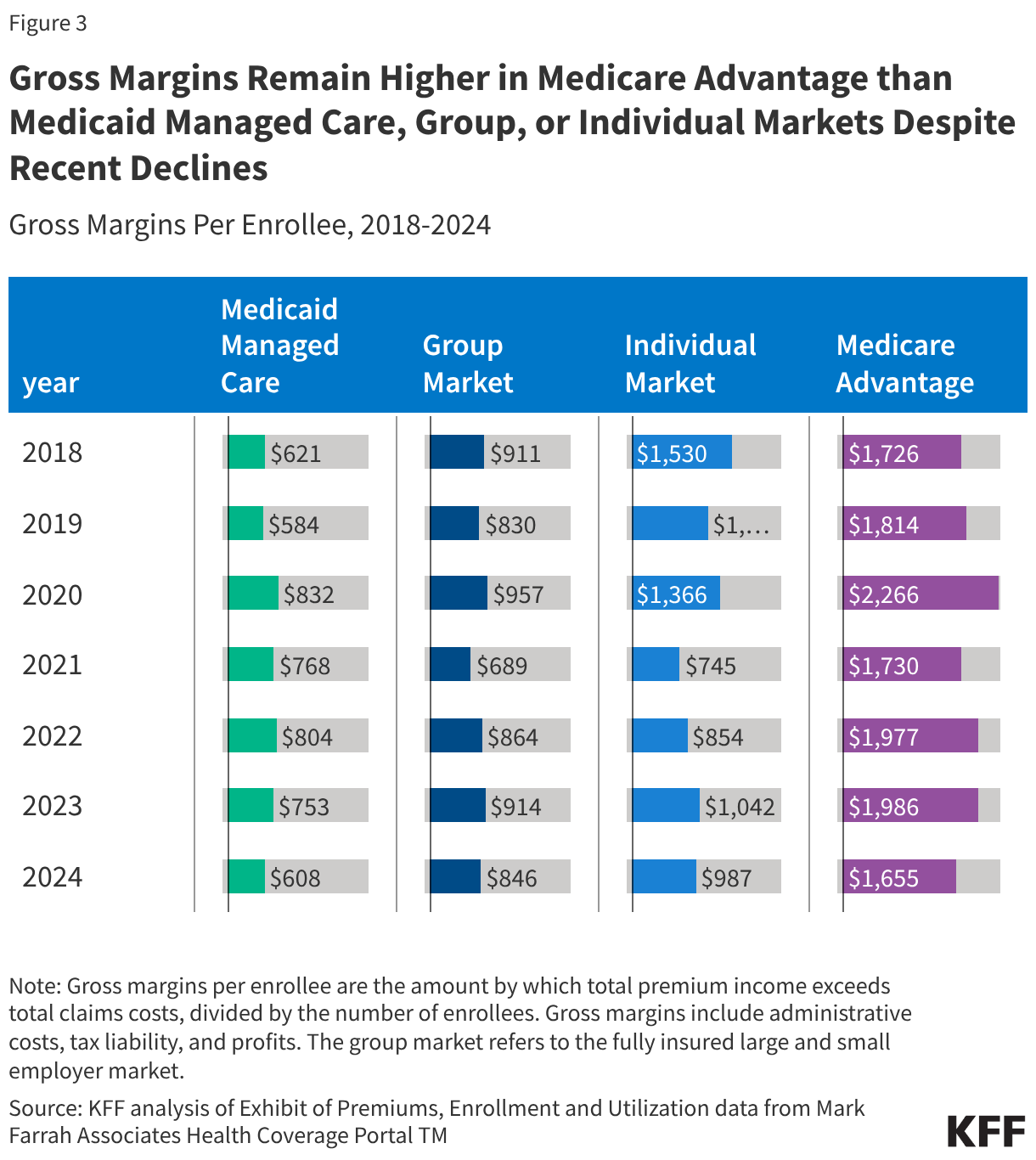
While gross margins are not equivalent to profitability, changes in gross margins can be indicative of changes in profitability (assuming administrative costs and tax liability are stable). Gross margins have declined from increases that occurred in 2020 during the initial phase of the COVID-19 pandemic. In 2024, all markets saw decreases in gross margins compared to 2023.
Medicaid Managed Care: Per enrollee gross margins in the Medicaid managed care market increased during the pandemic as policies prohibited states from disenrolling people from Medicaid in exchange for additional federal dollars. Gross margins decreased by 19% to $608 from 2023 to 2024, which is slightly higher than in 2019, before the pandemic. Starting in April 2023, “continuous enrollment” in Medicaid ended and states began disenrolling individuals who were no longer eligible or who did not complete the renewal process, and Medicaid/CHIP enrollment declined by more than 16% (about 15 million people) from March 2023 to December 2024. As millions were disenrolled, states and plans faced considerable rate setting uncertainty. A shift in member risk, characterized by an increase in acuity (or health risk) of the remaining population, and increasing utilization patterns began to emerge by late 2023, which may have contributed to the decrease in per enrollee gross margins seen from 2023 to 2024. States may use a variety of risk mitigation strategies, including “risk corridors” (where states and plans agree to share profit or losses), to provide financial protection and limits on financial risk for states and plans that may not be accounted for in the data used in this gross margin analysis. States may also make capitation rate adjustments (with CMS approval) when substantial coverage changes occur mid-year or adjustments are necessary to address unforeseen circumstances that increase benefit costs.
Medicare Advantage: Through the end of 2024, gross margins in the Medicare Advantage market averaged $1,655 per enrollee, which is 17% lower than in 2023 ($1,986), consistent with reports by the largest Medicare Advantage insurers of increased utilization beginning in late 2023 that extended through 2024. Additionally, the phase-in of changes to Medicare Advantage payments, stemming from revisions to how the federal government makes adjustments for the health status of enrollees, began in 2024 and reduced the pace at which revenue per enrollee grew. Per enrollee gross margins have consistently been larger than those in the individual, fully insured, and Medicaid managed care markets since 2018.
Group Market: Gross margins per enrollee for fully insured group plans declined by 7% from $914 to $846 from 2023 to 2024. This is the first time per enrollee gross margins in the fully insured group market have declined from the year prior since 2021, when they were the lowest in the past decade (not shown).
Individual Market: Individual market gross margins were about 5% lower in 2024 compared to 2023, going from $1,042 to $987 per enrollee. In 2018, following efforts to repeal the ACA and defunding of Cost Sharing Reduction subsidies, insurers raised individual market premiums substantially. These premium increases resulted in significantly higher margins than in earlier years. For context, gross margins per enrollee in 2024 were around 35% and 16% lower than in 2018 and 2019, respectively.
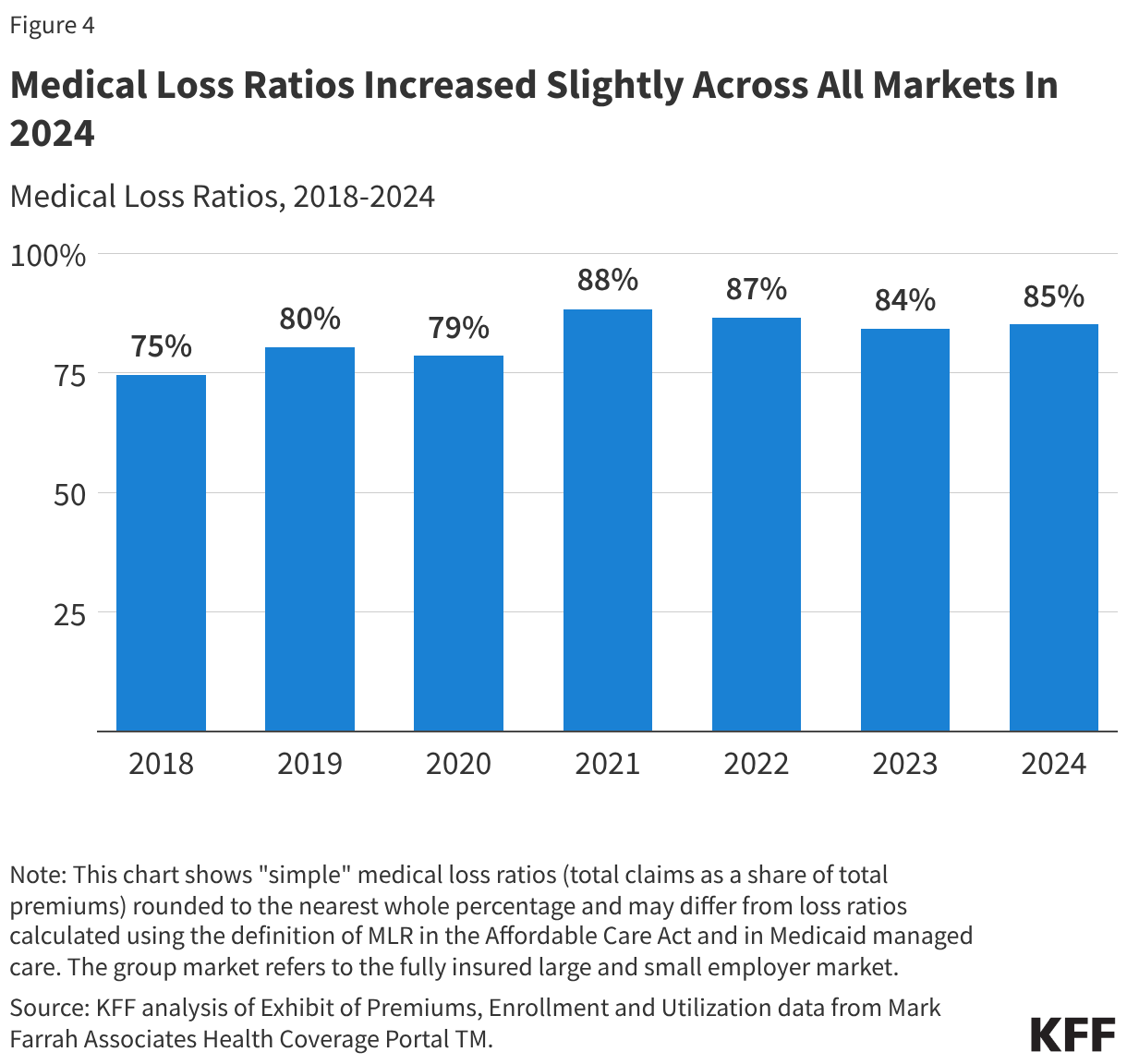
Trends in Medical Loss Ratios
Each health insurance market has different administrative needs and costs, so similar MLRs do not imply that the markets are similar to each other in profitability. Additionally, simple MLRs examined in this brief do not incorporate the effects of changes in tax law, such as the health insurer tax, which has been permanently repealed starting in 2021, was in effect in 2018 and 2020, but was not in 2019. While MLRs alone cannot convey whether a market is profitable in a particular year, if administrative costs hold mostly constant from one year to the next, a change in the MLR could imply a change in profitability.
Individual Market: The average individual market MLR in 2024 was similar to 2023, but higher than those seen in the years following the end of cost-sharing reduction payments. As mentioned earlier, 2018 and 2019 were exceptionally lucrative years for the individual market. Many plans fell short of the ACA’s MLR requirements and were therefore required to issue large rebates to consumers based on their 2018 and 2019 experience.
Group Market: The average MLR for group plans was stable between 2022 and 2023 at 86% but rose to its 2021 value of 88% in 2024. These are all higher than in the years prior, when MLRs ranged from 83% in 2018 and 2020 to 85% in 2019.
Medicaid Managed Care: Relative to 2023, the average MLR in 2024 for the Medicaid managed care market increased from 88% to 91% (implying a potential decrease in profitability). This is the highest Medicaid managed care average medical loss ratio observed in the past decade (data not fully shown). As previously discussed, states and plans faced considerable rate setting uncertainty after millions of people were disenrolled during the unwinding of the pandemic-era Medicaid continuous enrollment provision, resulting in acuity and utilization shifts within the remaining population. These factors may have contributed to the change in MLR seen from 2023 to 2024. Looking ahead, implementation of the 2025 federal budget reconciliation law’s Medicaid coverage and financing provisions could affect Medicaid managed care plans.
Medicare Advantage: Average MLRs in the Medicare Advantage market rose to 90% in 2024. That is higher than before and during the onset of the COVID-19 pandemic, from 2018-2020, when MLRs ranged from 83% to 86%. The increase of the MLR in the Medicare Advantage market could imply decreased profitability, consistent with higher utilization and the effects of phasing in a new risk-adjustment model. At the same time, it may be difficult to interpret changes in MLRs with increasing consolidation, driven in part by insurers purchasing related businesses, such as pharmacy benefit managers, physician groups, and post-acute care providers, because it is not entirely clear how insurers allocate expenses across different lines of business.
Medicare Advantage plans have both higher average costs and higher premiums (largely paid by the federal government), because Medicare covers an older, sicker population. So, even when Medicare Advantage insurers spend a similar share of their premiums on benefits as other insurers in other markets, the gross margins described above—which include profits and administrative costs—tend to be higher in Medicare Advantage plans.
This work was supported in part by Arnold Ventures. KFF maintains full editorial control over all of its policy analysis, polling, and journalism activities.
Methods
We analyzed insurer-reported financial data from Health Coverage PortalTM, a market database maintained by Mark Farrah Associates, which includes information from the National Association of Insurance Commissioners (NAIC). We used the “Exhibit of Premiums, Enrollment, and Utilization” annual report (accessed January 21, 2026) for this analysis. The dataset analyzed in this report does not include California HMOs regulated by California’s Department of Managed Health Care. Additionally, for Medicaid, there are four states (California, Delaware, New York, and Oregon) that have different reporting practices and therefore may only have partial or no NAIC data available for the years displayed.
We excluded plans in each segment of interest that filed negative values or have negative or zero dollars in premiums or claims. We also excluded plans reporting at least 1,000 hospital patient days incurred per 1,000 member months. We only included plans that were categorized as having a “medical” focus in our analysis and exclude “specialty” plans which are categorized as “ancillary or supplemental benefit plans.” We also excluded any plans from the U.S. territories. We corrected for plans that did not file “member months” or filed a zero “member month” value in the annual statement but did file current year membership by imputing these values. If, after imputing, plans still did not have “member months,” they were excluded.
The group market in this analysis only includes fully insured plans (but excludes Federal Employee Health Benefits Program plans and plans regulated by the California Department of Managed Health Care). NAIC defines “Medicaid” as “business where the reporting entity charges a premium and agrees to cover the full medical costs of Medicaid subscribers.” This explicitly excludes Administrative Services Only (ASO) plans. We only use “medical” focused plans to help exclude any specialty plans; however, prepaid ambulatory health plans (PAHPs), prepaid inpatient health plans (PIHPs), or Programs of All-Inclusive Care for the Elderly (PACE) plans may be included in the analysis due to NAIC’s definition of Medicaid.
Gross margins per enrollee were calculated by subtracting the sum of total incurred claims from the sum of unadjusted health premiums earned and dividing by the total number of members.
Premiums for Medicare Advantage plans primarily consist of federal payments made to plans and any additional amounts plans may charge their enrollees. Premiums for Medicare Advantage plans do not include payments for Medicare Part D benefits. Premiums for Medicaid may not reflect contractual adjustments related to risk corridors or other risk-sharing adjustments.
To calculate medical loss ratios, we divided the market-wide sum of total incurred claims by the sum of all unadjusted health premiums earned. MLRs in this analysis are simple loss ratios and therefore, may differ from loss ratios used to calculate rebates.
Appendix
Individual Market: The individual market includes coverage purchased by individuals and families through the Affordable Care Act’s exchanges (Marketplaces) as well as coverage purchased directly off-exchange, which includes both plans complying with the ACA’s rules and non-compliant coverage (e.g., grandfathered policies purchased before the ACA went into effect and some short-term plans). The federal government provided subsidies for low and middle-income people in the Marketplace and includes measures, such as risk adjustment, to help limit the financial liability of insurers. Insurers in the individual market receive premium payments from enrollees, plus any federal subsidies for people in the Marketplaces.
Some plans submitting data on the Exhibit of Premiums Enrollment and Utilization appear to be including some Children’s Health Insurance Program (CHIP) data in their Individual market filings. In a previous version of this analysis, we used the Supplemental Health Care Exhibit to address this. However, in this analysis, we opted to use the EPEU to ensure comparability.
Group Market: The fully insured group market serves employers, their employees and dependents who are enrolled in fully insured health plans. This market includes both small and large group plans but excludes employer-sponsored insurance plans that are self-funded, which account for 63% of workers with employer-sponsored insurance in 2024. This analysis does not capture metrics for the Federal Employee Health Benefit Program or California Managed Health Care plans. Roughly 25 million people from the fully insured group market in 2024 are accounted for in this analysis. Plans typically receive premium payments from both employers and their employees.
Medicaid Managed Care: The Medicaid managed care market includes managed care organizations (MCOs) that contract with state Medicaid programs to deliver comprehensive acute care (i.e., most physician and hospital services) to enrollees. As of July 2024, more than three-fourths (over 66 million people) of all Medicaid beneficiaries nationally received most or all of their care from comprehensive risk-based MCOs. There is significant variation across states with respect to services that are covered by MCOs.
In this analysis, the NAIC data we use defines “Medicaid” as “business where the reporting entity charges a premium and agrees to cover the full medical costs of Medicaid subscribers” and only explicitly excludes Administrative Services Only (ASO) plans from their reporting. While we only use “medically” focused plans to help exclude any specialty plans, PAHPs, PIHPs and PACE plans may not be excluded due to NAIC’s definition of Medicaid. Additionally, for Medicaid, there are four states (California, Delaware, New York, and Oregon) that have different reporting practices and therefore may only have partial or no NAIC data available for the years displayed. In other work, KFF defines comprehensive MCOs as managed care plans that provide comprehensive Medicaid acute care services and, in some cases, long-term services and supports as well. This excludes “limited benefit plans” including prepaid ambulatory health plans (PAHPs), prepaid inpatient health plans (PIHPs), and Programs of All-Inclusive Care for the Elderly (PACE) that may be included in this analysis.
Medicare Advantage: The Medicare Advantage market provides Medicare-covered benefits through private plans to around 33 million Medicare beneficiaries in 2024, which is over half of all Medicare beneficiaries in 2024. The federal government makes risk-adjusted payments (higher payments for sicker enrollees and lower payments for healthier enrollees) to plans (averaging nearly $14,823 per enrollee in 2024) to cover the cost of benefits covered under Medicare Parts A and B and supplemental benefits, such as dental, vision, hearing, and others, with additional payments for costs associated with prescription drug coverage. Some plans charge enrollees an additional premium.