Medicare’s Income-Related Premiums Will Rise for Some Higher-Income Beneficiaries Beginning in 2018
Some higher-income Medicare beneficiaries will have to pay more in Part B and Part D premiums starting in 2018, due to a provision in the Medicare Access and CHIP Reauthorization Act of 2015, a recently passed law to change how Medicare pays physicians.
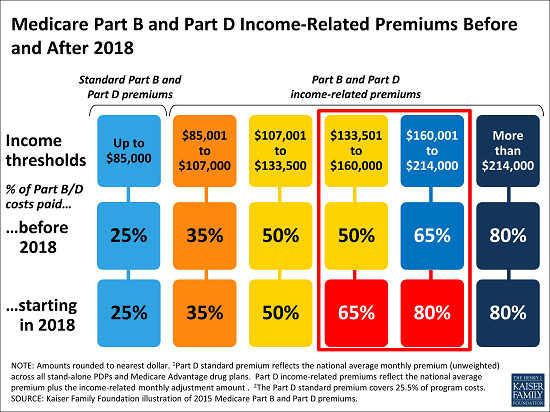
A Kaiser Family Foundation analysis finds that, as a result of the provision, Part B premiums are expected to rise from $238 per month to $310 per month for Medicare beneficiaries with incomes from $133,501 to $160,000 ($267,001-$320,000/couple) in 2018, based on projections of Part B program costs from the Medicare Trustees. This is because the law raises Medicare premiums to cover 65 percent of program costs (from 50 percent) for beneficiaries in this income bracket. Similarly, for beneficiaries with incomes between $160,001 to $214,000 ($320,001 to $428,000/couple), monthly Part B premiums are expected to rise from $310 to $381 per enrollee in 2018, covering 80 percent of program costs (rather than 65 percent).
Relatively few people on Medicare will be affected. Only 2 percent of beneficiaries would see their premiums rise due to this provision if it were implemented this year, the new analysis finds. Most beneficiaries will pay Medicare premiums that are set to cover 25 percent of program costs. In 2015, that translates into Part B premiums of about $105 a month for individuals with incomes of $85,000 or less in 2015. In 2018, the standard Part B premium is expected to be $119 per month.
The increase in premiums for some higher-income beneficiaries, designed to help offset the cost of the new law, is expected to increase Medicare’s premium revenues by $34.3 billion between 2018 and 2025, according to the Congressional Budget Office. For the full Kaiser analysis, including a broader examination of current requirements with respected to Medicare’s income-related premiums, visit kff.org.