Medicaid Eligibility for Families and Children – Issue Paper
Medicaid Eligibility for Families and Children
September 1998
Measured by enrollment, Medicaid is the largest health insurer in the country. According to the Urban Institute’s estimates, Medicaid covered 41.3 million Americans in 1996; Medicare, in comparison, covered 38 million. Moreover, millions of low-income Americans without private health insurance coverage are eligible for Medicaid but are not enrolled in the program. For example, researchers at the Agency for Health Care Policy Research recently estimated that in 1996 about 4.7 million uninsured children were eligible for Medicaid but not enrolled.1 If all of these children were enrolled in Medicaid, the number of children without some form of health insurance coverage would drop by 40 percent.
There are numerous reasons why Medicaid does not cover all of the children or adults who qualify. This Issue Paper focuses on one of those reasons: the complexity of Medicaid eligibility policy. This complexity makes the program difficult for low-income Americans to understand and for state Medicaid officials to administer. Yet within this complexity are options that enable states, if they so choose, to use their Medicaid programs as a policy tool to reduce — potentially dramatically — the number of children and adults without basic health care coverage.
This paper begins with an overview of Medicaid eligibility policy. It then turns to two groups of Americans — low-income children and nondisabled adults under 65 — and summarizes the statutory and regulatory “pathways” to Medicaid eligibility available to individuals to them.2 The paper concludes with a discussion of policy options available to states under current law for increasing Medicaid eligibility for these two groups. It also reviews the policy options available to the federal government for altering current law to expand Medicaid eligibility.
The complexity of Medicaid eligibility policy is just one reason why Medicaid does not cover all of the children or adults who qualify. Other reasons include burdensome application forms and procedures, lack of outreach efforts, and negative perceptions of Medicaid among low-income families.3 These issues are the subject of other analyses and are being explored in related Kaiser Commission projects.4
As CBO has recognized, states have Aa great deal of flexibility in operating the Medicaid program.5 For this reason, Medicaid eligibility policy, like Medicaid coverage policy and Medicaid payment policy, varies from state to state. This paper does not attempt to describe Medicaid eligibility policy in each state.6 Instead, the focus is on the federal policies that structure the eligibility choices that states make.
I. Overview of Medicaid Eligibility Policy
Medicaid eligibility policy reflects the basic structure of the program. Medicaid is a means-tested, federal-state, individual entitlement program with historical ties to the Aid to Families with Dependent Children (AFDC) and Supplemental Security Income (SSI) cash assistance programs. Medicaid’s policy premise of means-testing explains much about its income and resource rules. Medicaid’s association with AFDC and SSI has guided Medicaid’s historical eligibility categories. Finally, because Medicaid is an individual entitlement, both the states and the federal government have relied on eligibility policy as a tool for limiting their financial exposure for the cost of covered benefits.
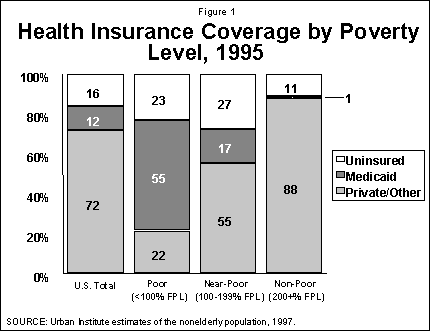
Medicaid’s role is to cover basic health and long-term care services for low-income Americans. However, being poor does not assure Medicaid coverage. As shown in Figure 1, Medicaid in 1995 covered only about 55 percent of the nonelderly poor, earning less than $12,590 for a family of three. Medicaid’s reach to individuals with incomes just above the poverty line is even more limited, covering only 17 percent of the near-poor. Despite Medicaid, low-income people are considerably more likely to be uninsured than those with higher incomes. While a portion of the low-income uninsured are eligible for Medicaid but not enrolled, a substantial share are excluded from Medicaid coverage by program eligibility rules that reflect policy choices at both the federal and state level.
At the federal level, eligibility policy choices are reflected in the authorization of federal Medicaid matching funds (on an open-ended basis) for the costs incurred by a state in paying for covered services on behalf of certain low-income individuals. Federal Medicaid matching funds are available to states for the costs of covering some categories of individuals but not others. If federal matching funds are not available for a particular category, it is unlikely that a state will extend Medicaid coverage to those categories of individuals, because the state would then bear the costs of care entirely at its own expense.
At the state level, eligibility policy choices are reflected in state decisions as to which optional eligibility categories and which income and resource criteria to adopt. There are certain eligibility groups — for example, pregnant women with family incomes at or below 133 percent of the federal poverty level ($1,513 per month for a family of three in 1998) — that all states opting to participate in Medicaid must cover. In addition, there are other categories for which states may receive federal matching funds if they choose to extend Medicaid coverage. However, the availability of federal matching funds for a particular category of individuals does not necessarily mean that a state will cover that category, since the state must still contribute its own matching funds toward the costs of coverage.
The terms on which federal Medicaid matching funds are available to states include five broad requirements relating to eligibility: categorical; income; resources; immigration status; and residency. Two of these broad requirements — income and resources — are financial in nature. The other three — categorical, immigration status, and residency — are non-financial. In order to qualify for Medicaid, an individual must meet both its financial and non-financial requirements.
Within each of these five broad requirements are “mandatory” and “optional” elements. It is important to understand the context in which these terms are used. State participation in Medicaid is voluntary, not mandatory. The federal government makes Medicaid matching funds available on an open-ended, entitlement basis to states that elect to participate in the program. In order to participate, states must offer coverage for basic benefits to certain populations — e.g., medically necessary physician and hospital services to certain low-income families and children.
States receive federal Medicaid matching funds for at least 50 percent and as much as 80 percent of the costs of this mandatory coverage, depending on the state. In exchange, states are also able to draw down federal Medicaid matching funds at the same rate for optional populations and services such as the low-income elderly and disabled at risk of nursing home and other expensive long-term care services. Similarly, within each of the five major eligibility requirements there are minimum policies states must follow and there are more expansive policies that states may adopt. According to the Health Care Financing Administration, 55 percent of all Medicaid spending paid for optional populations or optional services.7
A child or adult who establishes Medicaid eligibility is not, on the basis of that initial determination, entitled to maintain eligibility indefinitely. Federal Medicaid regulations require that states redetermine eligibility of a Medicaid beneficiary at least once every 12 months. This redetermination, like the original determination, is designed to ensure that a beneficiary continues to meet each of the financial and non-financial requirements for eligibility. Those beneficiaries, who due to a change in income, resources, or family composition no longer meet the eligibility requirements of their state through any pathway, lose their entitlement to Medicaid. There are some limited exceptions for certain categories such as pregnant women, who are entitled to continue Medicaid coverage for 60 days post-partum regardless of any change in financial or non-financial circumstances.
Fluctuations in monthly income are common among low-income families. These changes can lead to the loss of Medicaid coverage by a child or family whose income may spike during one part of the year but spends most of the year earning under the federal poverty level. This occurs commonly in states that use 1-month, 3-month, and 6-month redetermination periods. To address eligibility “churning,” the Balance Budget Act of 1997 gave states the option of extending Medicaid coverage with federal matching funds to children under 19 for a period of up to 12 months after the initial determination of eligibility regardless of any change in financial or non-financial circumstances that would otherwise make them ineligible. This option does not extend to low-income adults with dependent children.
Medicaid does not require that an individual who meets its categorical, income, resource, immigration status, and residency requirements also be uninsured. Medicaid treats insurance coverage as a payment source, not as an eligibility criterion. More specifically, private insurance coverage under Medicaid is a type of “third party liability” that the program uses to reduce its costs of coverage. In most cases, when a Medicaid beneficiary also has private coverage, the private insurer must pay first. Then Medicaid will pay for Medicaid-covered services for which the private insurer is not obligated to pay. This policy stands in sharp contrast to the approach taken under the new Child Health Insurance Program (CHIP), under which states are expressly prohibited from using federal CHIP matching funds to pay for services to children with private health insurance.8
Unlike employer-based insurance coverage, Medicaid eligibility is not directly tied to employment for many of the Medicaid coverage categories. For example, a pregnant woman whose income is equal to or less than 133 percent of the federal poverty level is eligible for Medicaid coverage in every state whether or not she worked before or during her pregnancy. On the other hand, as a result of the 1996 welfare law, a state has the option to deny Medicaid eligibility to non-pregnant women with dependent children with respect to whom the state has terminated cash assistance for refusal to work (states are not permitted to terminate Medicaid coverage to children for this reason).
The earnings flowing to an individual or a family from work will affect income eligibility for Medicaid. At income levels near Medicaid eligibility thresholds, a small increase in earnings can result in a loss in Medicaid eligibility even though the increase in earnings may not be sufficient to enable the worker to afford private health insurance coverage. To mitigate this disincentive to work or to increase the hours worked, states are required to extend “transitional” Medicaid coverage for up to one year to women (and their dependent children) who lose cash assistance due to earnings.
Figure 2: Major Medicaid Eligibility Pathways for Selected Groups
Mandatory Coverage Optional Coverage Low-income Children Primary Pathways Infants under age 1 with income < 133% FPL Infants under age 1 with income < 185% FPL Children age 1 to 6 with income < 133% FPL Children age 1 to 6 with income < 185% FPL Children age 6 to 15 with income < 100% FPL Children age 6 to 15 with income < 133% or 185% FPL Section 1931 children Targeted low-income children (CHIP children) Children in welfare-to-work families Transitional coverage for children in welfare-to-work families Title IV-E foster care children Non-Title IV-E foster care children Title IV-E adoption assistance children Non-Title IV-E adoption assistance children Other Pathways Medically needy Ribicoff children Children with Disabilities Primary Pathways Supplemental Security Income (SSI) recipients Katie Beckett children Home or community-based waiver children Other Pathways SSI recipients as of 8/22/96 Medically needy Pregnant Women Primary Pathways Pregnant women with income < 133% FPL Pregnant women with income < 185% FPL Other Pathways Medically needy Low-Income Adults Primary Pathways Certain adults in low-income families with children Adults in two-parent households with dependent children Other Pathways Medically needy COBRA continuation beneficiaries Return to top
Medicaid Eligibility for Families and Children
Policy Brief Part 1 Part 2 Part 3 Part 4 Part 5


