Data Note: Medicaid Managed Care Growth and Implications of the Medicaid Expansion
Introduction
The Medicaid program covers more than 74 million Americans, or 1 in 5, including low-income pregnant women, children, and parents, seniors, people with disabilities, and, in Medicaid expansion states, nearly all low-income nonelderly adults. Most states today rely heavily on risk-based managed care organizations to serve Medicaid beneficiaries. This Data Note discusses the current role of managed care in Medicaid and addresses differences in managed care growth between states that expanded Medicaid to low-income adults under the Affordable Care Act (ACA) and states that did not expand Medicaid.
Risk-based managed care is the dominant delivery system in Medicaid.
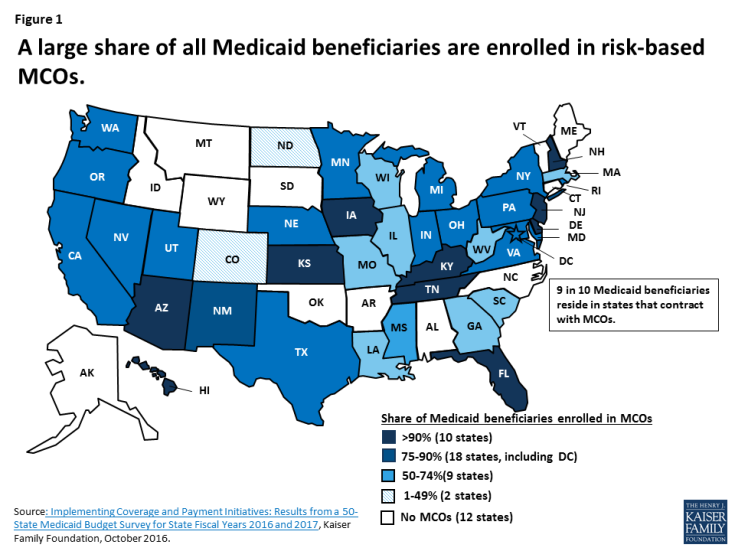
Going back as far as the 1970s, some state Medicaid programs, as an alternative to paying providers on a fee-for-service basis, contracted on a risk basis with private managed care organizations (MCOs) to serve selected beneficiary populations – primarily, pregnant women, children, and families. Over time, more states have taken up MCO contracting and states have also expanded their MCO programs to include both wider geographic areas and beneficiaries with more complex needs. Today, 39 states contract with MCOs and risk-based managed care is the dominant delivery system in Medicaid. As of July 2016, in 28 states – including 8 of the 10 states with the most Medicaid beneficiaries (California, New York, Texas, Florida, Ohio, Pennsylvania, Michigan, and Washington) – at least 75% of all Medicaid beneficiaries were enrolled in MCOs. In 10 of these 28 states, more than 90% of beneficiaries were enrolled in MCOs (Figure 1). In FY 2016, 43% of Medicaid spending was attributable to payments to MCOs, up from 28% in FY 2013.1
In 25 Medicaid expansion states, at least 80% of all newly eligible adults are in Managed care plans.
Thirty-two states (including the District of Columbia) have expanded Medicaid to low-income, nonelderly adults under the Affordable Care Act (ACA), and in these states, 11 million adults are newly eligible for Medicaid as a result. Most Medicaid expansion states (27) contract with MCOs to serve a large share of Medicaid beneficiaries. Expansion states account for 21 of the 28 states where at least 75% of beneficiaries are in MCOs, and seven of the 10 states with penetration rates above 90%. In nearly all 27 Medicaid expansion states with risk contracts, the share of newly eligible adults enrolled in MCOs is at least as high as the overall share of beneficiaries enrolled in MCOs. In 25 of these states, at least 80% of newly eligible adults are enrolled in MCOs, including 17 states where over 90% of expansion adults are enrolled in plans (Figure 2).
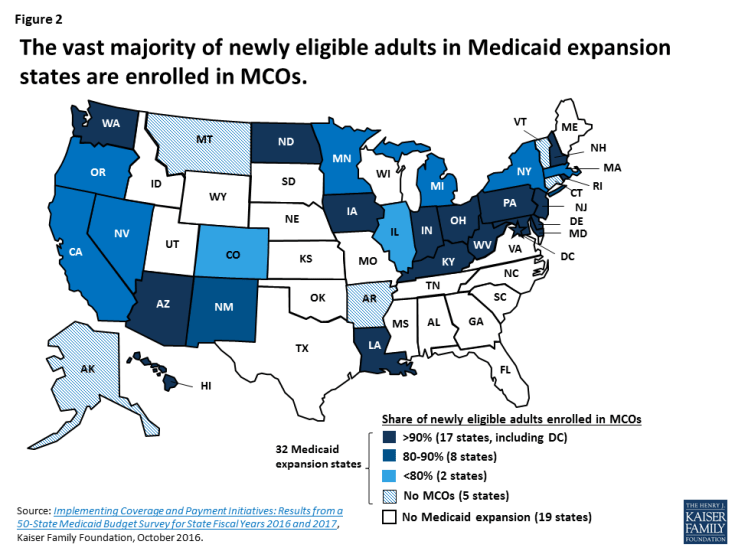
Figure 2: The vast majority of newly eligible adults in Medicaid expansion states are enrolled in MCOs.
Most MCO enrollment growth is occurring in Medicaid expansion states.
The 39 states operating Medicaid MCO programs include 27 expansion states and 12 non-expansion states. Medicaid MCO enrollment continues to grow in both groups of states. Data comparing MCO enrollment in December 2013, the month before the ACA Medicaid expansion took effect, and September 2016, show substantial managed care increases over this period, with the lion’s share of the increase in MCO enrollment occurring in expansion states.2 In the 19 expansion states with MCOs that reported both pre- and post-ACA data, MCO enrollment rose from 22.8 million to 36.1 million – an increase of 13.3 million beneficiaries, or 58% (Figure 3).3 The median increase in MCO enrollment in these states was 47%. In comparison, in the seven non-expansion states with MCOs that reported pre- and post-ACA data, MCO enrollment grew from 7.4 million to 10.8 million – an increase of 3.4 million beneficiaries, or 46%, and the median increase was 31%.4
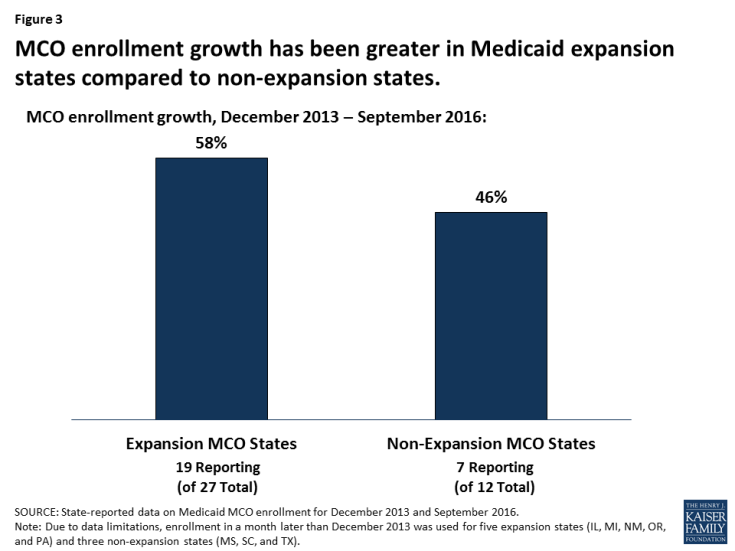
Figure 3: MCO enrollment growth has been greater in Medicaid expansion states compared to non-expansion states.
The larger increases in MCO enrollment in the Medicaid expansion states reflect a number of factors, including: the greater number of expansion versus non-expansion states with MCOs; the much larger number of Medicaid beneficiaries residing in the expansion/MCO versus non-expansion/MCO states (43.1 million versus 18.1 million in December 2016); and the expansion states’ heavy reliance on MCOs to serve newly eligible adults as well as other Medicaid beneficiaries. Expansion states account for 15 of the 21 states where more than 80% of Medicaid beneficiaries are in MCOs.
Conclusion
States are continuing to expand their use of comprehensive risk-based managed care. In the Kaiser Family Foundation’s most recent 50-state Medicaid budget survey, 11 of the 39 states with MCOs indicated that they took specific action in FY 2017 to increase the number of Medicaid enrollees in MCOs through geographic expansions, voluntary or mandatory enrollment of new groups, or mandatory enrollment of groups formerly enrolled on a voluntary basis. As both Medicaid expansion and non-expansion states broaden the size and scope of their MCO programs, a large and growing share of beneficiaries, increasingly including people with disabilities, poor seniors, and others with complex health care needs, are receiving their care in private managed care plans. The growing role of managed care in Medicaid has important implications for beneficiary access to care, in particular, because it shifts the onus of finding providers who accept Medicaid patients from the individual to MCOs, which are contractually responsible for establishing adequate provider networks to serve Medicaid enrollees.
Endnotes
Urban Institute estimates based on data from CMS (Form 64), as of April 2017.
In several states for which December 2013 data were not available, data from a later month were used to calculate MCO enrollment increases. See Endnotes 2 and 3 for detail.
The 19 states are AZ, CA, HI, IL (August 2014), IN, KY, LA, MA, MD, MI (August 2014), MN, NV, NM (March 2015), NY, OH, OR (January 2014), PA (August 2014), WA, and WV.
The seven states are FL, MS (January 2014), MO, SC (September 2014), TN, TX (June 2014), and WI.