How Well Does the Employment-Based Health Insurance System Work for Low-Income Families?
Part 3
What Explains the Coverage Decline?
Rapidly rising health care costs-or, more precisely, employers’ responses to costs-have contributed to the widespread erosion of employer coverage. As employers have shifted costs to workers, participation has dropped. Low-wage workers have been disproportionately affected by rising costs, losing access to coverage as well as finding participation more difficult. Their problems have been exacerbated by structural changes in labor markets, which have weakened the tie between jobs and health insurance.9
Constrained Employer Spending. A key factor behind the decline in employer coverage has been the rapid rise in health care costs. The cost of health insurance grew rapidly in the 1980s and early 1990s, far exceeding the growth in consumer prices generally. Between 1988 and 1996, the average premium for family coverage rose 9.8% per year, the premium for individual coverage increased 7.5% per year, while prices overall increased about 4% annually.10
Employers’ primary response to rapidly rising health care costs has not been to drop health care coverage for full-time workers. However, employers have constrained spending by requiring workers to pay a larger share of health insurance premiums, by tightening eligibility requirements for part-time workers (whose coverage has long been restricted) and, increasingly, in recent years, by replacing regular full-time employees with part-time and contingent workers.11
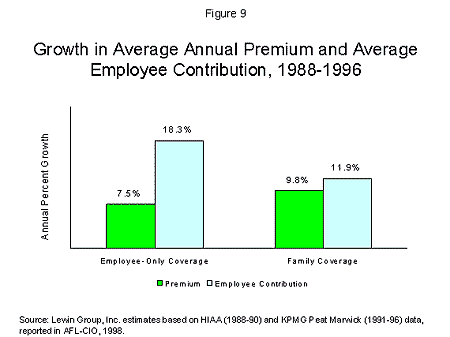
Workers’ average monthly contributions for single and family coverage rose steadily between 1988 and 1996 as workers paid a larger share of higher premiums.12 In fact, as shown in Figure 9, workers’ contributions rose more rapidly than premiums as employers shifted more of the costs of health insurance to workers, especially for non-family coverage. While average premiums for non-family coverage rose an average of 7.5% per year between 1988 and 1996, employees’ contributions rose much more rapidly–increasing by 18.3% per year.13
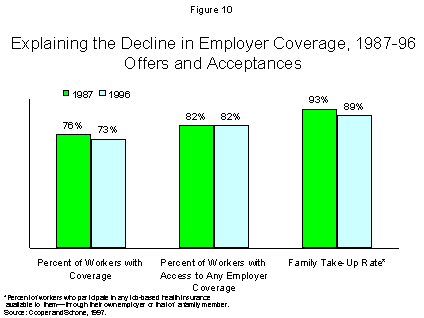
As employers have shifted costs to workers, some workers have dropped coverage, while those who have kept coverage are paying more. As shown in Figure 10, the proportion of workers participating in employer plans to which they had access fell from 93% in 1987 to 89% in 1996. Access to employer coverage was basically unchanged over this period–about 82 percent. Although the fact remains that most (about 70 percent) of the working uninsured lack access to coverage, the decline in coverage between 1987 and 1996 mostly reflects a drop in participation.14
This overall pattern obscures a worsening of access, as well as participation, for low-wage workers. Although participation rates have dropped most rapidly for the lowest wage workers, access to employer coverage has also declined for these workers. For example, among workers earning more than $15 per hour, the proportion with access to employer coverage increased from 92% in 1987 to 96% in 1996. In contrast, the proportion of low-wage workers (those earning less than $7 per hour) with access to employer coverage declined 5 percentage points over this same time period, from 60% to 55% [Table 2]. The large drop in coverage rates for the lowest wages workers is thus explained by a combination of declining participation and a decline in employer offerings.
Changes in Low-wage Labor Markets. For low-wage workers, costs and employer cost containment are not the only factors producing this deterioration. Structural changes in labor markets, that have occurred throughout the 1980s and 1990s, have contributed to the decline in coverage.
The main change in the labor market over the past two decades has been the widespread deterioration of wages, especially for those workers who initially had low wages, were without a college degree, were in blue collar or service occupations, or were in younger age brackets.15 From 1989 to 1996, the real hourly wage of the typical (median) worker fell 5.2%, while the wages of high-wage workers (90th percentile) increased 0.4%, and wages for low-wage workers (20th percentile) declined by 2.3%. Among low-wage men, the wage declines were even greater. Wages for low-wage men fell 6.4% between 1989-96.16 That is, wages for workers at the middle and at the bottom of the pay scale have not only failed to keep up with health care costs, they have declined in real terms. The large drop in participation rates for the lowest wage workers is understandable in light of the deterioration in wages for these workers. Employer actions that have led to coverage declines for all workers have thus had a disproportionate effect on the lowest wage workers.
Table 2 Change in Access, Family Take-up and Coverage, by Wage
1987-1996 Wage Level 1987 1996 Change 1987-96
Coverage $15 87 90 +3
Access to Employer Coverage* $15 92 96 +4
Family Take-Up Rate** $15 94 94 0 * Percent of workers with access to job-based insurance through their own employer or a family member s employer.
** Percent of workers with access to job-based insurance who are actually covered by it.
Source: Cooper and Schone, 1997.
The decline in access for low-wage workers also is rooted in structural labor market changes. Shifts in employment to low-paying sectors may account for most of this decline in access. As jobs have shifted from high-paying industries like manufacturing to low-paying sectors like retail trade and services, health insurance coverage has declined.17 In addition, the proportion of the workforce in “nontraditional” work arrangements–such as regular part-time work, contingent work, and self-employment–has grown in the past decade. The expansion of employment in these jobs is not large enough to explain much of the decline in coverage; nevertheless, since these jobs are less likely to come with health insurance benefits, the expansion of nontraditional work has contributed to the overall decline in coverage.18
Conclusion
Over the past decade, there has been a decline in employment-based health insurance coverage. The fall in coverage is a widespread phenomenon that goes beyond low-income families. However, often overlooked is that low-wage workers and low-income families–who started out at a disadvantage, with low rates of coverage–have borne the brunt of the decline. The gap in coverage between low-wage and high-wage workers has grown between 1987 and 1996 because the decline in coverage has been greatest for low-wage workers. Although Medicaid plays an important role in providing insurance coverage for many low-income families, including working families, Medicaid’s eligibility levels are constrained. Workers without children are, for the most part, precluded from coverage. Beyond Medicaid’s reach, therefore, many low-income working families are likely to be uninsured.
This paper was prepared for the Kaiser Commission on Medicaid and the Uninsured by Ellen O’Brien and Judith Feder, Institute for Health Care Research and Policy, Georgetown University.
Notes
1 In this Issue Paper, we rely on Current Population Survey estimates of employer health coverage and trends. Estimates of the proportion of families with various sources of insurance by income level are based on the Urban Institute’s TRIM-II model, which produces a different total estimate because it adjusts for the undercount of Medicaid beneficiaries in the CPS.
2 Workers ages 21-64 who are not self-employed.
3 The tax treatment of employment-based health insurance provides an incentive for employers to provide compensation to workers in the form of health coverage rather than in the form of wages subject to current taxation. The tax preference that the exclusion provides is substantial and has resulted in widespread access to health coverage. Yet, despite this fact–as this Paper describes–coverage rates for the lowest wage workers have traditionally been quite low and have declined significantly in the past two decades. The specific provisions of the exclusion provide a partial explanation. To qualify for the exclusion of employer-provided health coverage, employers’ health plans do not need to cover all workers. Although the tax code requires “non-discrimination”–a self-insured health plan may not discriminate in favor of highly compensated individuals as to ability to participate–employees who have not completed three years of service, those under age 25, and part-time or seasonal employees may be excluded from consideration. Moreover, insured health plans, as opposed to self-insured plans, are generally not subject to non-discrimination rules.
4 According to the Employee Benefits Supplement to the Current Population Survey, 51 million of the nearly 89 million private wage and salary workers in 1993 (or about 57% of private industry workers) had health care coverage through their employer. Of the 38 million workers without such coverage, about 50% were in firms that did not offer coverage, and 40% were in firms that offered benefits to at least some employees. (Information on whether the employer sponsored a health plan was not available for the remaining 10% of workers). See tabulations of the CPS Employee Benefits Supplement in U.S. Department of Labor. Report on the American Workforce (Washington, DC: GPO, 1995).
5 Based on an average premium for family coverage of $5,349 in 1996. KPMG Peat Marwick data cited in AFL-CIO, Paying More and Losing Ground: How Employer Cost-Shifting is Eroding Coverage of Working Families (Washington, DC: AFL-CIO,1998), p. 16.
6 These are “family take-up rates.” They measure the proportion of workers who take-up any employer plan available to them — through their own employer or through a family member’s employer. Workers’ participation rates in their own employer plans are lower (63% of the lowest wage workers and 85% of the highest wage workers participated in own employer plans they were offered) since some workers turn down their employer’s plan and choose to be covered under a family member’s plan.
7 Because of changes to the survey beginning with the March 1995 CPS, however, the estimates of employer coverage rates for 1994-96 are not comparable to data for prior years. The observed increase in employer coverage rates may be an artifact of changes in the survey questions.
8 John Holahan, Colin Winterbottom, and Shruti Rajan, “A Shifting Picture of Health Insurance Coverage,” Health Affairs 14(Winter 1995): 253-264.
9 On the more rapid drop in coverage for less educated workers see Peter Gottschalk, Trends in Wages and Health Insurance Status of Less Educated Workers. Menlo Park, CA: The Henry J. Kaiser Family Foundation; and Sherry Glied and Mark Stabile, “Graduation to Health Insurance Coverage: 1981-1996,” Working Paper 6276. (Cambridge, MA: National Bureau of Economic Research, 1997). Other studies of the decline in employer coverage include: Richard Kronick, “Health Insurance 1979-1989: The Frayed Connection between Employment and Insurance,” Inquiry 28(Winter 1991): 318-332; Deborah Chollet, “Employer-Based Health Insurance in a Changing Workforce,” Health Affairs 13(Spring 1, 1994): 315-26; Gregory Acs, “Trends in Health Insurance Coverage Between 1988 and 1991,” Inquiry 32(Spring 1995): 102-110; and Stephen Long and Joel Rogers, “Do Shifts Toward Service Industries, Part-time Work, and Self-Employment Explain the Rising Uninsured Rate?” Inquiry 32(Spring 1995): 111-117; and Paul Fronstin and Sarah Snider, “An Examination of the Decline in Employer Sponsored Health Insurance Between 1988 and 1993,” Inquiry 33(Winter 1996/1997): 317-325.
10 Data from KPMG Peat Marwick and Health Insurance Association of America, cited in General Accounting Office. “Private Health Insurance: Continued Erosion of Coverage Linked to Cost Pressures.” GAO/HEHS-97-122 (Washington, DC: GPO, 1997).
11 See Arne Kalleberg, Edith Rassell, and Ken Hudson, et. al., Nonstandard Work, Substandard Jobs (Washington, DC: Economic Policy Institute, 1997) and Thomas Rice, Nadereh Pourat, Rebecka Levan, et. al., “Trends in Job-Based Health Insurance Coverage.” (Los Angeles, CA: UCLA Center for Health Policy Research, June 1998).
12 The total nonfederal employer premium contribution fell from 85.1% to 83.9% between 1990 and 1996. In 1996 alone, this 1.2-percentage-point decrease in the employer’s share would represent a cost-shift of $3.6 billion to employees enrolled in employer-sponsored health plans. See Katherine R. Levit, Helen C. Lazenby, Bradley R. Braden, et. al. “National Health Spending Trends in 1996,” Health Affairs 17(January/February 1998), p. 46.
13 KPMG Peat Marwick data for 1991-1996 and HIAA data for 1988-1990 cited in AFL-CIO, “Paying More and Losing Ground: How Employer Cost-Shifting is Eroding Coverage of Working Families” (Washington, DC: AFL-CIO,1998), p. 16.
14 Philip Cooper and Barbara Schone. “More Offers, Fewer Takers for Employment Based Health Insurance: 1987 and 1996,” Health Affairs 16(November/December 1997): 142-149.
15 Lawrence Mishel, Jared Bernstein, and John Schmitt. The State of Working America, 1996-97 (Armonk, NY: M.E. Sharpe, 1997), p. 139.
16 Lawrence Mishel, Jared Bernstein, and John Scmitt. “Finally Real Wage Gains.” Issue Brief #127, July 17, 1998. Washington, DC: Economic Policy Institute.
17 See especially Chollet (1994).
18 See Arne Kalleberg, Edith Rassell, and Ken Hudson, et. al., Nonstandard Work, Substandard Jobs (Washington, DC: Economic Policy Institute, 1997). Return to top
Policy Brief Part 1 Part 2 Part 3
Library Index
