Medicaid Restructuring Under the American Health Care Act and Implications for Behavioral Health Care in the US
| Key Takeaways |
Medicaid is a major source of coverage and financing for people with behavioral health conditions, and enrollees benefit from a comprehensive array of mandatory and optional services.
The American Health Care Act proposes to end the enhanced federal financing for newly eligible adults and to repeal the requirement that state Medicaid plans cover essential health benefits, which include behavioral health conditions.
The American Health Care Act also proposes to convert federal Medicaid funding into a per capita cap, with a pre-set growth amount.
|
The Medicaid program serves as a safety net for many low-income individuals with behavioral health conditions by facilitating access to and financing numerous clinical and non-clinical services. Medicaid expansion to adults at or below 138% FPL, federal parity rules, and development of new models of service delivery have been particularly beneficial for Medicaid enrollees with behavioral health conditions. These changes have resulted in greater availability of and access to services, better coordinated care, and state savings. The American Health Care Act, released on March 6, 2017, proposes to repeal enhanced federal funding for adults eligible for coverage through the ACA’s Medicaid expansion and to limit federal financing through a per capita cap. On March 13, 2017, the Congressional Budget Office projected that the legislation could reduce federal deficits by $337 billion from 2017-2026 but could cause 14 million people to become uninsured. These projections are largely due to the significant changes to the Medicaid program, which could result in a 25% decrease in Medicaid spending by 2026 and could substantially alter Medicaid’s role for people with behavioral health conditions. This brief reviews Medicaid’s current role for this population and assesses the potential implications of this policy proposal.
Medicaid’s Current Role in Behavioral Health
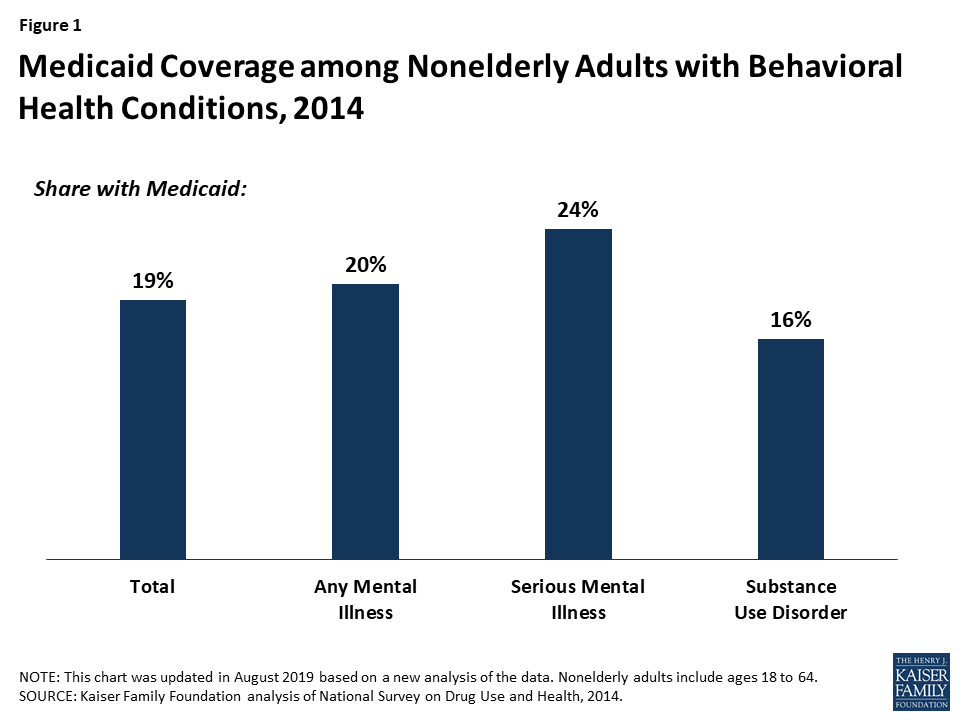
Medicaid, the federal-state health insurance program for poor and low-income individuals, is a major source of health coverage and financing for behavioral health care in the United States. The Medicaid program covers a disproportionate share of individuals with behavioral health conditions with 20% of adults with any mental illness, 24% of adults with serious mental illness (SMI), and 16% of adults with a substance use disorder (SUD) covered by Medicaid. In comparison, Medicaid covers 19% of adults with any behavioral health condition1 (Figure 1). Medicaid enrollees generally have more complex health needs than the general population, and the Medicaid program serves as a safety net for many low-income individuals who have limited options for obtaining health insurance coverage.
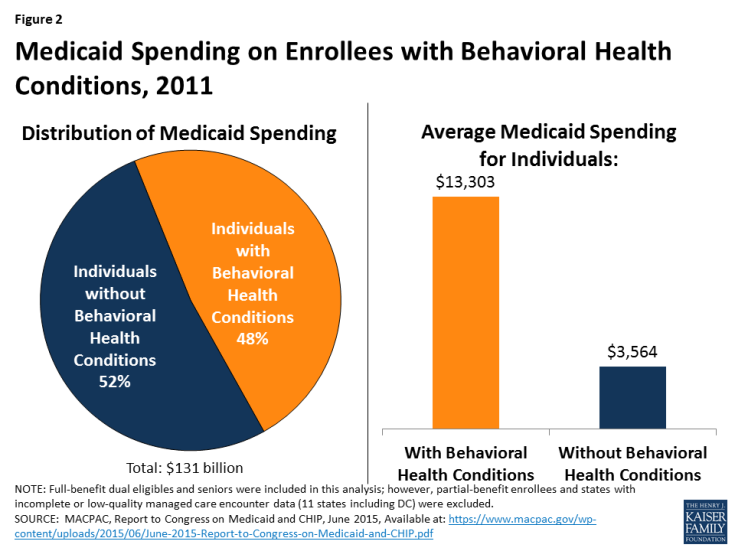
Medicaid’s behavioral health benefits are generally more comprehensive than other payers’2 and include not only acute care services but also long-term services and supports to enable many people with chronic illness to receive community-based versus institutional care. Some Medicaid services are “mandatory” services that all state must cover under federal law (e.g., hospital services and psychiatric treatment), but many, such as case management, prescription medication, and rehabilitative services, are provided at state option. Flexibility in Medicaid benefits coverage enables states to cover non-clinical behavioral health services, including those that have emerged as evidence-based practices for treating individuals with the greatest impairments (e.g., assertive community treatment (ACT)), and to adapt to changing patterns of care, such as the demand for medication-assisted treatment of opioids (MAT). Medicaid expenditures for behavioral health are significant both to the program and to national spending for behavioral health. Nationally, Medicaid funded 25% of all mental health spending and 21% of SUD funding in 2014.3 In 2011, average Medicaid spending for people with behavioral health conditions was nearly four times as much as it was for other enrollees ($13,303 vs. $3,564), and enrollees with behavioral health conditions accounted for 48% of Medicaid spending4 (Figure 2).
Medicaid coverage has expanded considerably with the passage of the Affordable Care Act and other policy changes, reaching more adults with behavioral health needs. States may now expand Medicaid eligibility to include almost all adults at or below 138% of the federal poverty level (FPL), or $27,821 for a family of three in 2016, and receive enhanced federal funding to finance the cost of this expansion. Traditionally, individuals could only be eligible for Medicaid if they both met income requirements and fell into a “category” of covered people, such as parents of dependent children or individuals with disabilities, which includes a mental illness that qualifies someone for Supplemental Security Income (SSI). These rules excluded many low-income adults without dependent children who had complex health needs, including substance use disorder or other behavioral health conditions, but did not meet criteria for having a disability. Low-income individuals who were historically ineligible for Medicaid were more likely to be males, non-Hispanic whites, older than age 45, living in the South, and slightly healthier than the Medicaid-eligible population.5 Because they were ineligible for Medicaid coverage and had limited access to other types of coverage, many of these people remained uninsured.
As of January 2017, 31 states and the District of Columbia had expanded Medicaid,6 and 11 million newly eligible adults had gained coverage under these expansions.7 States that expanded Medicaid receive higher federal matching funds for new Medicaid enrollees, known as enhanced Federal Medical Assistance Percentages (FMAP). States must offer a set of benefits for individuals newly eligible for Medicaid, known as “Alternative Benefit Plans” (ABP), which must cover a set of 10 essential health benefits, including mental health and SUD benefits. Numerous studies have documented that the Medicaid expansion has had positive effects on behavioral health services in states that expanded, including increased availability of and access to behavioral health services,8,9 decreases in unmet need for behavioral health services among low-income adults,10 better integration of behavioral health and primary care,11 increased mental health services and staffing at safety net facilities,12,13 and state savings from enhanced federal matching funds, particularly in behavioral health programs.14 In recent years, state Medicaid programs have also made strides in expanding the scope of benefits and service delivery models in behavioral health, often using state flexibility to design and test new approaches to care.
Federal parity rules also require Medicaid managed care organizations (which deliver care to the majority of Medicaid beneficiaries15) to cover behavioral health services at parity, which means that behavioral health services must be covered to the same extent as physical health services. Parity rules apply to several aspects of behavioral health treatment, including cost-sharing, deductibles, and treatment limits,16 with the goal of making behavioral health services accessible and affordable for Medicaid beneficiaries who would otherwise be unable to obtain care. All Medicaid ABPs must cover behavioral services at parity.
Medicaid also has undertaken many service delivery changes that have made behavioral health care more accessible and effective. For example, over a third of states (20) have taken advantage of the “health homes” plan option in Medicaid,17 which enables states to better coordinate care for enrollees with chronic conditions. Most Medicaid health homes programs include beneficiaries with behavioral health conditions (primarily serious mental illness),18 and through this benefit, providers can integrate and coordinate physical health, behavioral health, and long-term services and supports for enrollees. Other Medicaid programs have implemented other strategies to better integrate physical and behavioral health care, including universal screening for both physical and behavioral health conditions and the co-location of services at one facility,19 or expanded the availability of community-based services to help people with mental illness transition out of institutional-based care.20
Proposed Changes to Medicaid and Implications for Behavioral Health
Some proposals are calling for fundamental changes to the current Medicaid program. On March 6, 2017, the House unveiled the American Health Care Act, which proposes to substantially decrease federal funding for Medicaid enrollees. This decrease would be accomplished by ending the enhanced federal financing for individuals who become eligible because of the ACA’s Medicaid expansion and by converting federal Medicaid funding into a per capita cap. In addition, states would no longer be required to include essential health benefits, which include behavioral health services, in their ABPs. These changes would begin in 2020. These changes would likely make it difficult for states to finance and deliver services to residents with mental health and SUDs, increasing the burden on states at a time when systems are already stretched by a growing opioid crisis.
Ending of Enhanced Federal Financing
Ending enhanced federal financing for the Medicaid expansion population may lead to restrictions in eligibility among these enrollees, limiting the number of people who remain eligible for coverage. While some of these people may be able to qualify for the traditional Medicaid program based on having a disability, the process of gaining eligibility through this pathway requires a difficult and lengthy determination, during which individuals may lose coverage for significant amounts of time and may experience worsening symptoms as their conditions go untreated. Furthermore, individuals in the early stages of a potentially disabling condition, who do not yet meet criteria for disability under the Supplemental Security Income (SSI) program, could lose coverage for early intervention services that might forestall entry onto the SSI rolls. Although some individuals who gained coverage during the Medicaid expansion could have qualified for SSI and Medicaid prior to the expansion, qualifying for Medicaid based on income alone allows enrollees to obtain coverage more quickly and seamlessly, 21 which likely encouraged many of these individuals to finally obtain the coverage for which they had been eligible for a long time.
Limiting Medicaid eligibility has implications beyond reductions in Medicaid enrollment. A large body of literature demonstrates that Medicaid coverage helps facilitate access to needed care;22 thus, loss of coverage could lead to decreased access to early intervention and treatment services for behavioral health, which are essential for improving health outcomes. In addition to impacting health outcomes, untreated behavioral health conditions are associated with increased societal costs, which come from greater reliance on the emergency room, greater involvement with the criminal justice system, and loss of productivity resulting from being unable to work.23,24,25,26 Loss of coverage also has potential negative consequences for behavioral health providers, many of whom changed their operations in response to the ACA by, for example, accepting Medicaid and other insurance for the first time, and who saw a significant decline in uncompensated care costs under the ACA.27
Under the current structure of Medicaid, where the program operates as an entitlement and those with incomes up to 138% FPL are eligible, there are opportunities for states to modify their programs through the waiver process. It is possible that in response to the proposed changes, some states may seek Medicaid waivers to expand coverage. Medicaid waivers provide states an avenue to test new approaches in Medicaid that differ from federal program rules and can provide states considerable flexibility in how they operate their programs, beyond what is available under current law. Existing waivers include provisions not otherwise permitted under current Medicaid rules, such as premiums, copayments above statutory limits, healthy behavior incentives, or the provision of premium support for purchasing private coverage. 28 Individuals who are “medically frail,” which includes those with disabling mental disorders and chronic SUDs, are often exempt from many of the provisions in the current Medicaid waivers, so many people with behavioral health conditions are not affected by these provisions to the same extent as non-medically frail enrollees are.
While the previous administration did not approve waiver requests to impose work requirements for Medicaid, recent policy statements have indicated interest in imposing work requirements.29 These requirements may pose significant challenges to Medicaid enrollees with behavioral health conditions, many of whom could struggle to pay premiums or purchase private coverage or whose disabilities may preclude them from working. Furthermore, Medicaid rarely provides full coverage of supported employment, which is an evidence-based practice shown to increase employment in competitive jobs; without this benefit, people with behavioral health problems could face challenges complying with work requirements. Furthermore, it is not yet clear if medically frail enrollees would be eligible for exemptions to work requirements in the proposed policy changes.
Restructuring Medicaid Financing
In addition to limiting enhanced federal financing for the Medicaid expansion population, the House bill has proposed limiting federal financing for Medicaid through a per capita cap. Unlike current law where eligible individuals have an entitlement to coverage and states are guaranteed federal matching dollars with no pre-set limit, the proposal under consideration could eliminate both the entitlement and the guaranteed match to achieve budget savings and to make federal funding more predictable. To achieve budget savings, federal funding limits would be set at levels below expected levels if current law were to stay in place. In exchange for these federal caps, proposals could allow states to impose enrollment caps or waiting lists or reduce eligibility levels or offer states other increased flexibility to design and administer their programs. The proposal does not specify the rules for state matching payments or what core federal eligibility and coverage standards would be changed.
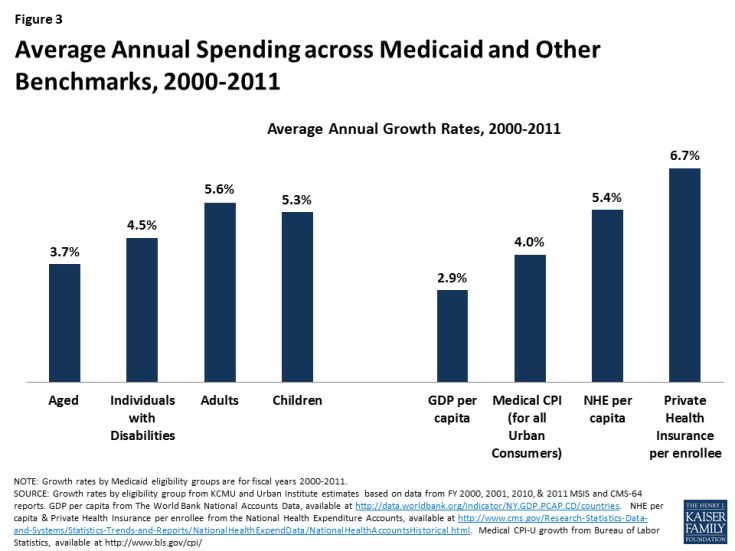
The proposal could substantially limit federal funds available to states to help them cover and finance behavioral health services. On March 13, 2017, the Department of Health and Human Services released a letter highlighting the Department’s aim to increase state flexibility and opportunities for state-level innovation. While states could gain new flexibility under the proposed plan, it is not clear what actions states could take to preserve benefits and enrollment that they cannot already do under federal Medicaid law.30 Medicaid spending is already relatively low (largely due to lower payment rates31), growing at rates below private health insurance and national health expenditures between 2000 and 2011 (Figure 3). Faced with more limited federal dollars, states could face incentives or pressure (due to limited budgets) to maximize the limited federal funding they would receive. These incentives may mean trimming benefit packages to lower per enrollee spending.
Given the relatively high cost among the population with behavioral health needs,32 and the high share of Medicaid program spending for behavioral health, it is likely that such populations or services would be a target for cuts under the proposed plan. Even though per capita caps are set at the average spending level for an eligibility group, there are significant variations even within states. Individuals with behavioral health conditions typically have greater service use and spending than other enrollees,4 making them among the costliest enrollees within an eligibility category. As such, policy actions to help states administer programs within the average per capita allotment for the group could disproportionately impact people with behavioral health needs.
For example, cuts to services considered “ancillary,” such as peer support, non-emergency transportation, non-clinical services, and prescription drugs, could have significant implications for individuals with behavioral health conditions, who rely heavily on many of these services. In particular, pressures to cut spending on prescription drugs would disproportionately affect behavioral health care, as central nervous system agents, which include psychiatric medications, are the largest drug class of prescription drugs, both in terms of total number of prescriptions and total spending.33 Furthermore, because states are no longer required to include essential health benefits in their ABPs, states may choose to exclude behavioral health services from the list of covered services for the Medicaid expansion population. Other potential changes, such as cuts to provider payment, could hinder provider participation in Medicaid, which could exacerbate the already limited availability of behavioral health providers who accept Medicaid. Notably, cuts that affect individuals with behavioral health needs could ultimately shift these costs to State Mental Health Agencies, which bear responsibility for financing services for people with no source of coverage for the services they need.
Furthermore, there is also substantial variation across states with regard to per enrollee spending. Under the proposed changes, the growth in federal Medicaid funding would not adjust for differences in underlying state health care costs; thus, enrollees living in costlier states could be especially impacted by per capita caps. In response to increased pressure to reduce costs, states with higher spending may be incentivized to reduce eligibility and coverage for optional groups, many of which include enrollees with behavioral health conditions.
Lastly, proposed changes to Medicaid could limit states’ ability to develop new models of care, respond to emerging health issues, or respond to changing economic conditions. Medicaid’s open-ended financing has enabled it develop innovative approaches to increasing community integration for enrollees with behavioral health conditions. It has also enabled Medicaid programs to respond to recent events such as the Great Recession, which saw an uptick in mental distress,34 or the recent opioid crisis, making the program a key component of the nation’s response to developing behavioral health crises. Because federal funding would be capped on a per person basis and limited to a pre-set growth rate, it would not change in response to new models of care and unforeseen events.
Conclusion
As research has shed light on the importance of addressing behavioral health in order to improve health outcomes and decrease costs, treatment of behavioral health conditions has become a greater priority for providers and policymakers. Medicaid has been an important resource for many low-income individuals with behavioral health conditions, and recent policy changes, including Medicaid expansion, federal parity rules, and service delivery changes, have further facilitated access to care. However, the proposal to limit the enhanced federal financing for the Medicaid expansion population and to limit federal financing for Medicaid through a per capita cap has important implications with regard to eligibility, coverage, access, and costs. Understanding the unique and complex needs of enrollees with behavioral health conditions, as well as the ways these proposals could affect the providers and systems that care for them, is a key component of evaluating the potential impact of this proposal.
This brief draws on a paper that was written as part of a series of papers commissioned by the Scattergood Foundation. The original paper can be found at: www.scattergoodfoundation.org.