Where is Medicaid Spending Headed? – Fact Sheet
Medicaid Enrollment and Spending Growth
Overview
In 1995, Medicaid provided health and long-term care for 34.8 million low-income, elderly, and disabled Americans at a cost of $157.3 billion, $151.8 billion for services and $5.5 billion for administration. After expanding considerably in the early 1990’s, Medicaid spending and enrollment growth have slowed markedly. Medicaid spending growth has declined from 22.4 percent per year to 9.5 percent per year between 1992 and 1995. Preliminary data suggest the growth rate for 1995-96 has fallen dramatically to about 3 percent; however, spending from 1996-2002 is projected by the Urban Institute to grow at 7.4 percent.
Beneficiary Growth: 1988-1995
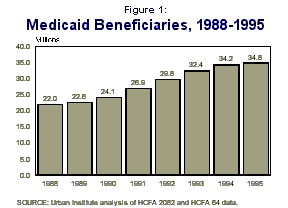
Medicaid enrollment growth has risen steadily over the last seven years. Between 1988 and 1995, the number of Medicaid beneficiaries grew 58 percent, from 22.0 million to 34.8 million (Figure 1). In part, the recession increased welfare and thus Medicaid enrollment. But much of this growth occurred between 1992 and 1994 and resulted largely from federal and state expansions in coverage of low-income pregnant women and children.
In addition, greater coverage of people with AIDS and actions that expanded SSI eligibility for disabled children increased coverage of disabled Medicaid beneficiaries. Eligibility expansions to assist low-income Medicare beneficiaries also increased the number of elderly Medicaid beneficiaries.
In recent years enrollment growth has leveled off. From 1992 to 1994, the number of beneficiaries grew 7.6 percent per year; the growth rate was only 1.8 percent between 1994 and 1995.
Future Medicaid Enrollment:
During the next six years, Medicaid enrollment is predicted by the Urban Institute to continue to grow at 1.6 percent, a rate similar to that of 1994-95. This would result in a total of 40.4 million beneficiaries in 2002.
Cost Explosion: 1988-1992
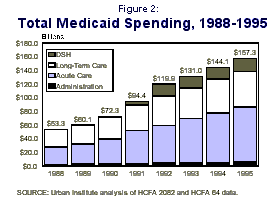
Between 1988 and 1992, Medicaid’s total (state and federal) costs more than doubled, growing from $53.5 billion in 1988 to $119.9 in 1992 (Figure 2). This growth rate of 22.4 percent per year made it one of the fastest growing components of state and federal budgets during that time. In 1988, federal spending on Medicaid accounted for about 2.5 percent of all federal spending; by 1992, Medicaid made up more than 5 percent of the federal budget.
Reasons Behind the Cost Explosion:
The rise in Medicaid’s costs between 1988 and 1992 was equally attributable to three factors: health care inflation, state financing practices (including the use of provider taxes and donations and disproportionate share hospital (DSH) payments) and expansions in enrollment due to legislative changes and the recession. Expansion in coverage of low-income women and children, the lowest cost Medicaid beneficiaries, accounted for most of the enrollment growth but only a fraction of the spending growth.
Spending Growth Slowdown: 1992-1995
Since 1992, Medicaid’s spending growth has slowed dramatically. Total Medicaid spending grew from $119.9 million in 1992 to $157.3 million in 1995–an average growth rate of 9.5 percent per year, substantially less than the 22.4 percent rate during the previous five years (Table 1).
Table 1: State and Federal Medicaid Expenditures, 1988-1995Spending (billions) Ave. Annual Growth Type of Spending 1988 1992 1995 1988-92 1992-95Total $53.5 $119.92 $157.3 22.4% 9.5% Benefits $50.6 $98.5 $132.8 18.1% 10.5% Acute $25.4 $55.5 $80.4 21.6% 13.1% Long-Term $25.1 $42.9 $52.3 14.3% 6.8% DSH $0.4 $17.5 $19.0 149.9% 2.7% Admin. $2.4 $3.9 $5.5 12.2% 12.6%
Reasons For Cost Slowdown:
Although it is difficult to quantify the precise contribution of each factor, the slowdown in the growth of Medicaid’s costs appears to be related to the following factors:
- Limitations on DSH: Federal legislation capped money available to states through DSH payments. After rising by more than 250 percent between 1991-92, DSH payments actually fell by 1 percent in 1992-93. Provider taxes and donations as financing mechanisms were also limited.
- Slower Enrollment Growth: After increases averaging 7.9 percent annually between 1988 and 1992, enrollment growth fell to 5.3 percent in the following three years. The earlier bursts in enrollemnt due to expanded eligibility for children and pregnant women have largely subsided. The improved economy and changes in AFDC also contributed to a slowing of enrollment growth.
- Slower Growth in Spending per Beneficiary: Declines in medical price inflation, enrollment of women and children into capitated managed care and limits on long-term care spending may have accounted for some of the slowdown in the growth of spending per beneficiary found among all beneficiary groups (Table 2).
Table 2: Average Spending per Beneficiary, 1988-1995Cost per Beneficiary Ave. Annual Growth Type of Beneficiary 1988 1992 1995 1988-92 1992-95All $2,298 $3,303 $3,816 9.5% 4.9% Elderly $5,794 $8,848 $10,166 11.2% 4.7% Blind & Disabled $5,619 $8,099 $8,685 9.6% 2.4% Families $848 $1,416 $1,728 13.7% 6.8%
Projected Spending: 1996-2002
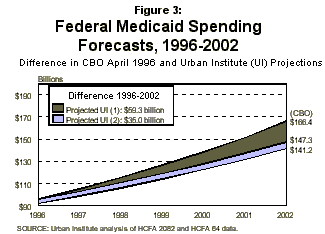
Although preliminary data show a slowdown in Medicaid spending growth from 1995 to 1996 to 3 percent, it is unlikely to remain this low in the future. Urban Institute projects Medicaid spending will increase 7.4 percent per year and will grow to $147 billion by 2002–$59 billion lowerthan CBO’s April 1996 baseline. If 1996 spending remains below the CBO baseline, total federal savings using the 7.4 percent growth rate could reach $94 billion from 1996 to 2002 (Figure 3). These findings suggest that Medicaid’s contribution to the federal deficit would be substantially smaller than predicted.
Source: Where is Medicaid Spending Headed? By John Holahan and David Liska, the Urban Institute, November 1996. Prepared for the Kaiser Commission on the Future of Medicaid.
Where is Medicaid Spending Headed?:Press Release Fact Sheet Report