The Implications of Federal SNAP Spending Cuts on Individuals with Medicaid, Medicare and Other Health Coverage
Nearly 53 million people of all ages in the United States live in households that experience food insecurity, meaning they are unable to access adequate food due to lack of money or other resources. The Supplemental Nutrition Assistance Program (SNAP) was established in 1964 as a federal aid program to address food insecurity among low-income households by providing a monthly benefit to help participants purchase food.
The GOP’s House and draft Senate budget reconciliation bill, known as the One Big Beautiful Bill Act, is working its way through Congress and would reduce federal spending on SNAP by $287 billion over 10 years. Cuts to SNAP would produce budgetary savings but could produce higher rates of food insecurity and poorer health outcomes in the long run. Several studies indicate that individuals who receive SNAP benefits have better health and lower rates of food insecurity than similar people who are eligible but not receiving these benefits. Food insecurity is associated with multiple chronic conditions, poorer self-reported health status, higher health care utilization, and lower rates of medication adherence.
In addition to SNAP cuts, the reconciliation bill would cut federal health program spending by more than $1 trillion over the next decade, including $793 billion from Medicaid and $268 billion from the ACA Marketplaces – the largest cuts to federal support for health programs in the nation’s history. According to Congressional Budget Office (CBO), the bill will increase the number of uninsured by 10.9 million within ten years. The combination of federal spending reductions on SNAP and health programs would mean many people are at risk of losing both food assistance and health coverage, primarily those enrolled in Medicaid.
This analysis, based on the U.S Census Bureau’s 2023 Survey of Income and Program Participation (SIPP), examines the distribution of SNAP recipients and rates of food insecurity, by source of coverage.
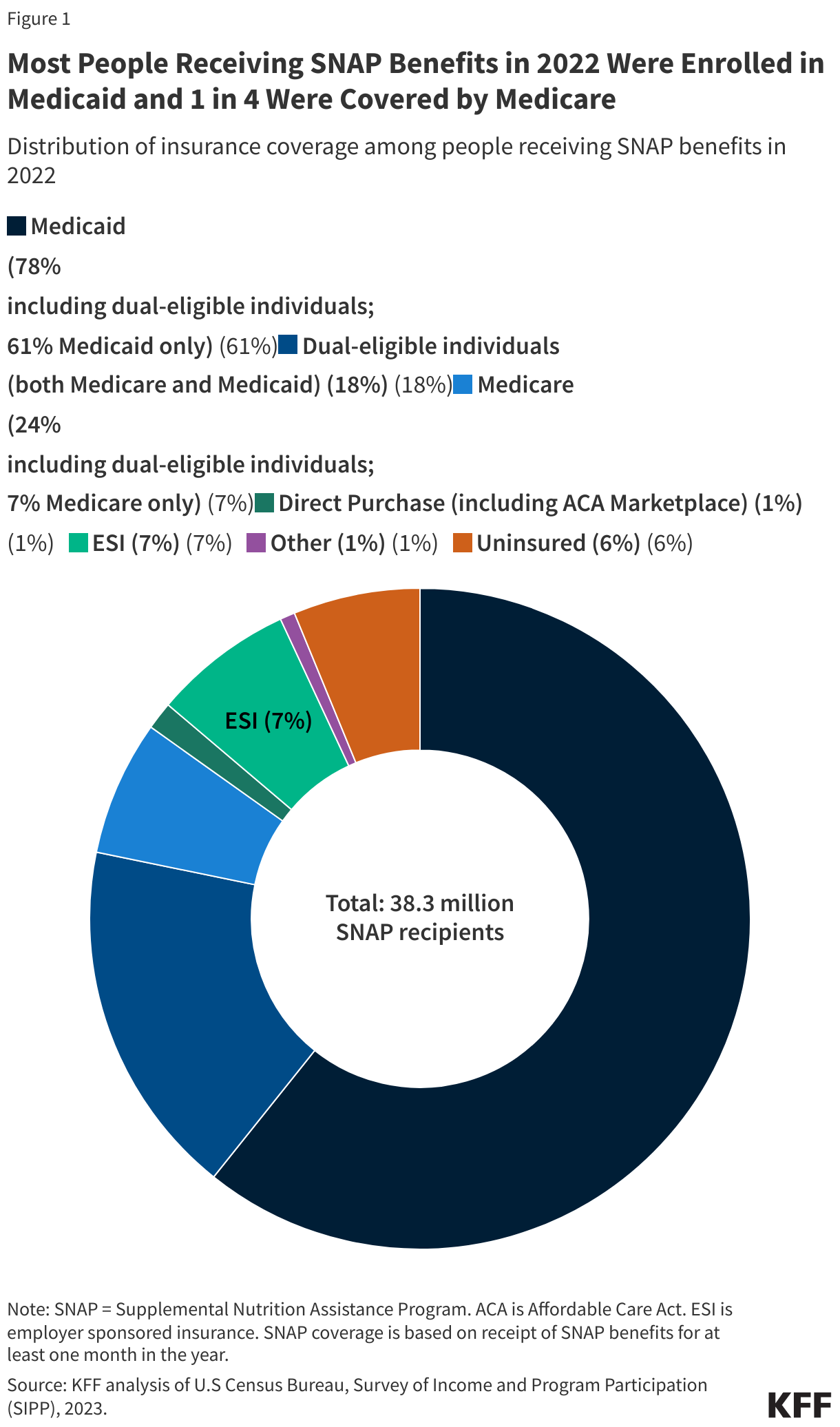
The majority (78%) of people who received SNAP benefits in 2022 were covered by Medicaid, including 18% who were covered by both Medicaid and Medicare.
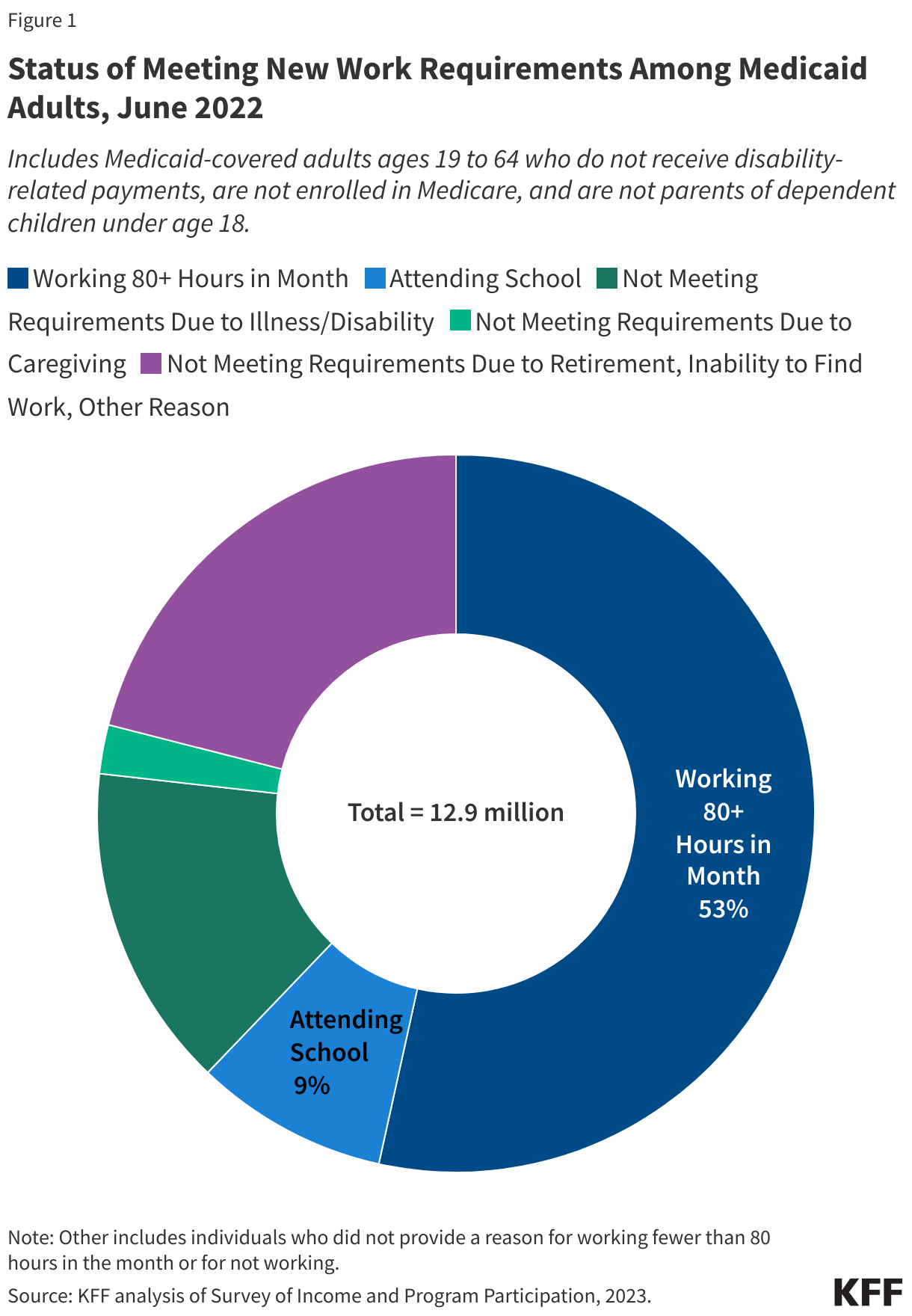
Nearly 30 million of the 38.3 million people receiving SNAP benefits in 2022 were enrolled in Medicaid (Figure 1). The overlap between the two programs reflects similar eligibility requirements for Medicaid and SNAP, though rules vary by state. Among Medicaid enrollees receiving SNAP benefits, 23.3 million were solely covered under Medicaid, while 6.7 million were also covered by Medicare (otherwise known as dual-eligible individuals). Medicaid was the primary source of coverage for children receiving SNAP, covering 88% of kids with SNAP, or approximately 13 million children.
A total of 9.2 million Medicare beneficiaries received food assistance benefits under SNAP, accounting for one in four (24%) SNAP recipients. Most Medicare beneficiaries with SNAP benefits (18% or 6.7 million) had supplemental coverage under Medicaid. In 2023, one in four Medicare beneficiaries lived on incomes below $21,000 per person.
Over 500,000 people who purchase health insurance coverage directly (mostly from ACA Marketplaces) received SNAP benefits in 2022. In addition, 2.4 million SNAP recipients were uninsured in 2022.
Some Medicaid enrollees who receive food assistance benefits from SNAP could lose both health insurance coverage and financial resources to supplement their food budgets as a result of the reconciliation bill.
Proposed changes in eligibility rules in both SNAP and Medicaid may jeopardize some people’s access to both adequate food and health care if various provisions of the bill take effect, in part because there is a significant overlap in eligibility requirements for Medicaid and SNAP across states. Four in 10 (40%) Medicaid enrollees receive SNAP benefits, compared to only 3% of those without Medicaid.
Recent KFF polling shows a majority of the public is worried about the consequences of significant reductions in federal Medicaid spending, and half of low-income adults reported their households having difficulty affording necessities, including food.
A CBO analysis of the House version of the reconciliation bill estimates that households in the lowest income decile could see a 4% decrease in resources by 2034, primarily due to changes in Medicaid and SNAP, while the highest income decile households would see a 2% increase in resources as a result of proposed tax cuts.
Many people enrolled in the programs slated for cuts in the reconciliation bill, including Medicaid and those receiving SNAP benefits, already experience food insecurity.
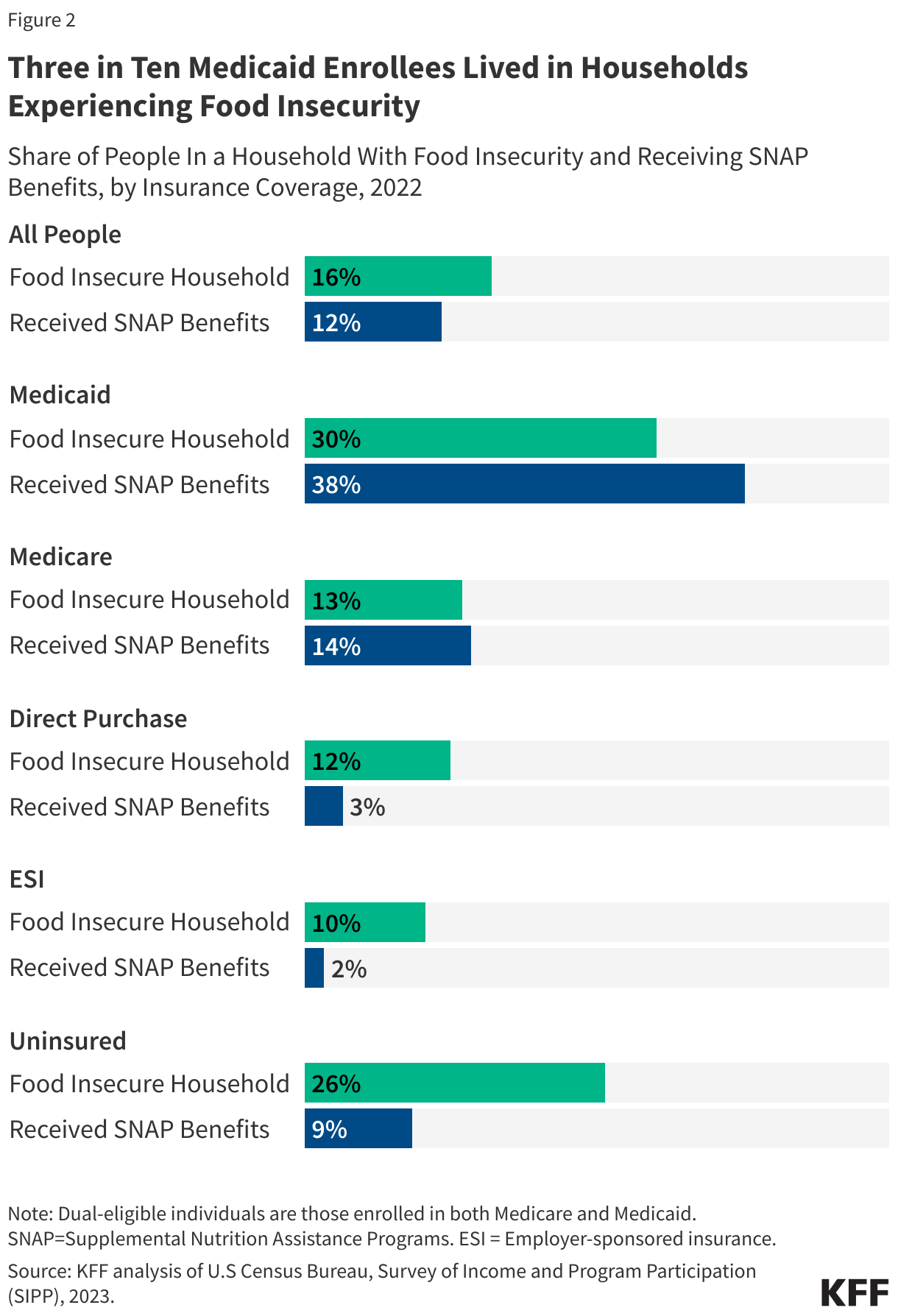
People living in households with and without SNAP report that they had problems affording food over the prior year. Overall, 52.8 million people lived in a household with food insecurity in 2022, including 30% of people enrolled in Medicaid (22.4 million), 13% of Medicare beneficiaries (8.7 million people), 26% of the uninsured, and 12% with coverage they purchased directly, including from ACA Marketplaces (Figure 2). A total of 14.6 million children lived in a household that experienced food insecurity in 2022.
Many households already struggling with food insecurity may be at risk of reduced SNAP benefits, or losing eligibility, at the same time they face new eligibility restrictions or higher costs for their healthcare. 22.4 million people enrolled in Medicaid experienced food insecurity, including 9.3 million children. Nearly 2 million people enrolled in direct purchase coverage in 2022 lived in a household experiencing food insecurity. Many of these households will face higher premium costs if Marketplace enhanced premium tax credits expire at the end of this year, increasing demands on some household budgets. Almost half of ACA Marketplace enrollees have incomes below 150 percent of the federal poverty level, $23,475 for an individual in 2025.
Among the 52.8 million people who reported food insecurity in their households in 2022, more than two-thirds (73%, or 38.6 million) were not receiving SNAP benefits. At the same time, even SNAP participants can experience food insecurity. Among the 38.3 million people receiving SNAP benefits in 2022, 37% (14 million) reported being unable to access adequate food due to lack of money or other resources.
Proposed cuts to SNAP could increase the number of people experiencing food insecurity and worsen affordability challenges for those already struggling to access food, as well as for those at risk of losing health insurance due to other changes in the legislation.
Methods
This analysis is based on the U.S Census Bureau’s 2023 Survey of Income and Program Participation (SIPP). The SIPP is a nationally representative, household-based survey that provides data on social program participation and eligibility, income, and labor force participation of the U.S non-institutional population. Health insurance source coverage was identified in the SIPP based on coverage held for at least 6 months of the calendar year. Respondents may report having more than one type of coverage in the survey instrument. In Figure 1, individuals are sorted into only one category of insurance coverage using the following hierarchy (Medicare, Medicaid, Direct Purchase (ACA), employer-sponsored insurance (ESI), Other, Uninsured). Throughout the analysis, dual enrolled Medicare and Medicaid people are included in both estimates unless specified otherwise. SIPP data provides estimates of multiple units of interest (i.e., person, family, or household). This analysis considers the person the unit of analysis.
SNAP coverage is defined as at least one month of coverage during the reference period (2022 calendar year), and the question is asked of all people.
The composite food security measure in the SIPP is assessed at the household-level, with responses provided by the household respondent applying to the entire household. The measure is based on the US Department of Agriculture Six-Item Short Form of the Food Security Survey Module and respondents were asked about the 2022 calendar year:
- The food that I [or we] bought often or sometimes didn’t last, and [I/we] didn’t have money to get more.
- I [or we] couldn’t afford to eat balanced meals often or sometimes of the time
- In the past 12 months, did you or other adults in your household ever cut the size of meals or skip meals because there wasn’t enough money for food?
- How often did you cut the size of your meals?
- [Among respondents with positive responses to questions 1-3] In the last 12 months, did you ever eat less than you felt you should because there wasn’t enough money for food?
- [Among respondents with positive responses to questions 1-3] In the last 12 months, were you ever hungry but didn’t eat because there wasn’t enough money for food?