The Role of Medicaid and Impact of the Medicaid Expansion for Veterans Experiencing Homelessness
Issue Brief
Key Takeaways
Veterans remain at higher risk of experiencing homelessness than the rest of the population. Although some veterans have access to health care through the Department of Veterans Affairs (VA), Medicaid plays an important role for this population, particularly those experiencing homelessness. This brief describes Medicaid’s role for veterans experiencing homelessness and provides insight into how the Affordable Care Act (ACA) Medicaid expansion has affected their coverage and access to care. It shows:
- Veterans are more likely to experience homelessness than the overall population, and those experiencing homelessness have significant health needs. Veterans make up about 9% of the adult population but constitute nearly 12% of persons experiencing homelessness. Veterans who are poor; have a disability, chronic health condition, or mental health issue; lack support networks; and/or have a history of substance use are at particularly high risk of experiencing homelessness.
- The ACA Medicaid expansion has led to increased coverage and access to care for veterans, including those experiencing homelessness. Medicaid plays an important role covering veterans who would otherwise be uninsured and supplements Medicare, private, VA or military coverage for others. Medicaid is particularly important for veterans experiencing homelessness who have high rates of chronic health conditions, disabilities, mental health issues, and alcohol or substance use disorders. Research shows that there have been gains in coverage among veterans overall since implementation of the Medicaid expansion. Moreover, data from Health Care for the Homeless (HCH) projects, which are clinics that serve individuals experiencing homelessness, show positive impacts of the Medicaid expansion for veterans experiencing homelessness. Specifically, data reported by nine HCH projects show higher rates of Medicaid coverage among veteran patients at HCH projects in expansion states than in non-expansion states. Further, four HCH projects able to report data for 2013 and 2016 show significant increases in the share of veteran patients covered by Medicaid over the period. Personal stories from veterans experiencing homelessness who gained coverage under the expansion and are connected to HCH projects also illustrate how Medicaid improved their access to care and health, providing greater stability in their overall lives.
- Restructuring of Medicaid at the federal level or through waivers sought by states would have significant implications for veterans experiencing homelessness. Reductions in Medicaid, particularly loss of the Medicaid expansion, would likely result in many of these individuals becoming uninsured and going without needed care, which would lead to greater instability in their lives. Moreover, increases in out of pocket costs and/or work requirements could pose significant challenges for these individuals given their complex health needs and limited resources.
Introduction
This brief provides an overview of Medicaid’s role supporting health coverage and care for veterans, including those experiencing homelessness. In addition, through data from Health Care for the Homeless (HCH) projects and individual stories, it examines how the Affordable Care Act (ACA) Medicaid expansion has affected coverage and care for veterans experiencing homelessness.
Homelessness among Veterans
Although the number of veterans experiencing homelessness on a given night has declined by 17% since 2015,1 veterans remain more likely to experience homelessness than the overall population.2 Veterans make up about 9% of the adult population but constitute nearly 12% of persons experiencing homelessness.3 While the exact number of veterans experiencing homelessness is unknown given the difficulty of tracking the homeless population, the U.S. Department of Housing and Urban Development (HUD) estimates that, in 2015, nearly 133,000 veterans experienced sheltered homelessness at some point throughout the year.4 They also estimate that on a given night in January 2016, 40,000 veterans experienced homelessness, including over 13,000 unsheltered homeless veterans living on the streets.5 ,6
Veterans experiencing homelessness have significant health needs that are often complicated and exacerbated by lack of housing. Veterans who are poor; have a disability, chronic health condition, or mental health issue; lack support networks; and/or have a history of substance use are at particularly high risk of experiencing homelessness.7 Veterans experiencing homelessness are disproportionately male (91%), young (43%), Black (39%), and live in a city (74%) as compared to the overall veteran population.8 Approximately 53% of veterans experiencing homelessness have some type of disability as compared to 28% of the overall veteran population.9 Homelessness is also associated with chronic health conditions, as these conditions can be a cause or preceding factor to homelessness or be the result of or exacerbated by lack of stable housing.10 Given the high needs of these individuals, homelessness is often associated with high rates of emergency department use and inpatient hospitalizations, and health complications.11
The Role of Medicaid and Impact of the Medicaid Expansion
The #ACA #Medicaid expansion has led to increased coverage for veterans, including those experiencing homelessness.
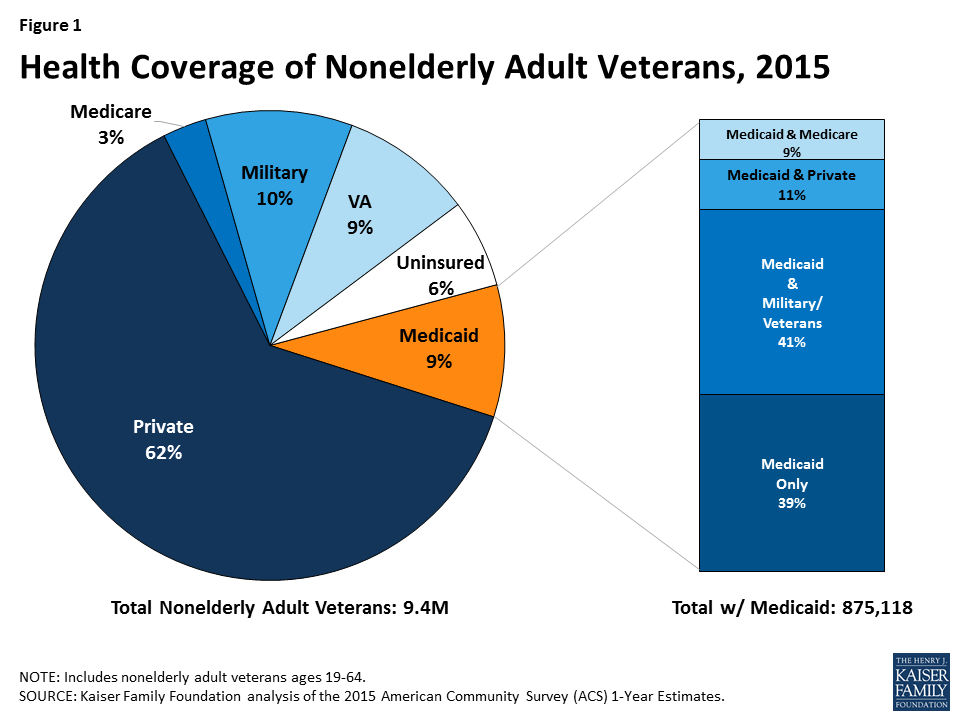
Medicaid plays an important role covering veterans who would otherwise be uninsured and supplements Medicare, private, VA or military coverage for others. Although the U.S. Department of Veterans Affairs (VA) offers health benefits to veterans, not all veterans can access care through the VA. Some veterans do not qualify for health benefits through the VA, some may not enroll even if they do qualify, and/or some veterans live outside of an area where a VA facility is located.12 As such, other sources of coverage, including Medicaid, are important for veterans. Medicaid covers 875,000, or nearly 1 in 10, nonelderly adult veterans overall (Figure 1). For nearly two in five nonelderly adult veterans (39%) with Medicaid coverage, Medicaid is their sole source of coverage. Medicaid serves as a supplement to military/VA, private, or Medicare coverage for the remaining 61% of veterans with Medicaid coverage, enhancing their ability to receive needed care and reducing out-of-pocket costs for care. Medicaid is particularly important for veterans experiencing homelessness who often lack access to other sources of coverage and have high rates of chronic health conditions, disabilities, mental health issues, and alcohol or substance use disorders.
Medicaid coverage among veterans has increased since implementation of the ACA Medicaid expansion in 2014, contributing to improvements in access to care and health outcomes. The ACA Medicaid expansion to adults with incomes up to 138% of poverty made many adults, particularly adults without dependent children, newly eligible for the program in the 32 states that have adopted the expansion. Research shows that since implementation of the expansion, Medicaid coverage among veterans has increased and their uninsured rate has fallen.13 ,14 ,15 Research also shows that the Medicaid expansion has had a positive impact on access to and utilization of care among the low-income population, and that nonelderly veterans with Medicaid coverage fare better on measures of access and utilization than those who are uninsured.16 ,17 As presented below, data from HCH projects and personal stories from individuals further show that the Medicaid expansion has had positive impacts on coverage, access to care, and health outcomes for veterans experiencing homelessness.
Data from Health Care for the Homeless Projects
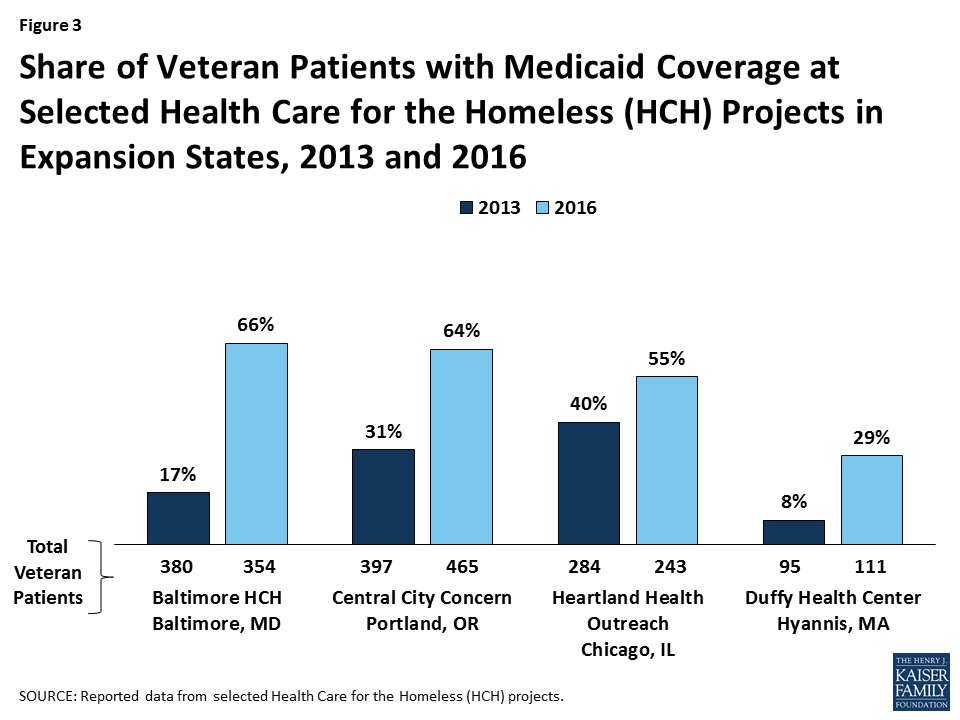
Data from a select number of HCH projects suggest that the Medicaid expansion led to broader Medicaid coverage among veterans experiencing homelessness. Specifically, data reported by nine HCH projects show that those in Medicaid expansion states have a much larger share of the veterans they serve covered by Medicaid (55%) compared those in non-expansion states (5%) (Figure 2). Moreover, four HCH projects in expansion states that were able to report data for both 2013 and 2016 show that the share of veterans they serve who have Medicaid coverage significantly increased from 2013 to 2016 (Figure 3).

Personal Stories from Veterans Experiencing Homelessness
Personal stories from veterans experiencing homelessness who enrolled in Medicaid under the expansion and are connected to care through HCH projects also illustrate how Medicaid has improved their access to care and health outcomes. These experiences show that Medicaid coverage has enabled these individuals to access preventive health services; receive treatment for serious health issues, like cancer; and manage chronic health conditions and recovery from substance use disorders. Without the Medicaid expansion, many of these individuals would likely be uninsured. In contrast, a profile from a veteran experiencing homelessness who remains uninsured because his state has not adopted the Medicaid expansion shows how he continues to face challenges accessing the care he needs.
Medicaid was instrumental in supporting C.J.’s diagnosis and treatment for prostate cancer.
C.J., a 62-year old man, spent 11 years in the Army, including two tours in Germany training new recruits. He returned home with his wife and children, working at Fort Meade before moving to Baltimore where he worked in construction. Two years ago, C.J. started to notice pain and swelling in his pelvis, which worsened over time and made his job lifting heavy equipment more difficult. He had health insurance through his employer, but he could not afford the out-of-pocket costs to access care. Eventually, C.J. had trouble walking and had to take unpaid medical leave. After several months, he was laid off, losing both his job and his insurance and ultimately landing up with nowhere to live. After connecting to a health center, he was enrolled in Medicaid under the Medicaid expansion. Following several tests and biopsies, C.J. was diagnosed with prostate cancer. Medicaid enabled him to access the daily radiation treatments he needed to treat his cancer and transportation to get to these appointments. C.J. is hoping to be declared in remission at his next appointment and is grateful that he was able to access the care he needed through Medicaid.
“I don’t want to think about what would have happened without Medicaid. It would be a fast road to digging my grave.”
Medicaid helps C.L. manage his chronic health conditions and supports his continued recovery from substance use.
C.L. is a 53-year old man who served in the Army National Guard from 1980-1982 and then served on active duty from 1982-1983. He completed two additional years with the National Guard between 1991 and 1993. C.L. worked for the city government for nearly 20 years and had stable housing and employer-sponsored insurance. Escalating mental health and substance use issues led to his loss of employment in 2012 and, with it, his health insurance. Though he previously qualified for VA benefits, he could no longer access them due to changes in eligibility rules based on length of service. As such, C.L. became uninsured. C.L. has been homeless since 2012 and is currently staying at a transitional housing program in Baltimore City. He has diabetes, high blood pressure, depression, and an opioid use disorder. In 2014, C.L. gained Medicaid coverage through the Medicaid expansion. He has found it a great relief to know that the physical and behavioral services he needs are covered.
“I just got a prostate check and that was normal. I had a colonoscopy too, and they found non-cancerous polyps so I have to go back to check that soon. If I were uninsured, I’d worry a lot about whether I could afford to get those cancer tests.”
Medicaid enabled W.B. to fully recover from a work injury and receive treatment for his behavioral health needs, allowing him once again to seek work.
W.B. is a 51-year old man living in Portland, Oregon who served in the Navy for a year. After his service, he worked in construction until 2016, when he fell off a ladder on the job and tore his rotator cuff. He needed surgery but was laid off, losing his income, health insurance, and housing all at once. Fortunately, W.B. was connected to a health center that quickly enrolled him in Medicaid under the Medicaid expansion. With Medicaid, W.B. was able to get surgery for his shoulder and physical therapy. During his recovery, W.B. stayed at a medical respite program because he had no safe place to recuperate, which Medicaid also covered. During his stay at the respite center, W.B. also began treatment for depression and alcohol use. W.B. is now recovered and looking to get back to work.
With Medicaid, R.M. can access the physical and behavioral services he needs to stay healthy.
R.M. is a 56-year old man who was in the 101st Airborne division with the U.S. Army between 1979 and 1983. He currently struggles with mental health and substance use disorders. R.M. needed colostomy surgery in 2009, when he was previously uninsured. He was able to obtain the surgery through a charity care arrangement with a local hospital but wore a colostomy bag for two years because he could not find anyone willing to do a reversal surgery to remove it while he was uninsured. With Medicaid, R.M. is now able to obtain the services he needs, including therapy to support his recovery and other mental health needs; eyeglasses and regular eye exams; and screenings and preventive care, including an HIV test and flu shots.
“Losing Medicaid would make me worry a lot–I was blessed to get a charity case on my colostomy, but that doesn’t happen a lot. You don’t find many places that do charity work.”
Medicaid provided K.B. timely treatment for colon cancer and enabled him to address other longstanding conditions.
K.B. is a 65-year old man in Chicago, Illinois who spent two years in the Army during the 1970s. He worked in phone sales for many years. However, after his mother died in 1987, he lost his job and home and faced challenges with alcohol use. K.B. stayed intermittently with his son, then his brother, and then was living in a tent in a local park. He was previously uninsured but enrolled in Medicaid in 2015, after visiting a local health center; though he is now 65, he is not yet enrolled in Medicare.Later in 2015, K.B. gained stable housing through a veteran’s initiative. In 2016, K.B. was diagnosed with colon cancer. His Medicaid coverage enabled him to access timely treatment, and he is now cancer-free. He also had surgery to relieve a spinal cord compression, helping him regain better use of his arms and hands. With Medicaid, K.B. also is receiving the care and medications he needs to manage his high blood pressure, PTSD, and depression; maintain his recovery from alcohol use; and continue to monitor his cancer.
“If I didn’t have Medicaid, it would be all downhill because there are not a lot of places that can afford to supply the medications that I need. Hypertension killed both my parents, so I need to take care of myself and see the doctor regularly.”
Without Medicaid, K.S. remains uninsured and is going without needed care and eyeglasses as well as the preventive care he would like for peace of mind.
K.S. is a 42-year old man who served in the National Guard between 1994-2001. He worked construction and metal fabrication jobs for most of his life, but was laid off in 2016. He exhausted his savings and became homeless. Outreach workers in Jacksonville, Florida found K.S. sleeping on the beach when they connected him to a health center and a shelter placement. K.S. currently works day labor jobs and is searching for full employment, having recently received an Associate’s degree from Florida State College.K.S. suffers from neuropathy in his right leg, which gives him problems with balance and muscle spasms, and has also recently started to get migraines. Because K.S. is uninsured, the local health center is trying to obtain a charity care voucher so that he can get a CAT scan at the local hospital. He used to wear glasses, but they were broken when he became homeless and he is not able to replace them. Having Medicaid would facilitate K.S.’s ability to get care to treat his existing conditions as well as the preventive care that he would like for peace of mind.
“It would be nice to get a regular check-up…. I know there’s a lot of things if they are caught in time, they can be managed, but if not, they can be catastrophic….You just hope there’s nothing wrong, but it’s a scary thing not knowing.”
Looking Forward
Though rates of homelessness have been on the decline among the veteran population, veterans remain overrepresented among the homeless population and at high risk of experiencing homelessness. Medicaid plays an important role for veterans, covering some who would otherwise be uninsured and supplementing Medicare, private, VA or military coverage for others. Medicaid coverage is particularly important for veterans experiencing homelessness who often lack access to other coverage options and have high rates of chronic health conditions, disabilities, mental health issues, and alcohol or substance use disorders. The ACA Medicaid expansion led to coverage gains among veterans, including those experiencing homelessness, providing them access to a broad range of services to manage ongoing physical and behavioral health conditions and support recovery from alcohol and substance use disorders when necessary.
Restructuring of Medicaid at the federal level or through waivers sought by states would have significant implications for veterans experiencing homelessness given their significant health needs and limited resources. Reductions in Medicaid, particularly loss of the Medicaid expansion, would likely result in many of these individuals becoming uninsured and going without needed care, which would lead to greater instability in their lives and make it more difficult for them to pursue work and stable living arrangements. Moreover, increases in out of pocket costs and/or work requirements could pose particular challenges for these individuals. Similarly, these individuals also would have difficulty affording out of pocket costs for care if moved to private coverage.
This brief was prepared by Samantha Artiga and Petry Ubri with the Kaiser Family Foundation and Barbara DiPietro of the National Health Care for the Homeless (HCH) Council. The authors express their deep appreciation to the veterans who shared their time and experiences to inform this brief.
Endnotes
- The U.S. Department of Housing and Urban Development, Obama Administration Announces Nearly 50 Percent Decline in Veteran Homelessness [Website], August 1, 2016, Accessed August 24, 2017, https://portal.hud.gov/hudportal/HUD?src=/press/press_releases_media_advisories/2016/HUDNo_16-117. ↩︎
- U.S. Department of Housing and Urban Development and U.S., Department of Veterans Affairs, Veteran Homelessness: A Supplemental Report to the 2009 Annual Homeless Assessment Report to Congress, (Washington, DC: HUD and VA, 2010), https://www.hudexchange.info/resources/documents/2009AHARveteransReport.pdf. ↩︎
- The U.S. Department of Housing and Urban Development, The 2015 Annual Homeless Assessment Report (AHAR) to Congress: Part 2: Estimates of Homelessness in the United States, (Washington, DC: HUD, October 2016), https://www.hudexchange.info/onecpd/assets/File/2015-AHAR-Part-2.pdf. ↩︎
- Ibid. ↩︎
- The U.S. Department of Housing and Urban Development, Obama Administration Announces Nearly 50 Percent Decline in Veteran Homelessness [Website], August 1, 2016, Accessed August 24, 2017, https://portal.hud.gov/hudportal/HUD?src=/press/press_releases_media_advisories/2016/HUDNo_16-117. ↩︎
- U.S. Department of Veterans Affairs, VA Programs for Homeless Veterans, (Washington, DC: VA, January 2017), https://va.gov/homeless/Homeless_Programs_General_Fact_Sheet_JAN_2017.pdf. ↩︎
- Jack Tsai and Robert A Rosenheck, “Risk Factors for Homelessness Among US Veterans,” U.S. Department of Veterans Affairs, public Access Author Manuscript, Epidemiological Review 37, (2015):177-195, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4521393/pdf/nihms-709743.pdf. ↩︎
- The U.S. Department of Housing and Urban Development, The 2015 Annual Homeless Assessment Report (AHAR) to Congress: Part 2: Estimates of Homelessness in the United States, (Washington, DC: HUD, October 2016), https://www.hudexchange.info/onecpd/assets/File/2015-AHAR-Part-2.pdf. ↩︎
- Ibid. ↩︎
- Fargo J, Metraux S, Byrne T, Munley E, Montgomery AE, Jones H, et al. “Prevalence and risk of homelessness among US veterans,” Prev Chronic Dis 2012;9:110112. ↩︎
- Thomas P O’Toole, Erin E Johnson, Matthew L Borgia, and Jennifer Rose, “Tailoring Outreach Efforts to Increase Primary Care Use Among Homeless Veterans: Results of a Randomized Controlled Trial,” Journal of General Internal Medicine 30, 7 (July 2015):866-898. ↩︎
- Sidath Viranga Panangala, Health Care for Veterans: Answers to Frequently Asked Questions, (Washington, DC: Congressional Research Service, April 2016), https://fas.org/sgp/crs/misc/R42747.pdf. ↩︎
- Michael Dworsky, Carrie M Farmer, and Mimi Shen, Veterans’ Health Insurance Coverage Under the Affordable Care Act and Implications of Repeal for the Department of Veterans Affairs, Prepared for the RWJ Foundation and the NY State Health Foundation, (Santa Monica, California: RAND Corporation, September 2017), http://nyshealthfoundation.org/uploads/resources/veterans-health-insurance-coverage-under-the-affordable-care-act.pdf. ↩︎
- Kaiser Family Foundation, Medicaid’s Role in Covering Veterans, (Washington, DC: KFF, June 2017), http://modern.kff.org/infographic/medicaids-role-in-covering-veterans/. ↩︎
- Jennifer Haley, Genevieve Kenney, and Jason Gates, Veterans Saw Broad Coverage Gains Between 2013 and 2015, Prepared with support from the Robert Wood Johnson Foundation, (Washington, DC: Urban Institute, April 2017), https://www.urban.org/sites/default/files/publication/89756/2001230-veterans-saw-broad-coverage-gains-between-2013-and-2015.pdf. ↩︎
- Larisa Antonisse, Rachel Garfield, Robin Rudowitz, and Samantha Artiga, The Effects of Medicaid Expansion under the ACA: Updated Findings from a Literature Review, (Washington, DC: Kaiser Family Foundation, February 2017), http://modern.kff.org/medicaid/issue-brief/the-effects-of-medicaid-expansion-under-the-aca-updated-findings-from-a-literature-review/. ↩︎
- Kaiser Family Foundation, Medicaid’s Role in Covering Veterans, (Washington, DC: KFF, June 2017), http://modern.kff.org/infographic/medicaids-role-in-covering-veterans/. ↩︎