Pulling It Together: Changing the HIV Testing Message
In 2006 the CDC began recommending routine HIV testing in health care settings for everyone between the ages of 13 and 64. Annual testing is recommended for people at highest risk. Our 2011 survey of Americans and HIV released last week — our eighth comprehensive survey of its kind — shows that more people are talking with their doctors about being tested for HIV, but that reported rates of actually getting tested have remained virtually flat for many years.
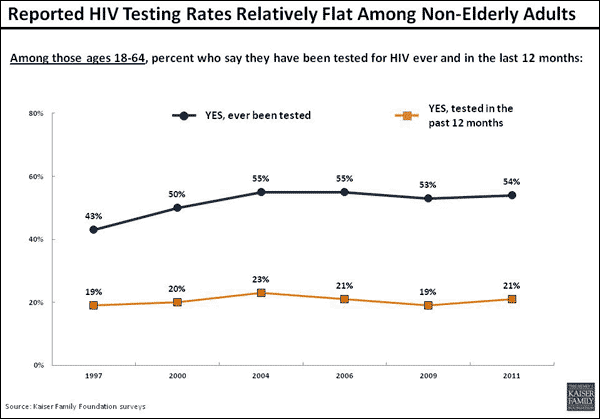
As a result, the CDC says that 21% of the more than 1.1 million Americans with HIV do not know their status. This means they are not getting ever more effective treatments that can forestall the onset of AIDS and delay or stop the progression of the disease. They are potentially unknowingly passing the virus on to their partners.
People in higher risk groups are a special concern (we could not survey all of the highest risk groups). Forty-three percent of non-elderly African Americans report being tested in the last year (and 77% ever); 47% of African Americans ages 18-29 (71% ever); and 26% of all adults ages 18-29 (48% ever). In addition, 45% of African Americans 30-49 report being tested in the last year. These rates are generally somewhat higher than for the public as a whole, but they have also remained stubbornly flat in recent years. It is reasonable to ask what the achievable testing rate is for any population group given barriers to testing such as stigma, denial of personal risk and obstacles to access to care, but now there are new reasons to do better.
Just last month, researchers found that HIV-positive people who take combination antiretroviral therapy (ART) can reduce the risk of transmitting the virus to their HIV-negative partners by 96 percent. We have known for a while that getting HIV-positive people into treatment can save their own lives. Now there is a broader public health benefit to getting people at-risk tested and into treatment. Doing so would not only help those individuals and their partners, but potentially change the course of the epidemic throughout a community.
So, what can be done to get HIV testing rates moving up?
CHANGE THE MESSAGE. Great emphasis has been placed for many years on making testing a routine part of people’s interaction with the medical system. This was originally part of a strategy to counteract stigma by making it easier and more routine to get an HIV test. The approach helped push testing rates up initially (the fact that 48% of young adults have been tested at some point in their lives is a public health success), but now years of flat testing rates suggest that something new is needed.
The research we now have on early detection and treatment offers a powerful new public health imperative for increasing the number of at-risk people who get tested. It also presents an opportunity to turn the HIV testing message on its head: from a “routine” part of a medical visit, to a proactive, even urgent message that gives people at risk a reason to want to be tested despite the barriers they sometimes face. The fact now is (and the message can be), that “HIV NEED NOT BECOME AIDS ANYMORE IF IT IS DETECTED EARLY”. People at risk, and their partners, now have a real incentive to overcome stigmatizing attitudes and denial of risk, but only if they know clearly what early detection and treatment can do.
EXPAND THE MEDIUM FOR THE MESSAGE. A more assertive testing message should work equally well for all testing “messengers” – physicians, family, friends and partners, community-based services providers, and the media. Providers are important messengers and medical settings are a key part of a multipronged strategy, but despite the emphasis on testing in medical settings they may not be the most important part.
Many of the most at risk groups avoid institutional settings (who can blame them?), and do not have medical encounters in any given year. In 2008, the last year for which there are national data, 42% of 18-29 year olds and 52% of African American 18-29 year olds did not visit a medical office, clinic or outpatient department during the year. A third of African American 18-29 year olds did not have a visit in the previous two years.
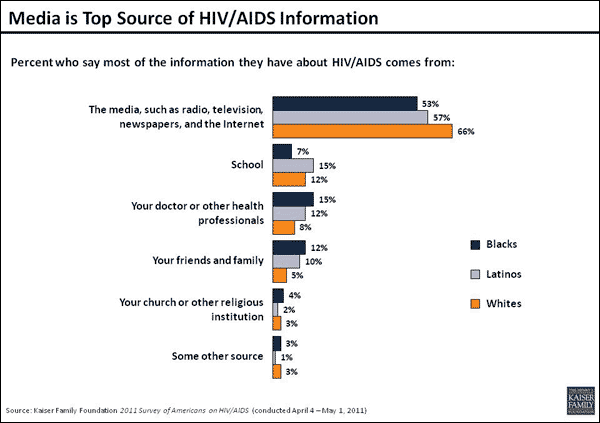
First and foremost, and I suppose for better and worse, people get their information primarily from media. In our new national survey people of all ages said the media was their number one source of information about HIV/AIDS, far ahead of schools, family and friends, and notably, physicians. They also said they wanted more information about HIV, including about testing. Medical settings and medical providers are a vital part of any testing strategy, but the data suggest that the media is our single most important messenger when it comes to promoting HIV testing. And based on my experience developing and operating prevention programs over thirty years, I personally believe that community based programs are most effective when it comes to reaching highest risk groups.
TARGET,TARGET,TARGET. Everybody involved in HIV/AIDS knows that a key to slowing the epidemic is to more effectively reach the highest risk groups and communities. So too, there is a need to target testing messages to the most at risk groups and communities. The new national HIV strategy developed by the Obama Administration, for the first time, recognizes this by calling for focusing HIV/AIDS resources overall on populations and areas of greatest need as a matter of national policy. Recently, the CDC mounted a focused effort to intensify testing in areas with higher infection rates, producing good results. It was noteworthy that inthe CDC initiative the chance of finding someone positive was about twice ashigh in nonmedical sites as in medical ones.
It was not good news to see in our new survey that HIV testing rates remain flat, even for higher-risk groups. But there is now a new imperative to change the testing message, potentially saving the lives of individuals at risk while at the same time changing the course of the epidemic in the most hard hit communities. I cannot, of course, be sure how effective a more proactive testing message will be unless we try it. But we know that testing rates for the higher risk groups have not moved in years and the research on early detection and treatment has now reached a stage where a new message that gives people a reason to want to be tested makes sense. It should be one that reaches out to people and communities at greatest risk and is less dependent on finding them in medical settings.
