The independent source for health policy research, polling, and news.
New Analysis Finds Inpatient Coronavirus Treatment Costs Could Top $20K for Patients with Employer Coverage
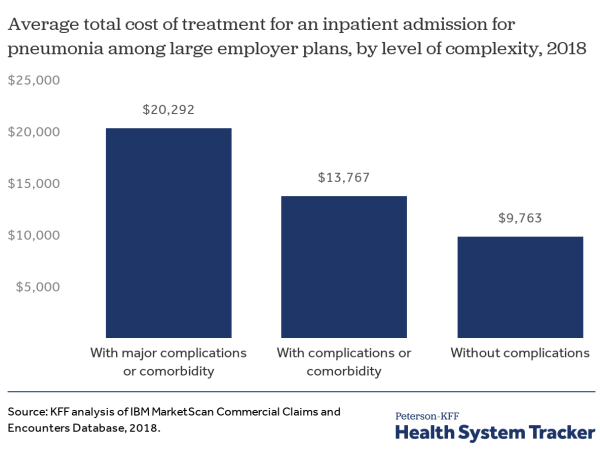
A new issue brief estimates potential coronavirus treatment costs to large employer health plans and their enrollees by looking at typical spending for hospital admissions for pneumonia. The analysis finds that, for pneumonia admissions with major complications and comorbidities, the average total cost is $20,292. In comparison, the average cost for a patient with no complications or comorbidities is $9,763.
Average out-of-pocket costs could exceed $1,300 for all admitted patients, including those without complications or comorbidities.
While complications and deaths associated with the novel coronavirus (COVID-19) are concentrated among older adults, who will have different estimated costs under Medicare, many younger patients are expected to become seriously ill as the pandemic spreads in the United States. Those covered by employer-sponsored plans can expect to have copayments and deductibles associated with coronavirus testing waived by their insurers, but will still be responsible for the out-of-pocket costs associated with their treatment.
The analysis is part of the Peterson-KFF Health System Tracker, an online information hub dedicated to monitoring and assessing the performance of the U.S. health system.
For more data, analysis, polling and journalism on the COVID-19 pandemic, visit our special resource page on kff.org.