Nursing Home Staff Vaccination Rates Vary Widely by State as Vaccination Mandates Take Effect
Nearly one in four COVID-19 deaths has been in a long-term care facility since the start of the pandemic. Due to the disproportionate impact of COVID-19 on this population, nursing home residents and staff were prioritized to receive the vaccine when the vaccine rollout began in Winter 2020-2021. Since then, CMS has implemented a health care worker vaccination mandate for providers that participate in Medicare and/or Medicaid. Although some states have sued to challenge this rule, it was recently allowed to take effect by the Supreme Court.
In part due to the litigation, facilities in different states have different deadlines to comply with the new rule. CMS guidance requires staff to have received their first vaccine dose or have a pending or approved exemption by January 27th in 26 states (25 states plus D.C.), including 25 that did not sue to challenge the rule, and Florida, where courts refused to block the rule. Additional CMS guidance sets a February 14th deadline for staff to have received their first vaccine dose or have a pending or approved exemption request after the Supreme Court allowed the rule to take effect in 24 other states that challenged the rule. Finally, CMS guidance sets a February 21 deadline for Texas, where a lawsuit was dismissed after the Supreme Court’s decision. All guidance specifies that if by the dose one deadline, a facility is above 80%, and has a plan to achieve a 100% single-dose staff vaccination rate within 60 days of the deadline, they will not be subject to additional enforcement action.
This data note presents completed vaccination and booster rates among nursing home staff, by state. This analysis does not categorize states or facilities by compliance since deadlines for all states have not passed and facility-level data is lagged. This analysis presents data on completed vaccinations at the state-level rather than at the facility-level, though this policy will be enforced at the facility-level. Future analyses will evaluate the share of facilities in each state in compliance with the rule once compliance deadlines for both doses have passed.
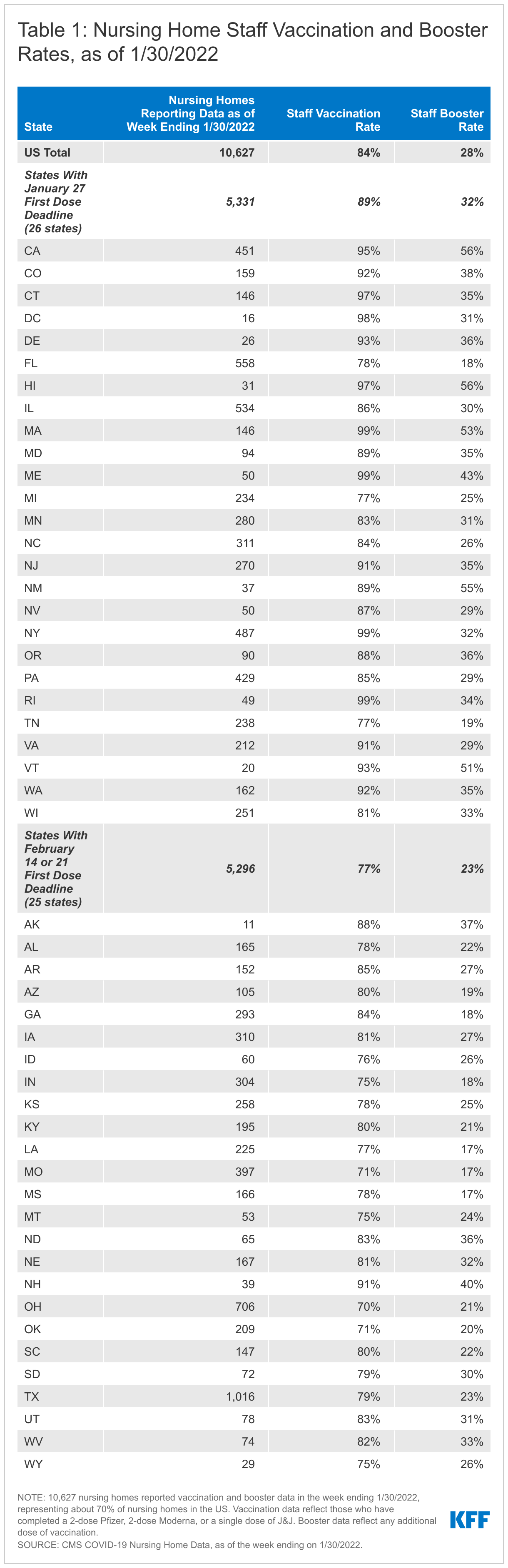
Completed vaccination refers to those who have completed a 2-dose Pfizer, 2-dose Moderna, or a single dose of J&J. Booster data reflect any additional dose of vaccination. This analysis uses federal nursing home data as of January 30th, 2022 to calculate staff vaccination and booster rates among the 26 states with the January 27th first-dose deadline, and as a baseline for assessing the remaining 25 states with first-dose deadlines that follow in February. The analysis is based on 10,627 nursing homes reporting complete data (approximately 70% of all nursing homes). The data in this piece were reported after the January 27 dose one deadline in 26 states; the dose one deadline has not yet passed in the remaining 25 states, as noted above. Table 1 provides detailed state-level data.
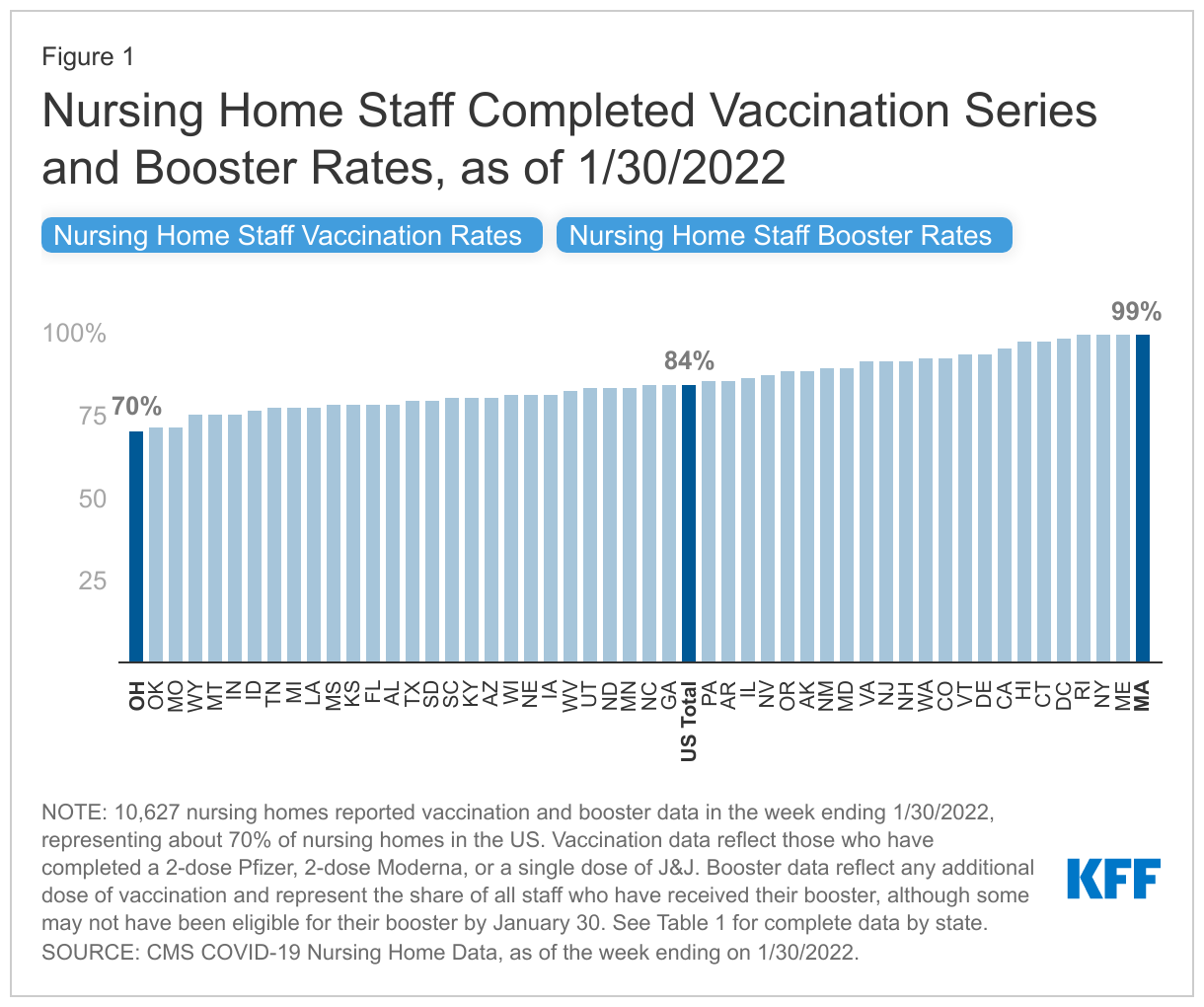
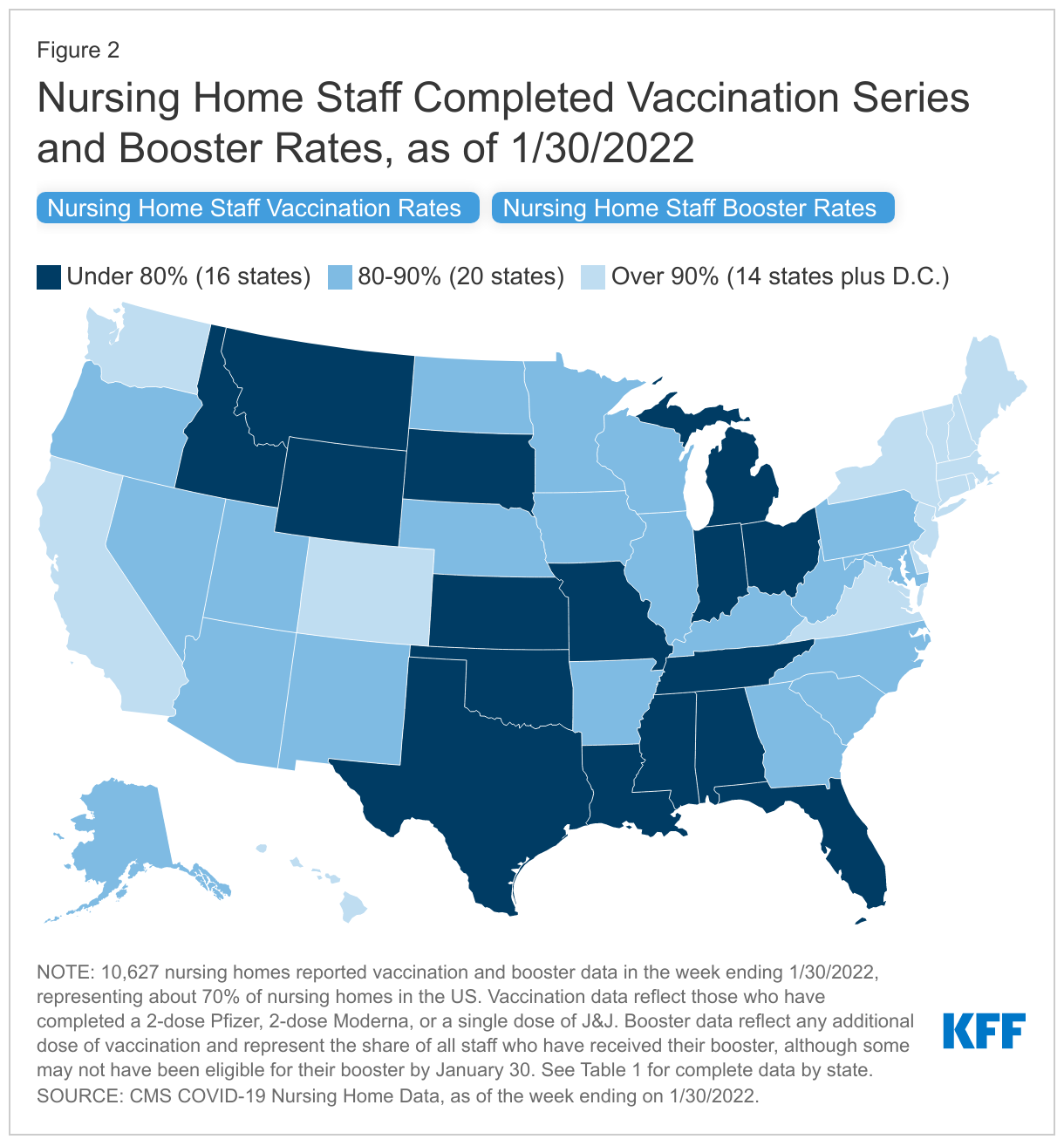
As the deadline for first doses for health care workers passed in 25 states + D.C., and approached in the remaining states, nursing home staff completed vaccination rates varied widely by state, ranging from 70% in Ohio to 99% in Maine, Rhode Island, New York, and Massachusetts for the week ending January 30th, 2022 (Figure 1 and Table 1). Nationally, the nursing home staff vaccination rate is about 84%. Twenty-three states reported staff vaccination rates higher than the national average. Of these 23 states, 14 states plus D.C. reported staff vaccination rates of over 90%. Four states reported a near-universal staff vaccination rate of 99%. Twenty-six states reported staff vaccination rates lower than the national average, with 16 of these states reporting even lower staff vaccination rates under 80% (Figure 2). All 16 of these states are located in the South, Midwest, and Rocky Mountain regions of the U.S. (Figure 2). CMS cited variation in staff vaccination rates by state and region as a factor leading to the adoption of the rule.
The 26 states that were subject to the January 27th deadline for the first dose of the COVID-19 vaccine reported higher completed vaccination rates (89%) than the 25 states subject to the February deadlines (77%) (Table 1). In the 26 states where staff were required to receive their first dose by January 27th, the completed staff vaccination rate was 89% as of January 30th. Nursing homes in the remaining 25 states subject to the February deadlines – February 14th (24 states) and February 21st (1 state) – reported a lower staff vaccination rate of 77%, likely reflecting a mix of federal mandate deadlines not yet passing, a lack of state and/or local mandates, and different degrees of vaccine hesitancy among staff.
While the new CMS rule does not require staff to receive booster shots, nursing home staff booster rates also vary across states, ranging from 17% in three states (Louisiana, Missouri, and Mississippi) to 56% in California (Figure 1 and Table 1). Nationally, booster rates among nursing home staff are about 28%. These values represent the share of all staff who have received their booster, although some who were vaccinated more recently may not have been eligible for their booster by January 30th (the most recent data published). Individuals who received the Pfizer-BioNTech or Moderna vaccines become eligible for boosters five months after completing their primary vaccination series. Individuals who received Johnson & Johnson’s Janssen vaccine are eligible for boosters two months after receiving their shot. States with the earlier dose one vaccination deadline also report higher booster rates than states with a later dose one vaccination deadline. State level variation in booster rates may reflect differences in attitudes or hesitancy about boosters.
In the aftermath of the Supreme Court’s decision allowing the rule to take effect, litigation challenging this rule continues in Louisiana, where 14 states challenging the rule are seeking to add new claims to their lawsuit, and Tennessee and Virginia are seeking to join the challengers' case against the federal government. The rule, which was issued as interim final, may also be revised as CMS reviews public comments before issuing a final rule. As the various deadlines pass, nursing homes could be subject to enforcement of this rule through a number of mechanisms, including civil monetary penalties, denial of payments, and termination of participation from the Medicare and Medicaid programs. CMS guidance emphasizes that their “primary goal is to bring health care facilities into compliance” and termination would likely occur “only after providing a facility with an opportunity to make corrections and come into compliance.” When issuing the rule, CMS acknowledged that some staff may leave their jobs because they do not want to receive the vaccine but cited examples of vaccine mandates adopted by health systems in Texas and Detroit and a long-term care parent corporation with 250 facilities as well as the New York state health care worker mandate, all of which resulted in high rates of compliance and few employee resignations. As with other Medicare and Medicaid federal provider requirements, state surveyors will have primary responsibility for enforcing the rule as part of routine inspections. However, CMS has notified states that it may reduce the amount of federal money that states receive to support facility oversight and redirect those funds to support federal oversight activities if states do not include facility compliance with all federal requirements in their oversight.