The Comstock Act: Implications for Abortion Care Nationwide
Key Takeaways
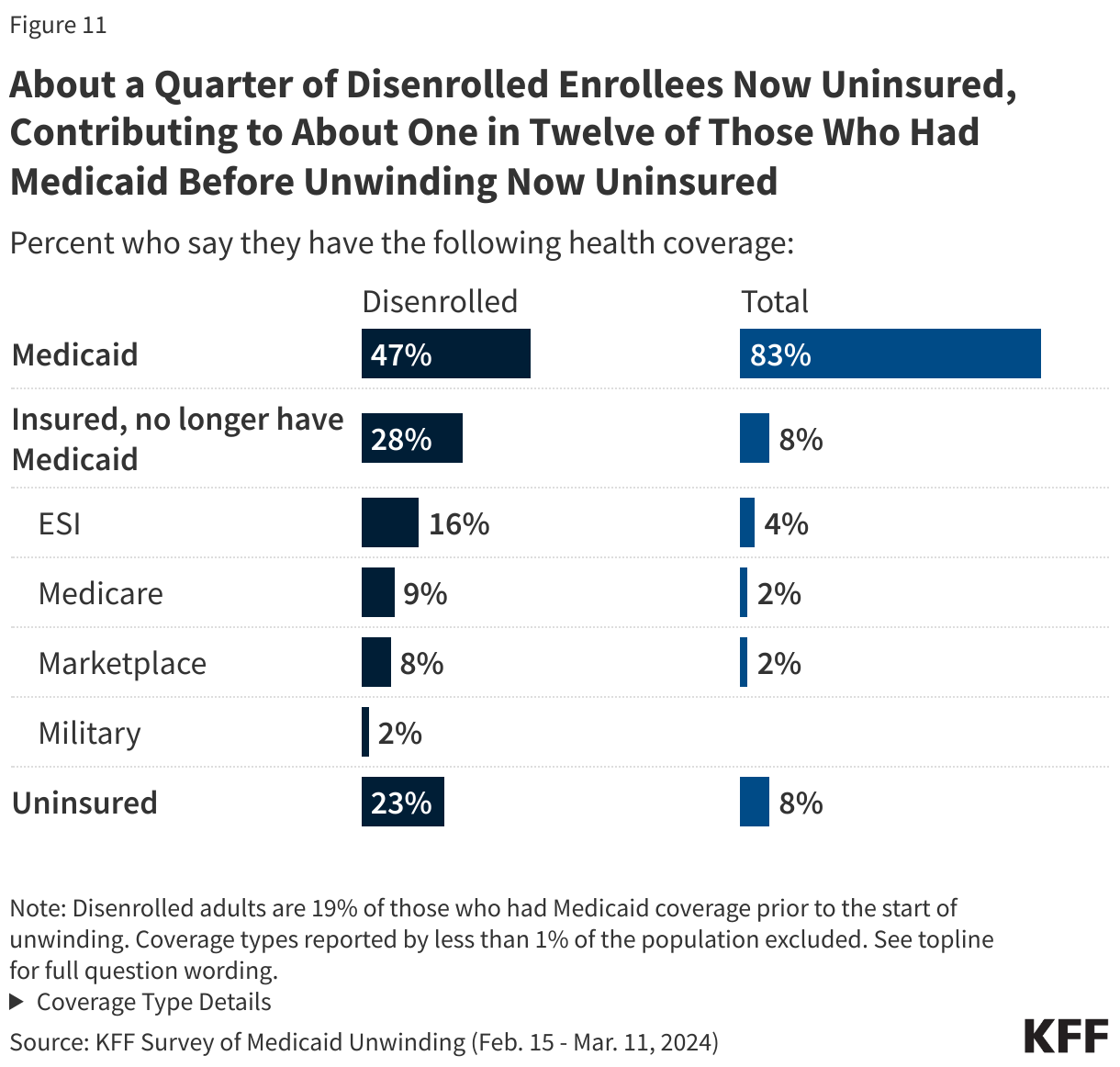
- The Comstock Act – an 1873 anti-vice law banning the mailing of obscene matter and articles used to produce abortion – could be used by a future presidential administration opposed to abortion rights to sharply restrict abortion nationwide. A literal interpretation of the Act could potentially also apply to materials used to produce all abortions, not just medication abortions; would not have exceptions; and could affect other medical care, such as miscarriage management.
- The Biden Administration’s Department of Justice has determined the Comstock Act only applies when the sender intends for the material or drug to be used for an illegal abortion, and because there are legal uses of abortion drugs in every state including to save the life of the pregnant person, there is no way to determine the intent of the sender. This interpretation, however, is not binding on future administrations.
- Anti-abortion organizations have asked federal courts to interpret the Comstock Act as a ban on the mailing and distribution of mifepristone– one of two drugs in the medication abortion regimen. While former President Trump has not publicly endorsed the enforcement of the Comstock Act, enforcement of the law has been outlined as a strategy recommended by conservative and anti-abortion leadership and may emerge as a key issue in the 2024 presidential election.
- The current law has been revised by Congress three times since it was passed, and prior efforts to remove the abortion references from the law have failed to garner sufficient legislative support. There are renewed efforts in the current Congress to repeal the law, but they face long odds given the current composition of the Congress.
Introduction
Abortion looms large in the 2024 presidential election with 1 in 8 voters saying abortion is most important to their vote. While Congress is unlikely to pass any abortion laws either protecting or restricting abortion, there is already a dormant law on the books that a future administration might seek to enforce. The Comstock Act – an 1873 anti-vice law banning the mailing and receiving of obscene matter, as well as articles used to produce abortions – could be used to sharply restrict abortion nationwide. In the aftermath of the Supreme Court’s Dobbs decision, anti-abortion activists have argued in federal court that the Comstock Act prohibits the mailing of the medication abortion pill, mifepristone, directly to patients, as well as the general distribution of the medication to physicians, hospitals, and pharmacies. A handful of cities and counties have passed local ordinances requiring their residents to comply with Comstock, making it unlawful to mail and/or receive abortion medications and “abortion related paraphernalia.” A literal interpretation of the 1873 law would have a far-reaching impact on the availability of abortion nationwide.
The Biden Administration’s Department of Justice (DOJ) maintains that this law should not be interpreted literally and therefore has not enforced it. However, the DOJ of an administration that is hostile to abortion, as is the presumed Republican candidate Donald Trump, may interpret the Comstock Act differently and choose to prosecute those who send or receive materials distributed for abortion care. In the recent oral argument for a case involving the FDA’s approval and regulation of the abortion drug mifepristone, Justices Alito and Thomas signaled that they would likely uphold the enforcement of the Comstock Act inviting future attention by the Courts. This brief provides background on the Comstock Act, reviews how it has been interpreted by the Biden Administration’s DOJ, and considers how it could be enforced by an administration that is hostile toward abortion to severely restrict the distribution of drugs and supplies used for abortion, with implications for abortion access in all states across the country.
What Are the Origins of the Comstock Act?
In 1873 – at the behest of anti-vice crusader, Anthony Comstock – Congress enacted a law banning the interstate mailing and receiving of “obscene, lewd, or lascivious” writings, or “any article or thing designed or intended for the prevention of conception or procuring an abortion.” In 1909, Congress enacted a similar law banning the use of express company or common carrier (such as FedEx or UPS) to mail “any drug, medicine, article, or thing designed, adapted, or intended for preventing conception or producing abortion, or for any indecent or immoral use.” These laws came to be known collectively as the Comstock Act. The scope of what constituted obscene or lewd material was far broader at the time, and in the late 1800s and early 1900s, the Comstock Act was used to prosecute a wide array of violations. These ranged from intent to mail magazines that detailed birth control methods, to the mailing of condoms and medical textbooks with illustrations of human anatomy, and even the mailing of letters discussing dating among unmarried people.
Over the last century, the application and enforcement of the Comstock Act has changed drastically and it has not been applied to the mailing of abortion materials in the last fifty years. In the 1930s, federal appeals courts ruled that the Act did not apply to the mailing of contraceptive materials if their intended use was not illegal. Federal court rulings throughout the years also limited the reach of the obscenity provisions. In 1930, a federal appeals court ruled that sex education materials did not inherently violate the Comstock Act and two Supreme Court rulings – one from 1957 and another from 1971 – narrowed the scope of material that is considered obscene, limiting the reach of the Act.
Congress has only amended the U.S. Code in a way that meaningfully affects these sections few times over the years. Following the landmark Supreme Court ruling in Griswold v. Connecticut (1965), Congress removed the references to contraception from the Comstock laws in 1971. In 1996, Section 1462 was extended to prohibit the sending of obscene materials through the internet. That same year – and in three subsequent years (1997, 1999, and 2001) – lawmakers introduced bills to remove the abortion language from the Comstock Act, but these proposed laws never made it out of committee or received a floor vote.
Although the reach of the Comstock Act has been severely limited since its enactment, most of the original act remains in the United States Code as Sections 1461 and 1462 of Title 18. Section 1461 declares as nonmailable matter:
“Every article or thing designed, adapted, or intended for producing abortion, or for any indecent or immoral use; and
Every article, instrument, substance, drug, medicine, or thing which is advertised or described in a manner calculated to lead another to use or apply it for producing abortion, or any indecent or immoral purpose . . .”
Section 1462 prohibits express companies or other common carriers from sending “any drug, medicine, article or thing designed, adapted, or intended for producing abortion.”
How Has the Biden Administration Approached Enforcement Post-Dobbs?
Although violations of most federal crimes are under the purview of the Department of Justice and its agencies, the U.S. Postal Service (USPS) also has partial authority to enforce the law. Due to its involvement in enforcing the Act, after the Supreme Court released its opinion in Dobbs, the General Counsel of the USPS asked the DOJ to address whether the Comstock Act criminalizes the mailing of mifepristone, one of the two medications used in the medication abortion regimen.
In response, the DOJ released a slip opinion, concluding that 18 U.S.C. § §1461 and 1462 – the Comstock Act – “does not prohibit the mailing, or delivery or receipt by mail, of mifepristone or misoprostol where the sender lacks the intent that the recipient of the drugs will use them unlawfully.” In support of its opinion, the DOJ cites federal appeals courts’ decisions from 1930s cases regarding the mailing of condoms and other articles that may be used as contraceptives, and information about contraceptives. In these cases, the courts held that these items had legal uses under state law and the mailing of these items is not illegal if the sender does not intend for them to be used unlawfully.
Additionally, the DOJ notes that because this more limited construction of the Comstock Act came long before the Supreme Court’s decisions in Griswold (1965) and Roe (1973) – the latter of which recognized a constitutional right to abortion – it is not dependent on the Court’s “recognition of constitutional rights regarding the prevention or termination of pregnancy.” In other words, the Court’s reversal of Roe does not change the applicability of Comstock, because appeals courts had been interpreting it in a much more limited fashion before the Court recognized a right to abortion.
Anti-Abortion Advocates’ Recent Reliance on the Comstock Act to Attempt to Limit Access to Abortion
Alliance for Hippocratic Medicine v. FDA
Among other claims they make about FDA’s approval of mifepristone, plaintiffs in this case argue that the FDA violated the Comstock Act when it approved the medication and its distribution, and when it modified the rules to prescribe and dispense, removing the in-person dispensing requirement and allowing mifepristone to be mailed directly to patients. Danco – the manufacturer of Mifeprex, the original brand of mifepristone that was approved in 2000 – and the FDA argues that the Biden DOJ’s interpretation of Comstock is correct, and that the mailing of mifepristone is not illegal if the sender did not intend for the medication to be used illegally. Neither the District Court for the Northern District of Texas, where this case originated, nor the Fifth Circuit Court, ruled on the Comstock arguments in the case. The Supreme Court heard oral arguments on March 26, 2024, and while it seems the court may hold that the plaintiff doctors and organizations do not have legal standing, Justices Alito and Thomas raised questions about the applicability of the Comstock Act. Justice Alito asked Solicitor General Prelogar, representing the FDA, why the FDA had not contended with the law in its decisions on expanding access to mifepristone through the mail. “This is a prominent provision. It’s not some obscure subsection of a complicated, obscure law,” Justice Alito said. “Everybody in this field knew about it.” Justice Thomas asked the lawyer representing Danco, the manufacturer, how she responds to an argument that mailing mifepristone and advertising it would violate the Comstock Act. These Justices seemed to be signaling that they would uphold enforcement of the Comstock Act if a future administration prosecutes the distribution and mailing of mifepristone and a challenge is brought to the Supreme Court.
2023 REMS and Letter from Attorneys General about Mailing Mifepristone
After the 2023 change to the Mifepristone Risk Evaluation Mitigation Strategies (REMS), which allowed certified pharmacies to dispense Mifepristone, and the subsequent announcements from Walgreens and CVS that they would dispense the medication through their pharmacies in states where abortion is legal, the Attorneys General from 20 different states sent a letter to Walgreens and CVS executives stating that federal law – through the Comstock Act – criminalizes the mailing of medication abortion. Federal crimes are under the purview of the federal government through its law enforcement agencies. Despite this, the letter from the Attorneys General argues that they have the ability to enforce the Comstock Act. In making this argument, they rely on the Racketeer Influenced and Corrupt Organizations Act (RICO). RICO’s definition for racketeering activity includes a reference to the obscenity provisions of 18 U.S.C. §§1461-1465 – the section of the U.S. Code that contains the Comstock Act. RICO itself contains civil remedies, which allow persons injured in their business or property by a violation of the Act to sue in federal district court. The Attorneys General argue that this civil remedy provision in the law would allow them to bring a civil action against anyone who violates their interpretation of the Comstock Act.
The Comstock Act has never been used to prosecute someone for mailing or distributing mifepristone. Further, it does not appear that the provisions that pertain to abortion in the Comstock Act are applicable under RICO, since RICO’s definition of racketeering specifically refers to the “obscene matter” provisions of the Comstock Act. And, the civil remedies are for persons injured by a violation of RICO, but it is unclear how the mailing of mifepristone would injure the business or property of a state. Still, this letter got considerable media attention. Walgreens and CVS have now begun to stock mifepristone in a handful of states and have indicated that they plan to expand to other states where it is permissible. This effectively limits the availability of the drug to states where abortion is not banned and where there is no state law limiting the dispensing of the drug in a pharmacy setting.
City and County Ordinances
Since November 2022, five cities – one in Illinois and four in New Mexico – and three counties – all in New Mexico – have passed ordinances requiring their residents to comply with 18 U.S.C. § § 1461 and 1462, which they are interpreting as criminalizing the shipping and/or receiving of abortion medications and “abortion related paraphernalia.” These ordinances are unlike older ordinances banning abortion within city or county limits, because they purport to enforce federal law and, thus, per their defenders, take precedence over state law protecting the right to abortion.
The Heritage Foundation Project 2025
The Heritage Foundation, a conservative think tank, has released its vision for 2025, Mandate for Leadership, which “represents the work of more than 350 leading conservatives and outlines a vision of conservative success at each federal agency during the next administration.” This blueprint includes a “Campaign to Enforce the Criminal Prohibitions in 18 U.S.C. §§ 1461 and 1462 [The Comstock Act] Against Provider and Distributors of Abortion Pills that Use the Mail.”
Could the Comstock Act Be Used to Restrict Abortion Access Nationally?
A future administration that is hostile to abortion rights may interpret the Comstock Act differently than the Biden Administration and could choose to prosecute those who send or receive materials used to cause abortions. Although many of the arguments presented by anti-abortion advocates focus on the mailing and distribution of mifepristone, a literal interpretation of the Comstock Act would implicate more than just this medication. It could also bar the distribution of misoprostol – the other drug used in the medication abortion regimen – and materials used in procedural abortions, such as dilators and suction catheters, and even gloves and speculums. This broad interpretation could also affect the distribution of medications that jeopardize pregnancies, even when they have other uses, such as methotrexate. A literal interpretation of the Comstock Act would criminalize sending and receiving shipments of any materials necessary to provide any kind of abortion care without exceptions, although it would be practically impossible to enforce.
An interpretation of the Comstock Act that bans the distribution of abortion medications and medical tools would also carry heavy implications for miscarriage management and other obstetric and gynecologic care, limiting clinicians’ ability to manage these conditions and thus pose additional threats to the health of pregnant people. Medical treatment for miscarriage management is often the same as abortion care, and the same kinds of materials that are used to provide abortion are also used to provide other obstetric and gynecologic care. A literal reading of the Comstock Act would criminalize the mailing of materials that can be used to provide abortion care without differentiating or accounting for whether these materials will be – or are intended to be – used to provide abortions. This means that if a medication, article, or material can be used to provide abortion care, mailing it will be illegal regardless of the intent of the sender or the recipient.
Since a literal application of the Comstock Act would have adverse effects on medical care well beyond abortion or pregnancy, and be nearly impossible to enforce, a future administration hostile to abortion may opt to enforce the Comstock Act selectively. The Project 2025 conservatives have proposed that the next DOJ enforce the Comstock Act by criminalizing the distribution of mifepristone or misoprostol or targeting enforcement on the distributors of abortion-related materials and abortion providers, with impacts in every state.
Alternatively, a future administration could take an even more limited approach to restrict distribution and focus on the FDA’s actions. Even if the Supreme Court were to dismiss the challenges to FDA’s rules allowing for mifepristone to be mailed directly to patients, an anti-abortion administration may try to revoke this FDA policy and once again only permit doctors to dispense the drugs in-person to patients, citing it is a violation of the Comstock Act to mail the drug. Recent data suggests that 16% of abortions are medication abortions provided via telehealth where the drugs are mailed directly to patients following a telehealth consultation.
On the Horizon
Abortion has emerged as a key issue in the 2024 presidential election, just as it has been in key state races since the Supreme Court overturned Roe v. Wade. The Biden Administration’s DOJ’s opinion on the Comstock Act is not binding on future administrations. There is currently interest among abortion rights legislators in Congress to repeal the Comstock Act, but discussions are in the early stages and repeal is unlikely in a closely divided Congress. Unless the U.S. Supreme Court rules definitively on the applicability of the Comstock Act as it pertains to mailing materials used for abortions – or Congress amends the U.S. Code – a subsequent DOJ may interpret the law differently and seek to prosecute violations. While former President Donald Trump indicated that he supports allowing states to make the decisions about abortion availability, his campaign has not issued any statements pertaining to the Comstock Act or its enforcement. However, leading anti-abortion and conservative organizations that support Trump’s candidacy have endorsed enforcement of the Comstock Act, also referred to as 18 U.S.C. §§1461 and 1462, in their blueprint for the 2025 presidential transition. While all eyes were on the Supreme Court before the Dobbs decision, the next president could take administrative actions to limit abortion access throughout the country, including in states where abortion is currently legal and protected.