U.S. International Family Planning & Reproductive Health: Requirements in Law and Policy
This fact sheet summarizes the major statutory requirements and policies pertaining to U.S. global family planning/reproductive health (FP/RH) efforts over time and identifies those currently in effect. These laws and policies collectively serve to direct how U.S. funds are spent, to where and which organizations funds are provided, and generally shape the implementation and define the scope of U.S. global FP/RH activities. It includes U.S. laws and annual requirements enacted by Congress through appropriations bills (statutory provisions) as well as executive branch policies and guidance specific to FP/RH (policy provisions). Each category lists provisions in chronological order.
Since early 2025, the Trump administration has frozen or eliminated funding for most FP/RH activities, although Congress has continued to appropriate funding for this work. See the KFF fact sheet of the status of FP/RH efforts.
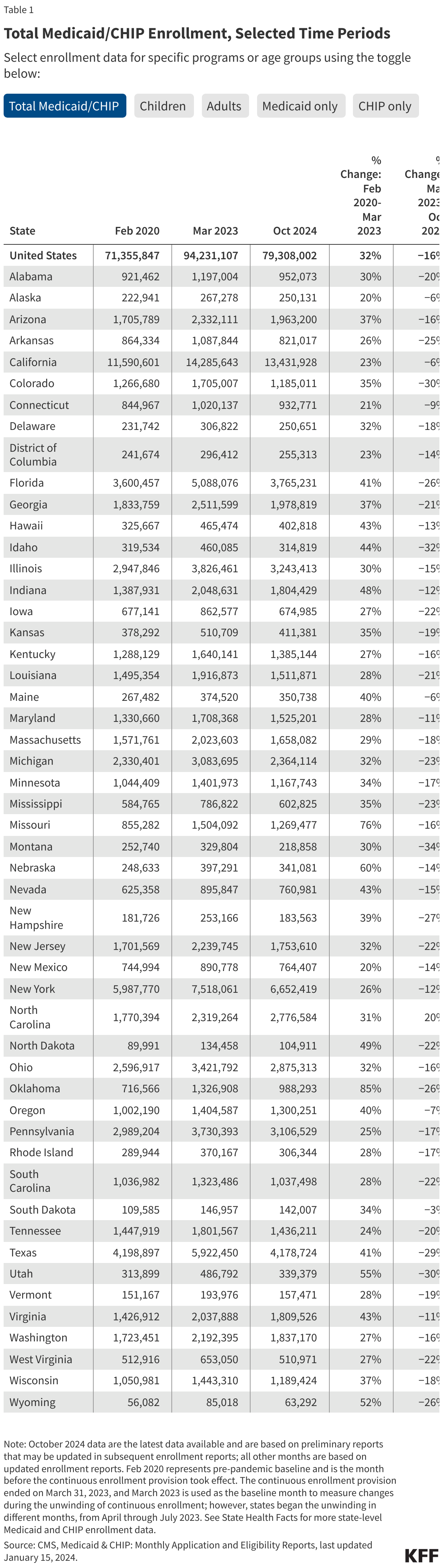
Table 1
Statutory Requirements and Policies for U.S. Global FP/RH Efforts (as of FY 2026)
| Provision (Year First Instituted) | Issue(s) | Applies to | Status |
|---|---|---|---|
| STATUTORY | |||
| Helms Amendment (1973) Prohibits the use of foreign assistance to pay for the performance of abortion as a method of family planning or to motivate or coerce any person to practice abortion. Note: meaning of “motivate” clarified by Leahy Amendment (1994); see below. | Abortion | All foreign assistance authorized under the Foreign Assistance Act of 1961(FAA); all funds under State-Foreign Operations Appropriations (State-Foreign Ops.) | Yes, in effect. Permanent law, amendment to the FAA. Also included in annual State-Foreign Ops. |
| Involuntary Sterilization Amendment (1978) Prohibits the use of funds to pay for involuntary sterilizations as a method of family planning or to coerce or provide a financial incentive to anyone to undergo sterilization. | Voluntarism/ Informed Choice & Consent; Incentives; Involuntary Sterilization | All foreign assistance authorized by the FAA of 1961; all foreign assistance funds under State-Foreign Ops. | Yes, in effect. Permanent law, amendment to the FAA. Also included in annual State-Foreign Ops. |
| Peace Corps Provision (1978) Prohibits Peace Corps funding from paying for an abortion for a Peace Corps volunteer or trainee; beginning in FY 2015, allows for payment in cases where the life of the woman is endangered by pregnancy or in cases of rape or incest.1 | Abortion | All Peace Corps funding | Yes, in effect. Included under the “Peace Corps” heading of the State-Foreign Ops. |
| Biden Amendment (1981) States that funds may not be used for biomedical research related to methods of or the performance of abortion or involuntary sterilization as a means of family planning. | Abortion; Involuntary Sterilization | All foreign assistance authorized by the FAA of 1961; all foreign assistance funds under State-Foreign Ops. | Yes, in effect. Permanent law, amendment to the FAA. Also included in annual State-Foreign Ops. |
| Siljander Amendment (1981) Prohibits the use of funds to lobby for or against abortion. When initially introduced, the amendment prohibited only lobbying for abortion, but in subsequent years Congress modified the language to include lobbying against abortion as well. | Abortion | All funds under State-Foreign Ops. | Yes, in effect. Included in annual State-Foreign Ops. |
| DeConcini Amendment (1985) Requires that U.S. funds be provided to organizations that offer, either directly or through referral to, information about access to a broad range of family planning methods and services. See Livingston-Obey Amendment (1986) below. | Voluntarism/ Informed Choice | All FP funds under State-Foreign Ops. | Yes, in effect. Included in annual State-Foreign Ops. |
| Kemp-Kasten Amendment (1985) Prohibits funding any organization or program, as determined by the President, that supports or participates in the management of a program of coercive abortion or involuntary sterilization. | UNFPA Funding; Abortion; Voluntarism/ Informed Choice & Consent; Involuntary Sterilization | All funds under State-Foreign Ops. as well as unobligated balances from prior appropriations acts | Yes, in effect. Included in annual State-Foreign Ops.2 each year; Presidents determined that it applied to UNFPA in FY85-FY92, FY02-FY08, FY17-FY20, FY25. |
| Involuntary Sterilization and Abortion Provision (1985) Specifies that U.S. foreign assistance funding could be withheld from a country or organization if the president certifies that the use of such funds would violate key provisions of the FAA of 1961 related to abortion or involuntary sterilization (namely the Helms, Biden, and Involuntary Sterilization Amendments). | Voluntarism/ Informed Choice & Consent; Incentives; Abortion; Involuntary Sterilization | All foreign assistance funds under State-Foreign Ops. | Yes, in effect. Included in annual State-Foreign Ops. |
| Livingston-Obey Amendment (1986) Prohibits discrimination by the U.S. government against organizations that offer only “natural family planning” for religious or conscientious reasons when the U.S. government is awarding related grants. All such applicants must comply with the requirements of the DeConcini Amendment (1985). | Voluntarism/ Informed Choice | All FP funds under State-Foreign Ops. | Yes, in effect. Included in annual State-Foreign Ops. |
| Leahy Amendment (1994) Clarifies Helms Amendment (1973) language that uses the term “motivate” by stating that “motivate” shall not be construed to prohibit, where legal, the provision of information or counseling about all pregnancy options. | Abortion; Voluntarism/ Informed Choice | All authorizing and appropriating legislation related to the State Dept., foreign operations, and related programs | Yes, in effect. Included in annual State-Foreign Ops. |
| Timing of Release of UNFPA Contribution Funds (1994) Not more than half of funding designated for the U.S. contribution to UNFPA is to be released before a particular date (varies by fiscal year). | UNFPA Funding | Funds made available to UNFPA | No, not in effect. Sometimes included in annual State-Foreign Ops. |
| Conditions on Availability of UNFPA Funds (UNFPA Segregated U.S. Contribution Account; UNFPA Does Not Fund Abortions; Prohibition on the Use of U.S. Funds in China by UNFPA) (1994) States that funds may not be made available to UNFPA unless: – UNFPA keeps the U.S. contribution to the agency in a separate account, not to be commingled with other funds, and – UNFPA does not fund abortions (note: language used beginning in FY00). It also prohibits UNFPA from using any funds from the U.S. contribution in their programming in China. | UNFPA Funding; Abortion | Funds made available to UNFPA | Yes, in effect. Included in annual State-Foreign Ops. |
| UNFPA Dollar-for-Dollar Withholding of Amount UNFPA Plans to Spend in China During Fiscal Year (1994) Reduces the U.S. contribution to UNFPA by one dollar for every dollar that UNFPA spends on its programming in China. | UNFPA Funding | Funds made available to UNFPA | Yes, in effect. Typically included in annual State-Foreign Ops. |
| Tiahrt Amendment (1998) Prohibits the use of targets/quotas and financial incentives3 in family planning projects and requires projects to provide comprehensible information on family planning methods. Protects people who choose not to use family planning from being denied rights or benefits and requires experimental family planning methods be provided only in the context of a scientific study. Intended to “promote voluntarism and prevent coercion in family planning programs,” it specifically prohibits three types of targets: total number of births, number of family planning acceptors, and acceptors of a particular method of family planning.4 | Voluntarism/ Informed Choice & Consent; Incentives and Disincentives | All FP funds under State-Foreign Ops. | Yes, in effect. Included in annual State-Foreign Ops. |
| Reallocation of Funds Not Made Available to UNFPA (2004) Provides for funds not made available to UNFPA to be reallocated to USAID’s family planning, maternal, and reproductive health activities/services (and, in some years, assistance to vulnerable children and victims of trafficking in persons).5 | UNFPA Funding | Funds appropriated for UNFPA | Yes, in effect. Typically included in annual State-Foreign Ops. |
| Medically Accurate Information on Condoms (2005) Ensures that information provided by U.S.-supported programs about the use of condoms is medically accurate information and includes the public health benefits and failure rates of such use. | Condoms | All funds under State-Foreign Ops. | Yes, in effect. Typically included in annual State-Foreign Ops. |
| POLICY | |||
| USAID Policy Paper on Population Assistance (1982) Outlines the longstanding USAID guidelines surrounding its fundamental programmatic principles of voluntarism and informed choice and consent.6 | Voluntarism/ Informed Choice & Consent | All FP/RH assistance provided by USAID | No longer in effect due to USAID’s dissolution. |
| Policy Determination 3 (PD-3): USAID Policy Guidelines on Voluntary Sterilization (1982) Describes guidelines for informed consent and voluntarism specifically for voluntary sterilization services, including provisions to ensure ready access to other contraceptive methods and prohibiting incentive payments that might induce a person to select voluntary sterilization over another method. | Voluntarism/ Informed Choice & Consent; Voluntary Sterilization | All FP/RH assistance provided by USAID | No longer in effect due to USAID’s dissolution. |
| Mexico City Policy (“Global Gag Rule”, 1984)7 As a condition for receiving U.S. family planning assistance, other global health assistance, and, now, also other U.S. foreign assistance (see “Applies to”), requires foreign NGOs and, now, U.S. NGOs, international organizations, foreign governments, and parastatals to certify that they will not provide or promote abortion as a method of family planning using funds from any source. The latest iteration of the policy under the second Trump administration iss called “Protecting Life in Foreign Assistance” and falls under the broader umbrella of the “Protecting Human Flourishing in Foreign Assistance Policy” (PHFFA Policy), which also requires certain organizations to certify they will not provide or promote “gender ideology” and “discriminatory equity ideology,” among other activities.. Included in the U.S. Department of State Standard Terms and Conditions (see entry below), when applicable. | Abortion | 1984- 2003: when in effect, was applied to FP assistance at USAID only. In 2003, expanded to include all FP assistance at USAID and the State Dept., exempting multilateral organizations and HIV/AIDS funding under PEPFAR. 2009-17: Not in effect. 2017-2021: applied to all global health assistance. 2021-2025t: Not in effect. 2025-present: applied to most foreign assistance at the State Department. | Yes, in effect.8 |
| USAID Post-Abortion Care Policy (2001) Clarifies that post-abortion care – the treatment of injuries or illnesses caused by legal or illegal abortion – is permitted under the Helms Amendment and that any restrictions under the Mexico City Policy, when in force, do not limit organizations from treating injuries or illnesses caused by legal or illegal abortions (i.e., providing post-abortion care). Notes USAID does not finance manual vacuum aspiration equipment purchase/distribution for any purpose. | Post-Abortion Care | All FP/RH assistance provided by USAID | No longer in effect due to USAID’s dissolution; however, the current Mexico City Policy does not restrict post-abortion care. |
| Guidance on the Definition and Use of the Global Health Programs Account: Section on Allowable Uses of Funds for Family Planning/Reproductive Health (2014) Outlines allowable uses of funds for FP/RH by providing a description of activities allowed and examples of activities not allowed, addressing not only FP/RH activities but also family planning activities’ integration with other global health and multisectoral activities. | FP/RH Activities; FP/RH System Strengthening Activities; Integrated FP Activities | All FP/RH assistance provided by USAID | No longer in effect due to USAID’s dissolution. |
| USAID Standard Provisions for Nongovernmental Organizations (U.S. and Non-U.S.) Outline requirements that must be attached to assistance agreements, including language implementing FP/RH legal and policy requirements described above (e.g., the Helms and Leahy Amendments.)9 | Voluntarism/ Informed Choice & Consent; Incentives; Abortion; Involuntary Sterilization; Condoms; FP/RH Activities | USAID assistance agreements | Yes, in effect in ongoing USAID award agreements with NGOs. |
| U.S. Department of State Standard Terms and Conditions (revised 10/01/2025) Outline requirements that must be attached to assistance agreements, including language implementing FP/RH legal and policy requirements described above (e.g., the Helms and Siljander Amendments.)10 Includes the Promoting Human Flourishing in Foreign Assistance Policy (PHFFA Policy) – in effect as of Feb. 26, 2026 – for foreign NGOs, U.S. NGOs, international organizations, and, when applicable, foreign governments and parastatals. | Voluntarism/ Informed Choice & Consent; Incentives; Abortion; Involuntary Sterilization; FP/RH Activities | State Department assistance agreements | Yes, in effect. |
- As noted in CRS, Abortion and Family Planning-Related Provisions in U.S. Foreign Assistance Legislation and Policy, July 2022: “No restrictions exist on funding for the medical evacuation of Peace Corps volunteers who decide to have an abortion. Under existing policy, the Peace Corps covers the cost of evacuation to a location where ‘medically adequate facilities’ for obtaining an abortion are available and where abortions are legally permissible.” ↩︎
- In most recent years, a provision is included requiring that any Kemp-Kasten determination that is made must be accompanied by the evidence and criteria used to make the determination. ↩︎
- USAID defines a target/quota as “a predetermined figure that a service provider or referral agent is assigned or required to affect or achieve” for the purposes of the Tiahrt Amendment. It states that “the key to interpreting ‘incentives’ is to see whether they are provided in exchange for accepting a method (in the case of a client) or linked to achievement of a predetermined target or quota (in the case of program personnel).” USAID Global Health eLearning Center, “FP Legislative & Policy Requirements (Updated),” online course, February 2009, authored by Debbie Gueye, MSI. ↩︎
- USAID Global Health eLearning Center, “FP Legislative & Policy Requirements (Updated),” online course, Feb. 2009, authored by Debbie Gueye, MSI. ↩︎
- Although such reallocation began in practice in FY 2002, it was first authorized by Congress in legislation beginning in FY 2004 with reference to FY 2002 and FY 2003 funds. ↩︎
- Informed Choice: Effective access to information on family planning choices and to the counseling, services, and supplies needed to help individuals choose to obtain or decline services; to seek, obtain, and follow up on a referral; or simply to consider the matter further. Voluntarism: Decision to use a specific method of family planning or to use any method of family planning is based upon the exercise of free choice and is not obtained by any special inducements or any element of force, fraud, deceit, duress or other forms of coercion or misrepresentation. USAID Global Health eLearning Center, “FP Legislative & Policy Requirements (Updated),” online course, Feb. 2009, authored by Debbie Gueye, MSI. ↩︎
- This policy was first instituted via presidential memorandum in 1984 by President Reagan. In 1993, it was rescinded by President Clinton, although it was briefly applied legislatively in 1999 (see “Status” column). In 2001, it was reinstated by President Bush, who expanded its applicability in 2003 to include family planning funds at the State Department (see “Applies to” column) with some exemptions. In 2009, it was rescinded by President Obama. In 2017, it was reinstated by President Trump, who expanded its applicability to include the vast majority of global health assistance furnished by all departments and agencies. In 2021, it was rescinded by President Biden. ↩︎
- Note that, with one exception, has been applied via Executive action. The exception was in FY 2000, when President Clinton agreed to a one-year legislative codification with a partial waiver of restrictions as part of a broader arrangement to pay the U.S. debt to the United Nations. See P.L. 106-113, Sec. 599D, and PAI, Global Gag Rule Timeline, July 12, 2011. ↩︎
- “M16. VOLUNTARY POPULATION PLANNING ACTIVITIES – MANDATORY REQUIREMENTS (MAY 2006) …
b. Prohibition on Abortion-Related Activities:
(1) No funds made available under this award will be used to finance, support, or be attributed to the following activities: (i) procurement or distribution of equipment intended to be used for the purpose of inducing abortions as a method of family planning; (ii) special fees or incentives to any person to coerce or motivate them to have abortions; (iii) payments to persons to perform abortions or to solicit persons to undergo abortions; (iv) information, education, training, or communication programs that seek to promote abortion as a method of family planning; and (v) lobbying for or against abortion. The term “motivate,” as it relates to family planning assistance, must not be construed to prohibit the provision, consistent with local law, of information or counseling about all pregnancy options.
(2)No funds made available under this award will be used to pay for any biomedical research which relates, in whole or in part, to methods of, or the performance of, abortions or involuntary sterilizations as a means of family planning. Epidemiologic or descriptive research to assess the incidence, extent, or consequences of abortions is not precluded.” ↩︎ - For example, one provision related to abortion included in the State Department Standard Terms and Conditions is:
“AA. Prohibition on use of funds for performance or research respecting abortions or involuntary sterilization
The recipient agrees that in accordance with 22 USC 2151b(f) Population planning and health programs no foreign assistance funds provided by the award shall be used to:
(1) pay for the performance of abortions as a method of family planning or to motivate or coerce any person to practice abortions (Helms Amendment, 1973).
(2) pay for the performance of involuntary sterilizations as a method of family planning or to coerce or provide any financial incentive to any person to undergo sterilizations (Involuntary Sterilization Amendment, 1978).
(3) pay for any biomedical research which relates, in whole or in part, to methods of, or the performance of, abortions or involuntary sterilization as a means of family planning (Biden Amendment, 1981).
Furthermore, the recipient agrees in accordance with the Department’s annual appropriation bill, that no funds provided by the award may be used to lobby for or against abortion (Siljander Amendment, 1981).” ↩︎