Snapshots: The Prevalence and Cost of Deductibles in Employer Sponsored Insurance
Over the past several years enrollees in employer-sponsored health plans have contributed more towards their care through the use of increased cost sharing. The growth in deductibles is one of the more visible increases in employee cost sharing.
A deductible is an amount that must be paid out-of-pocket by an enrollee before some or all services are covered by their health plan. Health plans may impose deductibles on specific services, such as outpatient surgery or pharmaceutical drugs, or require a general annual deductible which is applied to most or all services. In recent years, deductibles have become more common as employers attempt to reduce premium costs and ensure that workers have incentives to reduce utilization. Evidence shows that higher deductibles and other cost sharing reduce the use of health care by exposing enrollees to a larger share of their health care spending and thereby encourage them to be more selective with the services they consume.1
The Employer Health Benefits Survey has tracked changes in the prevalence and cost of deductibles in employer-sponsored health plans across time.2 In 2006 we changed the questions on deductibles to gather additional information on the different types of deductibles being used. Throughout this report, small firms are defined as those with 3 to 199 workers, and large firms are those with 200 or more workers. Deductibles are reported for single coverage and for in-network services.3
The Prevalence of General Annual Deductibles:
The percent of covered workers enrolled in a plan with a general annual deductible has increased significantly over time. In 2006, just over half (52%) of covered workers had a deductible for single coverage, compared with almost three-quarters (72%) in 2012.
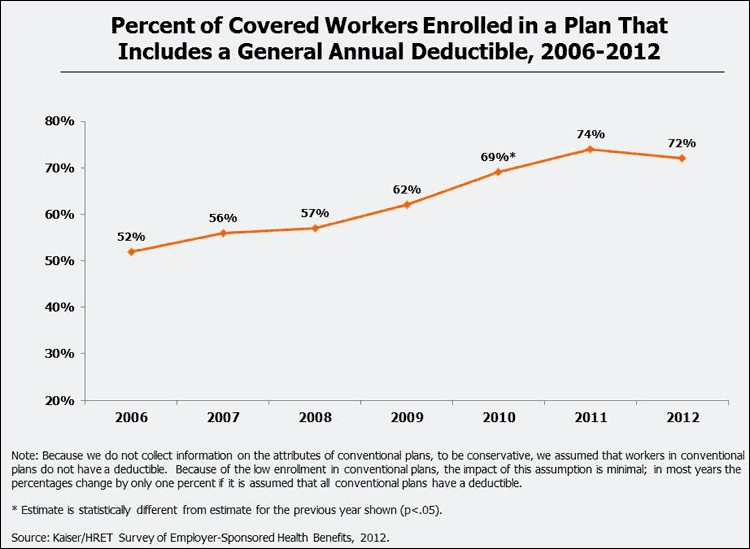
The number of covered workers with a general annual deductible is increasing both because of shifts in enrollment patterns among plan types as well as the increasing prevalence of deductibles within plan types. There are important differences in the use of deductibles among plan types; deductibles are much more common for workers enrolled in Preferred Provider Organizations (PPOs) than for workers enrolled in Health Maintenance Organizations (HMOs). Since 2006, the percentage of workers enrolled in plan types which are less likely to require a deductible, such as HMOs, has decreased (20% to 16%) and enrollment in High-Deductible Health Plans with Savings Options (HDHP/SOs) has increased (4% to 19%).4 We define high-deductible health plans with savings options as plans with a deductible of at least $1,000 and eligible for either a health reimbursement arrangement (HRAs) or Health Savings Account (HRAs).5
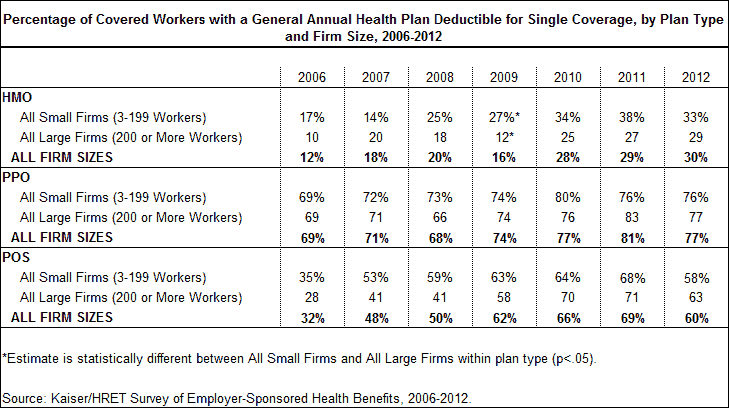
There has been a significant increase in the prevalence of deductibles for covered workers enrolled in each plan type (HMO, PPO, and POS) since 2006. For example, in 2012, 77% of covered workers enrolled in a PPO plan had a general annual deductible for single coverage, compared to 69% in 2006. General annual deductibles have become common for workers enrolled in HMO plans, growing from just 12% of workers enrolled in an HMO plan in 2006 to 30% in 2012.
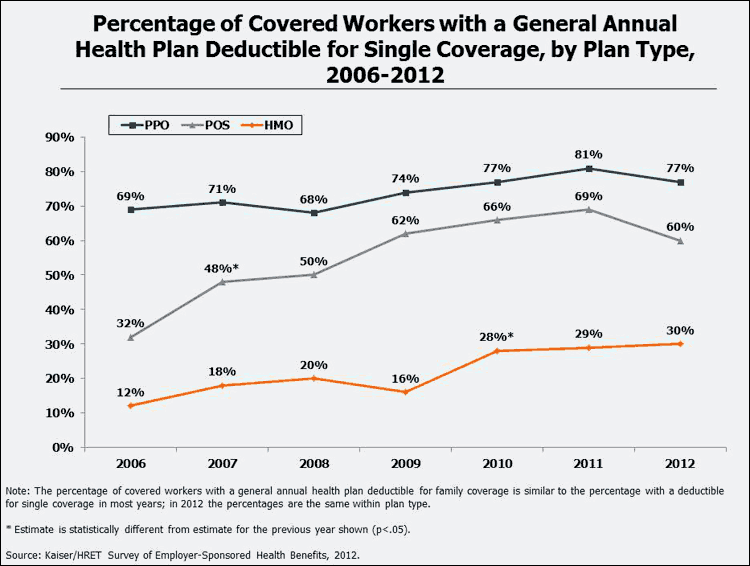
The Cost of General Annual Deductibles for Single Coverage:
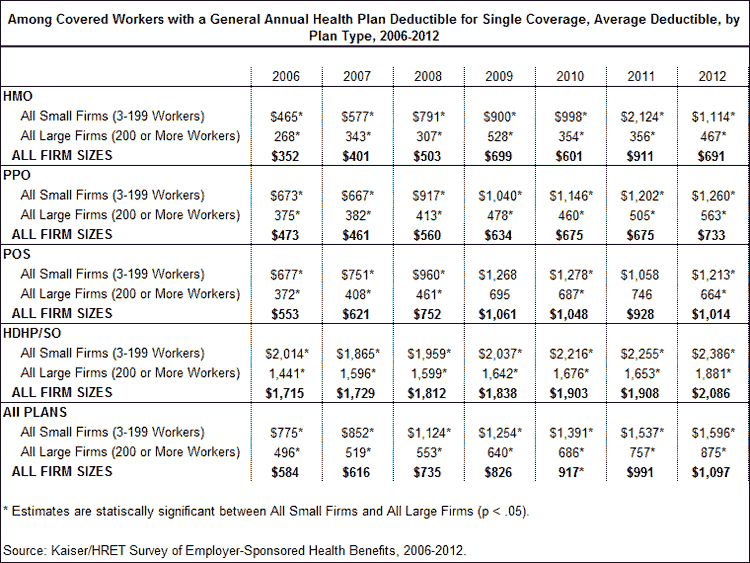
In addition to more workers facing a general deductible, the amount of these deductibles has also steadily increased. Since 2006, the average general annual deductible among covered workers who have a deductible for single coverage has increased for each plan type. Overall, the average general annual deductible is $1,097 for covered workers enrolled in a single coverage plan requiring a deductible; an increase of 88% since 2006, with significant annual increases in four of the last five years. There are significant differences in the costs of deductibles by plan type, with covered workers enrolled in HMO plans facing smaller deductibles than workers enrolled in HDHP/SOs.
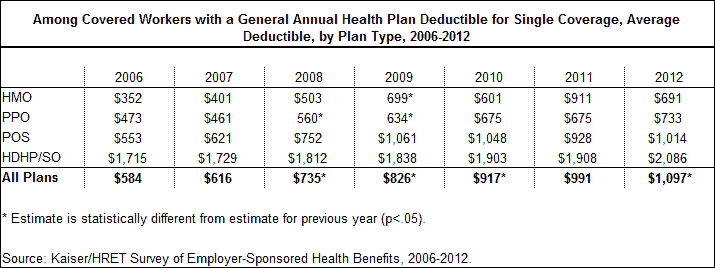
The growing prevalence and amount of deductibles has resulted in an increasing percentage of covered workers enrolled in a plan with high deductibles. In 2012, about a third (34%) of covered workers were enrolled in a plan with a deductible of a $1,000 or more compared to 10% in 2006, and 14% were enrolled in a plan with a deductible of $2,000 or more compared to 3% in 2006. The percentages of workers include workers who are enrolled in a high deductible plans with a savings account (HDHP/SO), such as an HSA or an HRA, and those who are in a plan without a savings account.
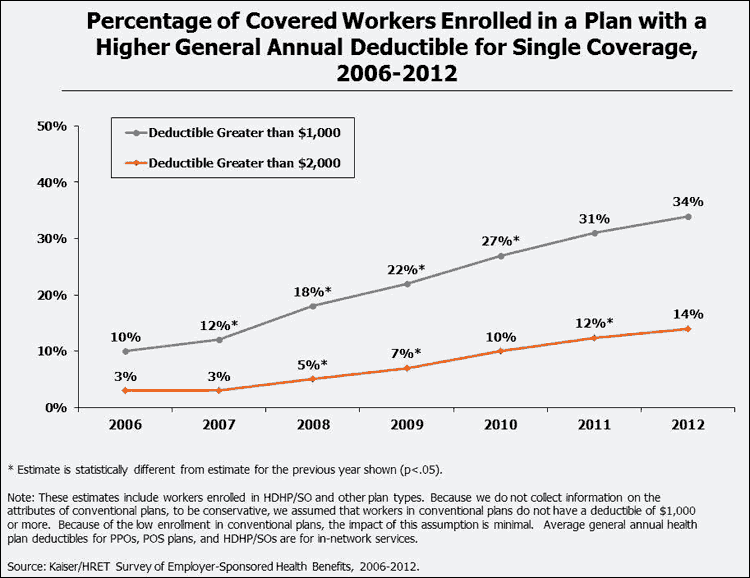
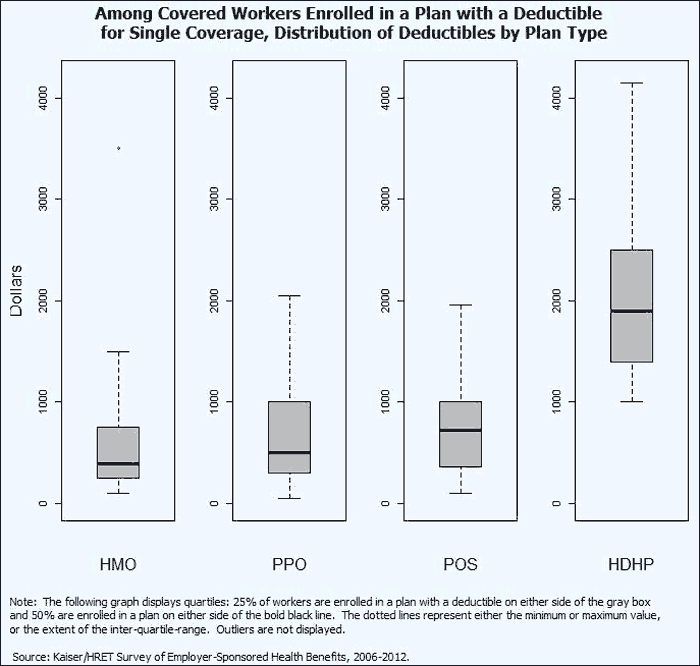
Deductibles levels also vary within plan types. The following graph displays quartiles: 25% of workers are enrolled in a plan with a deductible on either side of the gray box and 50% are enrolled in a plan on either side of the bold black line.6 For workers enrolled in an HMO plan, 25% of workers have a deductible less than $250 and 25% percent have a deductible of $750 or more. Twenty-five percent of workers enrolled in a PPO plan are enrolled in a plan with a deductible less than $300 and 25% are in a plan of $1,000 dollars are more. Deductibles are much higher for workers enrolled in HDHP/SO plans, with 25% of workers enrolled in a plan with a deductible between $1,000 and $1,400, and 25% of workers in a plan with a deductible greater than $2,500. Many workers enrolled in these plans have access to a savings option to pay for qualified medical expenses and may therefore be able to defer some of the cost of higher deductibles.
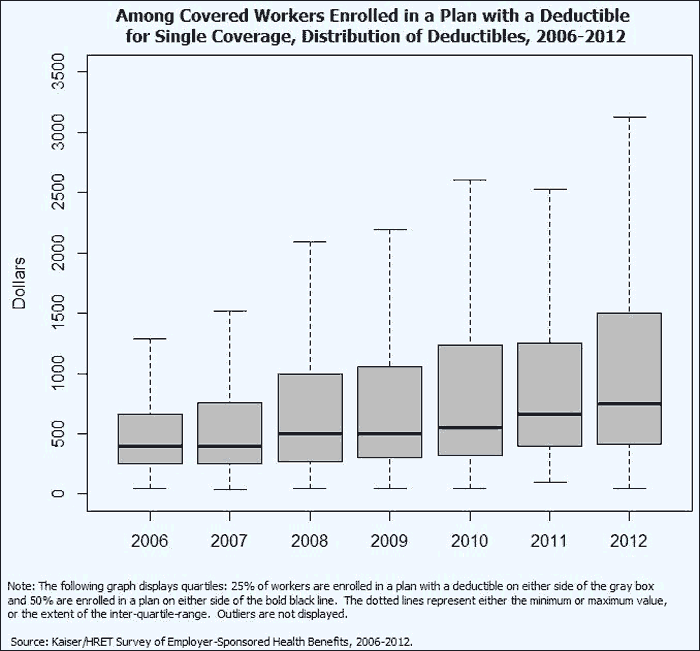
There is increasing variance in the average deductible across all plan types. In 2006, 50% of workers had a deductible between $250 and $665. In 2012, 50% of workers had a deductible between $417 and $1,500.7 With the growth of higher deductible plans over the past couple of years, some workers are facing much higher deductibles than others.
Differences in General Annual Deductibles for Single Coverage between Different Types of Firms:
While there are important differences in the cost-sharing structures used by small and large firms, the percentage of covered workers enrolled in a plan that requires a general annual deductible is similar between small and large firms within each plan type.
Although workers at small firms are no more likely to be enrolled in health coverage that includes a deductible, they typically face much higher deductibles than workers at large firms. The average deductible for covered workers enrolled in single coverage at a small firm is nearly twice as much as the deductible for covered workers at larger firms. Within PPOs, the plan type with largest enrollment, the average deductible for workers at small firms is $1,260, compared to $563 for workers at large firms. The average deductible among all plan types for workers at small firms is $1,596, more than the $875 dollars for covered workers at larger firms. Despite the higher deductibles for workers at small firms, the rate of growth for deductibles is similar between firms in either size category: the average single coverage deductible for workers at small firms has increased 106% since 2006, a statistically similar change to the 76% for covered workers at large firms.
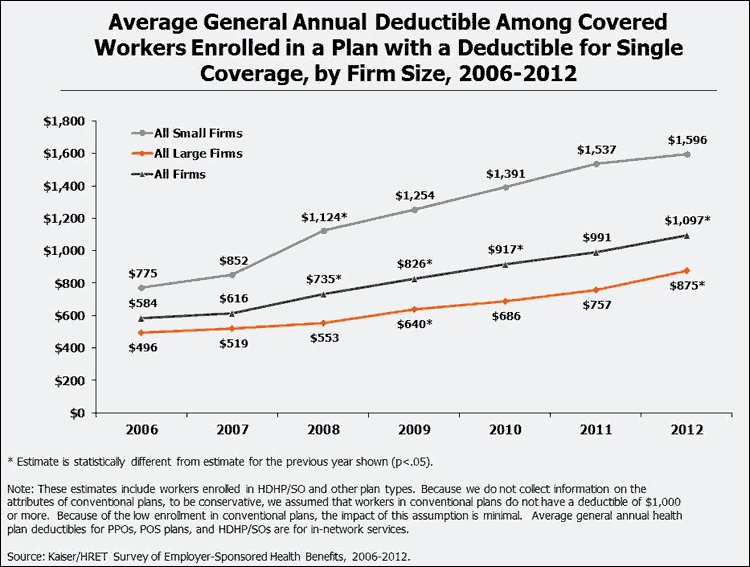
Plans with deductibles of over $1,000 have become much more commonplace for workers at small firms. Almost half of workers enrolled in a health plan at small firms face a deductible of $1,000 or more, compared to just over a quarter of workers enrolled at large firms (49% vs. 26%). A meaningful portion of covered workers at small firms are required to meet a deductible of $2,000 or more before most services are covered (27% at small firms compared to 7% at large firms). This is explained both by the higher enrollment in HDHP/SO plans at small firms, as well as higher deductibles for covered workers at small firms within each plan type.8
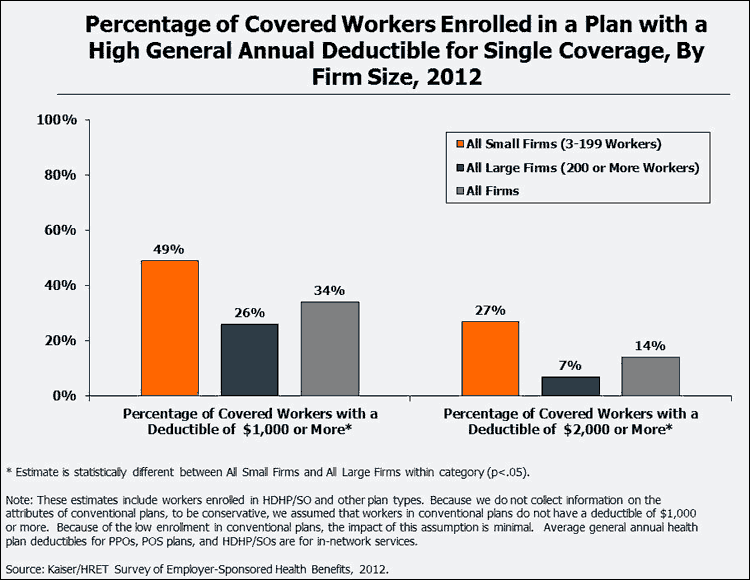
There are few differences in the proportion of workers enrolled in plans that are required to meet general annual deductibles between different firm characteristics, but there are significant differences in the average deductible amounts. Covered workers enrolled in PPO and POS plans with many higher-wage workers tend to have lower deductibles than their counterparts at firms with fewer higher-wage workers.9 Covered workers in HMO, PPO and HDHP/SO plans at firms with some unionized workers have lower general annual deductibles than workers at firms without unions.
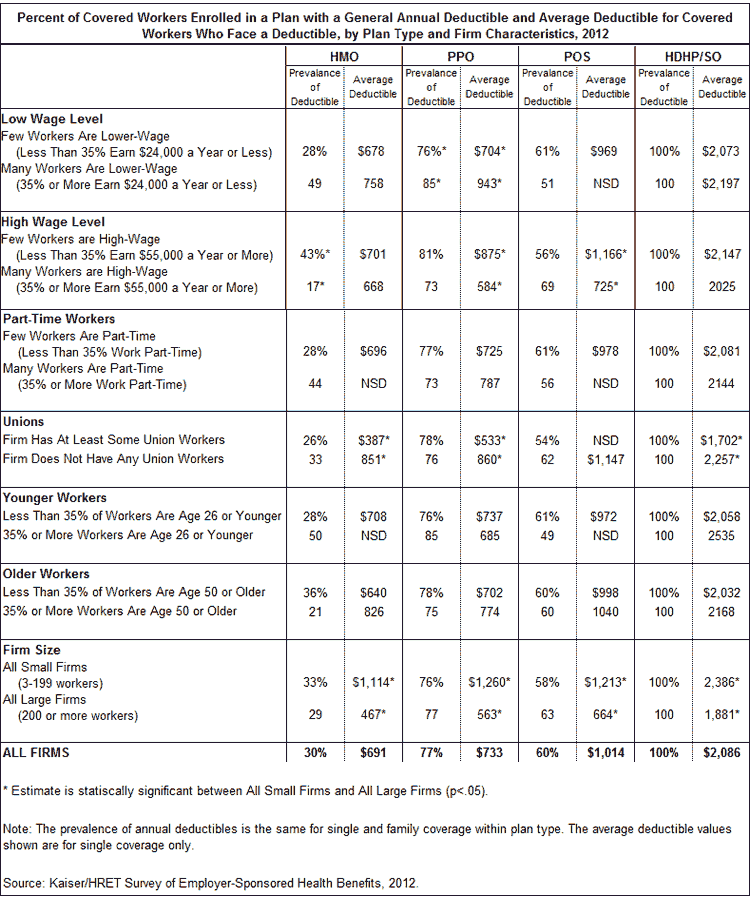
General Annual Deductibles Structure:
Health plans use a variety of structures for deductibles that effect how much cost sharing enrollees are exposed to. Many health plans will cover certain services even if an enrollee has not yet met the deductible. For example, a majority of enrollees receive coverage for primary care office visits and prescription drugs regardless of whether they have satisfied the deductible. This has remained consistent over time and, also, across HMO, PPO, and POS plan types. Additionally, with the implementation of the Affordable Care Act, coverage independent of general annual deductibles will expand to include preventive services, such as cardiovascular health and cancer screenings.10 By law HSA-qualified plans can only cover preventive care services before the deductible is met.
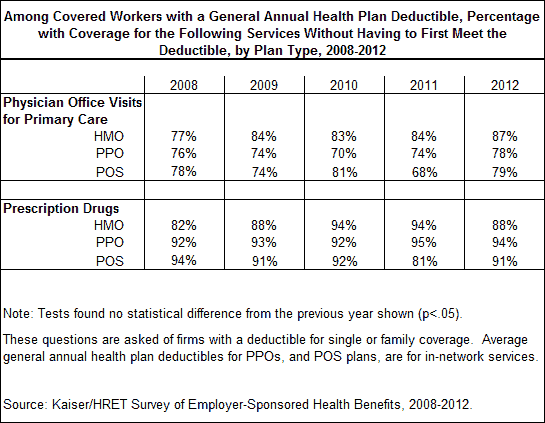
Service Specific Deductibles:
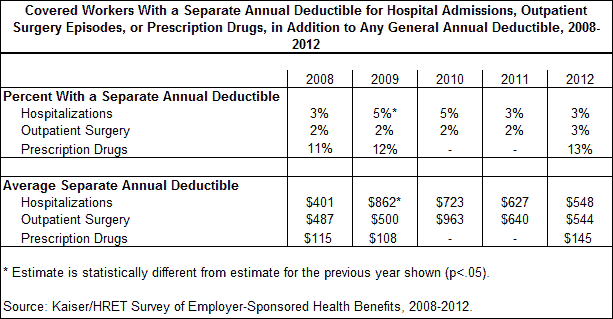
Both in addition to, and in lieu of, a general annual deductible, health plans may impose a service specific deductible (or a separate annual deductible). These plans require that an enrollee cover the first portion of costs for a specific service, such as an outpatient surgery or hospitalization. Employers may use service-specific deductibles as one method of decreasing their total costs towards an employee’s coverage. However, the prevalence of such deductibles has remained low over time. For example, only three percent of enrollees face aseparate annual deductible for hospitalizations or outpatient surgeries. Thirteen percent have a separate deductible for prescription drugs. The amount of these service-specific deductibles also shows little change over time. In 2012, the deductibles for hospitalizations and outpatient surgeries are roughly $550. A lower deductible is seen for prescription drugs ($145). Many plans have additional types of cost sharing, such as copays or coinsurances, for these services.
Conclusion:
In addition to contributing more towards premiums, covered workers are increasingly faced with higher cost sharing. A larger proportion of workers are required to meet a deductible prior to utilizing services and these deductibles are increasing in size. It has become commonplace for covered workers to be enrolled in a plan with a deductible of a $1,000 or more. While many working families have sufficient savings and coverage in case of a medical emergency.11 The growth in workers’ contributions and cost sharing may increasingly become a financial strain on some households.
This snapshot was prepared by Matthew Rae, Nirmita Panchal, and Gary Claxton of the Kaiser Family Foundation’s Health Care Marketplace Project.
Notes:
- “The Role of Consumer Copayments for Health Care: Lessons from the RAND Health Insurance Experiment and Beyond”. Kaiser Family Foundation. October 2006. http://www.kff.org/health-costs/report/the-role-of-consumer-copayments-for-health/
- The Employer Health Benefits Survey is a national probability survey of over 2,100 private and non-federal public firms with three or more employees. Interviews are conducted with HR directors and office managers about the firm’s HMO, PPO, POS, and HDHP/SO plan with the largest enrollment. For more information on the survey design and sampling methodology of the Employer Health Benefits Survey, see the Survey Design and Methods Section of the 2012 report. Significance differences are reported at the 0.05 level. http://www.kff.org/health-costs/report/employer-health-benefits-2012-annual-survey/ Kaiser/HRET Survey of Employer-Sponsored Health Benefits, 2012.
- Because of the variety of structures that employers use for family coverage, this snapshot looks at single coverage. For more information on family deductibles or the survey’s definition of deductibles see Section 7 of the 2012 report: http://www.kff.org/report-section/ehbs-2012-section-7/ Kaiser/HRET Survey of Employer-Sponsored Health Benefits, 2012.
- For more information on changes in enrollment patterns see exhibit 5.1 of the 2012 report:http://www.kff.org/report-section/ehbs-2012-section-5/ Kaiser/HRET Survey of Employer-Sponsored Health Benefits, 2012.
- By law, high-deductible plans with a health savings account (HSAs) have a general annual deductible of $1,200 or more. For more information about HDHP/SO plan see Section 8: http://www.kff.org/report-section/ehbs-2012-section-8/, Kaiser/HRET Survey of Employer-Sponsored Health Benefits, 2012.
- The dotted lines represent either the minimum or maximum value, or the extent of the inter-quartile-range. Outliers are not displayed.
- Both the 25th and 75th percentiles are significantly higher in 2012 compares against 2006.
- For more information on the differences in enrollment patterns between small and large firms see Exhibit 5.2: http://www.kff.org/report-section/ehbs-2012-section-5/. Kaiser/HRET Survey of Employer-Sponsored Health Benefits, 2012.
- Firms with many lower-wage workers are ones where 35% or more of employees earn $24,000 or less. Firms with many higher-wage workers are ones where 35% or more of employees earn $55,000 or more. Wage cutoffs are the inflation adjusted 25th and 75th percentile of national wages according to the National Compensation Survey: Occupational Earnings in the United States, 2010.
- For more information see: “Preventive Services Covered by Private Health Plans under the Affordable Care Act.” Kaiser Family Foundation. September 2011. http://www.kff.org/health-reform/fact-sheet/preventive-services-covered-by-private-health-plans/.
- Claxton, Gary & Jacobs, Paul. “Comparing the Assets Of Uninsured Households to Cost Sharing Under High-Deductible Health Plans”. Health Affairs. May 2008. 27:3 w214-w221.