
The independent source for health policy research, polling, and news.
Analysis: Individual Market Insurers Experienced Their Best Financial Year under the ACA in 2017, Though Subsequent Political and Policy Changes Complicate the Outlook for Future Years
Insurers in 2017 had their best financial year selling individual market health insurance since the Affordable Care Act began requiring guaranteed access to coverage for people with pre-existing conditions in 2014, though recent political and policy changes create new challenges for insurers trying to succeed in this market, new Kaiser Family Foundation analysis finds.
This analysis finds insurers posted their strongest performance in the individual market using two different financial indicators:
- The average share of health premiums paid out in claims (or medical loss ratio) fell to 82 percent in 2017 from 96 percent in 2016 and 103 percent in 2015.
- Average premiums collected in excess of claims (or gross margins) reached $79 in 2017 per member per month, up from $14 in 2016 and -$9 in 2015.
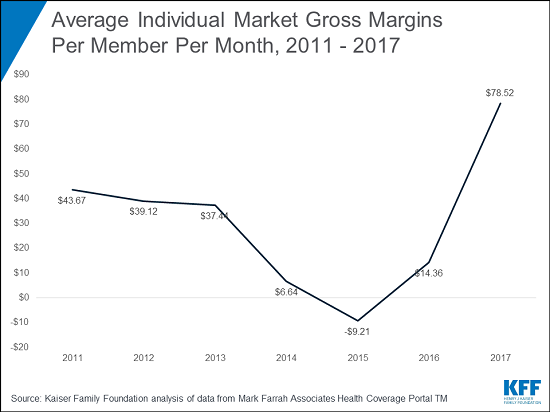
The strong financial performance suggests insurers on average priced their plans adequately last year, though the outlook for this year and next year is cloudier, given recent policy changes and political uncertainties that are driving up premiums and potentially pricing out healthy middle-class consumers.
The analysis notes those complicating factors include the Trump Administration’s decision to stop making cost-sharing subsidy payments to insurers; the repeal of the individual mandate penalty as part of tax reform legislation; and proposed regulations to expand loosely-regulated short-term insurance plans.
The analysis is based on insurer-reported financial data, including information from the National Association of Insurance Commissioners, compiled and maintained by Mark Farrah Associates.