KFF Tracking Poll on Health Information and Trust: Use of AI For Health Information and Advice
Findings
Key Takeaways
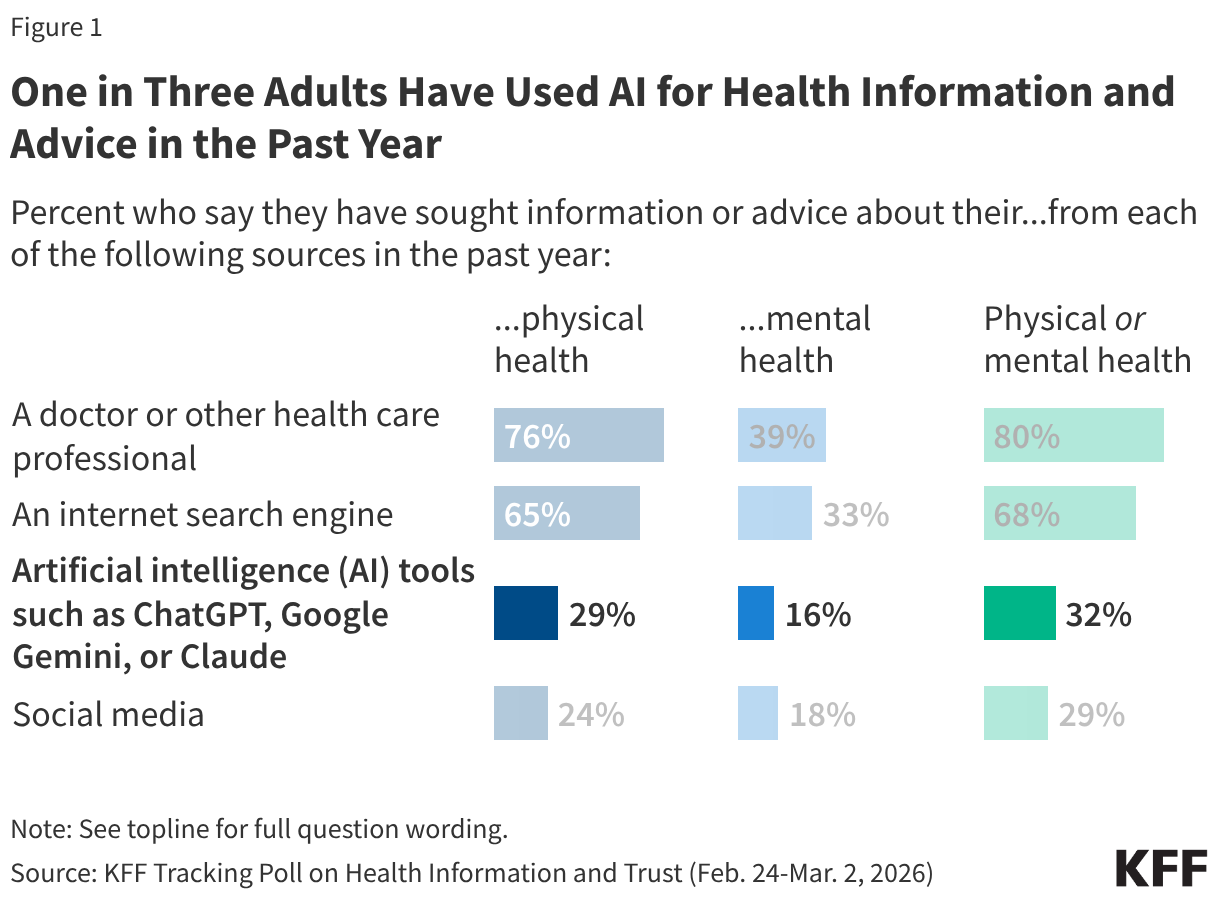
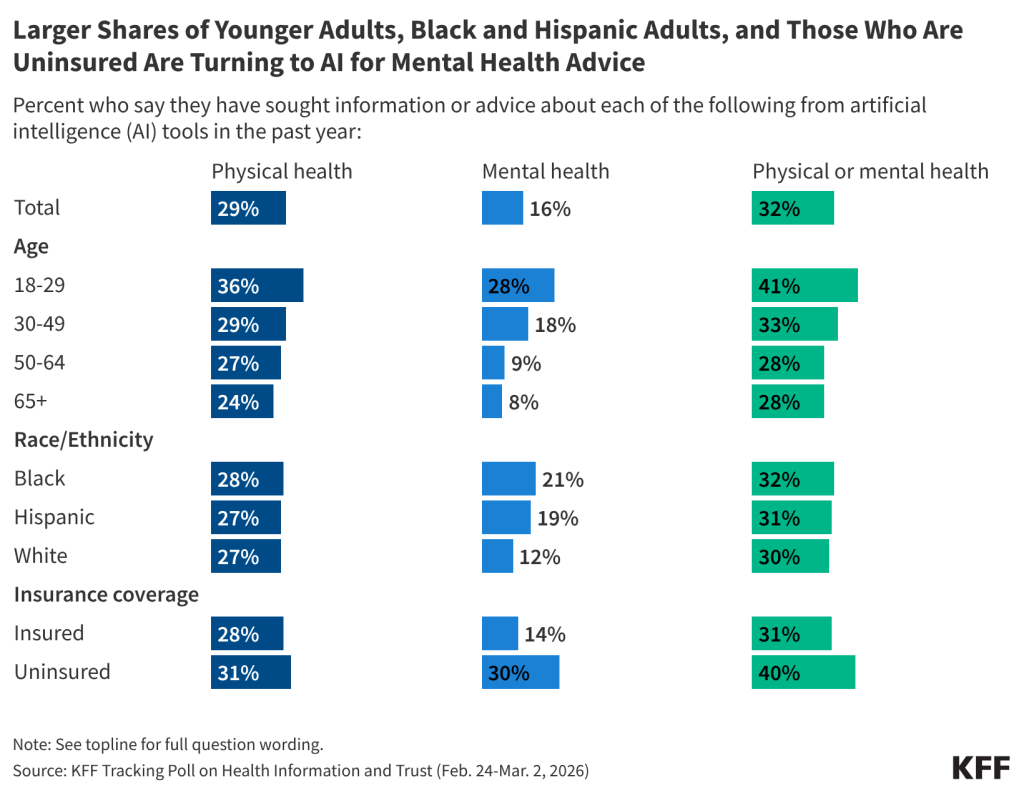
- With the recent explosion of consumer artificial intelligence (AI) tools and chatbots, KFF’s latest Tracking Poll on Health Information and Trust finds about a third (32%) of adults are turning to AI for health information and advice. This includes about three in ten (29%) who say they’ve used AI tools in the past year for information or advice about their physical health, and one in six (16%) who’ve used them for mental health information or advice. AI use is on par with the share who say they turn to social media for health information, but lags behind the shares saying they’ve sought health information from health care providers and internet search engines (where they may be encountering AI generated results, even if they are not looking for them).
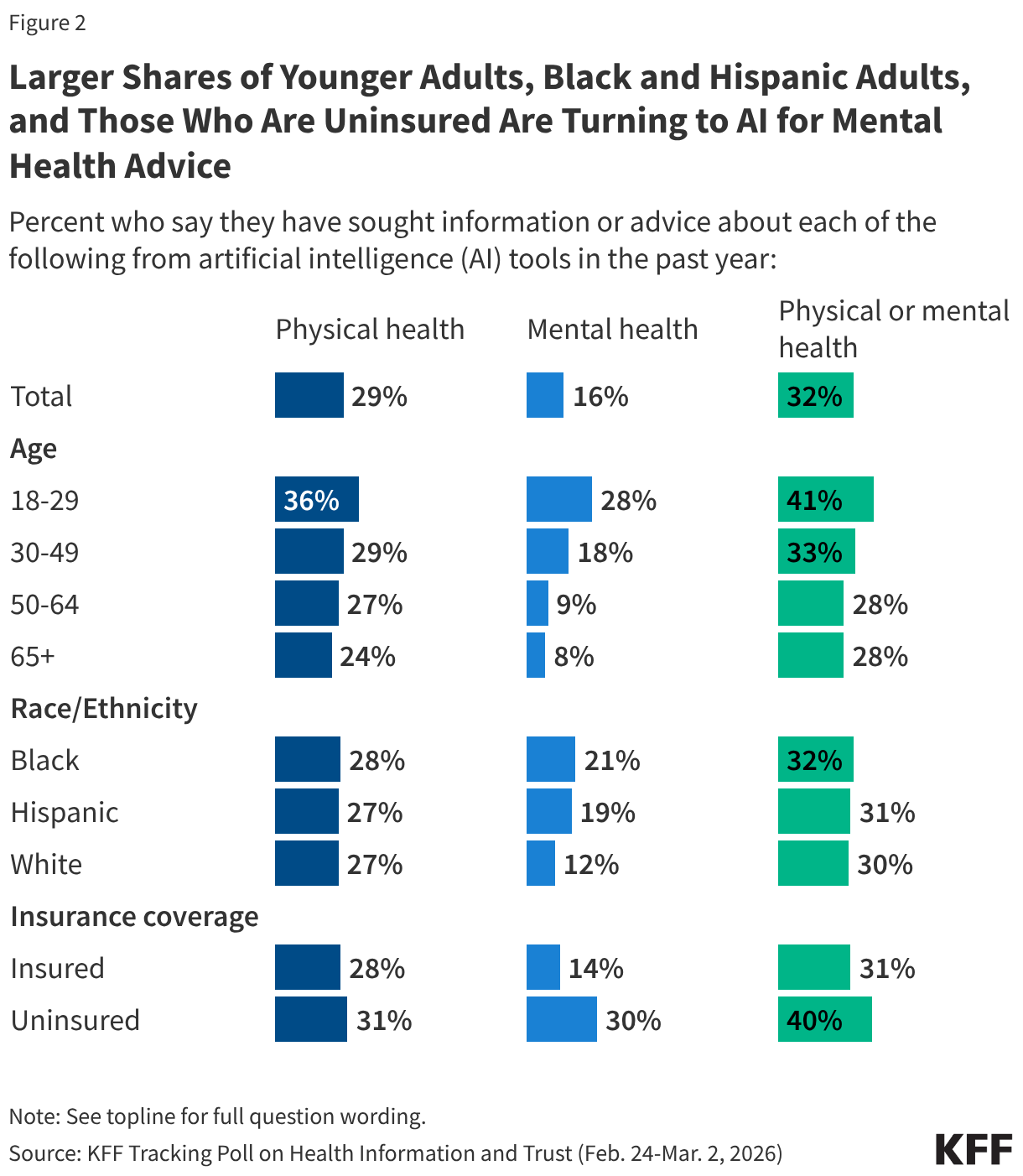
- Larger shares of younger adults, uninsured adults, Black adults, and Hispanic adults are turning to AI chatbots for mental health advice. About three in ten (28%) of those ages 18 to 29 say they’ve used AI for information about their mental health or emotional wellbeing in the past year, compared to about one in five (18%) adults ages 30 to 49 and about one in ten of those ages 50 and older. Uninsured adults are more likely than insured adults to say they’ve relied on AI for mental health advice (30% v. 14%), as are Black (21%) and Hispanic (19%) adults compared to White adults (12%).
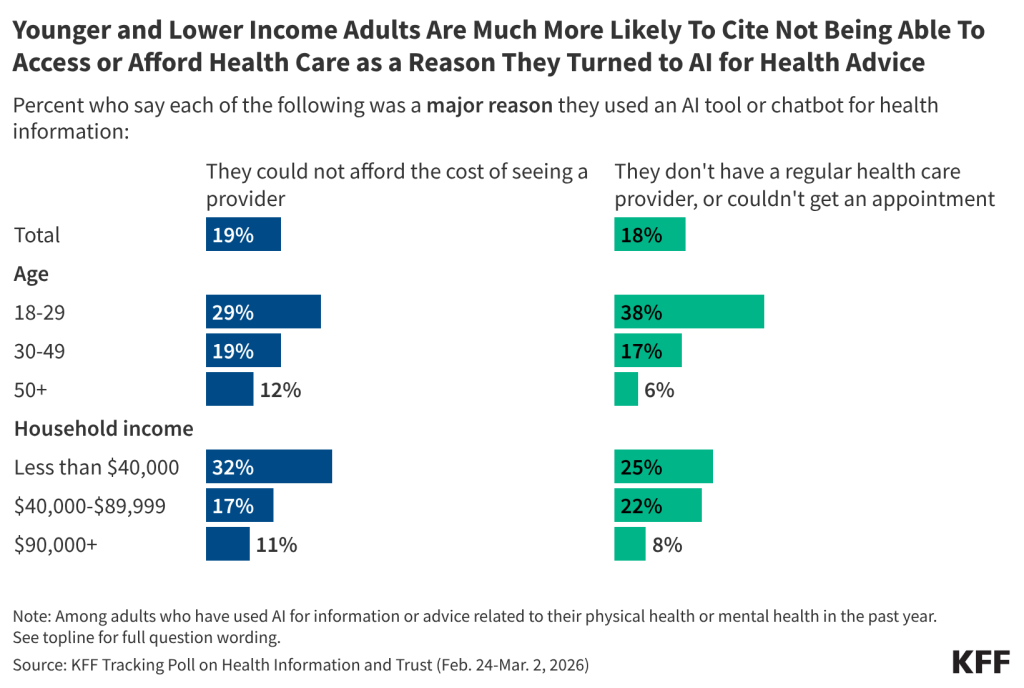
- Among the top reasons given for turning to AI for health information, most users (65%) say a desire for quick and immediate advice was a “major reason,” for doing so, while many also cite wanting to look up information before seeing a provider (41%) or feeling more comfortable looking up health questions privately (36%). Difficulty accessing or affording health care is also driving some to rely on AI for health information, particularly younger and lower-income users. About one in five AI health users cite not having a health care provider or not being able to get an appointment as a major reason they used AI for health advice, rising to four in ten (38%) among users ages 18 to 29. Another one in five users say difficulty affording health care was a major reason they relied on AI for health advice, rising to three in ten (29%) among users ages 18 to 29 and one-third (32%) among those with annual incomes below $40,000.
- A majority (77%) of the public says they are concerned about the privacy of personal medical information provided to AI tools, including similar majorities across age groups and those who use AI for health information. Despite these privacy concerns, about four in ten (41%) of those who have used AI for physical or mental health (amounting to 13% of all adults), say they’ve uploaded personal medical information into an AI tool or chatbot.
AI Use for Health Information and Advice
KFF’s latest Tracking Poll on Health Information and Trust finds that use of and exposure to artificial intelligence has become omnipresent in most Americans’ lives, and some are turning to these tools for health information and advice at a time when several technology companies have announced the launch of health-specific chatbots.
Overall, four in ten (39%) adults say they actively use AI tools at least several times a week, while eight in ten say they come across AI-generated content at least several times a week, even if they are not actively looking for it.
About a third (32%) of the public reports turning to AI chatbots for physical or mental health advice – rivaling social media as a health information source, but less common than reliance on health care providers or internet search engines. The share using AI for health advice includes about three in ten (29%) who say they’ve sought information or advice about their physical health from an AI tool or chatbot in the past year, as well as one in six (16%) who say they’ve sought information or advice about their mental health from AI tools in the past year. Comparably, large shares of the public report seeking physical or mental health information and advice from a health care professional (80%) or an internet search engine (68%) in the past year. Given that many search engines now provide AI-generated summaries of search results, much of the public may be getting AI-generated health information, even if they are not looking for it.
Use of AI tools for health information is more common among younger adults (as is AI use overall), particularly when it comes to mental health. Over one-third (36%) of adults ages 18 to 29 report using AI tools or chatbots for information or advice related to their physical health in the past year and about three in ten (28%) say the same about their mental health or emotional wellbeing. Those ages 18 to 29 are at least three times as likely as adults ages 50 and older to report using AI for mental health advice (28% v. 8%).
Larger shares of uninsured adults, Black adults, and Hispanic adults report turning to AI for mental health advice in the past year compared to fewer insured adults and White adults, respectively. Use of AI for physical health advice does not differ by race and ethnicity or health insurance status. Notably, race and ethnicity, age, and health insurance coverage are interrelated, as younger adults and Hispanic adults are more likely to be uninsured.
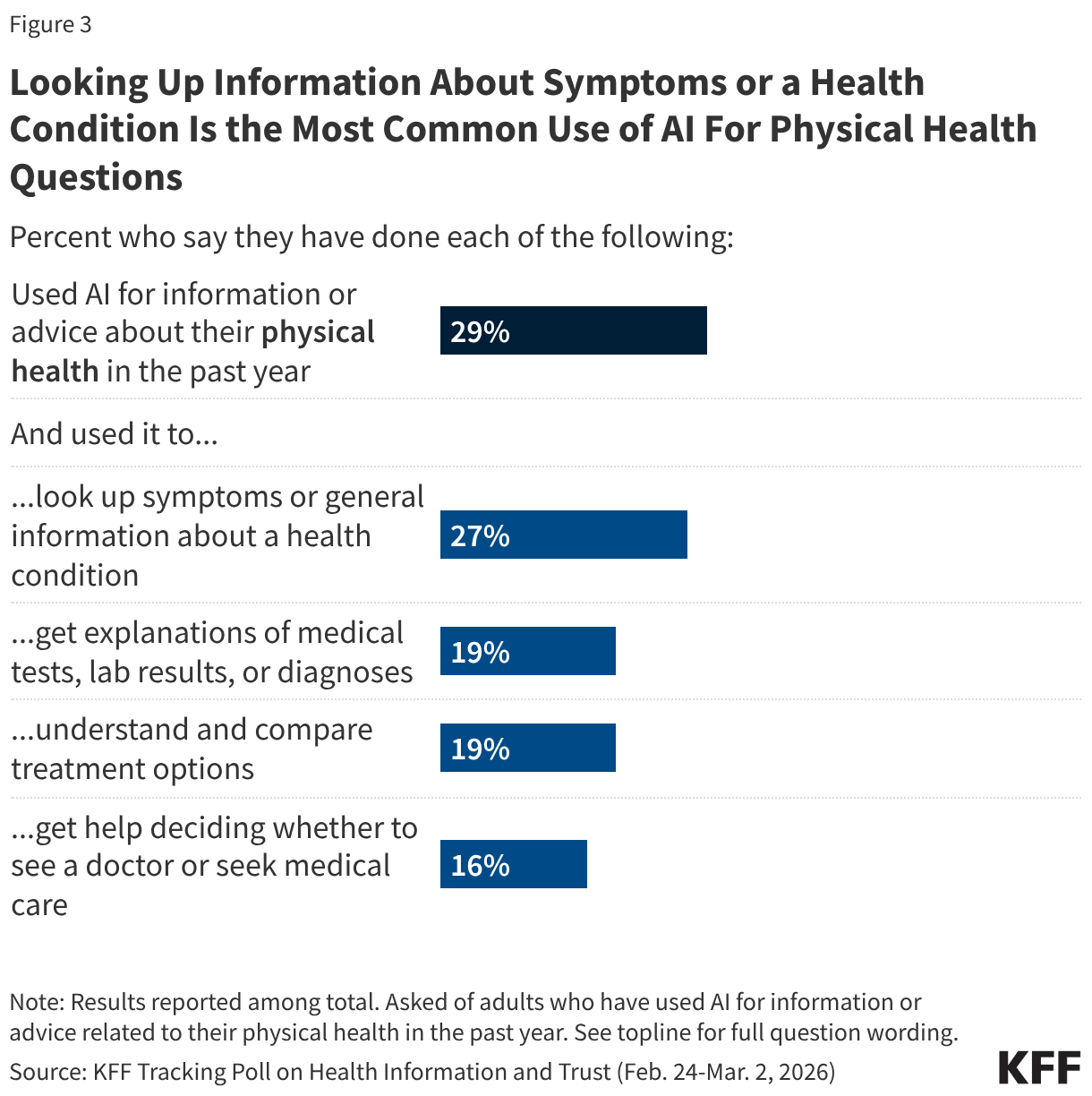
People report using AI for health information in various ways, but most commonly to look for general information about health conditions or symptoms. About a quarter (27%) of adults used AI for physical health questions in the past year and say they did so to look up symptoms or general information about health conditions. About one in five adults say they used AI to get explanations of medical tests, lab results, or diagnoses (19%) or understand and compare treatment options (19%), while about one in six (16%) say they used AI in the past year to get help deciding whether to see a doctor or seek medical care.
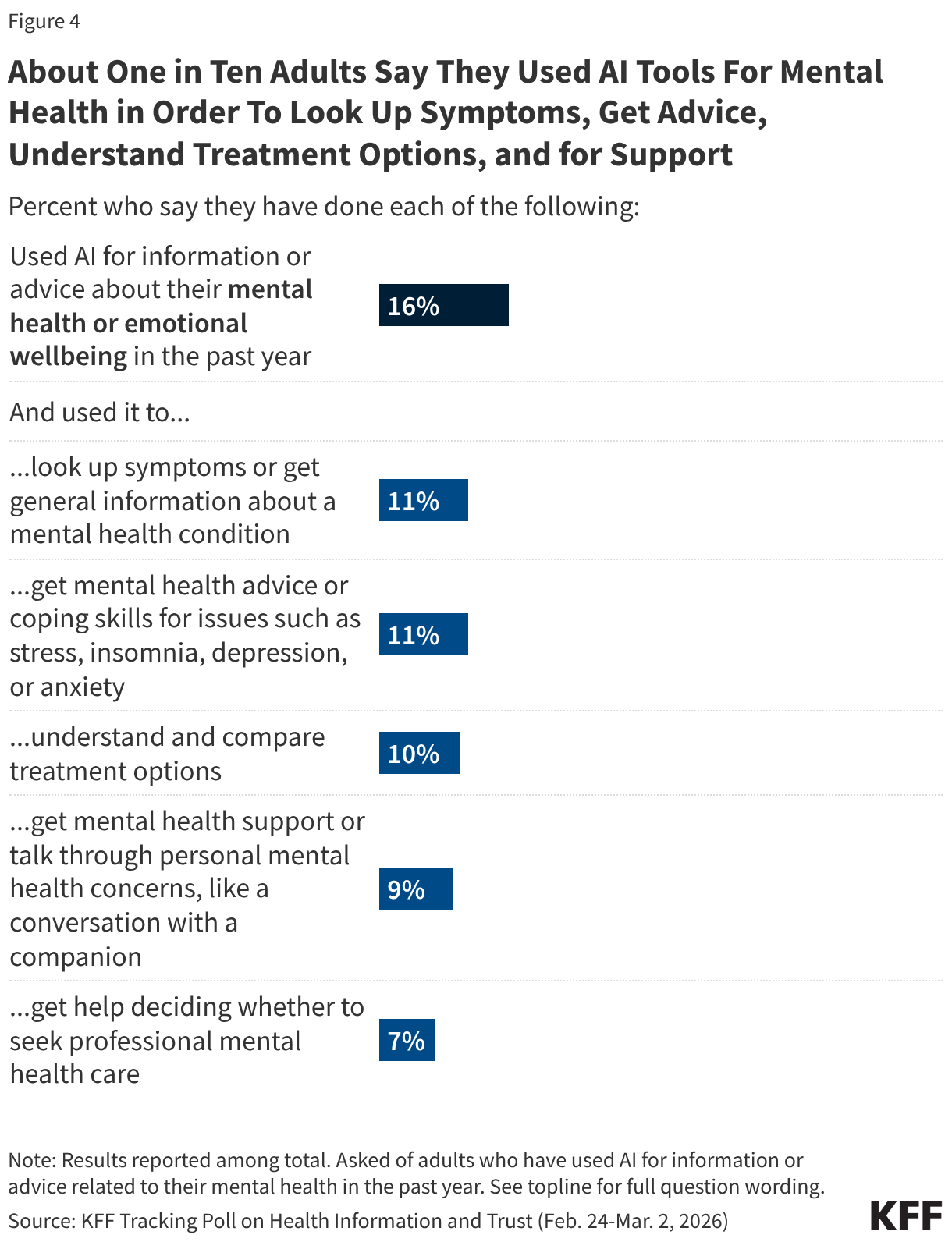
Overall, about one in ten adults say they used AI for information related to their mental health or emotional wellbeing in the past year and did so to look up symptoms or get general information about a mental health condition (11%), get advice or coping skills for mental health issues (11%), understand and compare treatment options (10%), or to talk through personal mental health concerns like a conversation with a companion (9%). Seven percent of adults say they turned to AI to get help deciding whether to seek professional mental health care.
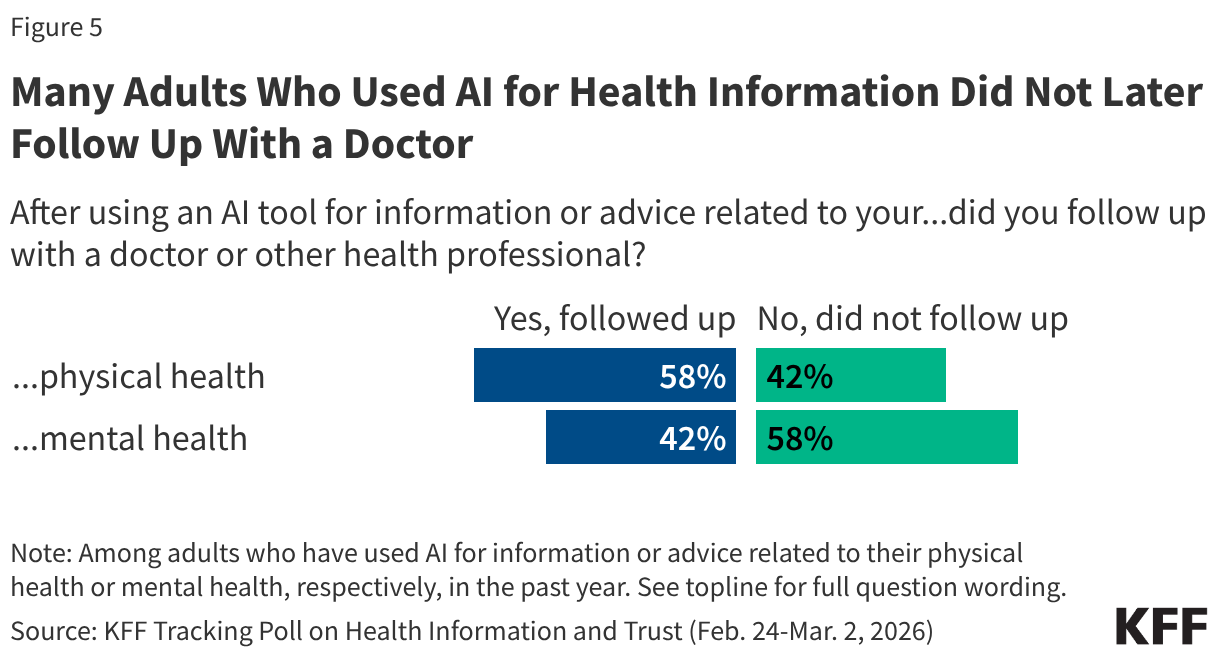
About six in ten (58%) adults who used AI for physical health advice in the past year say they later followed up with a doctor or health care provider after consulting an AI tool, while about four in ten (42%) of those who used AI for mental health say they followed up with a mental health professional.
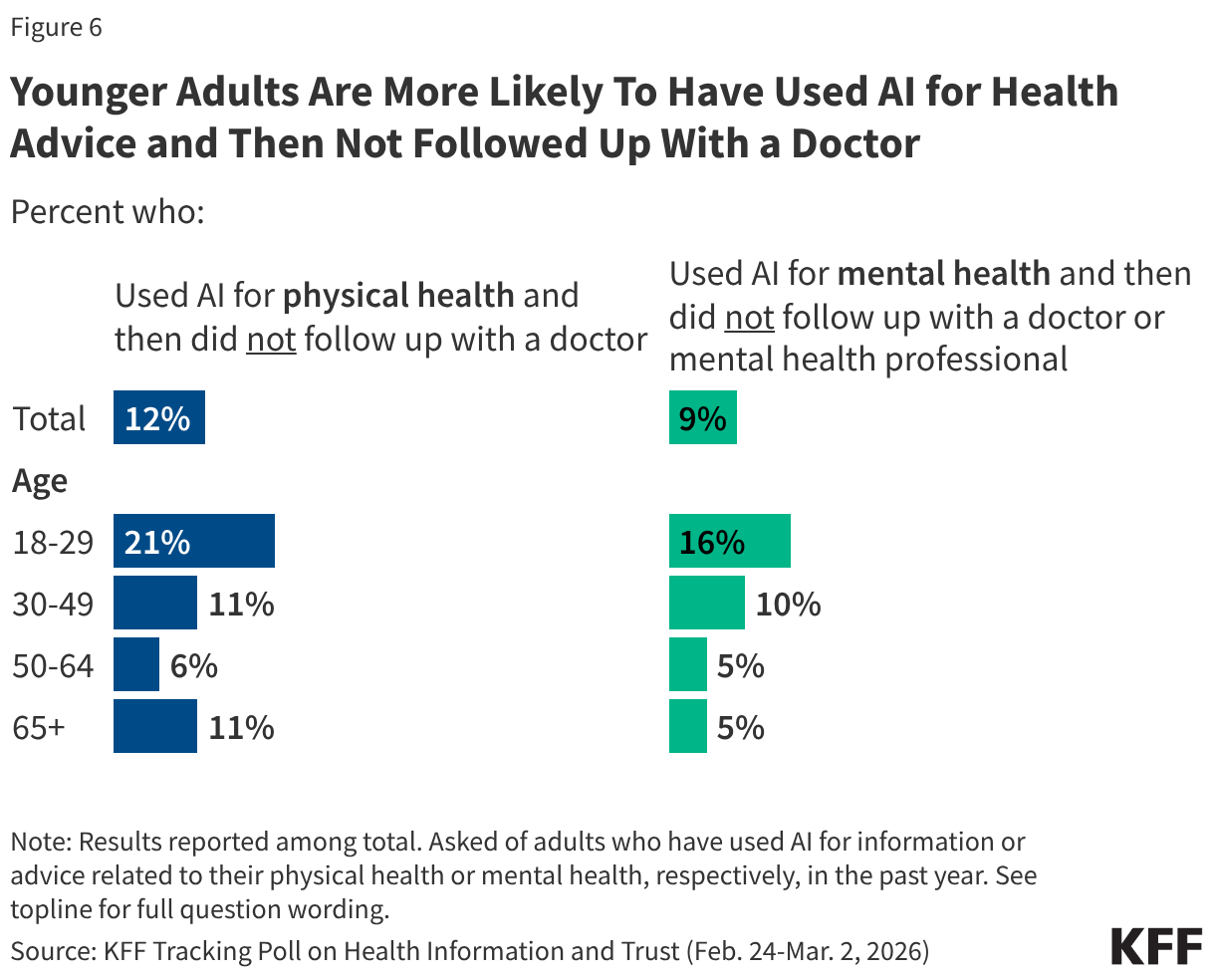
Overall, larger shares of younger adults compared with older adults report consulting AI for health information and then not following up with a doctor. About one in five (21%) adults ages 18 to 29 (who are more likely to have used AI for health in the first place) say they turned to AI for physical health advice in the past year and then did not follow up with a doctor – about twice the share of those ages 30 and older who report doing so. Similarly, about one in six (16%) adults ages 18 to 29 say they used AI for mental health advice in the past year and did not follow up with a doctor or mental health professional, more than twice the share of adults ages 50 and older who say the same.
Reasons for Using AI for Health Information and Advice
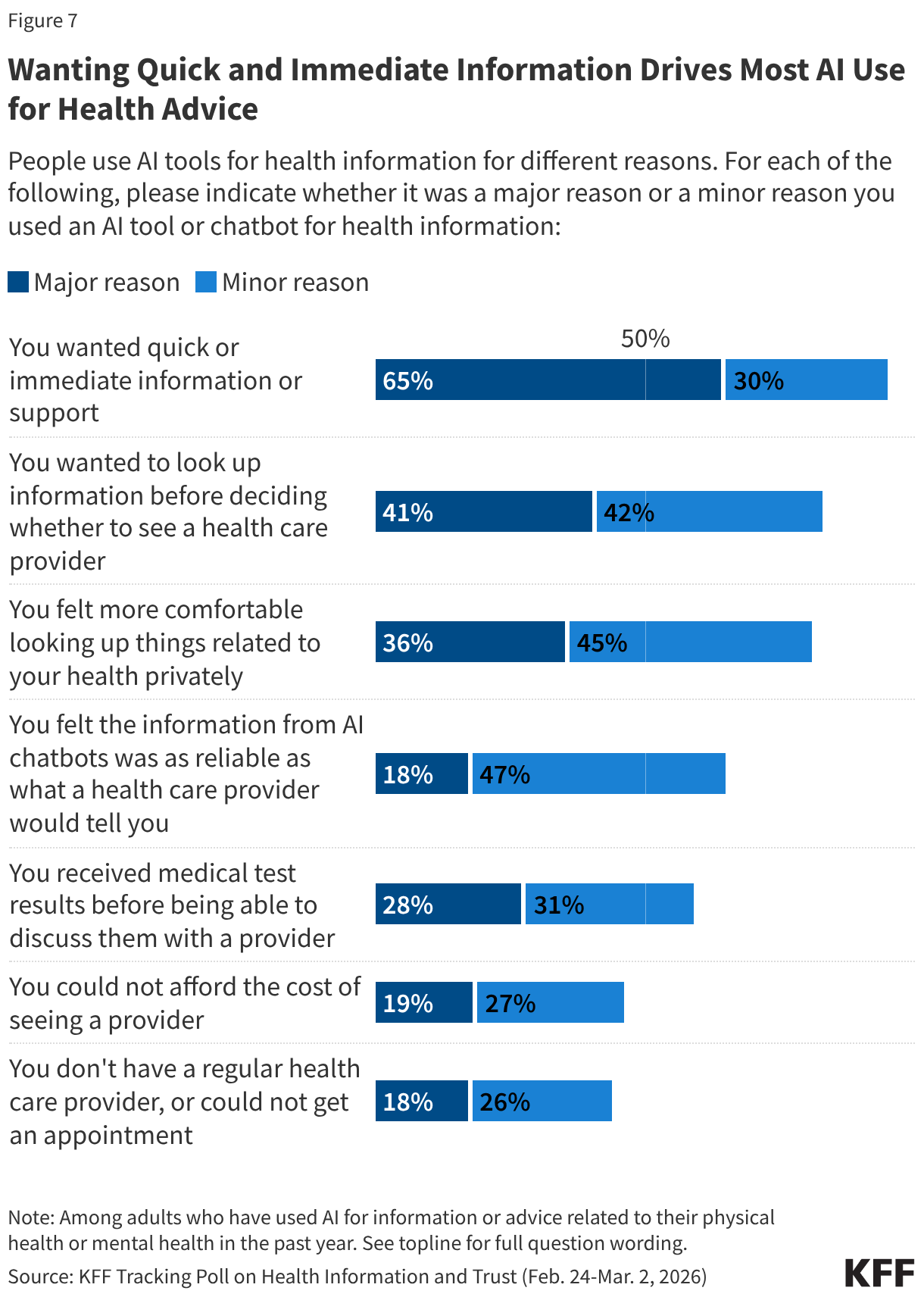
Among those who have used AI tools or chatbots for physical or mental health information in the past year (32% of all adults), most users (65%) cite wanting quick or immediate information or support as a “major reason” for doing so. Many users cite other “major” reasons, including that they wanted to look up information before deciding whether to see a provider (41%), they felt more comfortable looking up health-related topics privately (36%), or they received medical test results before being able to discuss them with provider (28%).
Some users say they turned to AI due to difficulty accessing or affording health care, with about one in five saying a “major reason” they used AI for health was because they could not afford the cost of seeing a provider (19%) or they don’t have a regular health care provider or could not get an appointment (18%).
While about one in five AI users (18%) say a “major reason” they used AI for health was because they felt the information was as reliable as what a health care provider would tell them, most users (65%) say this was at least a “minor reason” for using AI.
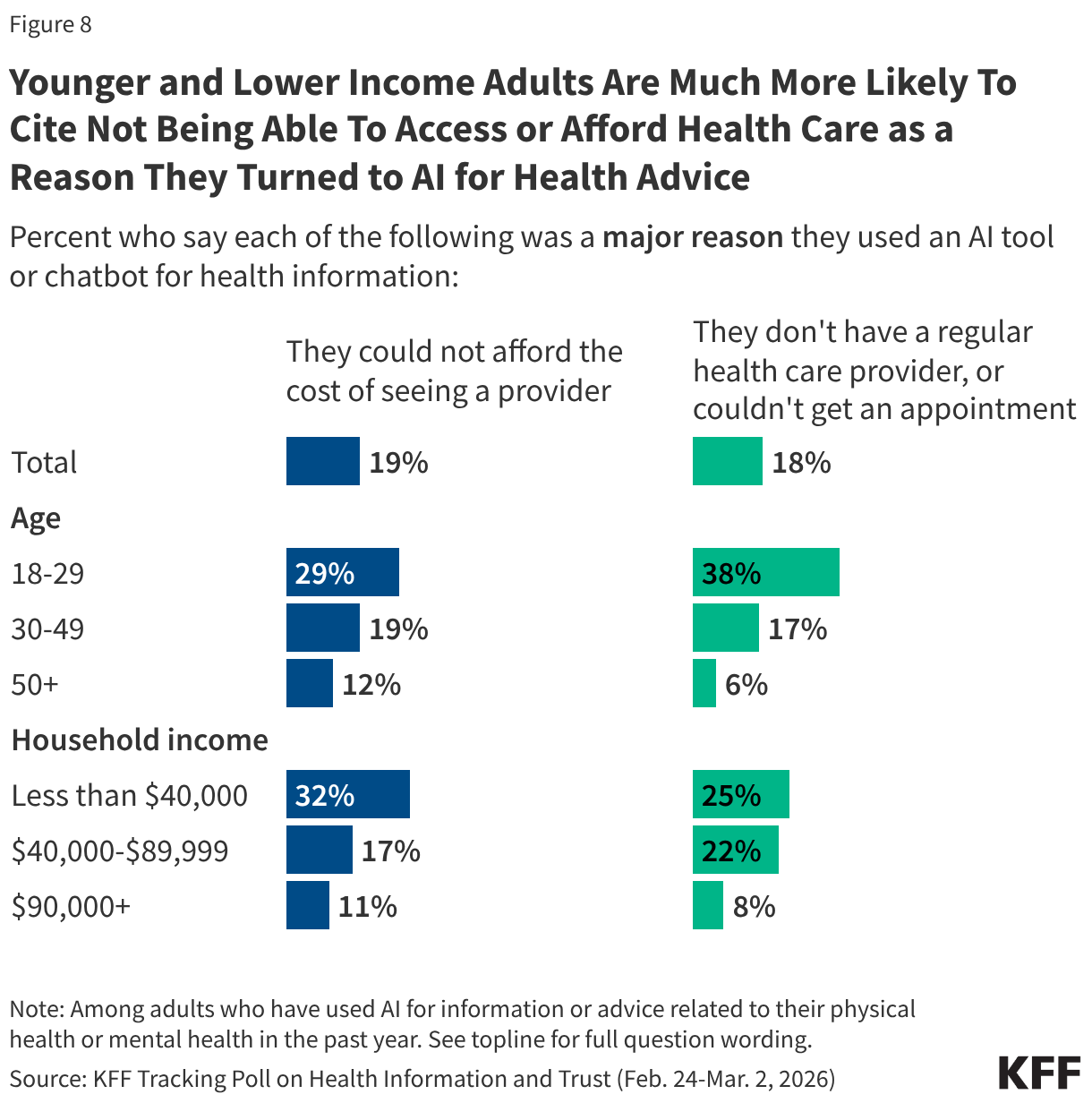
While wanting quick or immediate information is the top reason for using AI across groups, younger adults and lower-income adults are more likely to cite difficulty accessing or affording health care as their reason for relying on AI for health information. Among those who have used AI for health information in the past year, adults under age 30 are six times as likely as users 50 and older to cite not having a regular health care provider or being unable to get an appointment (38% v. 6%) and more than twice as likely to cite not being able to afford the cost of a provider (29% v. 12%) as major reasons for turning to AI for health advice. Among adults with annual household incomes less than $40,000 who have used AI for health, one-third (32%) cite not being able to afford a health care provider as a “major reason” for using AI, while one in four cite not having a regular health care provider.
Notably, younger adults are more likely than older adults to not have health insurance coverage and to have lower annual household incomes.
Trust and Satisfaction in AI for Health Information and Advice
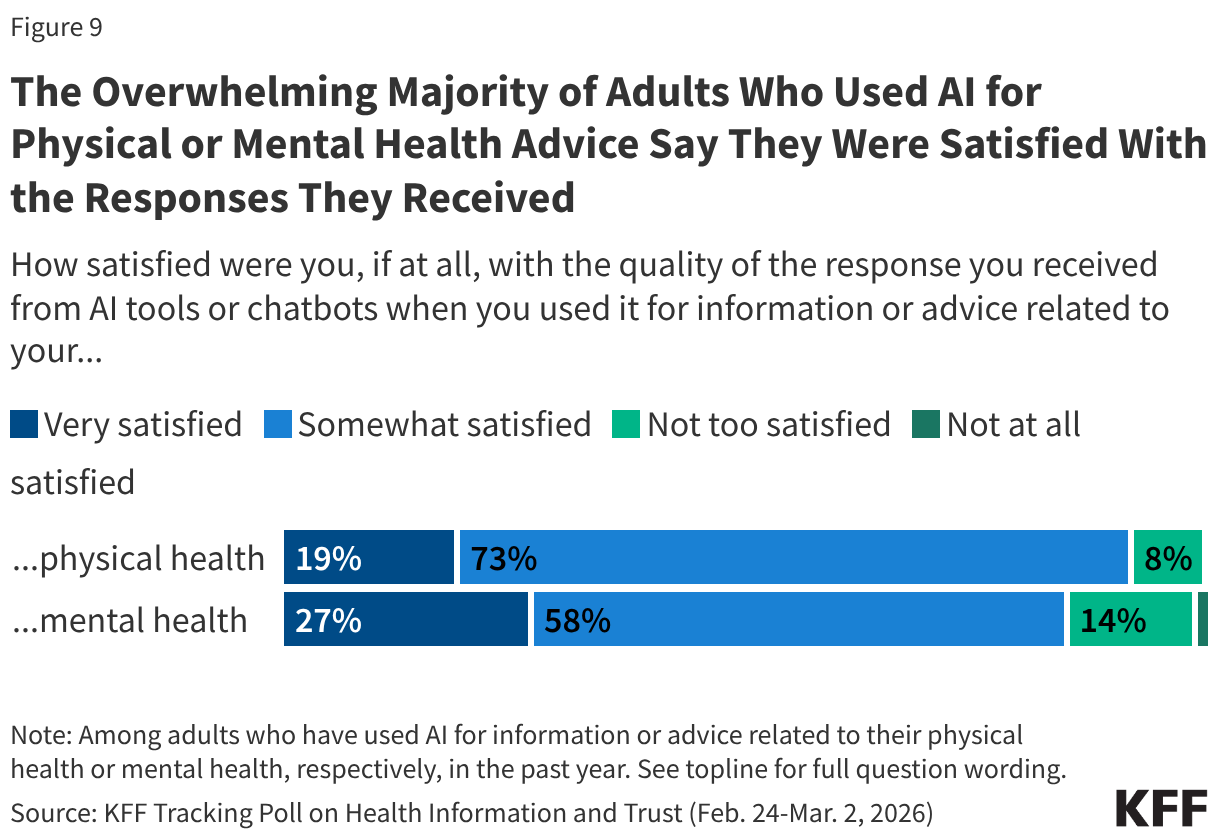
Among adults who used AI for physical or mental health advice in the past year, large majorities say they were at least “somewhat satisfied” with the quality of the responses they received related to their physical health (92%) or mental health (85%), though relatively small shares say they were “very satisfied” (19% and 27%, respectively).
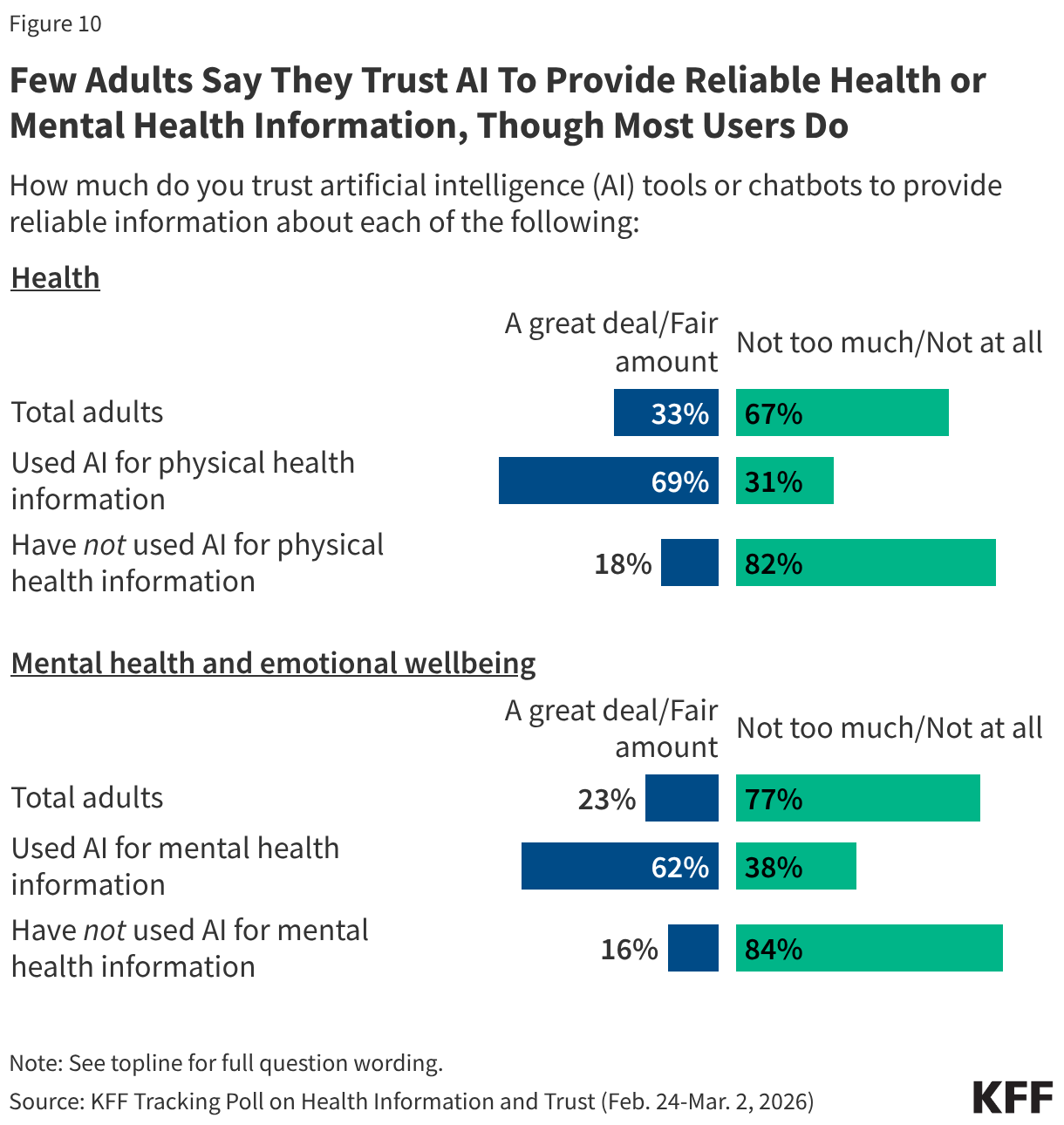
At least six in ten adults who have used AI for advice related to their physical health or mental health say they trust AI tools “a great deal” or “a fair amount” to provide reliable information about health (69%) or mental health (62%), respectively.
On the other hand, trust in AI tools for health information is relatively low among the public overall, and especially among those who have not used these tools. Trust in AI for health information drops to about one in five (18%) among adults who have not used AI for physical health advice, while trust in AI for mental health information drops to about one in six (16%) among those who have not used AI for mental health advice.
Privacy Concerns and Uploading Personal Medical Data to AI
Recently, several major technology companies have launched dedicated AI health products, promoting them as personalized health tools where users can connect and upload their medical records. Although most adults, including AI users, have concerns about privacy of personal medical information provided to AI chatbots, many who use AI for health still report uploading personal medical information to an AI tool or chatbot.
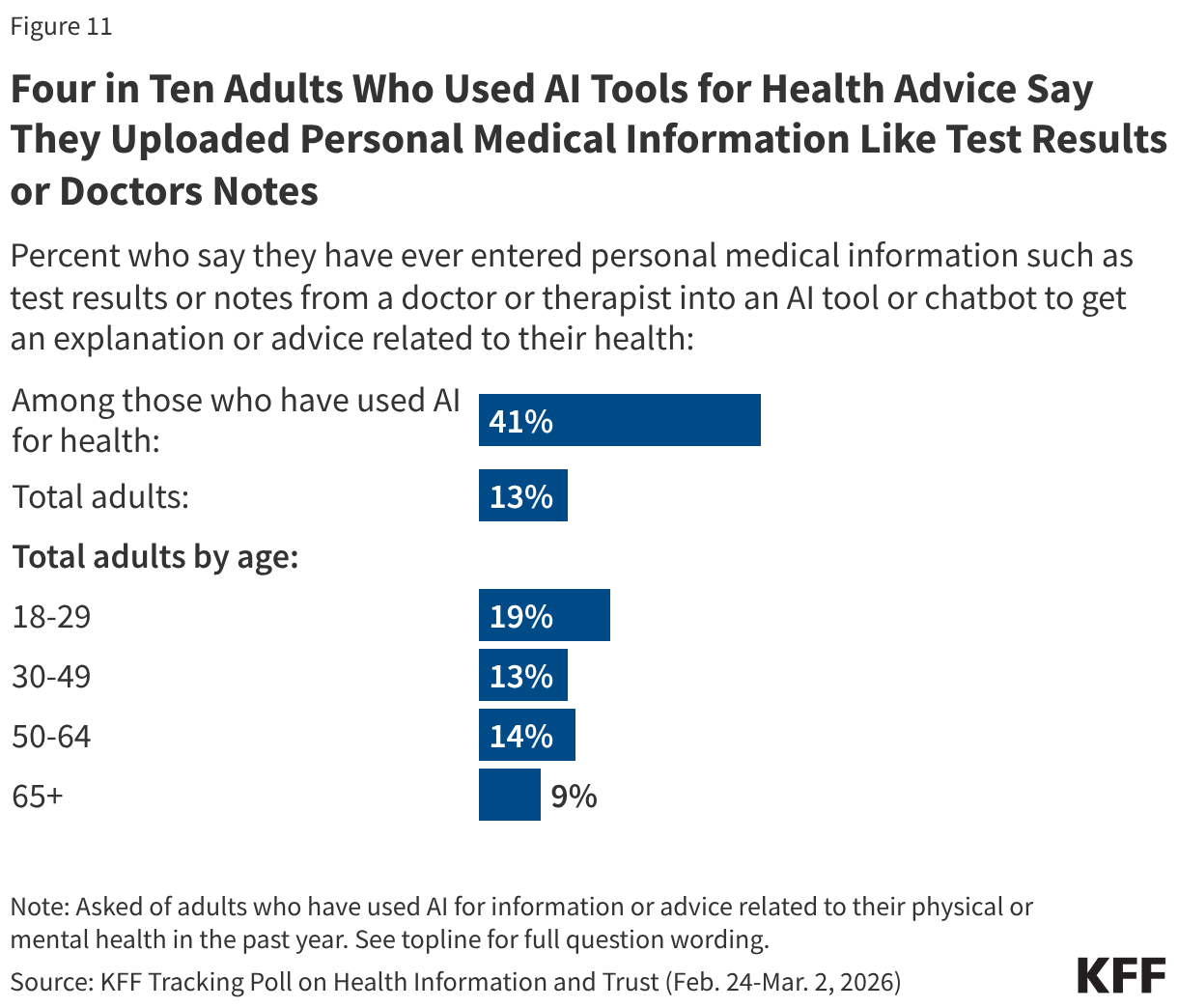
Among adults who have used AI for physical or mental health information in the past year (32% of all adults), about four in ten (41%) say they have uploaded personal medical information like test results or doctor’s notes. Overall, this means 13% of all adults say they have entered personal medical information into an AI tool to get an explanation or advice related to their health, rising to about one in five adults ages 18 to 29 (19%).
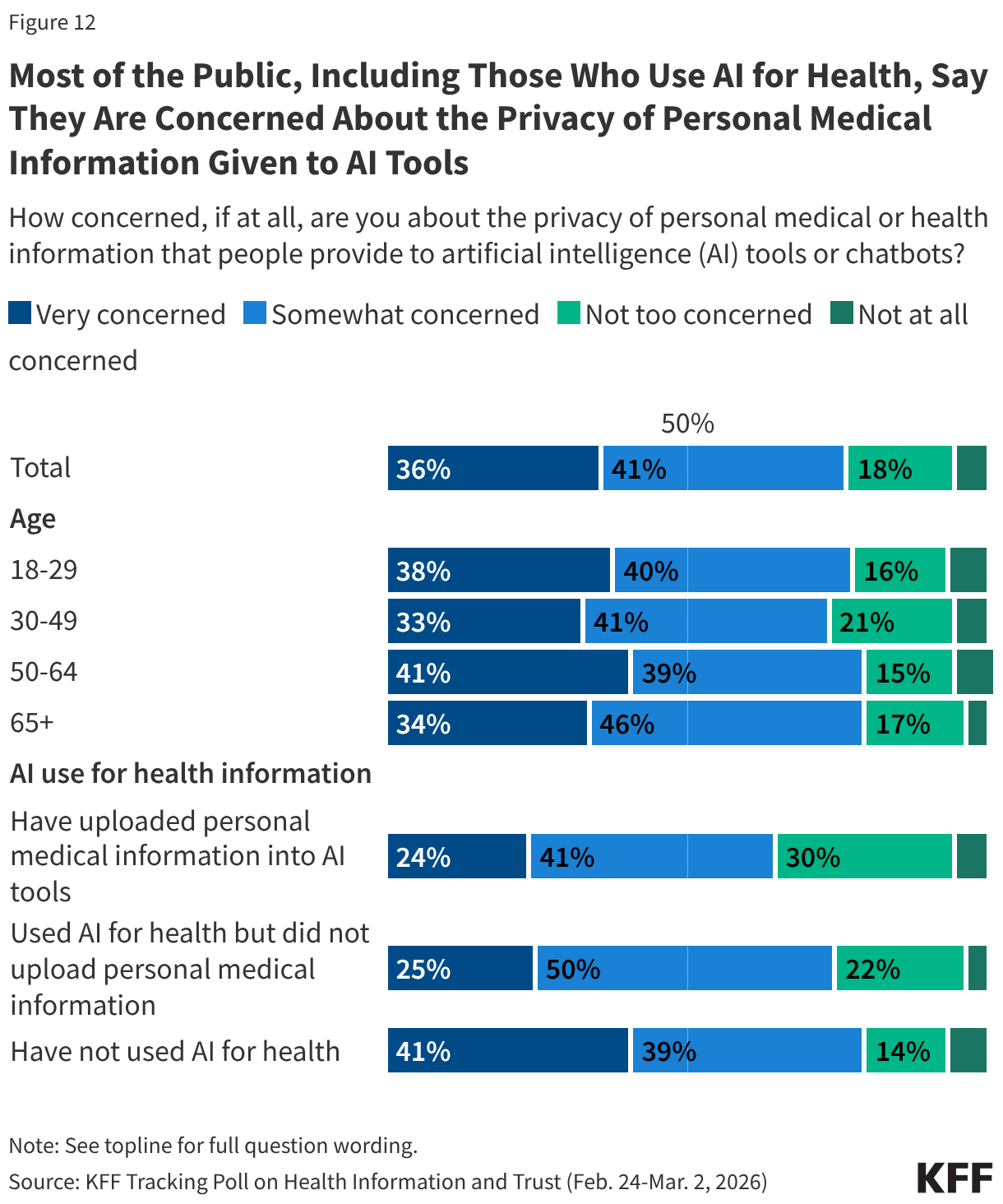
Although AI chatbots are commonly trained on user conversations, some AI companies have said that conversations with their health-specific AI tools won’t be used for training. Still, a large majority of the public, including most AI users, say they have concerns about the privacy of personal health information uploaded to AI chatbots. About three in four (77%) adults say they are either “very” or “somewhat” concerned about the privacy of personal medical information provided to AI tools, including similar shares across age groups.
Even among adults who report having entered personal medical information into an AI tool, most (65%) say they are concerned about privacy of this information, though just a quarter say they are “very concerned.”
Methodology
This KFF Health Tracking Poll/KFF Tracking Poll on Health Information and Trust was designed and analyzed by public opinion researchers at KFF. The survey was conducted February 24 – March 2, 2026, online and by telephone among a nationally representative sample of 1,343 U.S. adults in English (n=1,268) and in Spanish (n=75). The sample includes 1,019 adults (n=62 in Spanish) reached through the SSRS Opinion Panel either online (n=995) or over the phone (n=24). The SSRS Opinion Panel is a nationally representative probability-based panel where panel members are recruited randomly in one of two ways: (a) Through invitations mailed to respondents randomly sampled from an Address-Based Sample (ABS) provided by Marketing Systems Groups (MSG) through the U.S. Postal Service’s Computerized Delivery Sequence (CDS); (b) from a dual-frame random digit dial (RDD) sample provided by MSG. For the online panel component, invitations were sent to panel members by email followed by up to three reminder emails.
Another 324 (n=13 in Spanish) adults were reached through random digit dial telephone sample of prepaid cell phone numbers obtained through MSG. Phone numbers used for the prepaid cell phone component were randomly generated from a cell phone sampling frame with disproportionate stratification aimed at reaching Hispanic and non-Hispanic Black respondents. Stratification was based on incidence of the race/ethnicity groups within each frame. Among this prepaid cell phone component, 142 were interviewed by phone and 182 were invited to the web survey via short message service (SMS).
Respondents in the prepaid cell phone sample who were interviewed by phone received a $15 incentive via a check received by mail or an electronic gift card incentive. Respondents in the prepaid cell phone sample reached via SMS received a $10 electronic gift card incentive. SSRS Opinion Panel respondents received a $5 electronic gift card incentive (some harder-to-reach groups received a $10 electronic gift card). In order to ensure data quality, cases were removed if they failed two or more quality checks: (1) attention check questions in the online version of the questionnaire, (2) had over 30% item non-response, or (3) had a length less than one quarter of the mean length by mode. Based on this criterion, 1 case was removed.
The combined cell phone and panel samples were weighted to match the sample’s demographics to the national U.S. adult population using data from the Census Bureau’s 2024 Current Population Survey (CPS), September 2023 Volunteering and Civic Life Supplement data from the CPS, and the 2025 KFF Benchmarking Survey with ABS and prepaid cell phone samples. The demographic variables included in weighting for the general population sample are gender, age, education, race/ethnicity, region, civic engagement, frequency of internet use and political party identification. The weights account for differences in the probability of selection for each sample type (prepaid cell phone and panel). This includes adjustment for the sample design and geographic stratification of the cell phone sample, within household probability of selection, and the design of the panel-recruitment procedure.
The margin of sampling error including the design effect for the full sample is plus or minus 3 percentage points. Numbers of respondents and margins of sampling error for key subgroups are shown in the table below. For results based on other subgroups, the margin of sampling error may be higher. Sample sizes and margins of sampling error for other subgroups are available on request. Sampling error is only one of many potential sources of error and there may be other unmeasured error in this or any other public opinion poll. KFF public opinion and survey research is a charter member of the Transparency Initiative of the American Association for Public Opinion Research.
| Group | N (unweighted) | M.O.S.E. |
|---|---|---|
| Total | 1,343 | ± 3 percentage points |
| Party ID | ||
| Democrats | 449 | ± 6 percentage points |
| Independents | 449 | ± 6 percentage points |
| Republicans | 373 | ± 6 percentage points |
| MAGA Republicans/Republican leaning independents | 334 | ± 6 percentage points |
| Used AI for health information or advice in the past year | 458 | ± 6 percentage points |
| Used for physical health information | 407 | ± 6 percentage points |
| Used for mental health information | 234 | ± 8 percentage points |